Ciprofloxacin-Collagen Conjugate in the Wound Healing Treatment
Abstract
:1. Introduction
2. Experimental Section
2.1. Materials
2.2. Instruments
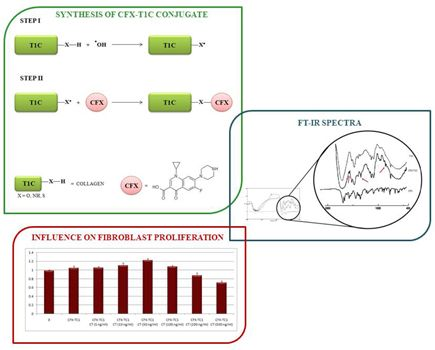
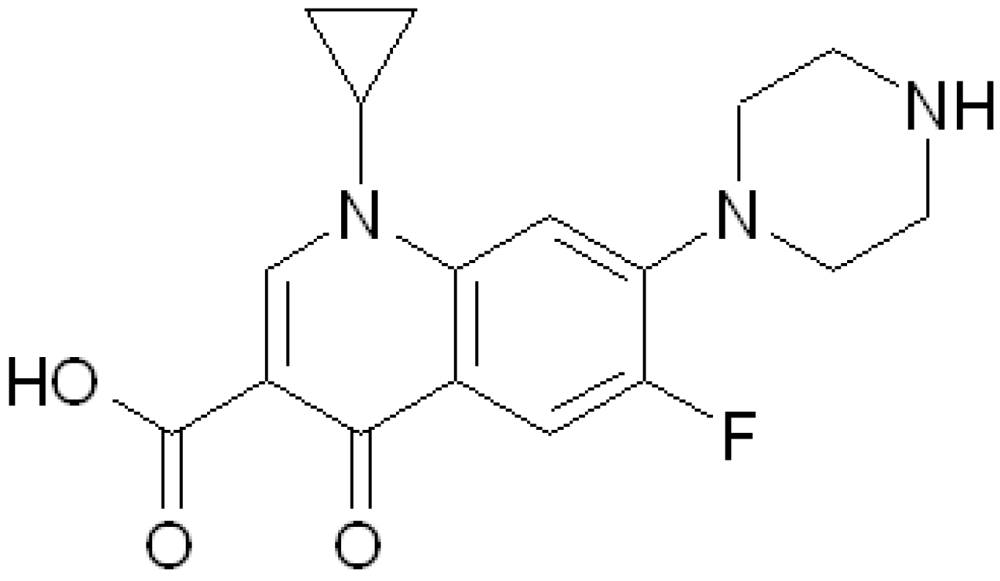
2.3. Synthesis of CFX-T1C Conjugate
2.4. Antibacterial Assay
2.5. Cell Proliferation and Viability Assay
3. Results and Discussion
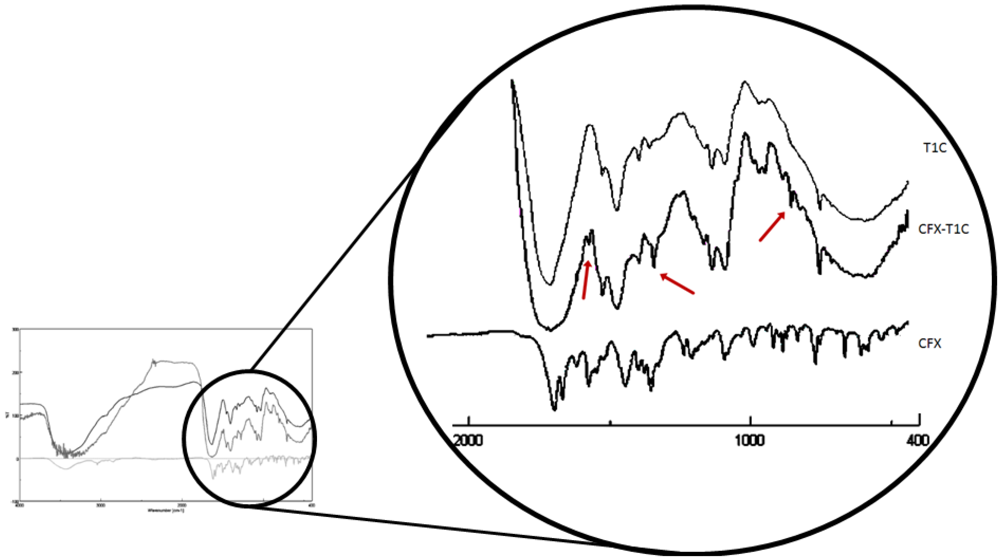
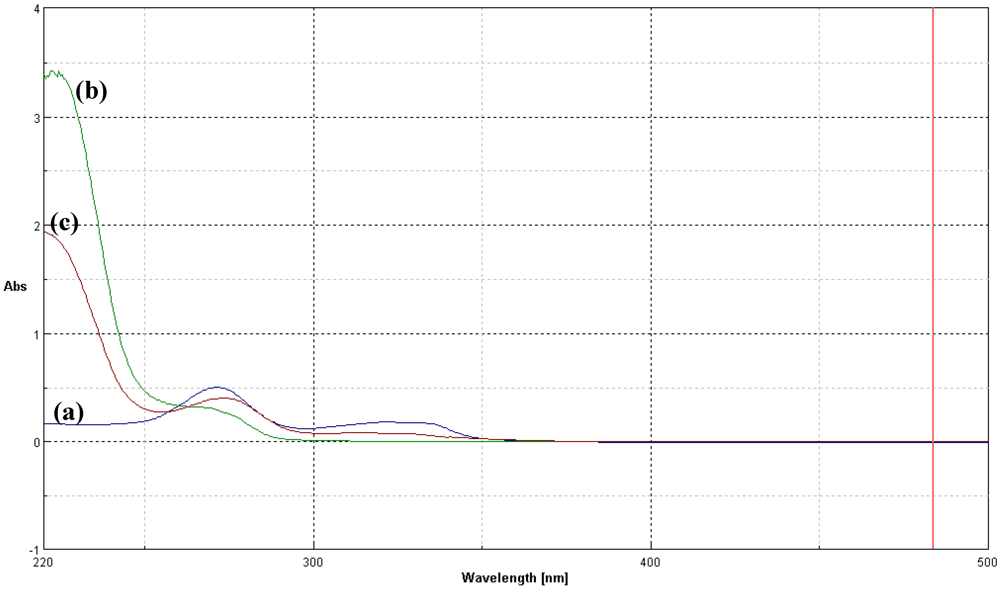
3.1. Synthesis and Characterization of CFX-T1C Conjugate

3.2. In Vitro Wound Healing Assays
3.2.1. Antibacterial Assay
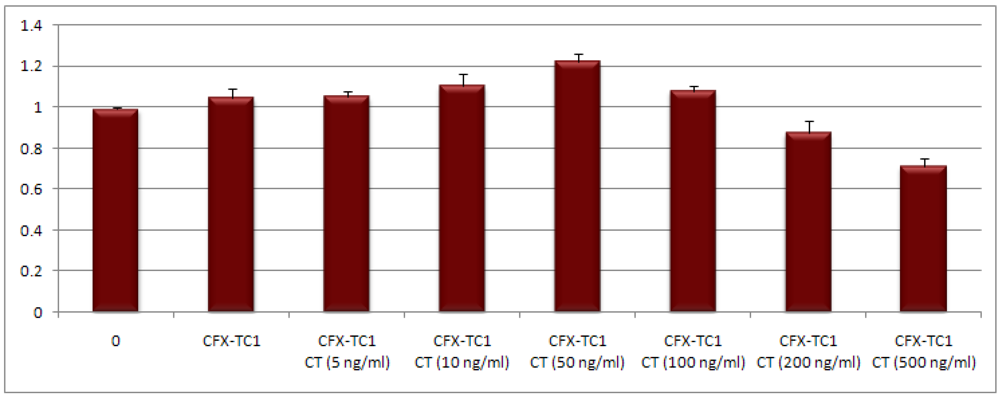
3.2.2. Influence of Catechin Blended CFX-T1C on Human fibroblast Skin Cells in Vitro
4. Conclusions
Conflict of Interest
Acknowledgments
References
- Shoulders, M.D.; Raines, R.T. Collagen structure and stability. Annu. Rev. Biochem. 2009, 78, 929–958. [Google Scholar] [CrossRef]
- Bailey, A.J.; Paul, R.G. Collagen is not so simple protein. J. Soc. Leathre Technol. Chem. 1998, 82, 104–118. [Google Scholar]
- Lee, C.H.; Singla, A.; Lee, Y. Biomedical applications of collagen. Int. J. Pharmaceut. 2001, 221, 1–22. [Google Scholar] [CrossRef]
- Antonio, F.; Guillem, R.; Sonia, T.; Clara, M.; Piergiorgio, G.; Valeria, C.; Gianluca, C.; Tzanov, T. Cross-linked collagen sponges loaded with plant polyphenols with inhibitory activity towards chronic wound enzymes. Biotechnol. J. 2011, 6, 1208–1218. [Google Scholar]
- Ueng, S.W.N.; Yuan, L.J.; Lin, S.S.; Liu, S.J.; Chan, E.C.; Chen, K.T.; Lee, M.S. In vitro and in vivo analysis of a biodegradable poly(lactide-co-glycolide) copolymer capsule and collagen composite system for antibiotics and bone cells delivery. J. Trauma 2011, 70, 1503–1509. [Google Scholar] [CrossRef]
- Beberok, A.; Buszman, E.; Wrzesniok, D.; Otreba, M.; Trzcionka, J. Interaction between ciprofloxacin and melanin: The effect on proliferation and melanization in melanocytes. Eur. J. Pharmacol. 2011, 669, 32–37. [Google Scholar] [CrossRef]
- Dizman, B.; Elasri, M.O.; Mathias, L.J. Synthesis and antibacterial activities of water-soluble methacrylate polymers containing quaternary ammonium compounds. J. Polym. Sci. Pol. Chem. 2006, 44, 5965–5973. [Google Scholar] [CrossRef]
- Adetutua, A.; Morgana, W.A.; Corcorana, O. Ethnopharmacological survey and in vitro evaluation of wound-healing plants used in south-western Nigeria. J. Ethnopharmacol. 2011, 137, 50–56. [Google Scholar] [CrossRef]
- Curcio, M.; Puoci, F.; Iemma, F.; Parisi, O.I.; Cirillo, G.; Spizzirri, U.G.; Picci, N. Covalent insertion of antioxidant molecules on chitosan by a free radical grafting procedure. J. Agric. Food Chem. 2009, 57, 5933–5938. [Google Scholar]
- Curcio, M.; Cirillo, G.; Parisi, O.I.; Iemma, F.; Spizzirri, U.G.; Altimari, I.; Picci, N.; Puoci, F. Poly(2-hydroxyethyl methacrylate)-quercetin conjugate as biomaterial in ophthalmology: An “ab initio” study. J. Funct. Biomater. 2011, 2, 1–17. [Google Scholar] [CrossRef]
- Spizzirri, U.G.; Iemma, F.; Puoci, F.; Cirillo, G.; Curcio, M.; Parisi, O.I.; Picci, N. Synthesis of antioxidant polymers by grafting of gallic acid and catechin on gelatin. Biomacromolecules 2009, 10, 1923–1930. [Google Scholar] [CrossRef]
- Spizzirri, U.G.; Parisi, O.I.; Iemma, F.; Cirillo, G.; Puoci, F.; Curcio, M.; Picci, N. Antioxidant-polysaccharide conjugates for food application by eco-friendly grafting procedure. Carbohyd. Polym. 2010, 79, 333–340. [Google Scholar] [CrossRef]
- Mertz, P.M.; Ovington, L.G. Wound-healing microbiology. Dermatol. Clinics 1993, 11, 739–747. [Google Scholar]
- Bowler, P.G.; Duerden, B.I.; Armstrong, D.G. Wound microbiology and associated approaches to wound management. Clinical Microbiol. Rev. 2001, 14, 2244–2269. [Google Scholar]
- Albu, M.G.; Ferdes, M.; Kaya, D.A.; Ghica, M.V.; Titorencu, I.; Popa, L.; Albu, L. Collagen wound dressings with anti-inflammatory activity. Mol. Cryst. Liq. Cryst. 2012, 555, 271–279. [Google Scholar]
- Woodley, D.T.; O’Keefe, E.J.; Prunerias, M. Cutaneous wound healing: A model for cell-matrix interaction. J. Am. Acad. Dermatol. 1985, 12, 420–433. [Google Scholar] [CrossRef]
- Mimura, Y.; Ihn, H.; Jinnin, M.; Asano, Y.; Yamane, K.; Tamaki, K. Epidermal growth factor induces fibronectin expression in human dermal fibroblasts via protein kinase C δ-signaling pathway. J. Invest. Dermatol. 2004, 122, 1390–1398. [Google Scholar] [CrossRef]
- Graham, M.F.; Diegelman, R.F.; Cohen, I.K. An in vitro model of fibroplasia: Simultaneous quantification of fibroblast proliferation, migration, and collagen synthesis. P. Soc. Exp. Biol. Med. 1984, 176, 302–308. [Google Scholar]
- Mensah, A.Y.; Sampson, J.; Houghton, P.J.; Hylands, P.J.; Westbrook, J.; Dunn, M.M.; Hughes, A.; Cherry, G.W. Effects of Buddlejaglobosa leaf and its constituents relevant to wound healing. J. Ethnopharmacol. 2001, 77, 219–226. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A.; Guerrieri, M.; Goteri, G.; Muzzarelli, C.; Armeni, T.; Ghiselli, R.; Cornelissen, M. The biocompatibility of dibutyryl chitin in the context of wound dressings. Biomaterials 2005, 26, 5844–5854. [Google Scholar]
- Paasche, G.; Ceschi, P.; Löbler, M.; Rösl, C.; Gomes, P.; Hahn, A.; Rohm, H.W.; Sternberg, K.; Lenarz, T.; Schmitz, K.-P.; Barcikowski, S.; Stöver, T. Effects of metal ions on fibroblasts and spiral ganglion cells. J. Neurosci. Res. 2011, 89, 611–617. [Google Scholar] [CrossRef]
- Idris, S.B.; Dånmark, S.; Finne-Wistrand, A.; Arvidson, K.; Albertsson, A.-C.; Bolstad, A.I.; Mustafa, K. Biocompatibility of polyester scaffolds with fibroblasts and osteoblast-like cells for bone tissue engineering. J. Bioact. Compat. Pol. 2010, 25, 567–583. [Google Scholar] [CrossRef]
- Ranzato, E.; Martinotti, S.; Burlando, B. Wound healing properties of jojoba liquid wax: An in vitro study. J. Ethnopharmacol. 2011, 134, 443–449. [Google Scholar] [CrossRef]
- Hincal, F.; Gürbay, A.; Favier, A. Biphasic response of ciprofloxacin in human fibroblast cell cultures. Nonlinearity Biol. Toxicol. Med. 2003, 1, 481–492. [Google Scholar] [CrossRef]
- Seto, Y.; Inoue, R.; Ochi, M.; Gandy, G.; Yamada, S.; Onoue, S. Combined use of in vitro phototoxic assessments and cassette dosing pharmacokinetic study for phototoxicity characterization of fluoroquinolones. AAPS J. 2011, 13, 482–492. [Google Scholar] [CrossRef]
- Gürbay, A.; Gonthier, B.; Barret, L.; Favier, A.; Hıncal, F. Cytotoxic effect of ciprofloxacin in primary culture of rat astrocytes and protection by Vitamin E. Toxicology 2007, 229, 54–61. [Google Scholar] [CrossRef]
- Kautzky, F.; Hartinger, A.; Kohler, L.D.; Vogt, H.-J. In vitro cytotoxicity of antimicrobial agents to human keratinocytes. J. Eur. Acad. Dermatol. 1996, 6, 159–166. [Google Scholar] [CrossRef]
- Kim, S.Y.; Kwak, J.S.; Shin, J.P.; Lee, S.H. Protection of the retina from ischemic injury by the free radical scavenger EGb-761 and zinc in the cat retina. Ophthalmologica 1998, 212, 268–274. [Google Scholar] [CrossRef]
- Stevenson, P.C.; Simmonds, M.S.; Sampson, J.; Houghton, P.J.; Grice, P. Wound healing activity of acylated iridoid glycosides from Scrophularianodosa. Phytother. Res. 2002, 16, 33–35. [Google Scholar]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Puoci, F.; Piangiolino, C.; Givigliano, F.; Parisi, O.I.; Cassano, R.; Trombino, S.; Curcio, M.; Iemma, F.; Cirillo, G.; Spizzirri, U.G.; et al. Ciprofloxacin-Collagen Conjugate in the Wound Healing Treatment. J. Funct. Biomater. 2012, 3, 361-371. https://doi.org/10.3390/jfb3020361
Puoci F, Piangiolino C, Givigliano F, Parisi OI, Cassano R, Trombino S, Curcio M, Iemma F, Cirillo G, Spizzirri UG, et al. Ciprofloxacin-Collagen Conjugate in the Wound Healing Treatment. Journal of Functional Biomaterials. 2012; 3(2):361-371. https://doi.org/10.3390/jfb3020361
Chicago/Turabian StylePuoci, Francesco, Cristiana Piangiolino, Francesco Givigliano, Ortensia Ilaria Parisi, Roberta Cassano, Sonia Trombino, Manuela Curcio, Francesca Iemma, Giuseppe Cirillo, Umile Gianfranco Spizzirri, and et al. 2012. "Ciprofloxacin-Collagen Conjugate in the Wound Healing Treatment" Journal of Functional Biomaterials 3, no. 2: 361-371. https://doi.org/10.3390/jfb3020361