Hemobilia Secondary to Transjugular Intrahepatic Portosystemic Shunt Procedure: A Case Report
Abstract
:1. Introduction
2. Case
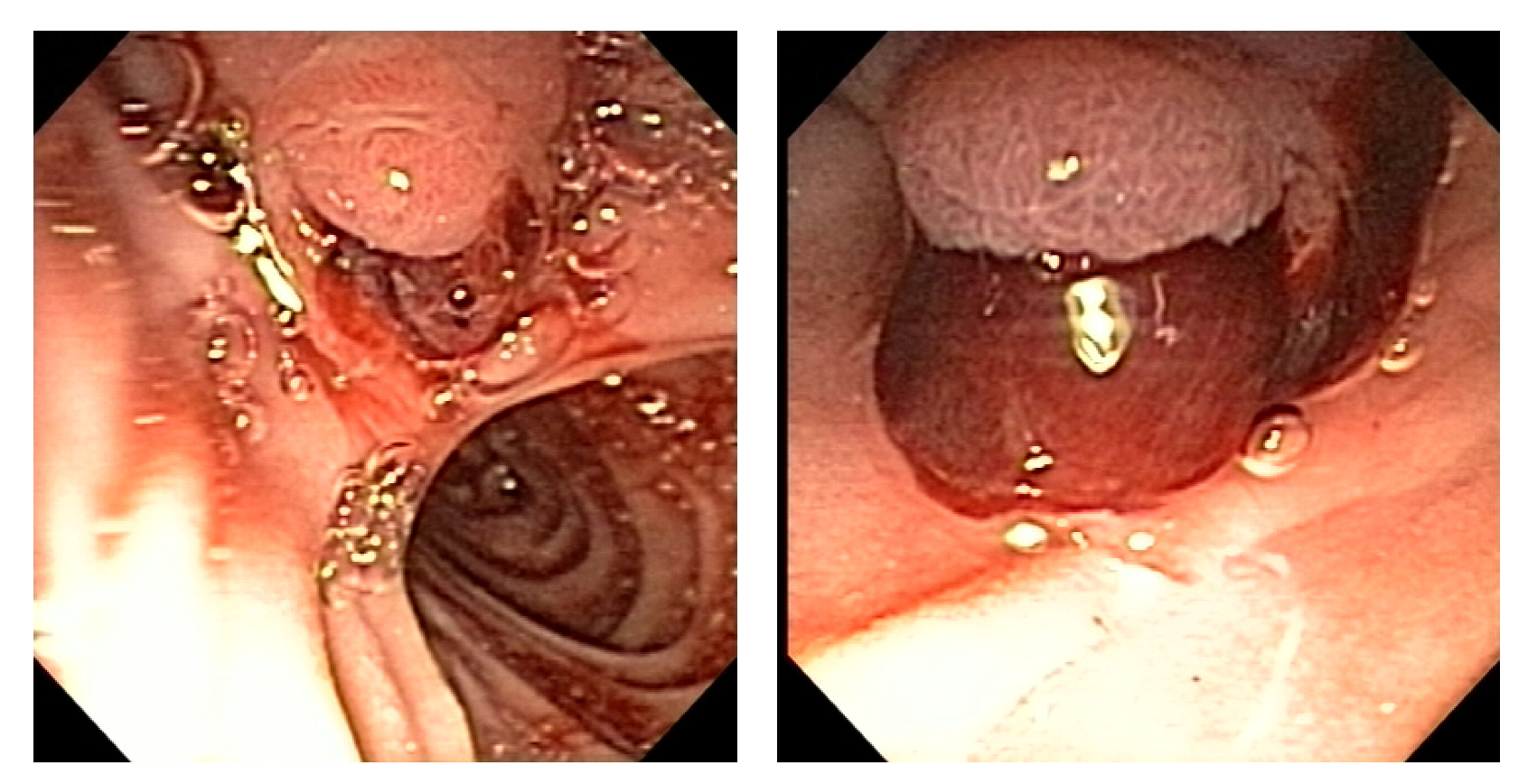
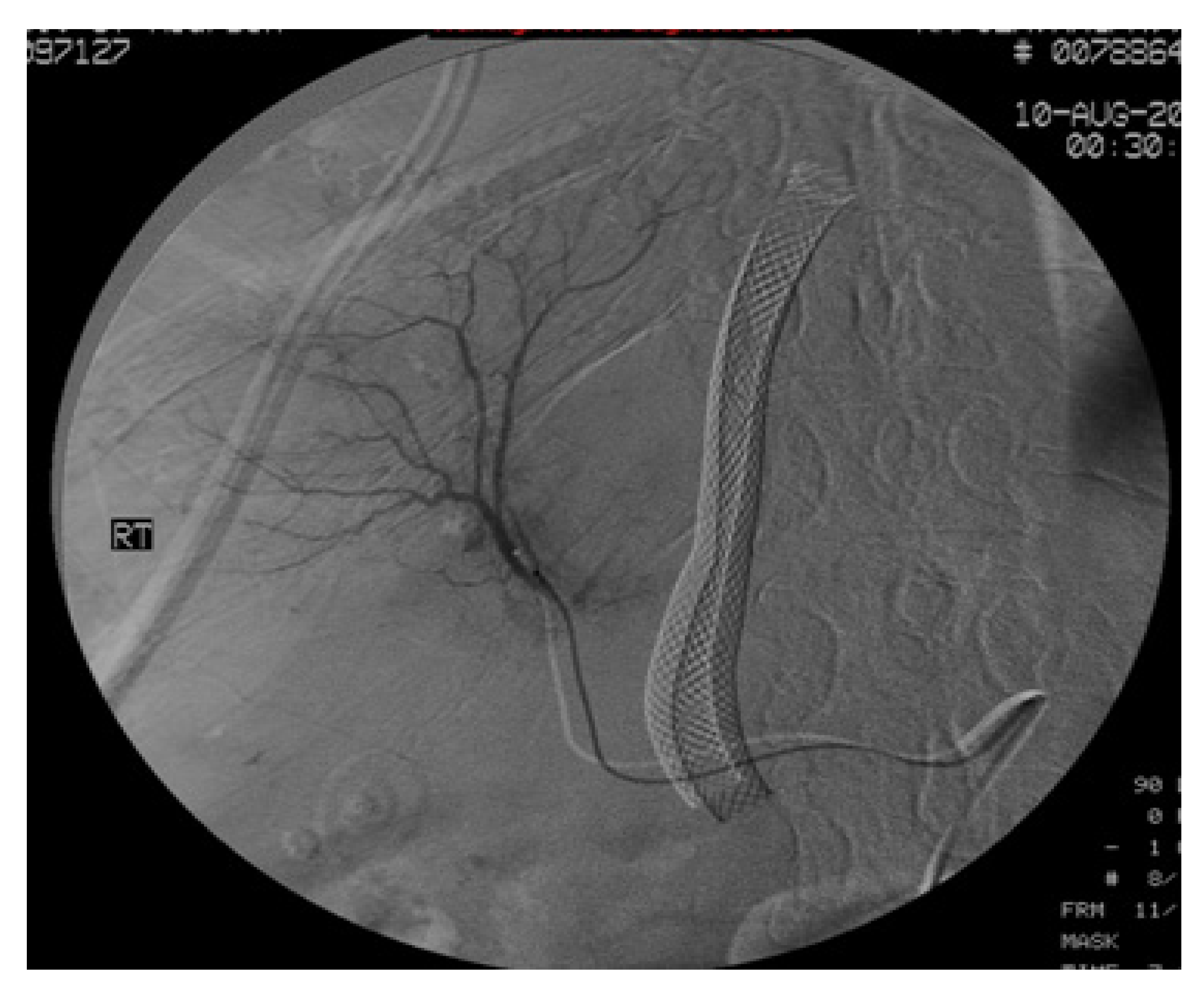

3. Discussion
| Complication of TIPS | Incidence |
|---|---|
| Direct procedure related mortality | 0–2% |
| 30 days mortality | 7%–45% |
| Aggravated or new encephalopathy | 5%–35% |
| Shunt stenosis/Occlusion | <5% |
| Infection (Infective endocarditis ) | |
| Bleeding from capsular perforation | <5% |
| Extra hepatic puncture of portal vein | <5% |
| Parenchymal injury to biliary tree or hepatic artery | <5% |
| Stent related complications—migration, infection | <5% |
| Contrast induced renal failure | |
| Cardiac arrhythmias/Heart failure | <5% |
| Shunt related complications = Encephalopathy, liver failure, pulmonary hypertension | |
| Umbilical hernia | |
| Radiation injury to Skin | |
| Other possible complications Include—Fever, muscle stiffness, bruising on the neck at point of catheter insertion |
4. Conclusion
Conflict of Interest
References
- Sandblom, P. Latrogenic hemobilia. Am. J. Surg. 1986, 151, 754–758. [Google Scholar] [CrossRef]
- Schouten van der Velden, A.P.; de Ruijter, W.M.; Janssen, C.M.; Schultze Kool, L.J.; Tan, E.C. Hemobilia as a late complication after blunt abdominal trauma: A case report and review of the literature. J. Emerg. Med. 2010, 39, 592–595. [Google Scholar] [CrossRef]
- Menzel, J.; Vestring, T.; Foerster, E.C.; Haag, K.; Roessle, M.; Domschke, W. Arterio-biliary fistula after transjugular intrahepatic portosystemic shunt: A life-threatening complication of the new technique for therapy of portal hypertension. Z. Gastroenterol. 1995, 33, 255–259. [Google Scholar]
- D’Abrigeon, G.; Blanc, P.; Bauret, P.; Taourel, P.; Larrey, D.; Michel, H. Hemobilia of late disclosure after placement of transjugular intrahepatic portacaval shunt. Gastroenterol. Clin. Biol. 1993, 17, 513–514. [Google Scholar]
- Rossle, M.; Siegerstetter, V.; Huber, M.; Ochs, A. The first decade of the transjugular intrahepatic portosystemic shunt (TIPS): State of the art. Liver 1998, 18, 73–89. [Google Scholar]
- Rosch, J.; Keller, F.S. Transjugular intrahepatic portosystemic shunt: Present status, comparison with endoscopic therapy and shunt surgery, and future prospectives. World J. Surg. 2001, 25, 337–345, discussion 345–346.. [Google Scholar] [CrossRef]
- Boyer, T.D.; Haskal, Z.J. The role of transjugular intrahepatic portosystemic shunt in the management of portal hypertension. Hepatology 2005, 41, 386–400. [Google Scholar]
- Freedman, A.J.; Sanyal, A.M.; Tisnado, J.; Cole, P.E.; Shiffman, M.L.; Luketic, V.A.; Purdum, P.P.; Darcy, M.D.; Posner, M.P. Complications of transjugular intrahepatic portosystemic shunt: A comprehensive review. Radiographics 1993, 13, 1185–1210. [Google Scholar]
- Sandblom, P.; Chabloz, R. Iatrogenic hemobilia. Rev. Med. Suisse Romande 1986, 106, 657–661. [Google Scholar]
- Khan, R.; Sapkota, B.; Goldenberg, G.; Mansour, M.; Notar-Francesco, V.; Cerulli, M.A. Bleeding bile (hemobilia): An obscure cause of upper gastrointestinal bleeding: Case report and review of the literature. Practical Gastroenterol. 2010, 34, 36–43. [Google Scholar]
- Sarr, M.G.; Kaufman, S.L.; Zuidema, G.D.; Cameron, J.L. Management of hemobilia associated with transhepatic internal biliary drainage catheters. Surgery 1984, 95, 603–607. [Google Scholar]
- Cahow, C.E.; Burrell, M.; Greco, R. Hemobilia following percutaneous transhepatic cholangiography. Ann. Surg. 1977, 185, 235–241. [Google Scholar] [CrossRef]
- Okuda, K.; Musha, H.; Nakajima, Y.; Takayasu, K.; Suzuki, Y.; Morita, M.; Yamasaki, T. Frequency of intrahepatic arteriovenous fistula as a sequela to percutaneous needle puncture of the liver. Gastroenterology 1978, 74, 1204–1207. [Google Scholar]
- Merrell, S.W.; Schnerder, P.D. Hemobilia—evolution of current diagnosis and treatment. West. J. Med. 1991, 155, 621–625. [Google Scholar]
- Sabate, M.; Ibanez, L.; Perez, E.; Vidal, X.; Buti, M.; Xiol, X.; Mas, A.; Guarner, C.; Forne, M.; Sola, R.; et al. Paracetamol in therapeutic dosages and acute liver injury: Causality assessment in a prospective case series. BMC Gastroenterol. 2011, 11. [Google Scholar] [CrossRef]
- Hendren, W.H.; Warshaw, A.L.; Fleischli, D.J.; Bartlett, M.K. Traumatic hemobilia: Non-operative management with healing documented by serial angiography. Ann. Surg. 1971, 174, 991–993. [Google Scholar]
- Mizobata, Y.; Yokota, J.; Yajima, Y.; Sakashita, K. Two cases of blunt hepatic injury with active bleeding from the right inferior phrenic artery. J. Trauma 2000, 48, 1153–1155. [Google Scholar] [CrossRef]
- Baker, A.R.; Corlett, S.K.; Cookson, J.B.; Carr-Locke, D.L. Hemobilia treated by nasobiliary catheterization. Am. J. Gastroenterol. 1987, 82, 783–785. [Google Scholar]
- Yoshida, J.; Donahue, P.E.; Nyhus, L.M. Hemobilia: Review experience with a worldwide problem. Am. J. Gastroenterol. 1987, 82, 448–453. [Google Scholar]
- Carpenter, C.M.; Bowers, J.H.; Luers, P.R.; Dixon, J.A.; Miller, F.J. Neodymium yttrium aluminum gamet laser treatment of hemobilia via percutaneous biliary catheter track. Radiology 1983, 148, 853–854. [Google Scholar]
- Ohnishi, K.; Yoshioka, H.; Ito, S.; Fujiwara, K. Prospective randomized controlled trial comparing percutaneous acetic acid injection and percutaneous ethanol injection for small hepatocellular carcinoma. Hepatology 1998, 27, 67–72. [Google Scholar] [CrossRef]
- Liu, T.T.; Hou, M.C.; Lin, H.C.; Chang, F.Y.; Lee, S.D. Life-threatening hemobilia caused by hepatic artery pseudoaneurysm: A rare complication of chronic cholangitis. World J. Gastroenterol. 2003, 9, 2883–2884. [Google Scholar]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Kaswala, D.; Gandhi, D.; Moroianu, A.; Patel, J.; Patel, N.; Klyde, D.; Brelvi, Z. Hemobilia Secondary to Transjugular Intrahepatic Portosystemic Shunt Procedure: A Case Report. J. Clin. Med. 2012, 1, 15-21. https://doi.org/10.3390/jcm1010015
Kaswala D, Gandhi D, Moroianu A, Patel J, Patel N, Klyde D, Brelvi Z. Hemobilia Secondary to Transjugular Intrahepatic Portosystemic Shunt Procedure: A Case Report. Journal of Clinical Medicine. 2012; 1(1):15-21. https://doi.org/10.3390/jcm1010015
Chicago/Turabian StyleKaswala, Dharmesh, Divyang Gandhi, Andrew Moroianu, Jina Patel, Nitin Patel, David Klyde, and Zamir Brelvi. 2012. "Hemobilia Secondary to Transjugular Intrahepatic Portosystemic Shunt Procedure: A Case Report" Journal of Clinical Medicine 1, no. 1: 15-21. https://doi.org/10.3390/jcm1010015
APA StyleKaswala, D., Gandhi, D., Moroianu, A., Patel, J., Patel, N., Klyde, D., & Brelvi, Z. (2012). Hemobilia Secondary to Transjugular Intrahepatic Portosystemic Shunt Procedure: A Case Report. Journal of Clinical Medicine, 1(1), 15-21. https://doi.org/10.3390/jcm1010015




