A Multi-Camera System for Bioluminescence Tomography in Preclinical Oncology Research
Abstract
:1. Introduction
2. Experimental Section
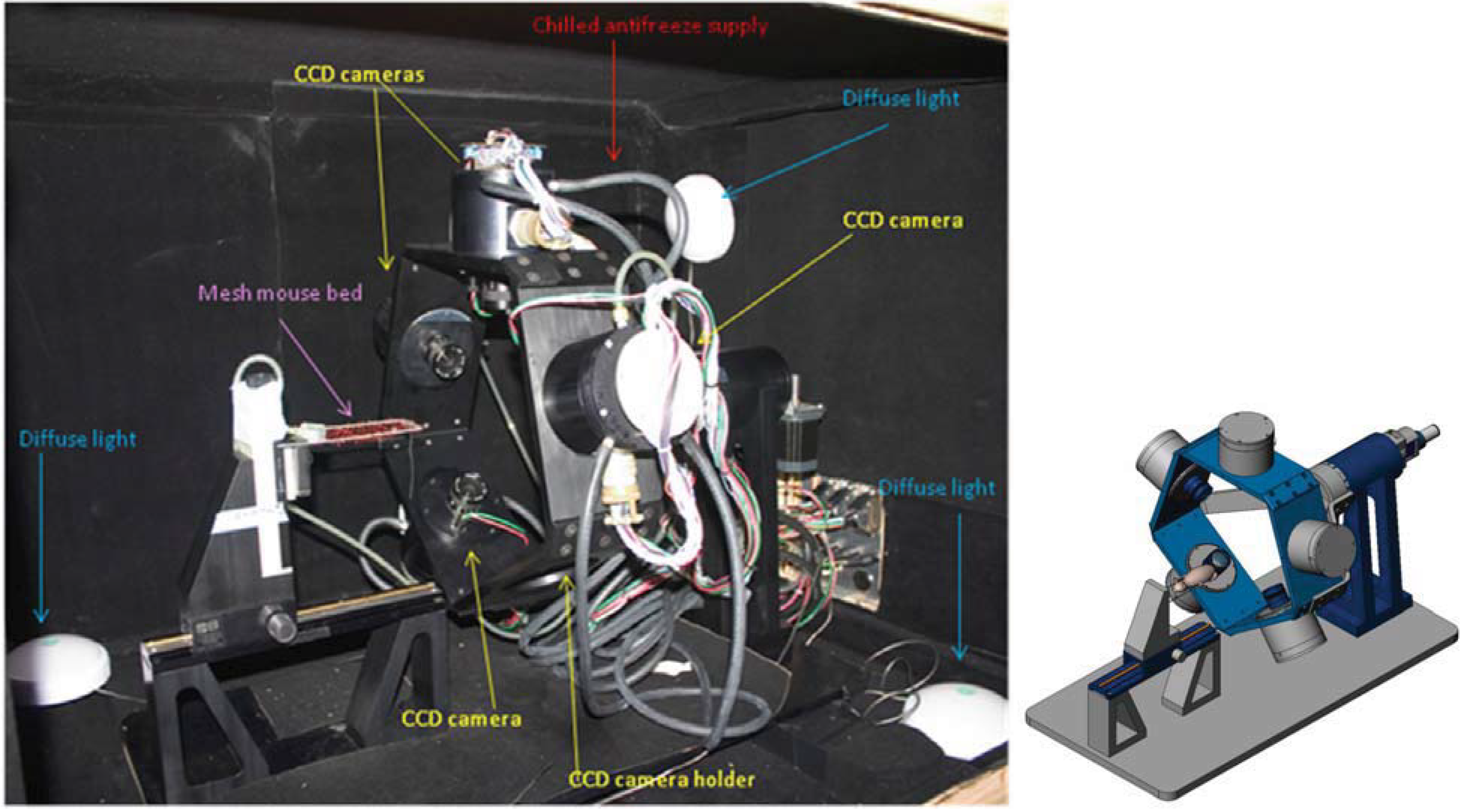
2.1. Device and Technological Rationale

2.2. High Sensitivity CCD Camera
2.3. Multiple Head Optical Imaging System
2.4. Image Reconstruction Software
- (1)
- Estimate the source location by backprojecting the experimental data into the volume discretized into voxels, calculate the intensity of reflection on boundary for each voxel j, and subtract its contribution from the transmitted part of intensity. The diffusion equation is used to determine the balance intensities for internal sources NS for the surface element in a single voxel.
- (2)
- For each voxel j determine an initial order approximation for the photon fluence:where µeff = (µ𝑎/D)1/2 The initial photon fluence φoj depends upon the pathlength from source in voxel i to voxel j on the surface, intensities in the detectors from source in medium pti, intensity estimates poi, the steady-state source power S′o, and the optical properties of the medium D and µ𝑎, the diffusion and absorption coefficients respectively.
- (3)
- Apply the iterative deblurring Expectation Maximization method to obtain a final reconstruction result φjn+1:where ⊗ denotes convolution procedure, ϱ is a Gaussian deblurring kernel, and n denotes the iteration number. In practice, the image reconstruction procedure takes 15–20 min on a desktop Linux workstation.
3. Results and Discussion
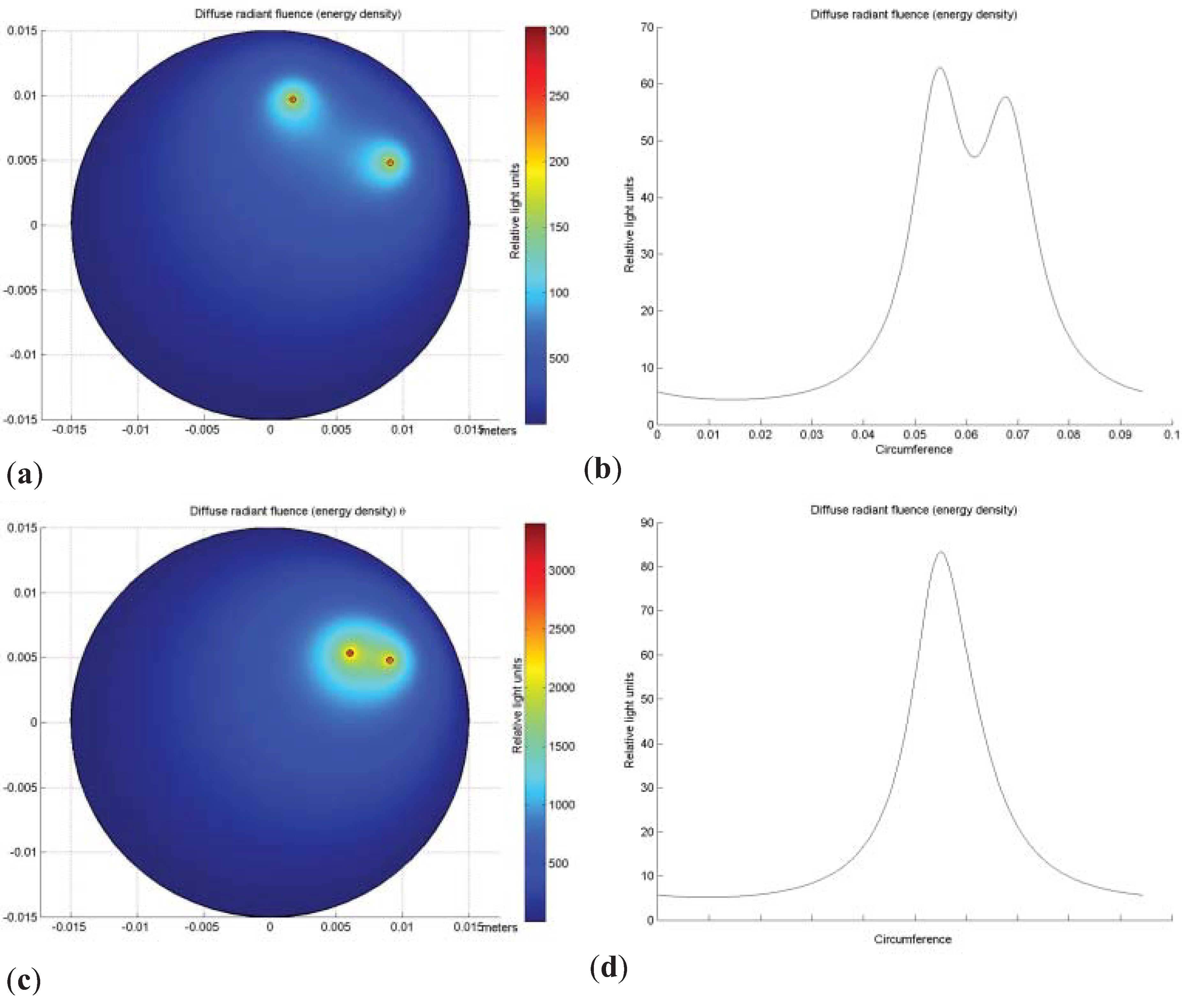
3.1. Validation Experiments in a Homogeneous Cylindrical Phantom

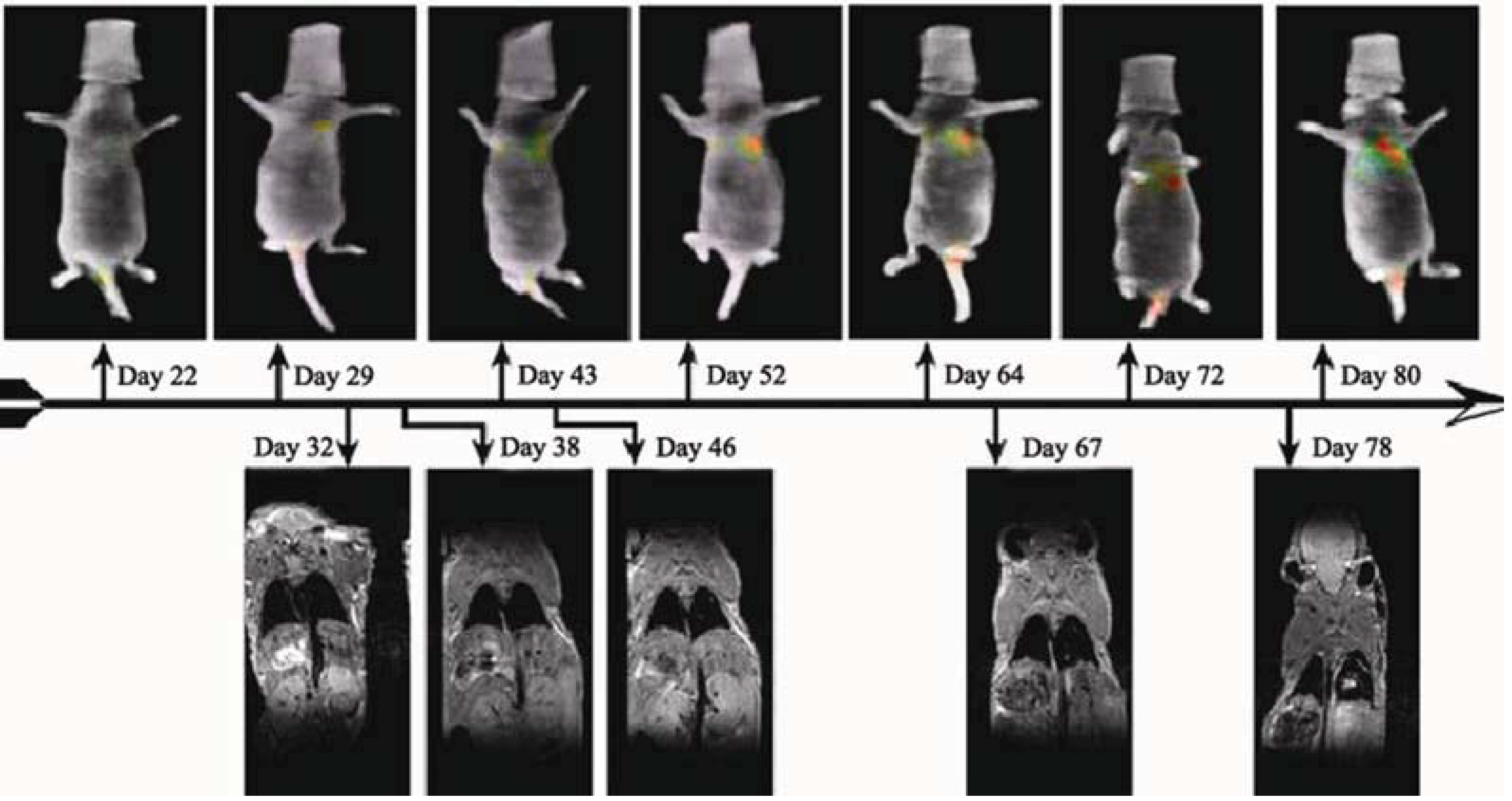
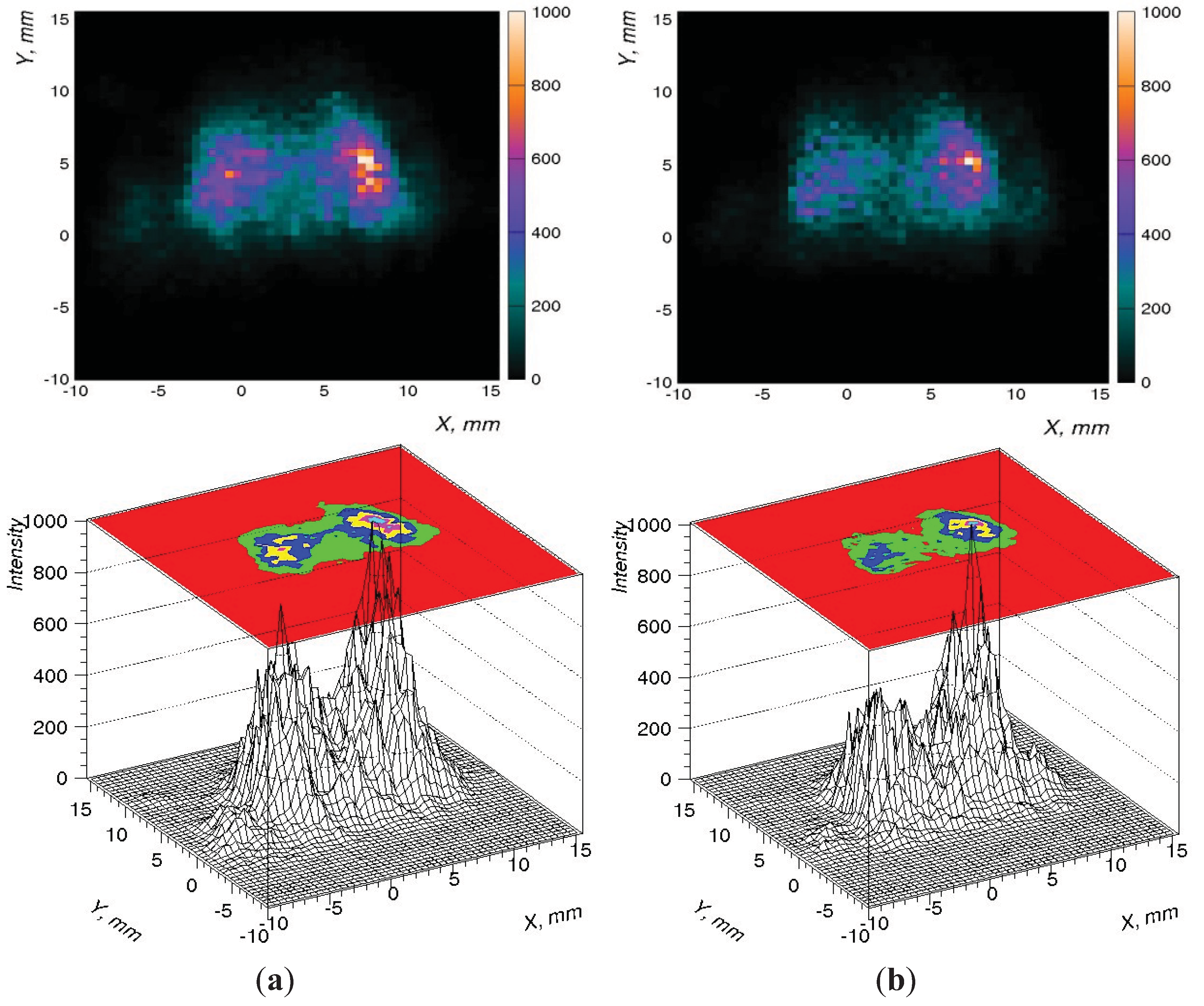
3.2. In Vivo Imaging in Lung Metastasis Models

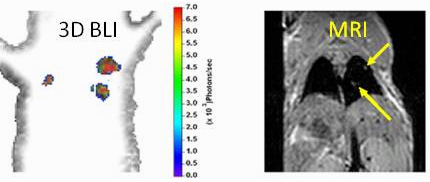
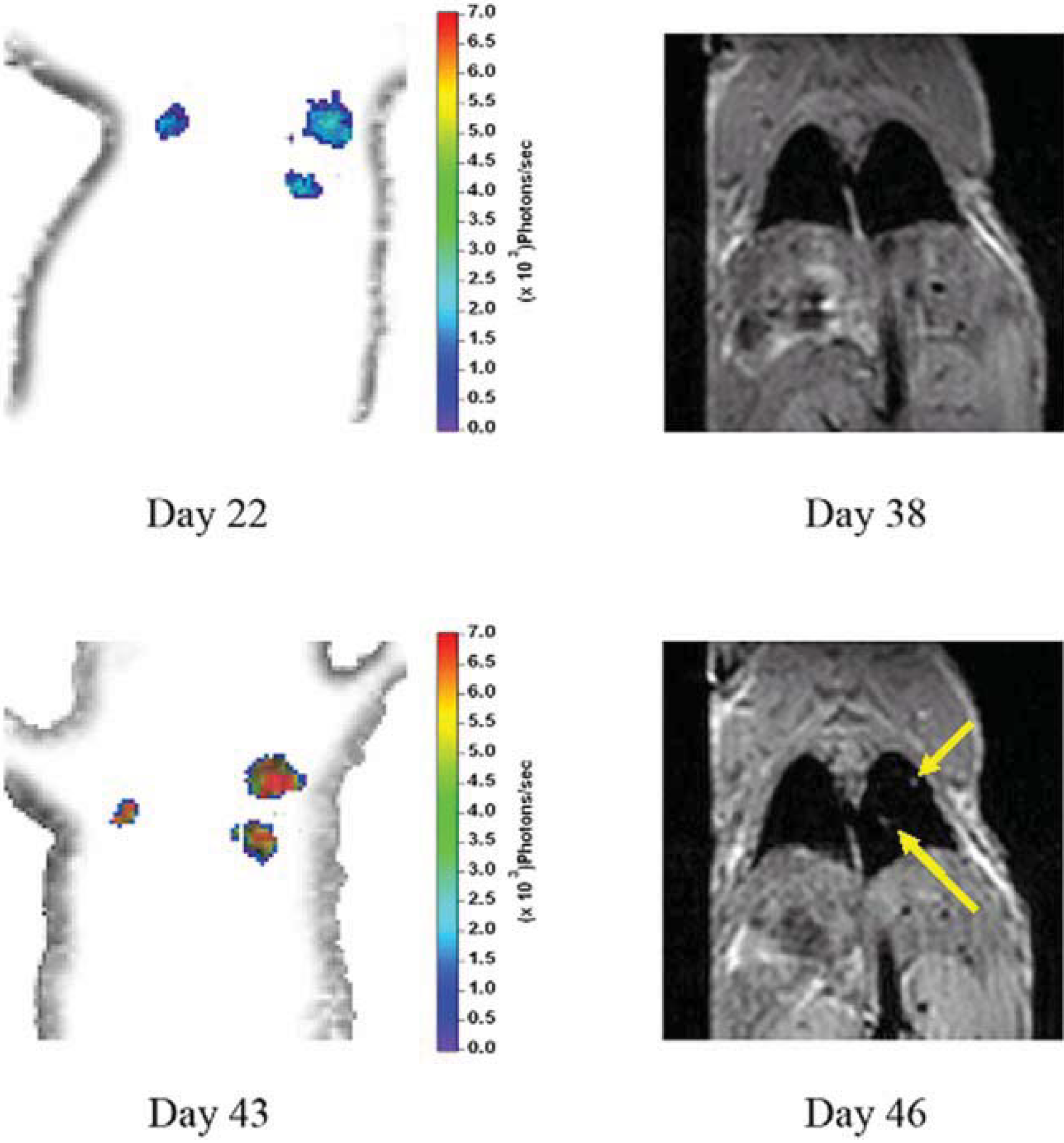
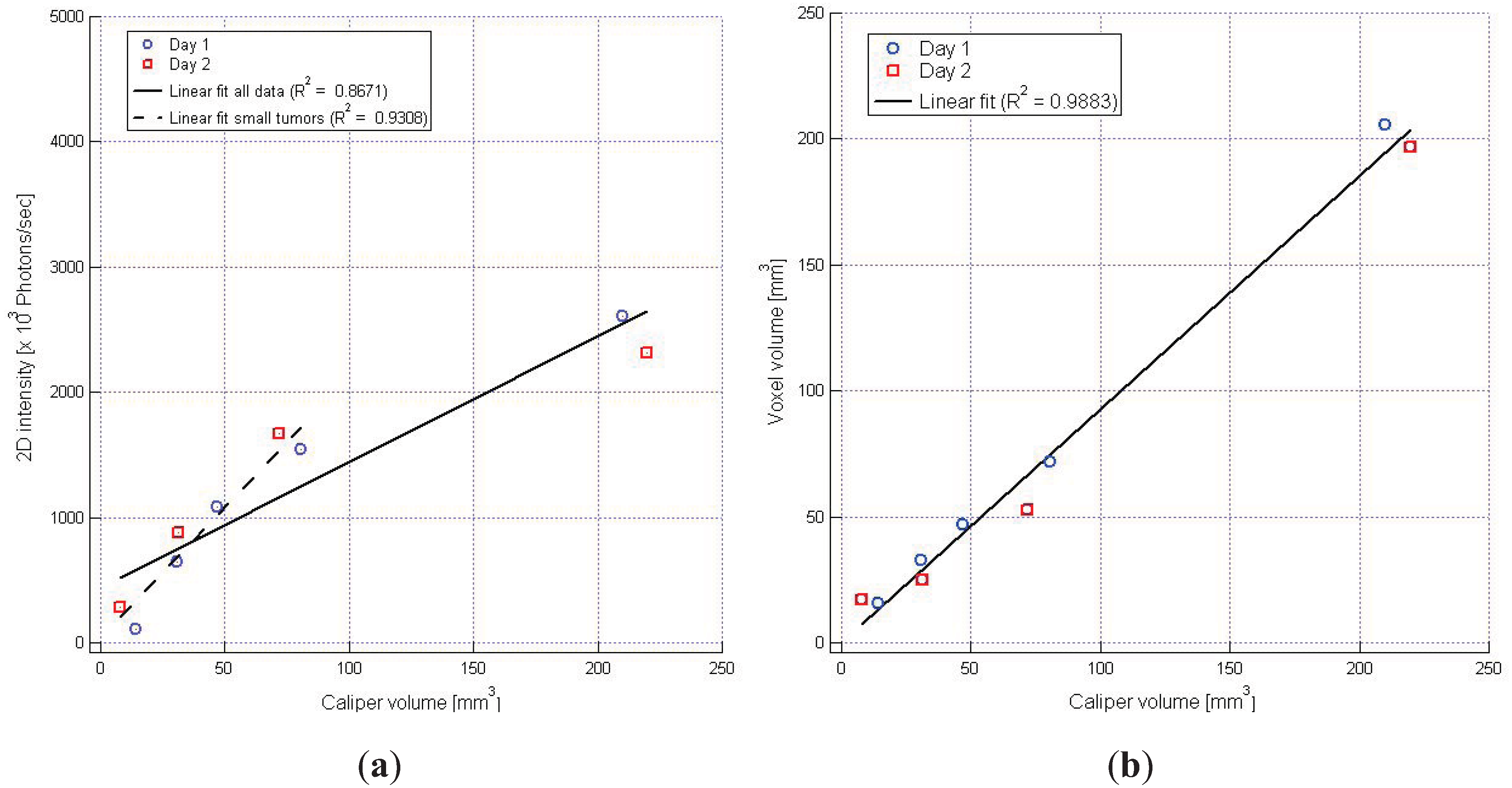
3.3. Multimodality in Vivo Comparison
4. Conclusions
Acknowledgments
Conflict of Interest
References
- Thorne, S.H.; Contag, C.H. Using in vivo bioluminescence imaging to shed light on cancer biology. Proc. IEEE 2005, 93, 750–762. [Google Scholar] [CrossRef]
- Villalobos, V.; Naik, S.; Piwnica-Worms, D. Current state of imaging protein-protein interactions in vivo with genetically encoded reporters. Annu. Rev. Biomed. Eng. 2007, 9, 321–349. [Google Scholar] [CrossRef]
- Weissleder, R.; Pittet, M.J. Imaging in the era of molecular oncology. Nature 2008, 452, 580–589. [Google Scholar] [CrossRef]
- O’Neill, K.; Lyons, S.K.; Gallagher, W.M.; Curran, K.M.; Byrne, A.T. Bioluminescent imaging: A critical tool in pre-clinical oncology research. J. Pathol. 2009, 220, 317–327. [Google Scholar]
- Prescher, J.A.; Contag, C.H. Guided by the light: Visualizing biomolecular processes in living animals with bioluminescence. Curr. Opin. Chem. Biol. 2010, 14, 80–89. [Google Scholar] [CrossRef]
- Hall, M.P.; Unch, J.; Binkowski, B.F.; Valley, M.P.; Butler, B.L.; Wood, M.G.; Otto, P.; Zimmerman, K.; Vidugiris, G.; Machleidt, T.; et al. Engineered luciferase reporter from a deep sea shrimp utilizing a novel imidazopyrazinone substrate. ACS Chem. Biol. 2012, 7, 1848–1857. [Google Scholar] [CrossRef]
- Liu, L.; Mason, R.P. Imaging β-galactosidase activity in human tumor xenografts and transgenic mice using a chemiluminescent substrate. PLoS ONE 2010, 5. [Google Scholar] [CrossRef]
- Bhaumik, S.; Lewis, X.Z.; Gambhir, S.S. Optical imaging of Renilla luciferase, synthetic Renilla luciferase, and firefly luciferase reporter gene expression in living mice. J. Biomed. Opt. 2004, 9, 578–586. [Google Scholar] [CrossRef]
- Rice, B.W.; Cable, M.D.; Nelson, M.B. In vivo imaging of light-emitting probes. J. Biomed. Opt. 2001, 6, 432–440. [Google Scholar] [CrossRef]
- Tromberg, B.J.; Shah, N.; Lanning, R.; Cerussi, A.; Espinoza, J.; Pham, T.; Svaasand, L.; Butler, J. Non-invasive in vivo characterization of breast tumors using photon migration spectroscopy. Neoplasia 2000, 2, 26–40. [Google Scholar] [CrossRef]
- Wang, G.; Cong, W.; Shen, H.; Qian, X.; Henry, M.; Wang, Y. Overview of bioluminescence tomography—A new molecular imaging modality. Front. Biosci. 2008, 13, 1281–1293. [Google Scholar] [CrossRef]
- Roncali, E.; Savinaud, M.; Levrey, O.; Rogers, K.L.; Maitrejean, S.; Tavitian, B. New device for real-time bioluminescence imaging in moving rodents. J. Biomed. Opt. 2008, 13, 054035. [Google Scholar] [CrossRef]
- Yan, H.; Lin, Y.; Barber, W.C.; Unlu, M.B.; Gulsen, G. A gantry-based tri-modality system for bioluminescence tomography. Rev. Sci. Instrum 2012, 83, 043708:1–043708:8. [Google Scholar]
- Feng, J.; Qin, C.; Jia, K.; Zhu, S.; Yang, X.; Tian, J. Bioluminescence tomography imaging in vivo: Recent advances. IEEE J. Sel. Top. Quant. Electron. 2012, 18, 1394–1402. [Google Scholar] [CrossRef]
- Cong, W.; Wang, G.; Kumar, D.; Liu, Y.; Jiang, M.; Wang, L.; Hoffman, E.; McLennan, G.; McCray, P.; Zabner, J.; Cong, A. Practical reconstruction method for bioluminescence tomography. Opt. Express 2005, 13, 6756–6771. [Google Scholar] [CrossRef]
- Ntziachristos, V.; Weissleder, R. Experimental three-dimensional fluorescence reconstruction of diffuse media by use of a normalized born approximation. Optics Letters 2001, 26, 893–895. [Google Scholar] [CrossRef]
- Graves, E.E.; Ripoll, J.; Weissleder, R.; Ntziachristos, V. A submillimeter resolution fluorescence molecular imaging system for small animal imaging. Med. Phys. 2003, 30, 901–911. [Google Scholar] [CrossRef]
- Kok, P.; Botha, C.P.; Dijkstra, J.; Kaijzel, E.; Que, I.; Löwik, C.W.G.M.; Reiber, J.H.C.; Lelieveldt, B.P.F.; Post, F.H. Integrated visualization of multi-angle bioluminescence imaging and micro CT. Proc. SPIE 2007, 6509. [Google Scholar] [CrossRef]
- Kuo, C.; Coquoz, O.; Troy, T.L.; Xu, H.; Rice, B.W. Three-dimensional reconstruction of in vivo bioluminescent sources based on multispectral imaging. J. Biomed. Opt. 2007, 12, 02447. [Google Scholar] [CrossRef]
- Li, C.; Mitchell, G.S.; Dutta, J.; Ahn, S.; Leahy, R.M.; Cherry, S.R. A three-dimensional multispectral fluorescence optical tomography imaging system for small animals based on a conical mirror design. Opt. Express 2009, 17, 7571–7585. [Google Scholar] [CrossRef]
- Li, C.; Yang, Y.; Mitchell, G.S.; Cherry, S.R. Simultaneous PET and multispectral 3-dimensional fluorescence optical tomography imaging system. J. Nucl. Med. 2011, 52, 1268–1275. [Google Scholar] [CrossRef]
- Gu, X.; Zhang, Q.; Larcom, L.; Jiang, H. Three-dimensional bioluminescence tomography with model-based reconstruction. Opt. Express 2004, 12, 3996–4000. [Google Scholar] [CrossRef]
- Chaudhari, A.J.; Darvas, F.; Bading, J.R.; Moats, R.A.; Conti, P.S.; Smith, D.J.; Cherry, S.R.; Leahy, R.M. Hyperspectral and multispectral bioluminescence optical tomography for small animal imaging. Phys. Med. Biol. 2005, 50, 5421–5441. [Google Scholar] [CrossRef]
- Dehghani, H.; Davis, S.C.; Jiang, S.; Pogue, B.W.; Paulsen, K.D.; Patterson, M.S. Spectrally resolved bioluminescence optical tomography. Optics Letters 2006, 31, 365–367. [Google Scholar] [CrossRef]
- Wang, G.; Shen, H.; Liu, Y.; Cong, A.; Cong, W.; Wang, Y.; Dubey, P. Digital spectral separation methods and systems for bioluminescence imaging. Opt. Express 2008, 16, 1719–1732. [Google Scholar] [CrossRef] [PubMed]
- Dehghani, H.; Davis, S.C.; Pogue, B.W. Spectrally resolved bioluminescence tomography using the reciprocity approach. Med. Phys. 2008, 35, 4863–4871. [Google Scholar] [CrossRef]
- Ahn, S.; Chaudhari, A.J.; Darvas, F.; Bouman, C.A.; Leahy, R.M. Fast iterative image reconstruction methods for fully 3D multispectral bioluminescence tomography. Phys. Med. Biol. 2008, 53, 3921–3942. [Google Scholar] [CrossRef]
- Lu, Y.; Zhang, X.; Douraghy, A.; Stout, D.; Tian, J.; Chan, T.F.; Chatziioannou, A.F. Source reconstruction for spectrally-resolved bioluminescence tomography with sparse a priori information. Opt. Express 2009, 17, 8062–8080. [Google Scholar] [CrossRef]
- Feng, J.; Qin, C.; Jia, K.; Han, D.; Liu, K.; Zhu, S.; Yang, X.; Tian, J. An adaptive regularization parameter choice strategy for multispectral bioluminescence tomography. Med. Phys. 2011, 38, 5933–5944. [Google Scholar] [CrossRef]
- Qin, C.; Yang, X.; Feng, J.; Liu, K.; Liu, J.; Yan, G.; Zhu, S.; Xu, M.; Tian, J. Adaptive improved element free Galerkin method for quasi- or multi-spectral bioluminescence tomography. Opt. Express 2009, 17, 21925–21934. [Google Scholar] [CrossRef]
- Virostko, J.M.; Powers, A.C.; Jansen, E.D. Validation of luminescent source reconstruction using spectrally resolved bioluminescence images. Proc. SPIE 2008, 6849. [Google Scholar] [CrossRef]
- Soloviev, V.Y. Tomographic bioluminescence imaging with varying boundary conditions. Appl. Optics 2007, 46, 2778–2784. [Google Scholar] [CrossRef]
- Wang, G.; Shen, H.; Cong, W.; Zhao, S.; Wei, G.W. Temperature-modulated bioluminescence tomography. Opt. Express 2006, 14, 7852–7871. [Google Scholar] [CrossRef]
- Jansen, E.D.; Pickett, P.M.; Mackanos, M.A.; Virostko, J. Effect of optical tissue clearing on spatial resolution and sensitivity of bioluminescence imaging. J. Biomed. Opt. 2006, 11, 041119. [Google Scholar] [CrossRef]
- Alexandrakis, G.; Rannou, F.R.; Chatziioannou, A.F. Effect of optical property estimation accuracy on tomographic bioluminescence imaging: Simulation of a combined optical-PET (OPET) system. Phys. Med. Biol. 2006, 51, 2045–2053. [Google Scholar] [CrossRef]
- Alexandrakis, G.; Rannou, F.R.; Chatziioannou, A.F. Tomographic bioluminescence imaging by use of a combined optical-PET (OPET) system: A computer simulation feasibility study. Phys. Med. Biol. 2005, 50, 4225–4241. [Google Scholar] [CrossRef]
- Yan, H.; Unlu, M.B.; Nalcioglu, O.; Gulsen, G. Bioluminescence tomography with structural and functional a priori information. Proc. SPIE 2010, 7557. [Google Scholar] [CrossRef]
- Naser, M.A.; Patterson, M.S.; Wong, J.W. Self-calibrated algorithms for diffuse optical tomography and bioluminescence tomography using relative transmission images. Biomed. Optics Express 2012, 3, 2794–2808. [Google Scholar] [CrossRef]
- Feng, J.; Qin, C.; Jia, K.; Zhu, S.; Liu, K.; Han, D.; Yang, X.; Gao, Q.; Tian, J. Total variation regularization for bioluminescence tomography with the split Bregman method. Appl. Optics 2012, 51, 4501–4512. [Google Scholar] [CrossRef]
- Guo, W.; Jia, K.; Zhang, Q.; Liu, X.; Feng, J.; Qin, C.; Ma, X.; Yang, X.; Tian, J. Sparse reconstruction for bioluminescence tomography based on the semigreedy method. Comput. Math. Methods Med. 2012, 2012. [Google Scholar] [CrossRef]
- Guo, W.; Jia, K.; Tian, J.; Han, D.; Liu, X.; Wu, P.; Feng, J.; Yang, X. An efficient reconstruction method for bioluminescence tomography based on two-step iterative shrinkage approach. Proc. SPIE 2012, 8313. [Google Scholar] [CrossRef]
- Guo, W.; Jia, K.; Tian, J.; Han, D.; Liu, X.; Liu, K.; Zhang, Q.; Feng, J.; Qin, C. Sparsity reconstruction for bioluminescence tomography based on an augmented lagrangian method. Proc. SPIE 2012, 8225. [Google Scholar] [CrossRef]
- Qin, C.; Zhu, S.; Feng, J.; Zhong, J.; Ma, X.; Wu, P.; Tian, J. Comparison of permissible source region and multispectral data using efficient bioluminescence tomography method. J. Biophoton. 2011, 4, 824–839. [Google Scholar] [CrossRef]
- Zhang, B.; Yang, X.; Qin, C.; Liu, D.; Zhu, S.; Feng, J.; Sun, L.; Liu, K.; Han, D.; Ma, X.; et al. A trust region method in adaptive finite element framework for bioluminescence tomography. Opt. Express 2010, 18, 6477–6491. [Google Scholar] [CrossRef] [PubMed]
- Slavine, N.V.; Lewis, M.A.; Richer, E.; Antich, P.P. Iterative reconstruction method for light emitting sources based on the diffusion equation. Med. Phys. 2006, 33, 61–68. [Google Scholar] [CrossRef]
- Paroo, Z.; Bollinger, R.A.; Braasch, D.A.; Richer, E.; Corey, D.R.; Antich, P.P.; Mason, R.P. Validating bioluminescence imaging as a high-throughput, quantitative modality for assessing tumor burden. Mol. Imag. 2004, 3, 117–124. [Google Scholar] [CrossRef]
- Unlu, M.B.; Gulsen, G. Effects of the time dependence of a bioluminescent source on the tomographic reconstruction. Appl. Optics 2008, 47, 799–806. [Google Scholar] [CrossRef]
- Hillman, E.M.C.; Moore, A. All-optical anatomical co-registration for molecular imaging of small animals using dynamic contrast. Nat. Photon. 2007, 1, 526–530. [Google Scholar] [CrossRef]
- Feng, J.; Jia, K.; Yan, G.; Zhu, S.; Qin, C.; Lv, Y.; Tian, J. An optimal permissible source region strategy for multispectral bioluminescence tomography. Opt. Express 2008, 16, 15640–15654. [Google Scholar] [CrossRef]
- Virostko, J.; Powers, A.C.; Jansen, E.D. Validation of luminescent source reconstruction using single-view spectrally resolved bioluminescence images. Appl. Optics 2007, 46, 2540–2547. [Google Scholar] [CrossRef]
- Han, W.M.; Wang, G. Theoretical and numerical analysis on multispectral bioluminescence tomography. IMA J. Appl. Math. 2007, 72, 67–85. [Google Scholar] [CrossRef]
- Han, W.M.; Cong, W.X.; Wang, G. Mathematical theory and numerical analysis of bioluminescence tomography. Inverse Probl. 2006, 22, 1659–1675. [Google Scholar] [CrossRef]
- Wang, G.; Li, Y.; Jiang, M. Uniqueness theorems in bioluminescence tomography. Med. Phys. 2004, 31, 2289–2299. [Google Scholar] [CrossRef]
- Cheng, X.L.; Gong, R.F.; Han, W.M. A new general mathematical framework for bioluminescence tomography. Comput. Meth. Appl. Mech. Eng. 2008, 197, 524–535. [Google Scholar] [CrossRef]
- Han, W.M.; Wang, G. Bioluminescence tomography: Biomedical background, mathematical theory, and numerical approximation. J. Comput. Math. 2008, 26, 324–335. [Google Scholar] [CrossRef]
- Lv, Y.; Tian, J.; Cong, W.; Wang, G.; Yang, W.; Qin, C.; Xu, M. Spectrally resolved bioluminescence tomography with adaptive finite element analysis: Methodology and simulation. Phys. Med. Biol. 2007, 52, 4497–4512. [Google Scholar] [CrossRef]
- Lv, Y.; Tian, J.; Cong, W.; Wang, G.; Luo, J.; Yang, W.; Li, H. A multilevel adaptive finite element algorithm for bioluminescence tomography. Opt. Express 2006, 14, 8211–8223. [Google Scholar] [CrossRef]
- Gong, W.; Li, R.; Yan, N.; Zhao, W. An improved error analysis for finite element approximation of bioluminescence tomography. J. Comput. Math. 2008, 26, 297–309. [Google Scholar]
- Kumar, D.; Cong, W.X.; Wang, G. Monte Carlo method for bioluminescence tomography. Indian J. Exp. Biol. 2007, 45, 58–63. [Google Scholar] [PubMed]
- Li, H.; Tian, J.; Zhu, F.; Cong, W.; Wang, L.V.; Hoffman, E.A.; Wang, G. A mouse optical simulation environment (MOSE) to investigate bioluminescent phenomena in the living mouse with the Monte Carlo method. Acad. Radiol. 2004, 11, 1029–1038. [Google Scholar] [CrossRef]
- Dikmen, Z.G.; Gellert, G.; Dogan, P.; Mason, R.; Antich, P.; Richer, E.; Wright, W.E.; Shay, J.E. A new diagnostic system in cancer research: Bioluminescent imaging (BLI). Turk. J. Med. Sci. 2005, 35, 65–70. [Google Scholar]
- Troy, T.; Jekic-McMullen, D.; Sambucetti, L.; Rice, B. Quantitative comparison of the sensitivity of detection of fluorescent and bioluminescent reporters in animal models. Mol. Imag. 2004, 3, 9–23. [Google Scholar] [CrossRef]
- Contero, A.; Richer, E.; Gondim, A.; Mason, R.P. High-throughput quantitative bioluminescence imaging for assessing tumor burden. Methods Mol. Biol. 2009, 574, 37–45. [Google Scholar] [CrossRef]
- Slavine, N.V.; McColl, R.W.; Richer, E.; Mason, R.P.; Antich, P.P. An Automated 3D Image-Processing Strategy for Small-Animal Bioluminescence Cancer Studies. In Proceedings of Biotechnology and Bioinformatics Symposium (BIOT-2008), Arlington, TX, USA, October 2008.
- Alhasan, M.K.; Liu, L.; Lewis, M.A.; Magnusson, J.; Mason, R.P. Comparison of optical and power Doppler ultrasound imaging for non-invasive evaluation of arsenic trioxide as a vascular disrupting agent in tumors. PLoS ONE 2012, 7. [Google Scholar] [CrossRef]
- Sarraf-Yazdi, S.; Mi, J.; Dewhirst, M.W.; Clary, B.M. Use of in vivo bioluminescence imaging to predict hepatic tumor burden in mice. J. Surg. Res. 2004, 120, 249–255. [Google Scholar] [CrossRef]
- Garbow, J.R.; Zhang, Z.; You, M. Detection of primary lung tumors in rodents by magnetic resonance imaging. Cancer Res. 2004, 64, 2740–2742. [Google Scholar] [CrossRef]
Appendix
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Lewis, M.A.; Richer, E.; Slavine, N.V.; Kodibagkar, V.D.; Soesbe, T.C.; Antich, P.P.; Mason, R.P. A Multi-Camera System for Bioluminescence Tomography in Preclinical Oncology Research. Diagnostics 2013, 3, 325-343. https://doi.org/10.3390/diagnostics3030325
Lewis MA, Richer E, Slavine NV, Kodibagkar VD, Soesbe TC, Antich PP, Mason RP. A Multi-Camera System for Bioluminescence Tomography in Preclinical Oncology Research. Diagnostics. 2013; 3(3):325-343. https://doi.org/10.3390/diagnostics3030325
Chicago/Turabian StyleLewis, Matthew A., Edmond Richer, Nikolai V. Slavine, Vikram D. Kodibagkar, Todd C. Soesbe, Peter P. Antich, and Ralph P. Mason. 2013. "A Multi-Camera System for Bioluminescence Tomography in Preclinical Oncology Research" Diagnostics 3, no. 3: 325-343. https://doi.org/10.3390/diagnostics3030325