A Disposable Microfluidic Virus Concentration Device Based on Evaporation and Interfacial Tension
Abstract
:1. Introduction
2. Theoretical Underpinnings
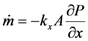
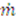 is the rate of evaporation, kx is the convective mass transfer coefficient, A is the area of the exchange surface,
is the rate of evaporation, kx is the convective mass transfer coefficient, A is the area of the exchange surface,  is the pressure gradient from the liquid/gas interface to the convective air flow channel [17].
is the pressure gradient from the liquid/gas interface to the convective air flow channel [17]. 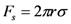
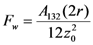
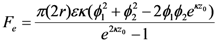
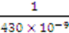 ) [21],
) [21], 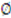 is the zeta potential of the interaction of the particle and the channel surface (here, assuming −40 mV for virus, and −100 mV for Teflon) [21,24,25]. The adhesion force is
is the zeta potential of the interaction of the particle and the channel surface (here, assuming −40 mV for virus, and −100 mV for Teflon) [21,24,25]. The adhesion force is
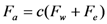
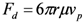
| Physical meaning | Parameter | Unit | Particles in the analyte | ||
|---|---|---|---|---|---|
| E. coli | influenza | influenza with surface treatment | |||
| particle radius | r | m | 5.00E−07 | 5.00E−08 | 5.00E−08 |
| liquid-vapor surface tension [21] | σ | N/m | 0.071 | 0.071 | 0.071 |
| liquid-substrate contact angle | θ | 50 | 50 | 10 | |
| rad | 0.87 | 0.87 | 0.17 | ||
| liquid-particle surface tension | Fs | N | 2.23E−07 | 2.23E−08 | 2.23E−08 |
| Fs,x | N | 1.43E−07 | 1.43E−08 | 2.20E−08 | |
| Fs,z | N | 1.71E−07 | 1.71E−08 | 3.87E−09 | |
| Hamaker constant when particles and substrate are in liquid [21] | A132 | J | 3.00E−20 | 3.00E−20 | 3.00E−20 |
| Minimum particle-substrate separation [21] | Z0 | m | 4.00E−10 | 4.00E−10 | 1.00E−09 |
| van der Waal's force | Fv | N | 1.56E−08 | 1.56E−09 | 2.50E−10 |
| permitivity of water [21] | ε | F/m | 7.00E−10 | 7.00E−10 | 7.00E−10 |
| reciprocal of Debye Length [21] | κ | 1/m | 2.33E+06 | 2.33E+06 | 2.33E+06 |
| zeta potential of particle [21] | φ1 | mV | −40 | −40 | −40 |
| zeta potential of Teflon [21] | φ2 | mV | −100 | −100 | −100 |
| electrostatic force | Fe | N | 9.87E−09 | −5.11E−12 | −5.11E−12 |
| Empirical indicator of concentration threshold | c | 7 | 11 | 16 | |
3. Materials and Methods
3.1. Device Fabrication
3.2. Visualizing Concentration with Fluorescent Beads

3.3. Viral Culture and Patient Sample Collection
3.5 Concentration of Influenza Viral Sample with Evaporation

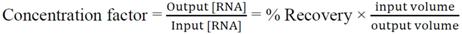
3.6. RNA Extraction
3.7. Quantification Using qRT-PCR
4. Results and Discussion
4.1 Fluorescent Beads Quantification

4.2. Concentration of Influenza Samples


5. Conclusions
Acknowledgements
References
- Castellanos, A.; Ramos, A.; Gonzlez, A.; Green, N.G.; Morgan, H. Electrohydrodynamics and dielectrophoresis in microsystems: Scaling laws. J. Phys. D Appl. Phys. 2003, 36, 2584–2597. [Google Scholar] [CrossRef]
- Jacoby, G.A.; Han, P. Detection of extended-spectrum beta-lactamases in clinical isolates of Klebsiella pneumoniae and Escherichia coli. J. Clin. Microbiol. 1996, 34, 908–911. [Google Scholar] [PubMed]
- Jie, W. Biased AC electro-osmosis for on-chip bioparticle processing. IEEE Trans. Nanotechnol. 2006, 5, 84–89. [Google Scholar] [CrossRef]
- Ocvirk, G.; Munroe, M.; Tang, T.; Oleschuk, R.; Westra, K.; Harrison, D.J. Electrokinetic control of fluid flow in native poly(dimethylsiloxane) capillary electrophoresis devices. Electrophoresis 2000, 21, 107–115. [Google Scholar] [CrossRef]
- Boguslaw, B.; Szumski, M.; Klodzinska, E.; Dahm, H. Separation of bacteria by capillary electrophoresis. J. Separ. Sci. 2003, 26, 1045–1049. [Google Scholar] [CrossRef]
- Lay, C.; Teo, C.Y.; Zhu, L.; Peh, X.L.; Ji, H.M.; Chew, B.-R.; Murthy, R.; Feng, H.H.; Liu, W.-T. Enhanced microfiltration devices configured with hydrodynamic trapping and a rain drop bypass filtering architecture for microbial cells detection. Lab Chip 2008, 8, 830–833. [Google Scholar] [CrossRef]
- Zhu, L.; Zhang, Q.; Feng, H.; Ang, S.; Chau, F.S.; Liu, W.-T. Filter-based microfluidic device as a platform for immunofluorescent assay of microbial cells. Lab Chip 2004, 4, 337–341. [Google Scholar] [CrossRef]
- Reichmuth, D.S.; Wang, S.K.; Barrett, L.M.; Throckmorton, D.J.; Einfeld, W.; Singh, A.K. Rapid microchip-based electrophoretic immunoassays for the detection of swine influenza virus. Lab Chip 2008, 8, 1319–1324. [Google Scholar] [CrossRef]
- Liu, R.H.; Yang, J.; Lenigk, R.; Bonanno, J.; Grodzinski, P. Self-contained, fully integrated biochip for sample preparation, polymerase chain reaction amplification, and DNA microarray detection. Anal. Chem. 2004, 76, 1824–1831. [Google Scholar] [CrossRef]
- Furdui, V.I.; Harrison, D.J. Immunomagnetic T cell capture from blood for PCR analysis using microfluidic systems. Lab Chip 2004, 4, 614–618. [Google Scholar] [CrossRef]
- Lien, K.-Y.; Lin, J.-L.; Liu, C.-Y.; Lei, H.-Y.; Lee, G.-B. Purification and enrichment of virus samples utilizing magnetic beads on a microfluidic system. Lab Chip 2007, 7, 868–875. [Google Scholar] [CrossRef]
- Berthier, E.; Warrick, J.; Yu, H.; Beebe, D.J. Managing evaporation for more robust microscale assays Part 1. Volume loss in high throughput assays. Lab Chip 2008, 8, 852–859. [Google Scholar] [CrossRef]
- Berthier, E.; Warrick, J.; Yu, H.; Beebe, D.J. Managing evaporation for more robust microscale assays Part 2. Characterization of convection and diffusion for cell biology. Lab Chip 2008, 8, 860–864. [Google Scholar] [CrossRef]
- Sharma, N.R.; Lukyanov, A.; Bardell, R.L.; Seifried, L.; Shen, M. Development of an evaporation-based microfluidic sample concentrator. Proc. SPIE 2008, 6886. [Google Scholar] [CrossRef]
- Timmer, B.H.; van Delft, K.M.; Olthuis, W.; Bergveld, P.; van den Berg, A. Micro-evaporation electrolyte concentrator. Sens. Actuator. BChem. 2003, 91, 342–346. [Google Scholar] [CrossRef]
- Walker, G.M.; Beebe, D.J. An evaporation-based microfluidic sample concentration method. Lab Chip 2002, 2, 57–61. [Google Scholar] [CrossRef]
- Zimmermann, M.; Bentley, S.; Schmid, H.; Hunziker, P.; Delamarche, E. Continuous flow in open microfluidics using controlled evaporation. Lab Chip 2005, 5, 1355–1359. [Google Scholar] [CrossRef]
- Zhang, J.Y.; Do, J.; Premasiri, W.R.; Ziegler, L.D.; Klapperich, C.M. Rapid point-of-care concentration of bacteria in a disposable microfluidic device using meniscus dragging effect. Lab Chip 2010, 10, 3265–3270. [Google Scholar] [CrossRef]
- Leng, J.; Lonetti, B.; Tabeling, P.; Joanicot, M.; Ajdari, A. Microevaporators for kinetic exploration of phase diagrams. Phys. Rev. Lett. 2006, 96, 084503:1–084503:4. [Google Scholar]
- Wang, F.; Chon, C.H.; Li, D. Particle separation by a moving air-liquid interface in a microchannel. J. Colloid Interface Sci. 2010, 352, 580–584. [Google Scholar] [CrossRef]
- Wong, T.-S.; Chen, T.-H.; Shen, X.; Ho, C.-M. Nanochromatography driven by the coffee ring effect. Anal. Chem. 2011, 83, 1871–1873. [Google Scholar] [CrossRef] [PubMed]
- Deegan, R.D.; Bakajin, O.; Dupont, T.F.; Huber, G.; Nagel, S.R.; Witten, T.A. Capillary flow as the cause of ring stains from dried liquid drops. Nature 1997, 389, 827–829. [Google Scholar] [CrossRef]
- Hu, H.; Larson, R.G. Marangoni effect reverses coffee-ring depositions. J. Phys. Chem. B 2006, 110, 7090–7094. [Google Scholar] [CrossRef]
- Schaldach, C.M.; Bourcier, W.L.; Shaw, H.F.; Viani, B.E.; Wilson, W.D. The influence of ionic strength on the interaction of viruses with charged surfaces under environmental conditions. J. Colloid Interface Sci. 2006, 294, 1–10. [Google Scholar] [CrossRef]
- Kirby, B.J.; Hasselbrink, E.F. Zeta potential of microfluidic substrates: 2. Data for polymers. Eelectrophoresis 2004, 25, 203–213. [Google Scholar] [CrossRef]
- World Health Organization (WHO). WHO Manual on Animal Influenza Diagnosis and Surveillance. Available online: http://www.wpro.who.int/emerging_diseases/documents/docs/manualonanimalaidiagnosisandsurveillance.pdf (accessed on 18 January 2013).
- Haldar, J.; Weight, A.K.; Klibanov, A.M. Preparation, application and testing of permanent antibacterial and antiviral coatings. Nat. Protocol. 2007, 2, 2412–2417. [Google Scholar] [CrossRef]
- CDC. CDC Protocol of Realtime RTPCR for Influenza A(H1N1). Available online: http://www.who.int/entity/csr/resources/publications/swineflu/CDCRealtimeRTPCR_SwineH1Assay-2009_20090430.pdf (accessed on 18 January 2013).
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Zhang, J.Y.; Mahalanabis, M.; Liu, L.; Chang, J.; Pollock, N.R.; Klapperich, C.M. A Disposable Microfluidic Virus Concentration Device Based on Evaporation and Interfacial Tension. Diagnostics 2013, 3, 155-169. https://doi.org/10.3390/diagnostics3010155
Zhang JY, Mahalanabis M, Liu L, Chang J, Pollock NR, Klapperich CM. A Disposable Microfluidic Virus Concentration Device Based on Evaporation and Interfacial Tension. Diagnostics. 2013; 3(1):155-169. https://doi.org/10.3390/diagnostics3010155
Chicago/Turabian StyleZhang, Jane Yuqian, Madhumita Mahalanabis, Lena Liu, Jessie Chang, Nira R. Pollock, and Catherine M. Klapperich. 2013. "A Disposable Microfluidic Virus Concentration Device Based on Evaporation and Interfacial Tension" Diagnostics 3, no. 1: 155-169. https://doi.org/10.3390/diagnostics3010155





