An Enhanced ELISPOT Assay for Sensitive Detection of Antigen-Specific T Cell Responses to Borrelia burgdorferi
Abstract
:1. Introduction
2. Materials and Methods
2.1. Isolation of Human Peripheral Blood Mononuclear Cells
2.2. ELISPOT Assays with PBMC
2.3. Measurement of IFN-γ Concentration in PBMC Supernatants
2.4. Western Blot Assay
2.5. Statistical Analysis
3. Results and Discussion
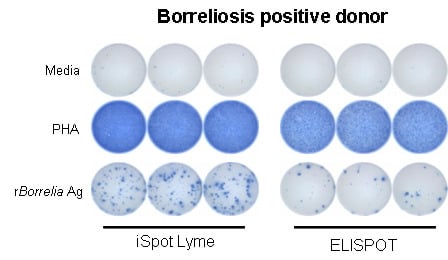
3.1. Enhanced Detection of Borrelia-Specific Reactive T Cells by the iSpot Lyme Assay
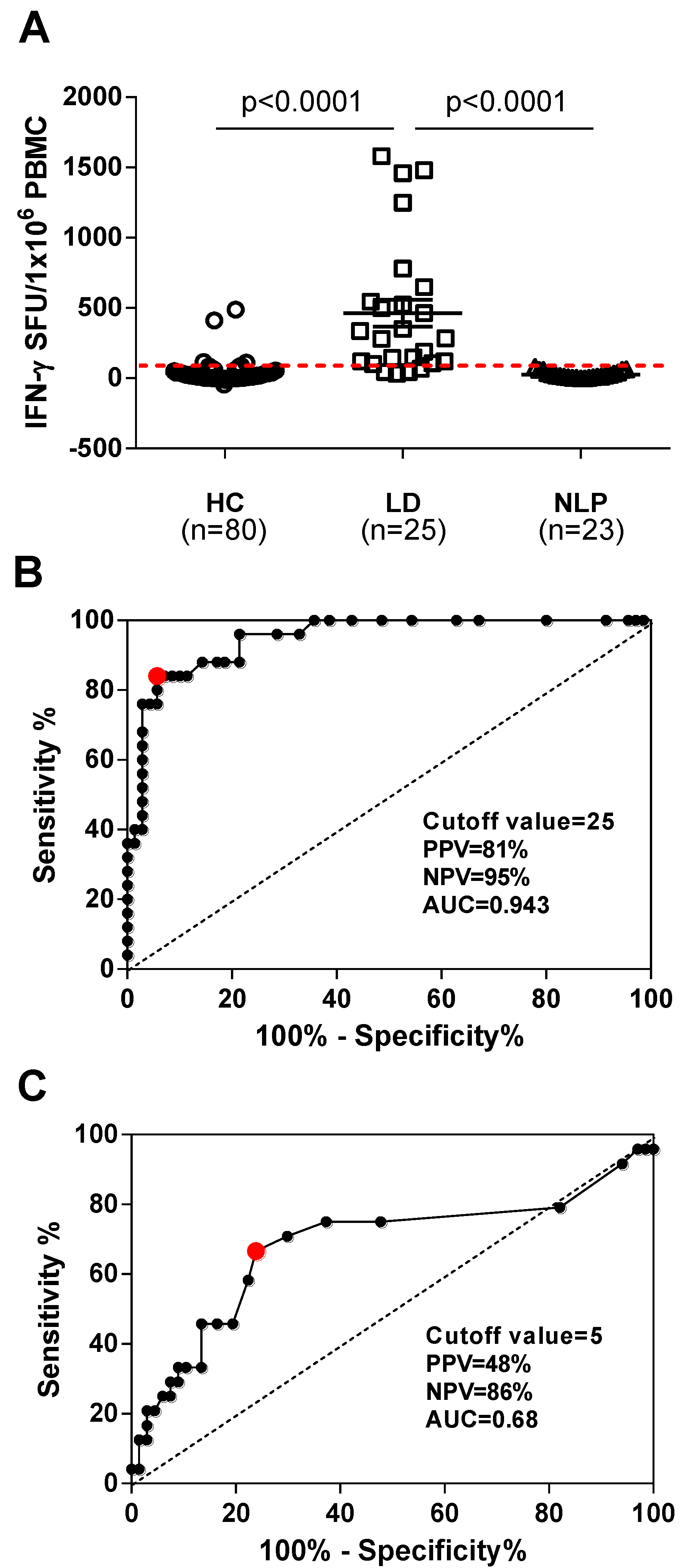
3.2. Evaluation of the Sensitivity and Specificity of the iSpot Lyme Assay as a Diagnostic Test

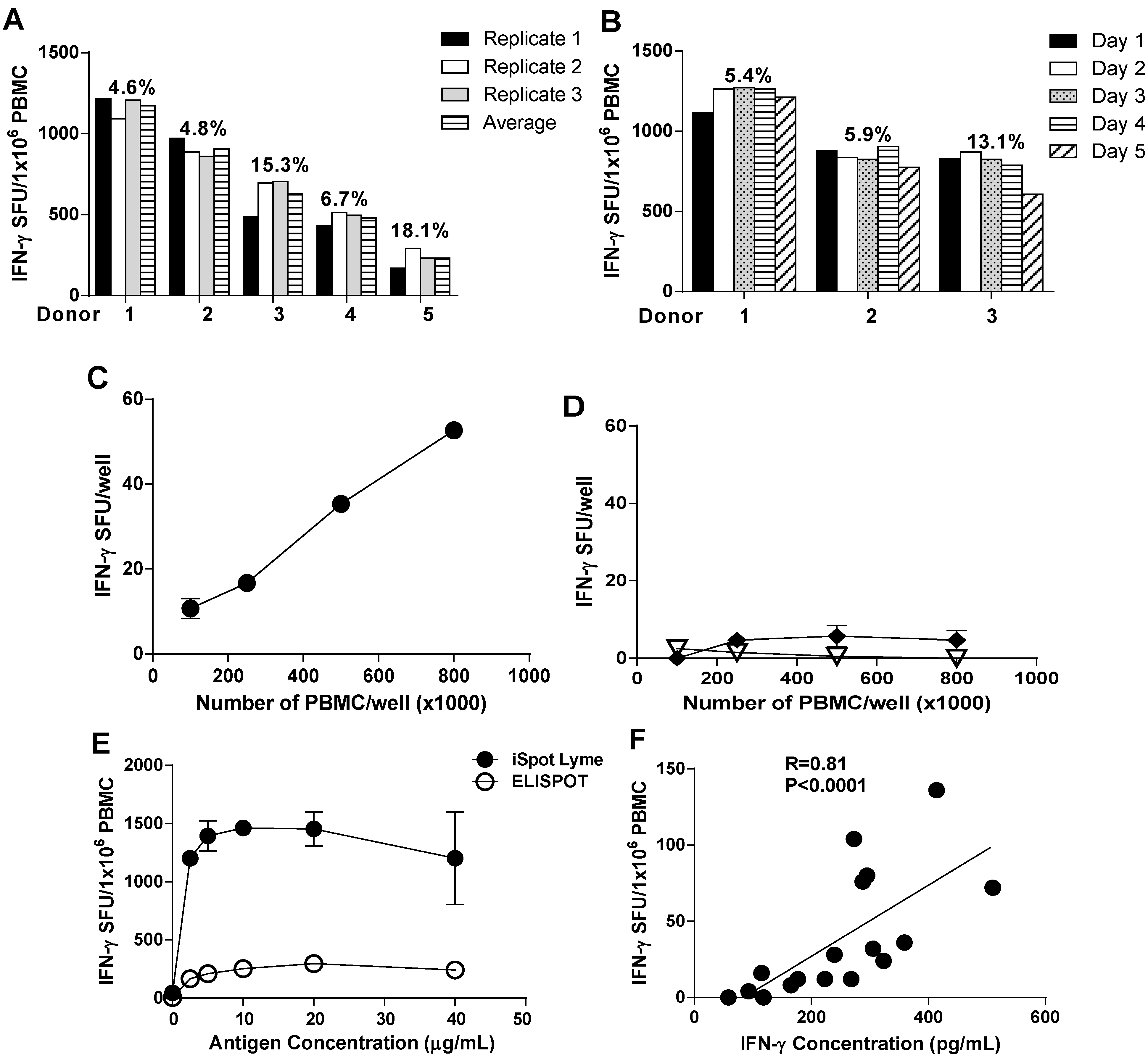
3.3. Optimization and Validation of the iSpot Lyme Assay
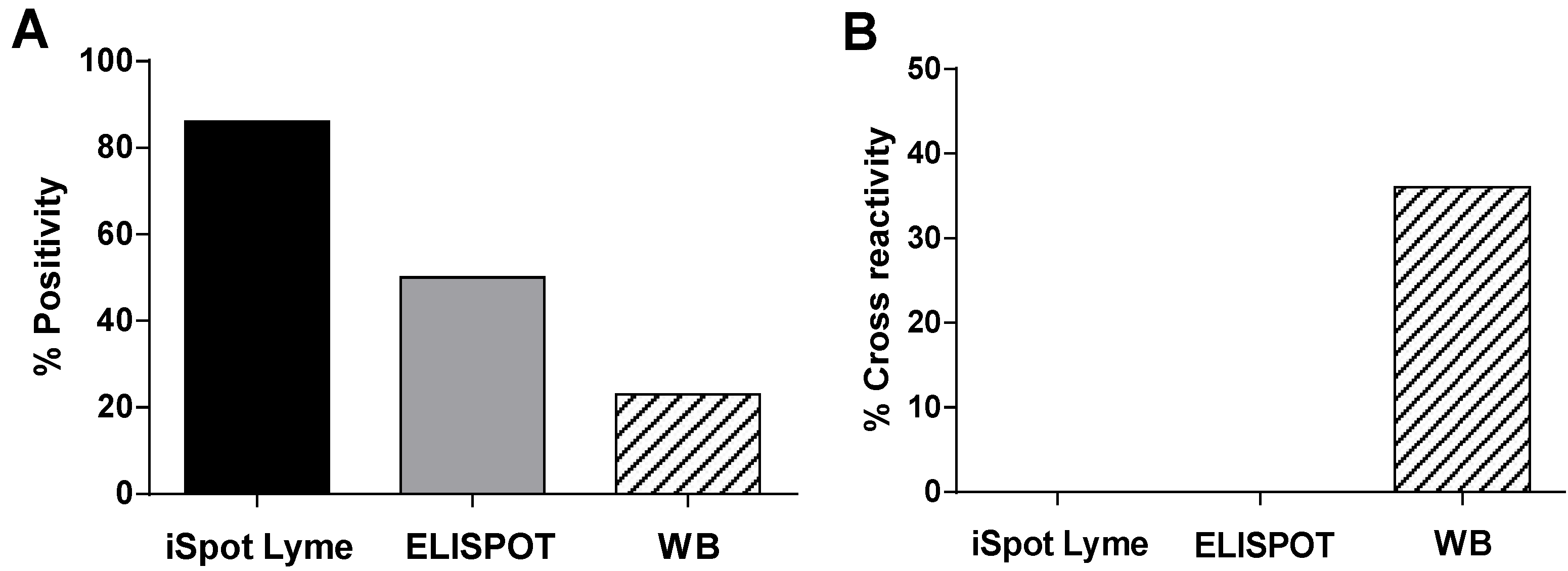
3.4. Comparisons between the iSpot Lyme Assay and Lyme Western Blot Assay
4. Conclusions
Acknowledgments
Conflicts of Interest
References
- Burgdorfer, W.; Barbour, A.G.; Hayes, S.F.; Benach, J.L.; Grunwaldt, E.; Davis, J.P. Lyme disease-a tick-borne spirochetosis? Science 1982, 216, 1317–1319. [Google Scholar]
- Steere, A.C. Lyme disease. N. Engl. J. Med. 2001, 345, 115–125. [Google Scholar] [CrossRef]
- Steere, A.C.; Coburn, J.; Glickstein, L. The emergence of Lyme disease. J. Clin. Invest. 2004, 113, 1093–1101. [Google Scholar]
- Centers for Disease Control and Prevention. Reported Cases of Lyme Disease by Year, United States, 2002–2011. Available online: http://www.cdc.gov/lyme/stats/chartstables/casesbyyear.html (accessed on 1 July 2013).
- Young, J.D. Underreporting of Lyme disease. N. Engl. J. Med. 1998, 338, 1629. [Google Scholar] [CrossRef]
- Gross, D.M.; Huber, B.T. Cellular and molecular aspects of Lyme arthritis. Cell. Mol. Life Sci. 2000, 57, 1562–1569. [Google Scholar] [CrossRef]
- Lim, L.C.; England, D.M.; DuChateau, B.K.; Glowacki, N.J.; Schell, R.F. Borrelia burgdorferi-specific T lymphocytes induce severe destructive Lyme arthritis. Infect. Immun. 1995, 63, 1400–1408. [Google Scholar]
- Chandra, A.; Wormser, G.P.; Klempner, M.S.; Trevino, R.P.; Crow, M.K.; Latov, N.; Alaedini, A. Anti-neural antibody reactivity in patients with a history of Lyme borreliosis and persistent symptoms. Brain Behav. Immun. 2010, 24, 1018–1024. [Google Scholar] [CrossRef]
- Ramesh, G.; Benge, S.; Pahar, B.; Philipp, M.T. A possible role for inflammation in mediating apoptosis of oligodendrocytes as induced by the Lyme disease spirochete Borrelia burgdorferi. J. Neuroinflammation 2012, 9, 72. [Google Scholar] [CrossRef]
- Aucott, J.; Morrison, C.; Munoz, B.; Rowe, P.C.; Schwarzwalder, A.; West, S.K. Diagnostic challenges of early Lyme disease: lessons from a community case series. BMC. Infect. Dis. 2009, 9, 79. [Google Scholar] [CrossRef]
- Dattwyler, R.J.; Volkman, D.J.; Halperin, J.J.; Luft, B.J.; Thomas, J.; Golightly, M.G. Specific immune responses in Lyme borreliosis. Characterization of T cell and B cell responses to Borrelia burgdorferi. Ann. N. Y. Acad. Sci. 1988, 539, 93–102. [Google Scholar] [CrossRef]
- Krause, A.; Burmester, G.R.; Rensing, A.; Schoerner, C.; Schaible, U.E.; Simon, M.M.; Herzer, P.; Kramer, M.D.; Wallich, R. Cellular immune reactivity to recombinant OspA and flagellin from Borrelia burgdorferi in patients with Lyme borreliosis. Complexity of humoral and cellular immune responses. J. Clin. Invest. 1992, 90, 1077–1084. [Google Scholar] [CrossRef]
- Aguero-Rosenfeld, M.E.; Wang, G.; Schwartz, I.; Wormser, G.P. Diagnosis of lyme borreliosis. Clin. Microbiol. Rev. 2005, 18, 484–509. [Google Scholar] [CrossRef]
- Seriburi, V.; Ndukwe, N.; Chang, Z.; Cox, M.E.; Wormser, G.P. High frequency of false positive IgM immunoblots for Borrelia burgdorferi in clinical practice. Clin. Microbiol. Infect. 2012, 18, 1236–1240. [Google Scholar]
- Brown, S.L.; Hansen, S.L.; Langone, J.J. Role of serology in the diagnosis of Lyme disease. JAMA 1999, 282, 62–66. [Google Scholar] [CrossRef]
- Brunner, M. New method for detection of Borrelia burgdorferi antigen complexed to antibody in seronegative Lyme disease. J. Immunol. Methods. 2001, 249, 185–190. [Google Scholar] [CrossRef]
- Tylewska-Wierzbanowska, S.; Chmielewski, T. Limitation of serological testing for Lyme borreliosis: evaluation of ELISA and western blot in comparison with PCR and culture methods. Wien. Klin. Wochenschr. 2002, 114, 601–605. [Google Scholar]
- Forsberg, P.; Ernerudh, J.; Ekerfelt, C.; Roberg, M.; Vrethem, M.; Bergstrom, S. The outer surface proteins of Lyme disease borrelia spirochetes stimulate T cells to secrete interferon-gamma (IFN-gamma): Diagnostic and pathogenic implications. Clin. Exp. Immunol. 1995, 101, 453–460. [Google Scholar]
- Horowitz, H.W.; Pavia, C.S.; Bittker, S.; Forseter, G.; Cooper, D.; Nadelman, R.B.; Byrne, D.; Johnson, R.C.; Wormser, G.P. Sustained cellular immune responses to Borrelia burgdorferi: Lack of correlation with clinical presentation and serology. Clin. Diagn. Lab. Immunol. 1994, 1, 373–378. [Google Scholar]
- Nordberg, M.; Forsberg, P.; Nyman, D.; Skogman, B.H.; Nyberg, C.; Ernerudh, J.; Eliasson, I.; Ekerfelt, C. Can ELISPOT be applied to a clinical setting as a diagnostic utility for Neuroborreliosis? Cells 2012, 1, 153–167. [Google Scholar] [CrossRef]
- Aguero-Rosenfeld, M.E.; Nowakowski, J.; Bittker, S.; Cooper, D.; Nadelman, R.B.; Wormser, G.P. Evolution of the serologic response to Borrelia burgdorferi in treated patients with culture-confirmed erythema migrans. J. Clin. Microbiol. 1996, 34, 1–9. [Google Scholar]
- Dressler, F.; Yoshinari, N.H.; Steere, A.C. The T-cell proliferative assay in the diagnosis of Lyme disease. Ann. Intern. Med. 1991, 115, 533–539. [Google Scholar] [CrossRef]
- Lastavica, C.C.; Snydman, D.R.; Schenkein, D.P.; Berardi, V.P.; Pariser, K.M. Demonstration of Borrelia burgdorferi in a patient with chronic Lyme arthritis. Zentralbl. Bakteriol. Mikrobiol. Hyg. A 1986, 263, 288. [Google Scholar]
- Dattwyler, R.J.; Volkman, D.J.; Luft, B.J.; Halperin, J.J.; Thomas, J.; Golightly, M.G. Seronegative Lyme disease. Dissociation of specific T- and B-lymphocyte responses to Borrelia burgdorferi. N. Engl. J. Med. 1988, 319, 1441–1446. [Google Scholar] [CrossRef]
- Hilton, E.; Tramontano, A.; DeVoti, J.; Sood, S.K. Temporal study of immunoglobin M seroreactivity to Borrelia burgdorferi in patients treated for Lyme borreliosis. J. Clin. Microbiol. 1997, 35, 774–776. [Google Scholar]
- Kalish, R.A.; McHugh, G.; Granquist, J.; Shea, B.; Ruthazer, R.; Steere, A.C. Persistence of immunoglobulin M or immunoglobulin G antibody responses to Borrelia burgdorferi 10–20 years after active Lyme disease. Clin. Infect. Dis. 2001, 33, 780–785. [Google Scholar] [CrossRef]
- Hagen, J.; Houchins, J.P.; Kalyuzhny, A.E. Combining ELISPOT and ELISA to measure amounts of cytokines secreted by a single cell. In Handbook of ELISPOT: Methods and Protocols, Methods in Molecular Biology, 2nd ed.; Kalyuzhny, A., Ed.; Springer Science+Business Media, LLC: New York, NY, USA, 2012; Volume 792, pp. 115–122. [Google Scholar]
- Lehmann, P.V.; Zhang, W. Unique Strengths of ELISPOT for T Cell Diagnostics. In Handbook of ELISPOT: Methods and Protocols, Methods in Molecular Biology, 2nd ed.; Kalyuzhny, A., Ed.; Springer Science+Business Media, LLC: New York, NY, USA, 2012; Volume 792, pp. 3–23. [Google Scholar]
- Tary-Lehmann, M.; Hamm, C.D.; Lehmann, P.V. Validating Reference Samples for Comparison in a Regulated ELISPOT Assay. In Validation of Cell-Based Assays in the GLP Setting: A Practical Guide, 1st ed.; Prabhakar, U., Kelley, M., Eds.; John Wiley & Sons, Ltd.: West Sussex, UK, 2008; pp. 127–146. [Google Scholar]
- Lalvani, A.; Pathan, A.A.; Durkan, H.; Wilkinson, K.A.; Whelan, A.; Deeks, J.J.; Reece, W.H.; Latif, M.; Pasvol, G.; Hill, A.V. Enhanced contact tracing and spatial tracking of Mycobacterium tuberculosis infection by enumeration of antigen-specific T cells. Lancet 2001, 357, 2017–2021. [Google Scholar] [CrossRef]
- Lalvani, A. Counting antigen-specific T cells: A new approach for monitoring response to tuberculosis treatment? Clin. Infect. Dis. 2004, 38, 757–759. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Signs and Symptoms of Lyme Disease, United States. 2013. Available online: http://www.cdc.gov/lyme/signs_symptoms/index.html (accessed on 1 July 2013).
- Wormser, G.P.; Dattwyler, R.J.; Shapiro, E.D.; Halperin, J.J.; Steere, A.C.; Klempner, M.S.; Krause, P.J.; Bakken, J.S.; Strle, F.; Stanek, G.; et al. The clinical assessment, treatment, and prevention of lyme disease, human granulocytic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2006, 43, 1089–1134. [Google Scholar]
- Gross, D.M.; Forsthuber, T.; Tary-Lehmann, M.; Etling, C.; Ito, K.; Nagy, Z.A.; Field, J.A.; Steere, A.C.; Huber, B.T. Identification of LFA-1 as a candidate autoantigen in treatment-resistant Lyme arthritis. Science 1998, 281, 703–706. [Google Scholar] [CrossRef]
- Widhe, M.; Jarefors, S.; Ekerfelt, C.; Vrethem, M.; Bergstrom, S.; Forsberg, P.; Ernerudh, J. Borrelia-Specific interferon-gamma and interleukin-4 secretion in cerebrospinal fluid and blood during Lyme borreliosis in humans: association with clinical outcome. J. Infect. Dis. 2004, 189, 1881–1891. [Google Scholar] [CrossRef]
- Widhe, M.; Skogman, B.H.; Jarefors, S.; Eknefelt, M.; Enestrom, G.; Nordwall, M.; Ekerfelt, C.; Croner, S.; Bergstrom, S.; Forsberg, P.; et al. Up-regulation of Borrelia-specific IL-4- and IFN-gamma-secreting cells in cerebrospinal fluid from children with Lyme neuroborreliosis. Int. Immunol. 2005, 17, 1283–1291. [Google Scholar] [CrossRef]
- Zhang, W.; Tary-Lehmann, M. Objective, User-Independent ELISPOT Data Analysis Based on Scientifically Validated Principles. In Validation of Cell-Based Assays in the GLP Setting: A Practical Guide, 1st ed.; Prabhakar, Uma, Kelley, Marian, Eds.; John Wiley & Sons, Ltd.: West Sussex, UK, 2008; pp. 126–147. [Google Scholar]
- Ekerfelt, C.; Forsberg, P.; Svenvik, M.; Roberg, M.; Bergstrom, S.; Ernerudh, J. Asymptomatic Borrelia-seropositive individuals display the same incidence of Borrelia-specific interferon-gamma (IFN-gamma)-secreting cells in blood as patients with clinical Borrelia infection. Clin. Exp. Immunol. 1999, 115, 498–502. [Google Scholar] [CrossRef]
- Zhang, W.; Caspell, R.; Karulin, A.Y.; Ahmad, M.; Haicheur, N.; Abdelsalam, A.; Johannesen, K.; Vignard, V.; Dudzik, P.; Georgakopoulou, K.; et al. LISPOT assays provide reproducible results among different laboratories for T-cell immune monitoring--even in hands of ELISPOT-inexperienced investigators. J. Immunotoxicol. 2009, 6, 227–234. [Google Scholar] [CrossRef]
- Hesse, M.D.; Karulin, A.Y.; Boehm, B.O.; Lehmann, P.V.; Tary-Lehmann, M. A T cell clone's avidity is a function of its activation state. J. Immunol. 2001, 167, 1353–1361. [Google Scholar]
- Fardy, J. Evaluation of Diagnositc Tests. In Methods of Molecular Biology, Clinical Epidemiology; Parfrey, P., Barrett, B., Eds.; Humana Press: Totowa, NJ, USA, 2009; Volume 473, pp. 127–136. [Google Scholar]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Jin, C.; Roen, D.R.; Lehmann, P.V.; Kellermann, G.H. An Enhanced ELISPOT Assay for Sensitive Detection of Antigen-Specific T Cell Responses to Borrelia burgdorferi. Cells 2013, 2, 607-620. https://doi.org/10.3390/cells2030607
Jin C, Roen DR, Lehmann PV, Kellermann GH. An Enhanced ELISPOT Assay for Sensitive Detection of Antigen-Specific T Cell Responses to Borrelia burgdorferi. Cells. 2013; 2(3):607-620. https://doi.org/10.3390/cells2030607
Chicago/Turabian StyleJin, Chenggang, Diana R. Roen, Paul V. Lehmann, and Gottfried H. Kellermann. 2013. "An Enhanced ELISPOT Assay for Sensitive Detection of Antigen-Specific T Cell Responses to Borrelia burgdorferi" Cells 2, no. 3: 607-620. https://doi.org/10.3390/cells2030607
APA StyleJin, C., Roen, D. R., Lehmann, P. V., & Kellermann, G. H. (2013). An Enhanced ELISPOT Assay for Sensitive Detection of Antigen-Specific T Cell Responses to Borrelia burgdorferi. Cells, 2(3), 607-620. https://doi.org/10.3390/cells2030607