PLGA-Based Microparticles for the Sustained Release of BMP-2
Abstract
: The development of growth factor delivery strategies to circumvent the burst release phenomenon prevalent in most current systems has driven research towards encapsulating molecules in resorbable polymer matrices. For these polymer release techniques to be efficacious in a clinical setting, several key points need to be addressed. This present study has investigated the encapsulation of the growth factor, BMP-2 within PLGA/PLGA-PEG-PLGA microparticles. Morphology, size distribution, encapsulation efficiency and release kinetics were investigated and we have demonstrated a sustained release of bioactive BMP-2. Furthermore, biocompatibility of the PLGA microparticles was established and released BMP-2 was shown to promote the differentiation of MC3T3-E1 cells towards the osteogenic lineage to a greater extent than osteogenic supplements (as early as day 10 in culture), as determined using alkaline phosphatase and alizarin red assays. This study showcases a potential BMP-2 delivery system which may now be translated into more complex delivery systems, such as 3D, mechanically robust scaffolds for bone tissue regeneration applications.1. Introduction
Bone repair may be necessitated by a number of situations including trauma, congenital defects, pathological deformation or revision surgery [1]. In some severe situations spontaneous bone regeneration may not occur [2]. The clinical gold standard in such a situation is bone grafting, but autologous grafting can lead to donor site morbidity and limited donor site availability; allogeneic grafting can lead to infection and rejection [3]. An alternative to grafting is the addition of a biomaterial or scaffold to the defect site to aid tissue regeneration. Most biomaterials alone lack efficacy and have been proven to perform better if combined with cells or bioactive molecules [4].
Growth factors are a group of bioactive molecules currently receiving large research attention in the field of tissue regeneration. They can be used to simulate natural repair processes with great specificity and effectiveness but disadvantages include their low stability, high cost, and the requirement for high doses (to counteract loss from burst release) to illicit a response which in turn may lead to negative side effects [5]. These problems could be reduced by using a sustained delivery approach [6] that has the potential to control both the rate and location of growth factor delivery. However, most delivery systems involve harsh chemical environments during manufacture which may not pose a problem for small drug molecules but may denature bioactive proteins and thereby reduce the activity of the growth factor [7-9].
Bone morphogenetic protein 2 (BMP-2) is the gold standard of growth factor treatment proven to regenerate bone and has been utilised successfully in many studies to date [10,11]. However, maintaining therapeutic concentrations is difficult due to a short half-life in vivo. Various delivery systems have been developed for BMP-2; some are based on collagen (although generally not delivering a sustained release such as Medtronic's INFUSE® [12]), tricalcium phosphate, demineralised bone matrix, hydrogels and polymers [11,13-19]. Some of these have proven to have unpredictable release profiles and many are overwhelmed by an initial high-burst release from the surface bound BMP-2. Consequently, an initial high dose of BMP-2 is often required to be loaded into the carrier in order to achieve active levels within the therapeutic window leading to elevated costs. There is therefore a strong clinical need for better carrier systems for the delivery of growth factors, which enable a sustained release and reduce the need for supra-physiological loading, thus driving down costs and associated biological complications.
Poly (lactic-co-glycolic acid) (PLGA) is a biocompatible, biodegradable polymer [20,21] with a history of over forty years use in medical resorbable sutures [22]. Protein encapsulation by a double emulsion method (water/oil/water) is a well regarded robust technique [23-25] with encapsulation efficiencies in the range of 42% to 100% [26-29]. It has been suggested that denaturation may occur at the water/oil interface but this can often be mitigated with the addition of surfactants and process optimisation [8,30]. Degradation of PLGA occurs by hydrolysis of ester bonds and is accelerated by water ingress [31]. By modifying the lactide:glycolide ratio, the chain length and the addition of plasticisers, the degradation rate of the polymer particles can be modified influencing the release profile.
The goal of this preliminary study was to validate a sustained release system that is composed of PLGA with the plasticiser PLGA-poly(ethylene glycol) (PEG)-PLGA for the formation of microparticles containing encapsulated BMP-2. The morphology, size, encapsulation efficiency of protein and release kinetics of the PLGA microparticle delivery system was characterised. We demonstrated sustained BMP-2 release over 2 weeks that stimulated MC3T3-E1 cells to differentiate and form bone-like mineral depositions. We also assessed the expression of alkaline phosphatase as an early marker of differentiation. This microparticle delivery system was also attached to a 3D scaffold with the future aim of supplementing a mechanically supportive scaffold with a sustained release system.
2. Results and Discussion
2.1. Microparticle Characterisation and Analysis
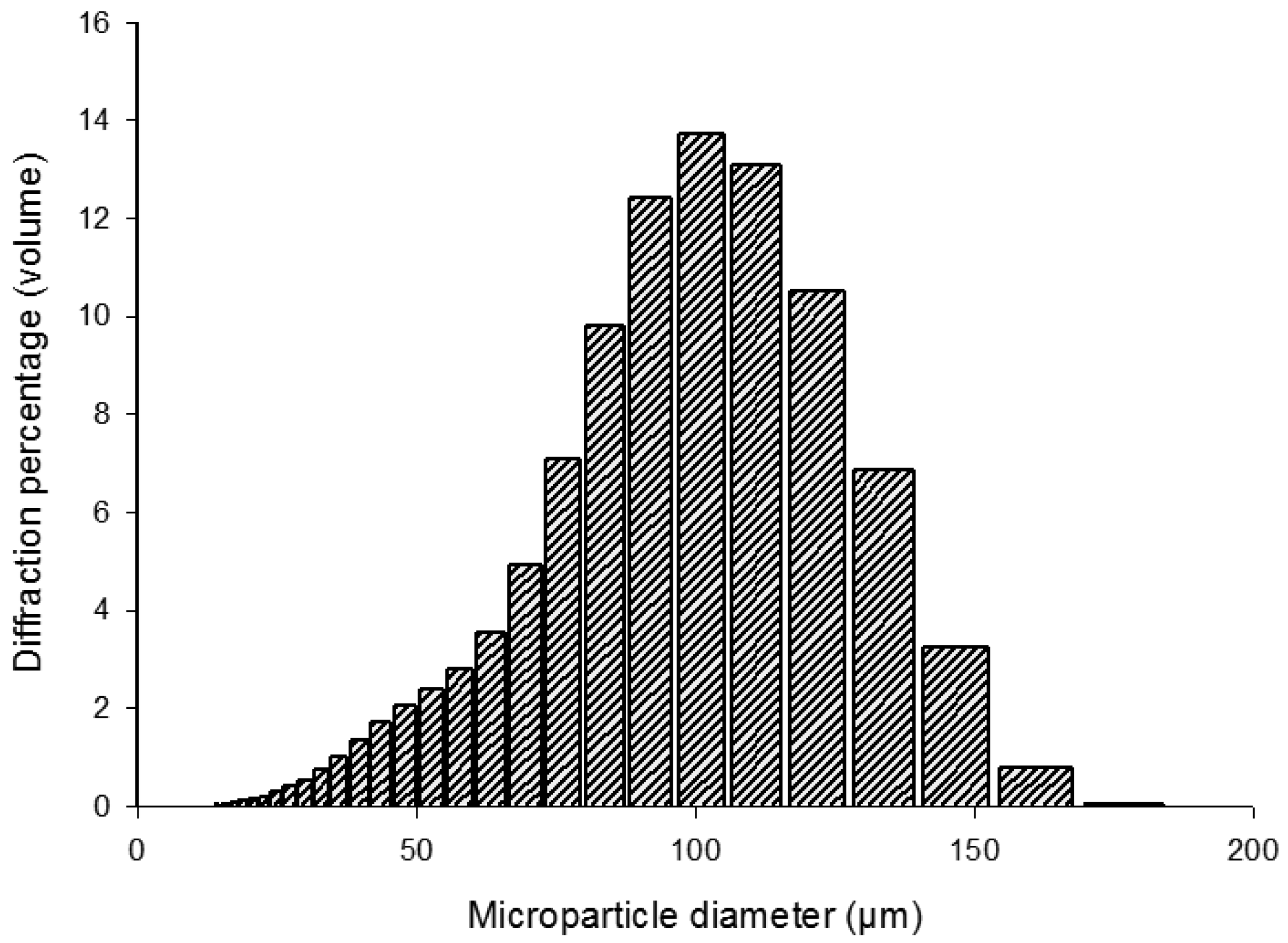
The mean diameter of the PLGA composite microparticles was 97.85 μm (SD ± 30.06). Multiple batches of microparticles formed under the same conditions demonstrated repeatable distributions. As a result of the emulsion process, the PLGA/PLGA-PEG-PLGA microparticles demonstrated a bell curve size distribution as shown in Figure 1.
The entrapment efficiency of PLGA/PLGA-PEG-PLGA composite microparticles was 57.1% (SD ± 4.4%). Scanning electron microscopy (SEM) images of the microparticles loaded with protein revealed a regular spherical morphology, which was not damaged by the process of protein incorporation (Figure 2). The apparent size of the microparticles ascertained with SEM is in agreement with the laser diffraction data.
This formulation of PLGA and PLGA-PEG-PLGA (90% PLGA, 10% PLGA-PEG-PLGA) mitigates the common problem of burst release [32]; delivering a sustained dose of protein as shown in Figure 3. Most delivery systems deliver a burst release during the first few hours often releasing over 60% of the encapsulated/surface bound product [11,33]. This burst release may still have therapeutic benefit as proven with products such as INFUSE® (Medtronic) (which has no sustained release system and relies on a burst delivery) but due to the short half-life in vivo of BMP-2, the therapeutic dose may be quickly depleted as the BMP-2 degrades. Furthermore a supra-physiological loading of BMP-2 is required in these systems which greatly increases the cost and may lead to several disadvantageous side-effects [34]. A therapeutic delivery system with the ability to sustain an active dose of BMP-2 may prove more effective in a clinical situation as it avoids the costly waste of BMP-2 and should demonstrate reduced side effects as no supra-physiological loading is required. Our system released protein gradually over a time course of 2 weeks, as shown in Figure 3, and did not demonstrate high initial burst release, indicating that the protein was encapsulated effectively within the microparticles (as opposed to being surface bound) and was releasing as the microparticles degraded with time. The inclusion of hydrophilic PLGA-PEG-PLGA is how the release profile was tailored. Once in a wet environment the PLGA-PEG-PLGA facilitated water ingress into the hydrophobic PLGA. This increased the rate of hydrolysis of the PLGA thereby increasing the rate of degradation and protein release. This mitigated the common lag phase seen in pure PLGA formulations whereby the surface-bound protein causes the initial burst release and a lag is observed until such time that the PLGA begins to degrade releasing entrapped protein [35,36]. This formulation is a slow release formulation, releasing 7% of the entrapped protein by day 13. Based on this release rate 5 mg of microparticles (as used in vitro) will release on average 18.5 ng of BMP-2 daily. This is above the lower limits shown to induce alkaline phosphatase (ALP) expression in MC3T3-E1 cells [37].
2.2. Cell Culture in 2D
2.2.1. Cells in Culture with PLGA Microparticles
After six days in culture, the MC3T3-E1 cells show clear differences in attachment and orientation towards the microparticles with and without BMP-2 inclusion. The BMP-2 releasing microparticles appear to offer a favourable environment over the tissue culture plastic, with cells attaching to and bridging between the microparticles preferentially. In contrast the control microparticles appear to have no enhanced adhesive properties on the cells. The cells display no orientation inclination around the non-BMP-2 containing spheres nor do they avoid growing adjacently to them, as depicted in Figure 4. The addition of exogenous BMP-2 has reportedly increased osteoblast attachment to titanium alloy by inducing a more extensive extracellular matrix thereby increasing surface contact of the cells with the alloy [38]. A similar process may be positively influencing cell attachment to the microparticles that are releasing BMP-2.
2.2.2. Analysis of Alkaline Phosphatase Activity
To assess the effect of different volumes of BMP-2 loaded microparticles on the differentiation of MC3T3-E1 cells, the activity of ALP was quantified at days 10, 17 and 24. ALP is an early marker of differentiation towards the osteoblastic lineage [39,40] and it is anticipated that BMP-2 released from the microparticles would push the cells towards the osteogenic lineage. As expected, the control group expressed low levels of ALP and there was no significant difference between time points, as depicted in Figure 5. The cells exposed to osteogenic media showed significantly higher levels of ALP at all time points (compared to control) indicating differentiation of the cell population. Small amounts (0.5 mg) of BMP-2 loaded microparticles induced an effect similar to that of the osteogenic control at day 10, although this decreased at day 17 and day 24. The expression of ALP at day 10 by cells cultured with 5 mg of microparticles containing BMP-2 was the most significant (more than 3-fold higher than the 0.5 mg BMP-2 group) remaining higher than the control at day 17 and not significantly different to any condition at day 24.
These results indicate that the BMP-2 released from the microparticles was bioactive at a concentration sufficient to have an osteogenic effect on the cells and the effect was more prevalent at earlier time points. This is consistent with ALP being regarded as an early marker of differentiation.
2.2.3. Observation of Mineralised Bone-Like Tissue
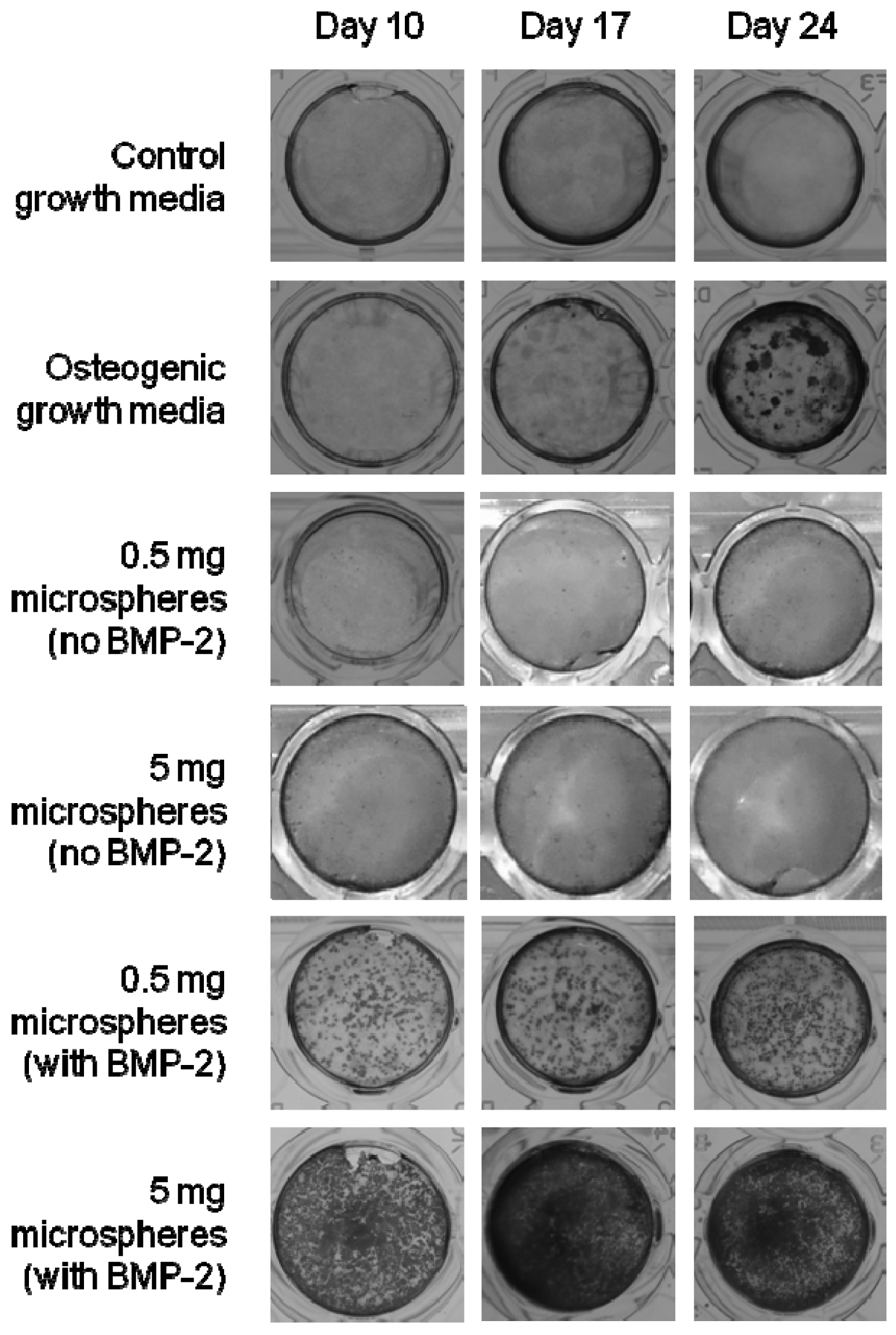
After 10, 17 and 24 days in culture, cells were stained with alizarin red to identify calcium phosphate mineral deposition (an indicator of differentiation) and photographed under optical microscopy. Figure 6 shows the results of this qualitative histochemical assay. The control samples also showed no positive staining. The positive control (cells cultured with osteogenic media) showed clear staining for calcium deposits at day 17 increasing at day 24. Interestingly, the cells cultured in the presence of the BMP-2 loaded microparticles show staining as early as day 10 for both sets of BMP-2 containing microparticles. Due to the mildly acidic conditions surrounding the degrading PLGA, the alizarin red stain appeared slightly yellow over time. This was a response of the stain to the pH condition. To verify that the PLGA composite was not giving a false positive, control microparticles were also cultured with MC3T3-E1′s and stained with alizarin red in an identical manner. They showed a clearly negative result for staining.
These results support the aforementioned alkaline phosphatase data (Figure 5) which indicate that the BMP-2 released from the microparticles is bioactive and inducing early differentiation of the MC3T3 cells compared with standard osteogenic induction techniques.
At higher magnification, a striking zonal deposition of alizarin red staining was observed which followed the contours of the microparticles, shown in Figure 7. This may be a result of the BMP-2 released from the microparticles creating concentration gradients which provided a non-homogenous differentiation environment. Interestingly the mineral deposition was not immediately adjacent to the microparticles but was consistently localised a short distance away from them.
2.3. Incorporation of Microparticles in 3D Scaffolds
Having established the ability of the microparticles to release BMP-2, we next attached the microparticles to a well-established 3D scaffold comprising medical grade ε-poly-caprolactone incorporating 20% (w/w) β-tricalcium phosphate (mPCL-TCP). This demonstrated the feasibility of incorporating the delivery system into a more mechanically robust scaffold environment providing a multifunctional scaffold which has both mechanical stability combined with growth factor releasing potential. Figure 8 shows the scaffold produced; further studies will verify the release in the 3D environment, cellular differentiation in the 3D environment and ultimately investigate the effect of the 3D composite scaffold on in vitro/in vivo bone regeneration.
3. Experimental Section
3.1. PLGA-PEG-PLGA Triblock Copolymer Preparation
The PLGA-PEG-PLGA triblock co-polymer was formed using a method outlined by Zentner et al. 2001 [41] and refined by Hou et al. 2008 [42]. It was synthesised using a ring opening polymerisation of cyclic dimers of D,L-lactide (Lancaster synthesis, Alfa Aesar) and Glycolide (Purac, Netherlands) with PEG 1,500 kDa (Sigma-Aldrich, UK) in the presence of the catalyst stannous octoate (Sigma-Aldrich, UK). The PEG was heated to 120 °C under vacuum, the temperature then raised to 150 °C, and the D,L-lactide and glycolide were added. The reaction was maintained at 150 °C for 30 minutes under a nitrogen atmosphere. The stannous octoate was then added and the reaction was allowed to proceed for 8 hours. The resultant copolymer was dissolved and precipitated in water in order to remove the unreacted lactide and glycolide. The PLGA-PEG-PLGA was then dried under vacuum and stored at −20 °C until required for use.
3.2. Microparticle Preparation
Poly(lactic-co-glycolic acid) (PLGA 85:15 DLG 4A, molecular weight 56 kDa, Lakeshore Biomaterials, Birmingham, Alabama, USA) microparticles were formed using a water in oil in water (w/o/w) emulsion method. An aqueous solution of human serum albumin (HSA, Sigma UK) and BMP-2 was added to a solution of PLGA and PLGA-PEG-PLGA (90%:10% respectively) in dichloromethane (Fisher Scientific, UK). These phases were homogenized (Silverson L5M homogeniser) for 2 min at 4,000 rpm to form the water in oil emulsion. This emulsion was added to a 200 mL aqueous solution of polyvinyl alcohol (PVA) (0.3%) and homogenized for 2 min at 2,000 rpm. This double emulsion was stirred magnetically for 4 hours at 300 rpm before the microparticles were filtered, washed and lyophilized. The concentration of the protein solution was 90 mg/mL HSA and 10 mg/mL BMP-2. The polymer was used at a mass of 1 gram in 5 mL dichloromethane. At these concentrations a 100 μL aliquot of protein solution (as used in the primary emulsion) gave a protein loading of 1% with respect to polymer mass. Control particles were loaded with a protein concentration of 100 mg/mL HSA and formed using the above method.
3.3. Microparticle Characterization
3.3.1. Determination of Size Distribution of Microparticles
Due to the high cost of BMP-2, some of the analysis was carried out on batches of microparticles analogous to those containing 0.1% (w/w) BMP-2 but with a lower loading of growth factor. To maintain the overall protein loading at 1% the ratio of HSA to BMP-2 was increased.
A suspension of the microparticles was prepared in double deionised water and sized using a laser diffraction method (Coulter LS230, fitted with the hazardous fluids module, Beckman Coulter, UK) while under agitation to prevent the particles settling.
3.3.2. Scanning Electron Microscopy
Microparticles of PLGA were gold sputter coated for 4.5 min at 30 mA (Baltzers SCD 030 gold sputter coater). Imaging was carried out with an accelerating voltage of 10 Kv (JEOL 6060LV variable pressure scanning electron microscope).
3.3.3. Determination of Protein Entrapment within the Microparticles
The measurement of the encapsulation efficiency of protein within the microparticles was a modification of an extraction method used by Morita et al. 2001 [43] based on techniques first explored by Sah et al. 1999 [8]. PLGA microparticles (10 mg) were incubated in 750 μL dimethyl sulphoxide (DMSO) (Fisher scientific) at room temperature for 1 hour, 2,150 μL of 0.5% SLS/0.02 N NaOH was added for a further incubation at room temperature for one hour. The resulting solution was measured using a bicinchoninic acid (BCA) protein assay kit (Thermo scientific) to ascertain the protein content and compared against a standard curve of HSA conducted at the same time. Sample (150 μL) and BCA working reagent (150 μL) were mixed and incubated for 2 hours at 37 °C and the absorbance at 462 nm measured using a Tecan infinite 200 plate reader.
3.4. Release Study
Aliquots of the microparticles (100 mg) were suspended in 3 mL of phosphate buffered saline (PBS) and then incubated at 37 °C under gentle agitation (orbital rocker set at 5 rpm). At regular intervals the PBS was completely replaced and assayed for protein content using the BCA assay kit. Calibration standards reflected the formulation of protein within the microparticles and were prepared in PBS.
3.5. Cell Culture
Murine calvaria pre-osteoblast (MC3T3-E1) cells were cultured with α-minimum essential medium (αMEM) (Invitrogen) supplemented with 10% (v/v) foetal calf serum (Invitrogen), 100 U/mL penicillin and 100 μg/mL streptomycin (Invitrogen) as the standard growth media. The osteogenic growth media included 10mM β-glycerophosphate, 0.1 mM ascorbate-2-phosphate and 100 nM dexamethasone. Cells were cultured at 37 °C in a humidified 5% CO2 atmosphere and the media was replenished twice weekly.
The MC3T3-E1 cells were seeded into 48-well tissue culture plates at 5 × 103 cells per well (1 × 104 cells per mL). The cells were cultured under six different conditions (n = 4) and assayed at three time points. During media changes, care was taken not to disturb/aspirate the PLGA microparticles.
3.6. Alizarin Red
Cells were washed with PBS and fixed with ice cold methanol. Alizarin red dye (Sigma) was prepared at a concentration of 20 mg/mL in water and the pH was adjusted using 0.5% (v/v) ammonium hydroxide so that it was in the range 4.1–4.3. The cells were incubated with the alizarin red stain for 5 min then washed several times with deionised water. The wells were photographed using standard photography (Sony DSC-W55) and under optical microscopy (Nikon Eclipse TS100—PixeLINK).
3.7. Alkaline Phosphatase
The cells were washed with PBS before being incubated at −20 °C in a solution of 0.1% Triton X-100 in 0.2 M Tris buffer, pH 8. The cell lysate was centrifuged for 10 min at 10,000 rpm at 4 °C and the supernatant added to a 96 well assay plate (100 μL/well) in triplicate to which 200 μL pNPP substrate solution was added (SigmaFAST, p-Nitrophenyl phosphate tablets N1891). A control well of 0.1% (v/v) Triton X-100 in 0.2 M Tris buffer was also assayed. The plate was incubated for 30 min (room temperature) and the absorbance measured at 405 nm (BIO RAD Benchmark Plus).
3.8. Microparticle Attachment to 3D Scaffolds
The microparticles were attached to fused deposition modelled scaffolds made from medical grade 8-poly-caprolactone incorporating 20% w/w β-tricalcium phosphate (mPCL-TCP) (Osteopore International, Singapore) by softening the microparticles with a 10% v/v DMSO solution (scaffolds were dipped for 5 seconds into the solvent solution and dry particles were added manually using a spatula). This technique allowed the microparticles to attach to the scaffolds without disrupting the morphology of either the microparticles or the scaffold (higher concentrations of DMSO adversely affected the microparticle morphology). The application of distilled water to the scaffolds helped evenly distribute the microparticles within the pores and the microparticles remained attached as the scaffold was dried.
For photographic purposes, microparticles were pre-stained with Oil red O (Sigma, UK) before attachment to the mPCL-TCP scaffolds. These stained microparticles were not used for cell culture.
3.9. Statistical Analysis
Statistical comparisons were carried out using the SPSS 18.0.1 software package. Comparisons were made using Tukey-Kramer analysis of variance (ANOVA) and results were considered significant if p < 0.05.
4. Conclusions
The shift in tissue engineering towards more regenerative approaches is increasingly focusing on the use of scaffolds and exogenous signalling molecules. While the delivery of small robust molecules such as drugs is fairly well understood, there remain uncertainties surrounding the delivery of an active protein from a resorbing polymer matrix. For these polymer release techniques to be efficacious in a clinical setting, several key areas such as entrapment efficiency, activity retention, and subsequent release of the protein need to be investigated. This present study has addressed the encapsulation of the growth factor BMP-2 within a polymer formulation candidate. Morphology, size distribution, encapsulation efficiency and release kinetics of the resultant microparticles have all been verified. This formulation has shown the ability to mitigate the large burst release, by the inclusion of a triblock co-polymer PLGA-PEG-PLGA in the formulation, usually seen in micro-delivery vehicles and offers a reproducible and sustained release. Furthermore biocompatibility of the PLGA microparticles and preferential cell behaviour towards BMP-2 loaded microparticles has been demonstrated. In contrast, negative control microparticles containing no BMP-2 have demonstrated no significant effect on cell behaviour. Both high and low levels of BMP-2 loaded PLGA microparticles have demonstrated the ability to release bioactive BMP-2 which stimulates osteogenic differentiation (ascertained using alkaline phosphatase and alizarin red assays) by day 10, outperforming cells cultured with osteogenically supplemented media which only showed mineral deposition at day 24. This study demonstrates a BMP-2 delivery system which may now be translated into more complex delivery systems such as 3D mechanically robust scaffolds which may be suitable for implantation into a load-bearing defect site.






| Time point | Blank microparticles (0.5 mg/well ± 20%) | Blank microparticles (5 mg/well ± 20%) | BMP-2 loaded microparticles (0.5 mg/well ± 20%) | BMP-2 loaded microparticles (5 mg/well ± 20%) | Control media | Osteogenic media |
|---|---|---|---|---|---|---|
| Day 10 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 |
| Day 17 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 |
| Day 24 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 | n = 4 |
Acknowledgments
This work was a collaboration between the University of Nottingham (UK) and the Queensland University of Technology (Australia) with funding from the Engineering and Physical Sciences Research Council (EPSRC) Doctoral Training Centre in Regenerative Medicine and The Australian Research Council Discovery Grant (DP089000).
References
- Lasanianos, N.G.; Kanakaris, N.K.; Giannoudis, P.V. Current management of long bone large segmental defects. Orthopaed. Trauma 2010, 24, 149–163. [Google Scholar]
- Luginbuehl, V.; Meinel, L.; Merkle, H.P.; Gander, B. Localized delivery of growth factors for bone repair. Eur. J. Pharm. Biopharm. 2004, 58, 197–208. [Google Scholar]
- Reichert, J.C.; Saifzadeh, S.; Wullschleger, M.E.; Epari, D.R.; Schütz, M.A.; Duda, G.N.; Schell, H.; van Griensven, M.; Redl, H.; Hutmacher, D.W. The challenge of establishing preclinical models for segmental bone defect research. Biomaterials 2009, 30, 2149–2163. [Google Scholar]
- Vinatier, C.; Mrugala, D.; Jorgensen, C.; Guicheux, J.; Noël, D. Cartilage engineering: A crucial combination of cells, biomaterials and biofactors. Trends Biotechnol. 2009, 27, 307–314. [Google Scholar]
- Ryoo, H.-M.; Lee, M.-H.; Kim, Y.-J. Critical molecular switches involved in BMP-2-induced osteogenic differentiation of mesenchymal cells. Gene 2006, 366, 51–57. [Google Scholar]
- Putney, S.D.; Burke, P.A. Improving protein therapeutics with sustained-release formulations. Nat. Biotech. 1998, 16, 153–157. [Google Scholar]
- van de Weert, M.; Hennink, W.E.; Jiskoot, W. Protein instability in poly(Lactic-co-Glycolic acid) microparticles. Pharm. Res. 2000, 17, 1159–1167. [Google Scholar]
- Sah, H. Stabilization of proteins against methylene chloride/water interface-induced denaturation and aggregation. J. Control. Release 1999, 58, 143–151. [Google Scholar]
- Jin, T.; Zhu, J.; Wu, F.; Yuan, W.; Geng, L.L.; Zhu, H. Preparing polymer-based sustained-release systems without exposing proteins to water-oil or water-air interfaces and cross-linking reagents. J. Control. Release 2008, 128, 50–59. [Google Scholar]
- Tsuji, K.; Bandyopadhyay, A.; Harfe, B.D.; Cox, K.; Kakar, S.; Gerstenfeld, L.; Einhorn, T.; Tabin, C.J.; Rosen, V. BMP2 activity, although dispensable for bone formation, is required for the initiation of fracture healing. Nat. Genet 2006, 38, 1424–1429. [Google Scholar]
- Sawyer, A.A.; Song, S.J.; Susanto, E.; Chuan, P.; Lam, C. X.F.; Woodruff, M.A.; Hutmacher, D.W.; Cool, S.M. The stimulation of healing within a rat calvarial defect by mPCL-TCP/collagen scaffolds loaded with rhBMP-2. Biomaterials 2009, 30, 2479–2488. [Google Scholar]
- Burkus, J.K.; Heim, S.E.; Gornet, M.F.; Zdeblick, T.A. Is INFUSE bone graft superior to autograft bone? an integrated analysis of clinical trials using the lt-cage lumbar tapered fusion device. J. Spinal Disorders Tech. 2003, 16, 113–122. [Google Scholar]
- Maeda, H.; Sano, A.; Fujioka, K. Controlled release of rhBMP-2 from collagen minipellet and the relationship between release profile and ectopic bone formation. Int. J. Pharm. 2004, 275, 109–122. [Google Scholar]
- Liang, G.; Yang, Y.; Oh, S.; L Ong, J.; Zheng, C.; Ran, J.; Yin, G.; Zhou, D. Ectopic osteoinduction and early degradation of recombinant human bone morphogenetic protein-2-loaded porous [beta]-tricalcium phosphate in mice. Biomaterials 2005, 26, 4265–4271. [Google Scholar]
- Jha, A.K.; Yang, W.; Kirn-Safran, C.B.; Farach-Carson, M.C.; Jia, X. Perlecan domain I-conjugated, hyaluronic acid-based hydrogel particles for enhanced chondrogenic differentiation via BMP-2 release. Biomaterials 2009, 30, 6964–6975. [Google Scholar]
- Calori, G.M.; Donati, D.; Di Bella, C.; Tagliabue, L. Bone morphogenetic proteins and tissue engineering: Future directions. Injury 2009, 40, S67–S76. [Google Scholar]
- Puppi, D.; Chiellini, F.; Piras, A.M.; Chiellini, E. Polymeric materials for bone and cartilage repair. Progr. Polym. Sci. 2010, 35, 403–440. [Google Scholar]
- Saito, N.; Murakami, N.; Takahashi, J.; Horiuchi, H.; Ota, H.; Kato, H.; Okada, T.; Nozaki, K.; Takaoka, K. Synthetic biodegradable polymers as drug delivery systems for bone morphogenetic proteins. Adv. Drug Delivery Rev. 2005, 57, 1037–1048. [Google Scholar]
- Rai, B.; Teoh, S.H.; Hutmacher, D.W.; Cao, T.; Ho, K.H. Novel PCL-based honeycomb scaffolds as drug delivery systems for rhBMP-2. Biomaterials 2005, 26, 3739–3748. [Google Scholar]
- Anderson, J.M.; Shive, M.S. Biodegradation and biocompatibility of PLA and PLGA microspheres. Adv. Drug Delivery Rev. 1997, 28, 5–24. [Google Scholar]
- Jain, R.A. The manufacturing techniques of various drug loaded biodegradable poly(lactide-co-glycolide) (PLGA) devices. Biomaterials 2000, 21, 2475–2490. [Google Scholar]
- Zolnik, B.S.; Burgess, D.J. Effect of acidic pH on PLGA microsphere degradation and release. J. Control. Release 2007, 122, 338–344. [Google Scholar]
- Meng, F.T.; Ma, G.H.; Qiu, W.; Su, Z.G. W/O/W double emulsion technique using ethyl acetate as organic solvent: Effects of its diffusion rate on the characteristics of microparticles. J. Control. Release 2003, 91, 407–416. [Google Scholar]
- Nihant, N.; Schugens, C.; Grandfils, C.; Jerome, R.; Teyssie, P. Polylactide microparticles prepared by double emulsion-evaporation: II. Effect of the poly(Lactide-co-Glycolide) composition on the stability of the primary and secondary emulsions. J. Colloid Interface Sci. 1995, 173, 55–65. [Google Scholar]
- Schugens, C.; Laruelle, N.; Nihant, N.; Grandfils, C.; Jérome, R.; Teyssié, P. Effect of the emulsion stability on the morphology and porosity of semicrystalline poly L-lactide microparticles prepared by w/o/w double emulsion-evaporation. J. Control. Release 1994, 32, 161–176. [Google Scholar]
- Yang, Y.-Y.; Chia, H.-H.; Chung, T.-S. Effect of preparation temperature on the characteristics and release profiles of PLGA microspheres containing protein fabricated by double-emulsion solvent extraction/evaporation method. J. Control. Release 2000, 69, 81–96. [Google Scholar]
- Yang, Y.-Y.; Chung, T.-S.; Ping Ng, N. Morphology, drug distribution, and in vitro release profiles of biodegradable polymeric microspheres containing protein fabricated by double-emulsion solvent extraction/evaporation method. Biomaterials 2001, 22, 231–241. [Google Scholar]
- Park, T.G.; Yong Lee, H.; Sung Nam, Y. A new preparation method for protein loaded poly(D, L-lactic-co-glycolic acid) microspheres and protein release mechanism study. J. Control. Release 1998, 55, 181–191. [Google Scholar]
- Péan, J.M.; Venier-Julienne, M.C.; Filmon, R.; Sergent, M.; Phan-Tan-Luu, R.; Benoit, J.P. Optimization of HSA and NGF encapsulation yields in PLGA microparticles. Int. J. Pharm. 1998, 166, 105–115. [Google Scholar]
- Kang, F.; Singh, J. Conformational stability of a model protein (bovine serum albumin) during primary emulsification process of PLGA microspheres synthesis. Int. J. Pharm. 2003, 260, 149–156. [Google Scholar]
- Siepmann, J.; Göpferich, A. Mathematical modeling of bioerodible, polymeric drug delivery systems. Adv. Drug Delivery Rev. 2001, 48, 229–247. [Google Scholar]
- Giteau, A.; Venier-Julienne, M.C.; Aubert-Pouëssel, A.; Benoit, J.P. How to achieve sustained and complete protein release from PLGA-based microparticles? Int. J. Pharm. 2008, 350, 14–26. [Google Scholar]
- Woodruff, M.A.; Rath, S.N.; Susanto, E.; Haupt, L.M.; Hutmacher, D.W.; Nurcombe, V.; Cool, S.M. Sustained release and osteogenic potential of heparan sulfate-doped fibrin glue scaffolds within a rat cranial model. J. Mol. Histol. 2007, 38, 425–433. [Google Scholar]
- Bessa, P.C.; Casal, M.; Reis, R.L. Bone morphogenetic proteins in tissue engineering: The road from laboratory to clinic, Part II (BMP delivery). J. Tissue Eng. Regenerative Med. 2008, 2, 81–96. [Google Scholar]
- Sandor, M.; Enscore, D.; Weston, P.; Mathiowitz, E. Effect of protein molecular weight on release from micron-sized PLGA microspheres. J. Control. Release 2001, 76, 297–311. [Google Scholar]
- Cleland, J.L.; Duenas, E.; Daugherty, A.; Marian, M.; Yang, J.; Wilson, M.; Celniker, A.C.; Shahzamani, A.; Quarmby, V.; Chu, H.; Mukku, V.; Mac, A.; Roussakis, M.; Gillette, N.; Boyd, B.; Yeung, D.; Brooks, D.; Maa, Y.-F.; Hsu, C.; Jones, A.J.S. Recombinant human growth hormone poly(lactic-co-glycolic acid) (PLGA) microspheres provide a long lasting effect. J. Control. Release 1997, 49, 193–205. [Google Scholar]
- Takuwa, Y.; Ohse, C.; Wang, E.A.; Wozney, J.M.; Yamashita, K. Bone morphogenetic protein-2 stimulates alkaline phosphatase activity and collagen synthesis in cultured osteoblastic cells, MC3T3-E1. Biochem. Biophys. Res. Commun. 1991, 174, 96–101. [Google Scholar]
- Shah, A.K.; Lazatin, J.; Sinha, R.K.; Lennox, T.; Hickok, N.J.; Tuan, R.S. Mechanism of BMP-2 stimulated adhesion of osteoblastic cells to titanium alloy. Biol. Cell 1999, 91, 131–142. [Google Scholar]
- Narayanan, K.; Srinivas, R.; Ramachandran, A.; Hao, J.; Quinn, B.; George, A. Differentiation of embryonic mesenchymal cells to odontoblast-like cells by overexpression of dentin matrix protein 1. Proc. Natl. Acad. Sci. USA 2001, 98, 4516–4521. [Google Scholar]
- Li, J.; Yun, H.; Gong, Y.; Zhao, N.; Zhang, X. Investigation of MC3T3-E1 cell behavior on the surface of GRGDS-coupled chitosan. Biomacromolecules 2006, 7, 1112–1123. [Google Scholar]
- Zentner, G.M.; Rathi, R.; Shih, C.; McRea, J.C.; Seo, M.-H.; Oh, H.; Rhee, B.G.; Mestecky, J.; Moldoveanu, Z.; Morgan, M.; Weitman, S. Biodegradable block copolymers for delivery of proteins and water-insoluble drugs. J. Control. Release 2001, 72, 203–215. [Google Scholar]
- Hou, Q.; Chau, D.Y.S.; Pratoomsoot, C.; Tighe, P.J.; Dua, H.S.; Shakesheff, K.M.; Rose, F.R.A.J. In situ gelling hydrogels incorporating microparticles as drug delivery carriers for regenerative medicine. J. Pharm. Sci. 2008, 97, 3972–3980. [Google Scholar]
- Morita, T.; Horikiri, Y.; Suzuki, T.; Yoshino, H. Applicability of various amphiphilic polymers to the modification of protein release kinetics from biodegradable reservoir-type microspheres. Eur. J. Pharm. Biopharm. 2001, 51, 45–53. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Kirby, G.T.S.; White, L.J.; Rahman, C.V.; Cox, H.C.; Qutachi, O.; Rose, F.R.A.J.; Hutmacher, D.W.; Shakesheff, K.M.; Woodruff, M.A. PLGA-Based Microparticles for the Sustained Release of BMP-2. Polymers 2011, 3, 571-586. https://doi.org/10.3390/polym3010571
Kirby GTS, White LJ, Rahman CV, Cox HC, Qutachi O, Rose FRAJ, Hutmacher DW, Shakesheff KM, Woodruff MA. PLGA-Based Microparticles for the Sustained Release of BMP-2. Polymers. 2011; 3(1):571-586. https://doi.org/10.3390/polym3010571
Chicago/Turabian StyleKirby, Giles T. S., Lisa J. White, Cheryl V. Rahman, Helen C. Cox, Omar Qutachi, Felicity R. A. J. Rose, Dietmar W. Hutmacher, Kevin M. Shakesheff, and Maria A. Woodruff. 2011. "PLGA-Based Microparticles for the Sustained Release of BMP-2" Polymers 3, no. 1: 571-586. https://doi.org/10.3390/polym3010571






