Baseline and Estimated Trends of Sodium Availability and Food Sources in the Costa Rican Population during 2004–2005 and 2012–2013
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Global Burden of Disease 2015 Risk Factors Collaborators. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016, 388, 1659–1724. Available online: https://www.ncbi.nlm.nih.gov/pubmed/27733284 (accessed on 28 July 2017).
- World Health Organization (WHO). Guideline: Sodium Intake for Adults and Children; WHO: Geneva, Switzerland, 2012; Available online: http://www.who.int/nutrition/publications/guidelines/sodium_intake_printversion.pdf (accessed on 28 July 2017).
- He, F.J.; MacGregor, G.A. A comprehensive review on salt and health and current experience of worldwide salt reduction programmes. J. Hum. Hypertens. 2009, 23, 363–384. Available online: https://www.ncbi.nlm.nih.gov/pubmed/19110538 (accessed on 15 June 2017). [PubMed]
- Lawes, C.M.; Vander Hoorn, S.; Rodgers, A.; International Society of Hypertension. Global burden of blood-pressure-related disease, 2001. Lancet 2008, 371, 1513–1518. Available online: https://www.ncbi.nlm.nih.gov/pubmed/18456100 (accessed on 28 August 2017). [PubMed]
- World Health Organization (WHO). Reducing Sodium Intake to Reduce Blood Pressure and Risk of Cardiovascular Diseases in Adults; e-Library of Evidence for Nutrition Actions (eLENA), WHO: Geneva, Switzerland, 2017; Available online: http://www.who.int/mediacentre/factsheets/fs317/en/ (accessed on 3 May 2017).
- GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016, 388, 1459–1544. Available online: https://www.researchgate.net/publication/308904659_Global_regional_and_national_life_expectancy_all-cause_mortality_and_cause-specific_mortality_for_249_causes_of_death_1980-2015_a_systematic_analysis_for_the_Global_Burden_of_Disease_Study_2015 (accessed on 29 July 2017).
- Caja Costarricense del Seguro Social. Vigilancia de los Factores de Riesgo Cardiovascular; Servicios Gráficos: San José, Costa Rica, 2011; p. 41. Available online: http://www.binasss.sa.cr/informesdegestion/vigilancia.pdf (accessed on 3 May 2017).
- Costa Rica. Ministerio de Salud, Instituto Costarricense de Investigación y Enseñanza en Nutrición y Salud, Caja Costarricense del Seguro Social y Organización Panamericana de la Salud. Encuesta Multinacional de Diabetes Mellitus, Hipertensión Arterial y Factores de Riesgo Asociados, Área Metropolitana, San José, 2004; El Ministerio: San José, Costa Rica, 2009; pp. 12–15. Available online: http://www2.paho.org/hq/index.php?option=com_docman&task=doc_view&gid=16262&Itemid=270 (accessed on 3 May 2017).
- Caja Costarricense del Seguro Social. Vigilancia de los Factores de Riesgo Cardiovascular. Segunda Encuesta, 2014; Editorial Nacional de Salud y Seguridad Social: San José, Costa Rica, 2016; pp. 34–92. Available online: http://www.binasss.sa.cr/informesdegestion/encuesta2014.pdf (accessed on 4 June 2017).
- World Health Organization. Salt Reduction. Available online: http://www.who.int/mediacentre/factsheets/fs393/en/ (accessed on 1 August 2017).
- He, F.J.; Campbell, N.R.; MacGregor, G.A. Reducing salt intake to prevent hypertension and cardiovascular disease. Rev. Panam. Salud Pública 2012, 32, 293–300. Available online: https://www.ncbi.nlm.nih.gov/pubmed/23299291 (accessed on 3 May 2017). [CrossRef] [PubMed]
- Sarno, F.; Moreira, R.; Bertazzi, R.; Henrique, D.; Gouvea, S.; Monteiro, C.A. Estimated sodium intake by the Brazilian population, 2002–2003. Rev. Saúde Pública 2009, 43, 1–6. Available online: https://www.ncbi.nlm.nih.gov/pubmed/19225699 (accessed on 6 May 2017).
- Sarno, F.; Claro, R.M.; Levy, R.B.; Bandoni, D.H.; Monteiro, C.A. Estimated sodium intake for the Brazilian population, 2008–2009. Rev. Saude Publica 2013, 47, 571–578. Available online: https://www.ncbi.nlm.nih.gov/pubmed/24346570 (accessed on 6 May 2017). [CrossRef] [PubMed]
- European Commission. Survey on Members States Implementation of the EU Salt Reduction Framework; Publications Office of the European Union: Luxemberg, Belgium, 2012; p. 14. Available online: http://ec.europa.eu/health//sites/health/files/nutrition_physical_activity/docs/salt_report1_en.pdf (accessed on 6 May 2017).
- Hlastan, R.; Zakotnik, J.M.; Seljak, B.K.; Polinick, R.; Blaznik, U.; Mis, N.F.; Erzen, I.; Ji, C.; Cappuccio, F.C. Estimation of sodium availability in food in Slovenia: Results from household food purchase data from 2000 to 2009. Slov. J. Public Health 2014, 53, 209–219. Available online: https://www.degruyter.com/view/j/sjph.ahead-of-print/sjph-2014-0021/sjph-2014-0021.xml (accessed on 6 May 2017).
- World Health Organization. Global Action Plan for the Prevention and Control of Noncommunicable Diseases 2013–2020; WHO document Production Services: Geneva, Switzerland, 2013; pp. 1–91. Available online: http://apps.who.int/iris/bitstream/10665/94384/1/9789241506236_eng.pdf?ua=1 (accessed on 6 May 2017).
- Instituto Nacional de Estadistica y Censos. Encuesta Nacional de Ingresos y Gastos de los Hogares 2013: Principales Resultados; INEC: San José, Costa Rica, 2014; Available online: http://www.inec.go.cr/sites/default/files/documentos/pobreza_y_presupuesto_de_hogares/gastos_de_los_hogares/metodologias/documentos_metodologicos/mepobrezaenig2013-2014-01_1.pdf (accessed on 6 May 2017).
- Instituto Nacional de Estadística y Censos. Encuesta Nacional de Ingresos y Gastos 2004: Principales Resultados; INEC: San José, Costa Rica, 2006; p. 302. [Google Scholar]
- USDA Food Composition Databases 2015. Available online: https://ndb.nal.usda.gov/ndb/search/list (accessed on 6 May 2017).
- Alfaro, T.; Salas, M.T.; Ascencio, M. Tabla de Composición de Alimentos de Costa Rica: Alimentos Fortificados; Instituto Costarricense de Investigación y Enseñanza en Nutrición y Salud: Tres Ríos, Costa Rica, 2006; p. 20. Available online: https://www.inciensa.sa.cr/vigilancia_epidemiologica/informes_vigilancia/tablas%20composicion/Alimentos%20fortificados.pdf (accessed on 6 May 2017).
- Blanco-Metzler, A.; Montero-Campos, M.A.; Fernández-Piedra, M. Tabla de Composición de Alimentos de Costa Rica. Macronutrientes y Fibra Dietética; Instituto Costarricense de Investigación y Enseñanza en Nutrición y Salud: Tres Ríos, Costa Rica, 2006; pp. 22–39. Available online: http://www.inciensa.sa.cr/vigilancia_epidemiologica/informes_vigilancia/tablas%20composicion/Macronutrientes%20y%20fibra.pdf (accessed on 6 May 2017).
- ValorNut (1) (Software). Available online: http://nutricion2.ucr.ac.cr/valornut/ (accessed on 6 May 2017).
- Greenfield, H.; Southgate, D.A.T. Food Composition Data. Production, Management and Use, 2nd ed.; FAO: Rome, Italy, 2003; p. 225. Available online: http://www.fao.org/docrep/008/y4705e/y4705e00.htm (accessed on 17 May 2017).
- Monteiro, C.A.; Bertazzi, R.; Claro, R.M.; de Castro, I.R.; Cannon, G. Increasing consumption of ultra-processed foods and likely impact on human health: evidence from Brazil. Public Health Nutr. 2010, 14, 5–13. Available online: https://www.cambridge.org/core/services/aop-cambridge-core/content/view/C36BB4F83B90629DA15CB0A3CBEBF6FA/S1368980010003241a.pdf/increasing_consumption_of_ultraprocessed_foods_and_likely_impact_on_human_health_evidence_from_brazil.pdf (accessed on 6 May 2017).
- COMIECO. Reglamento Técnico Centroamericano. In RTCA 67.01.60:10 Etiquetado Nutricional de Productos Alimenticios Preenvasados Para Consumo Humano Para la Poblacion a Partir de 3 Años de Edad; Diario Oficial La Gaceta N°71; Imprenta Nacional: San José, Costa Rica, 2011; Available online: https://extranet.who.int/nutrition/gina/sites/default/files/COMIECO%202011%20Etiquetado%20Nutricional%20de%20Productos%20Alimenticios%20Preenvasados%20para%20Consumo%20Humano.pdf (accessed on 13 June 2017).
- Downey, N.M.; Heath, R.W. Métodos Estadísticos Aplicados, 3rd ed.; Harla S.A. de C.V.: México City, México, 1973. [Google Scholar]
- Costa Rica. Ministerio de Salud. Estrategia Nacional Abordaje Integral de las Enfermedades Crónicas No Transmisibles y Obesidad 2014–2021; El Ministerio: San José, Costa Rica, 2014; 100p. Available online: http://www.iccp portal.org/sites/default/files/plans/CRI_B3_COR_Libro_Estrategia_ECNT.pdf (accessed on 7 May 2017).
- Costa Rica. Ministerio de Salud. Encuesta Basal de Factores de Riesgo Para Enfermedades no Transmisibles. Cartago 2001. Módulo 1: Factores Alimentarios; Ministerio de Salud: San José, Costa Rica, 2003.
- Brenes, M.; Villalobos, D. Evaluación del Estado Nutricional de un Grupo de Funcionarios con Hipertensión Arterial Atendidos en la Oficina de Bienestar y Salud, Sede Universitaria Rodrigo Facio de la Universidad de Costa Rica, 2012. Bachelor’s Thesis, Universidad de Costa Rica, San Pedro, Costa Rica, 2013. [Google Scholar]
- Instituto Nacional de Estadistica y Censos. Costo de la Canasta Basica Alimentaria, enero 2011. In Boletín Mensual Nueva Canasta Basica Alimentaria; INEC: San Jose, Costa Rica, 2011; p. 9. Available online: www.inec.go.cr/sites/default/files/documentos/economia/costo_canasta_basica_alimentaria/publicaciones/reeconomcba012011-01.pdf (accessed on 20 May 2017).
- De Mestral, C.; Mayén, A.L.; Petrovic, D.; Marques-Vidal, P.; Bochud, M.; Stringhini, S. Socioeconomic Determinants of Sodium Intake in Adult Populations of High-Income Countries: A Systematic Review and Meta-Analysis. Am. J. Public Health 2017, 107, 563. Available online: https://www.ncbi.nlm.nih.gov/pubmed/28272962 (accessed on 15 June 2017). [PubMed]
- Pan American Health Organization (PAHO). Salt Smart Americas: Guide for Country-Level Action; PAHO: Washington DC, USA, 2013; pp. 91–104. Available online: http://www2.paho.org/hq/index.php?option=com_content&view=article&id=8677%3A2013-technical-document-salt-smart-americas&catid=5387%3Asalt-reduction-media-center&Itemid=40601 (accessed on 3 May 2017).
- Holden, J.M.; Pehrsson, P.R.; Nickle, M.; Haytowitz, D.B.; Exler, J.; Showell, B.; Williams, J.; Thomas, R.G.; Ahuja, J.K.C.; Patterson, K.Y.; et al. USDA monitors levels of added sodium in commercial packaged and restaurant foods. Procedia Food Sci. 2013, 2, 60–67. Available online: http://ac.els-cdn.com/S2211601X13000114/1-s2.0-S2211601X13000114-main.pdf?_tid=57a8dd34-520d-11e7-ba88-00000aacb35d&acdnat=1497560471_7749e969b438c7a977b5ebad16c598c4 (accessed on 15 June 2017).
- Pan American Health Organization. Ultra-Processed Food and Drink Products in Latin America: Trends, Impact on Obesity, Policy Implications; PAHO: Washington DC, USA, 2015; Available online: http://iris.paho.org/xmlui/bitstream/handle/123456789/7699/9789275118641_eng.pdf?sequence=5&isAllowed=y (accessed on 14 May 2017).
- Reforma Norma Oficial para la Sal de Calidad Alimentaria, N° 30032-S. Diario Oficial La Gaceta N° 247. Alcance N 88-A a. Imprenta Nacional, San José, Costa Rica; 2001. Available online: http://www.pgrweb.go.cr/scij/Busqueda/Normativa/Normas/nrm_texto_completo.aspx?param1=NRTC&nValor1=1&nValor2=47668&nValor3=88169¶m2=1&strTipM=TC&lResultado=2&strSim=simp (accessed on 14 May 2017).
- Pan American Health Organization (PAHO). SaltSmart Consortiumn Consensus Statement to Advance Target Harmonization by Agreeing on Regional Targets for the Salt/Sodium Content of Key Food Categories. 2015. Available online: http://www2.paho.org/hq/index.php?option=com_docman&task=doc_download&gid=28929&Itemid=270&lang=en (accessed on 14 May 2017).
- Costa Rica. Ministerio de Salud. Plan Nacional Para la Reducción del Consumo de Sal/Sodio en la Población de Costa Rica, 2011–2021; El Ministerio: San José, Costa Rica, 2011; pp. 3–20. Available online: https://www.ministeriodesalud.go.cr/index.php/biblioteca-de-archivos/sobre-el-ministerio/politcas-y-planes-en-salud/planes-en-salud/1103-plan-nacional-para-la-reduccion-del-consumo-de-sal-sodio-en-la-poblacion-de-costa-rica-2011-2021/file (accessed on 14 May 2017).
| Zone | n | Energy (kcal/Person/Day) | Sodium (g/Person/Day) | Sodium (g/Person/Day/2000 kcal) | ||||
|---|---|---|---|---|---|---|---|---|
| 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | |
| Costa Rica | 1,134,433 | 1,396,747 | 2315 | 2390 | 3.9 | 4.6 a | 3.4 | 3.8 a |
| Urban | 705,111 | 1,023,061 | 2263 | 2344 | 3.6 | 4.4 a,b | 3.2 | 3.8 a,b |
| Rural | 429,322 | 373,686 | 2400 | 2531 | 4.5 | 5.2 a,b | 3.8 | 4.1 a,b |
| Quintile | n | Energy (kcal/Person/Day) | Sodium (g/Person/Day) | Sodium (g/Person/Day/2000kcal) | ||||
|---|---|---|---|---|---|---|---|---|
| 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | 2004–2005 | 2012–2013 | |
| Costa Rica | 1,134,433 | 1,396,747 | 2315 | 2390 | 3.9 | 4,6 a | 3.4 | 3.9 a |
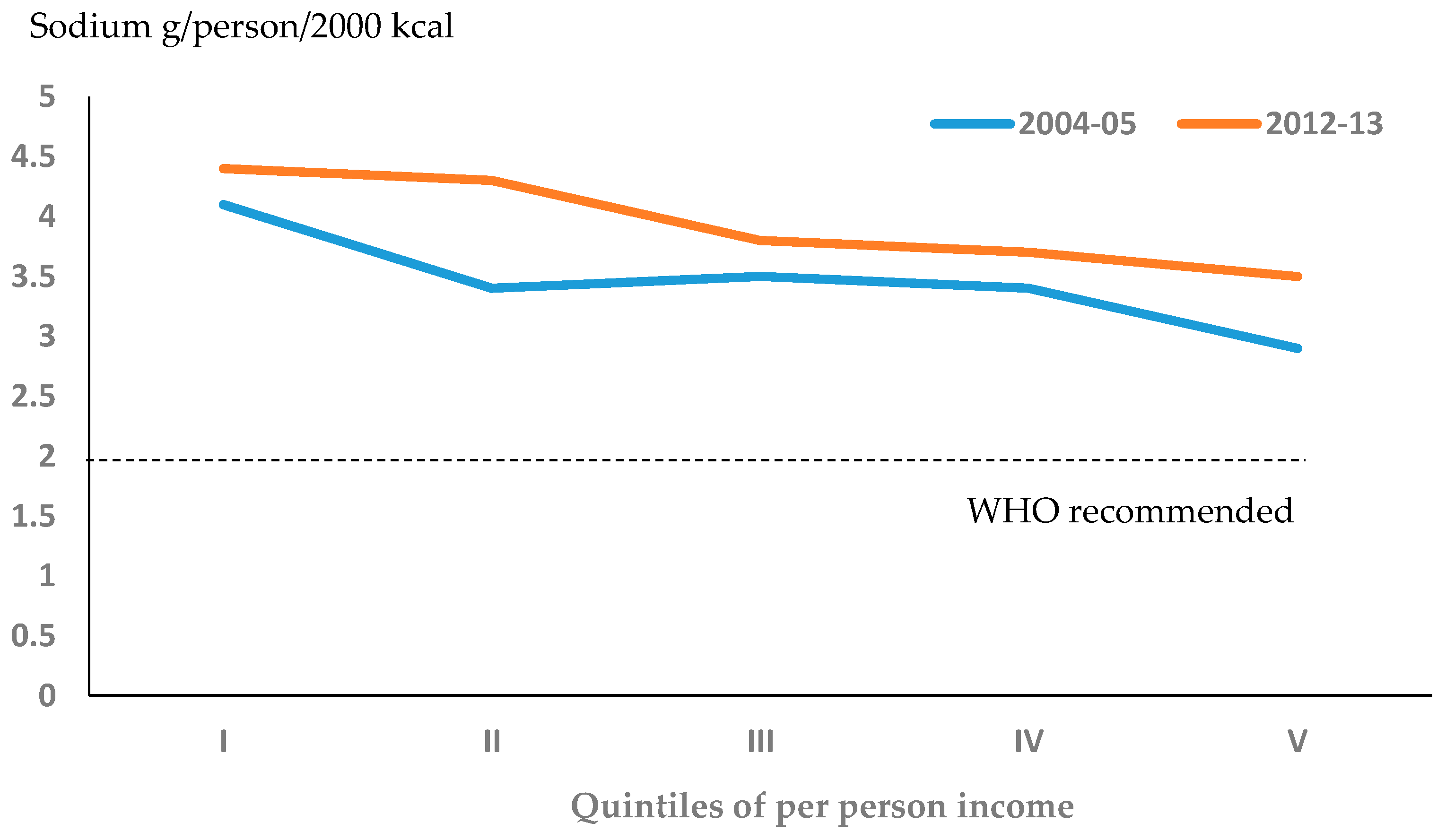
| I | 225,773 | 279,044 | 1896 | 1724 | 3.9 | 3,8 b | 4.1 | 4.4 b |
| II | 226,647 | 279,642 | 2065 | 2195 | 3.5 | 4.7 a | 3.4 | 4.3 a |
| III | 228,332 | 279,437 | 2276 | 2494 | 4.0 | 4.7 | 3.5 | 3.8 |
| IV | 226,503 | 279,409 | 2626 | 2679 | 4.4 | 4.9 a | 3.4 | 3.7 a |
| V | 227,178 | 279,215 | 2712 | 2669 | 3.9 | 4.7 a | 2.9 | 3.5 a |
| 2012–2013 | ||||||||
| Food Group | n | Costa Rica | Quintiles of Per Capita Income Distribution | |||||
| g/Person/Day | % | I | II | III | IV | V | ||
| Common salt (table or kitchen) | 1,396,747 | 2.78 | 60.2 | 72.4 b | 66.3 b | 61.6 b | 58.2 b | 45.2 b |
| Processed foods | 1,396,747 | 0.65 a | 14.2 a | 10.1 b | 10.9 b | 14.1 b | 15.8 b | 19.4 b |
| Sodium-based condiments | 1,396,747 | 0.61 a | 13.2 a | 11.8 b | 15.0 b | 13.1 b | 11.8 b | 14.0 b |
| Ready to eat meals | 1,396,747 | 0.33 a | 7.2 a | 2.4 b | 3.8 b | 6.1 b | 8.7 b | 14.3 b |
| In natura foods | 1,396,747 | 0.24 | 5.1 | 3.4 b | 4.0 b | 5.2 b | 5.5 b | 7.3 b |
| Total | 1,396,747 | 4.61 | 100 | 100 | 100 | 100 | 100 | 100 |
| 2004–2005 | ||||||||
| Food Group | n | Costa Rica | Quintiles of Per Capita Income Distribution | |||||
| g/person/day | % | I | II | III | IV | V | ||
| Common salt (table or kitchen) | 1,134,433 | 2.37 | 60.2 | 77.2 | 66.3 | 62.4 | 54.7 | 41.2 |
| Processed foods | 1,134,433 | 0.61 | 15.4 | 8.1 | 13.9 | 15.3 | 17.1 | 22.5 |
| Sodium-based condiments | 1,134,433 | 0.36 | 9.3 | 6.4 | 7.7 | 9.3 | 11.7 | 10.8 |
| Ready to eat meals | 1,134,433 | 0.38 | 9.8 | 5.1 | 7.6 | 8.0 | 10.7 | 17.2 |
| In natura foods | 1,134,433 | 0.21 | 5.4 | 3.2 | 4.6 | 4.9 | 5.8 | 8.3 |
| Total | 1,134,433 | 3.94 | 100 | 100 | 100 | 100 | 100 | 100 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Blanco-Metzler, A.; Moreira Claro, R.; Heredia-Blonval, K.; Caravaca Rodríguez, I.; Montero-Campos, M.D.l.A.; Legetic, B.; L’Abbe, M.R. Baseline and Estimated Trends of Sodium Availability and Food Sources in the Costa Rican Population during 2004–2005 and 2012–2013. Nutrients 2017, 9, 1020. https://doi.org/10.3390/nu9091020
Blanco-Metzler A, Moreira Claro R, Heredia-Blonval K, Caravaca Rodríguez I, Montero-Campos MDlA, Legetic B, L’Abbe MR. Baseline and Estimated Trends of Sodium Availability and Food Sources in the Costa Rican Population during 2004–2005 and 2012–2013. Nutrients. 2017; 9(9):1020. https://doi.org/10.3390/nu9091020
Chicago/Turabian StyleBlanco-Metzler, Adriana, Rafael Moreira Claro, Katrina Heredia-Blonval, Ivannia Caravaca Rodríguez, María De los A. Montero-Campos, Branka Legetic, and Mary R. L’Abbe. 2017. "Baseline and Estimated Trends of Sodium Availability and Food Sources in the Costa Rican Population during 2004–2005 and 2012–2013" Nutrients 9, no. 9: 1020. https://doi.org/10.3390/nu9091020
APA StyleBlanco-Metzler, A., Moreira Claro, R., Heredia-Blonval, K., Caravaca Rodríguez, I., Montero-Campos, M. D. l. A., Legetic, B., & L’Abbe, M. R. (2017). Baseline and Estimated Trends of Sodium Availability and Food Sources in the Costa Rican Population during 2004–2005 and 2012–2013. Nutrients, 9(9), 1020. https://doi.org/10.3390/nu9091020







