Pertussis: A Review of Disease Epidemiology Worldwide and in Italy
Abstract
:1. Introduction
2. Worldwide Epidemiology

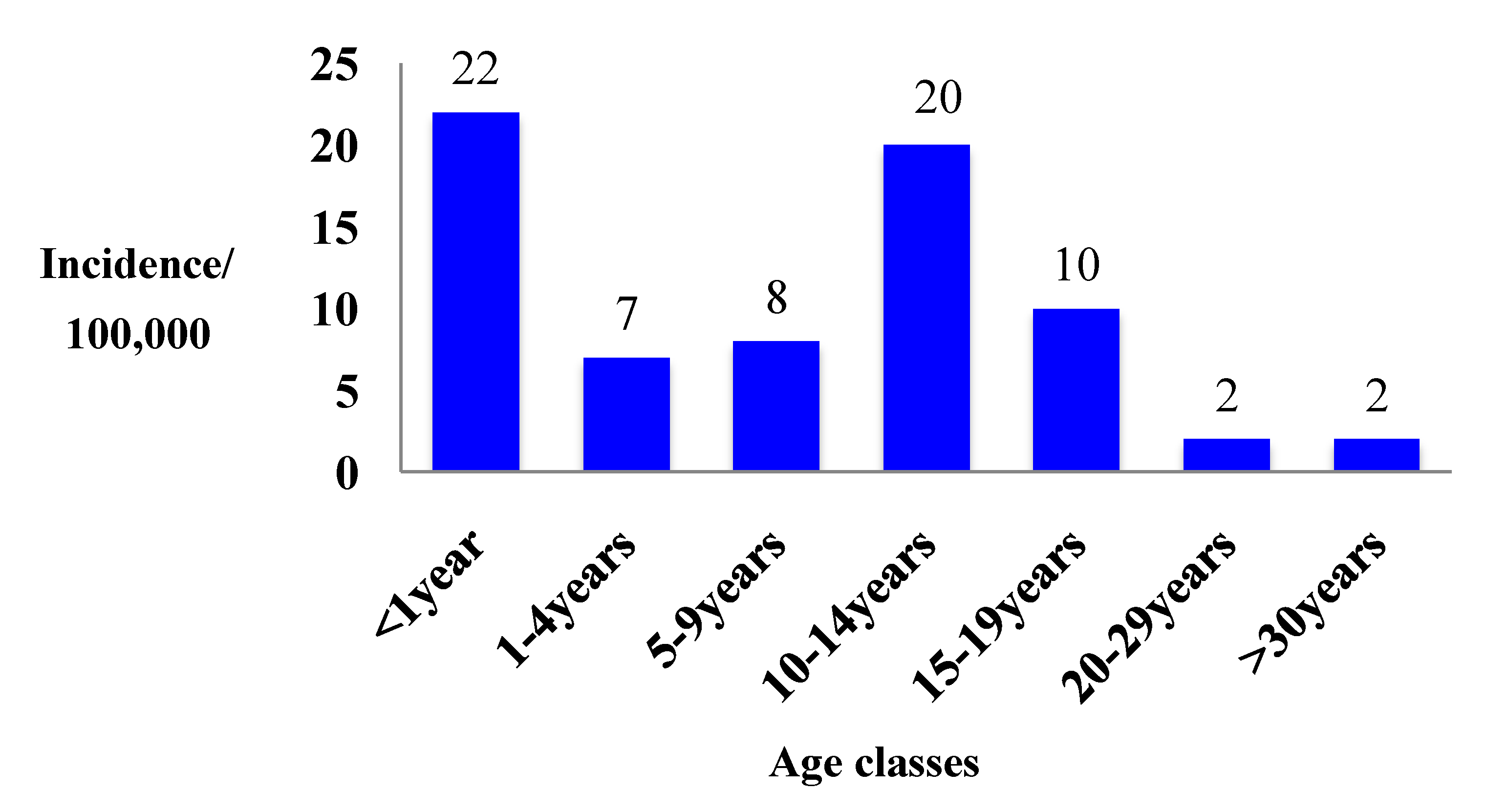
3. Epidemiology in Italy


4. Conclusions
- According to seroepidemiological studies, pertussis is a widespread, even if not adequately measurable, infectious disease.
- Pertussis continues to be a public-health issue even in countries with high immunization coverage.
- Immune protection, both natural and vaccine-induced, is not long lasting.
- Adolescents and adults may become a significant source of infection for unvaccinated or partially immunized newborns.
- The clinical features of pertussis in adolescents and adults make difficult the diagnosis, which should be based also on lab assessment.
- Passive surveillance, based on notification, is not a reliable system for the evaluation of pertussis’ incidence and an adequate surveillance should be adopted to evaluate both the burden of infection and the impact of immunization.
- The paradigm to evaluate before and after the preventive intervention is hardly applicable to pertussis.
Conflict of Interest
References
- Anderson, R.M.; May, R.M. Immunisation and herd immunity. Lancet 1990, 335, 641–645. [Google Scholar] [CrossRef]
- Anderson, R.M.; May, R.M. Infectious Diseases of Humans. Dynamics and Control, 1st ed; Oxford University Press: Oxford, UK, 1991. [Google Scholar]
- Kretzschmar, M.; Teunis, P.F.M.; Pebody, R.G. Incidence and reproductive numbers of pertussis: Estimates from serological and social contact data in five European countries. PLoS Med. 2012, 7, e1000291. [Google Scholar] [CrossRef]
- Blangiardi, F.; Ferrera, G. Reducing the risk of pertussis in newborn infants. JPMH 2009, 50, 206–216. [Google Scholar]
- Yaari, E.; Yafe-Zimerman, Y.; Schwartz, S.B.; Slater, P.E.; Shvarztman, P.; Andoren, N.; Branski, D.; Kerem, E. Clinical manifestations of Bordetella pertussis infection in immunized children and young adults. Chest 1999, 115, 1254–1258. [Google Scholar] [CrossRef]
- Cherry, J.D. Editorial commentary. Immunity to Pertussis. Clin. Infect. Dis. 2007, 44, 1278–1279. [Google Scholar] [CrossRef]
- de Greeff, S.C.; de Melker, H.E.; van Gageldonk, P.G.M.; Schellekens, J.F.P.; van der Klis, F.R.M.; Mollema, L.; Mooi, F.R.; Berbers, G.A.M. Seroprevalence of pertussis in the Netherlands: Evidence for increased circulation of Bordetella pertussis. PLoS ONE 2012, 5, e14183. [Google Scholar] [CrossRef]
- Tan, T.; Trindale, E.; Skowronski, D. Epidemiology of pertussis. Pediatr. Infect. Dis. J. 2005, 24, S10–S18. [Google Scholar]
- Lavine, J.; Brouitin, H.; Harvill, E.T.; Bjornstad, O.N. Imperfect vaccine-induced immunity and whooping cough transmission to infants. Vaccine 2011, 29, 11–16. [Google Scholar] [CrossRef] [Green Version]
- Heininger, U. Pertussis: What the pediatric infectious disease specialist should know. Pediatr. Infect. Dis. J. 2012, 31, 78–79. [Google Scholar]
- WHO. Pertussis vaccines: WHO position paper. Wkly. Epidemiol. Rec. 2010, 85, 385–400.
- Mills, K.H.G. Immunity to Bordetella pertussis. Microbes Infect. 2001, 3, 655–677. [Google Scholar] [CrossRef]
- Cherry, J.D. Epidemic pertussis in 2012—The resurgence of a vaccine-preventable disease. NEJM 2012, 367, 785–787. [Google Scholar] [CrossRef]
- Klein, N.P.; Bartlett, J.; Rowhani-Rahbar, A.; Fireman, B.; Baxter, R. Waning protection after fifth dose of acellular pertussis vaccine in children. NEJM 2012, 367, 1012–1019. [Google Scholar] [CrossRef]
- Witt, M.A.; Katz, P.H.; Witt, D.J. Unexpectedly limited durability of immunity following acellular pertussis vaccination in preadolescents in a North American outbreak. Clin. Infect. Dis. 2012, 54, 1730–1735. [Google Scholar] [CrossRef]
- CDC. Pertussis. Surveillance and Reporting. Trends. Available online: www.cdc.gov/pertussis/surv-reporting.html (accessed on 31 July 2011).
- CDC. Notes from the field: Pertussis—California, January–June 2010. MMWR Weekly 2010, 59, 817.
- CDPH. Pertussis report. 9 March 2011. Available online: www.cdph.ca.gov/Healthinfo/discond/Pages/Pertussis.aspx (accessed on 31 July 2011).
- CDC. Pertussis epidemic—Washington, 2012. MMWR Weekly 2012, 61, 517–522.
- Wendelboe, A.M.; Hudgens, M.G.; Poole, C.; Van Rie, A. Estimating the role of casual contact from the community in transmission of Bordetella pertussis to young infants. Emerg. Themes Epidemiol. 2007, 4, 15. [Google Scholar] [CrossRef]
- Jardine, A.; Conaty, S.J.; Lowbridge, C.; Staff, M.; Vally, H. Who gives pertussis to infants? Source of infection for laboratory confirmed cases less than 12 months of age during an epidemic, Sydney, 2009. Commun. Dis. Intell. 2010, 34, 116–121. [Google Scholar]
- Baptista, P.N.; Magalhaes, V.S.; Rodrigues, L.C. The role of adults in household outbreaks of pertussis. Int. J. Infect. Dis. 2010, 14, 111–114. [Google Scholar]
- EUVAC.NET. Pertussis surveillance report 2003–2007. Available online: www.euvac.net/graphics/euvac/pdf/pertussis2.pdf (accessed on 30 September 2011).
- Lutsar, I.; Anca, I.; Bakir, M.; Usonis, V.; Prymula, R.; Salman, N.; Grezesiowski, P.; Greenberg, M. Central European vaccination Advisory Group. Eur. J. Pediatr. 2009, 168, 407–415. [Google Scholar] [CrossRef]
- EUVAC.NET. Pertussis Surveillance Report 2009. Available online: www.euvac.net/graphics/euvac/pdf/pertussis_2009.pdf (accessed on 30 September 2011).
- Giammanco, A.; Chiarini, A.; Maple, P.A.C.; Andrews, N.; Pebody, R.; Gay, N.; Olander, R.M.; Fivet-Groyne, F.; Baron, S.; Tischer, A.; Swidsinski, S.; Schellekens, J.; Reizenstein, E. European Sero-epidemiology Network: Standardisation of the assay results for pertussis. Vaccine 2003, 22, 112–120. [Google Scholar] [CrossRef]
- De Melker, H.E.; Versteegh, F.G.; Conyn-Van Spaendonck, M.A.; Elvers, L.H.; Berbers, G.A.; van der Zee, A.; Schellekens, J.F. Specificity and sensitivity of high levels of immunoglobulin G antibodies against pertussis toxin in a single serum sample for diagnosis of infection with Bordetella pertussis. J. Clin. Microbiol. 2000, 38, 800–806. [Google Scholar]
- Binkin, N.J.; Salmaso, S.; Tozzi, A.E.; Scuderi, G.; Greco, D.; Greco, D. Epidemiology of pertussis in a developed country with low vaccination coverage: The Italian experience. Pediatr. Infect. Dis. J. 1992, 11, 653–656. [Google Scholar]
- Indagine 2008: Indagine di copertura vaccinale nazionale nei bambini e negli adolescenti. Rapporti ISTISAN 2009, 9, 29.
- Ministero della Sanità. Decreto Ministeriale 15 dicembre 1990. Sistema di sorveglianza sulle malattie infettive. Gazzetta Ufficiale 1991, 6, 8–18.
- ISS: Pertosse. Aspetti Epidemiologici. Available online: www.epicentro.iss.it/problemi/pertosse/epid.asp (accessed on 31 July 2011).
- Rota, M.C.; D’Ancona, F.; Massari, M.; Mandolini, D.; Giammanco, A.; Carbonari, P.; Salmaso, S.; Ciofi degli Atti, M.L. The serological study Group. How increased pertussis vaccination coverage is changing the epidemiology of pertussis in Italy. Vaccine 2005, 23, 5299–5305. [Google Scholar]
- Brooks, D.A.; Clover, R.C. Pertussis infection in the United States: Vaccination of adolescents and adults. J. Am. Board Fam. Med. 2006, 19, 603–611. [Google Scholar]
- Trollfors, B.; Dotevall, L.; Sundh, V.; Welinder-Olsson, C. Pertussis after end of a mass vaccination project—End of the “vaccination honey-moon”. Vaccine 2011, 29, 2444–2450. [Google Scholar]
- Elomaa, A.; He, Q.; Tran Minh, N.N.; Mertsola, J. Pertussis before and after the introduction of acellular pertussis vaccines in Finland. Vaccine 2009, 27, 5443–5449. [Google Scholar] [CrossRef]
- Gabutti, G.; Bergamini, M.; Bonanni, P.; Guido, M.; Fenoglio, D.; Giammanco, A.; Sindoni, L.; Zotti, C.; Boddi, V.; Bamfi, F.; Severini, R.; Bechini, A.; Boccalini, S.; Crovari, P. The Collaborative Group for the study of pertussis. Assessment of humoral and cell-mediated immunty against Bordetella pertussis in adolescent, adult and senior subjects in Italy. Epidemiol. Infect. 2008, 136, 1576–1584. [Google Scholar] [CrossRef]
- Marocco, A.; Assael, B.; Gabutti, G.; Guarino, A.; Lopalco, P.L.; Marchetti, F.; Ruggeri, F.M.; Titone, L.; Tozzi, A.E.; Vitali Rosati, G.; Zotti, C.; Franco, E. Hospitalisation associated with Rotavirus gastroenteritis in Italy, 2001–2003, evaluated by means of ICD9-CM diagnostic codes. Ig. Sanita Pubbl. 2006, 62, 215–244. [Google Scholar]
- Forsyth, K.D.; Wirsing von Konig, C.H.; Tan, T.; Caro, J.; Plotkin, S. Prevention of pertussis: Recommendations derived from the second Global Pertussis Iniatiative roundtable meeting. Vaccine 2007, 25, 2634–2642. [Google Scholar]
- Guiso, N. Bordetella pertussis and pertussis vaccines. Clin. Infect. Dis. 2009, 49, 1565–1569. [Google Scholar] [CrossRef]
- Cherry, J.D.; Grimpel, E.; Guiso, N.; Heininger, U.; Mertsola, J. Defining pertussis epidemiology. Clinical, microbiologic and serologic perspectives. Pediatr. Infect. Dis. J. 2005, 24, S25–S34. [Google Scholar] [CrossRef]
- Tozzi, A.E.; Pastore Celentano, L.; Ciofi degli Atti, M.L.; Salmaso, S. Diagnosis and management of pertussis. CMAJ 2005, 172, 509–515. [Google Scholar]
- Rendi-Wagner, P.; Tobias, J.; Moerman, L.; Goren, S.; Bassal, R.; Green, M.; Cohen, D. The seroepidemiology of Bordetella pertussis in Israel—Estimate of incidence of infection. Vaccine 2010, 28, 3285–3290. [Google Scholar] [CrossRef]
- Liu, B.C.; McIntyre, P.; Kaldor, J.M.; Quinn, H.; Ridda, I.; Banks, E. Pertussis in older adults: Prospective study of risk factors and morbidity. Clin. Infect. Dis. 2012, 55, 1450–1456. [Google Scholar]
- Ridda, I.; Yin, J.K.; King, C.; Raina MacIntyre, C.; McIntyre, P. The importance of pertussis in older adults: A growing case for reviewing vaccination strategy in the elderly. Vaccine 2012, 30, 6745–6752. [Google Scholar]
- CDC. Updated recommendations for use of tetanus toxoid, reduced diphtheria toxoid and acellular pertussis (Tdap) vaccine from the Advisory Committee on immunization practices, 2010. MMWR Weekly 2011, 60, 13–15.
- WHO. Conference report. Pertussis vaccines: WHO position paper—Recommendations. Vaccine 2011, 29, 2355–2356. [CrossRef]
- Wei, S.C.; Tatti, K.; Cushing, K.; Rosen, J.; Brown, K.; Cassiday, P.; Clark, T.; Olans, R.; Pawloski, L.; Martin, M.; Tondella, M.L.; Martin, S.C. Effectiveness of adolescent and adult tetanus, reduced-dose diphtheria and acellular pertussis vaccine against pertussis. Clin. Infect. Dis. 2010, 51, 315–321. [Google Scholar]
- Mertsola, J.; van der Meeren, O.; He, Q.; Linko-Parvinen, A.; Ramakrishnan, G.; Mannermaa, L.; Solia, M.; Pulkkinen, M.; Jacquet, L.M. Decennial administration of a reduce antigen content diphtheria and tetanus toxoids and acellular pertussis vaccine in young adults. Clin. Infect. Dis. 2010, 51, 656–662. [Google Scholar] [CrossRef]
- Proposta di Calendario Vaccinale per l’infanzia e l’adolescenza, a Cura di SItI, FIMP, SIP, Versione Finale Approvata l’8 Luglio 2010. Available online: www.societaitalianaigiene.org/cms/images/docs/calendariovaccinale/infanzia.pdf (accessed on 31 July 2011).
- Proposta di Calendario Vaccinale per gli Adulti e per Gli Anziani, Maggio 2011. Available online: www.societaitalianaigiene.org/cms/images/docs/calendariovaccinale/2011/adulti.pdf (accessed 31 July 2011).
- Coudeville, L.; van Rie, A.; Andre, P. Adult pertussis vaccination strategies and their impact on pertussis in the United States: Evaluation of routine and targeted (cocoon) strategies. Epidemiol. Infect. 2008, 136, 604–620. [Google Scholar]
- Coudeville, L.; van Rie, A.; Getsios, D.; Caro, J.; Crépey, P.; van Hung, N. Adult vaccination strategies for the control of pertussis in the United States: An economic evaluation including the dynamic population effects. PLoS ONE 2009, 4, e6284. [Google Scholar] [CrossRef]
- Wiese-Posselt, M.; Hellenbrand, W. Changes to the varicella and pertussis immunisation schedule in Germany 2009: Background, rationale and implementation. Euro. Surveill. 2010, 15, 19548. [Google Scholar]
- Prato, R.; Martinelli, D.; Marchetti, F.; Fortunato, F.; Tafuri, S.; Germinario, C.A. Feasibility of a cocoon strategy for prevention of pertussis in Italy: A survey of Prevention Department Healthcare Providers. PIDJ 2012, 31, 1304–1307. [Google Scholar]
- Bechini, A.; Tiscione, E.; Boccalini, S.; Levi, M.; Bonanni, P. Acellular pertussis vaccine use in risk groups (adolescents, pregnant women, newborns and health care workers): A review of evidences and recommendations. Vaccine 2012, 35, 5179–5190. [Google Scholar]
- Skowronski, D.M.; Janjua, N.Z.; Tsafack, E.P.; Ouakki, M.; Hoang, L.; de Serres, G. The number needed to vaccinate to prevent infant pertussis hospitalization and death through parent cocoon immunization. Clin. Infect. Dis. 2012, 54, 318–327. [Google Scholar] [CrossRef]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Gabutti, G.; Rota, M.C. Pertussis: A Review of Disease Epidemiology Worldwide and in Italy. Int. J. Environ. Res. Public Health 2012, 9, 4626-4638. https://doi.org/10.3390/ijerph9124626
Gabutti G, Rota MC. Pertussis: A Review of Disease Epidemiology Worldwide and in Italy. International Journal of Environmental Research and Public Health. 2012; 9(12):4626-4638. https://doi.org/10.3390/ijerph9124626
Chicago/Turabian StyleGabutti, Giovanni, and Maria Cristina Rota. 2012. "Pertussis: A Review of Disease Epidemiology Worldwide and in Italy" International Journal of Environmental Research and Public Health 9, no. 12: 4626-4638. https://doi.org/10.3390/ijerph9124626



