Prevalence of Children with Severe Fetal Alcohol Spectrum Disorders in Communities Near Rome, Italy: New Estimated Rates Are Higher than Previous Estimates
Abstract
:Objective:
Methods:
Results:
Conclusions:
1. Introduction
2. Methods
2.1. Institute of Medicine (IOM) Diagnostic Categories of FASD
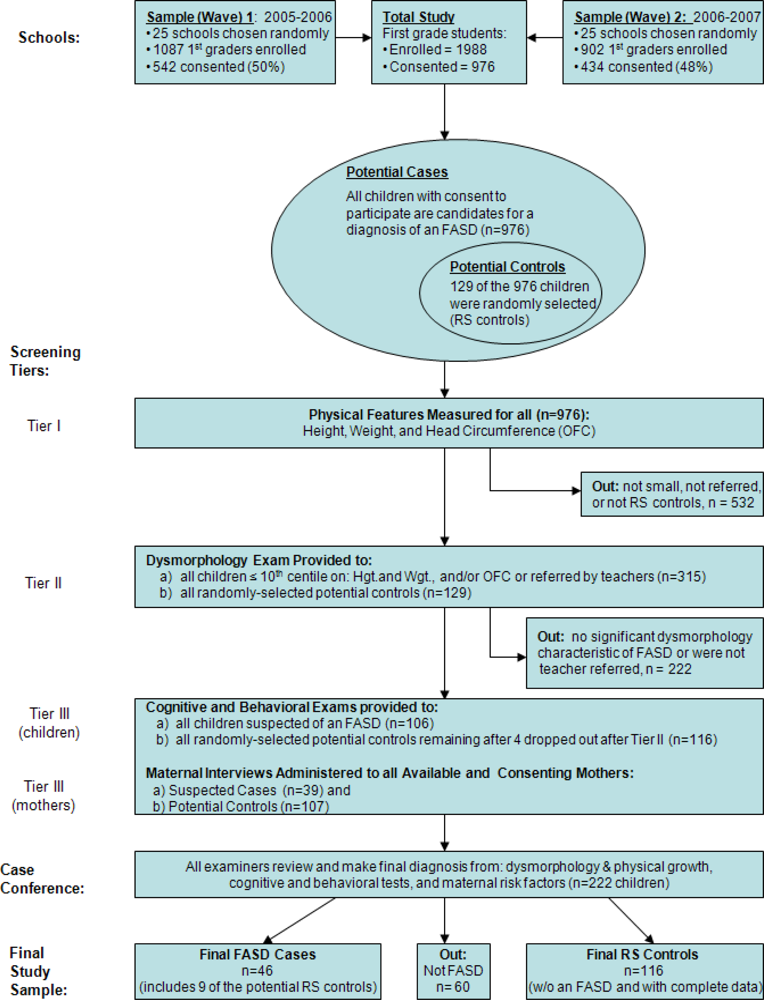
2.2. Overall Study Design and Sampling
2.3. The Two-Tiered System of Entry and Diagnosis Employed in the Study
2.4. Developmental (IQ, Cognitive and Behavioral) Testing for FASD Suspects and Controls
2.5. Maternal Interviews for Mothers of FASD Suspects and Controls
2.6. Statistical Analysis
3. Results
3.1. Demographic and Child Physical Traits
3.2. Neurodevelopmental Traits of Children
3.3. Maternal Traits
3.4. Correlation Analyses
3.5. Final Diagnosis Summary
FAS
PFAS
3.6. Prevalence Findings
4. Discussion
4.1. Prevalence Findings
4.2. Implications
4.3. Limitations
5. Conclusions
Acknowledgments
References
- Scianaro, L; Prusek, W; Loiodice, G. The fetal alcohol syndrome: Clinical observations. Minerva Pediatr 1978, 30, 1585–1588. [Google Scholar]
- Moretti, M; Montali, S. Fetal defects caused by the passive consumption of drugs. Pediatr. Med. Chir 1982, 4, 481–490. [Google Scholar]
- Calvani, M; Ghirelli, D; Calvani, M; Fortuna, C; Lalli, F; Marcolini, P. Fetal alcohol syndrome: Clinical, metabolic and immunologic follow-up in l4 cases. Minerva Pediatr 1985, 37, 77–88. [Google Scholar]
- Scotto, DT; Venturino, G; Sorrentino, I; Infuso, D; D’Amiano, G; Palmieri, G. Fetal alcoholic syndrome: A clinical case. Pediatr. Med. Chir 1993, 15, 525–529. [Google Scholar]
- Roccella, M; Testa, D. Fetal alcohol syndrome in developmental age. Neuropsychiatric aspects. Minerva Pediatr 2003, 55, 63–74. [Google Scholar]
- De Nigris, C; Awabdeh, F; Tomassini, A; Remotti, G. Alcool e gravidanza incidenza del fenomeno ed effetti sul neonato nella popolazione utente di un ospedale di Varese. Ann. Ostet. Ginecol. Med. Perinat 1981, 102, 419–430. [Google Scholar]
- Parazzini, F; Tozzi, L; Chatenoud, L; Restelli, S; Luchini, L; La Vecchia, C. Alcohol and risk of spontaneous abortion. Human Repr 1994, 9, 1950–1953. [Google Scholar]
- Parazzini, F; Chatenoud, L; Benzi, G; Di Cintio, E; Dal Pino, D; Tozzi, L; Fedele, L. Coffee and alcohol intake, smoking and risk of multiples pregnancy. Human Repr 1996, 11, 2306–2309. [Google Scholar]
- Primatesta, P; Del Corno, G; Bonazzi, MC; Waters, WE. Alcohol and pregnancy: an international comparison. J. Public Health Med 1993, 15, 69–76. [Google Scholar]
- Lazzaroni, F; Bonassi, S; Magnani, M; Calvi, A; Repetto, E; Serra, F; Podesta, F; Pearce, N. Moderate maternal drinking and outcome of pregnancy. Eur. J. Epidemiol 1993, 9, 599–606. [Google Scholar]
- Bonati, M; Fellin, G. Changes in smoking and drinking behaviour before and during pregnancy in Italian mothers: Implications for public health intervention. Int. J. Epidemiol 1991, 20, 927–932. [Google Scholar]
- Astley, SJ. Fetal alcohol syndrome prevention in Washington State: Evidence of success. Paediatr. Perinat. Epidemiol 2004, 18, 344–351. [Google Scholar]
- Sampson, PD; Streissguth, AP; Bookstein, FL; Little, RE; Clarren, SK; Dehaene, P; Hanson, JW; Graham, JM, Jr. Incidence of fetal alcohol syndrome and prevalence of alcohol-related neurodevelopmental disorder. Teratology 1997, 56, 317–326. [Google Scholar]
- Chavez, GF; Corderro, JF; Becerra, JE. Leading major congenital malformations among minority groups in the United States, 1981–1986. MMWR 1988, 37, 17–24. [Google Scholar]
- Egeland, GM; Perham-Hester, KA; Hook, EB. Use of capture-recapture analyses in fetal alcohol syndrome surveillance in Alaska. Am. J. Epidemiol 1995, 141, 335–341. [Google Scholar]
- Egeland, GM; Perham-Hester, KA; Gessner, BD; Ingle, D; Berner, JE; Middaugh, JP. Fetal alcohol syndrome in Alaska, 1977 through 1992: an administrative prevalence derived from multiple data sources. Am. J. Public Health 1998, 88, 781–786. [Google Scholar]
- Leversha, AM; Marks, RE. The prevalence of fetal alcohol syndrome in New Zealand. N Z Med. J 1995, 108, 502–505. [Google Scholar]
- May, PA; Gossage, JP; Kalberg, WO; Robinson, LK; Buckley, DG; Manning, M; Hoyme, HE. The Prevalence and Epidemiologic Characteristics of FASD from Various Research Methods with an Emphasis on In-School Studies. Dev. Disabil. Res. Rev 2009, 15, 176–192. [Google Scholar]
- Little, BB; Snell, LM; Rosenfeld, CR; Gilstrap, LC; Gant, NF. Failure to recognize fetal alcohol syndrome in newborn infants. AJDC 1990, 144, 1142–1146. [Google Scholar]
- Stratton, K; Howe, C; Battaglia, F. Fetal Alcohol Syndrome: Diagnosis, Epidemiology, Prevention, and Treatment; National Academy Press: Washington, DC, USA, 1996. [Google Scholar]
- Clarren, SK; Randels, SP; Sanderson, M; Fineman, RM. Screening for fetal alcohol syndrome in primary schools: a feasibility study. Teratology 2001, 63, 3–10. [Google Scholar]
- Abel, EL; Sokol, RJ. Incidence of fetal alcohol syndrome and economic impact of FAS-related anomalies. Drug Alcohol Depend 1987, 19, 51–70. [Google Scholar]
- Abel, EL; Sokol, RJ. A revised conservative estimate of the incidence of FAS and its economic impact. Alcohol. Clin. Exp. Res 1991, 15, 514–524. [Google Scholar]
- Abel, EL. Fetal Alcohol Abuse Syndrome: from Mechanisms to Prevention; CRC Press: Boca Raton, FL, USA, 1996. [Google Scholar]
- Abel, EL. An update on incidence of FAS: FAS is not an equal opportunity birth defect. Neurotoxicol. Teratol 1995, 17, 437–443. [Google Scholar]
- May, PA; Gossage, JP. The Prevalence of Fetal Alcohol Syndrome within Three New Mexico Ethnic Communities; The University of New Mexico, Center on Alcoholism, Substance Abuse, and Addictions: Albuquerque, NM, USA, 2002. [Google Scholar]
- May, PA; Hymbaugh, KJ. A pilot project on fetal alcohol syndrome among American Indians. Alcohol Health Res. World 1982, 7, 3–9. [Google Scholar]
- May, PA; Hymbaugh, KJ; Aase, JM; Samet, JM. Epidemiology of fetal alcohol syndrome among American Indians of the Southwest. Soc. Biol 1983, 30, 374–387. [Google Scholar]
- Quaid, J; Kirkpatrick, J; Nakamura, R; Aase, JM. Establishing the occurrence of FAS/FAE in a rural community. Provider 1993, 18, 71–75. [Google Scholar]
- Duimstra, C; Johnson, D; Kutsch, C; Wang, B; Zentner, M; Kellerman, S; Welty, TA. Fetal alcohol syndrome surveillance pilot project in American Indian communities in the Northern Plains. Public Health Rep 1993, 108, 225–229. [Google Scholar]
- May, PA; McCloskey, J; Gossage, JP. Fetal Alcohol Syndrome Among American Indians: Epidemiology, Issues, and Research. In Alcohol Use Among American Indians: Multiple Perspectives on a Complex Problem; Mail, PD, Heurtin-Roberts, S, Martin, SE, Howard, J, Eds.; National Institute on Alcohol Abuse and Alcoholism Research Monograph No. 37; National Institute on Alcohol Abuse and Alcoholism: Bethesda, MD, USA, 2002; pp. 321–369. [Google Scholar]
- May, PA; Brooke, L; Gossage, JP; Croxford, J; Adnams, C; Jones, KL; Robinson, L; Viljoen, D. Epidemiology of fetal alcohol syndrome in a South African community in the Western Cape Province. Am. J. Public Health 2000, 90, 1905–1912. [Google Scholar]
- May, PA; Brooke, LE; Gossage, JP; Snell, C; Hendricks, L; Croxford, J; Marais, A-S; Viljoen, DL. Maternal risk factors for fetal alcohol syndrome in the Western Cape Province of South Africa: A population-based study. Am. J. Public Health 2005, 95, 1190–1199. [Google Scholar]
- May, PA; Gossage, JP; Marais, AS; Adnams, CM; Hoyme, HE; Jones, KL; Robinson, LK; Khaole, NC; Snell, C; Kalberg, WO; Hendricks, L; Brooke, L; Stellavato, C; Viljoen, DL. The epidemiology of fetal alcohol syndrome and partial FAS in a South African community. Drug Alcohol Depen 2007, 88, 259–271. [Google Scholar]
- Viljoen, D; Croxford, J; Gossage, JP; Kodituwakku, PW; May, PA. Characteristics of mothers of children with fetal alcohol syndrome in the Western Cape Province of South Africa: A case control study. J. Stud. Alcohol 2002, 63, 6–17. [Google Scholar]
- Viljoen, DL; Gossage, JP; Adnams, CM; Jones, KL; Robinson, LK; Hoyme, HE; Snell, C; Khaole, N; Asante, KK; Findlay, R; Quinton, B; Brooke, LE; May, PA. Fetal alcohol syndrome epidemiology in a South African community: A second study of a very high prevalence area. J. Stud. Alcohol 2005, 5, 593–604. [Google Scholar]
- May, PA; Gossage, JP; Marais, AS; Hendricks, L; Snell, C; Tabachnick, BG; Stellavato, C; Buckley, DG; Brooke, L; Viljoen, DL. Maternal risk factors for fetal alcohol syndrome and partial fetal alcohol syndrome in south Africa: a third study. Alcohol. Clin. Exp. Res 2008, 32, 738–753. [Google Scholar]
- May, PA; Fiorentino, D; Gossage, JP; Kalberg, WO; Hoyme, HE; Robinson, LK; Coriale, G; Jones, KL; del Campo, M; Tarani, L; Romeo, M; Kodituwakku, PW; Deiana, L; Buckley, D; Ceccanti, M. The epidemiology of FASD in a province in Italy: Prevalence and characteristics of children in a random sample of schools. Alcohol. Clin. Exp. Res 2006, 30, 1562–1575. [Google Scholar]
- Kodituwakku, P; Coriale, G; Fiorentino, D; Aragon, A; Kalberg, WO; Buckley, D; Gossage, JP; Ceccanti, M; May, PA. Neurobehavioral characteristics of children with fetal alcohol spectrum disorders in communities from Italy: Preliminary results. Alcohol. Clin. Exp. Res 2006, 30, 1551–1561. [Google Scholar]
- Aragón, A; Coriale, G; Fiorentino, D; Kalberg, W; Buckley, D; Gossage, JP; Ceccanti, M; Mitchell, E; May, PA. Neuropsychological characteristics of Italian children with fetal alcohol spectrum disorders. Alcohol. Clin. Exp. Res 2008, 32, 1909–1919. [Google Scholar]
- Hoyme, HE; May, PA; Kalberg, WO; Kodituwakku, P; Gossage, JP; Trujillo, PM; Buckley, DG; Miller, JH; Aragon, AS; Khaole, N; Viljoen, DL; Jones, KL; Robinson, LK. A practical clinical approach to diagnosis of fetal alcohol spectrum disorders: Clarification of the 1996 institute of medicine criteria. Pediatrics 2005, 115, 39–47. [Google Scholar]
- Wurst, FM; Kelso, E; Weinmann, W; Pragst, F; Yegles, M; Sundström Poromaa, I. Measurement of direct ethanol metabolites suggests higher rate of alcohol use among pregnant women than found with the AUDIT—a pilot study in a population-based sample of Swedish women. Am J Obstet Gynecol 2008, 198, 407.e1–407.e5. [Google Scholar]
- Rustioni, DML. Prove di Valutazione Della Comprensione Linguistica; Organizzazione Speciali: Firenze, Italy, 1994. [Google Scholar]
- Raven, JC; Court, JH; Raven, J. Manual for Raven’s Progressive Matrices and Vocabulary Scales Section 1, General Overview and Section 2, Coloured Progressive Matrices; HK Lewis and Co, Ltd: London, UK, 1976. [Google Scholar]
- Rubini, V; Padovani, F. WISC-R Scala di Intelligenza Wechsler per Bambini Riveduta; Organizzazioni Speciali: Florence, Italy, 1986. (In Italaian). [Google Scholar]
- Streissguth, AP; Bookstein, FL; Barr, HM; Press, S; Sampson, PD. A fetal alcohol behavior scale. Alcohol. Clin. Exp. Res 1998, 22, 325–333. [Google Scholar]
- Pelham, WE, Jr; Gnagy, EM; Greenslade, KE; Milich, R. Teacher ratings of DSM-III-R symptoms for the disruptive behavior disorders. J. Am. Acad. Child Adolesc. Psychiatr 1992, 31, 210–218. [Google Scholar]
- Terreni, A; Tretti, ML; Corcella, PR; Cornoldi, C; Tressoldi, PE. Questionario Osservativo per l'identificazione Precoce Delle Difficoltà di Apprendimento (IPDA); Erickson: Trento, Italy, 2002. [Google Scholar]
- Dean, AG; Dean, JA; Burton, AH; Dicker, RC. A Word Processing, Database, and Statistics Program for Epidemiology on Microcomputers; Epi Info Version 6; USD, Inc.: Atlanta, GA, USA, 1996. [Google Scholar]
- Sokol, RJ; Miller, SI; Debanne, S; Golden, N; Collins, G; Kaplan, J; Martier, S. The Cleveland NIAAA prospective alcohol-in-pregnancy study: the first year. Neurobehav. Toxicol. Teratol 1981, 3, 203–209. [Google Scholar]
- Stoler, JM; Holmes, LB. Recognition of facial features of fetal alcohol syndrome in the newborn. Am. J. Med. Genet 2004, 127, 21–27. [Google Scholar]
- Autti-Rämö, I; Fagerlund, Å; Ervalahti, N; Korkman, M; Hoyme, HE. Fetal alcohol spectrum disorders in Finland: Clinical delineation of 77 older children and adolescents. Am. J. Med. Genet. A 2006, 140, 137–143. [Google Scholar]
- Aragón, A; Kalberg, W; Barela, LM; Tabachnick, BG; May, PA. Neuropsychological study of FASD in a sample of American Indian children: processing simple versus complex information. Alcohol. Clin. Exp. Res 2008, 32, 2136–2148. [Google Scholar]
- Petković, G; Barišić, I. FAS prevalence in a sample of urban schoolchildren in Croatia. Reprod. Toxicol 2010, 29, 237–241. [Google Scholar]
| Variable | Children In Study (n = 970) | Children With FAS (n = 8)**** | Children With PFAS (n = 36) | Control Children (n = 116) | P |
|---|---|---|---|---|---|
| Sex (%) | |||||
| Males | 50.6 | 37.5 | 52.8 | 52.6 | |
| Females | 49.4 | 62.5 | 47.2 | 47.4 | NS (0.706)a |
| Age (months) | |||||
| Mean (SD) | 79.5 (4.2) | 80.9 (2.9) | 79.4 (4.3) | 79.5 (3.5) | NS (0.577)b |
| Height (cm)* | |||||
| Mean (SD) | 121.5 (5.5) | 113.6 (3.6) | 118.0 (5.0) | 121.5 (4.9)** | <0.001b |
| Weight (kg)* | |||||
| Mean (SD) | 25.1 (5.2) | 18.8 (3.1) | 22.2 (3.7) | 25.1 (4.2)** | <0.001b |
| Children’s BMI* | |||||
| Mean (SD) | 16.8 (2.8) | 14.6 (2.9) | 15.9 (1.76) | 16.9 (2.3) | 0.002b |
| BMI Percentile* | |||||
| Mean (SD) | 60.9 (31.2) | 20.6 (32.6) | 51.4 (29.0) | 65.6 (29.4) | <0.001b |
| Occipital Circumference (OFC) (cm)* | |||||
| Mean (SD) | 51.9 (1.5) | 49.1 (1.0) | 50.6 (1.7) | 52.0 (1.3)** | <0.001b |
| Palpebral Fissure Length (PFL) (cm) | |||||
| Mean (SD) | 2.4 (0.1) | 2.4 (0.1) | 2.5 (0.1) | <0.001b | |
| Short Innercanthal Distance (ICD) (≤25%) | 25.0 | 19.4 | 6.0 | 0.022 | |
| Percent PFL is of ICD | |||||
| Mean(SD) | 84.0 (10.4) | 87.9 (9.9) | 89.4 (7.2) | NS (0.139)b | |
| Philtrum Length (cm) | |||||
| Mean | 1.5 (0.2) | 1.5 (0.2) | 1.4 (0.2) | 0.035 | |
| Hypoplastic Midface (%) | 62.5 | 30.6 | 12.9 | 0.001 a | |
| Maxillary Arc (cm) | |||||
| Mean | 23.3 (0.5) | 24.4 (1.1) | 24.9 (0.9) | <0.001 | |
| Mandibular Arc (cm) | |||||
| Mean (SD) | 23.9 (0.5) | 24.9 (1.2) | 25.6 (1.0) | <0.001 | |
| Strabismus (%) | 12.5 | 5.6 | 1.7 | 0.0034a | |
| Ptosis (%) | 0.0 | 8.3 | 0.0 | 0.005a | |
| Smooth Philtrum (%) | 87.5 | 91.7 | 13.8 | <0.001a | |
| Narrow Vermillion Border (%) | 100.0 | 94.4 | 21.6 | <0.001a | |
| Heart Murmur (%) | 12.5 | 0.0 | 1.7 | NS (0.060)a | |
| Clinodactyly (%) | 50.0 | 55.6 | 36.2 | NS (0.105)a | |
| Camptodactyly (%) | 0.0 | 13.9 | 4.3 | NS (0.088)a | |
| Dysmorphology Score*** | |||||
| Mean (SD) | 15.8 (1.9) | 11.2 (4.0) | 3.6 (2.9) | <0.001b | |
| Final Diagnosis FASD | ||||||
|---|---|---|---|---|---|---|
| FAS Mean Score (SD) | Partial FAS Mean Score (SD) | Controls Mean Score (SD) | Test Statistic *** | df | probability | |
| Child Variables | (n = 8) | (n = 36) | (n = 113) | |||
| Total dysmorphology score | 15.75bc (1.90) | 11.22ac (3.95) | 3.60ab (2.90) | F = 122.76 | 2/160 | <0.001 |
| Raven percentile | 50.62 (28.71) | 55.55c (22.28) | 70.97b (21.20) | F = 8.99 | 2/157 | <0.001 |
| Rustioni errors | 8.00 (3.91) | 7.76c (1.88) | 5.27b (2.51) | F = 8.37 | 2/85 | <0.001 |
| Rustioni qualitative | 3.13 (2.03) | 3.56c (2.09) | 4.78b (1.74) | F = 8.00 | 2/156 | <0.001 |
| Inattention DBD | 5.12 (7.01) | 7.28c (8.10) | 2.21b (3.72) | F = 12.97 | 2/154 | <0.001 |
| Hyperactivity DBD**** | 1.75 (2.71) | 4.86 (6.71) | 2.19 (4.26) | F = 4.23 | 2/156 | 0.016 |
| WISC-R Non-verbal IQ**** | 85.50 (22.21) | 95.42 (15.45) | 113.69 (17.48) | F = 11.03 | 2/71 | <0.001 |
| PBCL**** | 4.80 (5.76) | 7.37 (6.84) | 4.80 (5.76) | F = 6.20 | 2/136 | 0.003 |
| IDPA total score | 15.50 (4.98) | 17.03 (4.64) | 21.11 (5.78) | F = 9.68 | 2/151 | 0.001 |
| Maternal Variables | (n = 8) | (n = 34) | (n = 112) | |||
| Maternal age during index pregnancy | ||||||
| Mean (SD) | 31.50 (6.00) | 30.48 (5.20) | 29.25 (5.38) | F = 1.11 | 2/145 | NS(0.331) |
| Report drinking during pregnancy (%) | 50.0 | 54.8 | 40.0 | χ2 = 2.28 | 2/144 | NS(0.320) |
| Mean number of drinks current week** (SD) | 10.37 (18.92) | 1.78 (4.02) | 1.52 (2.80) | F = 10.94 | 2/145 | <0.001 |
| Mean drinks per current drinking day** (SD) | 1.56 (2.69) | .63 (.53) | .61 (.52) | F = 5.39 | 2/145 | 0.006 |
| Variable | Mothers of children with FASD (n = 39) | Control mothers (n = 107) | Test statistic P | OR (95% CI)d |
|---|---|---|---|---|
| Demographic and Socioeconomic Variables | ||||
| Mean Age (yrs) on day of interview (SD) | 37.2 (5.3) | 36.1 (5.4) | NS (0.260)b | |
| Educational attainment (%) | ||||
| Elementary | 7.7 | 1.9 | ||
| Junior high | 46.2 | 27.1 | ||
| Senior high | 23.1 | 51.4 | ||
| Beyond Senior High | 5.1 | 1.9 | ||
| College Degree | 17.9 | 17.8 | 0.015 a,e | |
| Religiosity Index - Mean (SD) | 4.8 (2.1) | 3.9 (2.2) | 0.025b | |
| Among those employed, actual job (%) | ||||
| Manual worker | 50.0 | 23.5 | ||
| Office worker | 44.4 | 54.4 | ||
| Manager in an office | 0.0 | 1.5 | ||
| Manager | 5.6 | 19.1 | ||
| Other | 0.0 | 1.5 | NS (0.212)a,e | |
| Substance Use Variables | (n = 30) | (n = 78) | ||
| Current drinker1 (of ever drinkers) - % | 93.3 | 97.4 | NS (0.311) | 0.37 (0.03–3.95) |
| Mean number of drinks last month2 | 20.3 (46.4) | 8.7 (12.0) | 0.045b | |
| (current drinkers) (SD) | ||||
| Among ever drinkers, drinking during: | ||||
| 1st trimester of pregnancy with index child - % | 53.3 | 36.7 | NS (0.115)a | 1.97 (0.77–5.08) |
| 2nd trimester of pregnancy with index child - % | 60.0 | 34.2 | 0.014a | 2.89 (1.11–7.60) |
| 3rd trimester of pregnancy with index child - % | 56.7 | 34.2 | 0.033a | 2.52 (0.97–6.56) |
| Current smoker (of those who ever smoked) - % | 34.8 | 57.7 | NS (0.067)a | 0.39 (0.12–1.22) |
| Percent smoked 3 months before index pregnancy (among ever smokers) | 73.9 | 71.2 | NS (0.806)a | 1.15 (0.33–4.07) |
| Percent who smoked during index pregnancy(ever smokers) | 31.8 | 28.8 | NS (0.798)a | 1.15 (0.34–3.87) |
| Diagnosis with direct confirmation of alcohol use during pregnancy | Diagnosis w/o direct confirmation of alcohol use during pregnancy | Total cases | (a)* Sample rates* | (b)** 95% Conf. Interval* | (c)*** Rate for all enrolled children | (d) Range of rates for all enrolled children* | (e) Cases in randomly selected group | (f) **** Sample rate from random selection | (g) ***** Widest range of rates from various methods | |
|---|---|---|---|---|---|---|---|---|---|---|
| FAS | 5 | 3 | 8 | 8.2 | 6.5–10.1 | 4.0 | 4.0–8.2 | 2 | 12.0 | 4.0–12.0 |
| PFAS | 21 | 15 | 36 | 36.9 | 32.7–40.6 | 18.1 | 18.1–36.9 | 7 | 46.3 | 18.1–46.3 |
| ARBD1 | 1 | 0 | 1 | 1.0 | - | 0.5 | 0.5–1.0 | - | 0.5 | 0.5–1.0 |
| ARND1 | 1 | 0 | 1 | 1.0 | - | 0.5 | 0.5–1.0 | - | 0.5 | 0.5–1.0 |
| Total | 28 | 18 | 46 | 47.1 | 33.4–62.6 | 23.1 | 23.1–47.1 | 9 | 59.4 | 23.1–62.6 |
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
May, P.A.; Fiorentino, D.; Coriale, G.; Kalberg, W.O.; Hoyme, H.E.; Aragón, A.S.; Buckley, D.; Stellavato, C.; Gossage, J.P.; Robinson, L.K.; et al. Prevalence of Children with Severe Fetal Alcohol Spectrum Disorders in Communities Near Rome, Italy: New Estimated Rates Are Higher than Previous Estimates. Int. J. Environ. Res. Public Health 2011, 8, 2331-2351. https://doi.org/10.3390/ijerph8062331
May PA, Fiorentino D, Coriale G, Kalberg WO, Hoyme HE, Aragón AS, Buckley D, Stellavato C, Gossage JP, Robinson LK, et al. Prevalence of Children with Severe Fetal Alcohol Spectrum Disorders in Communities Near Rome, Italy: New Estimated Rates Are Higher than Previous Estimates. International Journal of Environmental Research and Public Health. 2011; 8(6):2331-2351. https://doi.org/10.3390/ijerph8062331
Chicago/Turabian StyleMay, Philip A., Daniela Fiorentino, Giovanna Coriale, Wendy O. Kalberg, H. Eugene Hoyme, Alfredo S. Aragón, David Buckley, Chandra Stellavato, J. Phillip Gossage, Luther K. Robinson, and et al. 2011. "Prevalence of Children with Severe Fetal Alcohol Spectrum Disorders in Communities Near Rome, Italy: New Estimated Rates Are Higher than Previous Estimates" International Journal of Environmental Research and Public Health 8, no. 6: 2331-2351. https://doi.org/10.3390/ijerph8062331





