The Influence of Secondhand Smoke Exposure on Birth Outcomes in Jordan
Abstract
:1. Introduction
1.2. Hypotheses
- Increasing the reported average number of SHS exposure hours per week from home, work, and outside in the first, second, and third trimesters lead to decreasing the neonatal birth weight significantly after controlling for covariates.
- Women who reported higher average number of SHS exposure hours per week from home, work, and outside in the first, second, and third trimesters were at significantly greater risk for having a LBW neonate than women who reported lower average number of SHS exposure hours after controlling for covariates.
1.3. Health and Smoking Behavior in Jordan
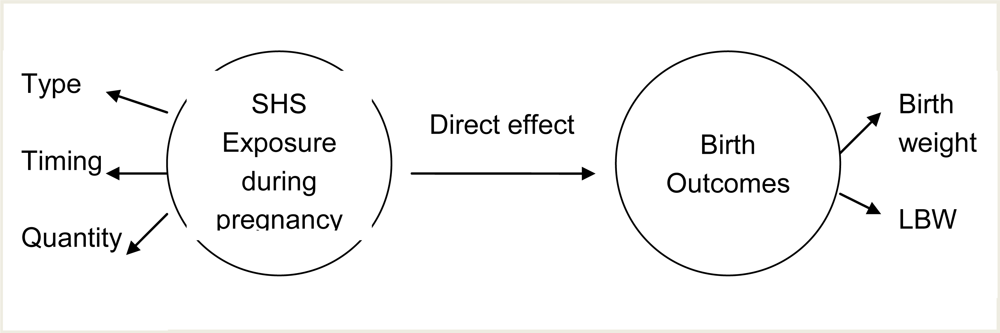
1.4. Theoretical Framework
1.5. Potential Covariates of Newborn Weight
2. Methods
2.1. Setting
2.2. Sampling
2.3. Measurement
Environmental tobacco smoke exposure questionnaire
Preliminary study
Medical records
3. Results
3.1. Maternal and Neonate’s Characteristics
3.2. Maternal Obstetric History and Current Delivery
3.3. Environmental Tobacco Smoke Exposure
3.4. Comparison between the Groups of Participants Who Had Normal Birth Weight Neonates and who had LBW Neonates
3.5. The Influence of SHS on Neonatal Birth Weight
3.6. The Risk of Having Low Birth Weight Neonate as a Result of SHS Exposure
4. Discussion
4.1. Significant Covariates
4.2 Practice Implications
4.3. Public Health Implications
4.4. Limitations
References
- U.S. Department of Health and Human Services. The Health Consequences of Involuntary Exposure To Tobacco Smoke: A Report Of The Surgeon General; Centers for Disease Control, Office of Smoking and Health: Rockville, MD, USA, 2006. [Google Scholar]
- Johansson, A; Halling, A; Hermansson, G. Indoor and outdoor smoking: Impact on children's health. Eur. J. Public Health 2003, 13, 61–66. [Google Scholar]
- Johansson, A; Hermansson, G; Ludvigsson, J. How should parents protect their children from environmental tobacco-smoke exposure in the home? Pediatrics 2004, 113, e291–e295. [Google Scholar]
- Seo, D; Bodde, AE; Torabi, MR. Salient environmental and perceptual correlates of current and established smoking for 2 representative cohorts of Indiana adolescents. J. School Health 2009, 79, 98–107. [Google Scholar]
- Seong, MW; Hwang, JH; Moon, JS; Ryu, HJ; Kong, SY; Um, TH; Park, JG; Lee, DH. Neonatal hair nicotine levels and fetal exposure to paternal smoking at home. Am. J. Epidemiol 2008, 168, 1140–1144. [Google Scholar]
- World Health Organization. Tobacco.
- Save the Children. State of the world’s newborns: A report from saving newborn lives; Save the Children Federation: Washington, DC, USA, 2001. [Google Scholar]
- Blanc, AK; Wardlaw, T. Monitoring low birth weight: an evaluation of international estimates and an updated estimation procedure. Bull. World Health Organ 2005, 83, 178–185. [Google Scholar]
- Central Intelligence Agency.
- Department of Statistics in Jordan.
- U.S. Census Bureau, Population Division.
- Demographic and Socioeconomic Statistics: World Health Statistics; World Health Organization: Geneva, Switzerland, 2007.
- World Health Organization. WHO Report on the Global Tobacco Epidemic 2008: The MPOWER Package.
- World Health Organization Statistical Information System. 2006 Core Health Indicators: World Health Statistics.
- Centers for Disease Control and Prevention; World Health Organization. Global School-Based Student Health Survey (GSSHS): Jordan GSSHS Report; Atlanta, GA, USA, 2007. [Google Scholar]
- Merrill, RM; Madanat, H; Layton, JB; Hanson, CL; Madsen, CC. Smoking prevalence, attitudes, and perceived smoking prevention control responsibilities and behaviors among physicians in Jordan. Int. Q. Community Health Educ 2006–2007, 26, 397–413. [Google Scholar]
- Haddad, LG; Petro-Nustas, W. Predictors of intention to quit smoking among Jordanian University students. Can. J. Public Health 2006, 97, 9–13. [Google Scholar]
- Haddad, LG; Malak, MZ. Smoking habits and attitudes towards smoking among university students in Jordan. Int. J. Nurs. Stud 2002, 39, 793–802. [Google Scholar]
- Khader, YS; Alsadi, AA. Smoking habits among university students in Jordan: Prevalence and associated factors. East. Mediterr. Health J 2008, 14, 897–904. [Google Scholar]
- Ma, GX; Tan, Y; Fang, CY; Toubbeh, JI; Shive, SE. Knowledge, attitudes and behavior regarding secondhand smoke among Asian Americans. Prev. Med 2005, 41, 446–453. [Google Scholar]
- U.S. Department of Health and Human Services. Healthy People 2010: Understanding and Improving Health, 2nd ed; U.S. Government Printing Office: Washington, DC, USA, 2000. [Google Scholar]
- World Health Organization. Promotion of Healthy Life Styles Including Oral Health, Tobacco, Nutrition and Rehabilitation.
- Andres, RL; Day, MC. Perinatal complications associated with maternal tobacco use. Semin. Neonatol 2000, 5, 231–241. [Google Scholar]
- Boutayeb, A; Boutayeb, S. The burden of non communicable diseases in developing countries. Int J Equity Health 2005, 4, 2:1–2:8. [Google Scholar]
- Centers for Disease Control and Prevention. Smoking during pregnancy—United States, 1990−2002. MMWR Morb. Mortal. Wkly. Rep 2004, 53, 911–915. [Google Scholar]
- Blake, SM; Murray, KD; El-Khorazaty, MN; Gantz, MG; Kiely, M; Best, D; Joseph, JG; El-Mohandes, AA. Environmental tobacco smoke avoidance among pregnant African-American nonsmokers. Am. J. Prev. Med 2009, 36, 225–234. [Google Scholar]
- Dejmek, J; Solansky, I; Podrazilova, K; Sram, R. The exposure of non smoking and smoking mothers to environmental tobacco smoke during different gestational phases and fetal growth. Environ. Health Perspect 2002, 110, 601–606. [Google Scholar]
- Goel, P; Radotra, A; Singh, I; Aggarwal, A; Dua, D. Effects of passive smoking on outcome in pregnancy. J. Postgrad. Med 2004, 50, 12–16. [Google Scholar]
- Andersson, R; Bergstrom, S. Maternal nutrition and socio-economic status as determinants of birthweight in chronically malnourished African women. Trop. Med. Int. Health 1997, 2, 1080–1087. [Google Scholar]
- Chan, A; Keane, RJ; Robinson, JS. The contribution of maternal smoking to preterm birth, small for gestational age, and low birth weight among aboriginal and non-aboriginal births in South Australia. Med. J. Aust 2001, 174, 389–393. [Google Scholar]
- Haug, K; Irgens, LM; Skjaerven, R; Markestad, T; Baste, V; Schreuder, P. Maternal smoking and birth weight: Effect modification of period, maternal age, and paternal smoking. Acta Obstet. Gynecol. Scand 2001, 79, 485–489. [Google Scholar]
- Hegaard, HK; Kjaergaard, H; Moller, LF; Wachmann, H; Ottesen, B. The effect of environmental tobacco smoke during pregnancy on birth weight. Acta Obstet. Gynecol. Scand 85, 675–681.
- Hong, R; Betancourt, JA; Ruiz-Beltran, M. Passive smoking as a risk factor of anemia in young children aged 0–35 months in Jordan. BMC Pediatrics 2007, 7, 16. [Google Scholar]
- Hruba, D; Kachlik, P. Influence of maternal active and passive smoking during pregnancy on birthweight in newborns. Cent. Eur. J. Public Health 2000, 8, 249–252. [Google Scholar]
- Jordanov, JS. Cotinine concentrations in amniotic fluid and urine of smoking, passive smoking and non-smoking pregnant women at term and in the urine of their neonates on 1st day of life. Eur. J. Pediatr 1990, 149, 734–737. [Google Scholar]
- Werler, M. Teratogen update: Smoking and reproductive outcomes. Teratology 1997, 55, 382–388. [Google Scholar]
- Leonardi-Bee, J; Smyth, A; Britton, J; Coleman, T. Environmental tobacco smoke and fetal health: Systematic review and meta analysis. Arch. Dis. Child. Fetal Neonatal Ed 2008, 93, F351–361. [Google Scholar]
- Boyle, MH; Racine, Y; Georgiades, K; Snelling, D; Hong, S; Omariba, W; Hurley, P; Rao-Melancini, P. The influence of economic development level, household wealth and maternal education on child health in the developing world. Soc. Sci. Med 2006, 63, 2242–2254. [Google Scholar]
- Smith, LC; Ruel, MT; Ndiaye, A. Why is child malnutrition lower in urban than in rural areas? Evidence from 36 developing countries. World Dev 2005, 33, 1285–1305. [Google Scholar]
- Feleke, Y; Enquoselassie, F. Maternal age, parity and gestational age on the size of the newborn in Addis Ababa. East Afr. Med. J 1999, 76, 468–471. [Google Scholar]
- Kawakita, A; Sato, K; Makino, H; Ikegami, H; Takayama, S; Toyama, Y; Umezawa, A. Nicotine acts on growth plate chondrocytes to delay skeletal growth through the alpha7 neuronal nicotinic acetylcholine receptor. PLoS One 2008, 3, e3945. [Google Scholar]
- Matt, GE; Quintana, PJ; Hovell, MF; Bernert, JT; Song, S; Novianti, N; Juarez, T; Floro, J; Gehrman, C; Garcia, M; Larson, S. Households contaminated by environmental tobacco smoke: Sources of infant exposures. Tob. Control 2004, 13, 29–37. [Google Scholar]
- Soliman, S; Pollack, HA; Warner, KE. Decrease in the prevalence of environmental tobacco smoke exposure in the home during the 1990s in families with children. Am. J. Public Health 2004, 94, 314–320. [Google Scholar]
- Tough, SC; Svenson, LW; Johnston, DW; Schopflocher, D. Characteristics of preterm delivery and low birthweight among 113,994 infants in Alberta: 1994−1996. Can. J. Public Health 2001, 92, 276–280. [Google Scholar]
- Cohen, JA. Power primer. Psychol. Bull 1992, 112, 155–159. [Google Scholar]
- Centers for Disease Control and Prevention. Overview of Pregnancy Risk Assessment Monitoring System (PRAMS).
- The Hashemite Kingdom of Jordan Ministry of Health: Annual Statistical Book; Ministry of Health: Amman, Jordan, 2008.
- Eliopoulos, C; Klein, J; Phan, MK; Knie, B; Greenwald, M; Chitayat, D; Koren, G. Hair concentrations of nicotine and cotinine in women and their newborn infants. J. Am. Med. Assoc 1994, 271, 621–623. [Google Scholar]
- Roquer, JM; Figueras, J; Botet, F; Jimenez, R. Influence on fetal growth of exposure to tobacco smoke during pregnancy. Acta Paediatr 1995, 84, 118–121. [Google Scholar]
- World Health Organization. Environmental Tobacco Smoke Seriously Endangers Children’s Health.
- Zhang, J; Ratcliffe, JM. Paternal smoking and birthweight in Shanghai. Am. J. Public Health 1993, 83, 207–210. [Google Scholar]
- Delgado-Rodriguez, M; Perez-Iglesias, R; Gomez-Olmedo, M; Bueno-Cavanillas, A; Galvez-Vargas, R. Risk factors for low birth weight: Results from a case-control study in southern Spain. Am. J. Phys. Anthropol 1998, 105, 419–424. [Google Scholar]
- Martinez, FD; Wright, AL; Taussig, LM. The effect of paternal smoking on the birthweight of newborns whose mothers did not smoke. Am. J. Public Health 1994, 84, 1489–1491. [Google Scholar]
- World Health Organization, Department of Reproductive Health and Research; United Nations Children’s Fund. Low Birthweight: Country, Regional, and Global Estimates; Geneva, Switzerland, 2004.
- World Health Organization. Women and the Tobacco Epidemic: Challenges for the 21st Century.
- The World Bank Group. Country Brief: Middle East and North African Region (MENA)-Jordan 1999.
- Misra, DP; Nguyen, RH. Environmental tobacco smoke and low birth weight: A hazard in the workplace? Environ. Health Perspect 1999, 107, 897–904. [Google Scholar]
| Frequency | Percent | |
|---|---|---|
| First month | 118 | 39.3 |
| Second month | 75 | 25.0 |
| Third month | 45 | 15.0 |
| Fourth month | 37 | 12.3 |
| Fifth month | 14 | 4.70 |
| Sixth month | 8 | 2.70 |
| Seventh month | 2 | 0.70 |
| Eight month | 1 | 0.30 |
| Total | 300 | 100 |
| Frequency | Percent | |
|---|---|---|
| Exposure from all places | 6 | 2.00 |
| Exposure from home and work only | 2 | 0.70 |
| Exposure from home and outside only | 165 | 55.00 |
| Exposure from work and outside only | 4 | 1.30 |
| Exposure from work only | 1 | 0.30 |
| Exposure from home only | 23 | 7.70 |
| Exposure from outside only | 91 | 30.30 |
| No exposure | 8 | 2.70 |
| Minimum # of SHS exposure hours/ week | Maximum # of SHS exposure hours/ week | Mean of SHS exposure hours in the first trimester | Mean of SHS exposure hours in the second trimester | Mean of SHS exposure hours in the third trimester | |
|---|---|---|---|---|---|
| Home | 2 | 35 | 13.09 | 13.20 | 13.10 |
| Work | 2 | 15 | 5.00 | 4.800 | 4.54 |
| Outside | 0.5 | 21 | 4.80 | 4.86 | 4.85 |
| NBW (n = 272) | LBW (n = 28) | t-test for equality of means | |||||
|---|---|---|---|---|---|---|---|
| M | SD | M | SD | t | DF | P | |
| Mother’s weight before pregnancy | 63.57 | 10.59 | 56.96 | 7.82 | 4.095 | 38.0 | 0.000 |
| Mother’s age | 28.13 | 5.47 | 27.00 | 5.96 | 1.027 | 298 | 0.305 |
| Mother’s height | 160.32 | 6.33 | 159.64 | 5.56 | 0.545 | 298 | 0.586 |
| Weight gain during pregnancy | 11.27 | 3.48 | 9.82 | 3.23 | 2.112 | 298 | 0.036 |
| Number of mother’s pregnancies | 3.53 | 2.19 | 3.21 | 2.77 | 0.715 | 298 | 0.475 |
| Number of years of education | 11.40 | 2.77 | 11.39 | 2.99 | 0.014 | 298 | 0.989 |
| Total family income | 197.65 | 96.08 | 225.00 | 171.02 | −0.833 | 28.8 | 0.412 |
| Gestational age of the neonate | 39.40 | 1.18 | 38.74 | 1.22 | 2.823 | 298 | 0.005 |
| Unstandardized coefficients | Standardized coefficients | ☼p | |||
|---|---|---|---|---|---|
| ♦B | *SE | ◙β | ○t | ||
| Number of hours per week in which the mother was exposed to SHS from her husband or someone else at home in the second trimester. | −17.92 | 2.24 | −0.38 | −8.00 | 0.000 |
| Number of hours per week in which the mother was exposed to SHS from outside in the second trimester. | −25.98 | 4.98 | −0.25 | −5.21 | 0.000 |
| Gestational age of the neonate. | 58.02 | 17.28 | 0.16 | 3.36 | 0.001 |
| Mother’s weight before pregnancy. | 6.85 | 2.03 | 0.16 | 3.37 | 0.001 |
| Number of hours per week in which the mother was exposed to SHS from work in the second trimester. | −51.54 | 16.31 | −0.14 | −3.16 | 0.002 |
| Weight gain during pregnancy. | 16.55 | 5.87 | 0.13 | 2.82 | 0.005 |
| 95% CI for OR | |||||
|---|---|---|---|---|---|
| B | P | OR | *Lower | **upper | |
| Mother’s weight before pregnancy | −0.068 | 0.026 | 0.935 | 0.881 | 0.992 |
| Mother’s height | 0.066 | 0.135 | 1.068 | 0.980 | 1.164 |
| Weight gain during pregnancy | −0.156 | 0.037 | 0.856 | 0.739 | 0.991 |
| Total family income | 0.002 | 0.278 | 1.002 | 0.998 | 1.006 |
| Gestational age of the neonate | −0.358 | 0.073 | 0.699 | 0.472 | 1.034 |
| Number of hours per week in which the mother was exposed to ETS from work in the second trimester | 0.286 | 0.017 | 1.331 | 1.052 | 1.684 |
| Number of hours per week in which the mother was exposed to ETS from her husband or someone else at home in the third trimester | 0.073 | 0.001 | 1.075 | 1.029 | 1.124 |
| Number of hours per week in which the mother was exposed to ETS from outside in the third trimester | 0.143 | 0.002 | 1.154 | 1.055 | 1.262 |
© 2010 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Abu-Baker, N.N.; Haddad, L.; Savage, C. The Influence of Secondhand Smoke Exposure on Birth Outcomes in Jordan. Int. J. Environ. Res. Public Health 2010, 7, 616-634. https://doi.org/10.3390/ijerph7020616
Abu-Baker NN, Haddad L, Savage C. The Influence of Secondhand Smoke Exposure on Birth Outcomes in Jordan. International Journal of Environmental Research and Public Health. 2010; 7(2):616-634. https://doi.org/10.3390/ijerph7020616
Chicago/Turabian StyleAbu-Baker, Nesrin N., Linda Haddad, and Christine Savage. 2010. "The Influence of Secondhand Smoke Exposure on Birth Outcomes in Jordan" International Journal of Environmental Research and Public Health 7, no. 2: 616-634. https://doi.org/10.3390/ijerph7020616
APA StyleAbu-Baker, N. N., Haddad, L., & Savage, C. (2010). The Influence of Secondhand Smoke Exposure on Birth Outcomes in Jordan. International Journal of Environmental Research and Public Health, 7(2), 616-634. https://doi.org/10.3390/ijerph7020616




