Analysis of Blood Concentrations of Zinc, Germanium, and Lead and Relevant Environmental Factors in a Population Sample from Shandong Province, China
Abstract
:1. Introduction
2. Materials and Methods
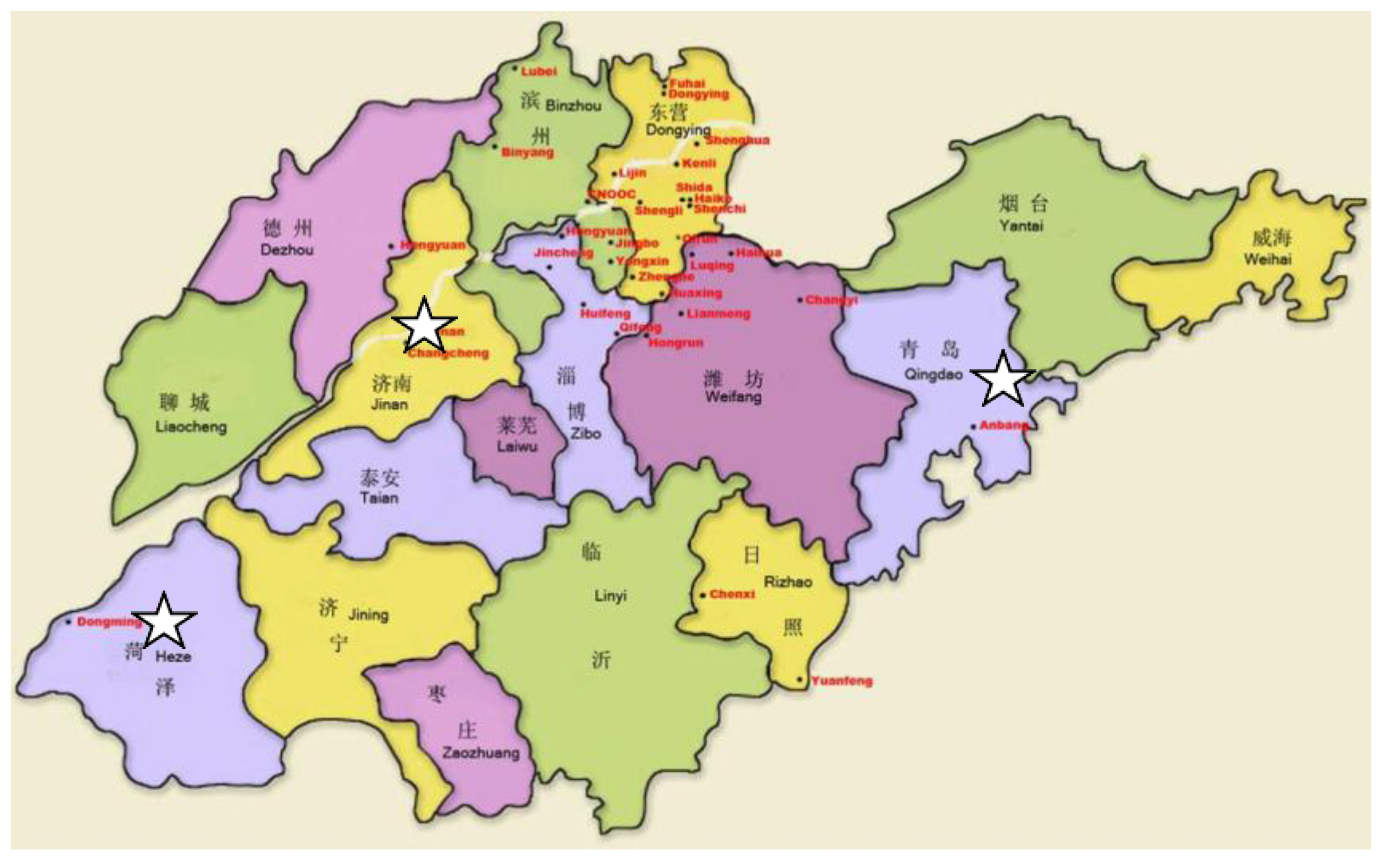
2.1. Subject Selection
2.2. Sample Preparation and Analysis
2.3. Quality Control
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Albertini, R.; Bird, M.; Doerrer, N.; Needham, L.; Robison, S.; Sheldon, L.; Zenick, H. The use of biomonitoring data in exposure and human health risk assessments. Environ. Health Perspect. 2006, 114, 1755–1762. [Google Scholar] [CrossRef] [PubMed]
- Minoia, C.; Pietra, R.; Sabbioni, E.; Ronchi, A.; Gatti, A.; Cavalleri, A.; Manzo, L. Trace element reference values in tissues from inhabitants of the European Community. III. The control of preanalytical factors in the biomonitoring of trace elements in biological fluids. Sci. Total Environ. 1992, 120, 63–79. [Google Scholar] [CrossRef]
- Korvela, M.; Lind, A.L.; Wetterhall, M.; Gordh, T.; Andersson, M.; Pettersson, J. Quantification of 10 elements in human cerebrospinal fluid from chronic pain patients with and without spinal cord stimulation. J. Trace Elements Med. Biol. 2016, 37, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Bloise, A.; Barca, D.; Gualtieri, A.F.; Pollastri, S.; Belluso, E. Trace elements in hazardous mineral fibres. Environ. Pollut. 2016, 216, 314–323. [Google Scholar] [CrossRef] [PubMed]
- Czarnek, K.; Terpiłowska, S.; Siwicki, A.K. Selected aspects of the action of cobalt ions in the human body. Cent. Eur. J. Immunol. 2015, 40, 236–242. [Google Scholar] [CrossRef] [PubMed]
- Anderson, R.A. Essentiality of chromium for human nutrition and health. Sci. Total Environ. 1989, 86, 75–81. [Google Scholar] [CrossRef]
- Van Bakel, M.M.; Printzen, G.; Wermuth, B.; Wiesmann, U.N. Antioxidant and thyroid hormone status in selenium deficient phenylketonuric and hyperphenylalaninemic patients. Am. J. Clin. Nutr. 2000, 72, 976–981. [Google Scholar] [PubMed]
- Araya, M.; Pizarro, F.; Olivares, M.; Arredondo, M.; González, M.; Méndez, M. Understanding copper homeostasis in humans and copper effects on health. Biol. Res. 2006, 39, 183–187. [Google Scholar] [CrossRef] [PubMed]
- Bonham, M.; O’Connor, J.M.; Hannigan, B.M.; Strain, J.J. The immune system as a physiological indicator of marginal copper status? Br. J. Nutr. 2002, 87, 393–403. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.D. Low dietary copper increases fecal free radical production, fecal water alkaline phosphatase activity and cytotoxicity in healthy men. J. Nutr. 2003, 133, 522–527. [Google Scholar] [PubMed]
- Sujiwattanarat, P.; Pongsanarakul, P.; Temsiripong, Y.; Temsiripong, T.; Thawornkuno, C.; Uno, Y.; Unajak, S.; Matsuda, Y.; Choowongkomon, K.; Srikulnath, K. Molecular cloning and characterization of Siamese crocodile (Crocodylus siamensis) copper, zinc superoxide dismutase (CSI-Cu, Zn-SOD) gene. Comp. Biochem. Physiol. A Mol. Integr. Physiol. 2016, 191, 187–195. [Google Scholar] [CrossRef] [PubMed]
- Maret, W.; Sandstead, H.H. Zinc requirements and the risks and benefits of zinc supplementation. J. Trace Elements Med. Biol. 2006, 20, 3–18. [Google Scholar] [CrossRef] [PubMed]
- Gmoshinskiĭ, I.V.; Munkhuu, B.; Mazo, V.K. Trace elements in human nutrition: Biological indices of zinc insufficiency. Vopr. Pitan. 2006, 75, 4–11. [Google Scholar] [PubMed]
- Zheng, J.; Zhang, Y.; Xu, W.; Luo, Y.; Hao, J.; Shen, X.L.; Yang, X.; Li, X.; Huang, K. Zinc protects HepG2 cells against the oxidative damage and DNA damage induced by ochratoxin A. Toxicol. Appl. Pharmacol. 2013, 268, 123–131. [Google Scholar] [CrossRef] [PubMed]
- Sharif, R.; Thomas, P.; Zalewski, P. The role of zinc in genomic stability. Mutat. Res. 2012, 733, 111–121. [Google Scholar] [CrossRef] [PubMed]
- Gazaryan, I.G.; Krasnikov, B.F.; Ashby, G.A.; Thorneley, R.N.; Kristal, B.S.; Brown, A.M. Zinc is a potent inhibitor of thiol oxidoreductase activity and stimulates reactive oxygen species production by lipoamide dehydrogenase. J. Biol. Chem. 2002, 277, 10064–10072. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.M.; Kristal, B.S.; Effron, M.S.; Shestopalov, A.I.; Ullucci, P.A.; Sheu, K.F.; Blass, J.P.; Cooper, A.J. Zn2+ inhibits alpha-ketoglutarate-stimulated mitochondrial respiration and the isolated alpha-ketoglutarate dehydrogenase complex. J. Biol. Chem. 2000, 275, 13441–13447. [Google Scholar] [CrossRef] [PubMed]
- Qiao, Y.; Zhang, W.; Tian, P.; Meng, F.; Zhu, H.; Jiang, X.; Liu, X.; Chu, P.K. Stimulation of bone growth following zinc incorporation into biomaterials. Biomaterials 2014, 35, 6882–6897. [Google Scholar] [CrossRef] [PubMed]
- Sharir, H.; Zinger, A.; Nevo, A.; Sekler, I.; Hershfinkel, M. Zinc released from injured cells is acting via the Zn2+-sensing receptor, ZnR, to trigger signaling leading to epithelial repair. J. Biol. Chem. 2010, 285, 26097–26106. [Google Scholar] [CrossRef] [PubMed]
- Cao, J.; Gao, Z.; Yan, J.; Li, M.; Su, J.; Xu, J.; Yan, C.H. Evaluation of trace elements and their relationship with growth and development of young children. Biol. Trace Element Res. 2016, 171, 270–274. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.S.; Choi, J.B.; Kim, H.J.; Park, S.B. Correlation between serum testosterone level and concentrations of copper and zinc in hair tissue. Biol. Trace Element Res. 2011, 144, 264–271. [Google Scholar] [CrossRef] [PubMed]
- Björndahl, L.; Kvist, U. A model for the importance of zinc in the dynamics of human sperm chromatin stabilization after ejaculation in relation to sperm DNA vulnerability. Syst. Biol. Reprod. Med. 2011, 57, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Ranasinghe, P.; Pigera, S.; Galappatthy, P.; Katulanda, P.; Constantine, G.R. Zinc and diabetes mellitus: Understanding molecular mechanisms and clinical implications. Daru 2015, 23, 44–56. [Google Scholar] [CrossRef] [PubMed]
- Slepchenko, K.G.; Daniels, N.A.; Guo, A.; Li, Y.V. Autocrine effect of Zn2+ on the glucose-stimulated insulin secretion. Endocrine 2015, 50, 110–122. [Google Scholar] [CrossRef] [PubMed]
- Mochizuki, K.; Murase, H.; Imose, M.; Kawakami, H.; Sawada, A. Improvement of scotopic electroretinograms and night blindness with recovery of serum zinclevels. Jpn. J. Ophthalmol. 2006, 50, 532–536. [Google Scholar] [CrossRef] [PubMed]
- Kraft, S.P.; Parker, J.A.; Matuk, Y.; Rao, A.V. The rat electroretinogram in combined zinc and vitamin A deficiency. Investig. Ophthalmol. Vis. Sci. 1987, 28, 975–984. [Google Scholar]
- Komai, M.; Goto, T.; Suzuki, H.; Takeda, T.; Furukawa, Y. Zinc deficiency and taste dysfunction, contribution of carbonic anhydrase, a zinc-metalloenzyme, to normaltaste sensation. Biofactors 2000, 12, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Fukasawa, T.; Orii, T.; Tanaka, M.; Suzuki, N.; Kanzaki, Y. Relation between drug-induced taste disorder and chelating behavior with zinc ion; statistical approach to the drug-induced taste disorder, part II. Chem. Pharm. Bull. 2008, 56, 1177–1180. [Google Scholar] [CrossRef] [PubMed]
- Desai, V.; Gaurav, I.; Kumar, M.V.; Gaurav, I.; Sharma, R. Molecular analysis of trace elements in oral submucous fibrosis and future perspective. Univers. Res. J. Dent. 2014, 4, 26–35. [Google Scholar] [CrossRef]
- Ray, J.G.; Ghosh, R.; Mallick, D.; Swain, N.; Gandhi, P.; Ram, S.S.; Selvaraj, S.; Rathore, A.; Mathummal, S.; Chakraborty, A. Correlation of trace elemental profiles in blood samples of Indian patients with leukoplakia and oral submucous fibrosis. Biol. Trace Element Res. 2011, 144, 295–305. [Google Scholar] [CrossRef] [PubMed]
- Hennigar, S.R.; Kelley, A.M.; McClung, J.P. Metallothionein and zinc transporter expression in circulating human blood cells as biomarkers of ZincStatus: A systematic review. Adv. Nutr. 2016, 7, 735–746. [Google Scholar] [CrossRef] [PubMed]
- Tomiyama, K.; Arakawa, Y. Zinc and tininduced apoptotic mechanisms in immune system and cranial nerve system. Nihon Rinsho 2016, 74, 1111–1119. [Google Scholar] [PubMed]
- Maywald, M.; Rink, L. Zinc supplementation induces CD4+CD25+Foxp3+ antigen-specific regulatory T cells and suppresses IFN-γ production by upregulation of Foxp3 and KLF-10 and downregulation of IRF-1. Eur. J. Nutr. 2016. [Google Scholar] [CrossRef] [PubMed]
- Beck, F.W.; Prasad, A.S.; Kaplan, J.; Fitzgerald, J.T.; Brewer, G.J. Changes in cytokine production and T cell subpopulations in experimentally induced zinc-deficient humans. Am. J. Physiol. 1997, 272, 1002–1007. [Google Scholar]
- Della Rovere, F.; Granata, A.; Pavia, R.; Tomaino, A.; Zirilli, A.; Monaco, F.; Familiari, D.; La Rocca, A.; Ientile, R.; Mondello, B.; et al. Vitamins A, E, microelements and membrane lipid peroxidation in patients with neoplastic disease treated with calcium antagonists and antagonists of receptors H2. Anticancer Res. 2004, 24, 1449–1453. [Google Scholar] [PubMed]
- Chen, J.F.; Shi, Q.J.; Zheng, S.Y. Experimental research of protective and therapeutic effects of zinc and vitamin E on mouse liver radiational damage. Hunan Yi Ke Da Xue Xue Bao 2001, 26, 207–210. [Google Scholar] [PubMed]
- Haberal, M.; Mavi, V.; Oner, G. The stabilizing effect of vitamin E, selenium and zinc on leucocyte membrane permeability: A study in vitro. Burns Incl. Therm. Inj. 1987, 13, 118–122. [Google Scholar] [CrossRef]
- Cai, C.; Lin, P.; Zhu, H.; Ko, J.K.; Hwang, M.; Tan, T.; Pan, Z.; Korichneva, I.; Ma, J. Zinc binding to MG53 protein facilitates repair of injury to cell membranes. J. Biol. Chem. 2015, 290, 13830–13839. [Google Scholar] [CrossRef] [PubMed]
- Yagi, T.; Asakawa, A.; Ueda, H.; Ikeda, S.; Miyawaki, S.; Inui, A. The role of zinc in the treatment of taste disorders. Recent Pat. Food Nutr. Agric. 2013, 5, 44–51. [Google Scholar] [CrossRef] [PubMed]
- Shweta, G.; Prantesh, J.; Shashvat, S. Isolated zinc deficiency causing severe microcytosis and sideroblastic anemia. Turk. J. Haematol. 2014, 31, 339–340. [Google Scholar] [CrossRef] [PubMed]
- Motooka, R.; Yamamoto, S. Copper deficiency myelopathy probably caused by long-lasting daily excessive intake of zinc. Rinsho Shinkeigaku 2016, 56, 690–693. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.; Jin, H.; Pi, J.; Jiang, J.H.; Liu, L.; Bai, H.H.; Yang, P.H.; Cai, J.Y. Anti-tumor activity evaluation of novel chrysin-organogermanium (IV) complex in MCF-7 cells. Bioorg. Med. Chem. Lett. 2013, 23, 5544–5551. [Google Scholar] [CrossRef] [PubMed]
- Jao, S.W.; Lee, W.; Ho, Y.S. Effect of germanium on 1,2-dimethylhydrazine-induced intestinal cancer in rats. Dis. Colon Rectum 1990, 33, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Yang, M.K.; Kim, Y.G. Protective role of germanium-132 against paraquat-induced oxidative stress in the livers of senescence-accelerated mice. J. Toxicol. Environ. Health A 1999, 58, 289–297. [Google Scholar] [PubMed]
- Wu, Z.; Chen, X.; Yang, K.; Xia, T. Studies on the hydroxyl free radical-scavenging effect of combined selenium and germanium. Wei Sheng Yan Jiu 2001, 30, 208–210. [Google Scholar]
- Mrema, J.E.; Slavik, M.; Davis, J. Spirogermanium: A new drug with antimalarial activity against chloroquine-resistant Plasmodium falciparum. Int. J. Clin. Pharmacol. Ther. Toxicol. 1983, 21, 167–171. [Google Scholar] [PubMed]
- Goodman, S. Therapeutic effects of organic germanium. Med. Hypotheses 1988, 26, 207–215. [Google Scholar] [CrossRef]
- DiMartino, M.J.; Lee, J.C.; Badger, A.M.; Muirhead, K.A.; Mirabelli, C.K.; Hanna, N. Antiarthritic and immunoregulatory activity of spirogermanium. J. Pharmacol. Exp. Ther. 1986, 236, 103–110. [Google Scholar] [PubMed]
- Lee, J.H.; Kim, K.W.; Yoon, M.Y.; Lee, J.Y.; Kim, C.J.; Sim, S.S. Anti-inflammatory effect of germanium-concentrated yeast against paw oedema is related to the inhibition of arachidonic acid release and prostaglandin E2 production in RBL 2H3 cells. Auton. Autacoid Pharmacol. 2005, 25, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Via, S. The role of trace elements in hematopoiesis. Terapevticheskiĭ Arkhiv 1963, 35, 3–14. [Google Scholar]
- Badger, A.M.; Mirabelli, C.K.; DiMartino, M. Generation of suppressor cells in normal rats by treatment with spirogermanium, a novel heterocyclic anticancer drug. Immunopharmacology 1985, 10, 201–207. [Google Scholar] [CrossRef]
- Nakamura, T.; Takeda, T.; Tokuji, Y. The oral intake of organic germanium, Ge-132, elevates α-Tocopherol levels in the Plas-ma and modulates hepatic gene expression profiles to promote immune activation in mice. Int. J. Vitam. Nutr. Res. 2014, 84, 183–195. [Google Scholar] [CrossRef] [PubMed]
- Hirayama, C.; Suzuki, H.; Ito, M.; Okumura, M.; Oda, T. Propagermanium: A nonspecific immune modulator for chronic hepatitis B. J. Gastroenterol. 2003, 38, 525–532. [Google Scholar] [PubMed]
- Li, Y.; Ren-Lu, H. Germanium and human healthy. Stud. Trace Elements Health 2005, 22, 60–61. [Google Scholar]
- Okada, K.; Okagawa, K.; Kawakami, K.; Kuroda, Y.; Morizumi, K.; Sato, H.; Morita, H.; Shimomura, S.; Saito, S. Renal failure caused by long-term use of a germanium preparation as an elixir. Clin. Nephrol. 1989, 31, 219–224. [Google Scholar] [PubMed]
- Krapf, R.; Schaffner, T.; Iten, P.X. Abuse of germanium associated with fatal lactic acidosis. Nephron 1992, 62, 351–356. [Google Scholar] [CrossRef] [PubMed]
- Kamijo, M.; Yagihashi, S.; Kida, K.; Narita, S.; Nakata, F. An autopsy case of chronic germanium intoxication presenting peripheral neuropathy, spinal ataxia, and chronic renal failure. Rinsho Shinkeigaku 1991, 31, 191–196. [Google Scholar] [PubMed]
- Schauss, A.G. Nephrotoxicity and neurotoxicity in humans from organogermanium compounds andgermanium dioxide. Biol. Trace Element Res. 1991, 29, 267–280. [Google Scholar] [CrossRef]
- Kim, K.M.; Lim, C.S.; Kim, S.; Kim, S.H.; Park, J.H.; Ahn, C.; Han, J.S.; Lee, J.S. Nephropathy and neuropathy induced by a germanium-containing compound. Nephrol. Dial. Transplant. 1998, 13, 3218–3219. [Google Scholar] [CrossRef] [PubMed]
- Dixon, C.; Hagemeister, F.; Legha, S.; Bodey, G. Pulmonary toxicity associated with spirogermanium. Cancer Treat Rep. 1984, 68, 907–908. [Google Scholar] [PubMed]
- Stewart, W.F.; Schwartz, B.S. Effects of lead on the adult brain: A 15-year exploration. Am. J. Ind. Med. 2007, 50, 729–739. [Google Scholar] [CrossRef] [PubMed]
- Lanphear, B.P.; Hornung, R.; Khoury, J.; Yolton, K.; Baghurst, P.; Bellinger, D.C.; Canfield, R.L.; Dietrich, K.N.; Bornschein, R.; Greene, T.; et al. Low-level environmental lead exposure and children’s intellectual function: An international pooled analysis. Environ. Health Perspect. 2005, 113, 894–899. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kupraszewicz, E.; Brzóska, M.M. Excessive ethanol consumption under exposure to lead intensifies disorders in bone metabolism: A study in a rat model. Chem. Biol. Interact. 2013, 203, 486–501. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Ochoa, I.; García-Vargas, G.; López-Carrillo, L.; Rubio-Andrade, M.; Morán-Martínez, J.; Cebrián, M.E.; Quintanilla-Vega, B. Low lead environmental exposure alters semen quality and sperm chromatin condensation in northern Mexico. Reprod. Toxicol. 2005, 20, 221–228. [Google Scholar] [CrossRef] [PubMed]
- Batra, N.; Nehru, B.; Bansal, M.P. Reproductive potential of male Portan rats exposed to various levels of lead with regard to zinc status. Br. J. Nutr. 2004, 91, 387–391. [Google Scholar] [CrossRef] [PubMed]
- Molina, R.M.; Phattanarudee, S.; Kim, J.; Thompson, K.; Wessling-Resnick, M.; Maher, T.J.; Brain, J.D. Ingestion of Mn and Pb by rats during and after pregnancy alters iron metabolism and behavior in off spring. Neurotoxicology 2011, 32, 413–422. [Google Scholar] [CrossRef] [PubMed]
- Ermentrout, R.M.; Layon, M.E.; Ackley, C.J.; Venkatesan, P.; Lowrey, C.H. The effects of lead and cadmium on GATA-1 regulated erythroid gene expression. Blood Cells Mol. Dis. 2006, 37, 164–172. [Google Scholar] [CrossRef] [PubMed]
- He, X.Y.; Yuan, L.Y.; Li, Y.T.; Li, M.; Chen, Y.; Yuan, H.; Wu, J.; Guo, C.Z.; Li, J. Cytotoxic responses and apoptosis in rat kidney epithelial cells exposed to lead. Biomed. Environ. Sci. 2016, 29, 529–533. [Google Scholar] [PubMed]
- Wilk, A.; Kalisińska, E.; Kosik-Bogacka, D.; Romanowski, M.; Różański, J.; Ciechanowski, K.; Słojewski, M.; Łanocha-Arendarczyk, N. Cadmium, lead and mercury concentrations in pathologically altered human kidneys. Environ. Geochem. Health 2016. [Google Scholar] [CrossRef] [PubMed]
- Cornelis, R.; Sabbioni, E.; Vander Venne, M.T. Trace element reference values in tissues from inhabitants of the European Community. Sci. Total Environ. 1994, 158, 191–226. [Google Scholar] [CrossRef]
- Wheal, M.S.; DeCourcy-Ireland, E.; Bogard, J.R.; Thilsted, S.H.; Stangoulis, J.C. Measurement of haem and total iron in fish, shrimp and prawn using ICP-MS: Implications for dietary iron intake calculations. Food Chem. 2016, 201, 222–229. [Google Scholar] [CrossRef] [PubMed]
- Feillet-Coudray, C.; Meunier, N.; Rambeau, M.; Brandolini-Bunlon, M.; Tressol, J.C.; Andriollo, M.; Mazur, A.; Cashman, K.D.; Coudray, C. Long-term moderate zinc supplementation increases exchangeable zinc pool masses in late-middle-aged men: The zenith study. Am. J. Clin. Nutr. 2005, 82, 103–110. [Google Scholar] [PubMed]
- Wessells, K.R.; Jorgensen, J.M.; Hess, S.Y.; Woodhouse, L.R.; Peerson, J.M.; Brown, K.H. Plasma zinc concentration responds rapidly to the initiation and discontinuation of short-term zinc supplementation in healthy men. J. Nutr. 2010, 140, 2128–2133. [Google Scholar] [CrossRef] [PubMed]
- Khandekar, R.N.; Raghunath, R.; Mishra, U.C. Levels of lead, cadmium, zinc and copper in the blood of an urban population. Sci. Total Environ. 1987, 66, 185–191. [Google Scholar] [CrossRef]
- Subramanian, K.S.; Meranger, J.C. Blood levels of cadmium, copper, lead and zinc in children in a British Columbia community. Sci. Total Environ. 1983, 30, 231–244. [Google Scholar] [CrossRef]
- Ding, C.; Zhu, C.; Liu, D.; Dong, M.; Zhang, A.H.; Pan, Y.J.; Yan, H.F. Inductively coupled plasma mass spectrometry for the simultaneous determination of thirty metals and metalloids elements in blood samples. Chin. J. Prev. Med. 2012, 46, 745–749. [Google Scholar]
- Bocca, B.; Madeddu, R.; Asara, Y.; Tolu, P.; Marchal, J.A.; Forte, G. Assessment of reference ranges for blood Cu, Mn, Se and Zn in a selected Italian population. J. Trace Element Med. Biol. 2011, 25, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.L.; Lu, L.; Pan, Y.J.; Ding, C.G.; Xu, D.Y.; Huang, C.F.; Pan, X.F.; Zheng, W. Baseline blood levels of manganese, lead, cadmium, copper, and zinc in residents of Beijing suburb. Environ. Res. 2015, 140, 10–17. [Google Scholar] [CrossRef] [PubMed]
- Bazzi, A.; Nriagu, J.O.; Linder, A.M. Determination of toxic and essential elements in children’s blood with inductively coupled plasma-mass spectrometry. J. Environ. Monit. 2008, 10, 1226–1232. [Google Scholar] [CrossRef] [PubMed]
- Moreno, M.A.; Marin, C.; Vinagre, F.; Ostapczuk, P. Trace element levels in whole blood samples from residents of the city Badajoz, Spain. Sci. Total Environ. 1999, 229, 209–215. [Google Scholar] [CrossRef]
- Joy, E.J.; Louise Ander, E.; Broadley, M.R.; Young, S.D.; Chilimba, A.D.; Hamilton, E.M.; Watts, M.J. Elemental composition of Malawian rice. Environ. Geochem. Health 2016. [Google Scholar] [CrossRef] [PubMed]
- Swamy, B.P.; Rahman, M.A.; Inabangan-Asilo, M.A.; Amparado, A.; Manito, C.; Chadha-Mohanty, P.; Reinke, R.; Slamet-Loedin, I.H. Advances in breeding for high grain Zinc in Rice. Rice 2016, 9, 49–64. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Huang, A.; Li, H. Investigation on the content of zinc, copper and chromium in the beverage industry. Stud. Trace Elements Health 2004, 21, 41–46. [Google Scholar]
- Fan, K.; Wang, X.; Tian, W. Six kinds of wine depends on the ICP-AES method in the determination of heavy metals. Chin. Public Health 2000, 16, 639. [Google Scholar]
- Wei, J. Investigation on 19 Trace Elements in Whole Blood among General Population in Chengde; Hebei Medical University: Shijiazhuang, China, 2006. [Google Scholar]
- Schroeder, H.A.; Balassa, J.J. Abnormal trace metals in man: Germanium. J. Chronic Dis. 1967, 20, 211–224. [Google Scholar] [CrossRef]
- Schultze, B.; Lind, P.M.; Larsson, A.; Lind, L. Whole blood and serum concentrations of metals in a Swedish population-based sample. Scand. J. Clin. Lab Investig. 2014, 74, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Ikeda, M.; Zhang, Z.W.; Shimbo, S.; Watanabe, T.; Nakatsuka, H.; Moon, C.S.; Matsuda-Inoguchi, N.; Higashikawa, K. Urban population exposure to lead and cadmium in east and south-east Asia. Sci. Total Environ. 2000, 249, 373–384. [Google Scholar] [CrossRef]
- Faro, A.R.; Pinto Wde, J.; Ferreira, A.P.; Barbosa Jr, F.; Souza, V.C.; Fujimoto, D.E.; Koifman, R.J.; Koifman, S. Serum cadmium levels in a sample of blood donors in the Western Amazon, Brazil, 2010–2011. Cad. Saude Publica 2014, 30, 403–414. [Google Scholar] [CrossRef] [PubMed]
- Farzin, L.; Amiri, M.; Shams, H.; Farzin, L.; Amiri, M.; Shams, H.; Faghih, M.A.A.; Moassesi, M.E. Blood levels of lead, cadmium, and mercury in residents of Tehran. Biol. Trace Element Res. 2008, 123, 14–26. [Google Scholar] [CrossRef] [PubMed]
- Nduka, J.K.; Orisakwe, O.E.; Ukaebgu, L.D.; Sokaibe, C.; Udowelle, N.A. Human health risk assessment of heavy metals in cosmetics in Nigeria. J. Cosmet. Sci. 2015, 66, 233–246. [Google Scholar] [PubMed]
- Zakaria, A.; Ho, Y.B. Heavy metals contamination in lipsticks and their associated health risks to lipstick consumers. Regul. Toxicol. Pharmacol. 2015, 73, 191–195. [Google Scholar] [CrossRef] [PubMed]
- Corbett, J.F. Cadmium, lead and nickel in hair care products in Turkey. J. Cosmet. Sci. 2015, 66, 65. [Google Scholar] [PubMed]
- Borowska, S.; Brzóska, M.M. Metals in cosmetics: Implications for human health. J. Appl. Toxicol. 2015, 35, 551–572. [Google Scholar] [CrossRef]
- Ozbek, N.; Akman, S. Determination of lead, cadmium and nickel in hennas and other hair dyes sold in Turkey. Regul. Toxicol. Pharmacol. 2016, 79, 49–53. [Google Scholar] [CrossRef] [PubMed]
- Kaličanin, B.; Velimirović, D. A Study of the Possible Harmful Effects of Cosmetic Beauty Products on Human Health. Biol. Trace Element Res. 2016, 170, 476–484. [Google Scholar] [CrossRef] [PubMed]
- Kristensen, L.J.; Taylor, M.P.; Evans, A.J. Reply to Gulson’s comments on “Tracing changes in atmospheric sourcesof lead contamination using lead isotopic compositions in Australian redwine”. Chemosphere 2016, 165, 579–584. [Google Scholar] [CrossRef] [PubMed]
- Kumar, V.; Tripathi, V.K.; Jahan, S.; Agrawal, M.; Pandey, A.; Khanna, V.K.; Pant, A.B. Lead intoxication synergies of the ethanol-induced toxic responses in neuronal cells—PC12. Mol. Neurobiol. 2015, 52, 1504–1520. [Google Scholar] [CrossRef] [PubMed]
- Taroni, M.; Zagà, V.; Bartolomei, P.; Gattavecchia, E.; Pacifici, R.; Zuccaro, P.; Esposito, M. 210Pb and 210Po concentrations in Italian cigarettes and effective dose evaluation. Health Phys. 2014, 107, 195–199. [Google Scholar] [CrossRef] [PubMed]
- Afridi, H.I.; Talpur, F.N.; Kazi, T.G.; Brabazon, D. Estimation of aluminum, arsenic, lead and nickel status in the samples of different cigarettes and their effect on human health of Irish smoker hypertensive consumers. Clin. Lab. 2015, 61, 1147–1156. [Google Scholar] [CrossRef] [PubMed]
- Forte, G.; Madeddu, R.; Tolu, P.; Asara, Y.; Marchal, J.A.; Bocca, B. Reference intervals for blood Cd and Pb in the general population of Sardinia (Italy). Int. J. Hyg. Environ. Health 2011, 214, 102–109. [Google Scholar] [CrossRef] [PubMed]

| Items | n | P5 | P25 | P50 | P75 | P95 | GM (95% CI) |
|---|---|---|---|---|---|---|---|
| Total population | 1302 | 1.41 | 2.40 | 3.10 | 3.83 | 5.02 | 3.14 (3.08–3.20) |
| Sex (p < 0.001) | |||||||
| Male | 765 | 1.32 | 2.29 | 3.00 | 3.74 | 4.86 | 3.04 (2.97–3.12) |
| Female | 537 | 1.55 | 2.51 | 3.26 | 3.99 | 5.13 | 3.28 (3.18–3.37) |
| Use of cosmetics (p = 0.991) | |||||||
| No | 1230 | 1.43 | 2.40 | 3.10 | 3.82 | 5.01 | 3.14 (3.08–3.20) |
| Yes | 72 | 1.23 | 2.35 | 3.08 | 3.97 | 5.35 | 3.14 (2.88–3.41) |
| Use of hair dye (p = 0.068) | |||||||
| No | 1190 | 1.43 | 2.41 | 3.13 | 3.84 | 5.03 | 3.16 (3.09–3.22) |
| Yes | 112 | 1.36 | 2.25 | 2.84 | 3.71 | 4.92 | 2.95 (2.76–3.14) |
| Age in years (p < 0.001) | |||||||
| 6–12 | 231 | 1.03 | 1.94 | 2.72 | 3.55 | 4.32 | 2.75 (2.61–2.88) |
| 12–16 | 214 | 1.65 | 2.49 | 3.17 | 3.70 | 4.91 | 3.13 (3.00–3.26) |
| 16–20 | 168 | 1.86 | 2.59 | 3.27 | 4.33 | 5.34 | 3.41 (3.24–3.58) |
| 20–30 | 187 | 1.78 | 2.89 | 3.63 | 4.27 | 5.56 | 3.61 (3.45–3.77) |
| 30–45 | 255 | 1.39 | 2.22 | 2.83 | 3.69 | 5.08 | 3.01 (2.88–3.15) |
| >45 | 247 | 1.52 | 2.38 | 3.05 | 3.81 | 4.77 | 3.10 (2.97–3.22) |
| Alcohol intake (p = 0.002) | |||||||
| No | 1110 | 1.40 | 2.39 | 3.08 | 3.75 | 4.93 | 3.09 (3.03–3.16) |
| Yes | 192 | 1.72 | 2.50 | 3.32 | 4.19 | 5.54 | 3.39 (3.22–3.56) |
| Smoking (p = 0.001) | |||||||
| No | 1111 | 1.36 | 2.39 | 3.07 | 3.77 | 4.96 | 3.10 (3.04–3.16) |
| Yes | 170 | 1.72 | 2.56 | 3.45 | 4.18 | 5.29 | 3.42 (3.25–3.59) |
| Former smoker | 21 | 1.44 | 2.28 | 2.73 | 3.52 | 5.35 | 2.91 (2.49–3.34) |
| Consumption of fried foods (p = 0.088) | |||||||
| 1–2 times per month | 842 | 1.40 | 2.39 | 3.06 | 3.76 | 4.91 | 3.10 (3.03–3.17) |
| 1–2 times per week | 380 | 1.49 | 2.43 | 3.19 | 3.87 | 5.19 | 3.17 (3.06–3.28) |
| Every day | 80 | 1.46 | 2.30 | 3.33 | 4.48 | 6.11 | 3.42 (3.12–3.72) |
| Items | n | P5 | P25 | P50 | P75 | P95 | GM (95% CI) |
|---|---|---|---|---|---|---|---|
| Total population | 1302 | 5.10 | 12.1 | 18.3 | 24.5 | 45.2 | 19.9 (19.3–20.6) |
| Sex (p = 0.095) | |||||||
| Male | 765 | 4.40 | 12.5 | 18.9 | 25.2 | 40.9 | 19.8 (19.0–20.6) |
| Female | 537 | 6.13 | 11.9 | 17.0 | 23.0 | 53.0 | 20.2 (19.1–21.3) |
| Use of cosmetics (p = 0.544) | |||||||
| No | 1230 | 5.11 | 12.2 | 18.3 | 24.6 | 43.3 | 19.9 (19.3–20.6) |
| Yes | 72 | 4.65 | 10.4 | 17.2 | 24.1 | 55.3 | 20.5 (17.1–23.9) |
| Use of hair dye (p = 0.016) | |||||||
| No | 1190 | 5.11 | 12.3 | 18.5 | 24.6 | 46.7 | 20.2 (19.5–20.8) |
| Yes | 112 | 4.99 | 10.9 | 15.3 | 22.6 | 38.7 | 17.6 (15.7–19.5) |
| Age in years (p < 0.001) | |||||||
| 6–12 | 231 | 1.04 | 9.96 | 17.9 | 23.1 | 27.0 | 16.2 (15.1–17.3) |
| 12–16 | 214 | 6.96 | 14.3 | 19.9 | 25.9 | 42.8 | 21.5 (20.0–23.0) |
| 16–20 | 168 | 9.61 | 15.0 | 22.8 | 45.2 | 62.2 | 29.3 (26.5–32.0) |
| 20–30 | 187 | 5.21 | 10.8 | 16.0 | 23.1 | 32.5 | 17.3 (16.0–18.5) |
| 30–45 | 255 | 4.89 | 12.6 | 19.4 | 26.8 | 42.5 | 20.9 (19.5–22.3) |
| >45 | 247 | 6.48 | 11.1 | 15.3 | 20.7 | 34.0 | 16.9 (15.8–17.9) |
| Alcohol intake (p = 0.001) | |||||||
| No | 1110 | 4.88 | 11.8 | 17.8 | 24.0 | 46.9 | 19.6 (18.9–20.3) |
| Yes | 192 | 6.44 | 13.8 | 20.8 | 28.0 | 41.5 | 21.7 (20.2–23.2) |
| Smoking (p = 0.148) | |||||||
| No | 1111 | 4.91 | 11.9 | 17.9 | 24.5 | 47.1 | 19.9 (19.2–20.6) |
| Yes | 170 | 5.70 | 13.8 | 18.9 | 24.6 | 36.4 | 19.9 (18.5–21.3) |
| Former smoker | 21 | 10.7 | 16.1 | 19.7 | 25.6 | 42.0 | 21.8 (17.9–25.6) |
| Consumption of fried foods (p < 0.001) | |||||||
| 1–2 times per month | 842 | 4.92 | 11.9 | 17.6 | 23.9 | 37.6 | 18.7 (18.0–19.4) |
| 1–2 times per week | 380 | 4.93 | 12.2 | 18.6 | 24.9 | 53.1 | 20.9 (19.5–22.3) |
| Every day | 80 | 7.31 | 16.1 | 23.6 | 40.4 | 63.4 | 28.5 (24.7–32.3) |
| Items | n | P5 | P25 | P50 | P75 | P95 | GM (95% CI) |
|---|---|---|---|---|---|---|---|
| Total population | 1302 | 3.00 | 12.5 | 20.9 | 32.2 | 56.0 | 24.1 (23.2–25.1) |
| Sex (p < 0.001) | |||||||
| Male | 765 | 4.48 | 14.0 | 22.9 | 35.2 | 58.9 | 26.6 (25.3–27.9) |
| Female | 537 | 2.05 | 10.3 | 17.9 | 28.4 | 47.6 | 20.6 (19.3–21.8) |
| Use of cosmetics (p = 0.019) | |||||||
| No | 1230 | 1.41 | 6.86 | 17.8 | 28.8 | 53.8 | 20.0 (16.0–24.0) |
| Yes | 72 | 3.69 | 12.7 | 21.1 | 32.4 | 56.3 | 24.4 (23.4–25.3) |
| Use of hair dye (p = 0.004) | |||||||
| No | 1190 | 0.12 | 9.12 | 17.9 | 27.1 | 49.0 | 19.6 (17.0–22.3) |
| Yes | 112 | 3.66 | 12.7 | 21.2 | 32.8 | 56.4 | 24.5 (23.5–25.5) |
| Age in years (p < 0.001) | |||||||
| 6–12 | 231 | 1.80 | 10.8 | 21.2 | 36.1 | 56.9 | 25.0 (22.7–27.3) |
| 12–16 | 214 | 7.48 | 18.0 | 25.6 | 35.6 | 53.4 | 27.7 (25.7–29.6) |
| 16–20 | 168 | 4.96 | 11.2 | 19.3 | 28.0 | 57.5 | 23.2 (20.4–26.0) |
| 20–30 | 187 | 5.33 | 14.9 | 22.3 | 34.3 | 56.5 | 26.9 (24.1–29.8) |
| 30–45 | 255 | 0.07 | 7.40 | 18.0 | 29.4 | 56.1 | 20.8 (18.6–22.9) |
| >45 | 247 | 4.99 | 12.8 | 18.6 | 27.4 | 55.0 | 22.13 (20.2–24.0) |
| Alcohol intake (p = 0.001) | |||||||
| No | 1110 | 2.67 | 12.0 | 20.4 | 31.5 | 51.6 | 23.4 (22.4–24.4) |
| Yes | 192 | 5.89 | 15.6 | 23.4 | 37.7 | 60.7 | 28.3 (25.6–31.0) |
| Smoking (p < 0.001) | |||||||
| No | 1111 | 2.62 | 11.9 | 19.9 | 31.5 | 51.6 | 23.1 (22.1–24.1) |
| Yes | 170 | 5.81 | 16.7 | 24.6 | 36.0 | 69.3 | 29.1 (26.3–32.0) |
| Former smoker | 21 | 5.20 | 22.0 | 25.2 | 42.6 | 153.0 | 37.9 (23.3–52.5) |
| Consumption of fried foods (p = 0.319) | |||||||
| 1–2 times per month | 842 | 2.94 | 12.5 | 20.6 | 32.4 | 56.8 | 24.1 (22.9–25.2) |
| 1–2 times per week | 380 | 3.56 | 12.1 | 21.2 | 31.6 | 53.0 | 23.8 (22.1–21.2) |
| Every day | 80 | 4.36 | 14.4 | 23.1 | 34.8 | 57.4 | 26.0 (22.5–29.5) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, L.; Xu, G.; Shao, H.; Zhang, Z.-H.; Pan, X.-F.; Li, J.-Y. Analysis of Blood Concentrations of Zinc, Germanium, and Lead and Relevant Environmental Factors in a Population Sample from Shandong Province, China. Int. J. Environ. Res. Public Health 2017, 14, 227. https://doi.org/10.3390/ijerph14030227
Li L, Xu G, Shao H, Zhang Z-H, Pan X-F, Li J-Y. Analysis of Blood Concentrations of Zinc, Germanium, and Lead and Relevant Environmental Factors in a Population Sample from Shandong Province, China. International Journal of Environmental Research and Public Health. 2017; 14(3):227. https://doi.org/10.3390/ijerph14030227
Chicago/Turabian StyleLi, Long, Guang Xu, Hua Shao, Zhi-Hu Zhang, Xing-Fu Pan, and Jin-Ye Li. 2017. "Analysis of Blood Concentrations of Zinc, Germanium, and Lead and Relevant Environmental Factors in a Population Sample from Shandong Province, China" International Journal of Environmental Research and Public Health 14, no. 3: 227. https://doi.org/10.3390/ijerph14030227





