Children’s Exposure to Secondhand Smoke during Ramadan in Jakarta, Indonesia
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. Measures
2.3. Data Transformation and Analyses
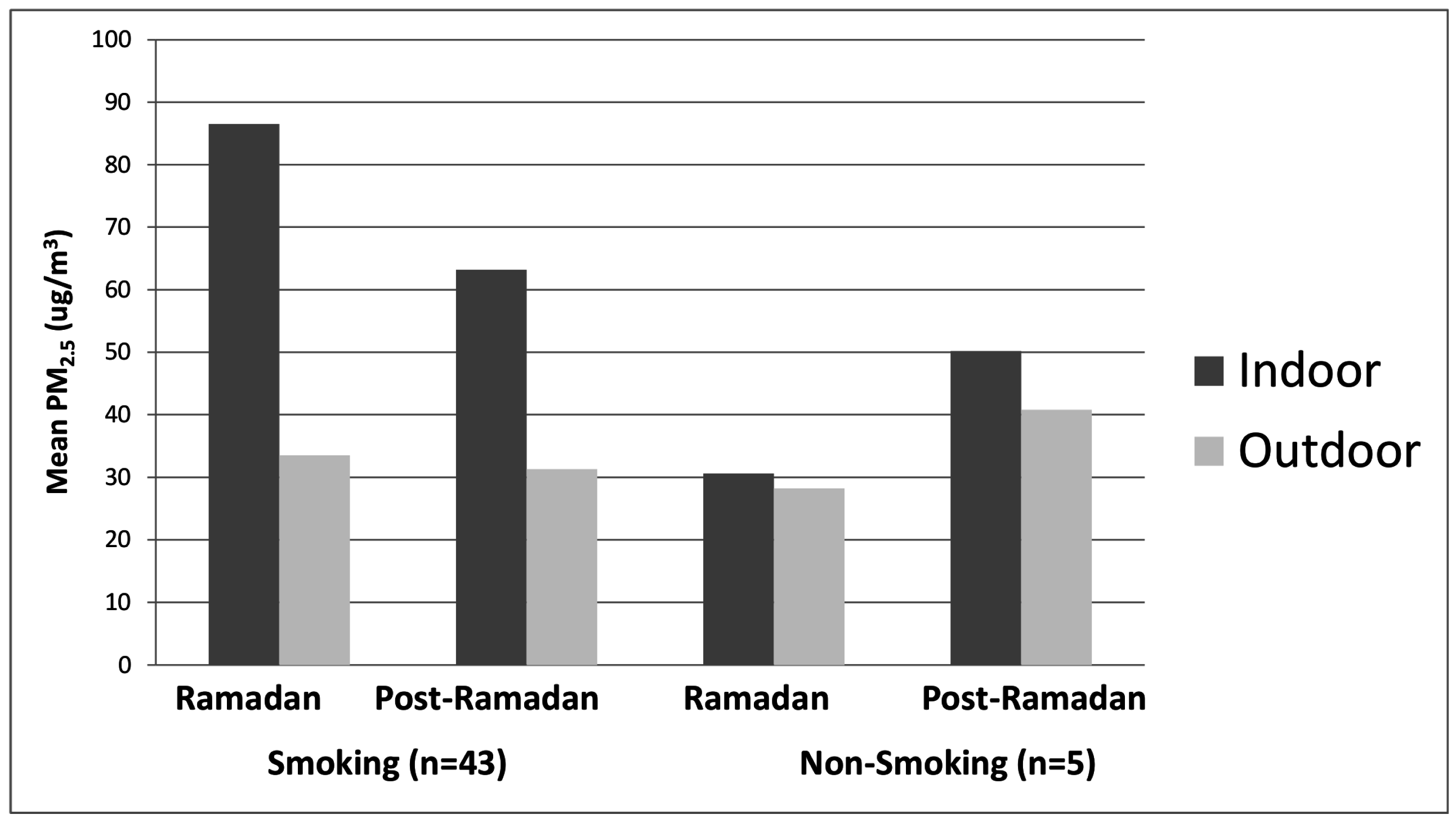
3. Results
3.1. Smoking Venues
3.2. Non-Smoking Venues
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Oberg, M.; Jaakkola, M.S.; Woodward, A.; Peruga, A.; Prüss-Ustün, A. Worldwide burden of disease from exposure to second-hand smoke: A retrospective analysis of data from 192 countries. Lancet 2011, 377, 139–146. [Google Scholar] [CrossRef]
- Eriksen, M.P.; Cerak, R.L. The diffusion and impact of clean indoor air laws. Annu. Rev. Public Health 2008, 29, 171–185. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services. The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2006.
- WHO Framework Convention on Tobacco. Guidelines for Implementation of Article 8 of the WHO; FCTC: Geneva, Switzerland, 2007. [Google Scholar]
- World Health Organization. WHO Report on the Global Tobacco Epidemic, 2009: Implementing Smoke-Free Environments; WHO Prevention of Noncommunicable Diseases: Geneva, Switzerland, 2009. [Google Scholar]
- King, B.A.; Mirza, S.A.; Babb, S.D. A cross-country comparison of secondhand smoke exposure among adults: Findings from the Global Adult Tobacco Survey (GATS). Tob. Control 2013, 22. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, S.J.; Tan, C. Overview of systematic reviews on the health-related effects of government tobacco control policies. BMC Public Health 2015, 15, 744. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Adult Tobacco Survey (GATS): Indonesia Report 2011; World Health Organization Regional Office for South-East Asia World Health House: New Delhi, India, 2012. [Google Scholar]
- World Health Organization. Global Youth Tobacco Survey (GYTS): Indonesia Report 2014; World Health Organization Regional Office for South-East Asia: New Delhi, India, 2015. [Google Scholar]
- World Health Organization. Profile on Implementation of WHO Framework Convention on Tobacco Control in the South-East Asia Region; World Health Organization Regional Office for South-East Asia: New Delhi, India, 2011. [Google Scholar]
- Euromonitor International. Passport: Tobacco in Indonesia; Chicago, IL, USA, 2013. [Google Scholar]
- Suhadi, D.S. Smoke-Free-Law in Jakarta: What Happened after Three Years of Implementation Pergub No 50/2012; Jakarta, Indonesia, 2015. [Google Scholar]
- Septiono, W.; Meyrowitsch, D.W. Family role towards smoking behaviour among Children in Jakarta. Kesmas Public Health J. 2014, 9, 58–63. [Google Scholar] [CrossRef]
- Hyland, A.; Travers, M.J.; Dresler, C.; Higbee, C.; Cummings, K.M. A 32-country comparison of tobacco smoke derived particle levels in indoor public places. Tob. Control 2008, 17, 159–165. [Google Scholar] [CrossRef] [PubMed]
- Apelberg, B.J.; Hepp, L.M.; Avila-Tang, E.; Gundel, L.; Hammond, S.K.; Hovell, M.F.; Hyland, A.; Klepeis, N.E.; Madsen, C.C.; Navas-Acien, A.; et al. Environmental monitoring of secondhand smoke exposure. Tob. Control 2013, 22, 147–155. [Google Scholar] [CrossRef] [PubMed]
- Jackson-Morris, A.; Bleymann, K.; Lyall, E.; Aslam, F.; Bam, T.S.; Chowdhury, I.; Daouda, E.A.; Espinosa, M.; Romo, J.; Singh, R.J.; et al. Low-cost air quality monitoring methods to assess compliance with smoke-free regulations: a multi-center study in six low- and middle-income countries. Nicotine Tob. Res. 2016, 18, 1258–1264. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Air Quality Guidelines for Particulate Matter, Ozone, Nitrogen Dioxide and Sulfur Dioxide; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- Ramahi, I.; Seidenberg, A.B.; Kennedy, R.D.; Rees, V.W. Secondhand smoke emission levels in enclosed public places during Ramadan. Eur. J. Public Health 2013, 23, 789–791. [Google Scholar] [CrossRef] [PubMed]
- Byron, M.J.; Cohen, J.E.; Gittelsohn, J.; Frattaroli, S.; Nuryunawati, R.; Jernigan, D.H. Influence of religious organisations’ statements on compliance with a smoke-free law in Bogor, Indonesia: A qualitative study. BMJ Open 2015, 5. [Google Scholar] [CrossRef] [PubMed]
- Kaufman, M.R.; Merritt, A.P.; Rimbatmaja, R.; Cohen, J.E. “Excuse me, sir. Please don’t smoke here”: A qualitative study of social enforcement of smoke-free policies in Indonesia. Health Policy Plan. 2015, 30, 995–1002. [Google Scholar] [CrossRef] [PubMed]
- Byron, M.J.; Suhadi, D.R.; Hepp, L.M. Secondhand tobacco smoke in public venues in three Indonesian cities. Med. J. Indones. 2013, 22, 232–237. [Google Scholar] [CrossRef]
- Fong, G.T.; Sansone, G.; Yan, M.; Craig, L.; Quah, A.C.K.; Jiang, Y. Evaluation of smoke-free policies in seven cities in China: Longitudinal findings from the ITC China Project (2007–2012). Tob. Control 2015, 24, iv14–iv20. [Google Scholar] [CrossRef] [PubMed]
- Reis, M.F.; Namorado, S.; Aguiar, P.; Precioso, J.; Nunes, B.; Veloso, L.; et al. Patterns of adherence to and compliance with the Portuguese smoke-free law in the leisure-hospitality sector. PLoS ONE 2014. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cains, T.; Cannata, S.; Poulos, R.; Ferson, M.J.; Stewart, B.W. Designated “no smoking” areas provide from partial to no protection from environmental tobacco smoke. Tob. Control 2004, 13, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Rosen, L.J.; Zucker, D.M.; Rosen, B.J.; Connolly, G.N. Second-hand smoke levels in Israeli bars, pubs and cafes before and after implementation of smoke-free legislation. Eur. J. Public Health 2011, 21, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Connolly, G.N.; Carpenter, C.M.; Travers, M.J.; Cummings, K.M.; Hyland, A.; Mulcahy, M.; Clancy, L. How smoke-free laws improve air quality: A global study of Irish pubs. Nicotine Tob. Res. 2009, 11, 600–605. [Google Scholar] [CrossRef] [PubMed]
- Hajizadeh, M.; Nandi, A. The socioeconomic gradient of secondhand smoke exposure in Children: Evidence from 26 low-income and middle-income countries. Tob. Control 2016. [Google Scholar] [CrossRef] [PubMed]
- Mao, A. Getting over the patriarchal barriers: Women’s management of men's smoking in Chinese families. Health Educ. Res. 2015, 30, 13–23. [Google Scholar] [CrossRef] [PubMed]
- Mao, A.; Bristow, K.; Robinson, J. Caught in a dilemma: Why do non-smoking women in China support the smoking behaviors of men in their families? Health Educ. Res. 2013, 28, 153–164. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Protection from Exposure to Secondhand Smoke: Policy Recommendations; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- Hovell, M.F.; Hughes, S.C. The behavioral ecology of secondhand smoke exposure: A pathway to complete tobacco control. Nicotine Tob. Res. 2009, 11, 1254–1264. [Google Scholar] [CrossRef] [PubMed]
- Hovell, M.; Wahlgren, D.; Adams, M. The logical and empirical basis for the behavioral ecological model. In Emerging Theories in Health Promotion Practice and Research; Ralph, J., Crosby, R.A., Kegler, M.C., Eds.; Jossey-Bass: San Francisco, CA, USA, 2009; pp. 415–449. [Google Scholar]
- Campaign for Tobacco Free Kids. Tactics to Undermine Smokefree Policies; Washington, DC, USA, 2009. [Google Scholar]
- Hurt, R.D.; Ebbert, J.O.; Achadi, A.; Croghan, I.T. Roadmap to a tobacco epidemic: Transnational tobacco companies invade Indonesia. Tob. Control 2012, 21, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Assunta, M.; Dorotheo, E.U. SEATCA Tobacco Industry Interference Index: A tool for measuring implementation of WHO Framework Convention on Tobacco Control Article 5.3. Tob. Control 2016, 25, 313–318. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Indoor air quality in hospitality venues before and after implementation of a clean indoor air law—Western New York, 2003. MMWR. Morb. Mortal. Wkly. Rep. 2004, 53, 1038–1041. [Google Scholar]
- Rosser, A. Contesting tobacco-control policy in Indonesia. Crit. Asian Stud. 2015, 47, 69–93. [Google Scholar] [CrossRef]
- Borland, R.; Yong, H.-H.; Siahpush, M.; Hyland, A.; Campbell, S.; Hastings, G.; Cummings, K.M.; Fong, G.T. Support for and reported compliance with smoke-free restaurants and bars by smokers in four countries: Findings from the International Tobacco Control (ITC) Four Country Survey. Tob. Control 2006, 15 (Suppl. 3), iii34–iii41. [Google Scholar] [CrossRef] [PubMed]
- Mons, U.; Nagelhout, G.E.; Allwright, S.; Guignard, R.; van den Putte, B.; Willemsen, M.C.; Fong, G.T.; Brenner, H.; Pötschke-Langer, M.; Breitling, L.P. Impact of national smoke-free legislation on home smoking bans: Findings from the International Tobacco Control Policy Evaluation Project Europe Surveys. Tob. Control 2013, 22, e2–e9. [Google Scholar] [CrossRef] [PubMed]
- Cheng, K.-W.; Glantz, S.A.; Lightwood, J.M. Association between smokefree laws and voluntary smokefree-home rules. Am. J. Prev. Med. 2011, 41, 566–572. [Google Scholar] [CrossRef] [PubMed]
- Cheng, K.-W.; Okechukwu, C.A.; McMillen, R.; Glantz, S.A. Association between clean indoor air laws and voluntary smokefree rules in homes and cars. Tob. Control 2015, 24, 168–174. [Google Scholar] [CrossRef] [PubMed]
- Dove, M.S.; Dockery, D.W.; Connolly, G.N. Smoke-free air laws and secondhand smoke exposure among nonsmoking youth. Pediatrics 2010, 126, 80–87. [Google Scholar] [CrossRef] [PubMed]
- Yong, H.-H.; Foong, K.; Borland, R.; Omar, M.; Hamann, S.; Sirirassamee, B.; Fong, G.T.; Fotuhi, O.; Hyland, A. Support for and reported compliance among smokers with smoke-free policies in air-conditioned hospitality venues in Malaysia and Thailand: Findings from the International Tobacco Control Southeast Asia Survey. Asia. Pac. J. Public Health 2010, 22, 98–109. [Google Scholar] [CrossRef] [PubMed]
| Central Tendency | Active Smoker Density | Active Smokers Present | Children Present | Non-Smoking Adults Present | ||||
|---|---|---|---|---|---|---|---|---|
| Ramadan | Post-Ramadan | Ramadan | Post- Ramadan | Ramadan | Post- Ramadan | Ramadan | Post- Ramadan | |
| Mean (SD) | 0.21 (0.22) | 0.17 (0.17) | 11.9 (12.4) | 8.0 (10.8) | 4.5 (4.6) | 3.3 (4.5) | 35.6 (22.5) | 30.7 (24.6) |
| Median (IQR) | 0.13 (0.18) | 0.11 (0.16) | 8.0 (11.3) | 6.0 (8.0) | 3.0 (6.8) | 2.0 (4.0) | 31.0 (28.8) | 22.0 (32.3) |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Luntungan, N.H.W.; Byron, M.J.; Hovell, M.F.; Rosen, L.J.; Anggraeni, A.; Rees, V.W. Children’s Exposure to Secondhand Smoke during Ramadan in Jakarta, Indonesia. Int. J. Environ. Res. Public Health 2016, 13, 952. https://doi.org/10.3390/ijerph13100952
Luntungan NHW, Byron MJ, Hovell MF, Rosen LJ, Anggraeni A, Rees VW. Children’s Exposure to Secondhand Smoke during Ramadan in Jakarta, Indonesia. International Journal of Environmental Research and Public Health. 2016; 13(10):952. https://doi.org/10.3390/ijerph13100952
Chicago/Turabian StyleLuntungan, Nurul (Nadia) H.W., M. Justin Byron, Melbourne F. Hovell, Laura J. Rosen, Annisa Anggraeni, and Vaughan W. Rees. 2016. "Children’s Exposure to Secondhand Smoke during Ramadan in Jakarta, Indonesia" International Journal of Environmental Research and Public Health 13, no. 10: 952. https://doi.org/10.3390/ijerph13100952







