Community Knowledge and Acceptance of Larviciding for Malaria Control in a Rural District of East-Central Tanzania
Abstract
:1. Introduction
2. Experimental Section
2.1. Study Area and Sampling
2.2. Data Collection
2.2.1. Quantitative Data
2.2.2. Qualitative Data
2.3. Ethical Considerations
2.4. Data Analysis
3. Results and Discussion
3.1. Qualitative Results
3.2. Quantitative Results
3.2.1. Socio-Demographic Characteristic of Respondents
| Variable | Response | Value |
|---|---|---|
| Sex | Male | 54.0% |
| Female | 46.0% | |
| Age (years) | Mean | 36.8 years (SD 11.9) |
| Education level | Ever attended school: | |
| Yes | 78.7% | |
| No | 21.3% | |
| Highest level attended: | ||
| Pre-primary | 0.5% | |
| Primary | 89.4% | |
| Secondary | 8.9% | |
| Higher | 1.2% | |
| Household characteristics | Mean number of people | 5.6 people (SD 2.2) |
| Mean number of children under 5 | 1.3 children (SD 0.7) | |
| Wealth Indicators - Own a: | Motorcycle/scooter | 8.8% |
| Bicycle | 74.3% | |
| Sewing machine | 8.2% | |
| Radio | 74.2% | |
| Television set | 6.4% | |
| Sofa | 19.7% | |
| Mobile phone | 65.5% | |
| Rooms in compound | 1 room | 8.6% |
| 2–3 rooms | 61.0% | |
| 4+ rooms | 30.4% | |
| House/land ownership | Owns house | 85.0% |
| Owns land | 70.9% |
3.2.2. Knowledge, Attitudes, and Practices Regarding Malaria and Larviciding
| Variable | Percentage |
|---|---|
| General Malaria Knowledge | |
| Knowledge that mosquitoes transmit malaria | 94.8% |
| Perception that there are mosquitoes in the respondent’s community | 99.1 |
| Knowledge of factors affecting mosquito population | |
| Rainfall | 21.2 |
| Stagnant water | 67.8 |
| Cleanliness of village/surroundings | 67.5 |
| Humidity | 6.5 |
| Knowledge of where mosquito larvae are found | |
| Stagnant water/irrigation ditches | 69.9 |
| Forest | 15.3 |
| Pit latrine | 7.7 |
| Vegetation around the house | 13.7 |
| Don’t know | 23.3 |
| Malaria Vector Control | |
| Knowledge that reducing mosquito population can help reduce malaria | 90.0 |
| Mention of actions that can reduce mosquito abundance | |
| Drain stagnant water | 35.4 |
| Clearing grass/bushes around home | 28.1 |
| Spray insecticides | 7.7 |
| Use larvicides | 8.4 |
| Clean environment around home | 59.9 |
| Use bed nets | 50.3 |
| Mention of actions that can reduce mosquito larvae abundance | |
| Drain stagnant water around home | 43.1 |
| Clearing grass/bushes around home | 18.8 |
| Use larvicides | 16.7 |
| Clean environment around home | 41.4 |
| Don’t Know | 25.9 |
| Variable | Percentage Responding Yes |
|---|---|
| Knowledge of larviciding | 17.8 |
| Trust in safety of larvicide | 73.1 |
| Permission for program to apply larvicide in bodies of water near home | 92.9 |
| Confidence that larviciding will reduce number of mosquitoes | 92.3 |
| Confidence that larviciding will reduce risk of getting malaria | 91.9 |
| Response | Very Likely | Likely | Neutral | Not Likely | Very Unlikely |
|---|---|---|---|---|---|
| Likelihood that larvicide is safe for humans and animals | 20.4% | 46.4% | 26.4% | 6.8% | 0.0% |
| Likelihood that larviciding will reduce number of mosquitoes | 18.2% | 46.7% | 26.8% | 8.2% | 0.1% |
| Likelihood that larviciding will reduce risk of malaria infection | 15.7% | 49.2% | 26.8% | 8.3% | 0.0% |
3.2.3. Willingness to Pay for a Larviciding Program
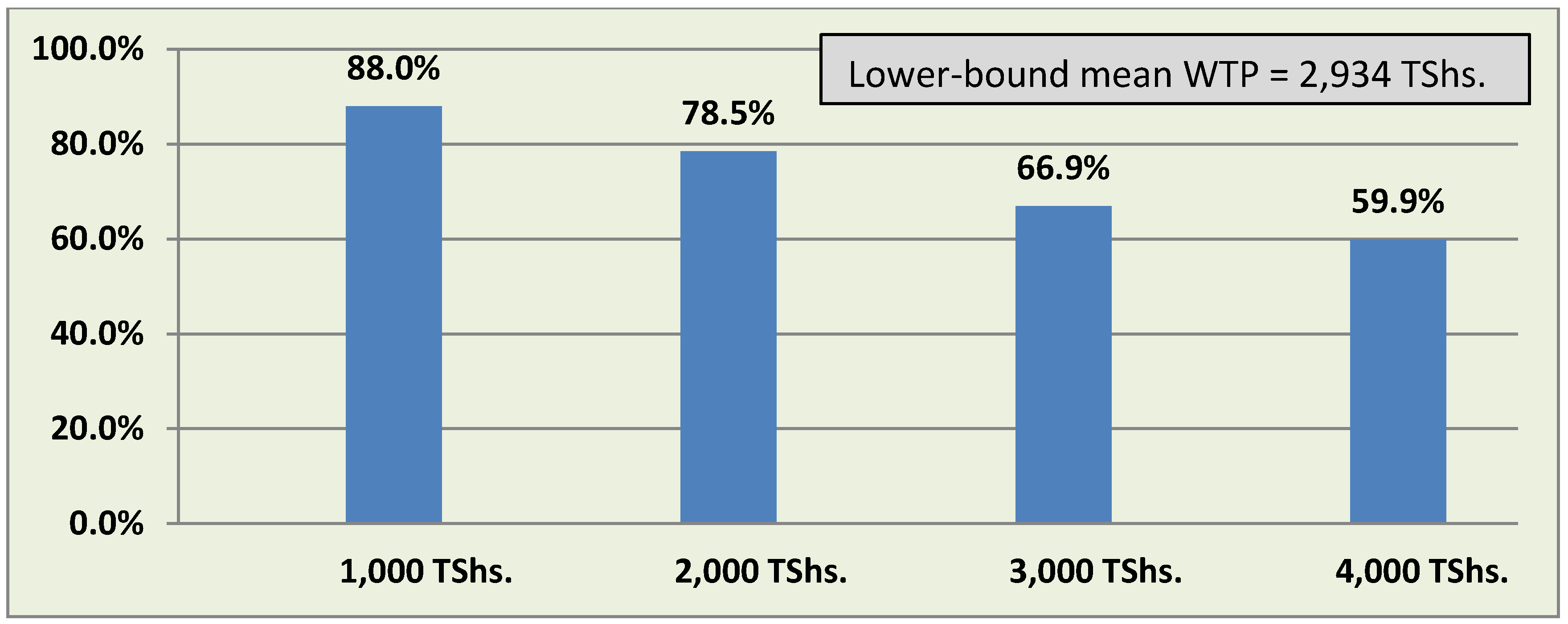
3.2.4. Regression Analysis
| Variable Type | Variable | Coefficient | 95% CI | z | p-Value |
|---|---|---|---|---|---|
| Demographics | Respondent age | −0.003 | −0.012–0.005 | −0.78 | 0.434 |
| Respondent ever attended school | 0.449 | 0.213–0.685 | 3.73 | 0.000 * | |
| Number of people in the household | 0.027 | −0.020–0.075 | 1.12 | 0.262 | |
| Respondent’s main occupation–crop farming | −0.122 | −0.391–0.148 | −0.88 | 0.377 | |
| Wealth | Improved roof (iron sheets instead of grass/leaves/mud) | 0.309 | 0.104–0.514 | 2.96 | 0.003 * |
| Reported malaria | ≥1 recent case of self-reported malaria in household (assessment of each member’s most recent fever if within past 3 months) | −0.048 | −0.252–0.155 | −0.47 | 0.641 |
| Attitudes towards larviciding | Trust in safety of larviciding | 0.350 | 0.107–0.593 | 2.82 | 0.005 * |
| Bid | Larviciding contribution amount | −0.340 | −0.429–−0.250 | −7.42 | 0.000 * |
3.3. Discussion
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization (WHO). World Malaria Report 2013; WHO: Geneva, Switzerland, 2013. [Google Scholar]
- Majambere, S.; Lindsay, S.W.; Green, C.; Kandeh, B.; Fillinger, U. Microbial larvicides for malaria control in The Gambia. Malar. J. 2007, 6, 76. [Google Scholar] [CrossRef]
- Fehn, C.F.; Carmichael, G.T.; Elmore, C.M.; Taylor, J.W. Operational experiences with Paris Green pellets in mosquito control. Mosq. News 1959, 19, 238–243. [Google Scholar]
- Walker, K.; Lynch, M. Contributions of Anopheles larval control to malaria suppression in tropical Africa: Review of achievements and potential. Med. Vet. Entomol. 2007, 21, 2–21. [Google Scholar] [CrossRef]
- Fillinger, U.; Ndenga, B.; Githeko, A.; Lindsay, S.W. Integrated malaria vector control with microbial larvicides and insecticide-treated nets in western Kenya: A controlled trial. Bull. World Health Org. 2009, 87, 655–665. [Google Scholar] [CrossRef]
- Magesa, S.M.; Athumani, Y.; Barongo, V.; Sambu, E.Z.; Senkoro, K.P.; Mboera, L.E.G.; Sandra, M.R.; Reynaldo, G.V.; Aramis, R.G.; Kitua, A.Y. Efficacy of Bacillus Thuringiensis var. Israelensis (Bactivec®) and Bacillus Sphaericus (Griselesf®) for Control of Mosquito Larvae: A Field Trial in Mvomero and Bagamoyo Districts, Tanzania; National Institute for Medical Research: Dar es Salaam, Tanzania, 2009. [Google Scholar]
- Fillinger, U.; Lindsay, S.W. Suppression of exposure to malaria vectors by an order of magnitude using microbial larvicides in rural Kenya. Trop. Med. Int. Health 2006, 11, 1629–1642. [Google Scholar] [CrossRef]
- Eder, E.; Schonbrunner, I. Toxicity of Bacillus thuringiensis israelensis on the nontarget organisms Triops cancriformis, Branchipus schaefferi, Leptestheria dahalacensis (crustacea: Branchiopoda: Notostraca, anostraca, spinicaudata). Open Environ. Poll. Toxicol. J. 2010, 2, 16–20. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Larval Source Management: A Supplementary Measure for Malaria Vector Control; WHO: Geneva, Switzerland, 2013. [Google Scholar]
- Killeen, G.; Fillinger, U.; Knols, B.G. Advantages of larval control for African malaria vectors: Low mobility and behavioural responsiveness of immature mosquito stages allow high effective coverage. Malar. J. 2002, 1. [Google Scholar] [CrossRef]
- Ministry of Health and Social Welfare (MoHSW). Medium Term Malaria Strategic Plan, 2008–2013; Ministry of Health and Social Welfare, Ed.; MoHSW: Dar es Salaam, Tanzania, 2008. [Google Scholar]
- Devine, G.J.; Killeen, G.F. The potential of a new larviciding method for the control of malaria vectors. Malar. J. 2010, 9, 1–4. [Google Scholar] [CrossRef]
- Geissbühler, Y.; Kannady, K.; Chaki, P.P.; Emidi, B.; Govella, N.J.; Mayagaya, V.; Kiama, M.; Mtasiwa, D.; Mshinda, H.; Lindsay, S.W.; et al. Microbial larvicide application by a large-scale, community-based program reduces malaria infection prevalence in urban Dar es Salaam, Tanzania. PLoS One 2009, 4. [Google Scholar] [CrossRef]
- Chaki, P.P.; Govella, N.J.; Shoo, B.; Hemed, A.; Tanner, M.; Fillinger, U.; Killeen, G.F. Achieving high coverage of larval-stage mosquito surveillance: Challenges for a community-based mosquito control programme in urban Dar es Salaam, Tanzania. Malar. J. 2009, 8. [Google Scholar] [CrossRef]
- Fillinger, U.; Kannady, K.; William, G.; Vanek, M.J.; Dongus, S.; Nyika, D.; Geissbuhler, Y.; Chaki, P.P.; Govella, N.J.; Mathenge, E.M.; et al. A tool box for operational mosquito larval control: Preliminary results and early lessons from the urban malaria control programme in Dar es Salaam, Tanzania. Malar. J. 2008, 7. [Google Scholar] [CrossRef]
- Mukabana, W.; Kannady, K.; Kiama, G.M.; Ijumba, J.; Mathenge, E.; Kiche, I.; Nkwengulila, G.; Mboera, L.; Mtasiwa, D.; Yamagata, Y.; et al. Ecologists can enable communities to implement malaria vector control in Africa. Malar. J. 2006, 5. [Google Scholar] [CrossRef]
- Mboera, L.E.G.; Mlozi, M.R.S.; Senkoro, K.P.; Rwegoshora, R.T.; Rumisha, S.F.; Mayala, S.F.; Shayo, E.H.; Senkondo, E.; Mutayoba, B.; Mwingira, V.; et al. Malaria and Agriculture in Tanzania: Impact of Land-Use and Agricultural Practices on Malaria Burden in Mvomero District; Tanzania National Institute for Medical Research: Dar es Salaam, Tanzania, 2007; ISBN 978-9987-9143-1-9. [Google Scholar]
- Mboera, L.E.G.; Senkoro, K.P.; Mayala, B.K.; Rumisha, S.F.; Rwegoshora, R.T.; Mlozi, M.R.S.; Shayo, E.H. Spatio-temporal variation in malaria transmission intensity in five agro-ecosystems in Mvomero district, Tanzania. Geospat. Health 2010, 4, 167–178. [Google Scholar]
- Mboera, L.E.G.; Shayo, E.H.; Senkoro, K.P.; Rumisha, S.F.; Mlozi, M.R.S.; Mayala, B.K. Knowledge, perceptions and practices of farming communities on linkages between malaria and agriculture. Acta Trop. 2009, 113, 139–144. [Google Scholar]
- Dickinson, K.; Randell, H.; Kramer, R.; Shayo, E. Summary of Findings from June 2007 Fieldwork in Mvomero District, Tanzania; Nicholas School of the Environment, Duke University: Durham, NC, USA, 2007. [Google Scholar]
- Brouwer, R.; Bateman, I.J. Benefits transfer of willingness to pay estimates and functions for health risk reductions: A cross country study. J. Health Econ. 2005, 24, 591–611. [Google Scholar] [CrossRef]
- Turnbull, B. The empirical distribution function with arbitrary grouped, censored, and truncated data. J. R. Stat. Soc. 1976, 38, 290–295. [Google Scholar]
- Carson, R.T.; Hanemann, W.M.; Kopp, R.J.; Krosnick, J.A.; Mitchell, R.C.; Presser, S.; Rudd, P.A.; Smith, V.K. Prospective Interim Lost Use Value Due to DDT and PCB Contamination in the Southern California Bight; The National Oceanic and Atmospheric Administration: Silver Spring, MD, USA, 1994. [Google Scholar]
- Castro, M.C.; Yamagata, Y.; Mtasiwa, D.; Tanner, M.; Utzinger, J.; Keiser, J.; Singer, B.H. Integrated urban malaria control: A case study in Dar es Salaam, Tanzania. Am. J. Trop. Med. Hyg. 2004, 71, 103–117. [Google Scholar]
- Maheu-Giroux, M.; Castro, M.C. Impact of community-based larviciding on the prevalence of malaria infection in Dar es Salaam, Tanzania. PLoS One 2013, 8. [Google Scholar] [CrossRef]
- Mboera, L.E.G.; Mazigo, H.D.; Rumisha, S.F.; Kramer, R.A. Towards malaria elimination and its implication for vector control, disease management, and livelihoods in Tanzania. Malar. World J. 2013, 4, 1–14. [Google Scholar]
- Keiser, J.; Singer, B.H.; Utzinger, J. Reducing the burden of malaria in different eco-epidemiological settings with environmental management: A systematic review. Lancet Infect. Dis. 2005, 5, 695–708. [Google Scholar] [CrossRef]
- Fillinger, U.; Knols, B.G.; Becker, N. Efficacy and efficiency of new Bacillus thuringiensis var israelensis and Bacillus sphaericus formulations against Afrotropical anophelines in western Kenya. Trop. Med. Int. Health 2003, 8, 37–47. [Google Scholar] [CrossRef]
- Shililu, J.I.; Tewolde, G.M.; Brantly, E.; Githure, J.I.; Mbogo, C.M.; Beier, J.C.; Fusco, R.; Novak, R.J. Efficacy of Bacillus thuringiensis israelensis, Bacillus sphaericus and Temephos for managing Anopheles larvae in Eritrea. J. Am. Mosq. Control Assoc. 2003, 19, 251–258. [Google Scholar]
- Mboera, L.E.G.; Mlozi, M.R.S.; Rumisha, S.F.; Bwana, V.M.; Malima, R.C.; Shayo, E.H.; Mayala, B.K.; Mlacha, T.; Nguruwe, R. Malaria, Ecosystems and Livelihoods in Kilosa District, Central Tanzania; National Institute for Medical Research: Dar es Salaam, Tanzania, 2013. [Google Scholar]
- Reddy, M.R.; Overgaard, H.J.; Abaga, S.; Reddy, V.P.; Caccone, A.; Kiszewski, A.E.; Slotman, M.A. Outdoor host seeking behaviour of Anopheles gambiae mosquitoes following initiation of malaria vector control on Bioko Island, Equatorial Guinea. Malar. J. 2011, 10. [Google Scholar] [CrossRef]
- Trapero-Bertran, M.; Mistry, H.; Shen, J.; Fox-Rushby, J. A systematic review and meta-analysis of willingness-to-pay values: The case of malaria control interventions. Health Econ. 2013, 22, 428–450. [Google Scholar] [CrossRef]
- Onwujekwe, O.; Malik, M.E.; Mustafa, S.H.; Mnzava, A. Socio-economic inequity in demand for insecticide-treated nets, in-door residual house spraying, larviciding and fogging in Sudan. Malar. J. 2005, 4. [Google Scholar] [CrossRef]
- Rogers, E.; Shoemaker, F.F. Communication of Innovations: A Cross-Cultural Approach; Free Press: New York, NY, USA, 1971. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Mboera, L.E.G.; Kramer, R.A.; Miranda, M.L.; Kilima, S.P.; Shayo, E.H.; Lesser, A. Community Knowledge and Acceptance of Larviciding for Malaria Control in a Rural District of East-Central Tanzania. Int. J. Environ. Res. Public Health 2014, 11, 5137-5154. https://doi.org/10.3390/ijerph110505137
Mboera LEG, Kramer RA, Miranda ML, Kilima SP, Shayo EH, Lesser A. Community Knowledge and Acceptance of Larviciding for Malaria Control in a Rural District of East-Central Tanzania. International Journal of Environmental Research and Public Health. 2014; 11(5):5137-5154. https://doi.org/10.3390/ijerph110505137
Chicago/Turabian StyleMboera, Leonard E. G., Randall A. Kramer, Marie Lynn Miranda, Stella P. Kilima, Elizabeth H. Shayo, and Adriane Lesser. 2014. "Community Knowledge and Acceptance of Larviciding for Malaria Control in a Rural District of East-Central Tanzania" International Journal of Environmental Research and Public Health 11, no. 5: 5137-5154. https://doi.org/10.3390/ijerph110505137
APA StyleMboera, L. E. G., Kramer, R. A., Miranda, M. L., Kilima, S. P., Shayo, E. H., & Lesser, A. (2014). Community Knowledge and Acceptance of Larviciding for Malaria Control in a Rural District of East-Central Tanzania. International Journal of Environmental Research and Public Health, 11(5), 5137-5154. https://doi.org/10.3390/ijerph110505137




