The Health Heterogeneity of and Health Care Utilization by the Elderly in Taiwan
Abstract
:1. Introduction
2. Universal National Health Insurance (NHI) In Taiwan
3. The Concept of Health Heterogeneity and Health Profile Identification
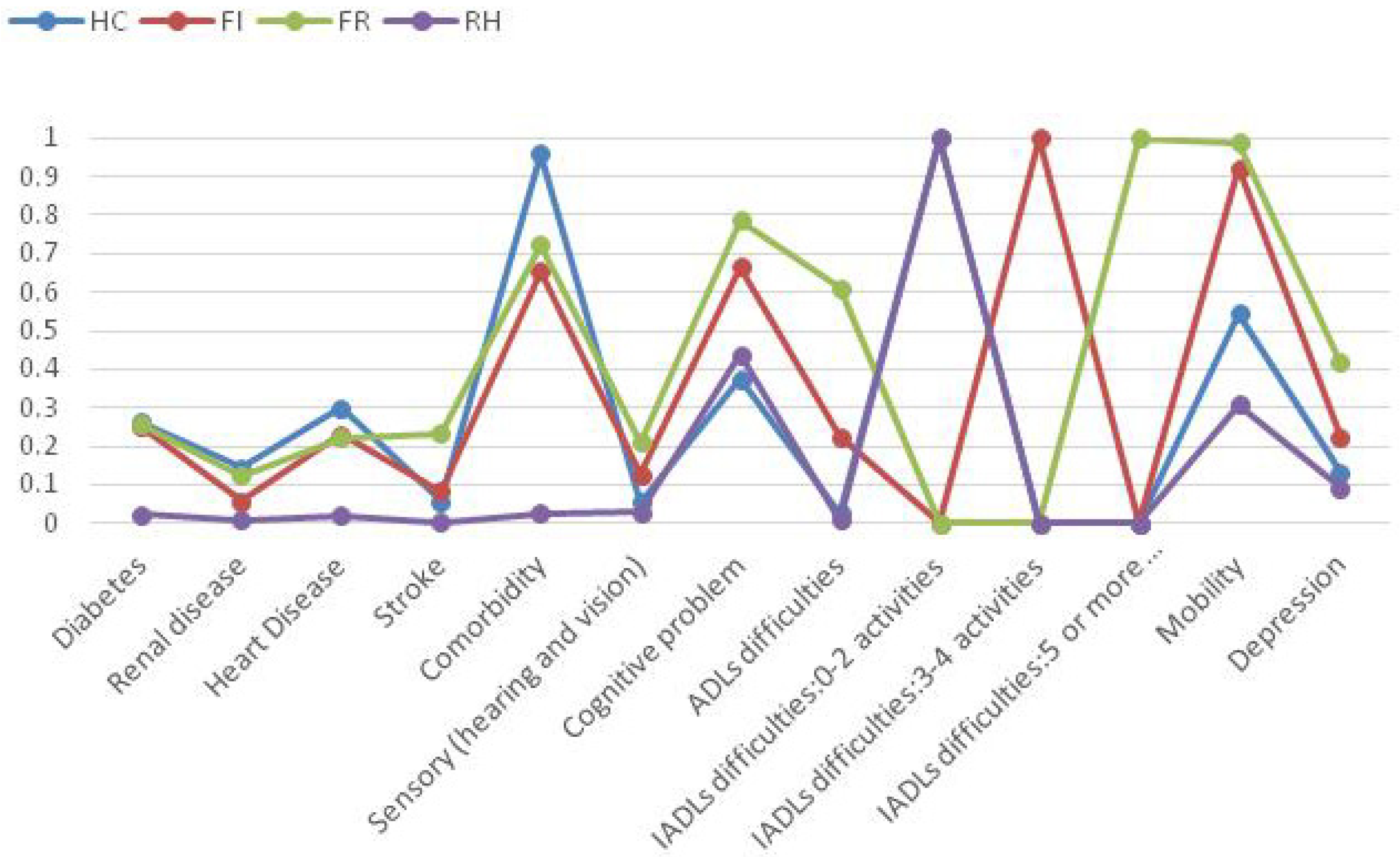
4. Socio-Demographic and Economic Determinants of Health Heterogeneity
5. The Effect of Health Profiles on Utilization of Health Care Services

6. Healthcare Expenditures in Each Health Profile, by Age and Gender
7. Other Factors Associated With Health Care Expenditures in the Health Behavior Model
8. Future Research
9. Conclusions
Acknowledgments
Conflicts of Interest
References
- Ministry of the interior. General Population Profile of Taiwan; Ministry of the Interior: Taipei, Taiwan, 2012.
- Huber, M.; Knottnerus, J.A.; Green, L.; van der Horst, H.; Jadad, A.R.; Kromhout, D.; Smid, H. How should we define health? BMJ 2011, 343. [Google Scholar] [CrossRef]
- Integrative Medicine and Patient-Centered Care. Available online: http://www.iom.edu/~/media/Files/Activity%20Files/Quality/IntegrativeMed/Integrative%20Medicine%20and%20Patient%20Centered%20Care.pdf (accessed on 28 October 2013).
- World Health Organization (WHO). Active Aging: A Policy Framework; WHO: Geneva, Switzerland, 2002. [Google Scholar]
- Pourbohloul, B.; Kieny, M.P. Complex systems analysis: Towards holistic approaches to health system planning and policy. Bull. World Health Organ. 2011, 89. [Google Scholar] [CrossRef]
- Muthen, L.K.; Muthen, B. Mplus: User’s Guide, version 7.0. Statistical analysis with latent variables. Muthen & Muthen: Los Angeles, LA, USA, 2012. [Google Scholar]
- Funderburk, J.S.; Maisto, S.A.; Sugarman, D.E.; Wade, M. The covariation of multiple risk factors in primary care: A latent class analysis. J. Behav. Med. 2008, 31, 525–535. [Google Scholar] [CrossRef]
- The National Health Insurance Statistics. 2011. Available online: http://www.nhi.gov.tw/english/index.aspx (accessed on 21 October 2013).
- Lin, M.H.; Liu, C.L.; Peng, L.N.; Chen, Y.T.; Chen, L.K. Demographic characteristics and clinical benefits of outpatient geriatric evaluation and management service in Taiwan. Arch. Gerontol. Geriatr. 2012, 55, 42–44. [Google Scholar] [CrossRef]
- National Health Insurance Research Database (2011). Available online: http://nhird.nhri.org.tw/ (accessed on 21 October 2013).
- Chen, L.; Yip, W.; Chang, M.C.; Lin, H.S.; Lee, S.D.; Chiu, Y.L.; Lin, Y.H. The effects of Taiwan’s National Health Insurance on access and health status of the elderly. Health Econ. 2007, 16, 223–242. [Google Scholar] [CrossRef]
- Chang, H.J.; Huang, S.C.; Chiang, T.P. Concentration of health care expenditures in Taiwan—Analysis of patient’s characteristics. Taiwan J. Public Health 2002, 21, 207–213. [Google Scholar]
- Ministry of Health and Welfare. Ten Year Long term Care Plan; Ministry of Health and Welfare: Taipei, Taiwan, 2012. Available online: http://sowf.moi.gov.tw/newpage/tenyearsplan.htm (accessed on 28 October 2013).
- Lafortune, L.; Beland, F.; Bergman, H.; Ankri, J. Health state profiles and service utilization in community-living elderly. Med. Care 2009, 47, 286–294. [Google Scholar] [CrossRef]
- Nie, J.X.; Wang, L.; Tracy, C.S.; Moineddin, R.; Upshur, R.E. Health care service utilization among the elderly: Findings from the Study to Understand the Chronic Condition Experience of the Elderly and the Disabled (SUCCEED project). J. Eval. Clin. Pract. 2008, 14, 1044–1049. [Google Scholar] [CrossRef]
- Wang, Y.T.; Teng, C.S. Need Assessment of Long-Term Care in Taiwan; Council for Economic Planning and Developmen: Taipei, Taiwan, 2009. [Google Scholar]
- Ministry of the interior. 2009 Report of the Senior Citizen Condition Survey; Ministry of the interior: Taipei, Taiwan, 2010.
- Olshansky, S.J.; Carnes, B.A. Ageing and health. Lancet 2010, 375, 26–27. [Google Scholar]
- Liu, L.F.; Tian, W.H.; Yao, H.P. Utilization of health care services by elderly people with National Health Insurance in Taiwan: The heterogeneous health profile approach. Health Policy 2012, 108, 246–255. [Google Scholar] [CrossRef]
- Knesebeck, O.; Luschen, G.; Cockerham, W.C.; Siegrist, J. Socioeconomic status and health among the aged in the United States and Germany: A comparative cross-sectional study. Soc. Scie. Med. 2003, 57, 1643–1652. [Google Scholar] [CrossRef]
- Huisman, M.; Kunst, A.E.; Mackenbach, J.P. Socioeconomic inequalities in morbidity among the elderly; A European overview. Soc. Sci. Med. 2003, 57, 861–873. [Google Scholar] [CrossRef]
- Schafer, I.; Hansen, H.; Schon, G.; Hofels, S.; Altiner, A.; Dahlhaus, A.; Gensichen, J.; Riedel-Heller, S.; Weyerer, S.; Blank, W.A.; et al. The influence of age, gender and socio-economic status on multimorbidity patterns in primary care. First results from the multicare cohort study. BMC Health Serv. Res. 2012, 12. [Google Scholar] [CrossRef]
- Gonzalez-Gonzalez, C.; Sanchez-Garcia, S.; Juarez-Cedillo, T.; Rosas-Carrasco, O.; Gutierrez-Robledo, L.M.; Garcia-Pena, C. Health care utilization in the elderly Mexican population: Expenditures and determinants. BMC Public Health 2011, 11. [Google Scholar] [CrossRef]
- Zunzunegui, M.V.; Alvarado, B.E.; Beland, F.; Vissandjee, B. Explaining health differences between men and women in later life: A cross-city comparison in Latin America and the Caribbean. Soc. Sci. Med. 2009, 68, 235–242. [Google Scholar] [CrossRef]
- Sonnenberg, C.M.; Beekman, A.T.; Deeg, D.J.; van Tilburg, W. Sex differences in late-life depression. Acta Psychiatr. Scand. 2000, 101, 286–292. [Google Scholar]
- Rahman, O.; Menken, J.; Kuhn, R. The impact of family members on the self-reported health of older men and women in a rural area of Bangladesh. Ageing Soc. 2004, 24, 903–920. [Google Scholar] [CrossRef]
- Dalstra, J.A.; Kunst, A.E.; Mackenbach, J.P.; EU Working Group on Socioeconomic Inequalities in Health. A comparative appraisal of the relationship of education, income and housing tenure with less than good health among the elderly in Europe. Soc. Sci. Med. 2006, 62, 2046–2060. [Google Scholar] [CrossRef]
- Portes, A. Social capital: Its origins and applications in modern sociology. Ann. Rev. Sociol. 1998, 24, 1–24. [Google Scholar] [CrossRef]
- Goldman, N.; Cornman, J.C.; Chang, M.C. Subjective Social Status: Evaluation of A New Instrument. In Presented at the Annual Meeting of the Population Association of America, Minneapolis, MN, USA, 2003.
- Hu, P.; Adler, N.E.; Goldman, N.; Weinstein, M.; Seeman, T.E. Relationship between subjective social status and measures of health in older Taiwanese persons. J. Am. Geriatr. Soc. 2005, 53, 483–488. [Google Scholar] [CrossRef]
- Kennedy, B.P.; Kawachi, I.; Glass, R.; Prothrow-Stith, D. Income distribution, socioeconomic status, and self rated health in the United States: Multilevel analysis. BMJ 1998, 317, 917–921. [Google Scholar]
- Kharicha, K.; Iliffe, S.; Harari, D.; Swift, C.; Gillmann, G.; Stuck, A.E. Health risk appraisal in older people 1: Are older people living alone an “at-risk” group? Br. J. Gen. Pract. 2007, 57, 271–276. [Google Scholar]
- Van Gelder, B.M.; Tijhuis, M.; Kalmijn, S.; Giampaoli, S.; Nissinen, A.; Kromhout, D. Marital status and living situation during a 5-year period are associated with a subsequent 10-year cognitive decline in older men: The FINE Study. J. Gerontol. B Psychol. Sci. Soc. Sci. 2006, 61, 213–219. [Google Scholar] [CrossRef]
- Li, L.W.; Zhang, J.; Liang, J. Health among the oldest-old in China: Which living arrangements make a difference? Soc. Sci. Med. 2009, 68, 220–227. [Google Scholar] [CrossRef]
- Williams, K.; Umberson, D. Marital status, marital transitions, and health: a gendered life course perspective. J. Health Soc. Behav. 2004, 45, 81–98. [Google Scholar] [CrossRef]
- Michael, Y.L.; Berkman, L.F.; Colditz, G.A.; Kawachi, I. Living arrangements, social integration, and change in functional health status. Am. J. Epidemiol. 2001, 153, 123–131. [Google Scholar] [CrossRef]
- Hughes, M.E.; Waite, L.J. Health in household context: Living arrangements and health in late middle age. J. Health Soc. Behav. 2002, 43, 1–21. [Google Scholar] [CrossRef]
- Lund, R.; Due, P.; Modvig, J.; Holstein, B.E.; Damsgaard, M.T.; Andersen, P.K. Cohabitation and marital status as predictors of mortality-an eight year follow-up study. Soc. Sci Med. 2002, 55, 673–679. [Google Scholar] [CrossRef]
- Grossman, M. On the concept of health capital and the demand for health. J. Polit. Econ. 1972, 80, 223–255. [Google Scholar]
- Mirowsky, J.; Ross, C.E. Education, learned effectiveness and health. Lond. Rev. Educ. 2005, 3, 205–220. [Google Scholar] [CrossRef]
- Adler, N.E.; Newman, K. Socioeconomic disparities in health: Pathways and policies. Health Aff. 2002, 21, 60–76. [Google Scholar] [CrossRef]
- Backlund, E.; Sorlie, P.D.; Johnson, N.J. The shape of the relationship between income and mortality in the United States: Evidence from the National Longitudinal Mortality Study. Ann. Epidemiol. 1996, 6, 12–20. [Google Scholar] [CrossRef]
- Ecob, R.; Smith, G.D. Income and health: What is the nature of the relationship? Soc. Sci. Med. 1999, 48, 693–705. [Google Scholar] [CrossRef]
- Coleman, J. Foundations of Social Theory; Harvard University Press: Cambridge, MA, USA, 1990. [Google Scholar]
- Woolcock, M. Social capital and economic development: Toward a theoretical synthesis and policy framework. Theory Soc. 1998, 27, 151–208. [Google Scholar] [CrossRef]
- Andersen, R.M. Revisiting the behavioral model and access to medical care: Does it matter? J. Health Soc. Behav. 1995, 36, 1–10. [Google Scholar] [CrossRef]
- Phillips, K.A.; Morrison, K.R.; Andersen, R.M.; Aday, L.A. Understanding the context ofhealth carehealth care utilization: Assessing environmental and provider-related variables in the behavioral model of utilization. Health Serv. Res. 1998, 33, 571–596. [Google Scholar]
- McNamee, P. A comparison of the grade of membership measure with alternative health indicators in explaining costs for older people. Health Econ. 2004, 13, 379–395. [Google Scholar] [CrossRef]
- Olshansky, S.J.; Perry, D.; Miller, R.A.; Butler, R.N. In pursuit of the longevity dividend. Scientist 2006, 20, 28–36. [Google Scholar]
- Fried, L.P.; Ferrucci, L.; Darer, J.; Williamson, J.D.; Anderson, G. Untangling the concepts of disability, frailty, and comorbidity: Implications for improved targeting and care. J. Gerontol. A Biol. Sci. Med. Sci. 2004, 59, 255–263. [Google Scholar] [CrossRef]
- Fried, T.R.; Bradley, E.H.; Williams, C.S.; Tinetti, M.E. Functional disability and health care expenditures for older persons. Arch. Intern. Med. 2001, 161, 2602–2607. [Google Scholar] [CrossRef]
- Mao, C.H. Social Support and Health Services Utilization among the Community Elderly in Miaoli, Taiwan, in Institute of health care Health Care Administration; ASIA University: Taichung, Taiwan, 2006. [Google Scholar]
- Chen, M.C. Decade Trend of Health Care Services Utilization among Population Aged over 40 in Taiwan Area, in Institute of Long-Term Care; ASIA University: Taichung, Taiwan, 2008. [Google Scholar]
- Xu, X.; Patel, D.A.; Vahratian, A.; Ransom, S.B. Insurance coverage and health care use among near-elderly women. Womens Health Issues 2006, 16, 139–148. [Google Scholar] [CrossRef]
- Schellhorn, M.; Stuck, A.E.; Minder, C.E.; Beck, J.C. Health services utilization of elderly Swiss: Evidence from panel data. Health Econ. 2000, 9, 533–545. [Google Scholar] [CrossRef]
- US Census Bureau. Statistical Abstract of the United States: 2010, 129th ed.Claitor’s Publishing Division: Los Angeles, LA, USA, 2010.
- De Meijer, C.A.; Koopmanschap, M.A.; d’Uva, T.B.; van Doorslaer, E. Determinants of long-term care spending: Age, time to death or disability? J. Health Econ. 2011, 30, 425–438. [Google Scholar] [CrossRef]
- Werblow, A.; Felder, S.; Zweifel, P. Population ageing and health care expenditure: A school of “red herrings”? Health Econ. 2007, 16, 1109–1126. [Google Scholar] [CrossRef]
- Comas-Herrera, A.; Wittenberg, R.; Pickard, L.; Knapp, M. Cognitive impairment in older people: Future demand for long-term care services and the associated costs. Int. J. Geriatr. Psych. 2007, 22, 1037–1045. [Google Scholar] [CrossRef] [Green Version]
- Yang, Z.; Norton, E.C.; Stearns, S.C. Longevity and health care expenditures: the real reasons older people spend more. J. Gerontol. B Psychol. Sci. Soc. Sci. 2003, 58, S2–S10. [Google Scholar] [CrossRef]
- Yoo, B.K.; Bhattacharya, J.; McDonald, K.M.; Garber, A.M. Impacts of informal caregiver availability on long-term care expenditures in OECD countries. Health Serv. Res. 2004, 39, 1971–1992. [Google Scholar] [CrossRef]
- Tsai, W.D.; Kan, K. Living arrangement and medical service utilization: evidence from Taiwan. In Presented at 2007 Annual Conference Information Wisconsin Economics Association Annual Conference, Wisconsin, WI, USA, 2007.
- Coughlin, T.A.; McBride, T.D.; Perozek, M.; Liu, K. Home care for the disabled elderly: Predictors and expected costs. Health Serv. Res. 1992, 27, 453–479. [Google Scholar]
- Lee, P.S. Determinants of Medical Services Utilization among Community Elderly, in Department of Public Health; Kaohsiung Medical University: Kaohsiung, Taiwan, 2003. [Google Scholar]
- De Meijer, C.A.; Koopmanschap, M.A.; Koolman, X.H.; van Doorslaer, E.K. The role of disability in explaining long-term care utilization. Med. Care 2009, 47, 1156–1163. [Google Scholar] [CrossRef]
- Crimmins, E.M. Trends in the health of the elderly. Annu. Rev. Public Health 2004, 25, 79–98. [Google Scholar] [CrossRef]
- Parker, M.G.; Thorslund, M. Health trends in the elderly population: Getting better and getting worse. Gerontologist 2007, 47, 150–158. [Google Scholar] [CrossRef]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Liu, L.-F. The Health Heterogeneity of and Health Care Utilization by the Elderly in Taiwan. Int. J. Environ. Res. Public Health 2014, 11, 1384-1397. https://doi.org/10.3390/ijerph110201384
Liu L-F. The Health Heterogeneity of and Health Care Utilization by the Elderly in Taiwan. International Journal of Environmental Research and Public Health. 2014; 11(2):1384-1397. https://doi.org/10.3390/ijerph110201384
Chicago/Turabian StyleLiu, Li-Fan. 2014. "The Health Heterogeneity of and Health Care Utilization by the Elderly in Taiwan" International Journal of Environmental Research and Public Health 11, no. 2: 1384-1397. https://doi.org/10.3390/ijerph110201384



