Basic Concepts in the Taxonomy of Health-Related Behaviors, Habits and Lifestyle
Abstract
:1. Introduction
2. Methods
Taxonomical Model
3. Results
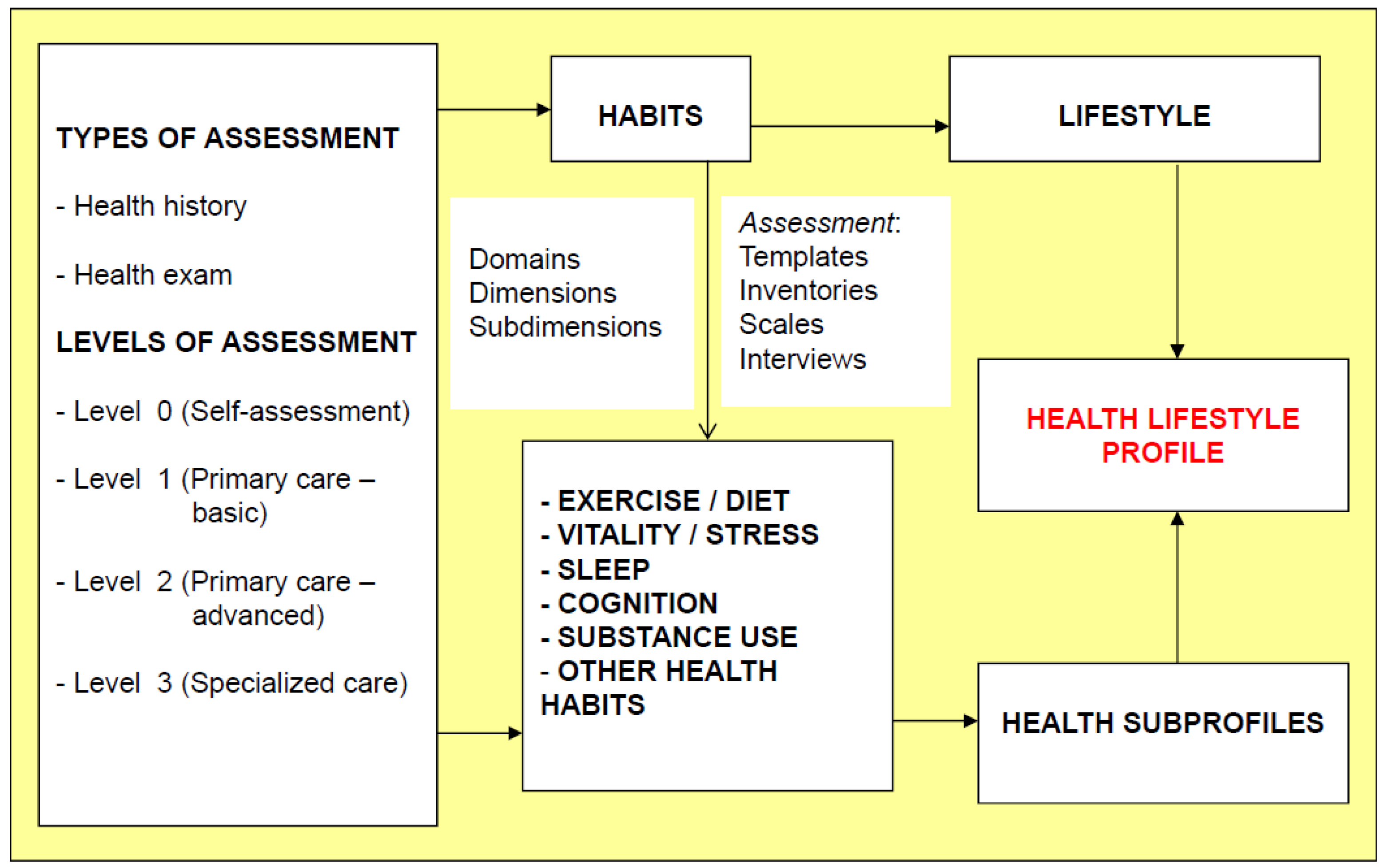
3.1. Basic Concepts
3.1.1. Health-Related Behaviors (HrB)
3.1.2. Health-Related Habits (HrH)
| Criteria | Specifications |
|---|---|
| 1. Clinical meaningfulness (Relevance to health) | The habit is meaningful from a clinical and a public health perspective. There is published evidence in the scientific literature of the relationship of the habit with a priority target in health (e.g., longevity, disability, health promotion), which could be evaluated using standard indicators like mortality, disability-adjusted life years, and years lived without disability). |
| 2. Quantifiability (measurabity) | Habits or behavior patterns linked with basic health functions can be broken down into a series of specific observable behaviors and/or behavioral patterns and are associated with health outcomes. By measuring specific behaviors and their combined pattern, one can determine an identifiable and objective pattern (e.g., watching more than three hours of television each day is a relevant indicator of sedentariness). It is possible to identify and describe the main components of each habit using specific standardized measurements. |
| 3. Temporal stability | Habits or behavior patterns linked with basic health functions are stable over time and are performed routinely, as opposed to occasionally. The habit, its behavior pattern or a key observed behavior persists for more than 12 months. |
| 4. Associated morbidity | The excess or the lack of use of the habit is associated to specific health conditions coded in the standard international health classification systems. |
| 5. Unitarity (non-redundancy) | A habit is not redundant with other habits and cannot be better considered a dimension within another domain (i.e., It fits as a category within the hierarchical classification) |
- ▪
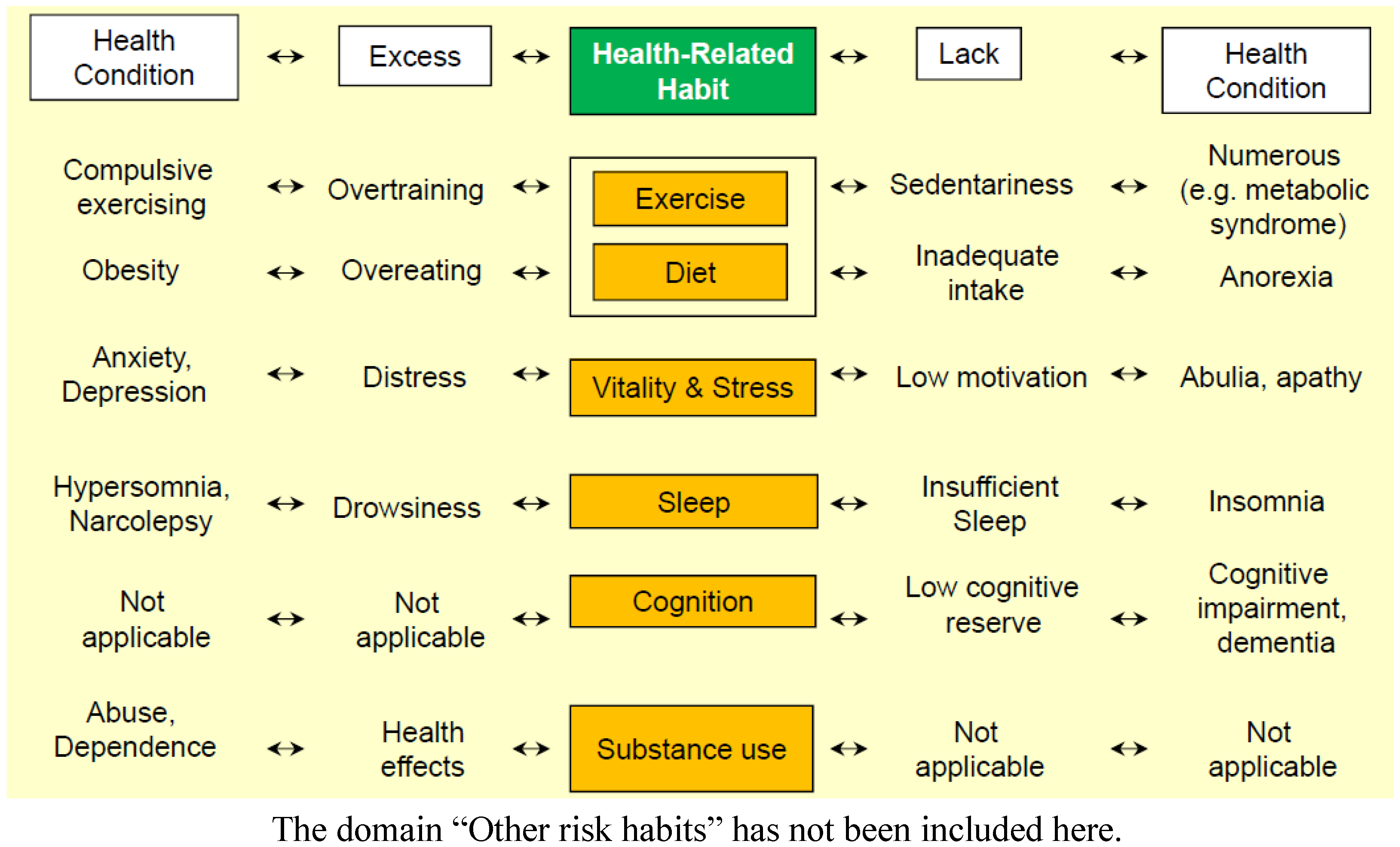
- Polarity: Habits can be classified into “positive health-related habits” (HrH+), complex behavioral patterns whose result is in increase in lifespan and in years lived without disability, and “negative health-related habits” (HrH−) associated with poor health and illness. In addition, two different patterns of polarity could be identified, when habits are represented in a continuum, unidimensional scale. From a clinical perspective some habits may be represented as bipolar/bidirectional within a continuum where proactive positive health (or enkrasia) [29] can be placed in the middle, and specific disorders associated either to excess or to lack of use are at the extremes (Figure 2). Two other HrH are better described as unipolar, ranging from optimal health to ill health related either to excess (substance use) or to lack of use (cognition).
- ▪
- Stages of change: Of the six basic HrH, three are directly related to motivation to change (diet/exercise, substance use, and other risk habits), and three are less directly linked (cognition, vitality/stress, and sleep). The stages of change model developed by Prochaska [25] includes the stages precontemplation, in which an individual has no intention of changing within 6 months, contemplation, in which an individual intends to change within 6 months, preparation, in which small steps are taken with the goal of changing behavior within 1 month, action, in which specific changes have occurred within the past 6 months, maintenance, the stage of variable duration in which relapse is actively avoided, and termination, in which the individual is no longer tempted to return to the behavior [26], with relapse being a time in which an individual moves backwards from maintenance or termination to other stages. An assessment of an individual’s stage of change regarding a particular behavior raises the clinical utility of an evaluation of HrH by guiding clinicians toward interventions appropriate for a given stage and by predicting likelihood of behavior change [27,28,29,30,31].
3.1.3. Health-Related Lifestyle (HrL)
3.1.4. Health Lifestyle Profile

3.2. Other Relevant Concepts
3.2.1. Health Reserve and Capital
3.2.2. Health Risk and Load
4. Discussion
5. Conclusions
Acknowledgements
Conflict of Interest
References
- Horder, T. Health with happiness. Br. Med. J. 1937, 2, 858–859. [Google Scholar] [CrossRef]
- Lalonde, M. A New Perspective on the Health of Canadians (Lalonde report 1973–1974); Minister of Supply and Services: Ottawa, ON, Canada; Available online: http://www.phac-aspc.gc.ca/ph-sp/pdf/perspect-eng.pdf (accessed on 21 April 2013).
- Kilmer, G.; Roberts, H.; Hughes, E.; Li, Y.; Valluru, B.; Fan, A.; Giles, W.; Mokdad, A.; Jiles, R. Surveillance of certain health behaviors and conditions among states and selected local areas-behavioral risk factor surveillance system (BRFSS), United States, 2006. MMWR Surveill. Summ. 2008, 57, 1–188. [Google Scholar]
- Hart, T.L.; Craig, C.L.; Griffiths, J.M.; Cameron, C.; Andersen, R.E.; Bauman, A.; Tudor-Locke, C. Markers of sedentarism: The joint Canada/U.S. survey of health. J. Phys. Act. Health 2011, 3, 361–371. [Google Scholar]
- Hamer, M.; Kivimaki, M.; Steptoe, A. Longitudinal patterns in physical activity and sedentary behaviour from mid-life to early old age: A substudy of the Whitehall II cohort. J. Epidemiol. Community Health. 2012, 12, 1110–1115. [Google Scholar] [CrossRef] [Green Version]
- U.S. Department of Health and Human Services (HHS), Healthy People 2010: Understanding and Improving Health; U.S. Government Printing Office (GPO): Washington, DC, USA, 2000.
- McCartney, G.; Hanlon, P. What can health professionals contribute to the challenge of sustainability? Public Health 2009, 123, 761–764. [Google Scholar] [CrossRef]
- Grandes, G.; Sanchez, A.; Sanchez-Pinilla, R.O.; Torcal, J.; Montoya, I.; Lizarraga, K.; Serra, J. Effectiveness of physical activity advice and prescription by physicians in routine primary care: A cluster randomized trial. Arch. Intern. Med. 2009, 169, 694–701. [Google Scholar] [CrossRef]
- Jansink, R.; Braspenning, J.; van der Weijden, T.; Niessen, L.; Elwyn, G.; Grol, R. Nurse-led motivational interviewing to change the lifestyle of patients with type 2 diabetes (mild-project): Protocol for a cluster, randomized, controlled trial on implementing lifestyle recommendations. BMC Health Serv. Res. 2009, 9. [Google Scholar] [CrossRef] [Green Version]
- Grandes, G.; Sanchez, A.; Cortada, J.M.; Balague, L.; Calderon, C.; Arrazola, A.; Vergara, I.; Millan, E. Is integration of healthy lifestyle promotion into primary care feasible? Discussion and consensus sessions between clinicians and researchers. BMC Health Serv. Res. 2008, 8. [Google Scholar] [CrossRef]
- Sanchez, A.; Grandes, G.; Cortada, J.M.; Pombo, H.; Balague, L.; Calderon, C. Modelling innovative interventions for optimising healthy lifestyle promotion in primary health care: “Prescribe vida saludable” Phase I research protocol. BMC Health Serv. Res. 2009, 9. [Google Scholar] [CrossRef]
- Korhonen, I.; Mattila, E.; Ahtinen, A.; Salminen, J.; Hopsu, L.; Lappalainen, R.; Leino, T. Personal health promotion through personalized health technologies—Nuadu experience. IEEE Eng. Med. Biol. Soc. 2009, 1, 316–319. [Google Scholar]
- Roma-Ferri, M.T.; Palomar, M. Analysis of health terminologies for use as ontologies in healthcare information systems. Gac. Sanit. 2008, 22, 421–433. [Google Scholar]
- Moner, D.; Maldonado, J.A.; Angulo, C.; Bosca, D.; Perez, D.; Abad, I.; Reig, E.; Robles, M. Standardization of discharge reports with the iso 13606 norm. IEEE Eng. Med. Biol. Soc. 2008, 1470–1473. [Google Scholar]
- Buetow, S.; Kiata, L.; Liew, T.; Kenealy, T.; Dovey, S.; Elwyn, G. Patient error: A preliminary taxonomy. Ann. Fam. Med. 2009, 7, 223–231. [Google Scholar] [CrossRef]
- Kilic, O.; Dogac, A. Achieving clinical statement interoperability using r-mim and archetype-based semantic transformations. IEEE Trans. Inf. Technol. Biomed. 2009, 13, 467–477. [Google Scholar] [CrossRef]
- Salvador-Carulla, L.; Walsh, C.O.; Alonso-Trujillo, F.; Gómez, R.; de Teresa, C.; Cabo-Soler, J.R.; Cano, A.; Ruiz, M. eVITAL: A preliminary taxonomy and electronic toolkit of health-related habits and lifestyle. Sci. World J. 2012. [Google Scholar] [CrossRef]
- Snow, D.A.; Rochford, E.B., Jr.; Worden, S.K.; Benford, R.D. Frame alignment processes, micromobilization, and movement participation. Am. Sociol. Rev. 1986, 51, 464–481. [Google Scholar] [CrossRef]
- Alonso-Trujillo, F.; Walsh, C.O.; Salvador-Carulla, L. eVITAL group. Methodology for the development of a taxonomy and toolkit to evaluate health related habits and lifestyle (eVITAL). BMC Res. Notes 2010, 3, 1–5. [Google Scholar] [CrossRef]
- International Classification of Functioning, Disability And Health (ICF); WHO: Geneva, Switzerland, 2001.
- World Health Organization, Health Promotion Glossary; WHO: Geneva, Switzerland, 1998.
- Noncommunicable Diseases and Mental Health Cluster. Noncommunicable Disease Prevention and Health Promotion Department. Aging and Life Course. Active aging: A policy framework; WHO: Geneva, Switzerland, 2002.
- Promoting Mental Health: Concepts, Emerging Evidence, Practice; WHO: Geneva, Switzerland, 2004.
- Mezzich, J.E.; Salloum, I.M.; Cloninger, C.R.; Salvador-Carulla, L.; Kirmayer, L.J.; Banzato, C.E.; Wallcraft, J.; Botbol, M. Person-centred integrative diagnosis: Conceptual bases and structural model. Can. J. Psychiatry 2010, 55, 701–708. [Google Scholar]
- Prochaska, J.O.; DiClemente, C.C. Stages and processes of self-change of smoking: Toward an integrative model of change. J. Consult. Clin. Psychol. 1983, 51, 390–395. [Google Scholar]
- Prochaska, J.O.; Velicer, W.F. The transtheoretical model of health behavior change. Am. J. Health Promot. 1997, 12, 38–48. [Google Scholar] [CrossRef]
- Prochaska, J.O.; Butterworth, S.; Redding, C.A.; Burden, V.; Perrin, N.; Leo, M.; Flaherty-Robb, M.; Prochaska, J.M. Initial efficacy of MI, TTM tailoring and HRI’s with multiple behaviors for employee health promotion. Prev. Med. 2008, 46, 226–231. [Google Scholar] [CrossRef]
- Salvador-Carulla, L.; Gibert, K.; Ochoa, S. Definition of “Functional dependency”. Implications for health and social policy. Aten. Primaria 2010, 42, 344–345. [Google Scholar] [CrossRef]
- Bowman, J.L. Stoicism, Enkrasia and Happiness; iUniverse Inc.: Bloomington, IN, USA, 2011. [Google Scholar]
- Bertholet, N.; Cheng, D.M.; Palfai, T.P.; Samet, J.H.; Saitz, R. Does readiness to change predict subsequent alcohol consumption in medical inpatients with unhealthy alcohol use? Addict. Behav. 2009, 34, 636–640. [Google Scholar] [CrossRef]
- Wright, J.A.; Velicer, W.F.; Prochaska, J.O. Testing the predictive power of the transtheoretical model of behavior change applied to dietary fat intake. Health Educ. Res. 2009, 24, 224–236. [Google Scholar]
- Seeman, T.E.; Singer, B.H.; Ryff, C.D.; Dienberg Love, G.; Levy-Storms, L. Social relationships, gender, and allostatic load across two age cohorts. Psychosom. Med. 2002, 64, 395–406. [Google Scholar]
- Prochaska, J.J.; Velicer, W.F.; Nigg, C.R.; Prochaska, J.O. Methods of quantifying change in multiple risk factor interventions. Prev. Med. 2008, 46, 260–265. [Google Scholar] [CrossRef]
- Reig Redondo, J. eSalud en la Europe de las Regiones: Conferencia de alto Nivel Sobre Aspectos de Políticas de eSalud, Málaga, 10–12 Mayo 2006; Available online: http://archivo.revistaesalud.com/index.php/revistaesalud/article/viewArticle/65 (accessed on 6 May 2013).
- Sedentary Behaviour Research Network. Letter to the editor: Standardized use of the terms “sedentary” and “sedentary behaviours”. Appl. Physiol. Nutr. MeTab. 2012, 37, 540–542. [CrossRef]
- McEachan, R.R.; Lawton, R.J.; Conner, M. Classifying health-related behaviours: Exploring similarities and differences amongst behaviours. Br. J. Health Psychol. 2010, 15, 347–366. [Google Scholar]
- Michie, S.; Ashford, S.; Sniehotta, F.F.; Dombrowski, S.U.; Bishop, A.; French, D.P. A refined taxonomy of behaviour change techniques to help people change their physical activity and healthy eating behaviours: The CALO-RE taxonomy. Psychol. Health 2011, 26, 1479–1498. [Google Scholar] [CrossRef]
- Sweet, S.S.; Fortier, M.S. Improving physical activity and dietary behaviours with single or multiple health behaviour interventions? A synthesis of meta-analyses and reviews. Int. J. Environ. Res. Public Health. 2010, 7, 1720–1743. [Google Scholar] [CrossRef]
- Good Health Adds Life to Years. Global Brief for World Health Day 2012; WHO: Geneva, Switzerland, 2012.
- Giannangelo, K.; Millar, J. Mapping SNOMED CT to ICD-10. Stud. Health Technol. Inform. 2012, 180, 83–87. [Google Scholar]
- Geyh, S.; Müller, R.; Peter, C.; Bickenbach, J.E.; Post, M.W.; Stucki, G.; Cieza, A. Capturing the psychologic-personal perspective in spinal cord injury. Am. J. Phys. Med. Rehabil. 2011, 90, 79–96. [Google Scholar] [CrossRef]
- Paviot, B.T.; Madden, R.; Moskal, L.; Zaiss, A.; Bousquet, C.; Kumar, A.; Lewalle, P.; Rodrigues, J.M. Development of a new international classification of health interventions based on an ontology framework. Stud. Health Technol. Inform. 2011, 169, 749–753. [Google Scholar]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Salvador-Carulla, L.; Alonso, F.; Gomez, R.; Walsh, C.O.; Almenara, J.; Ruiz, M.; Abellán, M.J.; Group, E. Basic Concepts in the Taxonomy of Health-Related Behaviors, Habits and Lifestyle. Int. J. Environ. Res. Public Health 2013, 10, 1963-1976. https://doi.org/10.3390/ijerph10051963
Salvador-Carulla L, Alonso F, Gomez R, Walsh CO, Almenara J, Ruiz M, Abellán MJ, Group E. Basic Concepts in the Taxonomy of Health-Related Behaviors, Habits and Lifestyle. International Journal of Environmental Research and Public Health. 2013; 10(5):1963-1976. https://doi.org/10.3390/ijerph10051963
Chicago/Turabian StyleSalvador-Carulla, Luis, Federico Alonso, Rafael Gomez, Carolyn O. Walsh, José Almenara, Mencía Ruiz, María José Abellán, and EVITAL Group. 2013. "Basic Concepts in the Taxonomy of Health-Related Behaviors, Habits and Lifestyle" International Journal of Environmental Research and Public Health 10, no. 5: 1963-1976. https://doi.org/10.3390/ijerph10051963




