1. Introduction
Arterial injury occurring during angioplasty and arteriosclerosis results in smooth muscle proliferation where endothelial cell injury is postulated to precede the smooth muscle proliferative response [
1]. Experimentally, similar endothelial injury can be produced in small animals by air drying a segment of an artery where within 14 days lesions in the arterial wall are evident [
2]. There is increasing evidence that vascular endothelium is injured by damaging free radical species in the spectrum of diseases [
3]. These radical molecules are capable of degrading the polyunsaturated acyl chains of membrane phospholipids (lipid peroxidation) hereby inducing pathologic changes in the underlying tissue [
4].
When seeking an ideal drug for the treatment of atherosclerotic lesions, two characteristics are required 1) inhibition of smooth muscle proliferation and 2) increase in scavenging of free radical species. Turmeric is such a drug. It has been shown to inhibit smooth muscle proliferation [
5], enhance endothelial cell proliferation [
6] and reduce oxidative damage in arteries, plasma and subcellular membranes [
7,
8,
9]. It is a yellow spice obtained from
Curcuma longa.Turmerin is a water-soluble protein derived from turmeric with a molecular weight of 24,000 Da [
10]. It has been shown to protect against DNA damage in calf thymus DNA and human peripheral lymphocytes [
11]. It has never been investigated for its effects on vascular diseases.
The objective of this study was to determine if turmerin could prevent the formation of atherosclerotic plaques. The specific aims of the study were to determine whether turmerin treatment would decrease intimal thickening of the smooth muscle cell layer (local representation) and to determine if it would protect against the oxidative damage of lipid peroxidation (systemic representation).
Materials and Methods
Turmerin preparation
Turmeric powder was obtained from Raja Foods (Lincolnwood, IL). Turmerin was obtained by boiling 1% turmeric solution for 30 minutes, centrifuging at 1200 x g for 10 minutes and passing the supernatant through 0.22 µ filter whose protein concentration corresponded to 80 µg/ml.
Animals
Anesthetized Lewis rats (n =12) weighing 200 ± 4.0 gms and about 2 months old were randomly assigned to two equal groups. Group I (6 Lewis rats) received local saline treatment (0.9% NaCl) in the carotid artery while Group II (6 Lewis rats) received local carotid turmerin (80µg/ml) and gavaged with 1ml turmerin daily. Rats were anesthetized with pentobarbital (50mg/kg) and the right carotid artery (3.0cm. length) was dissected out of the loose connective tissue and clamped in two places, 1.5 cm apart. The endothelium was washed at the proximal and distal ends of the artery with phosphate buffered saline (PBS) using a tuberculin syringe. The artery was treated with compressed air at 28 ml/min for 5 min [
12]. It was then flushed with PBS and clipped. The artery was then filled with saline for Group I and turmerin for Group II and allowed to incubate in the artery for 5 min. The artery was then flushed with saline, clips removed and bleeding stopped by applying gentle pressure for 2-3 min. The skin was then closed. Group I was gavaged with 1 ml of saline while Group II was gavaged with 1 ml of turmerin at 80 µg/ml for 14 days. After 14 days, blood was removed from the animals by puncturing the heart and the artery was removed for histology. The animals were finally sacrificed by pneumothorax.
Lipid peroxidation (MDA levels)
An aliquot of 100 µl of serum was incubated at 70
0C for 2 hours with 100 µl of 8.1% SDS, 2.5 µl of 2% betahydroxytoluene and 0.5 ml of thiobarbituric acid (TBA)-HCL which consisted of 15% w/v trichloroacetic acid in 0.375% TBA and 0.25 N HCL [
13]. After cooling , 1 ml of n-butanol was added, vortexed, centrifuged and the absorbence measured at 532 nm to quantitate the malondialdehyde (MDA) levels.
Lipid peroxidation (conjugated diene levels)
Lipid peroxidation measurement by conjugated dienes was performed [
14]. An aliquot of 500 µl of serum was extracted in chloroform-methanol (2:1) and dried in N
2. The dried extract was re-dissolved in cyclohexane and absorbency measured at 234 nm.
Histology
After 14 days, the carotid artery was removed from the animal and immersed in 10% formalin to be processed for H & E staining using standard histology techniques. Histology changes were determined by examining endothelial damage and wall thickening.
Statistical Analysis
Results are expressed as Means ± S.D. Student’s t-test and two-sample analysis using unequal variances were used; p≤0.05 was considered statistically significant.
Results
The histology gave us some indication with respect to endothelial regeneration. The controls showed a fine lining of the endothelial cells but had extensive proliferation and edema of smooth muscle cells in the media. Only one out of six rats showed very little proliferation in the intima with complete coverage of the endothelium with endothelial cells (
Figure 1). The remaining five rats had variable response with respect to endothelial repair and intima thickening.
Figure 1.
Cross section of common carotid artery 14 days after denudation by air-drying. A. Animals treated locally with turmerin for 5 mins and by daily gavaging with 1ml turmerin showed a reduced intima in 1/6 rats(x 40, H & E stain). B. Animals treated locally with saline for 5 mins and by daily gavaging with 1 ml saline showed an increased intima and hyper-proliferation and edema of smooth muscle cells. Only one out of six rats showed no proliferation in the intima while there was significant variation in controls.
Figure 1.
Cross section of common carotid artery 14 days after denudation by air-drying. A. Animals treated locally with turmerin for 5 mins and by daily gavaging with 1ml turmerin showed a reduced intima in 1/6 rats(x 40, H & E stain). B. Animals treated locally with saline for 5 mins and by daily gavaging with 1 ml saline showed an increased intima and hyper-proliferation and edema of smooth muscle cells. Only one out of six rats showed no proliferation in the intima while there was significant variation in controls.
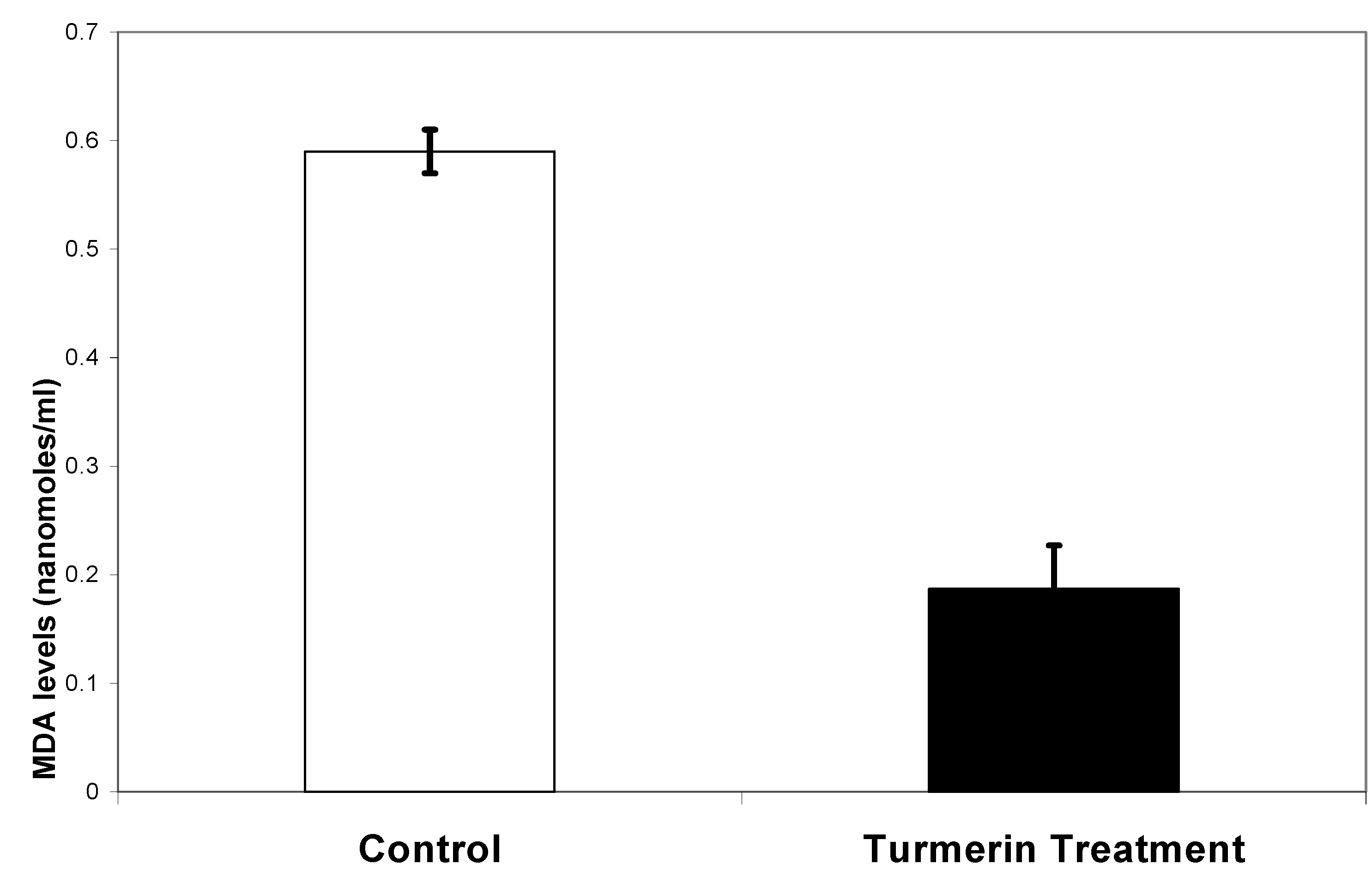
Lipid peroxidation as measured by MDA levels was 0.593 ± 0.02 nanomoles/ml for control while turmerin was 0.187± 0.04 nanomoles/ml (
Figure 2). There was a significant difference (p≤0.01) in MDA levels between the turmerin treatment and the saline control.
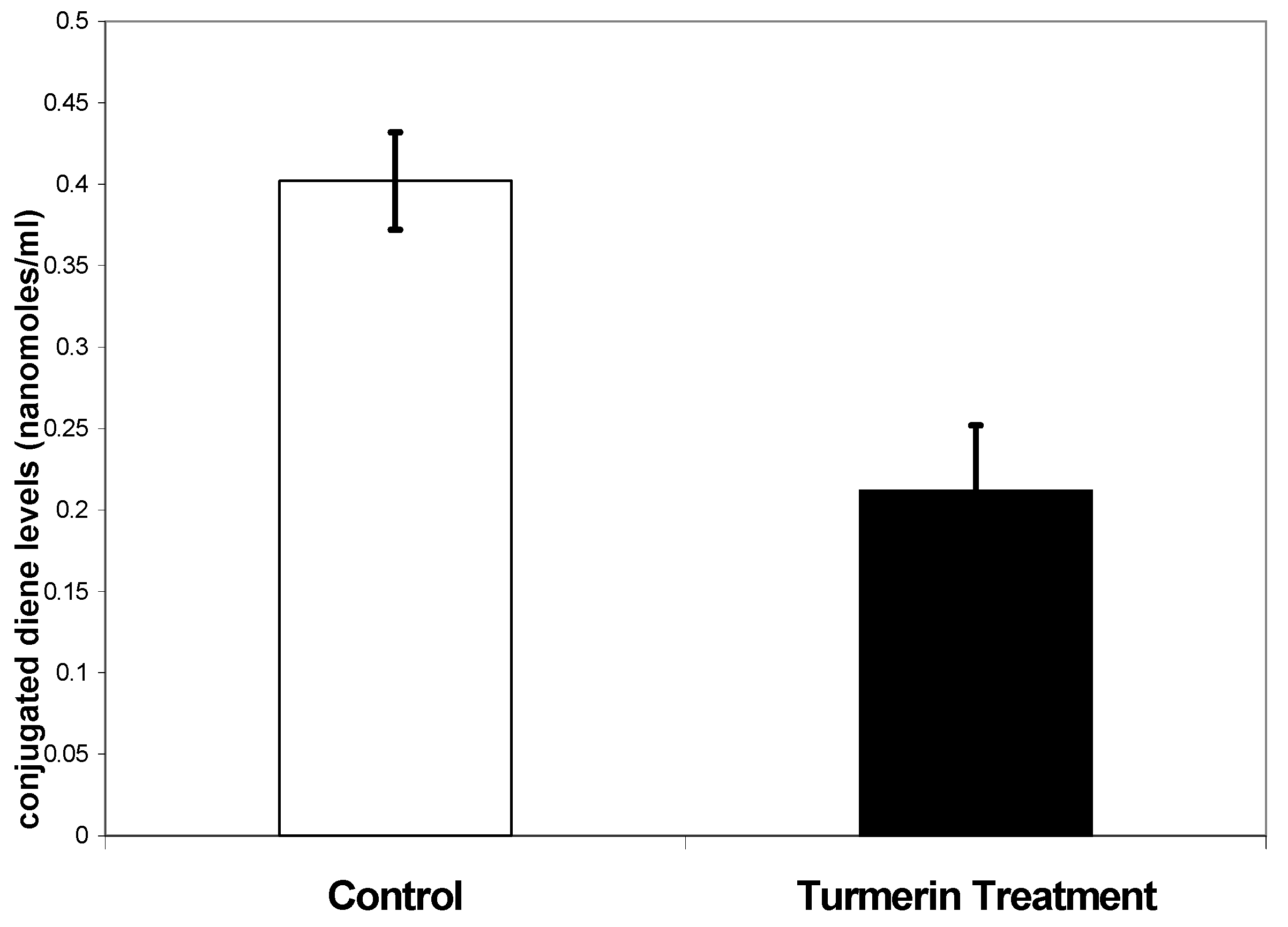
Lipid peroxidation as measured by conjugated diene levels was 0.402 ± 0.03 nanomoles/ml for controls while for turmerin was 0.212 ± 0.04 nanomoles/ml (
Figure 3). There was a significant difference (p≤0.05) in conjugated diene levels between the turmerin treatment and saline control.
Figure 2.
Lipid peroxidation as measured by MDA levels.
Figure 2.
Lipid peroxidation as measured by MDA levels.
Figure 3.
Lipid peroxidation as measured by conjugated dienes level.
Figure 3.
Lipid peroxidation as measured by conjugated dienes level.
Discussion
Arteriosclerosis, a vascular disease, involves endothelial cell injury and proliferation characterized by intimal hyperplasia. Injury results in migration of smooth muscle cells from the media and cell division in the intima [
15]. Extensive evidence suggests that reactive oxygen species are critically involved in the pathogenesis of cardiovascular diseases, such as atherosclerosis and myocardial ischemia-reperfusion injury. Consistent with this concept, the administration of exogenous antioxidants has been shown to be protective against oxidative cardiovascular injury. It has been demonstrated that antioxidants affect the gene expression of the neointimal response after balloon denudation [
16].
With this in mind, we investigated the effect of turmerin on the air denudation animal model. The air denudation of endothelial cells in an animal model offered a unique opportunity to study the effects of antioxidants on the oxidative stress produced by denudation on the alteration of relationship between endothelial loss and changes in the vessel.
The in-vivo studies using turmerin at 80 µg/ml showed that in-vitro tests of serum lipid peroxidation as detected by two methods had significant reduction in lipid peroxidation but the attenuation of damage in the tissue was inconsistent. Although there was significant reduction in serum peroxidation activity, the histological findings indicated that attenuation of the carotid artery injury could involve growth factors and food intake than decreased lipid peroxidation.
Turmerin at 800 ng/ml has been previously shown to cause no protection in hydrogen-peroxide induced renal endothelial cell injury [
17]. In this study, we have used an 80 µg/ml dose to treat rats and have shown that there is a protection from oxidative stress. However, the histology showed good healing of the denuded endothelium in only one of six rats. It is possible that if the dose of turmerin were to be increased, there would be sufficient protection provided so as to heal the endothelium as well as to decrease the intimal hyperplasia. Thus, this study shows promise that turmerin is effective in decreasing the systemic damage but a higher dose would be required for local application at the denuded artery. Additional experiments employing larger number of animals and a longer duration of treatment i.e., instead of 5 minutes may be a 10 minute local treatment at the site of injury may be required to show the beneficial effect of turmerin in vascular diseases.
Acknowledgements
Anelle Taylor was supported in part by the Howard Hughes Medical Institute and the base pair program.