[18F]-Fluorinated Carboplatin and [111In]-Liposome for Image-Guided Drug Delivery
Abstract
:1. Introduction
2. Results
2.1. Analysis
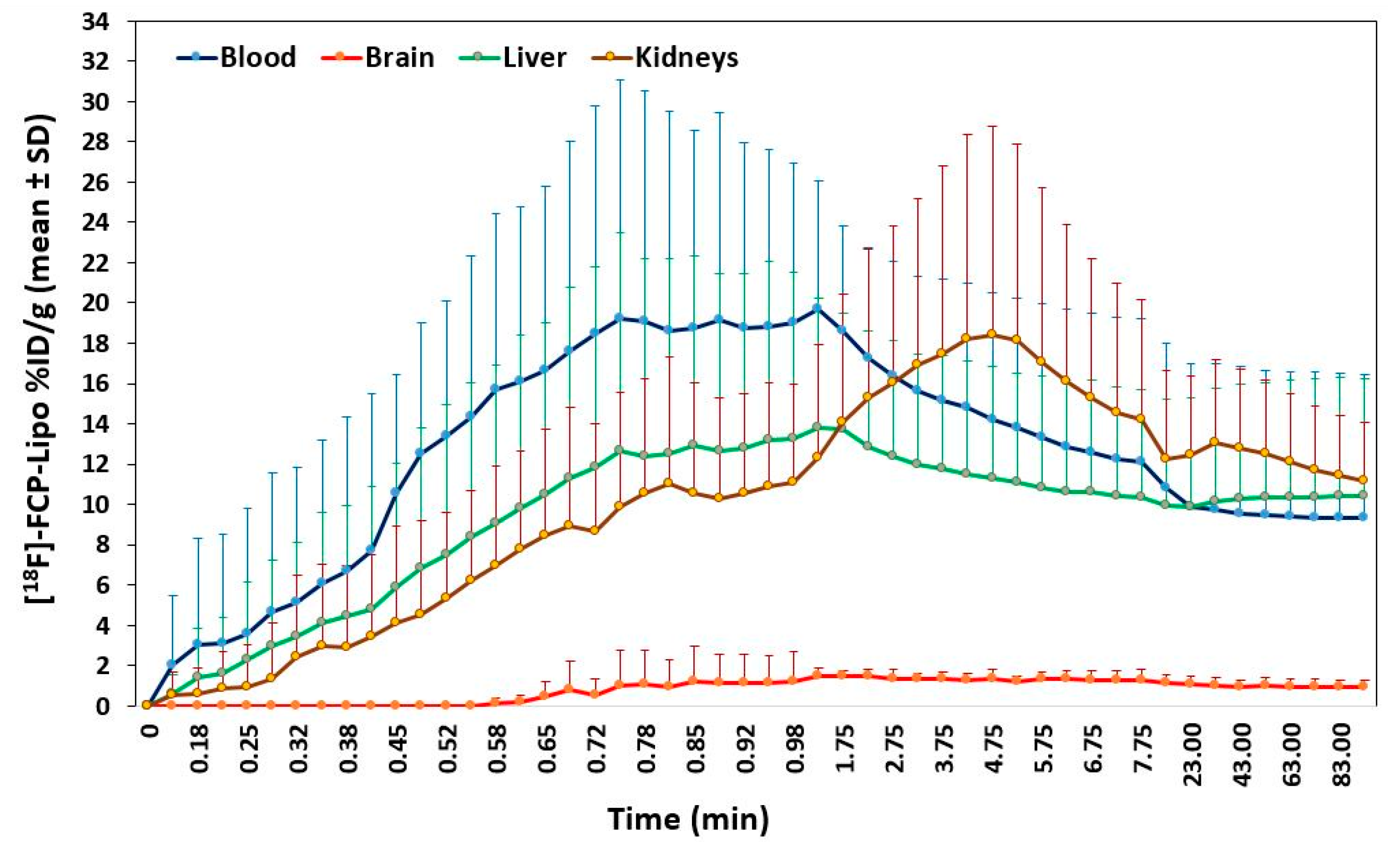
2.2. Biodistribution of [111In]-Liposome
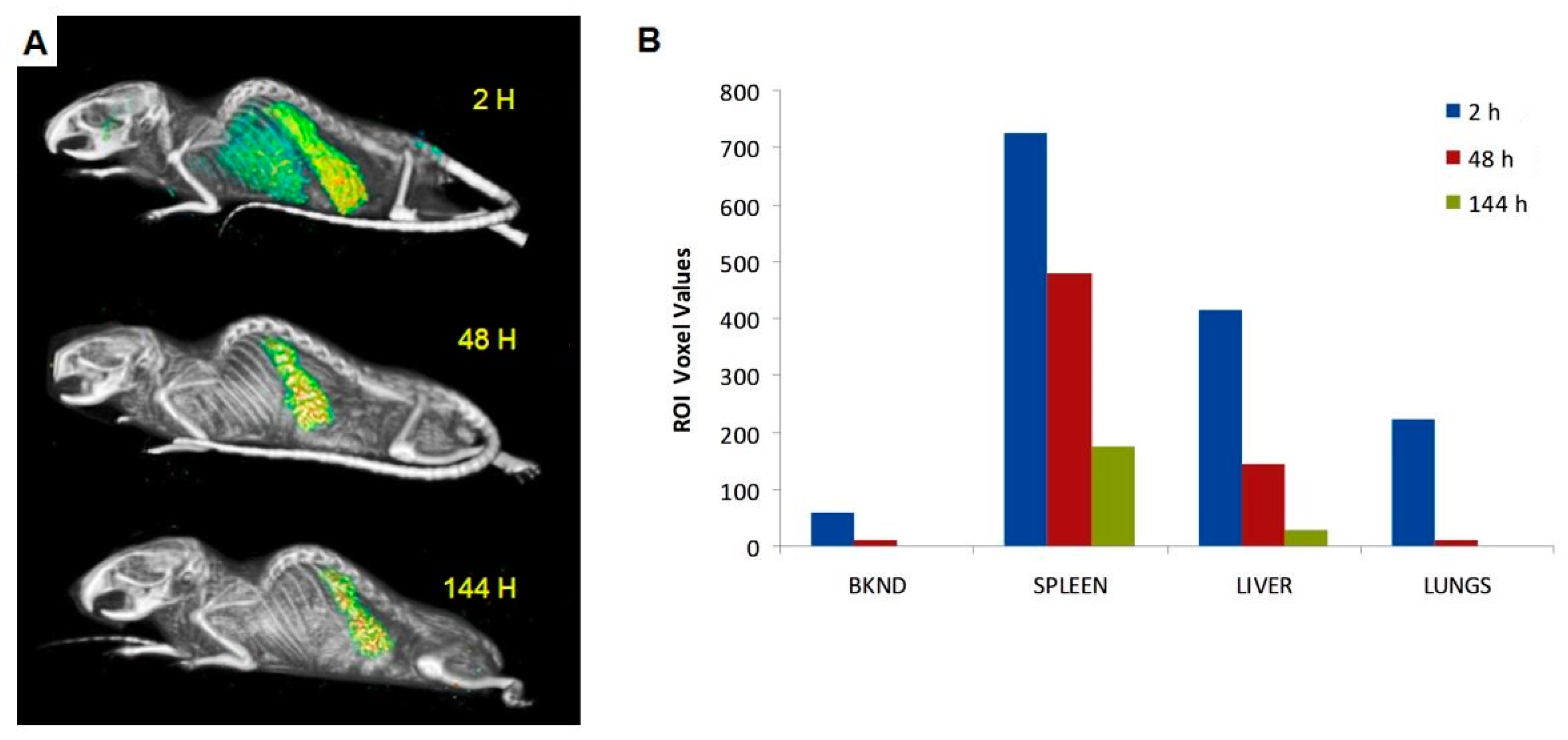
2.3. SPECT/CT Imaging of [111In]-Liposome
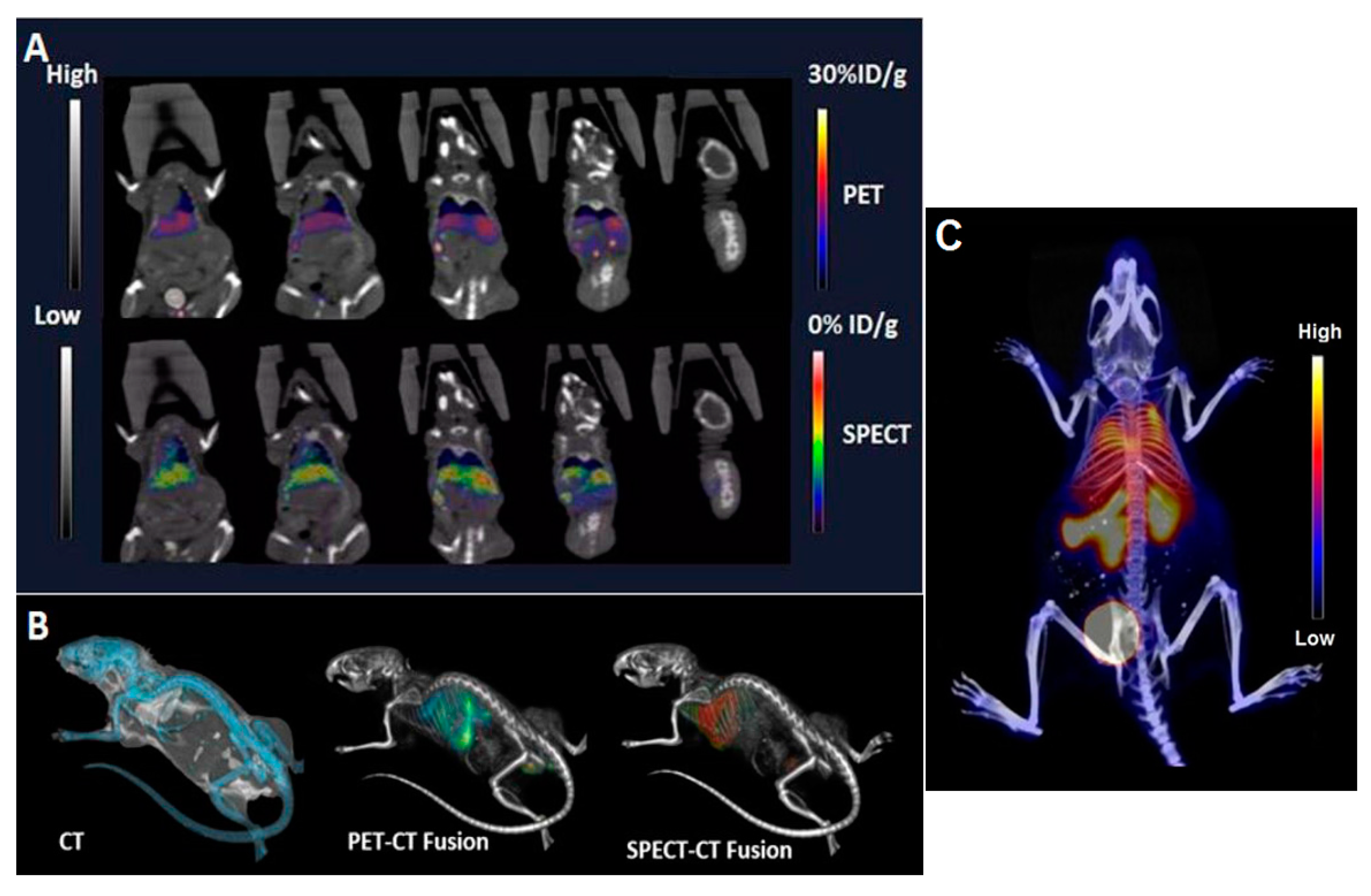
2.4. PET/SPECT/CT Imaging
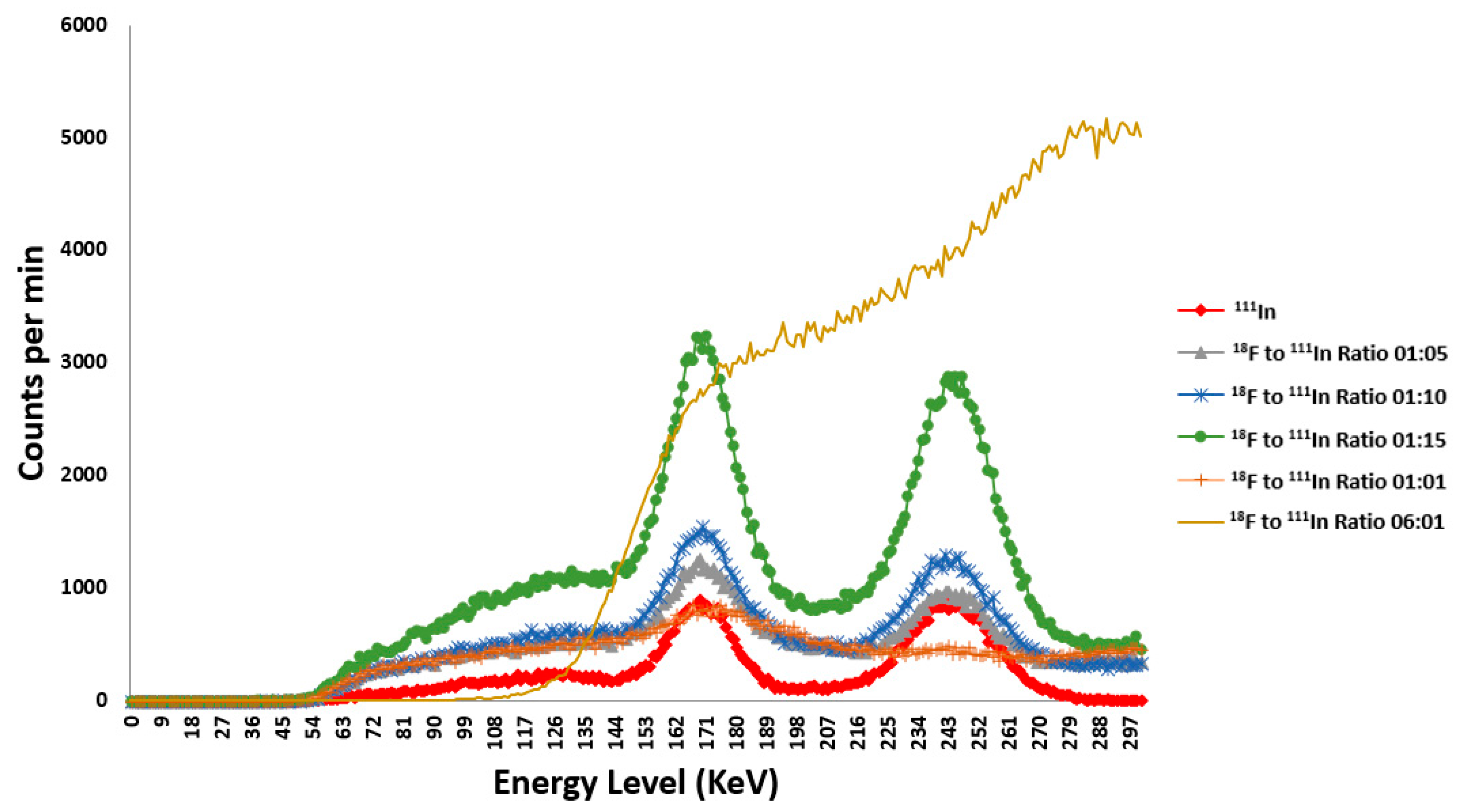
2.5. Optimization of Dual Radionuclide Imaging of 111In and 18F
3. Discussion
4. Materials and Methods
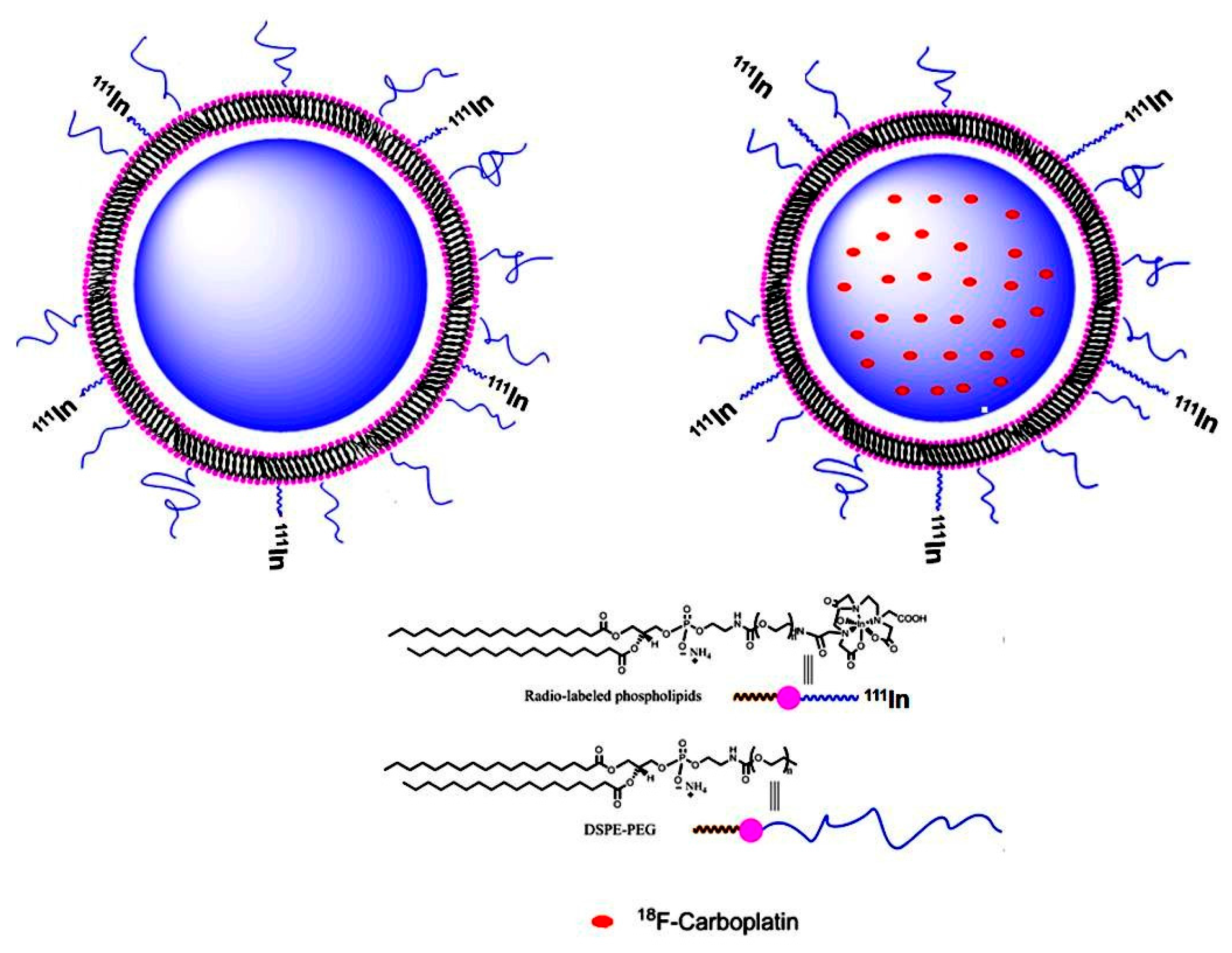
4.1. Synthesis of [111In]-Liposome
4.2. Synthesis of [18F]-FCP
4.3. [18F]-FCP encapsulation in [111In]-Liposomes
4.4. Biodistribution of [111In]-Liposome
4.5. In vivo SPECT/CT Imaging of [111In]-Liposome
4.6. PET/SPECT/CT of [18F]-FCP/[111In]-Liposome
4.7. Optimization of Dual-Radionuclide Imaging of 111In and 18F
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ahmad, M.Z.; Alkahtani, S.A.; Akhter, S.; Ahmad, F.J.; Ahmad, J.; Akhtar, M.S.; Mohsin, N.; Abdel-Wahab, B.A. Progress in nanotechnology-based drug carrier in designing of curcumin nanomedicines for cancer therapy: Current state-of-the-art. J. Drug Target. 2016, 24, 273–293. [Google Scholar] [CrossRef] [PubMed]
- Allen, T.M.; Cullis, P.R. Liposomal drug delivery systems: From concept to clinical applications. Adv. Drug Deliv. Rev. 2013, 65, 36–48. [Google Scholar] [CrossRef] [PubMed]
- Han, X.J.; Wei, Y.F.; Wan, Y.Y.; Jiang, L.P.; Zhang, J.F.; Xin, H.B. Development of a novel liposomal nanodelivery system for bioluminescence imaging and targeted drug delivery in ERBB2-overexpressing metastatic ovarian carcinoma. Int. J. Mol. Med. 2014, 34, 1225–1232. [Google Scholar] [CrossRef] [PubMed]
- Jha, S.; Sharma, P.; Malviya, R. Liposomal drug delivery system for cancer therapy: Advancement and patents. Recent Pat. Drug Deliv. Formul. 2016, 10, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Kshirsagar, N.A.; Pandya, S.K.; Kirodian, G.B.; Sanath, S. Liposomal drug delivery system from laboratory to clinic. J. Postgrad. Med. 2005, 51, S5–S15. [Google Scholar] [PubMed]
- Pattni, B.S.; Chupin, V.V.; Torchilin, V.P. New developments in liposomal drug delivery. Chem. Rev. 2015, 115, 10938–10966. [Google Scholar] [CrossRef] [PubMed]
- Puri, A.; Loomis, K.; Smith, B.; Lee, J.H.; Yavlovich, A.; Heldman, E.; Blumenthal, R. Lipid-based nanoparticles as pharmaceutical drug carriers: From concepts to clinic. Crit. Rev. Ther. Drug Carr. Syst. 2009, 26, 523–580. [Google Scholar] [CrossRef]
- Barenholz, Y. Doxil(r)—The first FDA-approved nano-drug: Lessons learned. J. Control Release 2012, 160, 117–134. [Google Scholar] [CrossRef] [PubMed]
- Soares, D.C.; de Oliveira, M.C.; dos Santos, R.G.; Andrade, M.S.; Vilela, J.M.; Cardoso, V.N.; Ramaldes, G.A. Liposomes radiolabeled with 159Gd-DTPA-BMA: Preparation, physicochemical characterization, release profile and in vitro cytotoxic evaluation. Eur. J. Pharm. Sci. 2011, 42, 462–469. [Google Scholar] [CrossRef] [PubMed]
- Ito, K.; Hamamichi, S.; Asano, M.; Hori, Y.; Matsui, J.; Iwata, M.; Funahashi, Y.; Umeda, I.O.; Fujii, H. Radiolabeled liposome imaging determines an indication for liposomal anticancer agent in ovarian cancer mouse xenograft models. Cancer Sci. 2016, 107, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Marik, J.; Tartis, M.S.; Zhang, H.; Fung, J.Y.; Kheirolomoom, A.; Sutcliffe, J.L.; Ferrara, K.W. Long-circulating liposomes radiolabeled with [18F]fluorodipalmitin ([18F]-FDP). Nucl. Med. Biol. 2007, 34, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Helbok, A.; Decristoforo, C.; Dobrozemsky, G.; Rangger, C.; Diederen, E.; Stark, B.; Prassl, R.; von Guggenberg, E. Radiolabeling of lipid-based nanoparticles for diagnostics and therapeutic applications: A comparison using different radiometals. J. Liposome Res. 2010, 20, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Harrington, K.J.; Rowlinson-Busza, G.; Syrigos, K.N.; Uster, P.S.; Abra, R.M.; Stewart, J.S. Biodistribution and pharmacokinetics of 111In-DTPA-labelled pegylated liposomes in a human tumour xenograft model: Implications for novel targeting strategies. Br. J. Cancer 2000, 83, 232–238. [Google Scholar] [CrossRef] [PubMed]
- Ogihara-Umeda, I.; Sasaki, T.; Kojima, S.; Nishigori, H. Optimal radiolabeled liposomes for tumor imaging. J. Nucl. Med. 1996, 37, 326–332. [Google Scholar] [PubMed]
- Chow, T.H.; Lin, Y.Y.; Hwang, J.J.; Wang, H.E.; Tseng, Y.L.; Pang, V.F.; Liu, R.S.; Lin, W.J.; Yang, C.S.; Ting, G. Therapeutic efficacy evaluation of 111In-labeled pegylated liposomal vinorelbine in murine colon carcinoma with multimodalities of molecular imaging. J. Nucl. Med. 2009, 50, 2073–2081. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.Y.; Wang, H.E.; Liu, R.S.; Teng, M.C.; Li, J.J.; Lu, M.; Wei, M.C.; Wong, T.T. Pharmacokinetic analysis of 111In-labeled liposomal doxorubicin in murine glioblastoma after blood-brain barrier disruption by focused ultrasound. PLoS ONE 2012, 7, e45468. [Google Scholar] [CrossRef] [PubMed]
- Mougin-Degraef, M.; Bourdeau, C.; Jestin, E.; Sai-Maurel, C.; Bourgeois, M.; Saec, P.R.; Thedrez, P.; Gestin, J.F.; Barbet, J.; Faivre-Chauvet, A. Doubly radiolabeled liposomes for pretargeted radioimmunotherapy. Int. J. Pharm. 2007, 344, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Presant, C.A.; Proffitt, R.T.; Turner, A.F.; Williams, L.E.; Winsor, D.; Werner, J.L.; Kennedy, P.; Wiseman, C.; Gala, K.; McKenna, R.J.; et al. Successful imaging of human cancer with indium-111-labeled phospholipid vesicles. Cancer 1988, 62, 905–911. [Google Scholar] [CrossRef]
- Kubo, A.; Nakamura, K.; Sammiya, T.; Katayama, M.; Hashimoto, T.; Hashimoto, S.; Kobayashi, H.; Teramoto, T. Indium-111-labelled liposomes: Dosimetry and tumour detection in patients with cancer. Eur. J. Nucl. Med. 1993, 20, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Seo, J.W.; Mahakian, L.M.; Tam, S.; Qin, S.; Ingham, E.S.; Meares, C.F.; Ferrara, K.W. The pharmacokinetics of Zr-89 labeled liposomes over extended periods in a murine tumor model. Nucl. Med. Biol. 2015, 42, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.G.; Gangangari, K.; Kalidindi, T.M.; Punzalan, B.; Larson, S.M.; Pillarsetty, N.V. Copper-64 labeled liposomes for imaging bone marrow. Nucl. Med. Biol. 2016, 43, 781–787. [Google Scholar] [CrossRef] [PubMed]
- Edmonds, S.; Volpe, A.; Shmeeda, H.; Parente-Pereira, A.C.; Radia, R.; Baguna-Torres, J.; Szanda, I.; Severin, G.W.; Livieratos, L.; Blower, P.J.; et al. Exploiting the metal-chelating properties of the drug cargo for in vivo positron emission tomography imaging of liposomal nanomedicines. ACS Nano 2016, 10, 10294–10307. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Zheng, J.; Gaddy, D.; Orcutt, K.D.; Leonard, S.; Geretti, E.; Hesterman, J.; Harwell, C.; Hoppin, J.; Jaffray, D.A.; et al. A gradient-loadable 64Cu-chelator for quantifying tumor deposition kinetics of nanoliposomal therapeutics by positron emission tomography. Nanomedicine 2015, 11, 155–165. [Google Scholar] [CrossRef] [PubMed]
- Jodal, L.; Afzelius, P.; Jensen, S.B. Influence of positron emitters on standard gamma-camera imaging. J. Nucl. Med. Technol. 2014, 42, 42–50. [Google Scholar] [CrossRef] [PubMed]
- Bartoli, A.; Belcari, N.; Guerra, A.D.; Fabbri, S. Simultaneous PET/SPECT imaging with the small animal scanner YAP-(S)PET. In Proceedings of the 2007 IEEE Nuclear Science Symposium Conference Record, Honolulu, HI, USA, 26 October–3 November 2007; pp. 3408–3413. [Google Scholar]
- Chapman, S.E.; Diener, J.M.; Sasser, T.A.; Correcher, C.; Gonzalez, A.J.; Avermaete, T.V.; Leevy, W.M. Dual tracer imaging of SPECT and PET probes in living mice using a sequential protocol. Am. J. Nucl. Med. Mol. Imaging 2012, 2, 405–414. [Google Scholar] [PubMed]
- Matsunari, I.; Kanayama, S.; Yoneyama, T.; Matsudaira, M.; Nakajima, K.; Taki, J.; Nekolla, S.G.; Tonami, N.; Hisada, K. Electrocardiographic-gated dual-isotope simultaneous acquisition spect using 18F-FDG and 99mTc-sestamibi to assess myocardial viability and function in a single study. Eur. J. Nucl. Med. Mol. Imaging 2005, 32, 195–202. [Google Scholar] [CrossRef] [PubMed]
- Dewkar, G.K.; Sundaresan, G.; Lamichhane, N.; Hirsch, J.; Thadigiri, C.; Collier, T.; Hartman, M.C.; Vaidyanthan, G.; Zweit, J. Microfluidic radiosynthesis and biodistribution of [18F] 2-(5-fluoro-pentyl)-2-methyl malonic acid. J. Label. Compd. Radiopharm. 2013, 56, 289–294. [Google Scholar] [CrossRef] [PubMed]
- Dewkar, G.K.; Jose, P.; Lamichhane, N.; Thadigiri, C.; Sundaresan, G.; Farrell, N.; Zweit, J. Abstract 4532: Fluorine-18-carboplatin derivative for imaging and therapeutic applications. Cancer Res. 2013, 73, 4532–4532. [Google Scholar] [CrossRef]
| Organs | 1 h | 6 h | 48 h |
|---|---|---|---|
| Blood | 26.72 ± 8.80 | 3.74 ± 0.49 | 0.15 ± 0.01 |
| Heart | 5.83 ± 0.73 | 1.11 ± 0.05 | 0.21 ± 0.00 |
| Lungs | 7.63 ± 1.01 | 1.97 ± 0.20 | 0.34 ± 0.00 |
| Liver | 15.05 ± 1.07 | 22.86 ± 3.86 | 7.71 ± 0.44 |
| Spleen | 65.92 ± 4.65 | 73.33 ± 12.13 | 45.01 ± 2.94 |
| Stomach | 0.70 ± 0.22 | 0.35 ± 0.07 | 0.20 ± 0.05 |
| Intestine | 2.12 ± 0.68 | 1.24 ± 0.13 | 0.66 ± 0.06 |
| Kidneys | 4.45 ± 0.35 | 1.62 ± 0.33 | 0.75 ± 0.05 |
| Skin | 1.39 ± 0.21 | 0.89 ± 0.18 | 0.62 ± 0.08 |
| Muscle | 0.73 ± 0.21 | 0.39 ± 0.09 | 0.23 ± 0.03 |
| Skull | 3.35 ± 0.48 | 0.94 ± 0.21 | 0.28 ± 0.04 |
| Brain | 0.60 ± 0.01 | 0.13 ± 0.01 | 0.01 ± 0.00 |
| Femur | 1.28 ± 0.10 | 0.99 ± 0.18 | 0.6 ± 0.10 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lamichhane, N.; Dewkar, G.K.; Sundaresan, G.; Mahon, R.N.; Zweit, J. [18F]-Fluorinated Carboplatin and [111In]-Liposome for Image-Guided Drug Delivery. Int. J. Mol. Sci. 2017, 18, 1079. https://doi.org/10.3390/ijms18051079
Lamichhane N, Dewkar GK, Sundaresan G, Mahon RN, Zweit J. [18F]-Fluorinated Carboplatin and [111In]-Liposome for Image-Guided Drug Delivery. International Journal of Molecular Sciences. 2017; 18(5):1079. https://doi.org/10.3390/ijms18051079
Chicago/Turabian StyleLamichhane, Narottam, Gajanan K. Dewkar, Gobalakrishnan Sundaresan, Rebecca N. Mahon, and Jamal Zweit. 2017. "[18F]-Fluorinated Carboplatin and [111In]-Liposome for Image-Guided Drug Delivery" International Journal of Molecular Sciences 18, no. 5: 1079. https://doi.org/10.3390/ijms18051079






