Neuroprotective Effects of Liraglutide for Stroke Model of Rats
Abstract
:1. Introduction
2. Results
2.1. Behavioral Amelioration in Liraglutide-Treated Rats
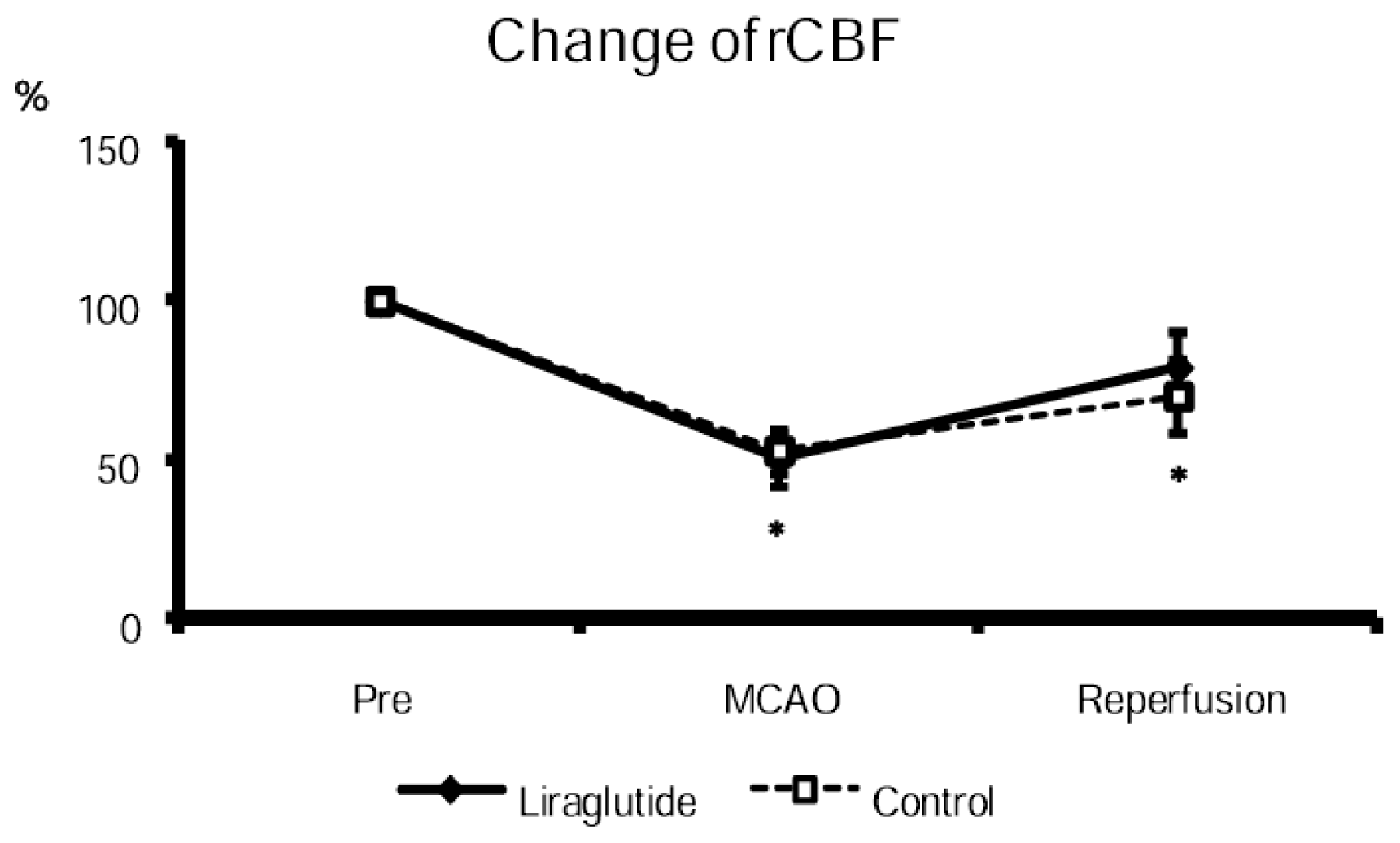
2.2. Changes of Cortical Cerebral Blood Flow
2.3. Effects of Liraglutide on Blood Glucose Level
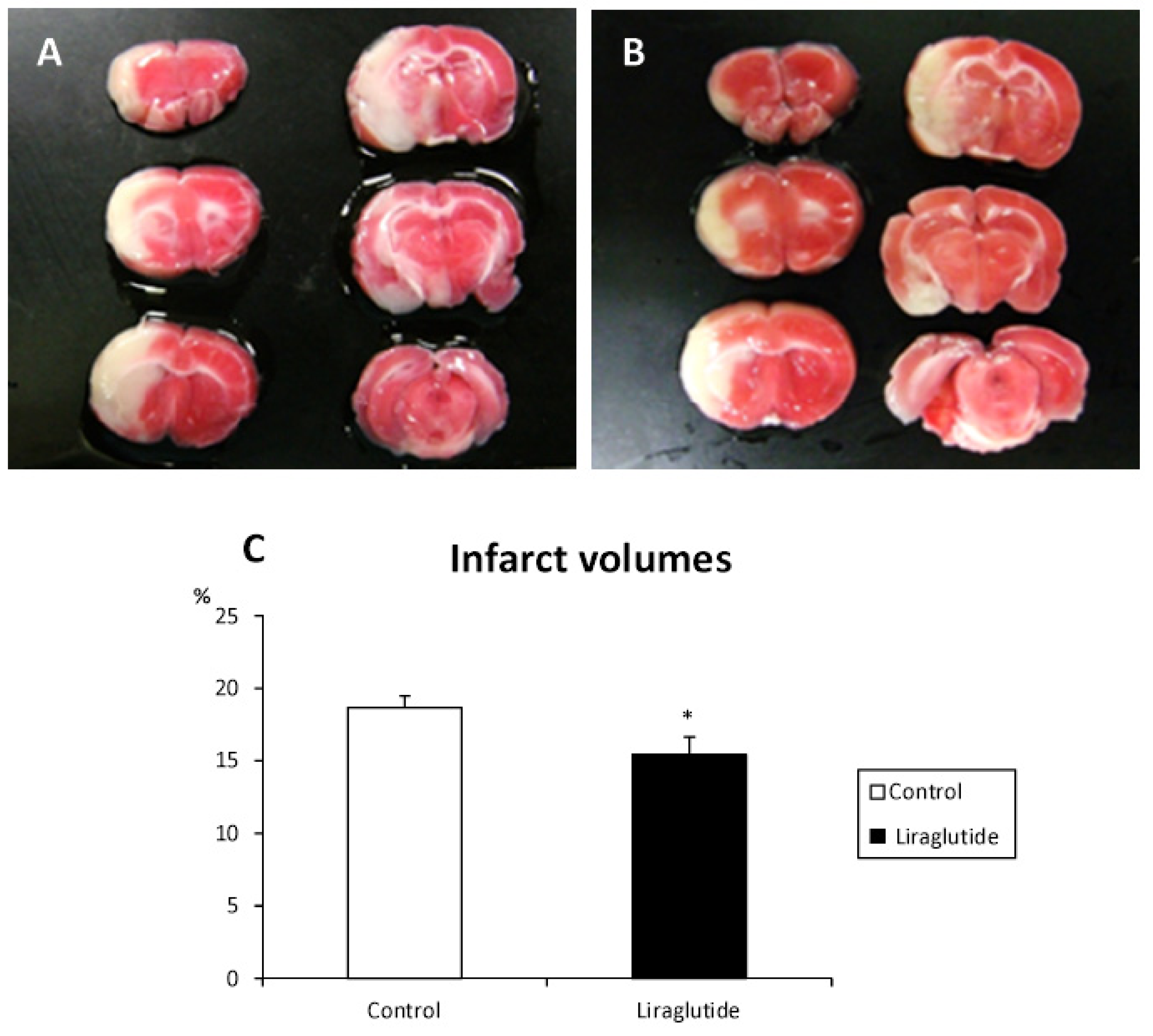
2.4. Reduction of Infarct Volumes in Liraglutide-Treated Rats
2.5. Decrease of d-ROMs in Liraglutide-Treated Rats
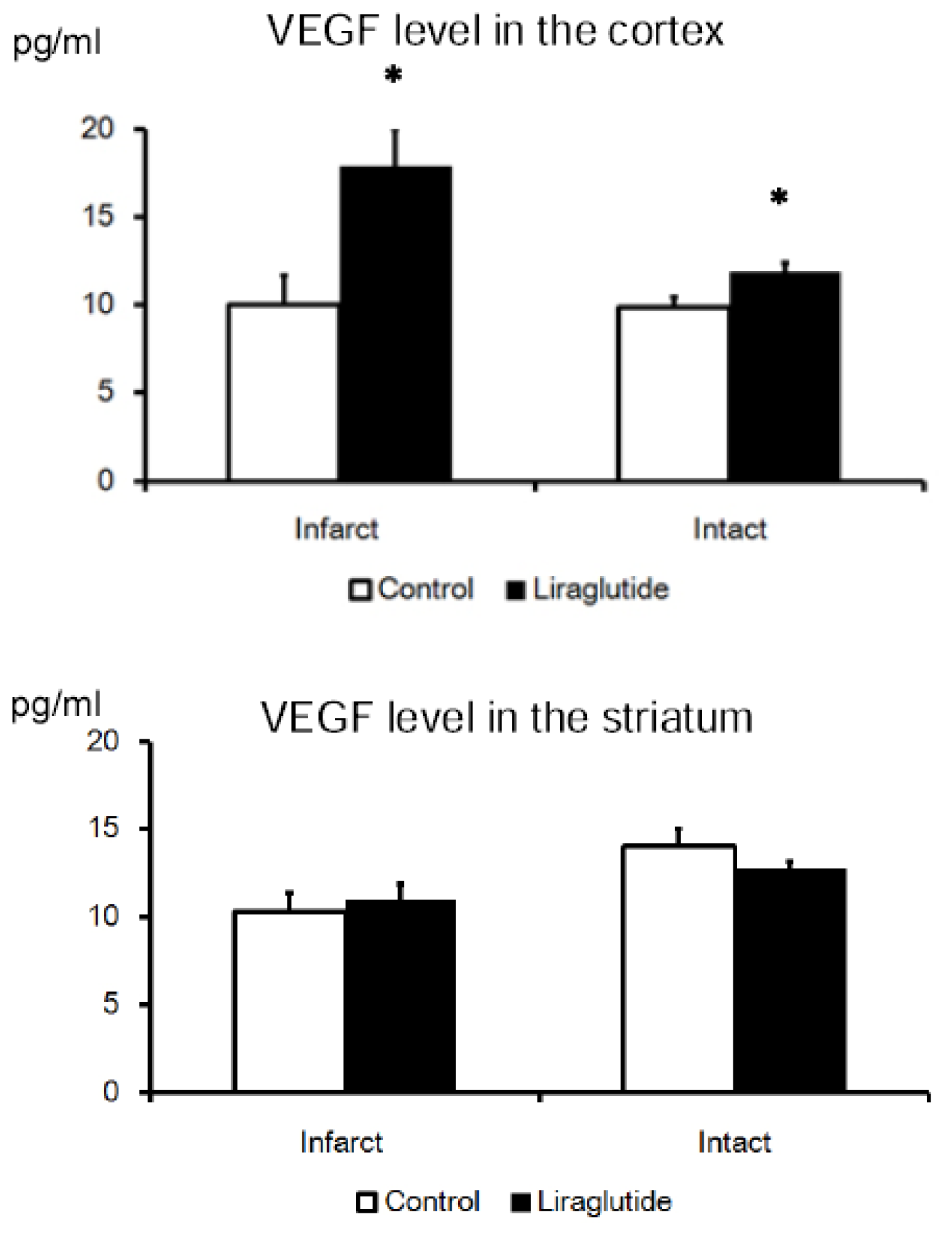
2.6. VEGF Upregulation in the Cortex of Liraglutide-Treated Rats, but Not in the Striatum
3. Discussion
3.1. GLP-1 Analogue and Diseases in the Central Nervous System
3.2. Anti-Oxidative Effects of GLP-1 and Its Analogue
3.3. Other Neuroprotective Mechanisms of GLP-1 Including Secretion of Neurohumoral Factors
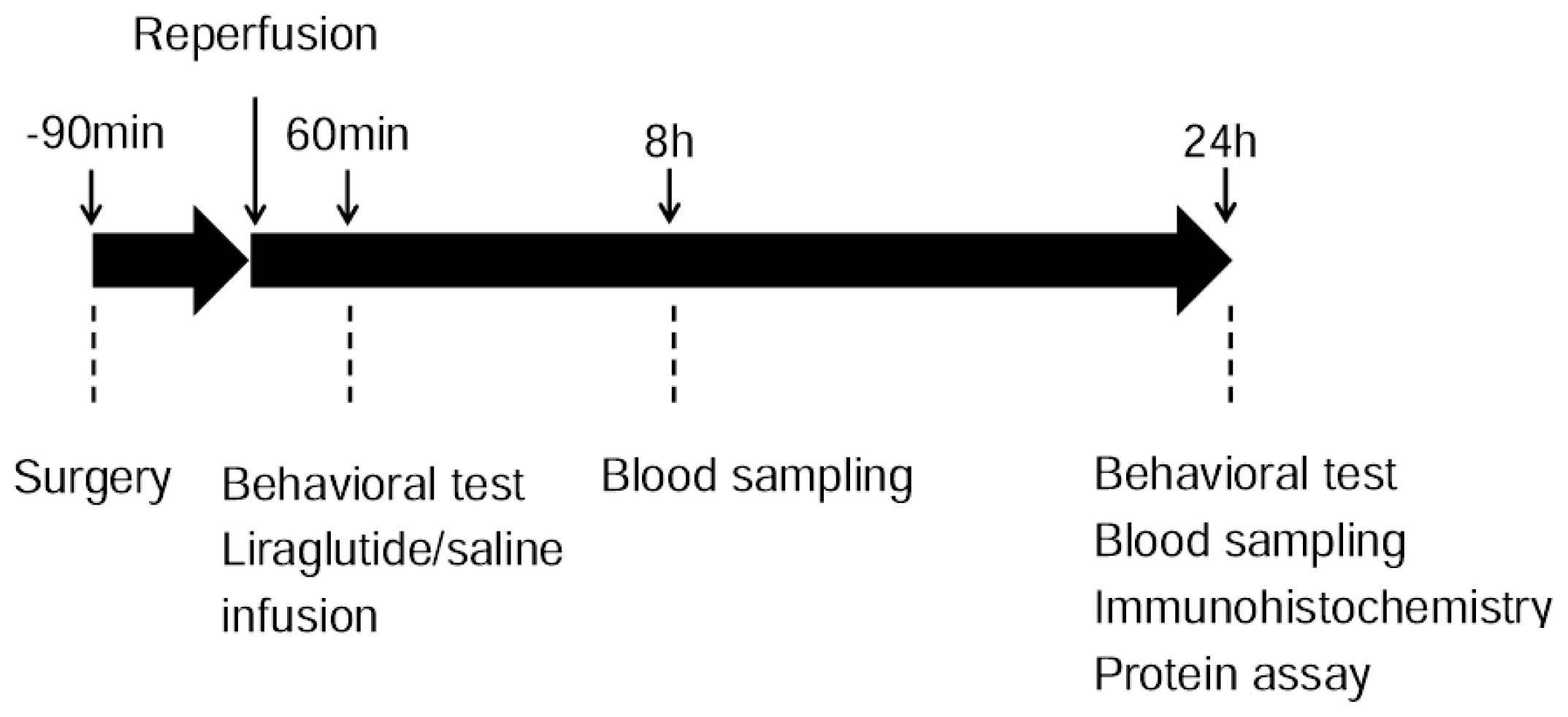
4. Experimental Section
4.1. Subjects
4.2. Experimental Groups
4.3. Transient Middle Cerebral Artery Occlusion
4.4. Measurement of Cortical Cerebral Blood Flow
4.5. Neurological Evaluation: Modified Bederson’s Score
4.6. Measurement of Blood Glucose Level
4.7. Measurement of the Infarct Volumes
4.8. Measurement of Oxidative Stress
4.9. VEGF ELISA
4.10. Statistical Analyses
5. Conclusions


Acknowledgments
Conflicts of Interest
References
- Nauck, M.A.; Meier, J.J. Glucagon-like peptide 1 and its derivatives in the treatment of diabetes. Regul. Pept 2005, 128, 135–148. [Google Scholar]
- Buse, J.B.; Rosenstock, J.; Sesti, G.; Schmidt, W.E.; Montanya, E.; Brett, J.H.; Zychma, M.; Blonde, L. LEAD-6 Study Group. Liraglutide once a day versus exenatide twice a day for type 2 diabetes: A 26-week randomised, parallel-group, multinational, open-label trial (LEAD-6). Lancet 2009, 374, 39–47. [Google Scholar]
- Holscher, C. Potential role of glucagon-like peptide-1 (GLP-1) in neuroprotection. CNS Drugs 2012, 26, 871–882. [Google Scholar]
- Darsalia, V.; Mansouri, S.; Ortsater, H.; Olverling, A.; Nozadze, N.; Kappe, C.; Iverfeldt, K.; Tracy, L.M.; Grankvist, N.; Sjoholm, A. Glucagon-like peptide-1 receptor activation reduces ischaemic brain damage following stroke in Type 2 diabetic rats. Clin. Sci 2012, 122, 473–483. [Google Scholar]
- Li, Y.; Chigurupati, S.; Holloway, H.W.; Mughal, M.; Tweedie, D.; Bruestle, D.A.; Mattson, M.P.; Wang, Y.; Harvey, B.K.; Ray, B.; et al. Exendin-4 ameliorates motor neuron degeneration in cellular and animal models of amyotrophic lateral sclerosis. PLoS One 2012, 7, e32008. [Google Scholar]
- Lee, C.H.; Yan, B.; Yoo, K.Y.; Choi, J.H.; Kwon, S.H.; Her, S.; Sohn, Y.; Hwang, I.K.; Cho, J.H.; Kim, Y.M.; et al. Ischemia-induced changes in glucagon-like peptide-1 receptor and neuroprotective effect of its agonist, exendin-4, in experimental transient cerebral ischemia. J. Neurosci. Res 2011, 89, 1103–1113. [Google Scholar]
- Teramoto, S.; Miyamoto, N.; Yatomi, K.; Tanaka, Y.; Oishi, H.; Arai, H.; Hattori, N.; Urabe, T. Exendin-4, a glucagon-like peptide-1 receptor agonist, provides neuroprotection in mice transient focal cerebral ischemia. J. Cereb. Blood Flow Metab 2011, 31, 1696–1705. [Google Scholar]
- Li, Y.; Perry, T.; Kindy, M.S.; Harvey, B.K.; Tweedie, D.; Holloway, H.W.; Powers, K.; Shen, H.; Egan, J.M.; Sambamurti, K.; et al. GLP-1 receptor stimulation preserves primary cortical and dopaminergic neurons in cellular and rodent models of stroke and Parkinsonism. Proc. Natl. Acad. Sci. USA 2009, 106, 1285–1290. [Google Scholar]
- Wang, M.D.; Huang, Y.; Zhang, G.P.; Mao, L.; Xia, Y.P.; Mei, Y.W.; Hu, B. Exendin-4 improved rat cortical neuron survival under oxygen/glucose deprivation through PKA pathway. Neuroscience 2012, 226, 388–396. [Google Scholar]
- McClean, P.L.; Parthsarathy, V.; Faivre, E.; Holscher, C. The diabetes drug liraglutide prevents degenerative processes in a mouse model of Alzheimer’s disease. J. Neurosci 2011, 31, 6587–6594. [Google Scholar]
- McClean, P.L.; Gault, V.A.; Harriott, P.; Holscher, C. Glucagon-like peptide-1 analogues enhance synaptic plasticity in the brain: A link between diabetes and Alzheimer’s disease. Eur. J. Pharmacol 2010, 630, 158–162. [Google Scholar]
- Egefjord, L.; Gejl, M.; Moller, A.; Braendgaard, H.; Gottrup, H.; Antropova, O.; Moller, N.; Poulsen, H.E.; Gjedde, A.; Brock, B.; et al. Effects of liraglutide on neurodegeneration, blood flow and cognition in Alzheimer’s disease—Protocol for a controlled, randomized double-blinded trial. Dan. Med. J 2012, 59, A4519. [Google Scholar]
- Hou, J.; Manaenko, A.; Hakon, J.; Hansen-Schwartz, J.; Tang, J.; Zhang, J.H. Liraglutide, a long-acting GLP-1 mimetic, and its metabolite attenuate inflammation after intracerebral hemorrhage. J. Cereb. Blood Flow Metab 2012, 32, 2201–2210. [Google Scholar]
- Padmasekar, M.; Lingwal, N.; Samikannu, B.; Chen, C.; Sauer, H.; Linn, T. Exendin-4 protects hypoxic islets from oxidative stress and improves islet transplantation outcome. Endocrinology 2013, 154, 1424–1433. [Google Scholar]
- Jimenez-Feltstrom, J.; Lundquist, I.; Salehi, A. Glucose stimulates the expression and activities of nitric oxide synthases in incubated rat islets: An effect counteracted by GLP-1 through the cyclic AMP/PKA pathway. Cell Tissue Res 2005, 319, 221–230. [Google Scholar]
- Erdogdu, O.; Eriksson, L.; Xu, H.; Sjoholm, A.; Zhang, Q.; Nystrom, T. Exendin-4 protects endothelial cells from lipoapoptosis by PKA, PI3K, eNOS, p38 MAPK, and JNK pathways. J. Mol. Endocrinol 2013, 50, 229–241. [Google Scholar]
- Morimoto, T.; Yasuhara, T.; Kameda, M.; Baba, T.; Kuramoto, S.; Kondo, A.; Takahashi, K.; Tajiri, N.; Wang, F.; Meng, J.; et al. Striatal stimulation nurtures endogenous neurogenesis and angiogenesis in chronic-phase ischemic stroke rats. Cell Transplant 2010, 20, 1049–1064. [Google Scholar]
- Hamilton, A.; Patterson, S.; Porter, D.; Gault, V.A.; Holscher, C. Novel GLP-1 mimetics developed to treat type 2 diabetes promote progenitor cell proliferation in the brain. J. Neurosci. Res 2011, 89, 481–489. [Google Scholar]
- Parthsarathy, V.; Holscher, C. Chronic treatment with the GLP1 analogue liraglutide increases cell proliferation and differentiation into neurons in an AD mouse model. PLoS One 2013, 8, e58784. [Google Scholar]
- Hunter, K.; Holscher, C. Drugs developed to treat diabetes, liraglutide and lixisenatide, cross the blood brain barrier and enhance neurogenesis. BMC Neurosci 2012, 13. [Google Scholar] [CrossRef] [Green Version]
- Xie, X.J.; Mo, Z.H.M.; Chen, K.; He, H.H.; Xie, Y.H. Glucagon-like peptide-1 improves proliferation and differentiation of endothelial progenitor cells via upregulating VEGF generation. Med. Sci. Monit 2011, 17, BR35–BR41. [Google Scholar]
- Yasuhara, T.; Date, I. Intracerebral transplantation of genetically engineered cells for Parkinson’s disease: Toward clinical application. Cell Transplant 2007, 16, 125–132. [Google Scholar]
- Yasuhara, T.; Shingo, T.; Date, I. The potential role of vascular endothelial growth factor in the central nervous system. Rev. Neurosci 2004, 15, 293–307. [Google Scholar]
- Borlongan, C.V.; Kaneko, Y.; Maki, M.; Yu, S.J.; Ali, M.; Allickson, J.G.; Sanberg, C.D.; Kuzmin-Nichols, N.; Sanberg, P.R. Menstrual blood cells display stem cell-like phenotypic markers and exert neuroprotection following transplantation in experimental stroke. Stem Cells Dev 2010, 19, 439–452. [Google Scholar]
- Guo, N.; Sun, J.; Chen, H.; Zhang, H.; Zhang, Z.; Cai, D. Liraglutide prevents diabetes progression in prediabetic OLETF rats. Endocr. J 2013, 60, 15–28. [Google Scholar]
- Baba, T.; Kameda, M.; Yasuhara, T.; Morimoto, T.; Kondo, A.; Shingo, T.; Tajiri, N.; Wang, F.; Miyoshi, Y.; Borlongan, C.V.; et al. Electrical stimulation of the cerebral cortex exerts antiapoptotic, angiogenic, and anti-inflammatory effects in ischemic stroke rats through phosphoinositide 3-kinase/Akt signaling pathway. Stroke 2009, 40, e598–e605. [Google Scholar]
- Kameda, M.; Shingo, T.; Takahashi, K.; Muraoka, K.; Kurozumi, K.; Yasuhara, T.; Maruo, T.; Tsuboi, T.; Uozumi, T.; Matsui, T.; et al. Adult neural stem and progenitor cells modified to secrete GDNF can protect, migrate and integrate after intracerebral transplantation in rats with transient forebrain ischemia. Eur. J. Neurosci 2007, 26, 1462–1478. [Google Scholar]
- Bederson, J.B.; Pitts, L.H.; Tsuji, M.; Nishimura, M.C.; Davis, R.L.; Bartkowski, H. Rat middle cerebral artery occlusion: Evaluation of the model and development of a neurologic examination. Stroke 1986, 17, 472–476. [Google Scholar]
- Liu, H.S.; Shen, H.; Harvey, B.K.; Castillo, P.; Lu, H.; Yang, Y.; Wang, Y. Post-treatment with amphetamine enhances reinnervation of the ipsilateral side cortex in stroke rats. NeuroImage 2011, 56, 280–289. [Google Scholar]
- Morishita, Y.; Hanawa, S.; Chinda, J.; Iimura, O.; Tsunematsu, S.; Kusano, E. Effects of aliskiren on blood pressure and the predictive biomarkers for cardiovascular disease in hemodialysis-dependent chronic kidney disease patients with hypertension. Hypertens. Res 2011, 34, 308–313. [Google Scholar]
© 2013 by the authors; licensee MDPI, Basel, Switzerland This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Sato, K.; Kameda, M.; Yasuhara, T.; Agari, T.; Baba, T.; Wang, F.; Shinko, A.; Wakamori, T.; Toyoshima, A.; Takeuchi, H.; et al. Neuroprotective Effects of Liraglutide for Stroke Model of Rats. Int. J. Mol. Sci. 2013, 14, 21513-21524. https://doi.org/10.3390/ijms141121513
Sato K, Kameda M, Yasuhara T, Agari T, Baba T, Wang F, Shinko A, Wakamori T, Toyoshima A, Takeuchi H, et al. Neuroprotective Effects of Liraglutide for Stroke Model of Rats. International Journal of Molecular Sciences. 2013; 14(11):21513-21524. https://doi.org/10.3390/ijms141121513
Chicago/Turabian StyleSato, Kenichiro, Masahiro Kameda, Takao Yasuhara, Takashi Agari, Tanefumi Baba, Feifei Wang, Aiko Shinko, Takaaki Wakamori, Atsuhiko Toyoshima, Hayato Takeuchi, and et al. 2013. "Neuroprotective Effects of Liraglutide for Stroke Model of Rats" International Journal of Molecular Sciences 14, no. 11: 21513-21524. https://doi.org/10.3390/ijms141121513




