Metabolic Profiles of Brain Metastases
Abstract
:1. Introduction
2. Results and Discussion
2.1. Histopathology
2.2. MR Metabolomics
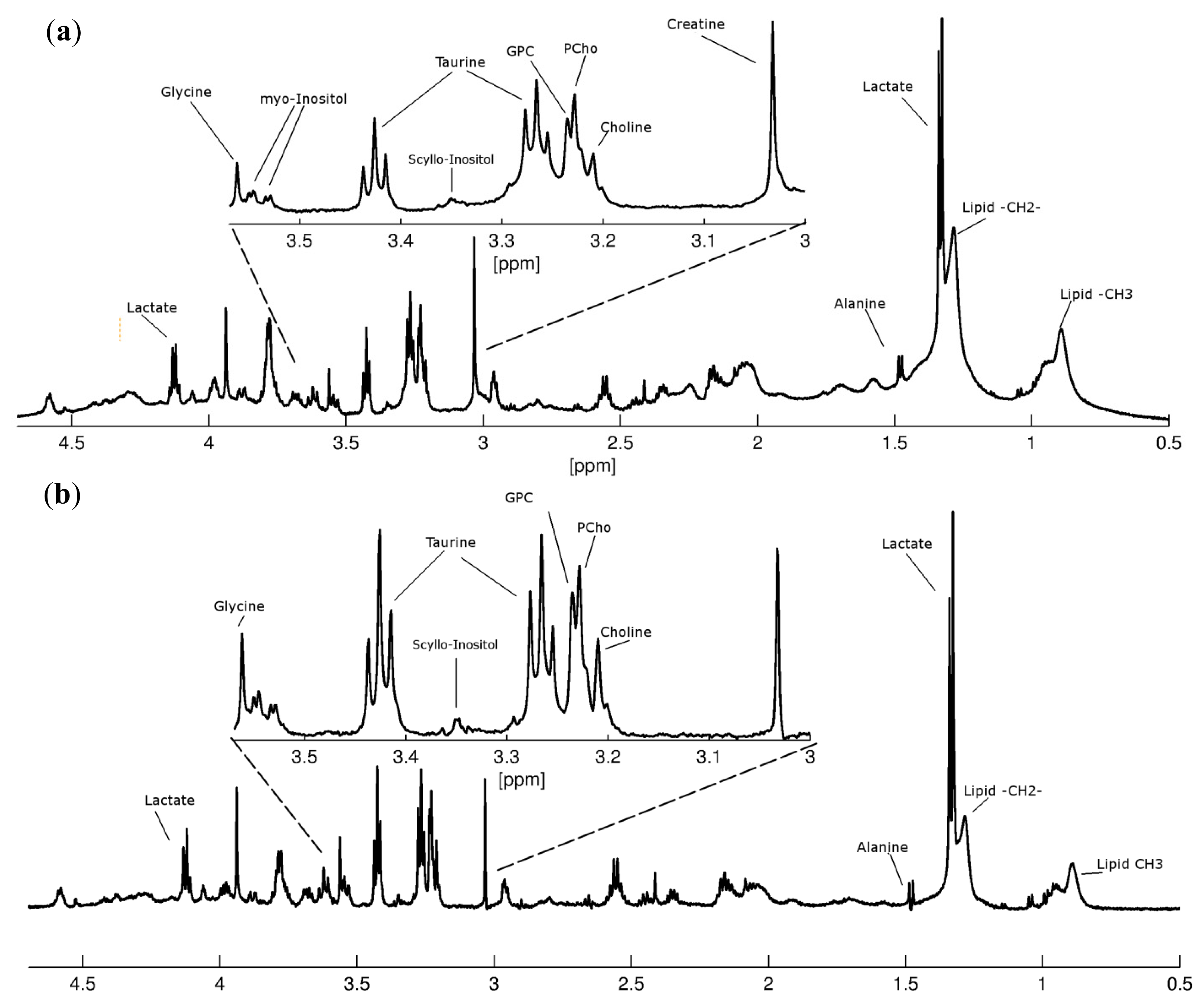
2.2.1. Brain Metastases and Lipid Metabolites
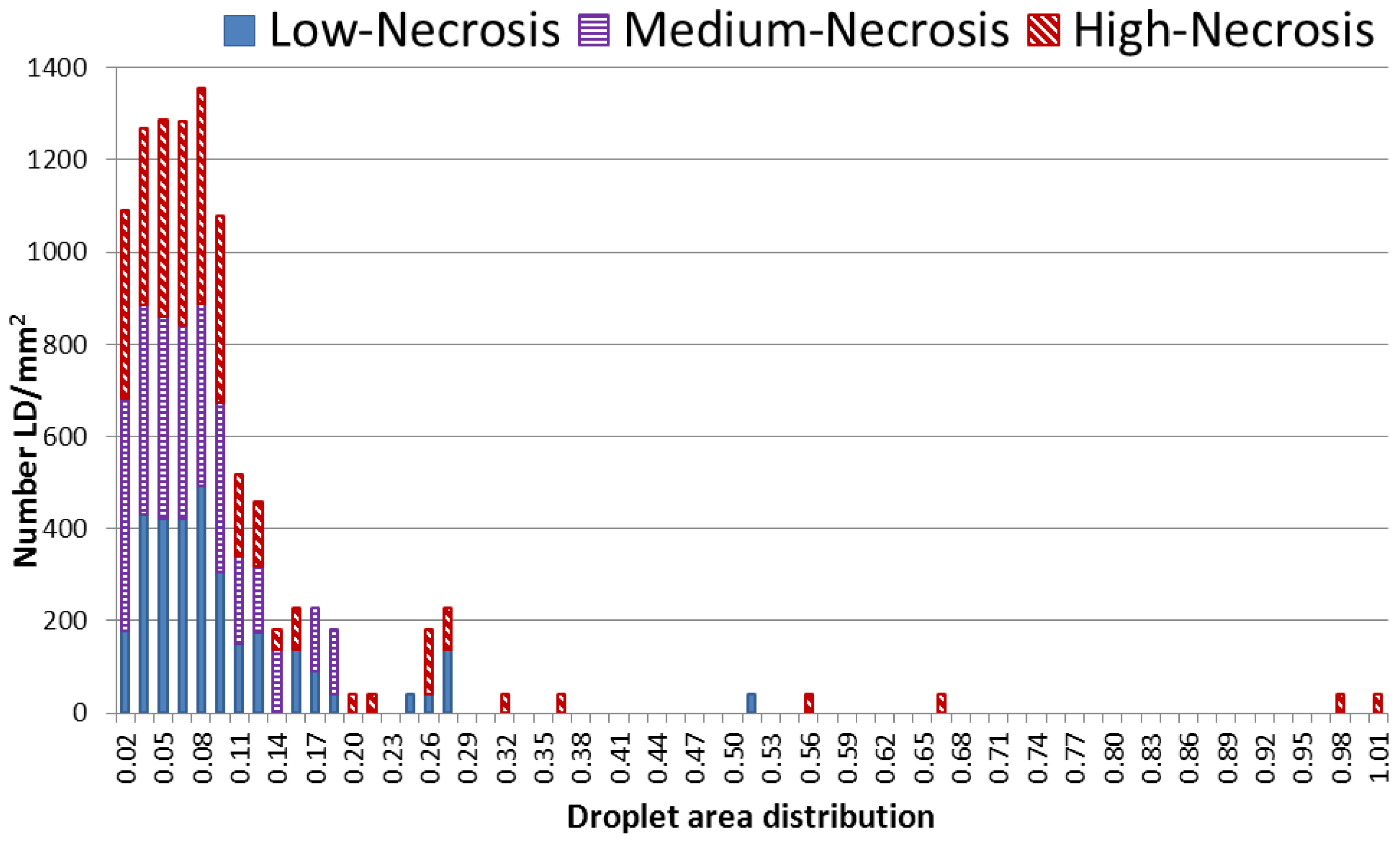
2.2.2. Nile Red Analysis of Lipid Droplets
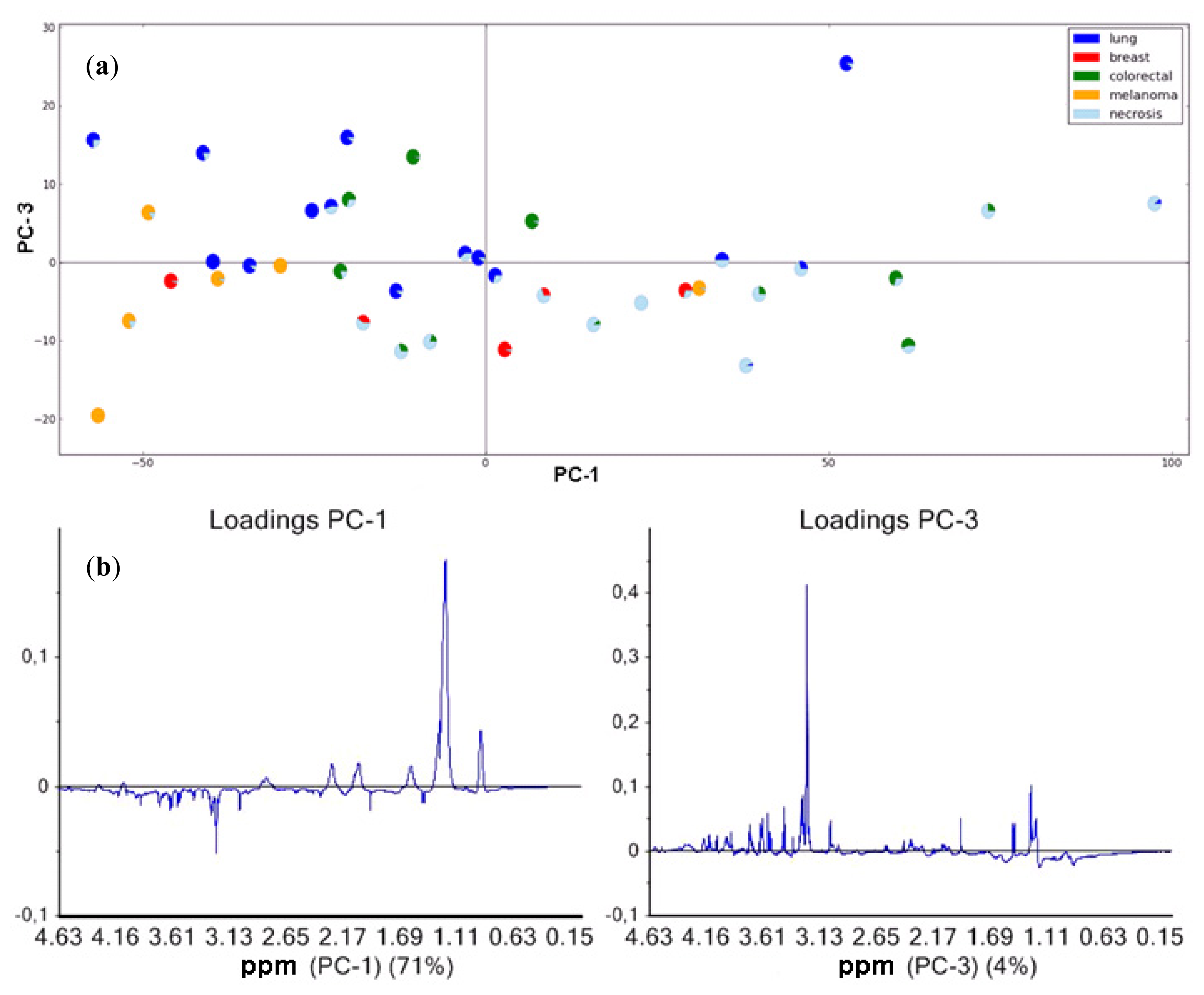
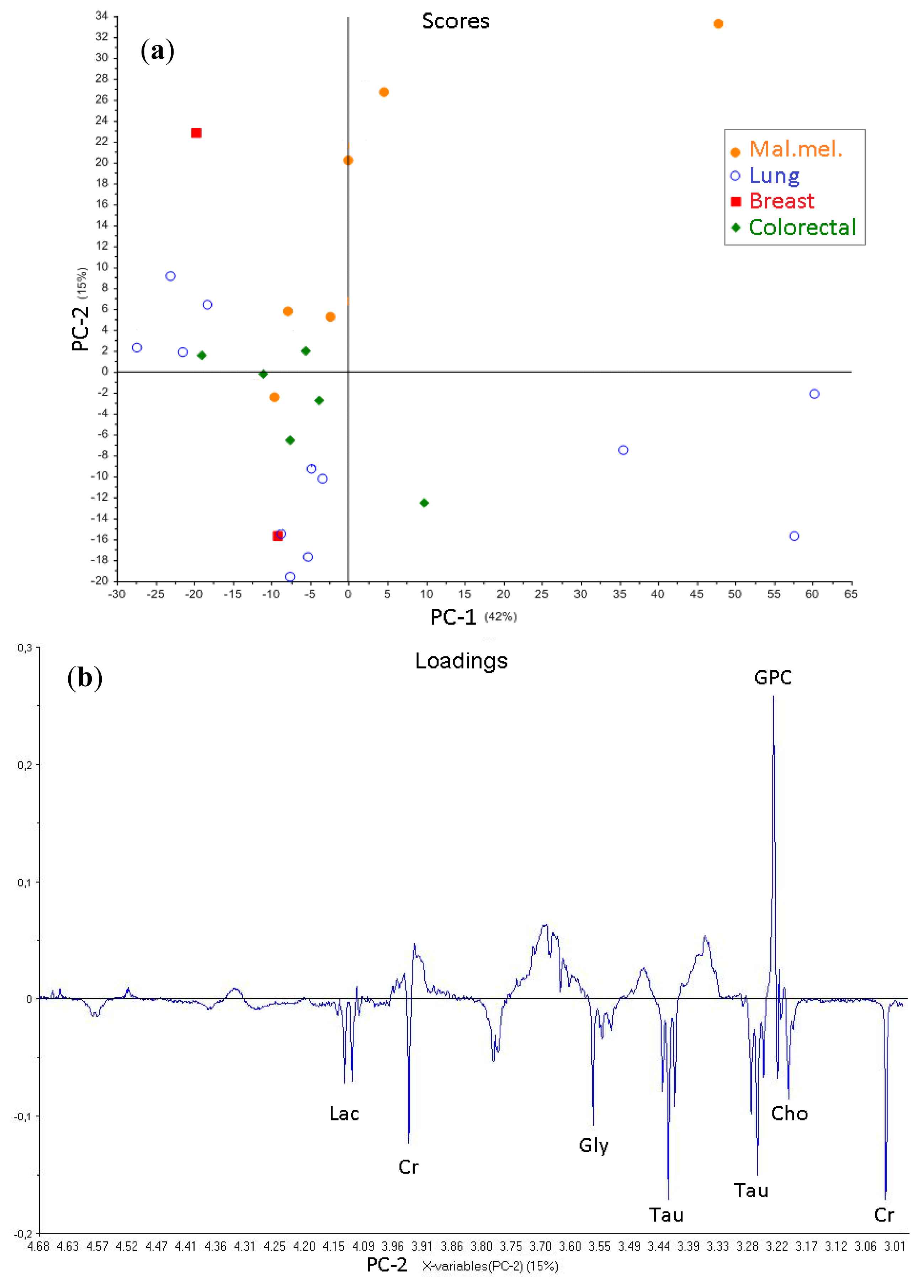
2.2.3. Brain Metastases and Low-Molecular-Weight Metabolites
3. Experimental Section
3.1. Patient and Sample Characterization
3.2. Sample Preparation and HR-MAS Experiments
3.3. Histopathological Examination
3.4. MR Metabolomics
4. Conclusions
Acknowledgments
- Conflict of InterestThe authors declare no conflict of interest.
References
- Barnholtz-Sloan, J.S.; Sloan, A.E.; Davis, F.G.; Vigneau, F.D.; Lai, P.; Sawaya, R.E. Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System. J. Clin. Oncol 2004, 22, 2865–2872. [Google Scholar]
- Gavrilovic, I.T.; Posner, J.B. Brain metastases: Epidemiology and pathophysiology. J. Neurooncol 2005, 75, 5–14. [Google Scholar]
- Gaspar, L.E.; Mehta, M.P.; Patchell, R.A.; Burri, S.H.; Robinson, P.D.; Morris, R.E.; Ammirati, M.; Andrews, D.W.; Asher, A.L.; Cobbs, C.S.; et al. The role of whole brain radiation therapy in the management of newly diagnosed brain metastases: A systematic review and evidence-based clinical practice guideline. J. Neurooncol 2010, 96, 17–32. [Google Scholar]
- Kalkanis, S.N.; Kondziolka, D.; Gaspar, L.E.; Burri, S.H.; Asher, A.L.; Cobbs, C.S.; Ammirati, M.; Robinson, P.D.; Andrews, D.W.; Loeffler, J.S.; et al. The role of surgical resection in the management of newly diagnosed brain metastases: A systematic review and evidence-based clinical practice guideline. J. Neurooncol 2010, 96, 33–43. [Google Scholar]
- Sperduto, C.M.; Watanabe, Y.; Mullan, J.; Hood, T.; Dyste, G.; Watts, C.; Bender, G.P.; Sperduto, P. A validation study of a new prognostic index for patients with brain metastases: the Graded Prognostic Assessment. J. Neurosurg 2008, 109, 87–89. [Google Scholar]
- Sperduto, P.W.; Berkey, B.; Gaspar, L.E.; Mehta, M.; Curran, W. A new prognostic index and comparison to three other indices for patients with brain metastases: An analysis of 1960 patients in the RTOG database. Int. J. Radiat. Oncol. Biol. Phys 2008, 70, 510–514. [Google Scholar]
- Nieder, C.; Marienhagen, K.; Geinitz, H.; Molls, M. Validation of the graded prognostic assessment index for patients with brain metastases. Acta Oncol 2009, 48, 457–459. [Google Scholar]
- Jakola, A.S.; Gulati, S.; Nerland, U.S.; Solheim, O. Surgical resection of brain metastases: the prognostic value of the graded prognostic assessment score. J. Neurooncol 2011, 105, 573–581. [Google Scholar]
- Jakola, A.S.; Gulati, S.; Nerland, U.S.; Solheim, O. Patient selection and clinical outcomes in patients operated for brain metastases--is specialty of the referring physicians a prognostic factor? Br. J. Neurosurg 2012, 26, 679–683. [Google Scholar]
- Tessem, M.B.; Selnaes, K.M.; Sjursen, W.; Trano, G.; Giskeodegard, G.F.; Bathen, T.F.; Gribbestad, I.S.; Hofsli, E. Discrimination of patients with microsatellite instability colon cancer using 1H HR MAS MR spectroscopy and chemometric analysis. J. Proteome Res 2010, 9, 3664–3670. [Google Scholar]
- Borgan, E.; Sitter, B.; Lingjaerde, O.C.; Johnsen, H.; Lundgren, S.; Bathen, T.F.; Sorlie, T.; Borresen-Dale, A.L.; Gribbestad, I.S. Merging transcriptomics and metabolomics--advances in breast cancer profiling. BMC Cancer 2010, 10. [Google Scholar] [CrossRef]
- Sitter, B.; Bathen, T.F.; Tessem, M.B.; Gribbestad, I.S. High-resolution magic angle spinning (HR MAS) MR spectroscopy in metabolic characterization of human cancer. Prog. Nucl. Mag. Res. Sp 2009, 54, 239–254. [Google Scholar]
- Martinez-Bisbal, M.C.; Celda, B. Proton magnetic resonance spectroscopy imaging in the study of human brain cancer. Q. J. Nucl. Med. Mol. Imaging 2009, 53, 618–630. [Google Scholar]
- Bathen, T.F.; Sitter, B.; Sjobakk, T.E.; Tessem, M.B.; Gribbestad, I.S. Magnetic resonance metabolomics of intact tissue: A biotechnological tool in cancer diagnostics and treatment evaluation. Cancer Res 2010, 70, 6692–6696. [Google Scholar]
- Cao, M.D.; Sitter, B.; Bathen, T.F.; Bofin, A.; Lonning, P.E.; Lundgren, S.; Gribbestad, I.S. Predicting long-term survival and treatment response in breast cancer patients receiving neoadjuvant chemotherapy by MR metabolic profiling. NMR Biomed 2012, 25, 369–378. [Google Scholar]
- Sjobakk, T.E.; Johansen, R.; Bathen, T.F.; Sonnewald, U.; Juul, R.; Torp, S.H.; Lundgren, S.; Gribbestad, I.S. Characterization of brain metastases using high-resolution magic angle spinning MRS. NMR Biomed 2008, 21, 175–185. [Google Scholar]
- Bertilsson, H.; Tessem, M.B.; Flatberg, A.; Viset, T.; Gribbestad, I.; Angelsen, A.; Halgunset, J. Changes in gene transcription underlying the aberrant citrate and choline metabolism in human prostate cancer samples. Clin. Cancer Res 2012, 18, 3261–3269. [Google Scholar]
- Callies, R.; Sri-Pathmanathan, R.M.; Ferguson, D.Y.; Brindle, K.M. The appearance of neutral lipid signals in the 1H NMR spectra of a myeloma cell line correlates with the induced formation of cytoplasmic lipid droplets. Magn. Reson. Med 1993, 29, 546–550. [Google Scholar]
- Hakumaki, J.M.; Kauppinen, R.A. 1H NMR visible lipids in the life and death of cells. Trends Biochem. Sci 2000, 25, 357–362. [Google Scholar]
- Hakumaki, J.M.; Liimatainen, T. Molecular imaging of apoptosis in cancer. Eur. J. Radiol 2005, 56, 143–153. [Google Scholar]
- Delikatny, E.J.; Chawla, S.; Leung, D.J.; Poptani, H. MR-visible lipids and the tumor microenvironment. NMR Biomed 2011, 24, 592–611. [Google Scholar]
- Howe, F.A.; Opstad, K.S. 1H MR spectroscopy of brain tumours and masses. NMR Biomed 2003, 16, 123–131. [Google Scholar]
- Sjobakk, T.E.; Johansen, R.; Bathen, T.F.; Sonnewald, U.; Kvistad, K.A.; Lundgren, S.; Gribbestad, I.S. Metabolic profiling of human brain metastases using in vivo proton MR spectroscopy at 3T. BMC Cancer 2007, 7. [Google Scholar] [CrossRef]
- Opstad, K.S.; Bell, B.A.; Griffiths, J.R.; Howe, F.A. Toward accurate quantification of metabolites, lipids, and macromolecules in HRMAS spectra of human brain tumor biopsies using LCModel. Magn. Reson. Med 2008, 60, 1237–1242. [Google Scholar]
- Opstad, K.S.; Bell, B.A.; Griffiths, J.R.; Howe, F.A. An investigation of human brain tumour lipids by high-resolution magic angle spinning 1H MRS and histological analysis. NMR Biomed 2008, 21, 677–685. [Google Scholar]
- Opstad, K.S.; Griffiths, J.R.; Bell, B.A.; Howe, F.A. Apparent T(2) relaxation times of lipid and macromolecules: a study of high-grade tumor spectra. J. Magn. Reson. Imaging 2008, 27, 178–184. [Google Scholar]
- Kuesel, A.C.; Sutherland, G.R.; Halliday, W.; Smith, I.C. 1H MRS of high grade astrocytomas: mobile lipid accumulation in necrotic tissue. NMR Biomed 1994, 7, 149–155. [Google Scholar]
- Righi, V.; Mucci, A.; Schenetti, L.; Bacci, A.; Agati, R.; Leonardi, M.; Schiavina, R.; Martorana, G.; Liguori, G.; Calabrese, C.; et al. Identification of mobile lipids in human cancer tissues by ex vivo diffusion edited HR-MAS MRS. Oncol. Rep 2009, 22, 1493–1496. [Google Scholar]
- Quintero, M.; Cabanas, M.E.; Arus, C. A possible cellular explanation for the NMR-visible mobile lipid (ML) changes in cultured C6 glioma cells with growth. Biochim. Biophys. Acta 2007, 1771, 31–44. [Google Scholar]
- Zoula, S.; Herigault, G.; Ziegler, A.; Farion, R.; Decorps, M.; Remy, C. Correlation between the occurrence of 1H-MRS lipid signal, necrosis and lipid droplets during C6 rat glioma development. NMR Biomed 2003, 16, 199–212. [Google Scholar]
- Duarte, I.F.; Rocha, C.M.; Barros, A.S.; Gil, A.M.; Goodfellow, B.J.; Carreira, I.M.; Bernardo, J.; Gomes, A.; Sousa, V.; Carvalho, L. Can nuclear magnetic resonance (NMR) spectroscopy reveal different metabolic signatures for lung tumours? Virchows Arch 2010, 457, 715–725. [Google Scholar]
- Greenspan, P.; Mayer, E.P.; Fowler, S.D. Nile red: A selective fluorescent stain for intracellular lipid droplets. J. Cell Biol 1985, 100, 965–973. [Google Scholar]
- Howe, F.A.; Barton, S.J.; Cudlip, S.A.; Stubbs, M.; Saunders, D.E.; Murphy, M.; Wilkins, P.; Opstad, K.S.; Doyle, V.L.; McLean, M.A.; et al. Metabolic profiles of human brain tumors using quantitative in vivo 1H magnetic resonance spectroscopy. Magn. Reson. Med 2003, 49, 223–232. [Google Scholar]
- Rocha, C.M.; Barros, A.S.; Gil, A.M.; Goodfellow, B.J.; Humpfer, E.; Spraul, M.; Carreira, I.M.; Melo, J.B.; Bernardo, J.; Gomes, A.; et al. Metabolic profiling of human lung cancer tissue by 1H high resolution magic angle spinning (HRMAS) NMR spectroscopy. J. Proteome Res 2010, 9, 319–332. [Google Scholar]
- Gulati, S.; Berntsen, E.M.; Solheim, O.; Kvistad, K.A.; Haberg, A.; Selbekk, T.; Torp, S.H.; Unsgaard, G. Surgical resection of high-grade gliomas in eloquent regions guided by blood oxygenation level dependent functional magnetic resonance imaging, diffusion tensor tractography, and intraoperative navigated 3D ultrasound. Minim. Invasive. Neurosurg 2009, 52, 17–24. [Google Scholar]
- Martinez-Bisbal, M.C.; Marti-Bonmati, L.; Piquer, J.; Revert, A.; Ferrer, P.; Llacer, J.L.; Piotto, M.; Assemat, O.; Celda, B. 1H and 13C HR-MAS spectroscopy of intact biopsy samples ex vivo and in vivo 1H MRS study of human high grade gliomas. NMR Biomed 2004, 17, 191–205. [Google Scholar]
- Sitter, B.; Sonnewald, U.; Spraul, M.; Fjosne, H.E.; Gribbestad, I.S. High-resolution magic angle spinning MRS of breast cancer tissue. NMR Biomed 2002, 15, 327–337. [Google Scholar]
- Wright, A.J.; Fellows, G.A.; Griffiths, J.R.; Wilson, M.; Bell, B.A.; Howe, F.A. Ex-vivo HRMAS of adult brain tumours: Metabolite quantification and assignment of tumour biomarkers. Mol. Cancer 2010, 9. [Google Scholar] [CrossRef]
- Savorani, F.; Tomasi, G.; Engelsen, S.B. icoshift: A versatile tool for the rapid alignment of 1D NMR spectra. J. Magn. Reson 2010, 202, 190–202. [Google Scholar]
- Wold, S.; Sjöström, M.; Eriksson, L. PLS-regression: A basic tool of chemometrics. Chemometr. Intell 2008, 58, 109–130. [Google Scholar]
- Snee, R.D. Validation of Regression Models: Methods and Examples. Technometrics 1977, 19, 415–428. [Google Scholar]
- Westerhuis, J.A.; Hoefsloot, H.C.J.; Smit, S.; Vis, D.J.; Smilde, A.K.; van Velzen, E.J.J.; van Duinhoven, J.P.M.; van Dorsten, F.A. Assessment of PLSDA cross validation. Metabolomics 2008, 4, 81–89. [Google Scholar]

| Origin of Carcinomas | |||||
|---|---|---|---|---|---|
| Variables | Total cohort | Lung | Colorectal | Breast | Melanoma |
| Numbers | 44 | 20 | 12 | 6 | 6 |
| Female/Male | 20/24 | 9/11 | 5/7 | 6/0 | 0/6 |
| Median Age at Surgery (Range) | 63 (37–80) | 69 (38–80) | 63 (43–81) | 53 (45–66) | 65 (53–76) |
| KPS%: | |||||
| 90–100 | 13 | 5 | 2 | 3 | 3 |
| 70–80 | 25 | 12 | 8 | 2 | 3 |
| <70 | 6 | 3 | 2 | 1 | 0 |
| Five Month Postoperative Survival | 28 | 12 | 9 | 4 | 3 |
| Origin Carcinomas of the Brain Metastases: | Tumor (%) | Necrosis (%) | Fibrosis (%) |
|---|---|---|---|
| Lung (n = 17) | 49 ± 31 | 36 ± 34 | 12 ± 17 |
| Colorectal (n = 11) | 35 ± 24 | 48 ± 32 | 14 ± 23 |
| Breast (n = 5) | 25 ± 5 | 34 ± 30 | 35 ± 27 |
| Malignant Melanoma (n = 6) | 83 ± 15 | 8 ± 8 | 10 ± 15 |
© 2013 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Sjøbakk, T.E.; Vettukattil, R.; Gulati, M.; Gulati, S.; Lundgren, S.; Gribbestad, I.S.; Torp, S.H.; Bathen, T.F. Metabolic Profiles of Brain Metastases. Int. J. Mol. Sci. 2013, 14, 2104-2118. https://doi.org/10.3390/ijms14012104
Sjøbakk TE, Vettukattil R, Gulati M, Gulati S, Lundgren S, Gribbestad IS, Torp SH, Bathen TF. Metabolic Profiles of Brain Metastases. International Journal of Molecular Sciences. 2013; 14(1):2104-2118. https://doi.org/10.3390/ijms14012104
Chicago/Turabian StyleSjøbakk, Torill E., Riyas Vettukattil, Michel Gulati, Sasha Gulati, Steinar Lundgren, Ingrid S. Gribbestad, Sverre H. Torp, and Tone F. Bathen. 2013. "Metabolic Profiles of Brain Metastases" International Journal of Molecular Sciences 14, no. 1: 2104-2118. https://doi.org/10.3390/ijms14012104





