Invasive Fungal Infections in the ICU: How to Approach, How to Treat
Abstract
:1. Introduction
2. Candida Invasive Disease
3. Incidence, Trends and Mortality
4. The Changing Epidemiology of Candida spp.
| C. glabrata | Most common in elderly patients |
| Most common in malignancies | |
| Geographic variation | |
| Associated to the use of specific antibiotics, (piperacillin/tazobactam, vancomycin) | |
| Common in patients under TPN and with CVC | |
| Isolation system | |
| Solid organ transplantation | |
| Fluconazole exposure | |
| C. parapsilosis | Nosocomial outbreaks |
| Formation of biofilms in CVC | |
| Implanted devices | |
| TPN | |
| Less susceptible to echinocandins | |
| The second most common isolated strain in children | |
| C. tropicalis | Haematological malignancies |
| Neutropenia | |
| C. krusei | Use of piperacillin/tazobactam, vancomycin |
| Innate resistance to fluconazole | |
| Haematological malignancies | |
| Neutropenia | |
| Recent gastrointestinal surgery | |
| Fluconazole exposure | |
| C. guiillermondi | Less susceptible to echinocandins |
| Less susceptible to fluconazole | |
| Intravascular catheters |
5. Laboratory Diagnostic Methods
6. Risk Factor Assessment
| Prolonged ICU stay |
| Treatment with corticosteroids |
| Diabetes mellitus |
| Advanced age |
| Central venous catheter |
| Gastrointestinal surgery |
| Total parenteral nutrition |
| Prolonged antimicrobial use |
| Pancreatitis |
| Immunosuppressive agents |
| Chemotherapy |
| High disease severity score (APACHE II > 20) |
| Neutropenia |
| Renal replacement therapy |
| Malnutrition |
| Multiple site colonisation |
| Burns over 50% of body sites |
| Major trauma |
| Authors | Aims and Criteria | Factors and Prediction Rule |
| Leon [56] | Surgical patients | “Candida score” Factors leading to invasive candidiasis development include multifocal colonisation, surgery on ICU admission, severe sepsis, TPN. A “Candida score” > 2.5 selects the non-neutropenic ICU patients who might benefit from early antifungal treatment |
| Agvald-Ȍhman [58] | To identify patients at risk of IC among those with a length of ICU stay of at least 7 days | Candida colonisation index ≥ 0.8 and recent extensive gastroabdominal surgery |
| Pittet [59] | Surgical and neonatal ICUs To identify patients in surgical and neonatal ICUs at increased risk of subsequent infection. | CCI = Candida Colonisation Index. Patients with CCI ≥ 0.5 at high risk. |
| Dupont [60] | Patients with severe peritonitis | Presence of at least three of female sex, cardiovascular failure, upper gastrointestinal tract origin, ongoing antimicrobial therapy predicts yeast isolation in the peritoneal fluid |
| Ostrosky-Zeichner [61] | To identify patients at increased risk of IC in medical and surgical ICUs | Any systemic antibiotic (days 1–3) ORCVC (days 1–3) AND at least TWO of the following: TPN (days 1–3), any dialysis (days 1–3), any major surgery (days 7–0), pancreatitis (days 7–0), steroid use (days -7–3). other immunosuppressive drug (days 7–0) |
| Hermsen [62] | Due to the high Negative Predictive Value, the rule applies best to identify patients who are LEAST likely to benefit from antifungal therapy | Current systemic broad-spectrum antibiotic use, CVC, TPN, abdominal surgery within last 7 days, steroid use, hospital LOS |
| Paphitou [63] | To identify patients at increased risk of invasive candidiasis in surgical ICUs | Presence of new onset hemodialysis, TPN, diabetes mellitus and broad-spectrum antibiotics predict invasive candidiasis |
| Ostrosky-Zeichner [64] | To identify patients at increased risk of invasive candidiasis in the ICU | Mechanical ventilation (days 1–3) AND CVC (days 1–3) AND at least ONE of the following TPN (days 1–3), any dialysis (days 1–3), any major surgery (days 7–0), pancreatitis (by CT or lipase >1000iu, days 7–0), steroid use (>1dose of prednisone equivalent to 20mg, days 7–0), other immunosuppressive drug (>1 dose, days 7–0) |
7. Aspergillus
8. Mucorales
| Diagnostic method | Aspergillus | Mucorales |
|---|---|---|
| Histopathology | Definite diagnosis | Definite diagnosis |
| Radiology | No specific findings | No specific findings |
| Blood cultures | Extremely rare | Extremely rare |
| Respiratory samples cultures | Sens: 10%–80% | Sens: 67%, Spec: 100% (BAL) |
| qPCR blood-BAL | Sens: 67%–100%, Spec: 55%–95% | Sens: 40%–90%, Spec: 100% |
| Antigen assays | Galactomannans (GMI) 1 > 0.5
Sens: 71% (BAL 88%), Spec: 89% 1 (BAL 86%) | Investigational
|
| 1,3-β-glucan
“Panfungal marker” | No | |
| Algorithms | EORTC/MSG criteria 2 Vandewoude and collegues 3 Sens: 61%, Spec: 92% |
9. Antifungal Compounds
9.1. The Role of Polyenes/Amphotericin B
9.2. Azoles
9.2.1. Itraconazole
9.2.2. Fluconazole
9.2.3. Voriconazole
9.2.4. Posaconazole
9.3. Echinocandins
9.4. Pyrimidine Analogues
10. Future Therapeutic Options
| Caspofungin | Micafungin | Anidulafungin |
|---|---|---|
| Some interactions with rifampin, phenytoin, carbamazepine, antiretroviral agents and dexamethasone [ 140] | Lacks efficacy and safety data in patients with severe hepatic impairment. | Does not undergo any degree of hepatic or renal metabolism |
| Interactions with cyclosporin A (liver function abnormalities) [ 141] | Reported formation of liver tumors in rodents rose some concern about its use ( in humans no similar effects have been shown) [ 142] | No dose adjustement is necessary in patients with hepatic or renal impairment |
| Antifungal drug | C. albicans | C. parapsilosis | C. glabrata | Aspergillus | Mucorales | Cryptococcus | Dose | Dose in Renal failure |
|---|---|---|---|---|---|---|---|---|
| AmB | S | S | S | S * | S | S | 0.5–1 mg/kg/d | same |
| lipAmB | S | S | S | S * | S | S | 3–5 mg/kg/d | same |
| Fluconazole | S | S | SDd - R | R | R | S | 800 mg (12 mg/kg) l d
400 mg (6 mg/kg) | Adjustment of the dose |
| Itraconazole | S | S | SDd - R | S | R | Ms | 200 mgIV/bid 2 d
then 200 mg/d | same |
| Posaconazole | S | S | SDd - R | S | S | S | 200 mg qid | Same in mild, moderate |
| Voriconazole | S | S | SDd - R | S | R | S | 400 mg/bid
then 200 mg/bid | IV not given inCrcl < 50 mL/min |
| Flucytosine | S | S | S | R | R | S | 50–150 mg/kg
in 4 doses | Adjustment of the dose |
| Caspofungin | S | Rc | S | S | R | R | 70 mg/d
l dthen 50 mg/d | same |
| Micafungin | S | Rc | S | S | R | R | 100 mg/d | same |
| Anidulafungin | S | Rc | S | S | R | R | 200 mg/d
l d, then 100 mg/d | same |
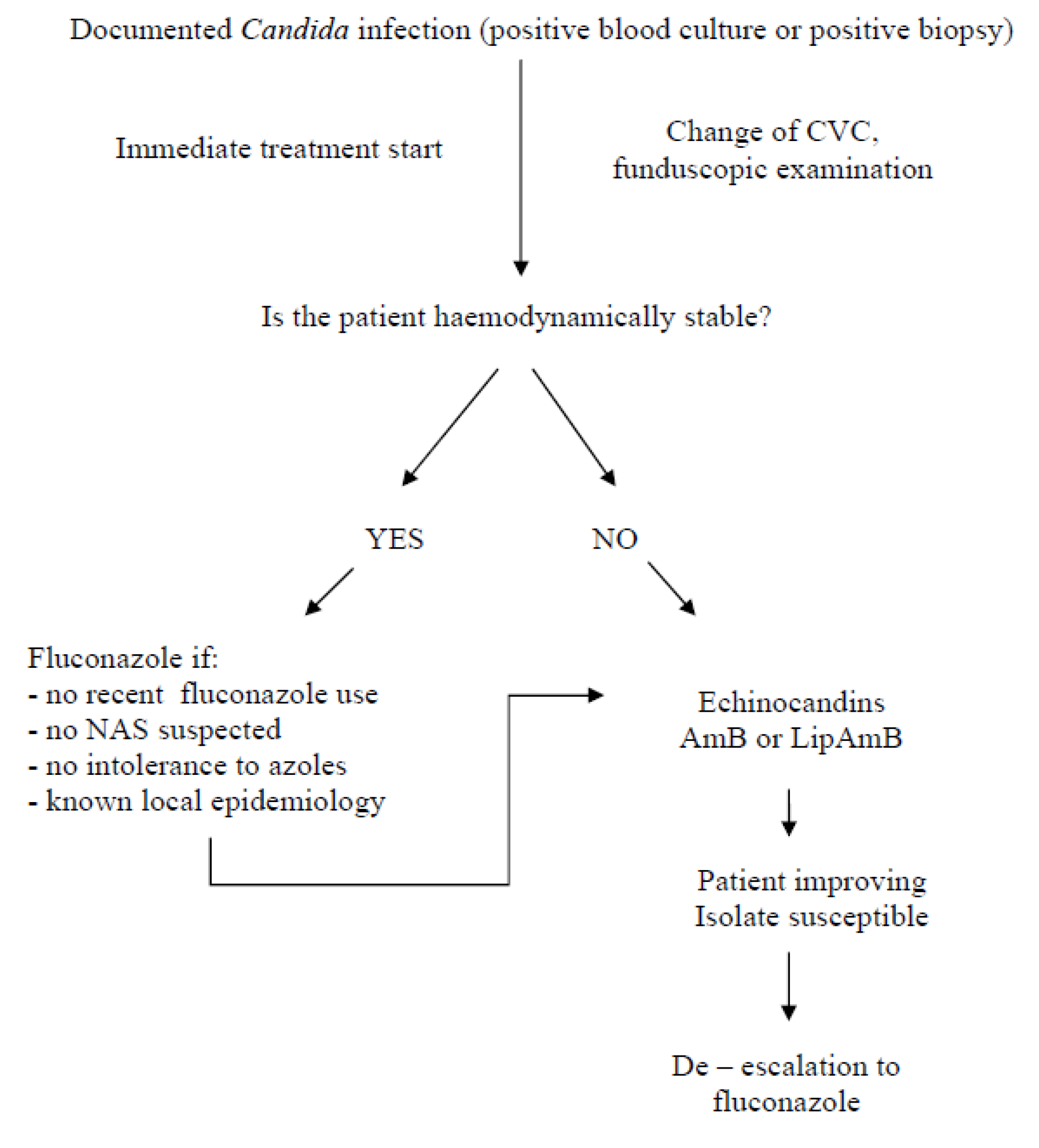
11. Management of Candidiasis in the ICU
11.1. Documented Invasive Candidiasis
| Society | First line | Alternative I | Alternative II |
|---|---|---|---|
| IDSA [114] | Fluconazole | AmB or lipid formulations of AmB (intolerance to others or limited availability) | Voriconazole |
| -stable patient, azole naïve | |||
| Echinocandins | |||
| -severe sepsis | |||
| -recent azole exposure | |||
| ESCMID [151] | Echinocandins | LipAmB, voriconazole | fluconazole, lcAmB |
| European Expert Opinion [152] | Fluconazole | lipidformulations of amphotericin B | |
| - stable patient | |||
| - susceptible isolate | |||
| Echinocandins | |||
| - severe sepsis | |||
| - micafungin last choice | |||
| Canadian clinical practice guidelines for invasive candidiasis in adults [150] | Fluconazole | LipAmB or AmB | |
| -stable patient, azole naïve | |||
| -unstable patient with C.parapsilosis | |||
| Echinocandins | |||
| -stable or unstable patient | |||
| -recent azole exposure | |||
| -avoid in C.parapsilosis | |||
| Joint recommendations of the German speaking mycological society [154] | Fluconazole | Lip AmB -critically ill, septic patients voriconazole | |
| -stable patient | |||
| -susceptible isolate | |||
| Echinocandins | |||
| -critically ill septic patient |
| Infection type | Suggested treatment |
|---|---|
| Pyelonephritis | fluconazole 3–6 mg/kg/d (14 days) or AmB 0.3–0.6 mg/kg/d for 1–7 days |
| Urinary fungus ball | Surgical removal recommended fluconazole 3–6 mg/kg/d or AmB 0.5–0.7 mg/kg/d |
| Candida osteomyelitis | fluconazole 6 mg/kg/d (6–12months) or LipAmB 3–5 mg/kg/d (weeks), then fluconazole for 6–12 months |
| Septic arthritis | fluconazole 6 mg/kg/d (6 weeks) or LipAmB 3–5 mg/kg/d (weeks) then fluconazole |
| CNS infection | LipAmB 3–5 mg/kg (±5FTC 25mg/kg/qid) several weeks, then fluconazole (6–12 mg/kg/d) daily or fluconazole 400–800 mg/d in LipAmB intolerance |
| Endocarditis | LipAmB 3–5 mg/kg (±5FTC 25mg/kg qid) or AmB 0.6–1 mg/kg/d (±5FTC 25 mg/kg) or an echinocandin |
| Suppurative thrombophlebitis | LipAmB 3–5 mg/kg/d or fluconazole 400–800 mg d or an echinocandins |
| Endophthalmitis | AmB 0.7–1 mg/kg plus 5FTC or fluconazole 6–12 mg/kg/d or LipAmB 3–5 mg/kg/d or voriconazole 6 mg/kg/12 h, then 3 mg/kg/12 h or echinocandins |
11.2. Combination Treatment
11.3. Other Treatment Options
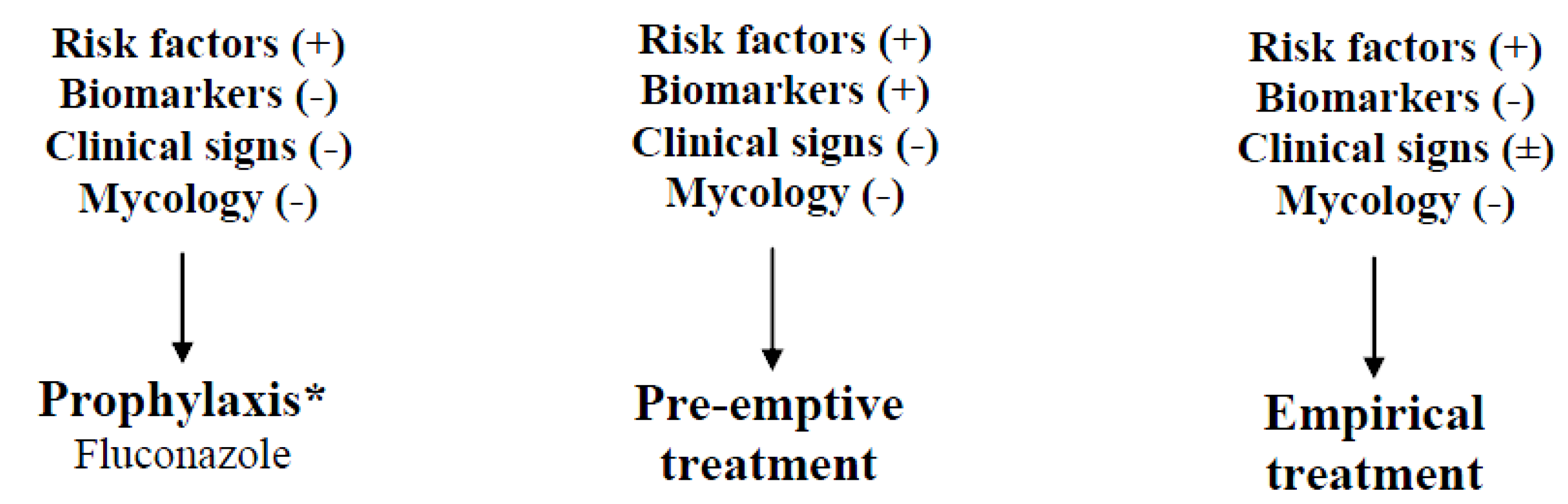
11.3.1. Prophylaxis
11.3.2. Pre-Emptive Treatment
11.3.3. Empirical Treatment
12. Treatment of Invasive Aspergillosis
13. Treatment Of Mucorales Infection
14. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Blot, S.; Dimopoulos, G.; Rello, J.; Vogelaers, D. Is Candida really a threat in the ICU? Curr. Opin. Crit. Care 2008, 14, 600–604. [Google Scholar] [CrossRef]
- Darouiche, R.O. Candida in the ICU. Clin. Chest Med. 2009, 30, 287–293. [Google Scholar] [CrossRef]
- Vincent, J.L.; Rello, J.; Marshall, J.; Silva, E.; Anzueto, A.; Martin, C.D.; Moreno, R.; Lipman, J.; Gomersall, C.; Sakr, Y. Konrad ReinhartInternational study of the prevalence and outcomes of infection in intensive care units. JAMA 2009, 21, 2323–2329. [Google Scholar]
- Falagas, M.E.; Apostolou, K.E.; Pappas, V.D. Attributable mortality of candidemia: A systematic review of matched cohort and case-control studies. Eur. J. Clin. Microbiol. Infect. Dis. 2006, 25, 419–425. [Google Scholar] [CrossRef]
- Gagne, J.J.; Goldfarb, N.I. Candidaemia in the in–patient setting. Expert Opin. Pharmacother. 2007, 8, 1643–1650. [Google Scholar] [CrossRef]
- Fridkin, K.; Jarvis, R. Epidemiology of nosocomial fungal infections. Clin. Microbiol. Rev. 1996, 9, 499–511. [Google Scholar]
- Pfaller, M.; Diekema, D.J. Epidemiology of invasive candidiasis: A persistent public health problem. Clin. Microbiol. Rev. 2007, 20, 133–163. [Google Scholar] [CrossRef]
- Tragiannidis, A.; Tsoulas, C.; Kerl, K.; Groll, A.H. Invasive candidiasis: Update on current pharmacotherapy options and future perspectives. Expert Opin. Pharmacother. 2013, 14, 1515–1528. [Google Scholar] [CrossRef]
- Asmundsdottir, L.R.; Erlendsdottir, H.; Haraldsson, G.; Guo, H.; Xu, J.; Gottfredsson, M. Molecular epidemiology of candidemia: Evidence of clusters of smoldering nosocomial infections. Clin. Infect. Dis. 2008, 47, e17–e24. [Google Scholar] [CrossRef]
- Concia, E.; Azzini, A.M.; Conti, M. Epidemiology, incidence and risk factors for invasive candidiasis in high-risk patients. Drugs 2009, 69, 5–14. [Google Scholar] [CrossRef]
- Wisplinghoff, H.; Bischoff, T.; Tallent, S.M.; Seifert, H.; Wenzel, RP.; Edmond, M.B. Nosocomial bloodstream infections in US hospitals: Analysis of 24,179 cases from a prospective nationwide surveillance study. Clin. Infect. Dis. 2004, 39, 309–317. [Google Scholar] [CrossRef]
- Almirante, B.; Rodriguez, D.; Park, B.J.; Cuenca-Estrella, M.; Planes, A.M.; Almela, M.; Mensa, J.; Sanchez, F.; Ayats, J.; Gimenezet, M.; et al. Epidemiology and predictors of mortality in cases of Candida bloodstream infection: Results from population-based surveillance, Barcelona, Spain, from 2002 to 2003. J. Clin. Microbiol. 2005, 43, 1829–1835. [Google Scholar] [CrossRef]
- Asmundsdottir, L.R.; Erlendsdottir, H.; Gottfredsson, M. Nationwide study of candidemia, antifungal use and antifungal drug resistance in Iceland, 2000 to 2011. J. Clin. Microbiol. 2013, 51, 841–848. [Google Scholar] [CrossRef]
- Tortorano, A.M.; Peman, J.; Bernhardt, H.; Klingspor, L.; Kibbler, C.C.; Faure, O.; Biraghi, E.; Canton, E.; Zimmermann, K.; Seaton, S.; et al. Epidemiology of candidaemia in Europe: Results of 28-month European Confederation of Medical Mycology (ECMM) hospital-based surveillance study. Eur. J. Clin. Microbiol. Infect. Dis. 2004, 23, 317–322. [Google Scholar] [CrossRef]
- Prowle, J.R.; Echeverri, J.E.; Ligabo, E.V.; Sherry, N.; Taori, G.C.; Crozier, T.M.; Biraghi, E.; Canton, E.; Zimmermann, K.; Seaton, S.; et al. Acquired bloodstream infection in the intensive care unit: Incidence and attributable mortality. Crit. Care 2011, 15, R100. [Google Scholar] [CrossRef]
- Meyer, E.; Geffers, C.; Gastmeier, P.; Schwab, F. No increase in primary nosocomial candidemia in 682 German intensive care units during 2006 to 2011. Euro. Surveill. 2013, 18. [Google Scholar] [CrossRef]
- Montagna, M.T.; Caggiano, G.; Lovero, G.; de Giglio, O.; Coretti, C.; Cuna, T.; Iatta, R.; Giglio, M.; Dalfino, L.; Bruno, F.; et al. Epidemiology of invasive fungal infections in the intensive care unit: Results of a multicenter Italian survey (AURORA Project). Infection 2013, 41, 645–653. [Google Scholar] [CrossRef]
- Quenot, J.P.; Binquet, C.; Kara, F.; Martinet, O.; Ganster, F.; Navellou, J.C.; Castelain, V.; Barraud, D.; Cousson, J.; Louis, G.; et al. The epidemiology of septic shock in French intensive care units: The prospective multicenter cohort EPISS study. Crit. Care 2013, 17, R65. [Google Scholar] [CrossRef]
- Tabah, A.; Koulenti, D.; Laupland, K.; Misset, B.; Valles, J.; Bruzzi de Carvalho, F.; Paiva, J.A.; Cakar, N.; Ma, X.; Eggimann, P.; et al. Characteristics and determinants of outcome of hospital-acquired bloodstream infections in intensive care units: The EUROBACT International Cohort Study. Intensiv. Care Med. 2012, 38, 1930–1945. [Google Scholar] [CrossRef]
- Alangaden, G.J. Nosocomial fungal infections: Epidemiology, infection control, and prevention. Infect. Dis. Clin. North. Am. 2011, 1, 201–225. [Google Scholar] [CrossRef]
- Mikulska, M.; Calandra, T.; Sanguinetti, M.; Poulain, D.; Viscoli, C. The use of mannan antigen and anti-mannan antibodies in the diagnosis of invasive candidiasis: Recommendations from the Third European Conference on Infections in Leukemia. Crit. Care 2010, 14, R222. [Google Scholar] [CrossRef]
- Zaoutis, T.E.; Argon, J.; Chu, J.; Berlin, J.A.; Walsh, T.J.; Feudtner, C. The epidemiology and attributable outcomes of candidemia in adults and children hospitalized in the United States: A propensity analysis. Clin. Infect. Dis. 2005, 41, 1232–1239. [Google Scholar] [CrossRef]
- Falagas, M.E.; Roussos, N.; Vardakas, K.Z. Relative frequency of albicans and the various non–albicans Candida spp among candidemia isolates from inpatients in various parts of the world: A systematic review. Int. J. Infect. Dis. 2010, 14, e954–e966. [Google Scholar] [CrossRef]
- Bloos, F.; Bayer, O.; Sachse, S.; Straube, E.; Reinhart, K.; Kortgen, A. Attributable costs of patients with candidemia and implications of polymerase chain reaction-based pathogen detection on antifungal therapy in patients with sepsis. J. Crit. Care 2013, 28, 2–8. [Google Scholar] [CrossRef]
- Hajjeh, R.A.; Sofair, A.N.; Harrison, L.H.; Lyon, G.M.; Arthington-Skaggs, B.A.; Mirza, S.A.; Phelan, M.; Morgan, J.; Lee-Yang, W.; Ciblak, M.A.; et al. Incidence of bloodstream infections due to Candida species and in vitro susceptibilities of isolates collected from 1998 to 2000 in a population-based active surveillance program. J. Clin. Microbiol. 2004, 42, 1519–1527. [Google Scholar] [CrossRef]
- Horn, D.L.; Neofytos, D.; Anaissie, E.J.; Fishman, J.A.; Steinbach, W.J.; Olyaei, A.J.; Marr, K.A.; Pfaller, M.A.; Chang, C.-H.; Webster, K.M. Epidemiology and outcomes of candidemia in 2019 patients: Data from the prospective antifungal therapy alliance registry. Clin. Infect. Dis. 2009, 48, 1695–1703. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Diekema, D.J.; Rinaldi, M.G.; Barnes, R.; Hu, B.; Veselov, A.V.; Tiraboschi, N.; Nagy, E.; Gibbs, D.L. Results from the ARTEMIS DISK Global Antifungal Surveillance Study: A 6.5-year analysis of susceptibilities of Candida and other yeast species to fluconazole and voriconazole by standardized disk diffusion testing. J. Clin. Microbiol. 2005, 43, 5848–5859. [Google Scholar] [CrossRef]
- Shorr, A.F.; Lazarus, D.R.; Sherner, J.H.; Jackson, W.L.; Morrel, M.; Fraser, V.J.; Kollef, M.H. Do clinical features allow for accurate prediction of fungal pathogenesis in bloodstream infections? Potential implications of the increasing prevalence of non-albicans candidemia. Crit. Care Med. 2007, 35, 1077–1083. [Google Scholar] [CrossRef]
- Bassetti, M.; Righi, E.; Costa, A.; Fasce, R.; Molinari, M.P.; Rosso, R.; Pallavicini, F.B.; Viscoli, C. Epidemiological trends in nosocomial candidemia in intensive care. BMC Infect. Dis. 2006, 6, 21. [Google Scholar] [CrossRef]
- Leroy, O.; Gangneux, J.P.; Montravers, P.; Mira, J.P.; Gouin, F.; Sollet, J.P.; Carlet, J.; Lortholary, O. Epidemiology, management, and risk factors for death of invasive Candida infections in critical care: A multicenter, prospective, observational study in France (2005–2006). Crit. Care Med. 2009, 37, 1612–1618. [Google Scholar] [CrossRef]
- Chow, J.K.; Golan, Y.; Ruthazer, R.; Karchmer, A.W.; Carmeli, Y.; Lichtenberg, D.A.; Chawla, V.; Young, J.A.; Hadley, S. Risk factors for albicans and non-albicans candidemia in the intensive care unit. Crit. Care Med. 2008, 36, 1993–1998. [Google Scholar] [CrossRef]
- Dimopoulos, G.; Ntziora, F.; Rachiotis, G.; Armaganidis, A.; Falagas, M.E. Candida albicans versus non-albicans intensive care unit-acquired bloodstream infections: Differences in risk factors and outcome. Anesth. Analg. 2008, 106, 523–529. [Google Scholar] [CrossRef]
- Marr, K.A.; Seidel, K.; White, T.C.; Bowden, R.A. Candidemia in allogeneic blood and marrow transplant recipients: Evolution of risk factors after the adoption of prophylactic fluconazole. J. Infect. Dis. 2000, 181, 309–316. [Google Scholar] [CrossRef]
- Playford, E.G.; Marriott, D.; Nguyen, Q.; Chen, S.; Ellis, D.; Slavin, M.; Sorrell, T.C. Candidemia in nonneutropenic critically ill patients: Risk factors for non-albicans Candida spp. Crit. Care Med. 2008, 36, 2034–2039. [Google Scholar] [CrossRef]
- Abi-Said, D.; Anaissie, E.; Uzun, O.; Raad, I.; Pinzcowski, H.; Vartivarian, S. The epidemiology of hematogenous candidiasis caused by different Candida species. Clin. Infect. Dis. 1997, 24, 1122–1128. [Google Scholar]
- Nguyen, M.H.; Wissel, M.C.; Shields, R.K.; Salomoni, M.A.; Hao, B.; Press, E.G.; Shields, R.M.; Cheng, S.; Mitsani, D.; Vadnerkar, A.; et al. Performance of Candida real-time polymerase chain reaction, beta-D-glucan assay, and blood cultures in the diagnosis of invasive candidiasis. Clin. Infect. Dis. 2012, 54, 1240–1248. [Google Scholar] [CrossRef]
- Guery, B.P.; Arendrup, M.C.; Auzinger, G.; Azoulay, E.; Borges, S.M.; Johnson, E.M.; Müller, E.; Putensen, C.; Rotstein, C.; Sganga, G.; et al. Management of invasive candidiasis and candidemia in adult non-neutropenic intensive care unit patients: Part I. Epidemiology and diagnosis. Intensiv. Care Med. 2009, 35, 55–62. [Google Scholar] [CrossRef]
- Ahmad, S.; Khan, Z. Invasive candidiasis: A review of nonculture-based laboratory diagnostic methods. Indian J. Med. Microbiol. 2012, 30, 264–269. [Google Scholar]
- Sendid, B.; Poirot, J.L.; Tabouret, M.; Bonnin, A.; Caillot, D.; Camus, D.; Poulain, D. Combined detection of mannanaemia and antimannan antibodies as a strategy for the diagnosis of systemic infection caused by pathogenic Candida species. J. Med. Microbiol. 2002, 51, 433–442. [Google Scholar]
- Koo, S.; Bryar, J.M.; Page, J.H.; Baden, L.R.; Marty, F.M. Diagnostic performance of the (1-->3)-beta-d-glucan assay for invasive fungal disease. Clin. Infect. Dis. 2009, 49, 1650–1659. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L.; Alexander, B.D.; Kett, D.H.; Vazquez, J.; Pappas, P.G.; Saeki, F.; Ketchum, P.A.; Wingard, J.; Schiff, R.; Tamura, H.; et al. Multicenter clinical evaluation of the (1-->3) beta-d-glucan assay as an aid to diagnosis of fungal infections in humans. Clin. Infect. Dis. 2005, 41, 654–659. [Google Scholar] [CrossRef]
- Sendid, B.; Tabouret, M.; Poirot, J.L.; Mathieu, D.; Fruit, J.; Poulain, D. New enzyme immunoassays for sensitive detection of circulating Candida albicans mannan and a.ntimannan antibodies: Useful combined test for diagnosis of systemic candidiasis. J. Clin. Microbiol. 1999, 37, 1510–1517. [Google Scholar]
- Prella, M.; Bille, J.; Pugnale, M.; Duvoisin, B.; Cavassini, M.; Calandra, T.; Marchetti, O. Early diagnosis of invasive candidiasis with mannan antigenemia and antimannan antibodies. Diagn. Microbiol. Infect. Dis. 2005, 51, 95–101. [Google Scholar] [CrossRef]
- Mokaddas, E.; Khan, Z.U.; Ahmad, S.; Nampoory, M.R.; Burhamah, M. Value of (1-3)-beta-d-glucan, Candida mannan and Candida DNA detection in the diagnosis of candidaemia. Clin. Infect. Dis. 2011, 17, 1549–1553. [Google Scholar]
- Peman, J.; Zaragoza, R. Current diagnostic approaches to invasive candidiasis in critical care settings. Mycoses 2010, 53, 424–433. [Google Scholar] [CrossRef]
- Posteraro, B.; De Pascale, G.; Tumbarello, M.; Torelli, R.; Pennisi, MA.; Bello, G.; Maviglia, R.; Fadda, G.; Sanguinetti, M.; Antonelli, M. Early diagnosis of candidemia in intensive care unit patients with sepsis: A prospective comparison of (1-->3)-beta-D-glucan assay, Candida score, and colonisation index. Crit. Care 2011, 15, R249. [Google Scholar] [CrossRef]
- Quindos, G.; Moragues, M.D.; Ponton, J. Is there a role for antibody testing in the diagnosis of invasive candidiasis? Rev. Iberoam. Micol. 2004, 21, 10–14. [Google Scholar]
- McMullan, R.; Metwally, L.; Coyle, P.V.; Hedderwick, S.; McCloskey, B.; O’Neill, H.J.; Patterson, C.C.; Thompson, G.; Webb, C.H.; Hay, R.J. A prospective clinical trial of a real-time polymerase chain reaction assay for the diagnosis of candidemia in nonneutropenic, critically ill adults. Clin. Infect. Dis. 2008, 46, 890–896. [Google Scholar] [CrossRef]
- Ahmad, S.; Khan, Z.; Mustafa, A.S.; Khan, Z.U. Seminested PCR for diagnosis of candidemia: Comparison with culture, antigen detection, and biochemical methods for species identification. J. Clin. Microbiol. 2002, 40, 2483–2489. [Google Scholar] [CrossRef]
- Marklein, G.; Josten, M.; Klanke, U.; Müller, E.; Horré, R.; Maier, T.; Kostrzewa, M.; Bierbaum, G.; Hoerauf, A.; Sahl, H.-G. Matrix-assisted laser desorption inozation-time of flight mass spectrometry for fast and reliable identification of clinical yeast isolates. J. Clin. Microbiol. 2009, 47, 2912–2917. [Google Scholar] [CrossRef]
- Shepard, J.R.; Addison, R.M.; Alexander, B.D.; Della-Latta, P.; Gherna, M.; Haase, G.; Hall, G.; Johnson, J.K.; Merz, W.G.; Peltroche-Llacsahuanga, H.; et al. Multicenter evaluation of the Candida albicans/Candida glabrata peptide nucleic acid fluorescent in situ hybridization method for simultaneous dual-color identification of C.albicans and C.glabrata directly from blood cultures bottles. J. Clin. Microbiol. 2009, 46, 50–55. [Google Scholar]
- Calderaro, A.; Martinelli, M.; Motta, F.; Larini, S.; Arcangeletti, M.C.; Medici, M.C.; Chezzi, C.; Conto, F. Comparison of peptide nucleic acid fluorescence in situ hybridization (PNA FISH) assays with culture based matrix-assisted laser desorption/ionization-time of flight (MALDI-TOF) Mass Spectrometry for the identification of bacteria and yeasts from blood cultures and cerebrospinal fluid cultures. Clin. Microbiol. Infect. 2013. [Google Scholar] [CrossRef]
- Luzzati, R.; Cavinato, S.; Giangreco, M.; Granà, G.; Centonze, S.; Deiana, M.L.; Biolo, G.; Barbone, F. Peripheral and total parenteral nutrition as the strongest risk factors for nosocomial candidemia in elderly patients: A matched case-control study. Mycoses 2013, 56, 664–671. [Google Scholar] [CrossRef]
- Muskett, H.; Shahin, J.; Eyres, G.; Harvey, S.; Rowan, K.; Harrison, D. Risk factors for invasive fungal disease in critically ill adult patients: A systematic review. Crit. Care 2011, 15, R287. [Google Scholar] [CrossRef]
- Hoffmann-Santos, H.D.; Paula, C.R.; Yamamoto, A.C.; Tadano, T.; Hahn, R.C. Six-year trend analysis of nosocomial candidemia and risk factors in two intensive care hospitals in Mato Grosso, Midwest Region of Brazil. Mycopathologia 2013, 176, 409–415. [Google Scholar] [CrossRef]
- Leon, C.; Ruiz-Santana, S.; Saavedra, P.; Castro, C.; Ubeda, A.; Loza, A.; Hernández-Viera, M.A. Usefulness of the “Candida score” for discriminating between Candida colonisation and invasive candidiasis in non-neutropenic critically ill patients: A prospective multicenter study. Crit. Care Med. 2009, 37, 1624–1633. [Google Scholar] [CrossRef]
- Blumberg, H.M.; Jarvis, W.R.; Soucie, J.M.; Edwards, J.E.; Patterson, J.E.; Pfaller, M.A.; Rangel-Frausto, M.S.; Rinaldi, M.G.; Saiman, L.; Wiblin, R.T.; et al. Risk factors for candidal bloodstream infections in surgical intensive care unit patients: The NEMIS prospective multicenter study. The National Epidemiology of Mycosis Survey. Clin. Infect. Dis. 2001, 33, 177–186. [Google Scholar] [CrossRef]
- Agvald-Ohman, C.; Klingspor, L.; Hjelmqvist, H.; Edlund, C. Invasive candidiasis in long-term patients at a multidisciplinary intensive care unit: Candida colonisation index, risk factors, treatment and outcome. Scand. J. Infect. Dis. 2008, 40, 145–153. [Google Scholar] [CrossRef]
- Pittet, D.; Monod, M.; Suter, P.M.; Frenk, E.; Auckenthaler, R. Candida colonisation and subsequent infections in critically ill surgical patients. Ann. Surgery 1994, 220, 751–758. [Google Scholar] [CrossRef]
- Dupont, H.; Bourichon, A.; Paugam-Burtz, C.; Mantz, J.; Desmonts, J.M. Can yeast isolation in peritoneal fluid be predicted in intensive care unit patients with peritonitis? Crit. Care Med. 2003, 31, 752–757. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L.; Sable, C.; Sobel, J.; Alexander, B.D.; Donowitz, G.; Kan, V.; Kauffman, C.A.; Kett, D.; Larsen, R.A.; Morrison, V.; et al. Multicenter retrospective development and validation of a clinical prediction rule for nosocomial invasive candidiasis in the intensive care setting. Eur. J. Clin. Microbiol. Infect. Dis. 2007, 26, 271–276. [Google Scholar] [CrossRef]
- Hermsen, E.D.; Zapapas, M.K.; Maiefski, M.; Rupp, M.E.; Freifeld, A.G.; Kalil, A.C. Validation and comparison of clinical prediction rules for invasive candidiasis in intensive care unit patients: A matched case-control study. Crit. Care 2011, 15, R198. [Google Scholar] [CrossRef]
- Paphitou, N.I.; Ostrosky-Zeichner, L.; Rex, J.H. Rules for identifying patients at increased risk for candidal infections in the surgical intensive care unit: Approach to developing practical criteria for systematic use in antifungal prophylaxis trials. Med. Mycol. 2005, 43, 235–243. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L. Clinical prediction rules for invasive candidiasis in the ICU: Ready for prime time? Crit. Care 2011, 15, 1–2. [Google Scholar] [CrossRef]
- Meersseman, W.; Lagrou, K.; Maertens, J.; van Wijngaerden, E. Invasive aspergillosis in the intensive care unit. Clin. Infect. Dis. 2007, 45, 205–216. [Google Scholar] [CrossRef]
- Dimopoulos, G.; Piagnerelli, M.; Berre, J.; Eddafali, B.; Salmon, I.; Vincent, J.L. Disseminated aspergillosis in intensive care unit patients: An autopsy study. J. Chemother. 2003, 15, 71–75. [Google Scholar] [CrossRef]
- Meersseman, W.; Vandecasteele, S.J.; Wilmer, A.; Verbeken, E.; Peetermans, W.E.; van Wijngaerden, E. Invasive aspergillosis in critically ill patients without malignancy. Am. J. Resp. Crit. Care Med. 2004, 170, 621–625. [Google Scholar] [CrossRef]
- Warris, A.; Verweij, P.E. Clinical implications of environmental sources for Aspergillus. Med. Mycol. 2005, 43, S59–S65. [Google Scholar] [CrossRef]
- Mehrad, B.; Paciocco, G.; Martinez, F.J.; Ojo, T.C.; Iannettoni, M.D.; Lynch, J.P. Spectrum of Aspergillus infection in lung transplant recipients: Case series and review of the literature. Chest 2001, 119, 169–175. [Google Scholar] [CrossRef]
- Pasqualotto, A.C.; Denning, D.W. Post-operative aspergillosis. Clin. Microbiol. Infect. 2006, 12, 1060–1076. [Google Scholar] [CrossRef]
- Dimopoulos, G.; Tsangaris, I.; Poulakou, G.; Panayiotides, J.; Tsaknis, G.; Orfanos, S.; Armaganides, A. Post-operative Aspergillus mediastinitis in a man who was immunocompetent: A case report. J. Med. Case Rep. 2010, 4, 312. [Google Scholar] [CrossRef]
- Barnes, P.D.; Marr, K.A. Risks, diagnosis and outcomes of invasive fungal infections in haematopoietic stem cell transplant recipients. Br. J. Haematol. 2007, 139, 519–531. [Google Scholar] [CrossRef]
- Cornillet, A.; Camus, C.; Nimubona, S.; Gandemer, V.; Tattevin, P.; Belleguic, C.; Chevrier, S.; Meunier, C.; Lebert, C.; Aupée, M.; et al. Comparison of epidemiological, clinical, and biological features of invasive aspergillosis in neutropenic and nonneutropenic patients: A 6-year survey. Clin. Infect. Dis. 2006, 43, 577–584. [Google Scholar] [CrossRef]
- Vandewoude, K.H.; Blot, S.I.; Depuydt, P.; Benoit, D.; Temmerman, W.; Colardyn, F.; Vogelaers, D. Clinical relevance of Aspergillus isolation from respiratory tract samples in critically ill patients. Crit. Care 2006, 10, R31. [Google Scholar] [CrossRef]
- Ruhnke, M.; Bohme, A.; Buchheidt, D.; Cornely, O.; Einsele, H.; Enzensberger, R.; Hebart, H.; Heinz, W.; Junghanss, C.; Karthaus, M.; et al. Diagnosis of invasive fungal infections in hematology and oncology--guidelines of the Infectious Diseases Working Party (AGIHO) of the German Society of Hematology and Oncology (DGHO). Ann. Haematol. 2003, 82, S141–S148. [Google Scholar] [CrossRef]
- Perfect, J.R.; Cox, G.M.; Lee, J.Y.; Kauffman, C.A.; de Repentigny, L.; Chapman, S.W.; Morrison, V.A.; Pappas, P.; Hiemenz, J.W.; Stevens, D.A. The impact of culture isolation of Aspergillus. species: A hospital-based survey of aspergillosis. Clin. Infect. Dis. 2001, 33, 1824–1833. [Google Scholar] [CrossRef]
- Horvath, J.A.; Dummer, S. The use of respiratory-tract cultures in the diagnosis of invasive pulmonary aspergillosis. Am. J. Med. 1996, 100, 171–178. [Google Scholar] [CrossRef]
- Soubani, A.O.; Chandrasekar, P.H. The clinical spectrum of pulmonary aspergillosis. Chest 2002, 121, 1988–1999. [Google Scholar] [CrossRef]
- Fukuda, T.; Boeckh, M.; Carter, R.A.; Sandmaier, B.M.; Maris, M.B.; Maloney, D.G.; Martin, P.J.; Storb, R.F.; Marr, K.A. Risks and outcomes of invasive fungal infections in recipients of allogeneic hematopoietic stem cell transplants after nonmyeloablative conditioning. Blood 2003, 102, 827–833. [Google Scholar] [CrossRef]
- Locatelli, F.; Barbui, A.; Limerutti, G.; Serra, R.; Libertucci, D.; Falda, M. Usefulness of sequential Aspergillus galactomannan antigen detection combined with early radiologic evaluation for diagnosis of invasive pulmonary aspergillosis in patients undergoing allogeneic stem cell transplantation. Transplant. Proc. 2006, 38, 1610–1613. [Google Scholar]
- Herbrecht, R.; Letscher-Bru, V.; Oprea, C.; Lioure, B.; Waller, J.; Campos, F.; Villard, O.; Liu, K.-L.; Natarajan-Amé, S.; Lutz, P.; et al. Aspergillus galactomannan detection in the diagnosis of invasive aspergillosis in cancer patients. J. Clin. Oncol. 2002, 20, 1898–1906. [Google Scholar] [CrossRef]
- Klont, R.R.; Mennink-Kersten, M.A.; Verweij, P.E. Utility of Aspergillus antigen detection in specimens other than serum specimens. Clin. Infect. Dis. 2004, 39, 1467–1474. [Google Scholar] [CrossRef]
- Digby, J.; Kalbfleisch, J.; Glenn, A.; Larsen, A.; Browder, W.; Williams, D. Serum glucan levels are not specific for presence of fungal infections in intensive care unit patients. Clin. Diagn. Lab. Immunol. 2003, 10, 882–885. [Google Scholar]
- Wengenack, N.L.; Binnicker, M.J. Fungal molecular diagnostics. Clin. Chest Med. 2009, 30, 391–408. [Google Scholar] [CrossRef]
- Hizel, K.; Kokturk, N.; Kalkanci, A.; Ozturk, C.; Kustimur, S.; Tufan, M. Polymerase chain reaction in the diagnosis of invasive aspergillosis. Mycoses 2004, 47, 338–342. [Google Scholar] [CrossRef]
- Halliday, C.; Hoile, R.; Sorrell, T.; James, G.; Yadav, S.; Shaw, P.; Bleakley, M.; Bradstock, K.; Chen, S. Role of prospective screening of blood for invasive aspergillosis by polymerase chain reaction in febrile neutropenic recipients of haematopoietic stem cell transplants and patients with acute leukaemia. Br. J. Haematol. 2006, 132, 478–486. [Google Scholar]
- Hsu, J.L.; Ruoss, S.J.; Bower, N.D.; Lin, M.; Holodniy, M.; Stevens, D.A. Diagnosing invasive fungal disease in critically ill patients. Crit. Rev. Microbiol. 2011, 37, 277–312. [Google Scholar] [CrossRef]
- Li, Y.; Gao, L.; Ding, Y.; Xu, Y.; Zhou, M.; Huang, W.; Jing, Y.; Li, H.; Wang, L.; Yu, L. Establishment and application of real-time quantitative PCR for diagnosing invasive aspergillosis via the blood in hematological patients: Targeting a specific sequence of Aspergillus 28S-ITS2. BMC Infect. Dis. 2013, 13, 255. [Google Scholar] [CrossRef]
- Springer, J.; Morton, C.O.; Perry, M.; Heinz, W.J.; Paholcsek, M.; Alzheimer, M.; Rogersb, T.R.; Barnesd, R.A.; Einselea, H.; Loeffler, J.; et al. Multicenter comparison of serum and whole-blood specimens for detection of Aspergillus DNA in high-risk hematological patients. J. Clin. Microbiol. 2013, 51, 1445–1450. [Google Scholar] [CrossRef]
- De Pauw, B.; Walsh, T.J.; Donnelly, J.P.; Stevens, D.A.; Edwards, J.E.; Calandra, T.; Pappas, P.G.; Maertens, J.; Lortholary, O.; Kauffman, C.A.; et al. Revised definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer/Invasive Fungal Infections Cooperative Group and the National Institute of Allergy and Infectious Diseases Mycoses Study Group (EORTC/MSG) Consensus Group. Clin. Infect. Dis. 2008, 46, 1813–1821. [Google Scholar] [CrossRef]
- Blot, S.I.; Taccone, F.S.; van den Abeele, A.M.; Bulpa, P.; Meersseman, W.; Brusselaers, N.; Dimopoulos, G.; Paiva, J.A.; Misset, B.; Rello, J.; et al. A clinical algorithm to diagnose invasive pulmonary aspergillosis in critically ill patients. Am. J. Resp. Crit. Care Med. 2012, 186, 56–64. [Google Scholar] [CrossRef]
- Zaragoza, R.; Peman, J.; Salavert, M.; Viudes, A.; Solé, A.; Jarque, I.; Monte, E.; Romá, E.; Cantón, E. Multidisciplinary approach to the treatment of invasive fungal infections in adult patients. Prophylaxis, empirical, preemptive or targeted therapy, which is the best in the different hosts? Ther. Clin. Risk Manag. 2008, 4, 1261–1280. [Google Scholar]
- Ribes, J.A.; Vanover-Sams, C.L.; Baker, D.J. Zygomycetes in human disease. Clin. Microbiol. Rev. 2000, 13, 236–301. [Google Scholar] [CrossRef]
- Petrikkos, G.; Skiada, A.; Lortholary, O.; Roilides, E.; Walsh, T.J.; Kontoyiannis, D.P. Epidemiology and clinical manifestations of mucormycosis. Clin. Infect. Dis. 2012, 54, S23–S34. [Google Scholar]
- Andresen, D.; Donaldson, A.; Choo, L.; Knox, A.; Klaassen, M.; Ursic, C.; Vonthethoff, L.; Krilis, S.; Konecny, P. Multifocal cutaneous mucormycosis complicating polymicrobial wound infections in a tsunami survivor from Sri Lanka. Lancet 2005, 365, 876–878. [Google Scholar] [CrossRef]
- Neblett Fanfair, R.; Benedict, K.; Bos, J.; Bennett, S.D.; Lo, Y.C.; Adebanjo, T.; Etienne, K.; Deak, E.; Derado, G.; Shieh, W.-J.; et al. Necrotizing cutaneous mucormycosis after a tornado in Joplin, Missouri, in 2011. N. Engl. J. Med. 2012, 367, 2214–2225. [Google Scholar] [CrossRef]
- Warkentien, T.; Rodriguez, C.; Lloyd, B.; Wells, J.; Weintrob, A.; Dunne, J.R.; Ganesan, A.; Li, P.; Bradley, W.; Gaskins, L.J.; et al. Invasive mold infections following combat-related injuries. Clin. Infect. Dis. 2012, 55, 1441–1449. [Google Scholar] [CrossRef]
- Maravi-Poma, E.; Rodriguez-Tudela, J.L.; de Jalon, J.G.; Manrique-Larralde, A.; Torroba, L.; Urtasun, J.; Salvador, B.; Montes, M.; Mellado, E.; Rodríguez-Albarrán, F.; et al. Outbreak of gastric mucormycosis associated with the use of wooden tongue depressors in critically ill patients. Intensiv. Care Med. 2004, 30, 724–728. [Google Scholar] [CrossRef]
- Lass-Florl, C. Zygomycosis: Conventional laboratory diagnosis. Clin. Microbiol. Infect. 2009, 15, 60–65. [Google Scholar] [CrossRef]
- Walsh, T.J.; Gamaletsou, M.N.; McGinnis, M.R.; Hayden, R.T.; Kontoyiannis, D.P. Early clinical and laboratory diagnosis of invasive pulmonary, extrapulmonary, and disseminated mucormycosis (zygomycosis). Clin. Infect. Dis. 2012, 54, S55–S60. [Google Scholar] [CrossRef]
- Millon, L.; Larosa, F.; Lepiller, Q.; Legrand, F.; Rocchi, S.; Daguindau, E.; Scherer, E.; Bellanger, A.P.; Leroy, J.; Grenouillet, F. Quantitative polymerase chain reaction detection of circulating DNA in serum for early diagnosis of mucormycosis in immunocompromised patients. Clin. Infect. Dis. 2013, 56, e95–e101. [Google Scholar] [CrossRef]
- Tawara, S.; Ikeda, F.; Maki, K.; Watabe, E.; Tawara, S.; Teratani1, N.; Goto1, T.; Tomishima, M.; Ohki, H.; Yamada, A.; et al. In vitro activities of a new lipopeptide antifungal agent, FK463, against a variety of clinically important fungi. Antimicrob. Agents Chemother. 2009, 44, 57–62. [Google Scholar]
- Neumann, A.; Baginski, M.; Winczewski, S.; Czub, J. The effect of sterols on amphotericin B self-aggregation in a lipid bilayer as revealed by free energy simulations. Biophys. J. 2013, 104, 1485–1494. [Google Scholar] [CrossRef]
- Ghannoum, M.A.; Rice, L.B. Antifungal agents: Mode of action, mechanisms of resistance, and correlation of these mechanisms with bacterial resistance. Clin. Microbiol. Rev. 1999, 12, 501–517. [Google Scholar]
- Pfaller, M.A.; Messer, S.A.; Boyken, L.; Tendolkar, S.; Hollis, R.J.; Diekema, D.J. Geographic variation in the susceptibilities of invasive isolates of Candida glabrata to seven systemically active antifungal agents: A global assessment from the ARTEMIS Antifungal Surveillance Program conducted in 2001 and 2002. J. Clin. Microbiol. 2004, 42, 3142–3146. [Google Scholar] [CrossRef]
- Messer, S.A.; Jones, R.N.; Fritsche, T.R. International surveillance of Candida spp. and Aspergillus spp.: Report from the SENTRY Antimicrobial Surveillance Program (2003). J. Clin. Microbiol 2006, 44, 1782–1787. [Google Scholar] [CrossRef]
- Sabatelli, F.; Patel, R.; Mann, P.A.; Mendrick, C.A.; Norris, C.C.; Hare, R.; Loebenberg, D.; Black, T.A.; McNicholas, P.M. In vitro activities of posaconazole, fluconazole, itraconazole, voriconazole, and amphotericin B against a large collection of clinically important molds and yeasts. Antimicrob. Agents Chemother. 2006, 50, 2009–2015. [Google Scholar] [CrossRef]
- Deray, G. Amphotericin B nephrotoxicity. J. Antimicrob. Chemother. 2002, 49, 37–41. [Google Scholar] [CrossRef]
- Blot, S.; Vandewoude, K. Management of invasive candidiasis in critically ill patients. Drugs 2004, 64, 2159–2175. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L.; Marr, K.A.; Rex, J.H.; Cohen, S.H. Amphotericin B: Time for a new “gold standard”. Clin. Infect. Dis. 2003, 37, 415–425. [Google Scholar] [CrossRef]
- Mistro, S.; Maciel Ide, M.; de Menezes, R.G.; Maia, Z.P.; Schooley, R.T.; Badaro, R. Does lipid emulsion reduce amphotericin B nephrotoxicity? A systematic review and meta-analysis. Clin. Infect. Dis. 2012, 54, 1774–1777. [Google Scholar] [CrossRef]
- Shigemi, A.; Matsumoto, K.; Ikawa, K.; Yaji, K.; Shimodozono, Y.; Morikawa, N.; Takeda, Y.; Yamada, K. Safety analysis of liposomal amphotericin B in adult patients: Anaemia, thrombocytopenia, nephrotoxicity, hepatotoxicity and hypokalaem. Int. J. Antimicrob. Agents 2011, 38, 417–420. [Google Scholar] [CrossRef]
- Adler-Moore, J.P.; Proffitt, R.T. Amphotericin B lipid preparations: What are the differences? Clin. Microb. Infect. 2008, 14, 25–36. [Google Scholar] [CrossRef]
- Pappas, P.G.; Kauffman, C.A.; Andes, D.; Benjamin, D.K., Jr.; Calandra, T.F.; Edwards, J.E., Jr. Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2009, 48, 503–535. [Google Scholar] [CrossRef]
- Mills, E.J.; Perri, D.; Cooper, C.; Nachega, J.B.; Wu, P.; Tleyjeh, I.; Phillips, P. Antifungal treatment for invasive Candida infections: A mixed treatment comparison meta-analysis. Ann. Clin. Microbiol. Antimicrob. 2009, 8, 23–31. [Google Scholar] [CrossRef]
- Povoa, P.; Goncalves-Pereira, J. Treatment of candidemia in adult patients without neutropenia--an inconvenient truth. Crit. Care 2011, 15, 114. [Google Scholar]
- Dreyfuss, D.; Ricard, J.D.; Gaudry, S. Amphotericin B deoxycholate for candidiasis in intensive care unit patients revisited: Medical, ethical, and financial implications. Am. J. Resp. Crit. Care Med. 2013, 187, 661–663. [Google Scholar] [CrossRef]
- Shoham, S.; Marwaha, S. Invasive fungal infections in the ICU. J. Intensiv. Care Med. 2010, 25, 78–92. [Google Scholar] [CrossRef]
- Baddley, J.W.; Patel, M.; Bhavnani, S.M.; Moser, S.A.; Andes, D.R. Association of fluconazole pharmacodynamics with mortality in patients with candidemia. Antimicrob. Agents Chemother. 2008, 52, 3022–3028. [Google Scholar] [CrossRef]
- Klepser, M.E.; Wolfe, E.J.; Jones, R.N.; Nightingale, C.H.; Pfaller, M.A. Antifungal pharmacodynamic characteristics of fluconazole and amphotericin B tested against Candida albicanst. Antimicrob. Agents Chemother. 1997, 41, 1392–1395. [Google Scholar]
- Playford, E.G.; Eggimann, P.; Calandra, T. Antifungals in the ICU. Curr. Opin. Infect. Dis. 2008, 21, 610–619. [Google Scholar] [CrossRef]
- Saari, T.I.; Laine, K.; Neuvonen, M.; Neuvonen, P.J.; Olkkola, K.T. Effect of voriconazole and fluconazole on the pharmacokinetics of intravenous fentanyl. Eur. J. Clin. Pharmacol. 2008, 64, 25–30. [Google Scholar] [CrossRef]
- Skrobik, Y.; Leger, C.; Cossette, M.; Michaud, V.; Turgeon, J. Factors predisposing to coma and delirium: Fentanyl and midazolam exposure, CYP3A5, ABCB1 and ABCG2 genetic polymorphisms and inflammatory factors. Crit. Care Med. 2013, 41, 999–1008. [Google Scholar] [CrossRef]
- Kullberg, B.J.; Sobel, J.D.; Ruhnke, M.; Pappas, P.G.; Viscoli, C.; Rex, J.H.; Cleary, J.D.; Rubinstein, E.; Church, L.W.P.; Brown, J.M.; et al. Voriconazole versus a regimen of amphotericin B followed by fluconazole for candidaemia in non-neutropenic patients: A randomised non-inferiority trial. Lancet 2005, 366, 1435–1442. [Google Scholar] [CrossRef]
- Johnson, L.B.; Kauffman, C.A. Voriconazole: A new triazole antifungal agent. Clin. Infect. Dis. 2003, 36, 630–637. [Google Scholar] [CrossRef]
- Manavathu, E.K.; Cutright, J.L.; Chandrasekar, P.H. Organism-dependent fungicidal activities of azoles. Antimicrob. Agents Chemother. 1998, 42, 3018–3021. [Google Scholar]
- Barry, A.L.; Brown, S.D. In vitro studies of two triazole antifungal agents (voriconazole [UK-109,496] and fluconazole) against Candida species. Antimicrob. Agents Chemother. 1996, 40, 1948–1949. [Google Scholar]
- Kauffman, C.A.; Zarins, L.T. In vitro activity of voriconazole against Candida species. Diagn. Microbiol. Infect. Dis. 1998, 31, 297–300. [Google Scholar] [CrossRef]
- Ally, R.; Schurmann, D.; Kreisel, W.; Carosi, G.; Aguirrebengoa, K.; Dupont, B.; Hodges, M.; Troke, P.; RomeroA, A.J. randomized, double-blind, double-dummy, multicenter trial of voriconazole and fluconazole in the treatment of esophageal candidiasis in immunocompromised patients. Clin. Infect. Dis. 2001, 33, 1447–1454. [Google Scholar] [CrossRef]
- Herbrecht, R.; Denning, D.W.; Patterson, T.F.; Bennett, J.E.; Greene, R.E.; Oestmann, J.W.; Kern, W.V.; Marr, K.A.; Ribaud, P.; Lortholary, O.; et al. Voriconazoleversus amphotericin B for primary therapy of invasive aspergillosis. N. Engl. J. Med. 2002, 347, 408–415. [Google Scholar] [CrossRef]
- Neofytos, D.; Lombardi, L.R.; Shields, R.K.; Ostrander, D.; Warren, L.; Nguyen, M.H.; Thompson, C.B.; Marr, K.A. Administration of voriconazole in patients with renal dysfunction. Clin. Infect. Dis. 2012, 54, 913–921. [Google Scholar] [CrossRef]
- Oude Lashof, A.M.; Sobel, J.D.; Ruhnke, M.; Pappas, P.G.; Viscoli, C.; Schlamm, H.T.; Kullberg, B.J. Safety and tolerability of voriconazole in patients with baseline renal insufficiency and candidemia. Antimicrob. Agents Chemother. 2012, 56, 3133–3137. [Google Scholar] [CrossRef]
- Pascual, A.; Csajka, C.; Buclin, T.; Bolay, S.; Bille, J.; Calandra, T.; Marchetti, O. Challenging recommended oral and intravenous voriconazole doses for improved efficacy and safety: Population pharmacokinetics-based analysis of adult patients with invasive fungal infections. Clin. Infect. Dis. 2012, 55, 381–390. [Google Scholar] [CrossRef]
- Pascual, A.; Calandra, T.; Bolay, S.; Buclin, T.; Bille, J.; Marchetti, O. Voriconazole therapeutic drug monitoring in patients with invasive mycoses improves efficacy and safety outcomes. Clin. Infect. Dis. 2008, 46, 201–211. [Google Scholar] [CrossRef]
- Alvarez-Lerma, F.; Nicolas-Arfelis, J.M.; Rodriguez-Borregan, J.C.; Díaz-Regañón, J.; Sa-Borges, M.; García-López, F.; Allepuz-Palau, A. Clinical use and tolerability of voriconazole in the treatment of fungal infections in critically ill patients. J. Chemother. 2005, 17, 417–427. [Google Scholar] [CrossRef]
- Ullmann, A.J.; Lipton, J.H.; Vesole, D.H.; Chandrasekar, P.; Langston, A.; Tarantolo, S.R.; Greinix, H.; de Azevedo, W.M.; Reddy, V.; Boparai, N.; et al. Posaconazole or fluconazole for prophylaxis in severe graft-versus-host disease. N. Engl. J. Med. 2007, 356, 335–347. [Google Scholar] [CrossRef]
- Greenberg, R.N.; Mullane, K.; van Burik, J.A.; Raad, I.; Abzug, M.J.; Anstead, G.; Herbrecht, R.; Langston, A.; Marr, K.A.; Schiller, G.; et al. Posaconazole as salvage therapy for zygomycosis. Antimicrob. Agents Chemother. 2006, 50, 126–133. [Google Scholar] [CrossRef]
- Georgopapadakou, N.H. Update on antifungals targeted to the cell wall: Focus on beta-1,3-glucan synthase inhibitors. Expert Opin. Investig. Drugs 2001, 10, 269–280. [Google Scholar] [CrossRef]
- Mean, M.; Marchetti, O.; Calandra, T. Bench-to-bedside review: Candida infections in the intensive care unit. Crit. Care 2008, 12, 204. [Google Scholar] [CrossRef]
- Stone, J.A.; Migoya, E.M.; Hickey, L.; Winchell, G.A.; Deutsch, P.J.; Ghosh, K.; Freeman, A.; Bi, S.; Desai, R.; Dilzer, S.C.; et al. Potential for interactions between caspofungin and nelfinavir or rifampin. Antimicrob. Agents Chemother. 2004, 48, 4306–4314. [Google Scholar] [CrossRef]
- Glockner, A. Treatment and prophylaxis of invasive candidiasis with anidulafungin, caspofungin and micafungin: Review of the literature. Eur. J. Med. Res. 2011, 16, 167–179. [Google Scholar] [CrossRef]
- Dimopoulos, G.; Antonopoulou, A.; Armaganidis, A.; Vincent, J.L. How to select an antifungal agent in critically ill patients. J. Crit. Care 2013, 28, 717–727. [Google Scholar] [CrossRef]
- Kett, D.; Shorr, A.F.; Reboli, A.C.; Reisman, A.L.; Biswas, P.; Schlamm, H.T. Anidulafungin compared with fluconazole in severely ill patients with candidaemia and other forms of invasive candidiasis: Support for the 2009 IDSA treatment guidelines for candidiasis. Crit. Care 2011, 15, R253. [Google Scholar] [CrossRef]
- Vermes, A.; Guchelaar, H.J.; Dankert, J. Flucytosine: A review of its pharmacology, clinical indications, pharmacokinetics, toxicity and drug interactions. J. Antimicrob. Chemother. 2000, 46, 171–179. [Google Scholar] [CrossRef]
- Matthews, R.C.; Rigg, G.; Hodgetts, S.; Carter, T.; Chapman, C.; Gregory, C.; Illidge, C.; Burnie, J. Preclinical assessment of the efficacy of mycograb, a human recombinant antibody against fungal HSP90. Antimicrob. Agents Chemother. 2003, 47, 2208–2216. [Google Scholar] [CrossRef]
- Morrell, M.; Fraser, V.J.; Kollef, M.H. Delaying the empiric treatment of candida bloodstream infection until positive blood culture results are obtained: A potential risk factor for hospital mortality. Antimicrob. Agents Chemother. 2005, 49, 3640–3645. [Google Scholar] [CrossRef]
- Garey, K.W.; Rege, M.; Pai, M.P.; Mingo, D.E.; Suda, K.J.; Turpin, R.S.; Bearden, D.T. Time to initiation of fluconazole therapy impacts mortality in patients with candidemia: A multi-institutional study. Clin. Infect. Dis. 2006, 43, 25–31. [Google Scholar] [CrossRef]
- Garrouste-Orgeas, M.; Timsit, J.F.; Tafflet, M.; Misset, B.; Zahar, J.R.; Soufir, L.; Lazard, T.; Jamali, S.; Mourvillier, B.; Cohen, Y.; et al. Excess risk of death from intensive care unit-acquired nosocomial bloodstream infections: A reappraisal. Clin. Infect. Dis. 2006, 42, 1118–1126. [Google Scholar] [CrossRef]
- Skrobik, Y.; Laverdiere, M. Why Candida sepsis should matter to ICU physicians. Crit. Care Clin. 2013, 29, 853–864. [Google Scholar] [CrossRef]
- Bow, E.; Evans, G.; Fuller, J.; Laverdière, M.; Rotstein, C.; Rennie, R.; Shafran, S.D.; Sheppard, D.; Carle, S.; Phillips, P.; et al. Canadian clinical practice guidelines for invasive candidiasis in adults. Can. J. Infect. Dis. Med. Microbiol. 2010, 21, e122–e150. [Google Scholar]
- Cornely, O.A.; Bassetti, M.; Calandra, T.; Garbino, J.; Kullberg, B.J.; Lortholary, O.; Meersseman, W.; Akova, M.; Arendrup, M.C.; Arikan-Akdagli, S.; et al. ESCMID guidelines for the diagnosis and management of Candida diseases 2012: Non- neutropenic adult patients. Clin. Microbiol. Infect. 2012, 18, 19–37. [Google Scholar] [CrossRef]
- Kullberg, B.J.; Verweij, P.E.; Akova, M.; Arendrup, M.C.; Bille, J.; Calandra, T.; Cuenca-Estrella, M.; Herbrecht, R.; Jacobs, F.; Kalin, M.; et al. European expert opinion on the management of invasive candidiasis in adults. Clin. Microbiol. Infect. 2011, 17, 1–12. [Google Scholar]
- Limper, A.H.; Knox, K.S.; Sarosi, G.A.; Ampel, N.M.; Bennett, J.E.; Catanzaro, A.; Davies, S.F.; Dismukes, W.E.; Hage, C.A.; Marr, K.A.; et al. An official American Thoracic Society statement: Treatment of fungal infections in adult pulmonary and critical care patients. Am. J. Resp. Crit. Care Med. 2011, 183, 96–128. [Google Scholar] [CrossRef]
- Ruhnke, M.; Rickerts, V.; Cornely, O.; Buchheidt, D.; Glöckner, A.; Heinz, W.; Höhl, R.; Horré, R.; Karthaus, M.; Kujath, P.; Willinger, B.; et al. Diagnosis and therapy of Candida infections: Joint recommendations of the German Speaking Mycological Society and the Paul–Ehrlich-Society for Chemotherapy. Mycoses 2011, 54, 279–310. [Google Scholar] [CrossRef]
- Labbe, A.C.; Pepin, J.; Patino, C.; Castonguay, S.; Restieri, C.; Laverdiere, M. A single-centre 10-year experience with Candida bloodstream infections. Can. J. Infect. Dis. Med. Microbiol. 2009, 20, 45–50. [Google Scholar]
- Pfaller, M.A.; Messer, S.A.; Moet, G.J.; Jones, R.N.; Castanheira, M. Candida bloodstream infections: Comparison of species distribution and resistance to echinocandin and azole antifungal agents in Intensive Care Unit (ICU) and non-ICU settings in the SENTRY Antimicrobial Surveillance Program (2008–2009). Int. J. Antimicrob. Agents 2011, 38, 65–69. [Google Scholar] [CrossRef]
- Nucci, M.; Anaissie, E.; Betts, R.F.; Dupont, B.F.; Wu, C.; Buell, D.N.; Kovanda, L.; Lortholary, O. Early removal of central venous catheter in patients with candidemia does not improve outcome: Analysis of 842 patients from 2 randomized clinical trials. Clin. Infect. Dis. 2010, 51, 295–303. [Google Scholar] [CrossRef]
- Walsh, T.J.; Rex, J.H. All catheter-related candidemia is not the same: Assessment of the balance between the risks and benefits of removal of vascular catheters. Clin. Infect. Dis. 2002, 34, 600–602. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L. Combination antifungal therapy: A critical review of the evidence. Clin. Microbiol. Infect. 2008, 14, 65–70. [Google Scholar] [CrossRef]
- Senn, L.; Eggimann, P.; Ksontini, R.; Pascual, A.; Demartines, N.; Bille, J.; Calandra, T.; Marchetti, O. Caspofungin for prevention of intra-abdominal candidiasis in high-risk surgical patients. Intensiv. Care Med. 2009, 35, 903–908. [Google Scholar] [CrossRef]
- Silvestri, L.; van Saene, H.K.; Milanese, M.; Gregori, D. Impact of selective decontamination of the digestive tract on fungal carriage and infection: Systematic review of randomized controlled trials. Intensiv. Care Med. 2005, 31, 898–910. [Google Scholar] [CrossRef]
- Garbino, J.; Lew, D.P.; Romand, J.A.; Hugonnet, S.; Auckenthaler, R.; Pittet, D. Prevention of severe Candida infections in nonneutropenic, high-risk, critically ill patients: A randomized, double-blind, placebo-controlled trial in patients treated by selective digestive decontamination. Intensiv. Care Med. 2002, 28, 1708–1717. [Google Scholar] [CrossRef]
- Pelz, R.K.; Hendrix, C.W.; Swoboda, S.M.; Diener-West, M.; Merz, W.G.; Hammond, J.; Lipsett, P.A. Double-blind placebo-controlled trial of fluconazole to prevent candidal infections in critically ill surgical patients. Ann. Surg. 2001, 233, 542–548. [Google Scholar] [CrossRef]
- Swoboda, S.M.; Merz, W.G.; Lipsetta, P.A. Candidemia: The impact of antifungal prophylaxis in a surgical intensive care unit. Surg. Infect. 2003, 4, 345–354. [Google Scholar] [CrossRef]
- Eggimann, P.; Francioli, P.; Bille, J.; Schneider, R.; Wu, MM.; Chapuis, G.; Chiolero, R. Fluconazole prophylaxis prevents intra-abdominal candidiasis in high-risk surgical patients. Crit. Care Med. 1999, 27, 1066–1072. [Google Scholar] [CrossRef]
- Grewe, M.; Tsiotos, G.G.; Luque de-Leon, E.; Sarr, M.G. Fungal infection in acute necrotizing pancreatitis. J. Am. Coll. Surg. 1999, 188, 408–414. [Google Scholar] [CrossRef]
- De Waele, J.J.; Vogelaers, D.; Blot, S.; Colardyn, F. Fungal infections in patients with severe acute pancreatitis and the use of prophylactic therapy. Clin. Infect. Dis. 2003, 37, 208–213. [Google Scholar] [CrossRef]
- Cruciani, M.; de Lalla, F.; Mengoli, C. Prophylaxis of Candida infections in adult trauma and surgical intensive care patients: A systematic review and meta-analysis. Intensiv. Care Med. 2005, 31, 1479–1487. [Google Scholar] [CrossRef]
- Playford, E.G.; Webster, A.C.; Sorrell, T.C.; Craig, J.C. Antifungal agents for preventing fungal infections in non-neutropenic critically ill and surgical patients: Systematic review and meta-analysis of randomized clinical trials. J. Antimicrob. Chemother. 2006, 57, 628–638. [Google Scholar] [CrossRef]
- Shorr, A.F.; Chung, K.; Jackson, W.L.; Waterman, P.E.; Kollef, M.H. Fluconazole prophylaxis in critically ill surgical patients: A meta-analysis. Crit. Care Med. 2005, 33, 1928–1935. [Google Scholar] [CrossRef]
- Vardakas, K.Z.; Samonis, G.; Michalopoulos, A.; Soteriades, E.S.; Falagas, M.E. Antifungal prophylaxis with azoles in high-risk, surgical intensive care unit patients: A meta-analysis of randomized, placebo-controlled trials. Crit. Care Med. 2006, 34, 1216–1224. [Google Scholar] [CrossRef]
- Lam, S.W.; Eschenauer, G.A.; Carver, P.L. Evolving role of early antifungals in the adult intensive care unit. Crit. Care Med. 2009, 37, 1580–1593. [Google Scholar] [CrossRef]
- Piarroux, R.; Grenouillet, F.; Balvay, P.; Tran, V.; Blasco, G.; Millon, L.; Boillot, A. Assessment of preemptive treatment to prevent severe candidiasis in critically ill surgical patients. Crit. Care Med. 2004, 32, 2443–2449. [Google Scholar] [CrossRef]
- Hanson, K.E.; Pfeiffer, C.D.; Lease, E.D.; Balch, A.H.; Zaas, A.K.; Perfect, J.R.; Alexander, B.D. Beta-d-glucan surveillance with preemptive anidulafungin for invasive candidiasis in intensive care unit patients: A randomized pilot study. PloS one 2012, 7, e42282. [Google Scholar]
- Schuster, M.G.; Edwards, J.E., Jr.; Sobel, J.D.; Darouiche, R.O.; Karchmer, A.W.; Hadley, S.; Slotman, G.; Panzer, H.; Biswas, P.; Rex, J.H. Empirical fluconazole versus placebo for intensive care unit patients: A randomized trial. Ann. Intern. Med. 2008, 149, 83–90. [Google Scholar]
- Golan, Y. Empiric anti-Candida therapy for patients with sepsis in the ICU: How little is too little? Crit. Care 2009, 13, 180. [Google Scholar] [CrossRef]
- Cornely, O.A.; Maertens, J.; Bresnik, M.; Ebrahimi, R.; Dellow, E.; Herbrecht, R.; Donnelly, J.P. Efficacy outcomes in a randomised trial of liposomal amphotericin B based on revised EORTC/MSG 2008 definitions of invasive mould disease. Mycoses 2011, 54, e449–e455. [Google Scholar] [CrossRef]
- Walsh, T.J.; Anaissie, E.J.; Denning, D.W.; Herbrecht, R.; Kontoyiannis, D.P.; Marr, K.A.; Morrison, V.A.; Segal, B.H.; Steinbach, W.J.; Stevens, D.A.; et al. Treatment of aspergillosis: Clinical practice guidelines of the Infectious Diseases Society of America. Clin. Infect. Dis. 2008, 46, 327–360. [Google Scholar] [CrossRef]
- Maertens, J.; Raad, I.; Petrikkos, G.; Boogaerts, M.; Selleslag, D.; Petersen, F.B.; Sable, C.A.; Kartsonis, N.A.; Ngai, A.; Taylor, A.; et al. Efficacy and safety of caspofungin for treatment of invasive aspergillosis in patients refractory to or intolerant of conventional antifungal therapy. Clin. Infect. Dis. 2004, 39, 1563–1571. [Google Scholar] [CrossRef]
- Sutton, D.A.; Sanche, S.E.; Revankar, S.G.; Fothergill, A.W.; Rinaldi, M.G. In vitro amphotericin B resistance in clinical isolates of Aspergillus terreus, with a head-to-head comparison to voriconazole. J. Clin. Microbiol. 1999, 37, 2343–2345. [Google Scholar]
- Alcazar-Fuoli, L.; Mellado, E.; Alastruey-Izquierdo, A.; Cuenca-Estrella, M.; Rodriguez-Tudela, J.L. Aspergillus section Fumigati: Antifungal susceptibility patterns and sequence-based identification. Antimicrob. Agents Chemother. 2008, 52, 1244–1251. [Google Scholar] [CrossRef]
- Kousha, M.; Tadi, R.; Soubani, A.O. Pulmonary aspergillosis: A clinical review. Eur. Resp. J. 2011, 20, 156–174. [Google Scholar]
- Safdar, A. Strategies to enhance immune function in hematopoietic transplantation recipients who have fungal infections. Bone Marrow Transplant. 2006, 38, 327–337. [Google Scholar] [CrossRef]
- Price, T.H.; Bowden, R.A.; Boeckh, M.; Bux, J.; Nelson, K.; Liles, W.C.; Dale, D.C. Phase I/II trial of neutrophil transfusions from donors stimulated with G-CSF and dexamethasone for treatment of patients with infections in hematopoietic stem cell transplantation. Blood 2000, 95, 3302–3309. [Google Scholar]
- Ullmann, A.J.; Cornely, O.A. Antifungal prophylaxis for invasive mycoses in high risk patients. Curr. Opin. Infect. Dis. 2006, 19, 571–576. [Google Scholar] [CrossRef]
- Kontoyiannis, D.P.; Lewis, R.E. How I treat mucormycosis. Blood 2011, 118, 1216–1224. [Google Scholar] [CrossRef]
© 2014 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Paramythiotou, E.; Frantzeskaki, F.; Flevari, A.; Armaganidis, A.; Dimopoulos, G. Invasive Fungal Infections in the ICU: How to Approach, How to Treat. Molecules 2014, 19, 1085-1119. https://doi.org/10.3390/molecules19011085
Paramythiotou E, Frantzeskaki F, Flevari A, Armaganidis A, Dimopoulos G. Invasive Fungal Infections in the ICU: How to Approach, How to Treat. Molecules. 2014; 19(1):1085-1119. https://doi.org/10.3390/molecules19011085
Chicago/Turabian StyleParamythiotou, Elisabeth, Frantzeska Frantzeskaki, Aikaterini Flevari, Apostolos Armaganidis, and George Dimopoulos. 2014. "Invasive Fungal Infections in the ICU: How to Approach, How to Treat" Molecules 19, no. 1: 1085-1119. https://doi.org/10.3390/molecules19011085






