Migration of the Lag Screw after Intramedullary Treatment of AO/OTA 31.A2.1-3 Pertrochanteric Fractures Does Not Result in Higher Incidence of Cut-Outs, Regardless of Which Implant Was Used: A Comparison of Gamma Nail with and without U-Blade (RC) Lag Screw and Proximal Femur Nail Antirotation (PFNA)
Abstract
:1. Introduction
2. Materials and Methods
2.1. Diagnosis, Surgical Technique and Aftercare
2.2. Outcome Parameters
2.3. Complications
2.4. Statistical Analysis
3. Results
3.1. Time to Cut Out/Treatment
3.2. Migration of the Lag Screw/Blade
3.3. Functional Outcome
4. Discussion
Limitations
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Sandmann, G.; Biberthaler, P. Pertrochanteric femoral fractures in the elderly. Unfallchirurg 2015, 118, 447–462. [Google Scholar] [CrossRef] [PubMed]
- Baumgaertner, M.; Socci, A.; Casemyr, N.; Leslie, M. Implant options for the treatment of intertrochanteric fractures of the hip: Rationale, evidence, and recommendations. Bone Joint J. 2017, 99, 128–133. [Google Scholar] [CrossRef]
- Jun, L.; Augusto, R.; Sousa, M.; Zamboni, C.; Durigan, J.R.; Hungria, J.S.; Mercadante, M.T.; Christian, R.W.; Hungria, J.O.S. Late postoperative analysis of the tip-apex distance (TAD) in pertrochanteric fractures: Is there an accommodation of the implant within the bone? Injury 2017, 48, 54–56. [Google Scholar] [CrossRef]
- Carulli, C.; Piacentini, F.; Paoli, T.; Civinini, R.; Innocenti, M. A comparison of two fixation methods for femoral trochanteric fractures: A new generation intramedullary system vs sliding hip screw. Clin. Cases Miner Bone Metab. 2017, 14, 40–47. [Google Scholar] [CrossRef] [PubMed]
- Niu, E.; Ms, A.Y.; Harris, A.H.S.; Bishop, J. Which fixation device is preferred for surgical treatment of intertrochanteric hip fractures in the United States? A survey of orthopaedic surgeons. Clin. Orthop. Relat. Res. 2015, 473, 3647–3655. [Google Scholar] [CrossRef]
- Matre, K.; Ivar, L.; Gjertsen, J.; Vinje, T.; Espehaug, B.; Meling, J. Sliding hip screw versus IM nail in reverse oblique trochanteric and subtrochanteric fractures. A study of 2716 patients in the Norwegian Hip Fracture Register. Injury 2013, 44, 735–742. [Google Scholar] [CrossRef]
- Ozkan, K.; Eceviz, E.; Unay, K. Treatment of reverse oblique trochanteric femoral fractures with proximal femoral nail. Int. Orthop. 2011, 35, 595–598. [Google Scholar] [CrossRef]
- Kregor, P.J.; Obremskey, W.T.; Kreder, H.J.; Swiontkowski, M.F. Unstable pertrochanteric femoral fractures. J. Orthop. Trauma 2014, 28, 25–28. [Google Scholar] [CrossRef] [PubMed]
- Radaideh, A.M.; Qudah, H.A.; Audat, Z.A.; Jahmani, R.A.; Yousef, I.R.; Saleh, A.A. Functional and radiological results of proximal femoral nail antirotation (PFNA) osteosynthesis in the treatment of unstable pertrochanteric fractures. J. Clin. Med. 2018, 7. [Google Scholar] [CrossRef]
- Hoffmann, S.; Paetzold, R.; Stephan, D.; Püschel, K.; Buehren, V.; Augat, P. Biomechanical evaluation of interlocking lag screw design in intramedullary nailing of unstable pertrochanteric fractures. J Orthop Trauma 2013, 27, 483–490. [Google Scholar] [CrossRef]
- Zhang, H.; Zhu, X.; Pei, G.; Zeng, X.; Zhang, N.; Xu, P.; Chen, D.; Yu, W.; Zhang, X. A retrospective analysis of the InterTan nail and proximal femoral nail anti-rotation in the treatment of intertrochanteric fractures in elderly patients with osteoporosis: A minimum follow-up of 3 years. J. Orthop. Surg. Res. 2017, 12, 1–8. [Google Scholar] [CrossRef]
- Bojan, A.; Beimel, C.; Speitling, A.; Taglang, G.; Ekholm, C.; Jönsson, A. 3066 consecutive Gamma Nails. 12 years experience at a single centre. BMC Musculoskelet. Disord. 2010, 11, 1–10. [Google Scholar] [CrossRef]
- Geller, J.A.; Saifi, C.; Morrison, T.A. Tip-apex distance of intramedullary devices as a predictor of cut-out failure in the treatment of peritrochanteric elderly hip fractures. Int. Orthop. 2010, 34, 719–722. [Google Scholar] [CrossRef]
- Aicale, R.; Maffulli, N. Greater rate of cephalic screw mobilisation following proximal femoral nailing in hip fractures with a tip – apex distance (TAD) and a calcar referenced TAD greater than 25mm. J. Orthop. Surg. Res. 2018, 13, 1–9. [Google Scholar] [CrossRef]
- Chinzei, N.; Hiranaka, T.; Niikura, T.; Tsuji, M. Comparison of the sliding and femoral head rotation among three different femoral head fixation devices for trochanteric fractures. Clin. Orthop. Surg. 2015, 7, 291–297. [Google Scholar] [CrossRef]
- Lenich, A.; Vester, H.; Nerlich, M.; Mayr, E.; Stöckle, U.; Füchtmeier, B. Clinical comparison of the second and third generation of intramedullary devices for trochanteric fractures of the hip—Blade vs screw. Injury 2010, 41, 1292–1296. [Google Scholar] [CrossRef]
- Queally, J.; Harris, E.; Handoll, H.; Parker, M. Intramedullary nails for extracapsular hip fractures in adults. Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef]
- Lang, N.W.; Arthold, C.; Joestl, J.; Gormasz, A.; Boesmueller, S.; Hajdu, S.; Sarahrudi, K. Does an additional antirotation U-Blade (RC) lag screw improve treatment of AO / OTA 31 A1-3 fractures with gamma 3 nail? Injury 2016, 47, 2733–2738. [Google Scholar] [CrossRef]
- Ma, K.; Wang, X.; Luan, F.; Xu, H.; Fang, Y.; Min, J.; Luan, H.X.; Yang, F.; Zheng, H.; He, S.J. Proximal femoral nails antirotation, Gamma nails, and dynamic hip screws for fixation of intertrochanteric fractures of femur: A meta-analysis. Orthop. Traumatol. Surg. Res. 2014, 100, 859–866. [Google Scholar] [CrossRef] [Green Version]
- Mueller, M. Classification and international AO-documentation of femur fractures. Unfallheilkunde 1980, 83, 251–259. [Google Scholar]
- Maggi, S.; Siviero, P.; Wetle, T.; Besdine, R.W. A multicenter survey on profile of care for hip fracture: Predictors of mortality and disability. Osteoporos. Int. 2010, 21, 223–231. [Google Scholar] [CrossRef] [PubMed]
- Bottle, A.; Aylin, P. Mortality associated with delay in operation after hip fracture: Observational study. BMJ 2006, 55, 947–951. [Google Scholar] [CrossRef]
- Kostuj, T.; Smektala, R.; Schulze-Raestrup, U.; Müller-Mai, C. Pertrochanteric fractures. What impact do surgical timing and implant choice have on the outcome? Unfallchirurg 2013, 116, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Smektala, R.; Endres, H.G.; Dasch, B.; Maier, C.; Trampisch, H.J.; Bonnaire, F.; Pientka, L. The effect of time-to-surgery on outcome in elderly patients with proximal femoral fractures. BMC Musculoskelet. Disord. 2008, 9, 171. [Google Scholar] [CrossRef]
- Parker, M. Cutting-out of the dynamic hip screw related to its position. J. Bone Joint Surg. Br. 1992, 74, 625. [Google Scholar] [CrossRef]
- Cleveland, M.; Bosworth, D.M.; Thompson, F.R.; Wilson, H.J.J.; Ishizuka, T. A ten-year analysis of intertrochanteric fractures of the femur. J. Bone Jt. Surgery Am. 1959, 41, 1399–1408. [Google Scholar] [CrossRef]
- Parmar, V.; Kumar, S.; Aster, A.; Harper, W.H. Review of methods to quantify lag screw placement in hip fracture fixation. Acta Orthopædica. Belgica. 2005, 3, 260–263. [Google Scholar]
- Kashigar, A.; Vincent, A.; Gunton, M.J.; Safir, O.; Kuzyk, P.R.T. Predictors of failure for cephalomedullary nailing of proximal femoral fractures. Bone Jt. J. 2014, 96, 1029–1034. [Google Scholar] [CrossRef]
- Parker, M.J.; Palmer, C.R. A new mobility score for predicting mortality after hip fractures. J. Bone Joint Surg. Br. 1993, 75, 797–798. [Google Scholar] [CrossRef]
- Georgiannos, D.; Lampridis, V.; Bisbinas, I. Complications following treatment of trochanteric fractures with the gamma3 nail: Is the latest version of gamma nail superior to its predecessor? Surg. Res. Pract. 2014, 2014, 3–8. [Google Scholar] [CrossRef]
- Andruszkow, H.; Frink, M.; Frömke, C.; Suntardjo, S.; Krettek, C.; Hildebrand, F. Tip apex distance, hip screw placement, and neck shaft angle as potential risk factors for cut-out failure of hip screws after surgical treatment of intertrochanteric fractures. Int. Orthop. 2012, 11, 2347–2354. [Google Scholar] [CrossRef]
- Murena, L.; Moretti, A.; Meo, F.; Saggioro, E.; Barbati, G.; Ratti, C. Predictors of cut-out after cephalomedullary nail fixation of pertrochanteric fractures: A retrospective study of 813 patients. Arch Orthop. Trauma Surg. 2018, 138, 351–359. [Google Scholar] [CrossRef]
- Liu, Y.; Tao, R.; Liu, F.; Wang, Y.; Zhou, Z.; Cao, Y.; Wang, H. Mid-term outcomes after intramedullary fixation of peritrochanteric femoral fractures using the new proximal femoral nail antirotation (PFNA). Injury 2010, 41, 810–817. [Google Scholar] [CrossRef]
- Simmermacher, R.K.J.; Ljungqvist, J.; Bail, H.; Hockerts, T.; Vochteloo, A.J.H.; Ochs, U.; Werken, C.v.; AO-PFNA studygroup. The new proximal femoral nail antirotation (PFNA) in daily practice: Results of a multicentre clinical study. Injury 2008, 39, 932–939. [Google Scholar] [CrossRef]
- Kraus, M.; Krischak, G.; Wiedmann, K.; Riepl, C.; Gebhard, F.; Jöckel, J.A.; Scola, A. Clinical evaluation of PFNA® and relationship between the tip-apex distance and mechanical failure. Unfallchirurg 2011, 114, 470–478. [Google Scholar] [CrossRef]
- Kammerlander, C.; Gebhard, F.; Meier, C.; Lenich, A.; Linhart, W.; Clasbrummel, B.; Neubauer-Gartzke, T.; Garcia-Alonso, M.; Pavelka, T.; Blauth, M. Standardised cement augmentation of the PFNA using a perforated blade: A new technique and preliminary clinical results. A prospective multicentre trial. Injury 2011, 42, 1484–1490. [Google Scholar] [CrossRef] [Green Version]
- Iwakura, T.; Niikura, T.; Lee, S.Y.; Sakai, Y.; Nishida, K.; Kuroda, R.; Kurosaka, M. Case report breakage of a third generation gamma nail: A case report and review of the literature. Case Rep. Orthop. 2013, 2013, 1–5. [Google Scholar] [CrossRef]
- Bojan, A.J.; Beimel, C.; Taglang, G.; Collin, D.; Ekholm, C.; Jönsson, A. Critical factors in cut-out complication after gamma nail treatment of proximal femoral fractures. BMC Musculoskelet. Disord. 2013, 14, 1–9. [Google Scholar] [CrossRef]
- Morvan, A.; Boddaert, J.; Cohen-Bittan, J.; Picard, H.; Pascal-Mousselard, H.; Khiami, F. Risk factors for cut-out after internal fixation of trochanteric fractures in elderly subjects. Orthop. Traumatol. Surg. Res. 2018, 104, 1183–1187. [Google Scholar] [CrossRef]
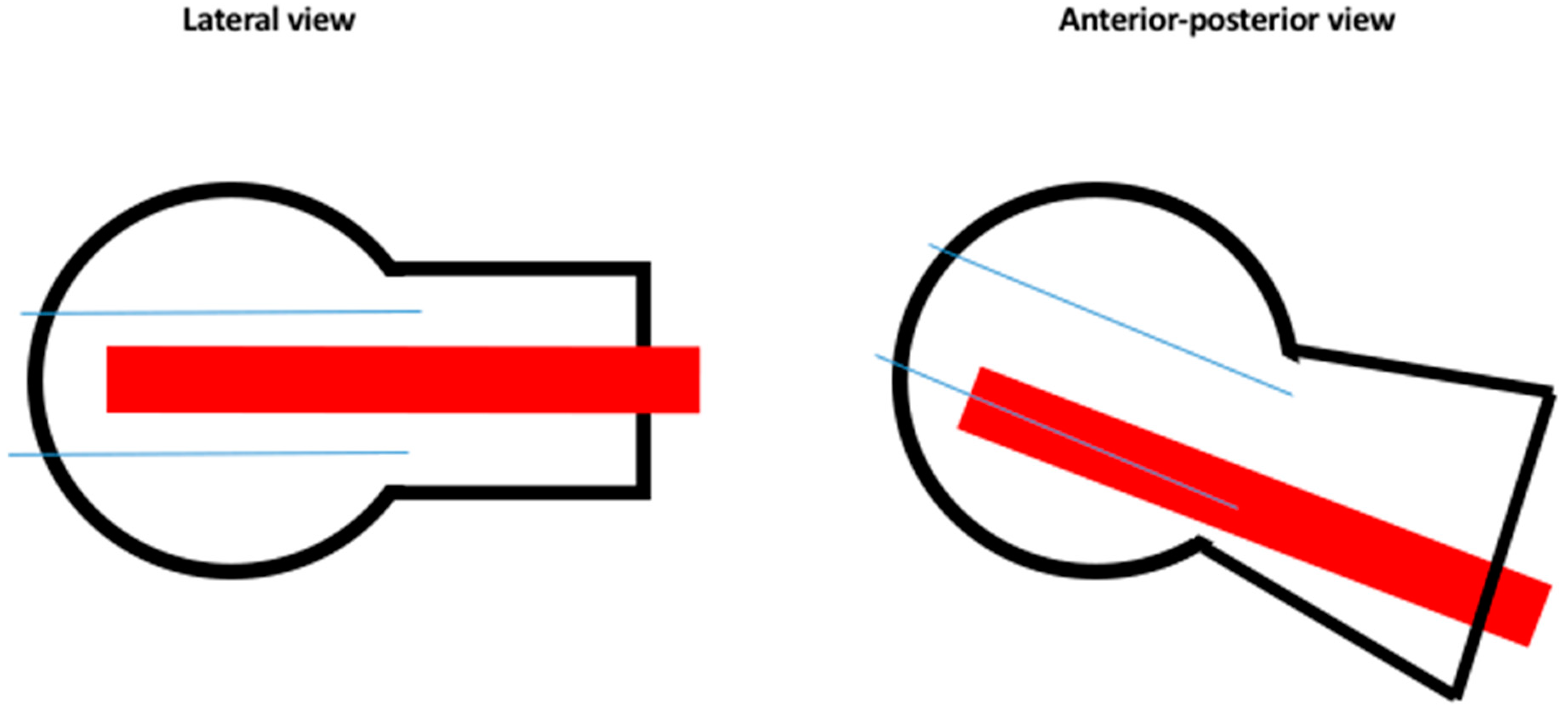
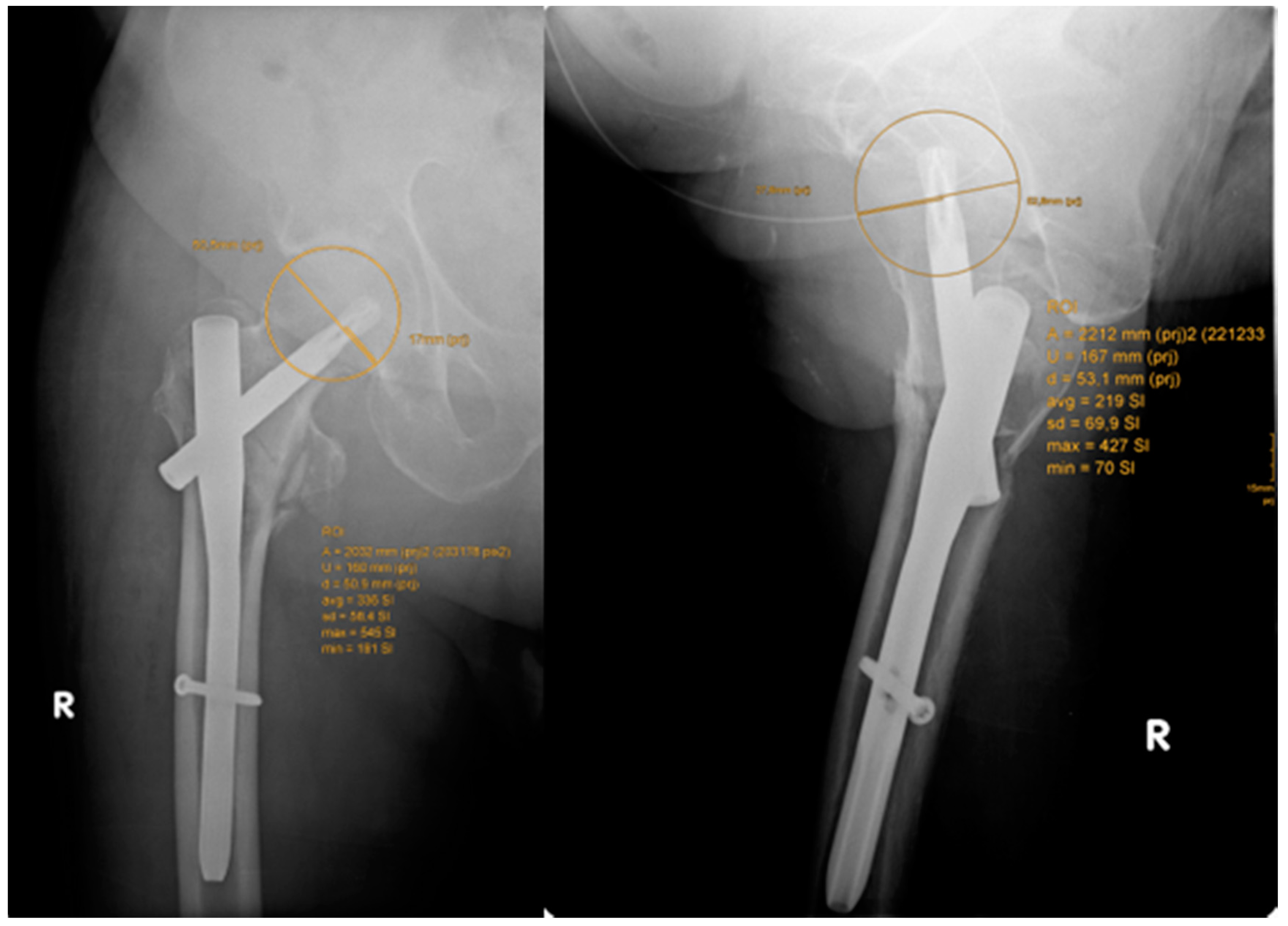
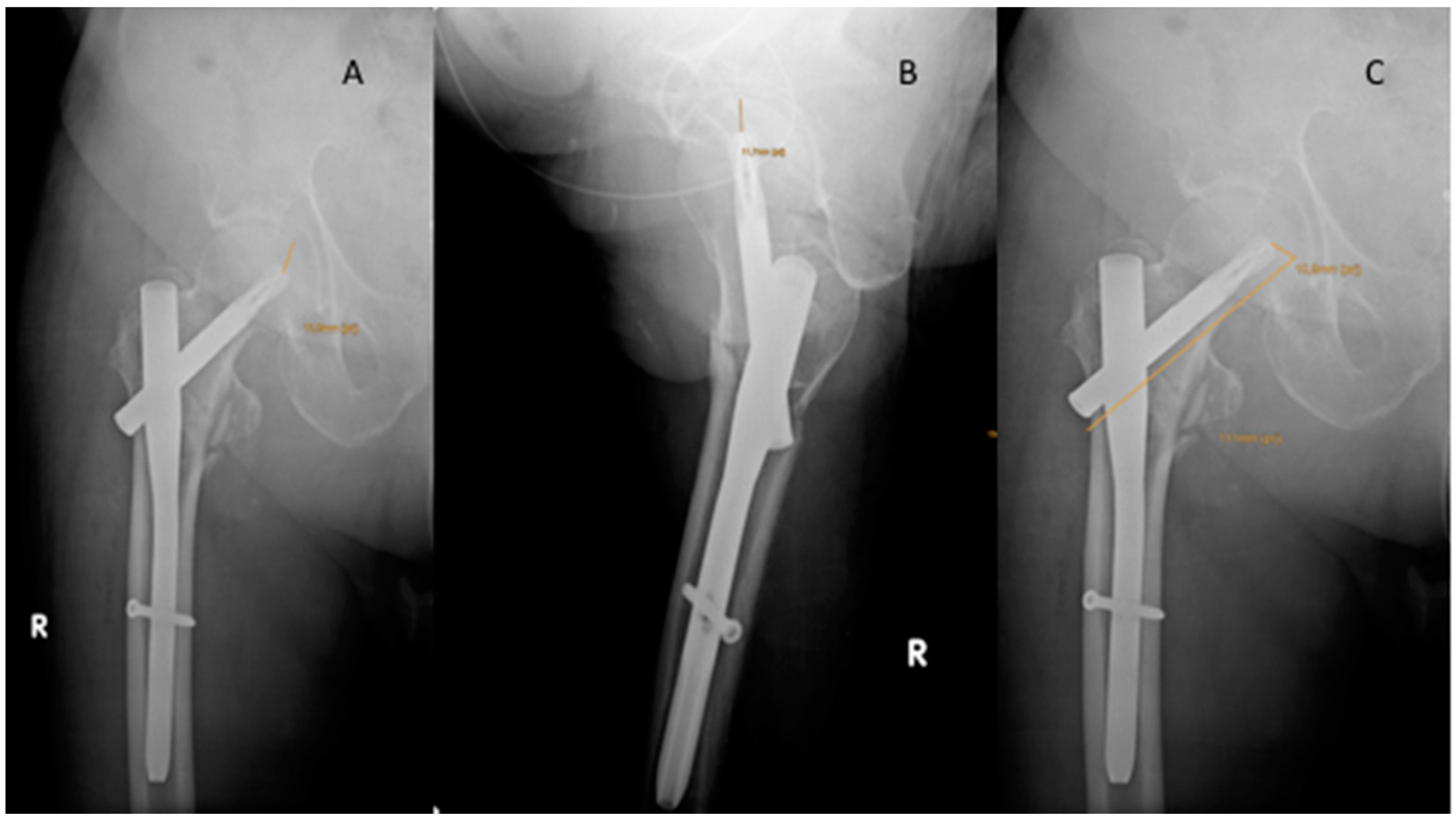
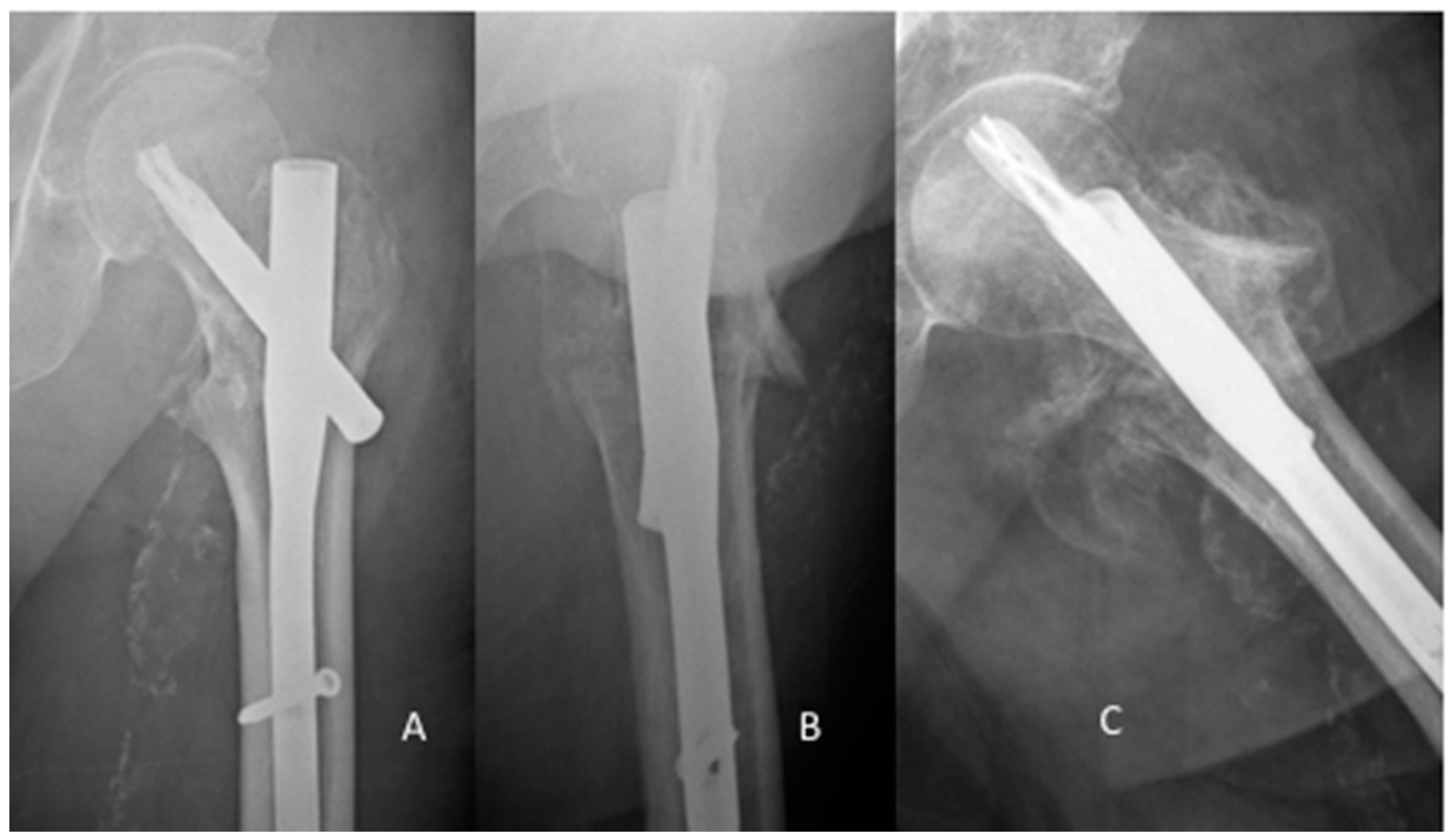
| PFNA | Gamma | U-Blade | Total | |
|---|---|---|---|---|
| (n = 86) | (n = 82) | (n = 69) | (n = 237) | |
| Male/Female | 15/71 | 19/63 | 11/58 | 45/192 |
| Age (years) | 80.7±11.7 | 82.0 ± 10.0 | 83.2 ± 9.6 | 81.9 ± 10.5 |
| BMI (kg/m2) | 23.4 ± 3.8 | 23.9 ± 4.6 | 24.6 ± 4.0 | 24.0 ± 4.1 |
| Operation (min) | 56.5 ± 22.4 | 57.1 ± 25.3 | 67.8 ± 23.8 * | 60.5 ± 23.8 |
| Lateralization | 3 | 5 | 10 | 22 |
| Cut-out | 1 | 3 | 2 | 6 |
| Infection (superficial) | 2 | 2 | 0 | 4 |
| Complications requiring surgery | 4 (4.7%) | 12 (14.6%) | 4 (5.7%) | 8.4% |
| PFNA | Gamma | U-Blade | Total | |
|---|---|---|---|---|
| Parker’s ratio AP | 45.1 ± 8.0 | 43.2 ± 8.1 | 47.8 ± 6.6 | 45.3 ± 7.8 |
| Parker’s ratio AP f/u | 54.6 ± 8.7 * | 45.1 ± 8.3 | 49.2 ± 7.7 | 49.8 ± 8.9 |
| Parker’s ratio LAT | 54.3 ± 7.7 | 55.2 ± 8.0 | 50.8 ± 7.2 | 53.6 ± 7.8 |
| Parker’s ratio LAT f/u | 53.7 ± 8.4 | 55.9 ± 7.1 | 49.3 ± 6.4 | 53.0 ± 7.9 |
| CalTAD | 12.6 ± 2.9 | 12.5 ± 2.9 | 14.2 ± 3.6 | 13.3 ± 3.3 |
| TAD | 20.4 ± 5.0 | 18.2 ± 4.8 | 16.5 ± 3.9 | 18.5 ± 4.8 |
| Lateral overhang | 14% | 8% | 8% | 10% |
| PFNA | Gamma | U-Blade | Total | |
|---|---|---|---|---|
| Number | 1 | 3 | 2 | 6 |
| Parker’s ratio AP | 39 | 48.7 ± 5.6 | 50.5 ± 3.5 | 47.9 ± 5.8 |
| Parker’s ratio LAT | 67 | 58.3 ± 7.6 | 60.5 ± 4.9 | 56.6 ± 11.6 |
| CalTAD | 18.7 | 14.6 ± 1.4 | 15.0 ± 1.4 | 15.3 ± 1.9 |
| TAD | 32.8 * | 18.3 ± 5.9 | 17.1 ± 4.3 | 20.0 ± 7.3 |
| Lateral overhang | 6% | 11% | 7% | 9% |
| PFNA | Gamma | U-Blade | Total | |
|---|---|---|---|---|
| Implant breakage | 3 | 3 | ||
| lateralization | 1 | 2 | 3 | |
| Wound infection | 1 * | 1 * | 2 | |
| Secondary femur fracture | 1 | 1 | 2 | |
| Non-union | 1 | 1 | ||
| Overall % | 2.3% | 8.5% | 2.9% | 4.6% |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lang, N.W.; Breuer, R.; Beiglboeck, H.; Munteanu, A.; Hajdu, S.; Windhager, R.; Widhalm, H.K. Migration of the Lag Screw after Intramedullary Treatment of AO/OTA 31.A2.1-3 Pertrochanteric Fractures Does Not Result in Higher Incidence of Cut-Outs, Regardless of Which Implant Was Used: A Comparison of Gamma Nail with and without U-Blade (RC) Lag Screw and Proximal Femur Nail Antirotation (PFNA). J. Clin. Med. 2019, 8, 615. https://doi.org/10.3390/jcm8050615
Lang NW, Breuer R, Beiglboeck H, Munteanu A, Hajdu S, Windhager R, Widhalm HK. Migration of the Lag Screw after Intramedullary Treatment of AO/OTA 31.A2.1-3 Pertrochanteric Fractures Does Not Result in Higher Incidence of Cut-Outs, Regardless of Which Implant Was Used: A Comparison of Gamma Nail with and without U-Blade (RC) Lag Screw and Proximal Femur Nail Antirotation (PFNA). Journal of Clinical Medicine. 2019; 8(5):615. https://doi.org/10.3390/jcm8050615
Chicago/Turabian StyleLang, Nikolaus Wilhelm, Robert Breuer, Hannes Beiglboeck, Alexandru Munteanu, Stefan Hajdu, Reinhard Windhager, and Harald Kurt Widhalm. 2019. "Migration of the Lag Screw after Intramedullary Treatment of AO/OTA 31.A2.1-3 Pertrochanteric Fractures Does Not Result in Higher Incidence of Cut-Outs, Regardless of Which Implant Was Used: A Comparison of Gamma Nail with and without U-Blade (RC) Lag Screw and Proximal Femur Nail Antirotation (PFNA)" Journal of Clinical Medicine 8, no. 5: 615. https://doi.org/10.3390/jcm8050615






