Bioactive and Biodegradable Nanocomposites and Hybrid Biomaterials for Bone Regeneration
Abstract
:1. Introduction
2. 3D Scaffold Design for Bone Regeneration
3. Scaffold Material Selection
3.1. Biocompatible and Biodegradable Polymers
| Melting Point (°C) | Glass Transition temperature (°C) | Tensile Modulus (GPa) | Degradation Time (months) | Degradation Products | |
|---|---|---|---|---|---|
| Poly(L-lactic acid) | 173–178 | 60–65 | 1.5–2.7 | >24 | L-lactic acid |
| Poly (D,L-lactic acid) | Amorphous | 55–60 | 1.9 | 12–16 | D,L-lactic acid |
| Poly (Glycolic acid) | 225–230 | 35–40 | 5–7 | 3–4 | Glycolic acid |
| Poly (ε-caprolactone) | 58–63 | –60 | 0.4–0.6 | >24 | Caproic acid |
| Poly (D,L-lactic-co-glycolic acid) (50/50) | Amorphous | 50–55 | 1.4–2.8 | 3–6 | D,L-lactic acid and glycolic acid |
| Poly (D,L-lactic-co-glycolic acid (85/15) | Amorphous | 50–55 | 1.4–2.8 | 3–6 | D,L-lactic acid and glycolic acid |
| Poly(D,L-lactic-co-glycolic acid) (90/10) | Amorphous | 50–55 | – | <3 | D,L-lactic acid and glycolic acid |
3.2. Bioceramics
3.2.1. Calcium Phosphates
3.2.2. Bioactive Glasses
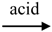 HO-M(OR)3 + R-OH
HO-M(OR)3 + R-OH4. Emerging Biomaterials: Nanocomposites and Organic-Inorganic Hybrids
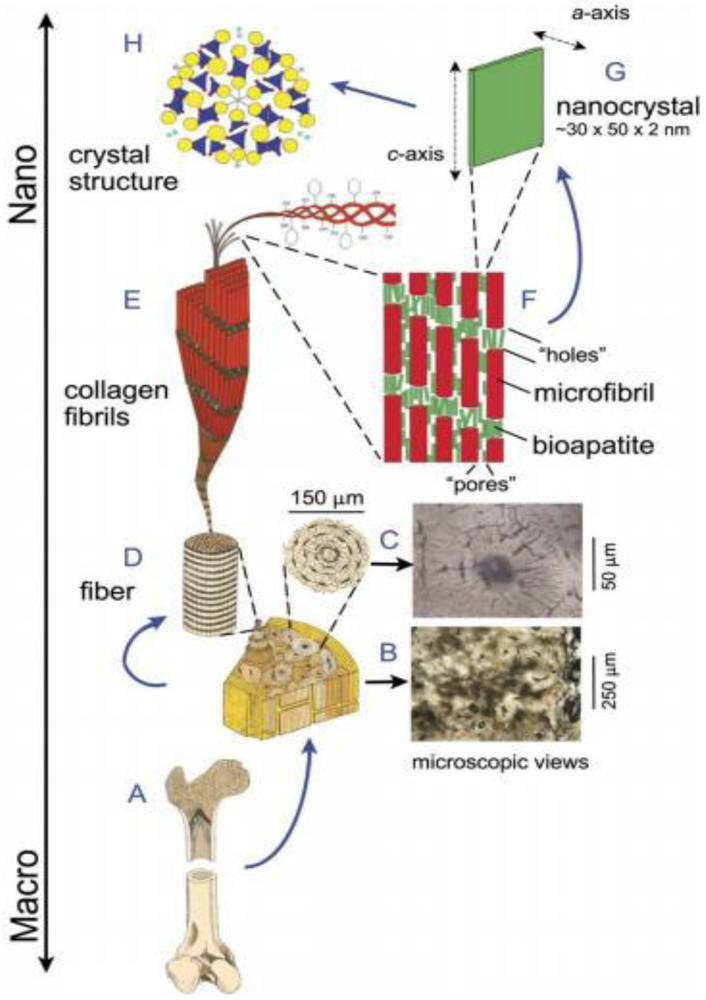
4.1. HA Based Nanocomposites
4.1.1. Conventional HA-Based Nanocomposites
4.1.2. Surface modified HA-Based Nanocomposites

4.2. Bioactive Glass Based Nanocomposites
4.2.1. Conventional BG-Based Nanocomposites
4.2.2. Surface Modified BG-Based Nanocomposites
4.3. Sol-Gel Derived Organic-Inorganic Hybrids
4.3.1. Class I Sol-Gel Derived O/I Hybrids
4.3.2. Class II Sol-Gel Derived O/I Hybrids
5. Conclusions and Future Prospects

| Material | Scaffold Fabrication Method | Mechanical Properties | In vitro | In vivo | Reference | |
|---|---|---|---|---|---|---|
| Modulus | Strength | |||||
| PLLA/HA | Phase separation, electrospinning | 8.3 MPa (compressive) | 3 MPa (tensile) | + | − | [122,128] |
| PLLA/collagen/HA | Electrospinning | - | 2 MPa (tensile) | + | − | [128] |
| PU/PCL/HA | Salt leaching/phase separation | 1.26 MPa (tensile) | - | + | + | [123,127] |
| PLLA/g-HA | Solvent casting (dense) | 2.5–4 GPa (tensile) | 58–75 MPa (tensile) | + | − | [131,132,135] |
| PCL/g-HA | Salt leaching/phase separation | 0.75 MPa (compressive) | 70 Pa (compressive) | − | − | [133] |
| PLGA/g-HA | Solvent casting (dense), salt leaching | 3.7 MPa (tensile), | 75 MPa (tensile), 2.31 MPa (compressive) | + | + | [137,138,139] |
| PLLA/BG | Thermally induced phase-separation | 8 MPa (compressive) | 0.35 MPa (compressive) | − | − | [140] |
| PLA/BG, PCL/BG | Electrospinning/thermal pressing (dense) | − | − | + | − | [143,145] |
| PLLA/g-BG | Solvent casting (dense) | 3 GPa (tensile) | 69.2 MPa (tension) | + | − | [147,148] |
| O/I Hybrid Monoliths | Sol-gel (dense) | 600 MPa (tensile) | 21 MPa (tensile) | − | − | [117,163] |
| O/I Hybrid Scaffolds | Sol-gel/Foaming | − | 0.3 MPa (compressive) | − | − | [107,152] |

Acknowledgments
References
- Einhorn, T.A. Clinically applied models of bone regeneration in tissue engineering research. Clin. Orthop. Relat. Res. 1999, 367, S59–S67. [Google Scholar] [CrossRef]
- Bucholz, R.W. Nonallograft osteoconductive bone graft substitutes. Clin. Orthop. Relat. Res. 2002, 395, 44–52. [Google Scholar] [CrossRef]
- Hak, D.J. The use of osteoconductive bone graft substitutes in orthopedic trauma. J. Am. Acad. Orthop. Surg. 2007, 15(9), 525–536. [Google Scholar]
- Kelly, C.M.; Wilkins, R.M. Treatment of benign bone lesions with an injectable calcium sulfate-based bone graft substitute. Orthopedics 2004, 27 Suppl. 1, S131–S135. [Google Scholar]
- Le Geros, R.Z. Calcium phosphates in oral biology and medicine. Monogr. Oral. Sci. 1991, 15, 1–201. [Google Scholar]
- Nery, E.B.; le Geros, R.Z.; Lynch, K.L.; Lee, K. Tissue response to biphasic calcium phosphate ceramic with different ratios of HA/beta TCP in periodontal osseous defects. J. Periodontol. 1992, 63(9), 729–735. [Google Scholar] [CrossRef]
- Woolf, A.D.; Pfleger, B. Burden of major musculoskeletal conditions. Bull. World Health Organ. 2003, 81(9), 646–656. [Google Scholar]
- Burg, K.J.; Porter, S.; Kellam, J.F. Biomaterial developments for bone tissue engineering. Biomaterials 2000, 21(23), 2347–2359. [Google Scholar] [CrossRef]
- Laurencin, C.T.; Khan, Y.; Kofron, M.; El-Amin, S.; Botchwey, E.; Yu, X.; Cooper, J.A., Jr. The ABJS Nicolas Andry Award: Tissue engineering of bone and ligament: A 15-year perspective. Clin. Orthop. Relat. Res. 2006, 447, 221–236. [Google Scholar] [CrossRef]
- Bauer, T.W.; Muschler, G.F. Bone graft materials. An overview of the basic science. Clin. Orthop. Relat. Res. 2000, 371, 10–27. [Google Scholar] [CrossRef]
- Salgado, A.J.; Coutinho, O.P.; Reis, R.L. Bone tissue engineering: state of the art and future trends. Macromol. Biosci. 2004, 4(8), 743–765. [Google Scholar] [CrossRef] [Green Version]
- Hutmacher, D.W. Scaffolds in tissue engineering bone and cartilage. Biomaterials 2000, 21(24), 2529–2543. [Google Scholar] [CrossRef]
- Tomford, W.W. Transmission of disease through transplantation of musculoskeletal allografts. J. Bone Joint Surg. Am. 1995, 77A(11), 1742–1754. [Google Scholar]
- Laurencin, C.; Khan, Y.; El-Amin, S.F. Bone graft substitutes. Expert Rev. Med. Devic. 2006, 3(1), 49–57. [Google Scholar] [CrossRef]
- Caplan, A.I.; Goldberg, V.M. Principles of tissue engineered regeneration of skeletal tissues. Clin. Orthop. Relat. Res. 1999, 367, S12–S16. [Google Scholar] [CrossRef]
- Vacanti, C.A.; Bonassar, L.J. An overview of tissue engineered bone. Clin. Orthop. Relat. Res. 1999, 367, S375–S381. [Google Scholar] [CrossRef]
- Hutmacher, D.W.; Schantz, J.T.; Lam, C.X.; Tan, K.C.; Lim, T.C. State of the art and future directions of scaffold-based bone engineering from a biomaterials perspective. J. Tissue Eng. Regen. Med. 2007, 1(4), 245–260. [Google Scholar] [CrossRef]
- Cancedda, R.; Giannoni, P.; Mastrogiacomo, M. A tissue engineering approach to bone repair in large animal models and in clinical practice. Biomaterials 2007, 28(29), 4240–4250. [Google Scholar] [CrossRef]
- Stevens, M.M.; Marini, R.P.; Schaefer, D.; Aronson, J.; Langer, R.; Shastri, V.P. In vivo engineering of organs: The bone bioreactor. Proc. Natl. Acad. Sci. USA 2005, 102(32), 11450–11455. [Google Scholar]
- Brekke, J.H.; Toth, J.M. Principles of tissue engineering applied to programmable osteogenesis. J. Biomed. Mater. Res. 1998, 43(4), 380–398. [Google Scholar] [CrossRef]
- Yang, S.; Leong, K.F.; Du, Z.; Chua, C.K. The design of scaffolds for use in tissue engineering. Part I. Traditional factors. Tissue Eng. 2001, 7(6), 679–689. [Google Scholar] [CrossRef]
- Oh, S.H.; Park, I.K.; Kim, J.M.; Lee, J.H. In vitro and in vivo characteristics of PCL scaffolds with pore size gradient fabricated by a centrifugation method. Biomaterials 2007, 28(9), 1664–1671. [Google Scholar] [CrossRef]
- Mondrinos, M.J.; Dembzynski, R.; Lu, L.; Byrapogu, V.K.; Wootton, D.M.; Lelkes, P.I.; Zhou, J. Porogen-based solid freeform fabrication of polycaprolactone-calcium phosphate scaffolds for tissue engineering. Biomaterials 2006, 27(25), 4399–4408. [Google Scholar]
- Xu, Q.; Ren, X.W.; Chang, Y.N.; Wang, J.W.; Yu, L.; Dean, K. Generation of microcellular biodegradable polycaprolactone foams in supercritical carbon dioxide. J. Appl. Polym. Sci. 2004, 94(2), 593–597. [Google Scholar] [CrossRef]
- Jenkins, M.J.; Harrison, K.L.; Silva, M.M.C.G.; Whitaker, M.J.; Shakesheff, K.M.; Howdle, S.M. Characterisation of microcellular foams produced from semi-crystalline PCL using supercritical carbon dioxide. Eur. Polym. J. 2006, 42(11), 3145–3151. [Google Scholar] [CrossRef]
- Di Maio, E.; Mensitieri, G.; Iannace, S.; Nicolais, L.; Li, W.; Flumerfelt, R.W. Structure optimization of polycaprolactone foams by using mixtures of CO2 and N2 as blowing agents. Polym. Eng. Sci. 2005, 45(3), 432–441. [Google Scholar] [CrossRef]
- Reignier, J.; Huneault, M.A. Preparation of interconnected poly(epsilon-caprolactone) porous scaffolds by a combination of polymer and salt particulate leaching. Polymer 2006, 47(13), 4703–4717. [Google Scholar] [CrossRef] [Green Version]
- Draghi, L.; Resta, S.; Pirozzolo, M.G.; Tanzi, M.C. Microspheres leaching for scaffold porosity control. J. Mater. Sci.:Mater. Med. 2005, 16(12), 1093–1097. [Google Scholar] [CrossRef]
- Grenier, S.; Sandig, M.; Mequanint, K. Smooth muscle alpha-actin and calponin expression and extracellular matrix production of human coronary artery smooth muscle cells in 3D scaffolds. Tissue Eng. A 2009, 15(10), 3001–3011. [Google Scholar] [CrossRef]
- Grenier, S.; Sandig, M.; Mequanint, K. Polyurethane biomaterials for fabricating 3D porous scaffolds and supporting vascular cells. J. Biomed. Mater. Res. A 2007, 82A(4), 802–809. [Google Scholar] [CrossRef]
- Hou, Q.P.; Grijpma, D.W.; Feijen, J. Porous polymeric structures for tissue engineering prepared by a coagulation, compression moulding and salt leaching technique. Biomaterials 2003, 24(11), 1937–1947. [Google Scholar]
- Murphy, W.L.; Dennis, R.G.; Kileny, J.L.; Mooney, D.J. Salt fusion: An approach to improve pore interconnectivity within tissue engineering scaffolds. Tissue Eng. 2002, 8(1), 43–52. [Google Scholar] [CrossRef]
- Grenier, S.; Sandig, M.; Holdsworth, D.W.; Mequanint, K. Interactions of coronary artery smooth muscle cells with 3D porous polyurethane scaffolds. J. Biomed. Mater. Res. A 2009, 89A(2), 293–303. [Google Scholar] [CrossRef]
- Yang, Q.; Chen, L.; Shen, X.Y.; Tan, Z.Q. Preparation of polycaprolactone tissue engineering scaffolds by improved solvent casting/particulate leaching method. J. Macromol. Sci. B 2006, 45(6), 1171–1181. [Google Scholar] [CrossRef]
- Hou, Q.P.; Grijpma, D.W.; Feijen, J. Preparation of interconnected highly porous polymeric structures by a replication and freeze-drying process. J. Biomed. Mater. Res. B 2003, 67B(2), 732–740. [Google Scholar] [CrossRef]
- Coombes, A.G.; Rizzi, S.C.; Williamson, M.; Barralet, J.E.; Downes, S.; Wallace, W.A. Precipitation casting of polycaprolactone for applications in tissue engineering and drug delivery. Biomaterials 2004, 25(2), 315–325. [Google Scholar]
- Wutticharoenmongkol, P.; Sanchavanakit, N.; Pavasant, P.; Supaphol, P. Preparation and characterization of novel bone scaffolds based on electrospun polycaprolactone fibers filled with nanoparticles. Macromol. Biosci. 2006, 6(1), 70–77. [Google Scholar] [CrossRef]
- Li, W.J.; Laurencin, C.T.; Caterson, E.J.; Tuan, R.S.; Ko, F.K. Electrospun nanofibrous structure: a novel scaffold for tissue engineering. J. Biomed. Mater. Res. 2002, 60(4), 613–621. [Google Scholar] [CrossRef]
- Izquierdo, R.; Garcia-Giralt, N.; Rodriguez, M.T.; Caceres, E.; Garcia, S.J.; Gomez-Ribelles, J.L.; Monleon, M.; Monllau, J.C.; Suay, J. Biodegradable PCL scaffolds with an interconnected spherical pore network for tissue engineering. J. Biomed. Mater. Res. A 2008, 85(1), 25–35. [Google Scholar]
- Lebourg, M.; Sabater-Serra, R.; Mas-Estelles, J.; Hernandez-Sanchez, F.; Gomez-Ribelles, J.L.; Suay-Anton, J. Biodegradable polycaprolactone scaffold with controlled porosity obtained by modified particle-leaching technique. J. Mater. Sci. Mater. Med. 2008, 19(5), 2047–2053. [Google Scholar] [CrossRef]
- Hou, Q.; Grijpma, D.W.; Feijen, J. Preparation of interconnected highly porous polymeric structures by a replication and freeze-drying process. J. Biomed. Mater. Res. B 2003, 67(2), 732–740. [Google Scholar]
- Draghi, L.; Resta, S.; Pirozzolo, M.G.; Tanzi, M.C. Microspheres leaching for scaffold porosity control. J. Mater. Sci. Mater. Med. 2005, 16(12), 1093–1097. [Google Scholar] [CrossRef]
- Thein-Han, W.W.; Misra, R.D.K. Biomimetic chitosan “nanohydroxyapatite composite scaffolds for bone tissue engineering. Acta Biomater. 2009, 5(4), 1182–1197. [Google Scholar] [CrossRef]
- Thein-Han, W.W.; Kitiyanant, Y.; Misra, R.D.K. Chitosan as scaffold matrix for tissue engineering. Mater. Sci. Tech. 2008, 24(9), 1062–1075. [Google Scholar] [CrossRef]
- Jayakumar, R.; Menon, D.; Manzoor, K.; Nair, S.V.; Tamura, H. Biomedical applications of chitin and chitosan based nanomaterials A short review. Carbohydrate Polym. 20 1082, (2), 227–232. [Google Scholar]
- Srinivasan, S.; Jayasree, R.; Chennazhi, K.P.; Nair, S.V.; Jayakumar, R. Biocompatible alginate/nano bioactive glass ceramic composite scaffolds for periodontal tissue regeneration. Carbohydrate Polym. 2011, 87(1), 274–283. [Google Scholar]
- Gunatillake, P.A.; Adhikari, R. Biodegradable synthetic polymers for tissue engineering. Eur. Cell Mater. 2003, 5, 1–16, disscussion 16. [Google Scholar]
- Rezwan, K.; Chen, Q.Z.; Blaker, J.J.; Boccaccini, A.R. Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 2006, 27(18), 3413–3431. [Google Scholar] [CrossRef]
- Puppi, D.; Chiellini, F.; Piras, A.M.; Chiellini, E. Polymeric materials for bone and cartilage repair. Prog. Polym. Sci. 2010, 35, 403–440. [Google Scholar] [CrossRef]
- Middleton, J.C.; Tipton, A.J. Synthetic biodegradable polymers as orthopedic devices. Biomaterials 2000, 21(23), 2335–2346. [Google Scholar] [CrossRef]
- Ulery, B.D.; Nair, L.S.; Laurencin, C.T. Biomedical applications of biodegradable polymers. J. Polym. Sci. B Polym. Phys. 2011, 49(12), 832–864. [Google Scholar] [CrossRef]
- Athanasiou, K.A.; Agrawal, C.M.; Barber, F.A.; Burkhart, S.S. Orthopedic applications for PLA-PGA biodegradable polymers. Arthroscopy 1998, 14(7), 726–737. [Google Scholar] [CrossRef]
- Bendix, D. Chemical synthesis of polylactide and its copolymers for medical applications. Polym. Degrad. Stabil. 1998, 59(1–3), 129–135. [Google Scholar] [CrossRef]
- Hubbell, J.A. Synthetic biodegradable polymers for tissue engineering and drug delivery. Curr. Opin. Solid St. Mater. Sci. 1998, 3(3), 246–251. [Google Scholar] [CrossRef]
- El-Ghannam, A. Bone reconstruction: from bioceramics to tissue engineering. Expert Rev. Med. Devic. 2005, 2(1), 87–101. [Google Scholar] [CrossRef]
- Wilson, J.; Low, S.B. Bioactive ceramics for periodontal treatment: Comparative studies in the Patus monkey. J. Appl. Biomater. 1992, 3(2), 123–129. [Google Scholar] [CrossRef]
- Posner, A.S. Crystal chemistry of bone mineral. Physiol. Rev. 1969, 49(4), 760–792. [Google Scholar]
- Le Geros, R.Z. Properties of osteoconductive biomaterials: Calcium phosphates. Clin. Orthop. Relat. Res. 2002, 395, 81–98. [Google Scholar] [CrossRef]
- Le Geros, R.Z.; Le Geros, J.P. Dense hydroxyapatite. In An Introduction to Bioceramics; Hench, L.L., Wilson, J., Eds.; World Scientific: Singapore, Singapore, 1993; pp. 139–180. [Google Scholar]
- Pang, Y.X.; Bao, X. Influence of temperature, ripening time and calcination on the morphology and crystallinity of hydroxyapatite nanoparticles. J. Eur. Ceram. Soc. 2003, 23(10), 1697–1704. [Google Scholar] [CrossRef]
- Jevtic, M.; Mitri, M.; kapin, S.; Janar, B.; Ignjatovi, N.; Uskokovi, D. Crystal structure of hydroxyapatite nanorods synthesized by sonochemical homogeneous precipitation. Cryst. Growth Des. 2008, 8(7), 2217–2222. [Google Scholar] [CrossRef]
- Tas, A.C. Formation of calcium phosphate whiskers in hydrogen peroxide (H2O2) solutions at 90 °C. J. Am. Ceram. Soc. 2007, 90(8), 2358–2362. [Google Scholar] [CrossRef]
- Liu, D.M.; Troczynski, T.; Tseng, W.J. Water-based sol-gel synthesis of hydroxyapatite: process development. Biomaterials 2001, 22(13), 1721–1730. [Google Scholar] [CrossRef]
- Taş, A.C. Molten salt synthesis of calcium hydroxyapatite Whiskers. J. Am. Ceram. Soc. 2001, 84(2), 295–300. [Google Scholar]
- Ins, S.N.; Yury, V.K.; Oleg, I.L.; Gustaaf, V.; Himadri, S.G.; Francisco, G.; Masahiro, Y. An effective morphology control of hydroxyapatite crystals via hydrothermal synthesis. Crys. Growth Des. 2009, 9(1), 466–474. [Google Scholar]
- Kaili, L.; Jiang, C.; Yingjie, Z.; Wei, W.; Guofeng, C.; Yi, Z.; Meiling, R. A facile one-step surfactant-free and low-temperature hydrothermal method to prepare uniform 3D structured carbonated apatite flowers. Cryst. Growth Des. 2009, 9(1), 177–181. [Google Scholar]
- Costa, D.O.; Dixon, S.J.; Rizkalla, A.S. One- and three-dimensional growth of hydroxyapatite nanowires during sol-gel-hydrothermal synthesis. ACS Appl. Mater. Interfaces 2012, 4, 1490–1499. [Google Scholar] [CrossRef]
- Oonishi, H.K.S.; Iwaki, H. Comparative bone formation in several kinds of bioceramic granules. In Proceedings of the 8th International Symposium on Ceramics in Medicine; Wilson, J.H.L., Greenspan, D., Eds.; Elsevier Science Ltd.: Tokyo, Japan, 1995; pp. 137–144. [Google Scholar]
- LeGeros, R.Z.; Lin, S.; Rohanizadeh, R.; Mijares, D.; Le Geros, J.P. Biphasic calcium phosphate bioceramics: Preparation, properties and applications. J. Mater. Sci. Mater. Med. 2003, 14(3), 201–209. [Google Scholar] [CrossRef]
- Wilke, A.; Orth, J.; Lomb, M.; Fuhrmann, R.; Kienapfel, H.; Griss, P.; Franke, R.P. Biocompatibility analysis of different biomaterials in human bone marrow cell cultures. J. Biomed. Mater. Res. 1998, 40(2), 301–306. [Google Scholar] [CrossRef]
- Ciapetti, G.; Ambrosio, L.; Savarino, L.; Granchi, D.; Cenni, E.; Baldini, N.; Pagani, S.; Guizzardi, S.; Causa, F.; Giunti, A. Osteoblast growth and function in porous poly epsilon-caprolactone matrices for bone repair: A preliminary study. Biomaterials 2003, 24(21), 3815–3824. [Google Scholar]
- Li, P. Biomimetic nano-apatite coating capable of promoting bone ingrowth. J. Biomed. Mater. Res. A 2003, 66(1), 79–85. [Google Scholar] [CrossRef]
- Scaglione, S.; Ilengo, C.; Fato, M.; Quarto, R. Hydroxyapatite-coated polycaprolacton wide mesh as a model of open structure for bone regeneration. Tissue Eng.A 2009, 15(1), 155–163. [Google Scholar] [CrossRef]
- Borsari, V.; Fini, M.; Giavaresi, G.; Tschon, M.; Chiesa, R.; Chiusoli, L.; Salito, A.; Rimondini, L.; Giardino, R. Comparative in vivo evaluation of porous and dense duplex titanium and hydroxyapatite coating with high roughnesses in different implantation environments. J. Biomed. Mater. Res. A 2009, 89(2), 550–560. [Google Scholar]
- Bigi, A.; Fini, M.; Bracci, B.; Boanini, E.; Torricelli, P.; Giavaresi, G.; Aldini, N.N.; Facchini, A.; Sbaiz, F.; Giardino, R. The response of bone to nanocrystalline hydroxyapatite-coated Ti13Nb11Zr alloy in an animal model. Biomaterials 2008, 29(11), 1730–1736. [Google Scholar]
- Vasudev, D.V.; Ricci, J.L.; Sabatino, C.; Li, P.; Parsons, J.R. In vivo evaluation of a biomimetic apatite coating grown on titanium surfaces. J. Biomed. Mater. Res. A 2004, 69(4), 629–636. [Google Scholar]
- Schliephake, H.; Scharnweber, D.; Dard, M.; Robetaler, S.; Sewing, A.; Huttmann, C. Biological performance of biomimetic calcium phosphate coating of titanium implants in the dog mandible. J. Biomed. Mater. Res. A 2003, 64(2), 225–234. [Google Scholar]
- Du, C.; Meijer, G.J.; van de Valk, C.; Haan, R.E.; Bezemer, J.M.; Hesseling, S.C.; Cui, F.Z.; de Groot, K.; Layrolle, P. Bone growth in biomimetic apatite coated porous Polyactive 1000PEGT70PBT30 implants. Biomaterials 2002, 23(23), 4649–4656. [Google Scholar] [CrossRef]
- Dekker, R.J.; de Bruijn, J.D.; Stigter, M.; Barrere, F.; Layrolle, P.; van Blitterswijk, C.A. Bone tissue engineering on amorphous carbonated apatite and crystalline octacalcium phosphate-coated titanium discs. Biomaterials 2005, 26(25), 5231–5239. [Google Scholar] [CrossRef]
- Lickorish, D.; Guan, L.; Davies, J.E. A three-phase, fully resorbable, polyester/calcium phosphate scaffold for bone tissue engineering: Evolution of scaffold design. Biomaterials 2007, 28(8), 1495–1502. [Google Scholar] [CrossRef]
- Nagano, M.; Nakamura, T.; Kokubo, T.; Tanahashi, M.; Ogawa, M. Differences of bone bonding ability and degradation behaviour in vivo between amorphous calcium phosphate and highly crystalline hydroxyapatite coating. Biomaterials 1996, 17(18), 1771–1777. [Google Scholar] [CrossRef]
- Geesink, R.G. Osteoconductive coatings for total joint arthroplasty. Clin. Orthop. Relat. Res. 2002, 395, 53–65. [Google Scholar] [CrossRef]
- Barrere, F.; van der Valk, C.M.; Dalmeijer, R.A.; Meijer, G.; van Blitterswijk, C.A.; de Groot, K.; Layrolle, P. Osteogenecity of octacalcium phosphate coatings applied on porous metal implants. J. Biomed. Mater. Res. A 2003, 66(4), 779–788. [Google Scholar]
- Habibovic, P.; van der Valk, C.M.; van Blitterswijk, C.A.; de Groot, K.; Meijer, G. Influence of octacalcium phosphate coating on osteoinductive properties of biomaterials. J. Mater. Sci. Mater. Med. 2004, 15(4), 373–380. [Google Scholar] [CrossRef]
- Habibovic, P.; Li, J.P.; van der Valk, C.M.; Meijer, G.; Layrolle, P.; van Blitterswijk, C.A.; de Groot, K. Biological performance of uncoated and octacalcium phosphate-coated Ti6A14V. Biomaterials 2005, 26(1), 23–36. [Google Scholar]
- Hench, L.L.; Splinter, R.J.; Allen, W.C.; Greenlee, T.K. Bonding mechanisms at the interface of ceramic prosthetic materials. J. Biomed. Mater. Res. 1971, 5(6), 117–141. [Google Scholar] [CrossRef]
- Salinas, A.J.; Martin, A.I.; Vallet-Regi, M. Bioactivity of three CaO-P2O5-SiO2 sol-gel glasses. J. Biomed. Mater. Res. 2002, 61(4), 524–532. [Google Scholar] [CrossRef]
- Weinstein, A.M.; Klawitter, J.J.; Cook, S.D. Implant-bone interface characteristics of bioglass dental implants. J. Biomed. Mater. Res. 1980, 14(1), 23–29. [Google Scholar] [CrossRef]
- Hench, L.L. Bioceramics: From concept to clinic. J. Amer. Ceram. Soc. 1991, 74(7), 1487–1510. [Google Scholar] [CrossRef]
- Li, R.; Clark, A.E.; Hench, L.L. An investigation of bioactive glass powders by sol-gel processing. J. Appl. Biomater. 1991, 2(4), 231–239. [Google Scholar] [CrossRef]
- Hench, L.L.; West, J.K. The sol-gel process. Chem. Rev. 1990, 90(1), 33–72. [Google Scholar] [CrossRef]
- Saravanapavan, P.; Hench, L.L. Mesoporous calcium silicate glasses. I. Synthesis. J. Non-Cryst. Solids 2003, 318(1–2), 1–13. [Google Scholar] [CrossRef]
- Jones, J.R.; Ehrenfried, L.M.; Hench, L.L. Optimising bioactive glass scaffolds for bone tissue engineering. Biomaterials 2006, 27(7), 964–973. [Google Scholar] [CrossRef]
- Pereira, M.M.; Clark, A.E.; Hench, L.L. Calcium phosphate formation on sol-gel-derived bioactive glasses in vitro. J. Biomed. Mater. Res. 1994, 28(6), 693–698. [Google Scholar] [CrossRef]
- Arcos, D.; Vallet-Regi, M. Sol-gel silica-based biomaterials and bone tissue regeneration. Acta Biomater. 2010, 6(8), 2874–2888. [Google Scholar] [CrossRef]
- Lobel, K.D.; Hench, L.L. In vitro adsorption and activity of enzymes on reaction layers of bioactive glass substrates. J. Biomed. Mater. Res. 1998, 39(4), 575–579. [Google Scholar] [CrossRef]
- Day, R.M.; Boccaccini, A.R.; Shurey, S.; Roether, J.A.; Forbes, A.; Hench, L.L.; Gabe, S.M. Assessment of polyglycolic acid mesh and bioactive glass for soft-tissue engineering scaffolds. Biomaterials 2004, 25(27), 5857–5866. [Google Scholar]
- Ohgushi, H.; Dohi, Y.; Yoshikawa, T.; Tamai, S.; Tabata, S.; Okunaga, K.; Shibuya, T. Osteogenic differentiation of cultured marrow stromal stem cells on the surface of bioactive glass ceramics. J. Biomed. Mater. Res. 1996, 32(3), 341–348. [Google Scholar] [CrossRef]
- Livingston, T.; Ducheyne, P.; Garino, J. In vivo evaluation of a bioactive scaffold for bone tissue engineering. J. Biomed. Mater. Res. 2002, 62(1), 1–13. [Google Scholar] [CrossRef]
- Gatti, A.M.; Valdre, G.; Andersson, O.H. Analysis of the in vivo reactions of a bioactive glass in soft and hard tissue. Biomaterials 1994, 15(3), 208–212. [Google Scholar] [CrossRef]
- Xynos, I.D.; Edgar, A.J.; Buttery, L.D.; Hench, L.L.; Polak, J.M. Ionic products of bioactive glass dissolution increase proliferation of human osteoblasts and induce insulin-like growth factor II mRNA expression and protein synthesis. Biochem. Biophys. Res. Commun. 2000, 276(2), 461–465. [Google Scholar] [CrossRef]
- Jell, G.; Stevens, M.M. Gene activation by bioactive glasses. J. Mater. Sci. Mater. Med. 2006, 17(11), 997–1002. [Google Scholar] [CrossRef]
- Xynos, I.D.; Hukkanen, M.V.; Batten, J.J.; Buttery, L.D.; Hench, L.L.; Polak, J.M. Bioglass 45S5 stimulates osteoblast turnover and enhances bone formation in vitro: Implications and applications for bone tissue engineering. Calcif. Tissue Int. 2000, 67(4), 321–329. [Google Scholar] [CrossRef]
- Hench, L.L.; Polak, J.M. Third-generation biomedical materials. Science 2002, 295(5557), 1014–1017. [Google Scholar] [CrossRef]
- Rezwan, K.; Chen, Q.Z.; Blaker, J.J.; Boccaccini, A.R. Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 2006, 27(18), 3413–3431. [Google Scholar] [CrossRef]
- Lee, K.H.; Rhee, S.H. The mechanical properties and bioactivity of poly(methyl methacrylate)/SiO2-CaO nanocomposite. Biomaterials 2009, 30(20), 3444–3449. [Google Scholar] [CrossRef]
- Pereira, M.M.; Jones, J.R.; Orefice, R.L.; Hench, L.L. Preparation of bioactive glass-polyvinyl alcohol hybrid foams by the sol-gel method. J. Mater. Sci. Mater. med. 2005, 16(1), 1045–1050. [Google Scholar] [CrossRef]
- Jo, J.H.; Lee, E.J.; Shin, D.S.; Kim, H.E.; Kim, H.W.; Koh, Y.H.; Jang, J.H. In vitro/in vivo biocompatibility and mechanical properties of bioactive glass nanofiber and poly(epsilon-caprolactone) composite materials. J. Biomed. Mater. Res. B 2009, 91B(1), 213–220. [Google Scholar] [CrossRef]
- Cho, J.; Joshi, M.S.; Sun, C.T. Effect of inclusion size on mechanical properties of polymeric composites with micro and nano particles. Compos. Sci. Technol. 2006, 66(13), 1941–1952. [Google Scholar] [CrossRef]
- Wang, M.; Joseph, R.; Bonfield, W. Hydroxyapatite-polyethylene composites for bone substitution: Effects of ceramic particle size and morphology. Biomaterials 1998, 19(24), 2357–2366. [Google Scholar] [CrossRef]
- Chen, B.; Sun, K. Poly ([epsilon]-caprolactone)/hydroxyapatite composites: Effects of particle size, molecular weight distribution and irradiation on interfacial interaction and properties. Polym. Test. 2005, 24(1), 64–70. [Google Scholar] [CrossRef]
- Roeder, R.K.; Sproul, M.M.; Turner, C.H. Hydroxyapatite whiskers provide improved mechanical properties in reinforced polymer composites. J. Biomed. Mater. Res. A 2003, 67(3), 801–812. [Google Scholar]
- Pasteris, J.D.; Wopenka, B.; Valsami-Jones, E. Bone and tooth mineralization: Why apatite? Elements 2008, 4(2), 97–104. [Google Scholar] [CrossRef]
- Webster, T.J.; Ergun, C.; Doremus, R.H.; Siegel, R.W.; Bizios, R. Specific proteins mediate enhanced osteoblast adhesion on nanophase ceramics. J. Biomed. Mater. Res. 2000, 51(3), 475–83. [Google Scholar] [CrossRef]
- Loher, S.; Reboul, V.; Brunner, T.J.; Simonet, M.; Dora, C.; Neuenschwander, P.; Stark, W.J. Improved degradation and bioactivity of amorphous aerosol derived tricalcium phosphate nanoparticles in poly(lactide-co-glycolide). Nanotechnology 2006, 17(8), 2054–2061. [Google Scholar]
- Rhee, S.H.; Lee, Y.K.; Lim, B.S.; Yoo, J.J.; Kim, H.J. Evaluation of a novel poly(epsilon-caprolactone)-organosiloxane hybrid material for the potential application as a bioactive and degradable bone substitute. Biomacromolecules 2004, 5(4), 1575–1579. [Google Scholar] [CrossRef]
- Rhee, S.H. Bone-like apatite-forming ability and mechanical properties of poly(epsilon-caprolactone)/silica hybrid as a function of poly(epsilon-caprolactone) content. Biomaterials 2004, 25(7–8), 1167–1175. [Google Scholar] [CrossRef]
- Martin, A.I.; Salinas, A.J.; Vallet-Regi, M. Bioactive and degradable organic-inorganic hybrids. J. Eur. Ceram. Soc. 2005, 25(16), 3533–3538. [Google Scholar] [CrossRef]
- Roeder, R.K.; Sproul, M.M.; Turner, C.H. Hydroxyapatite whiskers provide improved mechanical properties in reinforced polymer composites. J. Biomed. Mater. Res. A 2003, 67A(3), 801–812. [Google Scholar] [CrossRef]
- Bhumiratana, S.; Grayson, W.L.; Castaneda, A.; Rockwood, D.N.; Gil, E.S.; Kaplan, D.L.; Vunjak-Novakovic, G. Nucleation and growth of mineralized bone matrix on silk-hydroxyapatite composite scaffolds. Biomaterials 2011, 32(11), 2812–2820. [Google Scholar]
- Muller, F.A.; Gbureck, U.; Kasuga, T.; Mizutani, Y.; Barralet, J.E.; Lohbauer, U. Whisker-reinforced calcium phosphate cements. J. Am. Ceram. Soc. 2007, 90(11), 3694–3697. [Google Scholar] [CrossRef]
- Wei, G.; Ma, P.X. Structure and properties of nano-hydroxyapatite/polymer composite scaffolds for bone tissue engineering. Biomaterials 2004, 25(19), 4749–4757. [Google Scholar] [CrossRef]
- Boissard, C.I.R.; Bourban, P.E.; Tami, A.E.; Alini, M.; Eglin, D. Nanohydroxyapatite/poly(ester urethane) scaffold for bone tissue engineering. Acta Biomaterialia 2009, 5(9), 3316–3327. [Google Scholar] [CrossRef]
- Jack, K.S.; Velayudhan, S.; Luckman, P.; Trau, M.; Grøndahl, L.; Cooper-White, J. The fabrication and characterization of biodegradable HA/PHBV nanoparticle-polymer composite scaffolds. Acta Biomater. 2009, 5(7), 2657–2667. [Google Scholar] [CrossRef]
- Jayabalan, M.; Shalumon, K.T.; Mitha, M.K.; Ganesan, K.; Epple, M. Effect of hydroxyapatite on the biodegradation and biomechanical stability of polyester nanocomposites for orthopedic applications. Acta Biomater. 2010, 6(3), 763–775. [Google Scholar] [CrossRef]
- Asran, A.S.; Henning, S.; Michler, G.H. Polyvinyl alcohol-collagen-hydroxyapatite biocomposite nanofibrous scaffold: Mimicking the key features of natural bone at the nanoscale level. Polymer 2010, 51(4), 868–876. [Google Scholar] [CrossRef]
- Laschke, M.W.; Strohe, A.; Menger, M.D.; Alini, M.; Eglin, D. In vitro and in vivo evaluation of a novel nanosize hydroxyapatite particles/poly(ester-urethane) composite scaffold for bone tissue engineering. Acta Biomater. 2010, 6(6), 2020–2027. [Google Scholar] [CrossRef]
- Prabhakaran, M.P.; Venugopal, J.; Ramakrishna, S. Electrospun nanostructured scaffolds for bone tissue engineering. Acta Biomater. 2009, 5(8), 2884–2893. [Google Scholar] [CrossRef]
- Depan, D.; Venkata Surya, P.K.C.; Girase, B.; Misra, R.D.K. Organic/inorganic hybrid network structure nanocomposite scaffolds based on grafted chitosan for tissue engineering. Acta Biomater. 2011, 7(5), 2163–2175. [Google Scholar] [CrossRef]
- Helwig, E.; Sandner, B.; Gopp, U.; Vogt, F.; Wartewig, S.; Henning, S. Ring-opening polymerization of lactones in the presence of hydroxyapatite. Biomaterials 2001, 22(19), 2695–2702. [Google Scholar] [CrossRef]
- Hong, Z.; Qiu, X.; Sun, J.; Deng, M.; Chen, X.; Jing, X. Grafting polymerization of L-lactide on the surface of hydroxyapatite nano-crystals. Polymer 2004, 45(19), 6699–6706. [Google Scholar]
- Hong, Z.; Zhang, P.; He, C.; Qiu, X.; Liu, A.; Chen, L.; Chen, X.; Jing, X. Nano-composite of poly(l-lactide) and surface grafted hydroxyapatite: Mechanical properties and biocompatibility. Biomaterials 2005, 26(32), 6296–6304. [Google Scholar] [CrossRef]
- Wang, Y.; Dai, J.; Zhang, Q.; Xiao, Y.; Lang, M. Improved mechanical properties of hydroxyapatite/poly(ε-caprolactone) scaffolds by surface modification of hydroxyapatite. Appl. Surf. Sci. 2010, 256(20), 6107–6112. [Google Scholar] [CrossRef]
- Zeng, L.; Wang, H.; Fu, G.; Jiang, J.; Zhang, X. A new approach for synthesis of the comb-shaped poly (ε-caprolactone) brushes on the surface of nano-hydroxyapatite by combination of ATRP and ROP. J. Colloid Interface Sci. 2010, 352(1), 36–42. [Google Scholar] [CrossRef]
- Qiu, X.Y.; Hong, Z.K.; Hu, J.L.; Chen, L.; Chen, X.S.; Jing, X.B. Hydroxyapatite surface modified by L-lactic acid and its subsequent grafting polymerization of L-lactide. Biomacromolecules 2005, 6(3), 1193–1199. [Google Scholar]
- Wang, Y.; Zhang, X.; Yan, J.; Xiao, Y.; Lang, M. Surface modification of hydroxyapatite with poly(methyl methacrylate) via surface-initiated ATRP. Appl. Surf. Sci. 2011, 257(14), 6233–6238. [Google Scholar] [CrossRef]
- Hong, Z.K.; Zhang, P.B.; Liu, A.X.; Chen, L.; Chen, X.S.; Jing, X.B. Composites of poly(lactide-co-glycolide) and the surface modified carbonated hydroxyapatite nanoparticles. J. Biomed. Mater. Res. A 2007, 81A(3), 515–522. [Google Scholar] [CrossRef]
- Zhang, P.; Hong, Z.; Yu, T.; Chen, X.; Jing, X. In vivo mineralization and osteogenesis of nanocomposite scaffold of poly(lactide-co-glycolide) and hydroxyapatite surface-grafted with poly(l-lactide). Biomaterials 2009, 30(1), 58–70. [Google Scholar] [CrossRef]
- Cui, Y.; Liu, Y.; Jing, X.; Zhang, P.; Chen, X. The nanocomposite scaffold of poly(lactide-co-glycolide) and hydroxyapatite surface-grafted with L-lactic acid oligomer for bone repair. Acta biomater. 2009, 5(7), 2680–2692. [Google Scholar] [CrossRef]
- Hong, Z.; Reis, R.L.; Mano, J.F. Preparation and in vitro characterization of scaffolds of poly(L-lactic acid) containing bioactive glass ceramic nanoparticles. Acta Biomater. 2008, 4(5), 1297–1306. [Google Scholar] [CrossRef] [Green Version]
- Hong, Z.; Reis, R.L.; Mano, J.F. Preparation and in vitro characterization of novel bioactive glass ceramic nanoparticles. J. Biomed. Mater. Res. A 2009, 88(2), 304–313. [Google Scholar]
- Hong, Z.K.; Liu, A.X.; Chen, L.; Chen, X.S.; Jing, X.B. Preparation of bioactive glass ceramic nanoparticles by combination of sol-gel and coprecipitation method. J. Non-Cryst. Solids 2009, 355(6), 368–372. [Google Scholar] [CrossRef]
- Kim, H.W.; Lee, H.H.; Chun, G.S. Bioactivity and osteoblast responses of novel biomedical nanocomposites of bioactive glass nanofiber filled poly(lactic acid). J. Biomed. Mater. Res. A 2008, 85(3), 651–663. [Google Scholar]
- Kim, H.W.; Song, J.H.; Kim, H.E. Bioactive glass nanofiber-collagen nanocomposite as a novel bone regeneration matrix. J. Biomed. Mater. Res. A 2006, 79(3), 698–705. [Google Scholar]
- Lee, H.H.; Yu, H.S.; Jang, J.H.; Kim, H.W. Bioactivity improvement of poly(epsilon-caprolactone) membrane with the addition of nanofibrous bioactive glass. Acta Biomater. 2008, 4(3), 622–629. [Google Scholar] [CrossRef]
- Kim, H.W.; Kim, H.E.; Knowles, J.C. Production and potential of bioactive glass nanofibers as a next-generation biomaterial. Adv. Funct. Mater. 2006, 16(12), 1529–1535. [Google Scholar] [CrossRef]
- Liu, A.X.; Hong, Z.K.; Zhuang, X.L.; Chen, X.S.; Cui, Y.; Liu, Y.; Jing, X.B. Surface modification of bioactive glass nanoparticles and the mechanical and biological properties of poly(L-lactide) composites. Acta Biomater. 2008, 4(4), 1005–1015. [Google Scholar] [CrossRef]
- Liu, A.X.; Wei, J.C.; Chen, X.S.; Jing, X.B.; Cui, Y.; Liu, Y. Novel composites of poly(l-lactide) and surface modified bioactive SiO2-CaO-P2O5 gel nanoparticles: Mechanical and biological properties. Chin. J. Polym. Sci. 2009, 27(3), 415–426. [Google Scholar] [CrossRef]
- Sanchez, C.; Julia, B.; Belleville, P.; Popall, M. Applications of hybrid organic–inorganic nanocomposites. J. Mater. Chem. 2005, 15, 3559–3592. [Google Scholar] [CrossRef]
- Jones, J.R. New trends in bioactive scaffolds: The importance of nanostructure. J. Eur. Ceram. Soc. 2009, 29(7), 1275–1281. [Google Scholar] [CrossRef]
- Niea, K.; Wang, W.P.; Lu, F.; Zhu, Q. Effects of specific bonding interactions in poly(q-caprolactone)/silica hybrid materials on optical transparency and melting behavior. Mater. Lett. 2005, 59, 1325–1328. [Google Scholar] [CrossRef]
- Pereira, M.M.; Jones, J.R.; Hench, L.L. Bioactive glass and hybrid scaffolds prepared by sol-gel method for bone tissue engineering. Adv. Appl. Ceram. 2005, 104(1), 35–42. [Google Scholar] [CrossRef]
- Chen, Q.; Kamitakahara, M.; Miyata, N.; Kokubo, T.; Nakamura, T. Preparation of bioactive PDMS-modified CaO-SiO2-TiO2 hybrids by the sol-gel method. J. Sol-Gel Sci. Techn. 2000, 19(1–3), 101–105. [Google Scholar] [CrossRef]
- Salinas, A.J.; Merino, J.M.; Babonneau, F.; Gil, F.J.; Vallet-Regi, M. Microstructure and macroscopic properties of bioactive CaO-SiO2-PDMS hybrids. J. Biomed. Mater. Res. B 2007, 81B(1), 274–282. [Google Scholar] [CrossRef]
- Chen, Q.; Miyata, N.; Kokubo, T.; Nakamura, T. Bioactivity and mechanical properties of PDMS-modified CaO-SiO2-TiO2 hybrids prepared by sol-gel process. J. Biomed. Mater. Res. 2000, 51(4), 605–611. [Google Scholar] [CrossRef]
- Chen, Q.; Miyata, N.; Kokubo, T. Bioactivity and mechanical properties of poly (dimethylsiloxane) modified calcia-silica hybrids with added titania. J. Am. Ceram. Soc. 2003, 86(5), 806–810. [Google Scholar] [CrossRef]
- Tian, D.; Blacher, S.; Dubois, P.; Jerome, R. Biodegradable and biocompatible inorganic-organic hybrid materials—2. Dynamic mechanical properties, structure and morphology. Polymer 1998, 39(4), 855–864. [Google Scholar] [CrossRef]
- Tian, D.; Blacher, S.; Pirard, J.P.; Jerome, R. Biodegradable and biocompatible inorganic-organic hybrid materials. 3. A valuable route to the control of the silica porosity. Langmuir 1998, 14(7), 1905–1910. [Google Scholar] [CrossRef]
- Tian, D.; Dubois, P.; Jerome, R. Biodegradable and biocompatible inorganic-organic hybrid materials .1. Synthesis and characterization. J. Polym. Sci. Pol. Chem. 1997, 35(11), 2295–2309. [Google Scholar] [CrossRef]
- Rhee, S.H.; Choi, J.Y.; Kim, H.M. Preparation of a bioactive and degradable poly(epsilon-caprolactone)/silica hybrid through a sol-gel method. Biomaterials 2002, 23(24), 4915–4921. [Google Scholar] [CrossRef]
- Rhee, S.H. Effect of molecular weight of poly(epsilon-caprolactone) on interpenetrating network structure, apatite-forming ability, and degradability of poly(epsilon-caprolactone)/silica nano-hybrid materials. Biomaterials 2003, 24(10), 1721–1727. [Google Scholar] [CrossRef]
- Kangming-Nie, S.Z.; Lu, F.; Zhu, Q. Inorganic-organic hybrids involving poly(e-caprolactone) and silica network: Hydrogen-bonding interactions and isothermal crystallization kinetics. J. Polym. Sci. B 2005, 43, 2594–2603. [Google Scholar] [CrossRef]
- Rhee, S.H. Effect of calcium salt content in the poly(epsilon-caprolactone)/silica nanocomposite on the nucleation and growth behavior of apatite layer. J. Biomed. Mater. Res. A 2003, 67A(4), 1131–1138. [Google Scholar] [CrossRef]
- Jandt, K.D. Evolutions, revolutions and trends in biomaterials science—A perspective. Adv. Eng. Mater. 2007, 9(12), 1035–1050. [Google Scholar] [CrossRef]
- Murugan, R.; Ramakrishna, S. Development of nanocomposites for bone grafting. Compos. Sci. Technol. 2005, 65(15–16), 2385–2406. [Google Scholar] [CrossRef]
- Rho, J.Y.; Kuhn-Spearing, L.; Zioupos, P. Mechanical properties and the hierarchical structure of bone. Med. Eng. Phys. 1998, 20(2), 92–102. [Google Scholar] [CrossRef]
- Reilly, D.T.; Burstein, A.H. The elastic and ultimate properties of compact bone tissue. J. Biomech. 1975, 8(6), 393–405. [Google Scholar] [CrossRef]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Allo, B.A.; Costa, D.O.; Dixon, S.J.; Mequanint, K.; Rizkalla, A.S. Bioactive and Biodegradable Nanocomposites and Hybrid Biomaterials for Bone Regeneration. J. Funct. Biomater. 2012, 3, 432-463. https://doi.org/10.3390/jfb3020432
Allo BA, Costa DO, Dixon SJ, Mequanint K, Rizkalla AS. Bioactive and Biodegradable Nanocomposites and Hybrid Biomaterials for Bone Regeneration. Journal of Functional Biomaterials. 2012; 3(2):432-463. https://doi.org/10.3390/jfb3020432
Chicago/Turabian StyleAllo, Bedilu A., Daniel O. Costa, S. Jeffrey Dixon, Kibret Mequanint, and Amin S. Rizkalla. 2012. "Bioactive and Biodegradable Nanocomposites and Hybrid Biomaterials for Bone Regeneration" Journal of Functional Biomaterials 3, no. 2: 432-463. https://doi.org/10.3390/jfb3020432





