Open Access Integrated Therapeutic and Diagnostic Platforms for Personalized Cardiovascular Medicine
Abstract
:1. Introduction
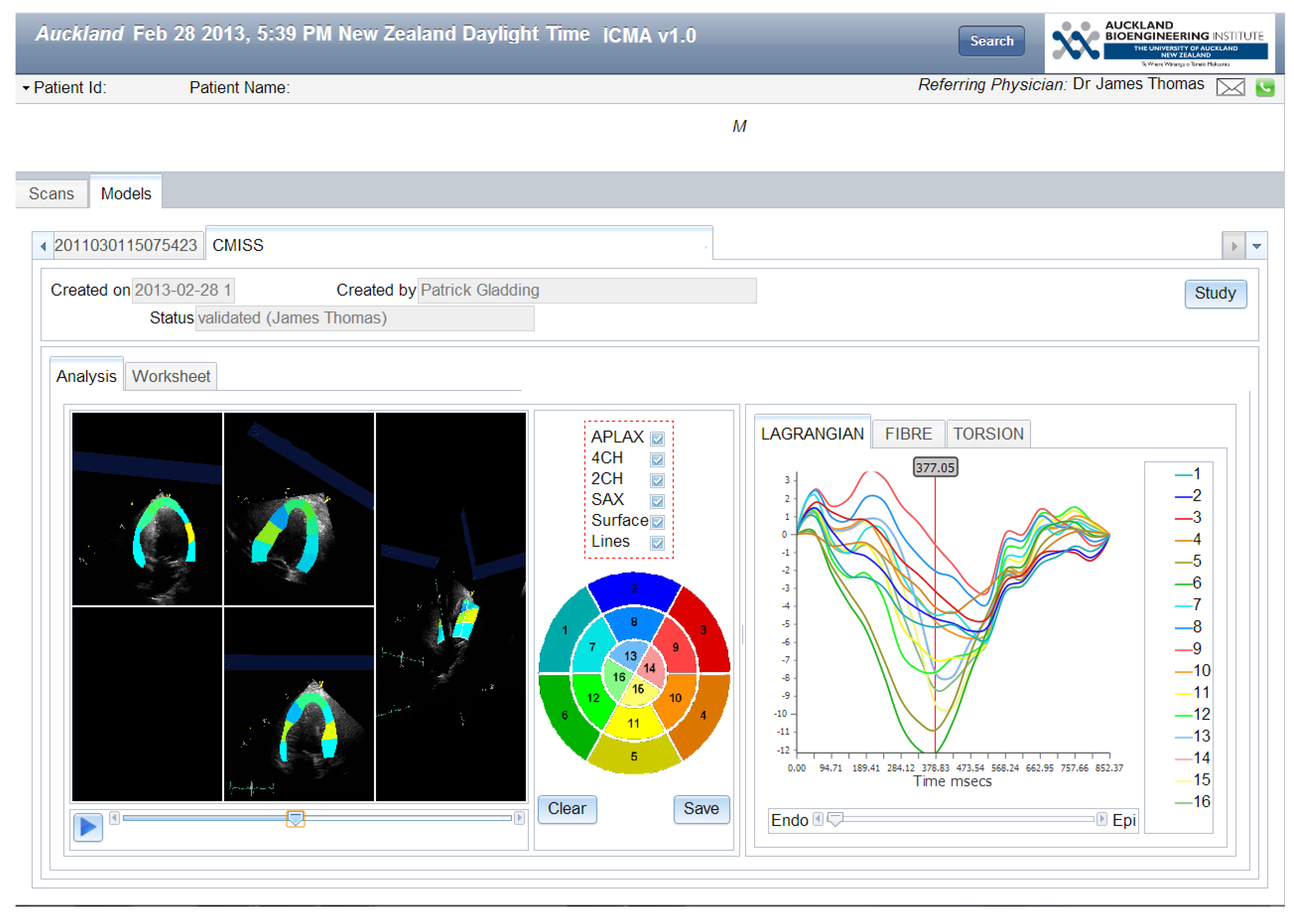
2. Personalized Cardiac Imaging using Ultrasound

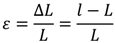
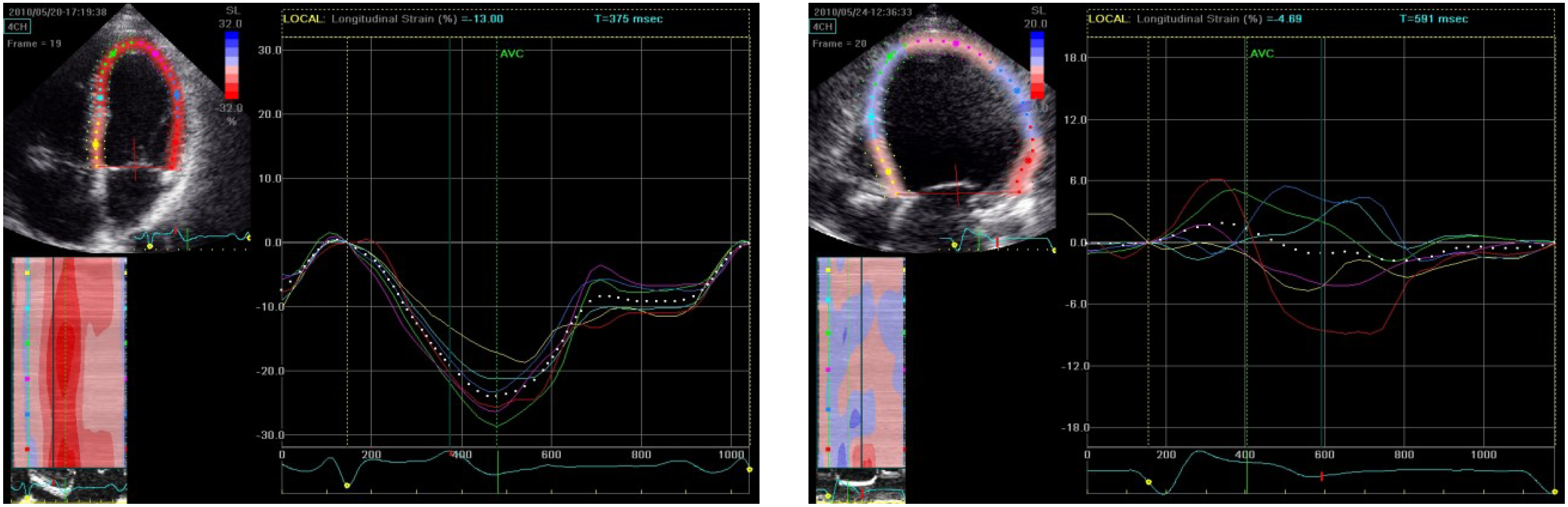
3. The Integrated Cardiovascular (ICV) Project

4. The Human Physiome Project
5. Advanced Electrocardiography

6. Cardiovascular Biomarkers for Personalized Medicine
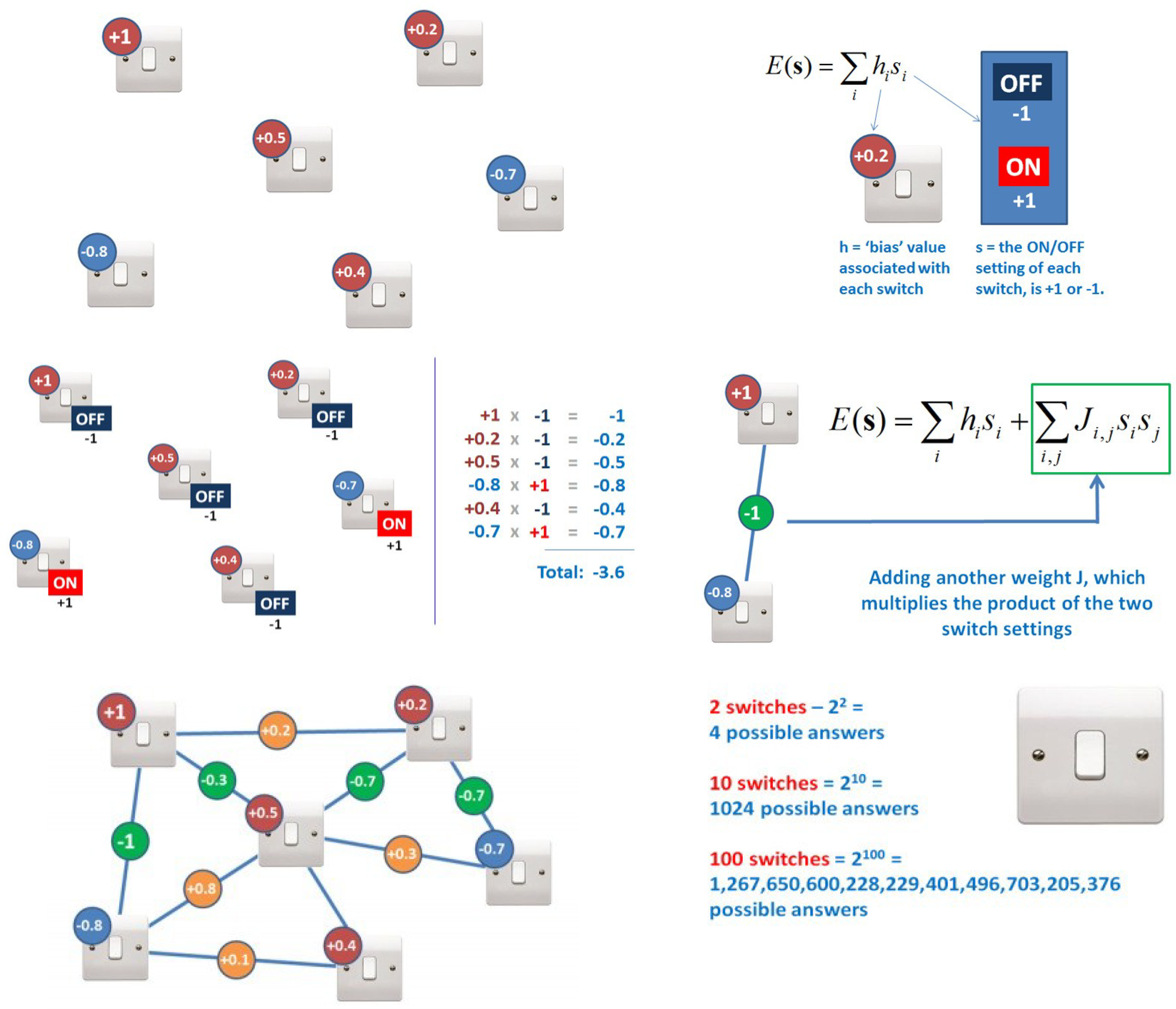
7. Bioinformatics and Supercomputing
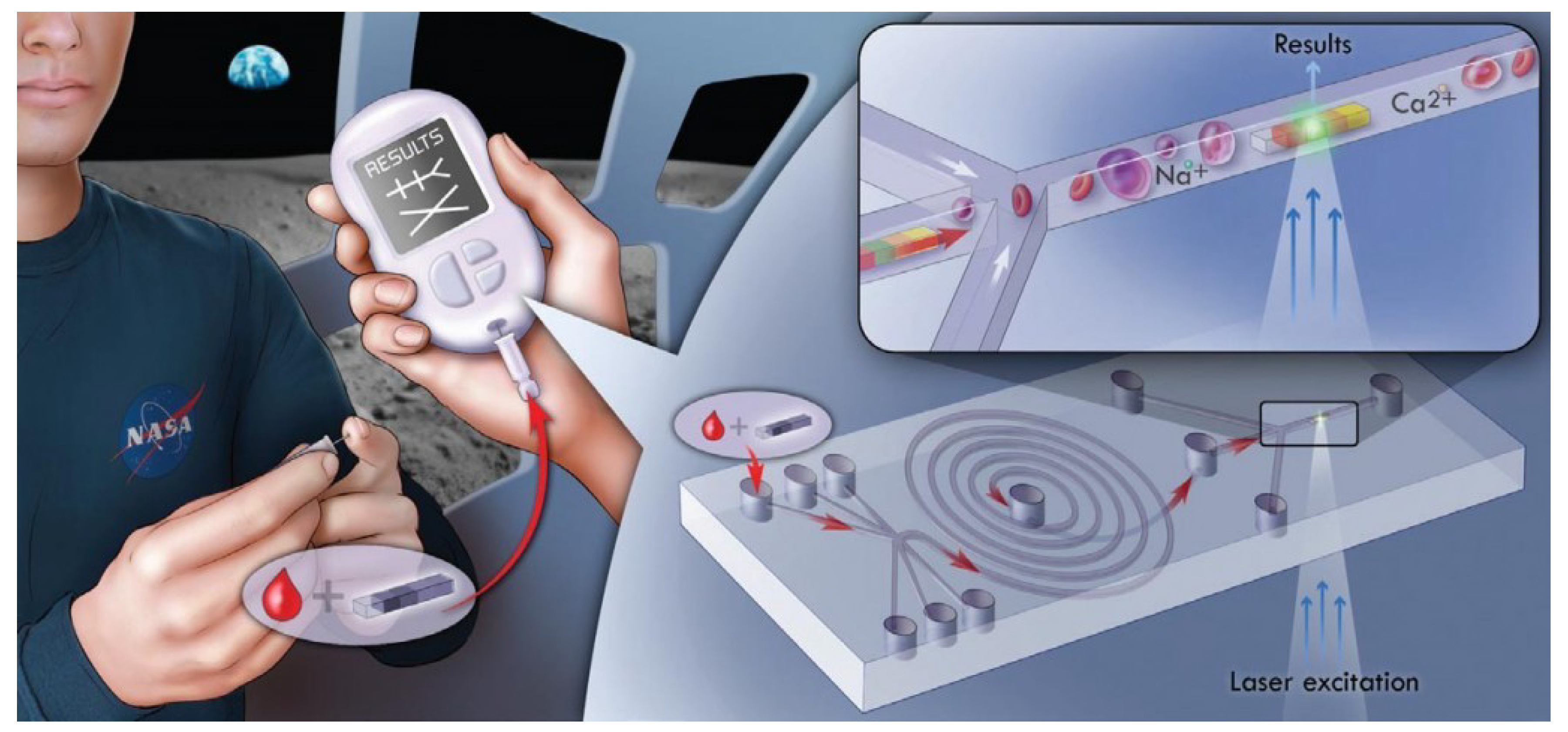
8. Cardiovascular Genomics and Handheld Point-of-Care Platforms

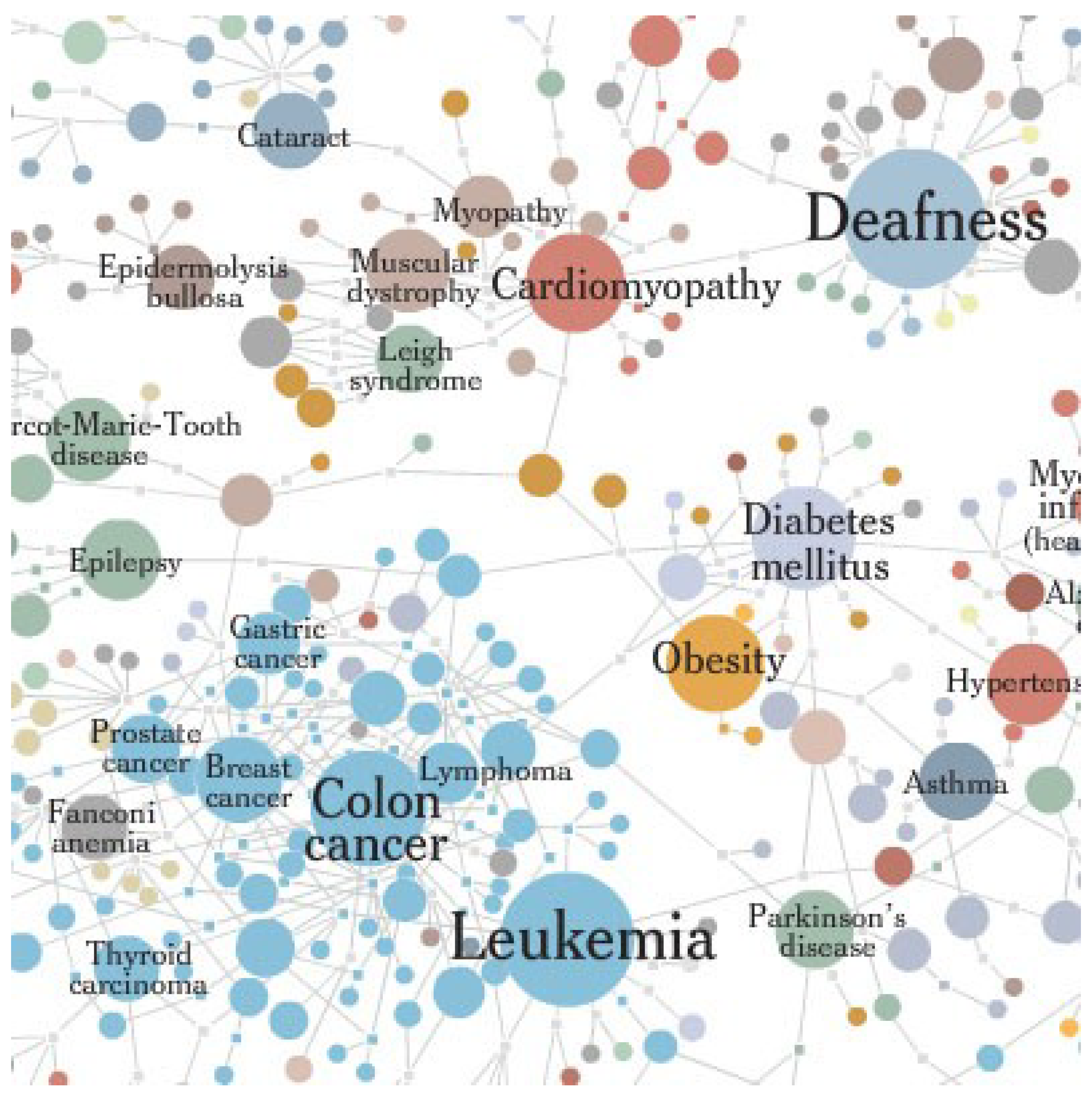
9. Network Medicine: A Holographic Universe

10. Case Presentations
11. Discussion
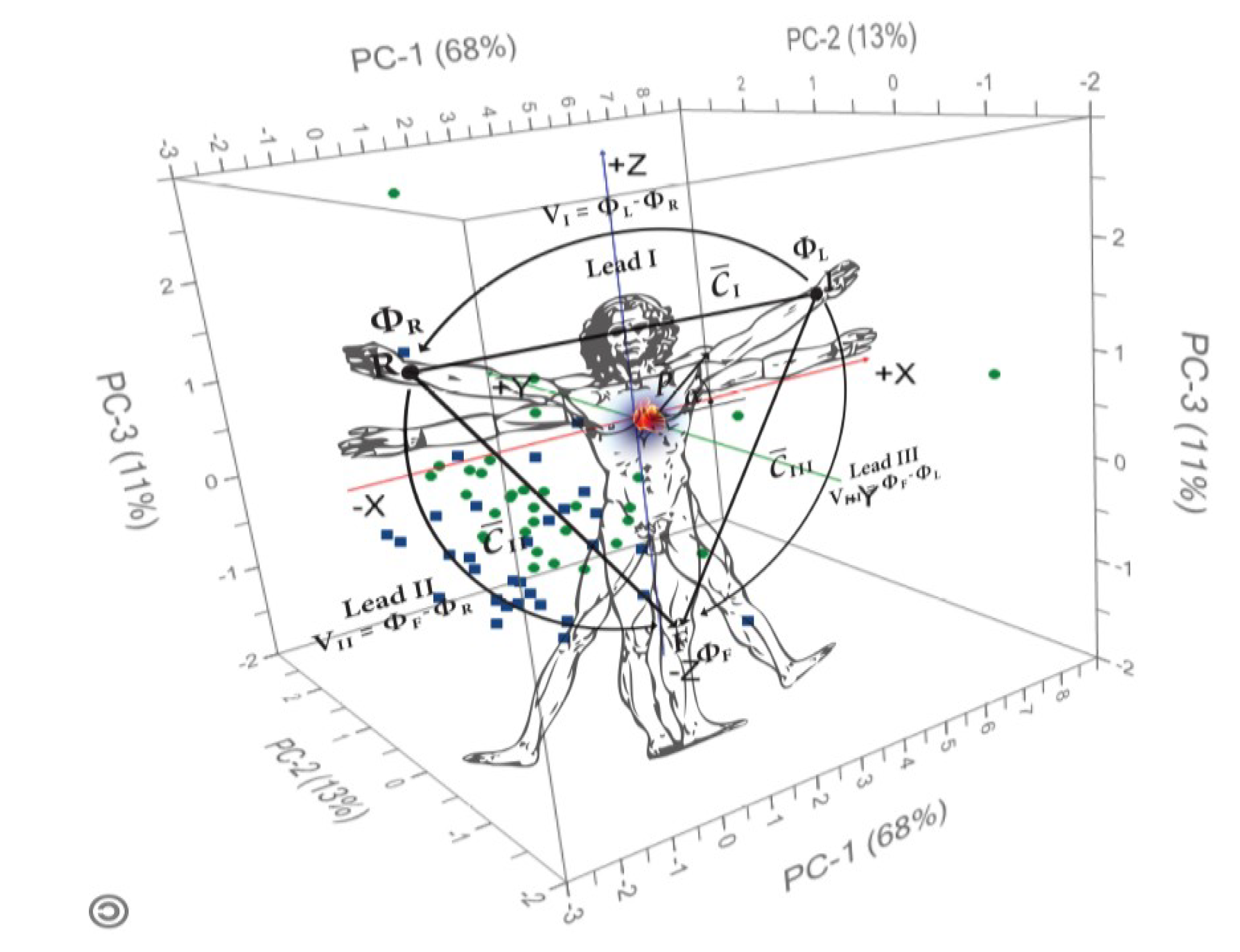
Case 1: Acute Myocardial Infarction
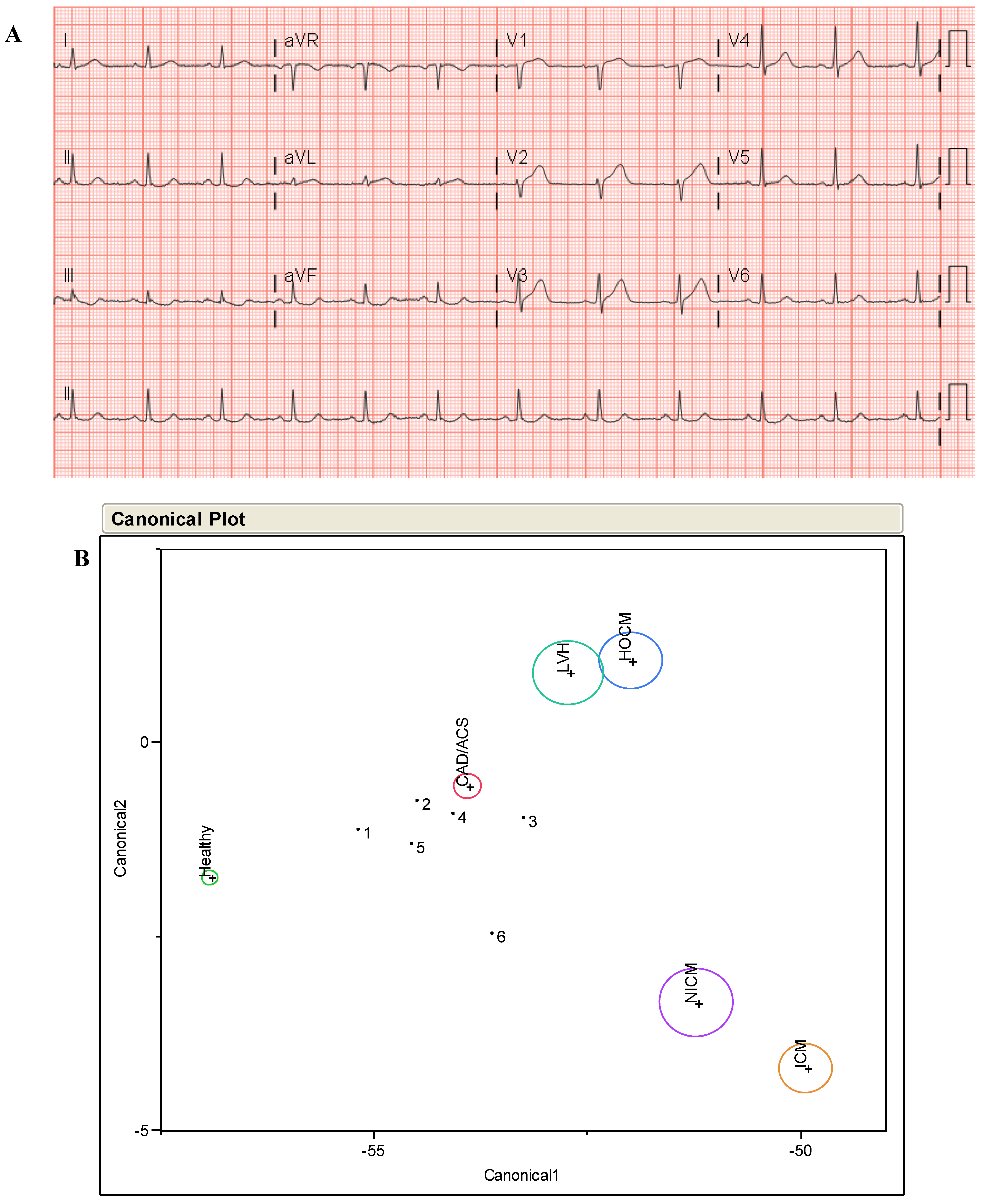
Case 2: Chemotherapy Associated Cardiotoxicity

Case 3: Hereditary Cardiomyopathy
Case 4: Pharmacogenomics and Stent Thrombosis
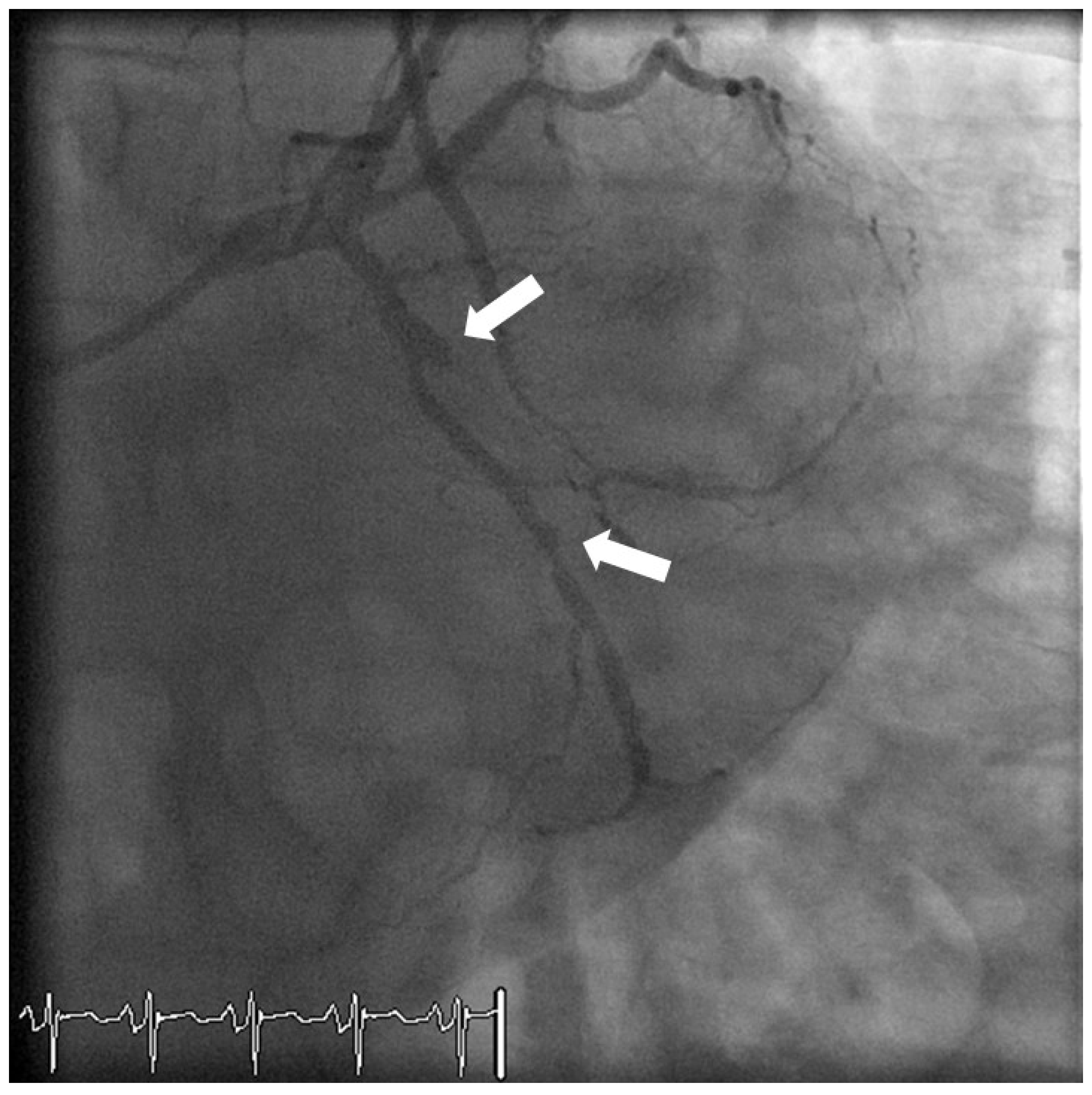
Case 5: Lamin A Associated Cardiomyopathy
Acknowledgments
Conflicts of Interest
References
- Lloyd-Jones, D.; Adams, R.; Carnethon, M.; De Simone, G.; Ferguson, T.B.; Flegal, K.; Ford, E.; Furie, K.; Go, A.; Greenlund, K.; et al. Heart disease and stroke statistics—2009 update. Circulation 2009, 119, 480–486. [Google Scholar] [CrossRef]
- Iglehart, J.K. The new era of medical imaging—Progress and pitfalls. N. Engl. J. Med. 2006, 354, 2822–2828. [Google Scholar] [CrossRef]
- Levin, D.C.; Rao, V.M.; Parker, L.; Frangos, A.J.; Sunshine, J.H. Recent trends in utilization of cardiovascular imaging: How important are they for radiology? J. Am. Coll. Radiol. 2005, 2, 736–739. [Google Scholar] [CrossRef]
- Picano, E. Economic and biological costs of cardiac imaging. Cardiovasc. Ultrasound. 2005, 3, e13. [Google Scholar] [CrossRef] [Green Version]
- Hope, J. Biobazaar: The Open Source Revolution and Biotechnology; Harvard University Press: Cambridge, MA, USA, 2009. [Google Scholar]
- Topol, E.J. The Creative Destruction of Medicine; Basic Books: New York, NY, USA, 2012. [Google Scholar]
- Picano, E.; Lombardi, M.; Neglia, D.; Lazzeri, M. sustainability of medical imaging in cardiology. Recenti Prog. Med. 2006, 97, 652–662. [Google Scholar]
- Picano, E. Sustainability of medical imaging. Br. Med. J. 2004, 328, 578–580. [Google Scholar] [CrossRef]
- Stoylen, A.; Heimdal, A.; Bjornstad, K.; Torp, H.G.; Skjaerpe, T. Strain rate imaging by ultrasound in the diagnosis of regional dysfunction of the left ventricle. Echocardiography 1999, 16, 321–329. [Google Scholar] [CrossRef]
- Cho, J.S.; Kim, K.H.; Lee, W.S.; Yoon, H.J.; Yoon, N.S.; Hong, Y.J.; Park, H.W.; Kim, J.H.; Ahn, Y.; Jeong, M.H.; et al. Usefulness of peak systolic strain measurement by automated function imaging in the prediction of coronary perfusion in patients with acute myocardial infarction. Korean J. Intern. Med. 2010, 25, 260–268. [Google Scholar] [CrossRef]
- Sawaya, H.; Sebag, I.A.; Plana, J.C.; Januzzi, J.L.; Ky, B.; Cohen, V.; Gosavi, S.; Carver, J.R.; Wiegers, S.E.; Martin, R.P.; et al. Early detection and prediction of cardiotoxicity in chemotherapy-treated patients. Am. J. Cardiol. 2011, 107, 1375–1380. [Google Scholar] [CrossRef]
- Sawaya, H.; Sebag, I.A.; Plana, J.C.; Januzzi, J.L.; Ky, B.; Tan, T.C.; Cohen, V.; Banchs, J.; Carver, J.R.; Wiegers, S.E.; et al. Assessment of echocardiography and biomarkers for the extended prediction of cardiotoxicity in patients treated with anthracyclines, taxanes, and trastuzumab. Circ. Cardiovasc. Imaging 2012, 5, 596–603. [Google Scholar] [CrossRef]
- Negishi, K.; Negishi, T.; Hare, J.L.; Haluska, B.A.; Plana, J.C.; Marwick, T.H. Independent and incremental value of deformation indices for prediction of trastuzumab-induced cardiotoxicity. J. Am. Soc. Echocardiogr. 2013, 26, 493–498. [Google Scholar] [CrossRef]
- Geisler, T.; Schaeffeler, E.; Dippon, J.; Winter, S.; Buse, V.; Bischofs, C.; Zuern, C.; Moerike, K.; Gawaz, M.; Schwab, M. CYP2C19 and nongenetic factors predict poor responsiveness to clopidogrel loading dose after coronary stent implantation. Pharmacogenomics 2008, 9, 1251–1259. [Google Scholar] [CrossRef]
- Kaul, S.; Miller, J.G.; Grayburn, P.A.; Hashimoto, S.; Hibberd, M.; Holland, M.R.; Houle, H.C.; Klein, A.L.; Knoll, P.; Lang, R.M.; et al. A suggested roadmap for cardiovascular ultrasound research for the future. J. Am. Soc. Echocardiogr. 2011, 24, 455–464. [Google Scholar] [CrossRef]
- Gladding, P.A.; Anwar, S.; Negishi, K.; Popovic, Z.; Hussan, J.R.; Marwick, T.; Hunter, P.; Kassemi, M.; Levine, B.; Thomas, J. Modeling the heart from echocardiography strain data, collected on the international space station. J. Am. Coll. Cardiol. 2011, 57, E1255. [Google Scholar] [CrossRef]
- Main, M.L.; Foltz, D.; Firstenberg, M.S.; Bobinsky, E.; Bailey, D.; Frantz, B.; Pleva, D.; Baldizzi, M.; Meyers, D.P.; Jones, K.; et al. Real-time transmission of full-motion echocardiography over a high-speed data network: Impact of data rate and network quality of service. J. Am. Soc. Echocardiogr. 2000, 13, 764–770. [Google Scholar] [CrossRef]
- Hamilton, D.R.; Sargsyan, A.E.; Martin, D.S.; Garcia, K.M.; Melton, S.L.; Feiveson, A.; Dulchavsky, S.A. On-orbit prospective echocardiography on international space station crew. Echocardiography 2011, 28, 491–501. [Google Scholar] [CrossRef]
- Martin, D.; Borowski, A.; Bungo, M.W.; Dulchavsky, S.; Gladding, P.; Greenberg, N.; Hamilton, D.; Levine, B.D.; Norwoord, K.; Platts, S.H.; et al. Extreme Tele-Echocardiography: Methodology for Remote Guidance of In-Flight Echocardiography Aboard the International Space Station. In Proceedings of American Society of Echocardiography (ASE) 23rd Annual Scientific Sessions, National Harbor, MD, USA, 30 June–3 July 2012.
- Negishi, K.; Anwar, S.; Popovic, Z.B.; Borowski, A.; Martin, D.S.; Bungo, M.F.; Levine, B.D.; Thomas, J.D. Impact of Spaceflight on Myocardial Strain: An Interim Analysis from The Integrated Cardiovascular Study; NASA Human Research Program Investigators’ Workshop: Houston, TX, USA, 2012. [Google Scholar]
- Singh, S.; Bansal, M.; Maheshwari, P.; Adams, D.; Sengupta, S.P.; Price, R.; Dantin, L.; Smith, M.; Kasliwal, R.R.; Pellikka, P.A.; et al. American society of echocardiography: Remote echocardiography with web-based assessments for referrals at a distance (ase-reward) study. J. Am. Soc. Echocardiogr. 2013, 26, 221–233. [Google Scholar] [CrossRef]
- Hunter, P.; Robbins, P.; Noble, D. The iups human physiome project. Pflugers Arch. 2002, 445, 1–9. [Google Scholar] [CrossRef]
- Anwar, S.; Gladding, P.; Negishi, K.; Popovic, Z.; Thomas, J. Comparison of longitudinal strain by speckle tracking of polar vs dicom images. Heart Lung Circ. 2011, 20, 385. [Google Scholar]
- Sox, H.C., Jr.; Garber, A.M.; Littenberg, B. The resting electrocardiogram as a screening test. A clinical analysis. Ann. Intern. Med. 1989, 111, 489–502. [Google Scholar] [CrossRef]
- Ashley, E.A.; Raxwal, V.; Froelicher, V. An evidence-based review of the resting electrocardiogram as a screening technique for heart disease. Prog. Cardiovasc. Dis. 2001, 44, 55–67. [Google Scholar] [CrossRef]
- Levy, D.; Labib, S.B.; Anderson, K.M.; Christiansen, J.C.; Kannel, W.B.; Castelli, W.P. Determinants of sensitivity and specificity of electrocardiographic criteria for left ventricular hypertrophy. Circulation 1990, 81, 815–820. [Google Scholar] [CrossRef]
- Davie, A.P.; Francis, C.M.; Love, M.P.; Caruana, L.; Starkey, I.R.; Shaw, T.R.; Sutherland, G.R.; McMurray, J.J. Value of the electrocardiogram in identifying heart failure due to left ventricular systolic dysfunction. Br. Med. J. 1996, 312. [CrossRef]
- Hedberg, P.; Lonnberg, I.; Jonason, T.; Nilsson, G.; Pehrsson, K.; Ringqvist, I. Electrocardiogram and B-type natriuretic peptide as screening tools for left ventricular systolic dysfunction in a population-based sample of 75-year-old men and women. Am. Heart J. 2004, 148, 524–529. [Google Scholar] [CrossRef]
- Schlegel, T.T.; Kulecz, W.B.; Feiveson, A.H.; Greco, E.C.; DePalma, J.L.; Starc, V.; Vrtovec, B.; Rahman, M.A.; Bungo, M.W.; Hayat, M.J.; et al. Accuracy of advanced versus strictly conventional 12-lead ecg for detection and screening of coronary artery disease, left ventricular hypertrophy and left ventricular systolic dysfunction. BMC Cardiovasc. Disord. 2010, 10, e28. [Google Scholar] [CrossRef]
- Jain, A.K.; Duin, R.P.W.; Mao, J. Statistical pattern recognition: A review. IEEE Trans. Pattern Anal. Mach. Intell. 2000, 22, 4–37. [Google Scholar] [CrossRef]
- Poplack Potter, S.L.; Holmqvist, F.; Platonov, P.G.; Steding, K.; Arheden, H.; Pahlm, O.; Starc, V.; McKenna, W.J.; Schlegel, T.T. Detection of hypertrophic cardiomyopathy is improved when using advanced rather than strictly conventional 12-lead electrocardiogram. J. Electrocardiol. 2010, 43, 713–718. [Google Scholar] [CrossRef]
- Garrod, A.E. The lancet. The incidence of alkaptonuria: A study in chemical individuality. Nutr. Rev. 1975, 33, 81–83. [Google Scholar] [CrossRef]
- Sabatine, M.S.; Morrow, D.A.; de Lemos, J.A.; Jarolim, P.; Braunwald, E. Detection of acute changes in circulating troponin in the setting of transient stress test-induced myocardial ischaemia using an ultrasensitive assay: Results from TIMI 35. Eur. Heart J. 2009, 30, 162–169. [Google Scholar]
- Wilson, S.R.; Sabatine, M.S.; Braunwald, E.; Sloan, S.; Murphy, S.A.; Morrow, D.A. Detection of myocardial injury in patients with unstable angina using a novel nanoparticle cardiac troponin I assay: Observations from the PROTECT-TIMI 30 Trial. Am. Heart J. 2009, 158, 386–391. [Google Scholar] [CrossRef]
- Djulbegovic, M.; Beyth, R.J.; Neuberger, M.M.; Stoffs, T.L.; Vieweg, J.; Djulbegovic, B.; Dahm, P. Screening for prostate cancer: Systematic review and meta-analysis of randomized controlled trials. Br. Med. J. 2010, 341, c4543. [Google Scholar]
- Reichlin, T.; Hochholzer, W.; Bassetti, S.; Steuer, S.; Stelzig, C.; Hartwiger, S.; Biedert, S.; Schaub, N.; Buerge, C.; Potocki, M.; et al. Early diagnosis of myocardial infarction with sensitive cardiac troponin assays. N. Engl. J. Med. 2009, 361, 858–867. [Google Scholar] [CrossRef]
- Rosjo, H.; Varpula, M.; Hagve, T.A.; Karlsson, S.; Ruokonen, E.; Pettila, V.; Omland, T.; Group, F.S. Circulating high sensitivity troponin t in severe sepsis and septic shock: Distribution, associated factors, and relation to outcome. Intens. Care Med. 2011, 37, 77–85. [Google Scholar] [CrossRef]
- Lewis, G.D.; Wei, R.; Liu, E.; Yang, E.; Shi, X.; Martinovic, M.; Farrell, L.; Asnani, A.; Cyrille, M.; Ramanathan, A.; et al. Metabolite profiling of blood from individuals undergoing planned myocardial infarction reveals early markers of myocardial injury. J. Clin. Investig. 2008, 118, 3503–3512. [Google Scholar] [CrossRef]
- Teul, J.; Garcia, A.; Tunon, J.; Martin-Ventura, J.L.; Tarin, N.; Bescos, L.L.; Egido, J.; Barbas, C.; Ruperez, F.J. Targeted and non-targeted metabolic time trajectory in plasma of patients after acute coronary syndrome. J. Pharmaceut. Biomed. Anal. 2011, 56, 343–351. [Google Scholar] [CrossRef]
- Bodi, V.; Sanchis, J.; Morales, J.M.; Marrachelli, V.G.; Nunez, J.; Forteza, M.J.; Chaustre, F.; Gomez, C.; Mainar, L.; Minana, G.; et al. Metabolomic profile of human myocardial ischemia by nuclear magnetic resonance spectroscopy of peripheral blood serum: A translational study based on transient coronary occlusion models. J. Am. Coll. Cardiol. 2012, 59, 1629–1641. [Google Scholar] [CrossRef]
- Addona, T.A.; Shi, X.; Keshishian, H.; Mani, D.R.; Burgess, M.; Gillette, M.A.; Clauser, K.R.; Shen, D.; Lewis, G.D.; Farrell, L.A.; et al. A pipeline that integrates the discovery and verification of plasma protein biomarkers reveals candidate markers for cardiovascular disease. Nat. Biotechnol. 2011, 29, 635–643. [Google Scholar] [CrossRef]
- Sabatine, M.S.; Liu, E.; Morrow, D.A.; Heller, E.; McCarroll, R.; Wiegand, R.; Berriz, G.F.; Roth, F.P.; Gerszten, R.E. Metabolomic identification of novel biomarkers of myocardial ischemia. Circulation 2005, 112, 3868–3875. [Google Scholar] [CrossRef]
- Carbonnelle, E.; Mesquita, C.; Bille, E.; Day, N.; Dauphin, B.; Beretti, J.L.; Ferroni, A.; Gutmann, L.; Nassif, X. Maldi-tof mass spectrometry tools for bacterial identification in clinical microbiology laboratory. Clin. Biochem. 2011, 44, 104–109. [Google Scholar] [CrossRef]
- Brennan, M.L.; Reddy, A.; Tang, W.H.; Wu, Y.; Brennan, D.M.; Hsu, A.; Mann, S.A.; Hammer, P.L.; Hazen, S.L. Comprehensive peroxidase-based hematologic profiling for the prediction of 1-year myocardial infarction and death. Circulation 2010, 122, 70–79. [Google Scholar] [CrossRef]
- Tonelli, M.; Sacks, F.; Arnold, M.; Moye, L.; Davis, B.; Pfeffer, M.; Cholesterol, F.T.; Investigators, R.E.T. Relation between red blood cell distribution width and cardiovascular event rate in people with coronary disease. Circulation 2008, 117, 163–168. [Google Scholar] [CrossRef]
- Loscalzo, J.; Kohane, I.; Barabasi, A.L. Human disease classification in the postgenomic era: A complex systems approach to human pathobiology. Mol. Syst. Biol. 2007, 3, e124. [Google Scholar]
- Research, M. Epistasis gwas for 7 common diseases. Available online: http://datamarket.azure.com/dataset/microsoftresearch/epistasisgwas (accessed on 11 July 2013).
- Johnson, M.W.; Amin, M.H.; Gildert, S.; Lanting, T.; Hamze, F.; Dickson, N.; Harris, R.; Berkley, A.J.; Johansson, J.; Bunyk, P.; et al. Quantum annealing with manufactured spins. Nature 2011, 473, 194–198. [Google Scholar] [CrossRef]
- Sengupta, P.P.; Marwick, T.H.; Narula, J. Adding dimensions to unimodal cardiac images. JACC Cardiovasc. Imag. 2011, 4, 816–818. [Google Scholar] [CrossRef]
- Scott, S.A.; Sangkuhl, K.; Stein, C.M.; Hulot, J.S.; Mega, J.L.; Roden, D.M.; Klein, T.E.; Sabatine, M.S.; Johnson, J.A.; Shuldiner, A.R. Clinical pharmacogenetics implementation consortium (cpic) guidelines for cytochrome p450-2c19 (cyp2c19) genotype and clopidogrel therapy: 2013 update. Clin. Pharmacol. Ther. 2013. [Google Scholar] [CrossRef]
- Link, E.; Parish, S.; Armitage, J.; Bowman, L.; Heath, S.; Matsuda, F.; Gut, I.; Lathrop, M.; Collins, R. Slco1b1 variants and statin-induced myopathy—A genomewide study. N. Engl. J. Med. 2008, 359, 789–799. [Google Scholar] [CrossRef]
- Pare, G.; Eriksson, N.; Lehr, T.; Connolly, S.; Eikelboom, J.; Ezekowitz, M.D.; Axelsson, T.; Haertter, S.; Oldgren, J.; Reilly, P.; et al. Genetic determinants of dabigatran plasma levels and their relation to bleeding. Circulation 2013, 127, 1404–1412. [Google Scholar] [CrossRef]
- Johnson, J.A.; Gong, L.; Whirl-Carrillo, M.; Gage, B.F.; Scott, S.A.; Stein, C.M.; Anderson, J.L.; Kimmel, S.E.; Lee, M.T.; Pirmohamed, M.; et al. Clinical Pharmacogenetics Implementation Consortium Guidelines for CYP2C9 and VKORC1 genotypes and warfarin dosing. Int. J. Clin. Pharmacol. Ther. 2011, 90, 625–629. [Google Scholar] [CrossRef]
- Ellinor, P.T.; Lunetta, K.L.; Albert, C.M.; Glazer, N.L.; Ritchie, M.D.; Smith, A.V.; Arking, D.E.; Muller-Nurasyid, M.; Krijthe, B.P.; Lubitz, S.A.; et al. Meta-analysis identifies six new susceptibility loci for atrial fibrillation. Nat. Genet. 2012, 44, 670–675. [Google Scholar]
- Lubitz, S.A.; Sinner, M.F.; Lunetta, K.L.; Makino, S.; Pfeufer, A.; Rahman, R.; Veltman, C.E.; Barnard, J.; Bis, J.C.; Danik, S.P.; et al. Independent susceptibility markers for atrial fibrillation on chromosome 4q25. Circulation 2010, 122, 976–984. [Google Scholar] [CrossRef] [Green Version]
- Parvez, B.; Shah, A.; Muhammad, R.; Shoemaker, M.; Graves, A.J.; Heckbert, S.R.; Xu, H.; Ellinor, P.T.; Benjamin, E.J.; Alonso, A.; et al. Replication of a risk prediction model for ambulatory incident atrial fibrillation using electronic medical record. Circulation 2012, 126, A18578. [Google Scholar]
- Parvez, B.; Vaglio, J.; Rowan, S.; Muhammad, R.; Kucera, G.; Stubblefield, T.; Carter, S.; Roden, D.; Darbar, D. Symptomatic response to antiarrhythmic drug therapy is modulated by a common single nucleotide polymorphism in atrial fibrillation. J. Am. Coll. Cardiol. 2012, 60, 539–545. [Google Scholar] [CrossRef]
- Benjamin Shoemaker, M.; Muhammad, R.; Parvez, B.; White, B.W.; Streur, M.; Song, Y.; Stubblefield, T.; Kucera, G.; Blair, M.; Rytlewski, J.; et al. Common atrial fibrillation risk alleles at 4q25 predict recurrence after catheter-based atrial fibrillation ablation. Heart Rhythm 2013, 10, 394–400. [Google Scholar] [CrossRef]
- Husser, D.; Adams, V.; Piorkowski, C.; Hindricks, G.; Bollmann, A. Chromosome 4q25 variants and atrial fibrillation recurrence after catheter ablation. J. Am. Coll. Cardiol. 2010, 55, 747–753. [Google Scholar]
- Parvez, B.; Benjamin Shoemaker, M.; Muhammad, R.; Richardson, R.; Jiang, L.; Blair, M.A.; Roden, D.M.; Darbar, D. Common genetic polymorphism at 4q25 locus predicts atrial fibrillation recurrence after successful cardioversion. Heart Rhythm 2013, 10, 849–855. [Google Scholar] [CrossRef]
- Qiu, F.; Gu, K.; Yang, B.; Ding, Y.; Jiang, D.; Wu, Y.; Huang, L.L. DNA assay based on monolayer-barcoded nanoparticles for mass spectrometry in combination with magnetic microprobes. Talanta 2011, 85, 1698–1702. [Google Scholar] [CrossRef]
- Taira, S.; Osaka, I.; Shimma, S.; Kaneko, D.; Hiroki, T.; Kawamura-Konishi, Y.; Ichiyanagi, Y. Oligonucleotide analysis by nanoparticle-assisted laser desorption/ionization mass spectrometry. Analyst 2012, 137, 2006–2010. [Google Scholar] [CrossRef]
- Smith, A.D.; Cowan, J.O.; Brassett, K.P.; Herbison, G.P.; Taylor, D.R. Use of exhaled nitric oxide measurements to guide treatment in chronic asthma. N. Engl. J. Med. 2005, 352, 2163–2173. [Google Scholar] [CrossRef]
- Rhodes, J.M.; Middleton, P.; Jewell, D.P. The lactulose hydrogen breath test as a diagnostic test for small-bowel bacterial overgrowth. Scand. J. Gastroenterol. 1979, 14, 333–336. [Google Scholar] [CrossRef]
- Cikach, F.S., Jr.; Dweik, R.A. Cardiovascular biomarkers in exhaled breath. Prog. Cardiovasc. Dis. 2012, 55, 34–43. [Google Scholar] [CrossRef]
- Martinez-Lozano Sinues, P.; Kohler, M.; Zenobi, R. Human breath analysis may support the existence of individual metabolic phenotypes. PLoS One 2013, 8, e59909. [Google Scholar] [CrossRef]
- Samara, M.A.; Tang, W.H.; Cikach, F., Jr.; Gul, Z.; Tranchito, L.; Paschke, K.M.; Viterna, J.; Wu, Y.; Laskowski, D.; Dweik, R.A. Single exhaled breath metabolomic analysis identifies unique breathprint in patients with acute decompensated heart failure. J. Am. Coll. Cardiol. 2013, 61, 1463–1464. [Google Scholar] [CrossRef]
- Phillips, M.; Cataneo, R.N.; Greenberg, J.; Grodman, R.; Salazar, M. Breath markers of oxidative stress in patients with unstable angina. Heart Dis. 2003, 5, 95–99. [Google Scholar] [CrossRef]
- Bhasin, M.K.; Dusek, J.A.; Chang, B.H.; Joseph, M.G.; Denninger, J.W.; Fricchione, G.L.; Benson, H.; Libermann, T.A. Relaxation response induces temporal transcriptome changes in energy metabolism, insulin secretion and inflammatory pathways. PLoS One 2013, 8, e62817. [Google Scholar]
- Miekisch, W.; Schubert, J.K.; Noeldge-Schomburg, G.F. Diagnostic potential of breath analysis—Focus on volatile organic compounds. Clin. Chim. Acta 2004, 347, 25–39. [Google Scholar] [CrossRef]
- Shevade, A.V.; Homer, M.L.; Kisor, A.K.; Yen, S.-P.S.; Lara, L.M.; Zhou, H.; Manatt, K.S.; Gluck, S.; Ryan, M.A. The Technology Demonstration of the Third Generation Jpl Electronic Nose on the International Space Station. In Human Olfactory Displays and Interfaces: Odor Sensing and Presentation; IGI Global: Hershey, PA, USA, 2013; pp. 275–295. [Google Scholar]
- Ryan, M.A.; Hanying, Z.; Buehler, M.G.; Manatt, K.S.; Mowrey, V.S.; Jackson, S.P.; Kisor, A.K.; Shevade, A.V.; Homer, M.L. Monitoring space shuttle air quality using the jet propulsion laboratory electronic nose. Sens. J. IEEE 2004, 4, 337–347. [Google Scholar]
- Zhou, H.; Homer, M.; Shevade, A.; Ryan, M. Nonlinear least-squares based method for identifying and quantifying single and mixed contaminants in air with an electronic nose. Sensors 2005, 6, 1–18. [Google Scholar] [CrossRef]
- Kateb, B.; Ryan, M.A.; Homer, M.L.; Lara, L.M.; Yin, Y.; Higa, K.; Chen, M.Y. Sniffing out cancer using the JPL electronic nose: A pilot study of a novel approach to detection and differentiation of brain cancer. NeuroImage 2009, 47, T5–T9. [Google Scholar]
- Gardy, J.L.; Johnston, J.C.; Sui, S.J.H.; Cook, V.J.; Shah, L.; Brodkin, E.; Rempel, S.; Moore, R.; Zhao, Y.; Holt, R.; et al. Whole-genome sequencing and social-network analysis of a tuberculosis outbreak. N. Engl. J. Med. 2011, 364, 730–739. [Google Scholar] [CrossRef]
- Loscalzo, J. Personalized cardiovascular medicine and drug development: Time for a new paradigm. Circulation 2012, 125, 638–645. [Google Scholar] [CrossRef]
- Christakis, N.A.; Fowler, J.H. The spread of obesity in a large social network over 32 years. N. Engl. J. Med. 2007, 357, 370–379. [Google Scholar] [CrossRef]
- Christakis, N.A.; Fowler, J.H. The collective dynamics of smoking in a large social network. N. Engl. J. Med. 2008, 358, 2249–2258. [Google Scholar] [CrossRef]
- Lin, D.; Hollander, Z.; Meredith, A.; Stadnick, E.; Sasaki, M.; Cohen Freue, G.; Qasimi, P.; Mui, A.; Ng, R.T.; Balshaw, R.; et al. Molecular signatures of end-stage heart failure. J. Card. Fail. 2011, 17, 867–874. [Google Scholar] [CrossRef]
- Sinnaeve, P.R.; Donahue, M.P.; Grass, P.; Seo, D.; Vonderscher, J.; Chibout, S.D.; Kraus, W.E.; Sketch, M., Jr.; Nelson, C.; Ginsburg, G.S.; et al. Gene expression patterns in peripheral blood correlate with the extent of coronary artery disease. PLoS One 2009, 4, e7037. [Google Scholar] [CrossRef]
- Rosenberg, S.; Elashoff, M.R.; Beineke, P.; Daniels, S.E.; Wingrove, J.A.; Tingley, W.G.; Sager, P.T.; Sehnert, A.J.; Yau, M.; Kraus, W.E.; et al. Multicenter validation of the diagnostic accuracy of a blood-based gene expression test for assessing obstructive coronary artery disease in nondiabetic patients. Ann. Intern. Med. 2010, 153, 425–434. [Google Scholar] [CrossRef]
- Pham, M.X.; Teuteberg, J.J.; Kfoury, A.G.; Starling, R.C.; Deng, M.C.; Cappola, T.P.; Kao, A.; Anderson, A.S.; Cotts, W.G.; Ewald, G.A.; et al. Gene-expression profiling for rejection surveillance after cardiac transplantation. N. Engl. J. Med. 2010, 362, 1890–1900. [Google Scholar] [CrossRef]
- Dudley, J.T.; Sirota, M.; Shenoy, M.; Pai, R.K.; Roedder, S.; Chiang, A.P.; Morgan, A.A.; Sarwal, M.M.; Pasricha, P.J.; Butte, A.J. Computational repositioning of the anticonvulsant topiramate for inflammatory bowel disease. Sci. Transl. Med. 2011, 3, 96ra76. [Google Scholar] [CrossRef]
- Lussier, Y.A.; Chen, J.L. The emergence of genome-based drug repositioning. Sci. Transl. Med. 2011, 3, 96ps35. [Google Scholar] [CrossRef]
- Ramsey, B.W.; Davies, J.; McElvaney, N.G.; Tullis, E.; Bell, S.C.; Dřevínek, P.; Griese, M.; McKone, E.F.; Wainwright, C.E.; Konstan, M.W.; et al. A CFTR potentiator in patients with cystic fibrosis and the G551D mutation. N. Engl. J. Med. 2011, 365, 1663–1672. [Google Scholar] [CrossRef] [Green Version]
- Dormuth, C.R.; Hemmelgarn, B.R.; Paterson, J.M.; James, M.T.; Teare, G.F.; Raymond, C.B.; Lafrance, J.P.; Levy, A.; Garg, A.X.; Ernst, P.; et al. Use of high potency statins and rates of admission for acute kidney injury: Multicenter, retrospective observational analysis of administrative databases. Br. Med. J. 2013, 346, f880. [Google Scholar] [CrossRef]
- Preiss, D.; Seshasai, S.R.; Welsh, P.; Murphy, S.A.; Ho, J.E.; Waters, D.D.; DeMicco, D.A.; Barter, P.; Cannon, C.P.; Sabatine, M.S.; et al. Risk of incident diabetes with intensive-dose compared with moderate-dose statin therapy: A meta-analysis. JAMA 2011, 305, 2556–2564. [Google Scholar] [CrossRef]
- Erogbogbo, F.; May, J.; Swihart, M.; Prasad, P.N.; Smart, K.; El-Jack, S.; Korcyk, D.; Webster, M.; Stewart, R.; Zeng, I.; et al. Bioengineering Silicon Quantum Dot Theranostics using a Network Analysis of Metabolomic and Proteomic Data in Cardiac Ischemia. Theranostics 2013, in press. [Google Scholar]
- Winter, P.M.; Caruthers, S.D.; Zhang, H.; Williams, T.A.; Wickline, S.A.; Lanza, G.M. Antiangiogenic synergism of integrin-targeted fumagillin nanoparticles and atorvastatin in atherosclerosis. J. Am. Coll. Cardiol. Img. 2008, 1, 624–634. [Google Scholar] [CrossRef]
- Lillie, E.O.; Patay, B.; Diamant, J.; Issell, B.; Topol, E.J.; Schork, N.J. The n-of-1 clinical trial: The ultimate strategy for individualizing medicine? Pers. Med. 2011, 8, 161–173. [Google Scholar] [CrossRef]
- Jani, I.V.; Peter, T.F. How point-of-care testing could drive innovation in global health. N. Engl. J. Med. 2013, 368, 2319–2324. [Google Scholar] [CrossRef]
- Weidenbach, M.; Wick, C.; Pieper, S.; Quast, K.J.; Fox, T.; Grunst, G.; Redel, D.A. Augmented reality simulator for training in two-dimensional echocardiography. Comput. Biomed. Res. 2000, 33, 11–22. [Google Scholar] [CrossRef]
- Cornetta, K.; Brown, C.G. Balancing personalized medicine and personalized care. Acad. Med. 2013, 88, 309–313. [Google Scholar] [CrossRef]
- Joshi, K.; Ghodke, Y.; Shintre, P. Traditional medicine and genomics. J. Ayurveda Integr. Med. 2010, 1, 26–32. [Google Scholar] [CrossRef]
- Koeth, R.A.; Wang, Z.; Levison, B.S.; Buffa, J.A.; Org, E.; Sheehy, B.T.; Britt, E.B.; Fu, X.; Wu, Y.; Li, L.; et al. Intestinal microbiota metabolism of l-carnitine, a nutrient in red meat, promotes atherosclerosis. Nat. Med. 2013. [Google Scholar] [CrossRef]
- de Chardin, P.T. The Phenomenon of Man; Harper & Row: New York, NY, USA, 1965. [Google Scholar]
- Members, W.C.; Antman, E.M.; Anbe, D.T.; Armstrong, P.W.; Bates, E.R.; Green, L.A.; Hand, M.; Hochman, J.S.; Krumholz, H.M.; Kushner, F.G.; et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction—Executive summary. Circulation 2004, 110, 588–636. [Google Scholar] [CrossRef]
- Steg, P.G.; James, S.K.; Atar, D.; Badano, L.P.; Lundqvist, C.B.; Borger, M.A.; Di Mario, C.; Dickstein, K.; Ducrocq, G.; Fernandez-Aviles, F.; et al. ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur. Heart J. 2012, 33, 2569–2619. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; White, H.D.; Jaffe, A.S.; Apple, F.S.; Galvani, M.; Katus, H.A.; Newby, L.K.; Ravkilde, J.; Chaitman, B.; et al. Universal definition of myocardial infarction. Eur. Heart J. 2007, 28, 2525–2538. [Google Scholar] [CrossRef]
- Herman, D.S.; Lam, L.; Taylor, M.R.; Wang, L.; Teekakirikul, P.; Christodoulou, D.; Conner, L.; DePalma, S.R.; McDonough, B.; Sparks, E.; et al. Truncations of titin causing dilated cardiomyopathy. N. Engl. J. Med. 2012, 366, 619–628. [Google Scholar] [CrossRef]
- Mitsuhashi, H.; Hayashi, Y.K.; Matsuda, C.; Noguchi, S.; Wakatsuki, S.; Araki, T.; Nishino, I. Specific phosphorylation of ser458 of a-type lamins in lmna-associated myopathy patients. J. Cell Sci. 2010, 123, 3893–3900. [Google Scholar] [CrossRef]
- Zhavoronkov, A.; Smit-McBride, Z.; Guinan, K.J.; Litovchenko, M.; Moskalev, A. Potential therapeutic approaches for modulating expression and accumulation of defective lamin a in laminopathies and age-related diseases. J. Mol. Med. 2012, 90, 1361–1389. [Google Scholar] [CrossRef]
- Liu, G.H.; Suzuki, K.; Qu, J.; Sancho-Martinez, I.; Yi, F.; Li, M.; Kumar, S.; Nivet, E.; Kim, J.; Soligalla, R.D.; et al. Targeted gene correction of laminopathy-associated lmna mutations in patient-specific ipscs. Cell Stem Cell 2011, 8, 688–694. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Gladding, P.A.; Cave, A.; Zareian, M.; Smith, K.; Hussan, J.; Hunter, P.; Erogbogbo, F.; Aguilar, Z.; Martin, D.S.; Chan, E.; et al. Open Access Integrated Therapeutic and Diagnostic Platforms for Personalized Cardiovascular Medicine. J. Pers. Med. 2013, 3, 203-237. https://doi.org/10.3390/jpm3030203
Gladding PA, Cave A, Zareian M, Smith K, Hussan J, Hunter P, Erogbogbo F, Aguilar Z, Martin DS, Chan E, et al. Open Access Integrated Therapeutic and Diagnostic Platforms for Personalized Cardiovascular Medicine. Journal of Personalized Medicine. 2013; 3(3):203-237. https://doi.org/10.3390/jpm3030203
Chicago/Turabian StyleGladding, Patrick A., Andrew Cave, Mehran Zareian, Kevin Smith, Jagir Hussan, Peter Hunter, Folarin Erogbogbo, Zoraida Aguilar, David S. Martin, Eugene Chan, and et al. 2013. "Open Access Integrated Therapeutic and Diagnostic Platforms for Personalized Cardiovascular Medicine" Journal of Personalized Medicine 3, no. 3: 203-237. https://doi.org/10.3390/jpm3030203



