Estimating the Influence of Housing Energy Efficiency and Overheating Adaptations on Heat-Related Mortality in the West Midlands, UK
Abstract
1. Introduction
2. Methods
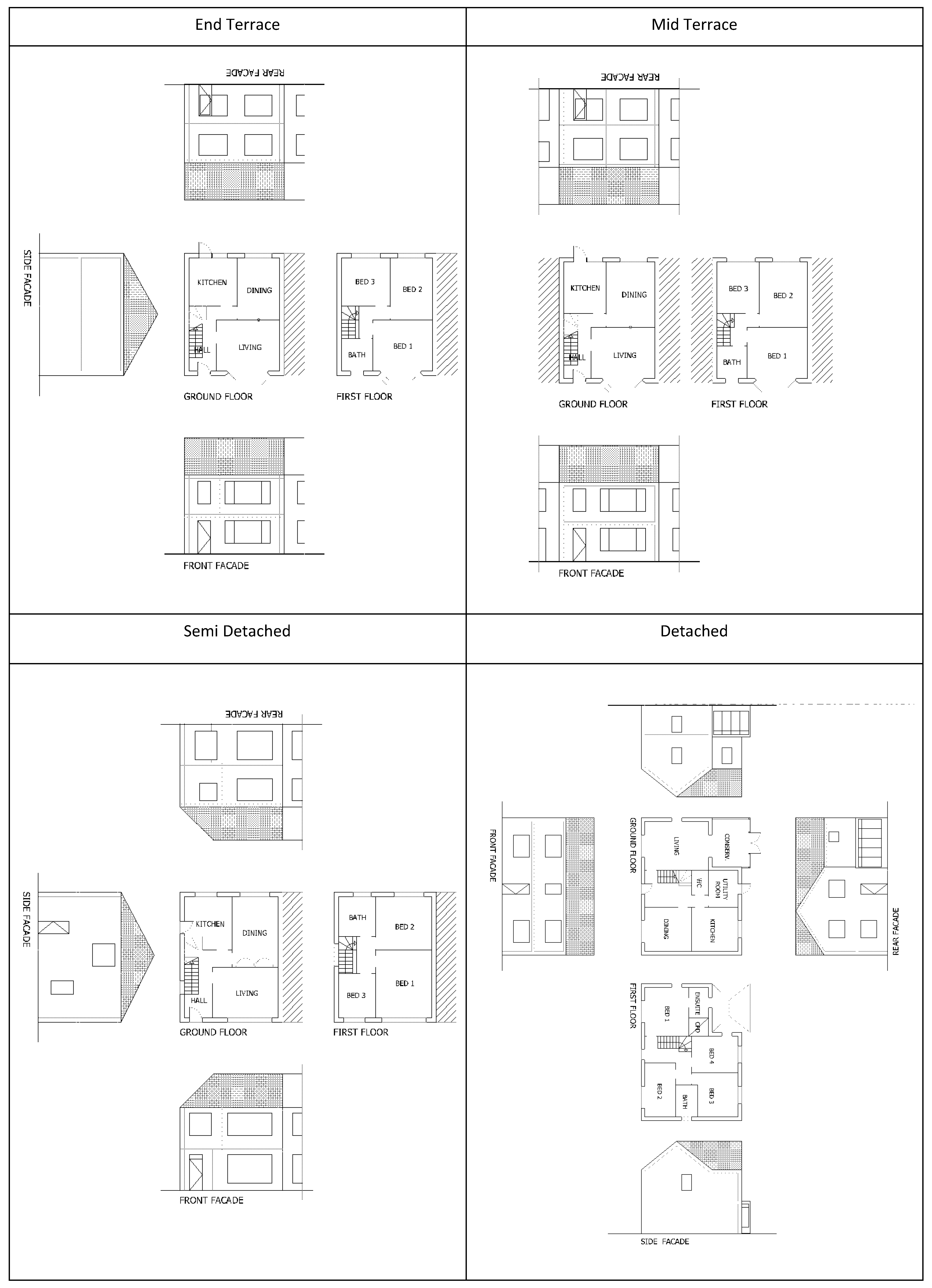
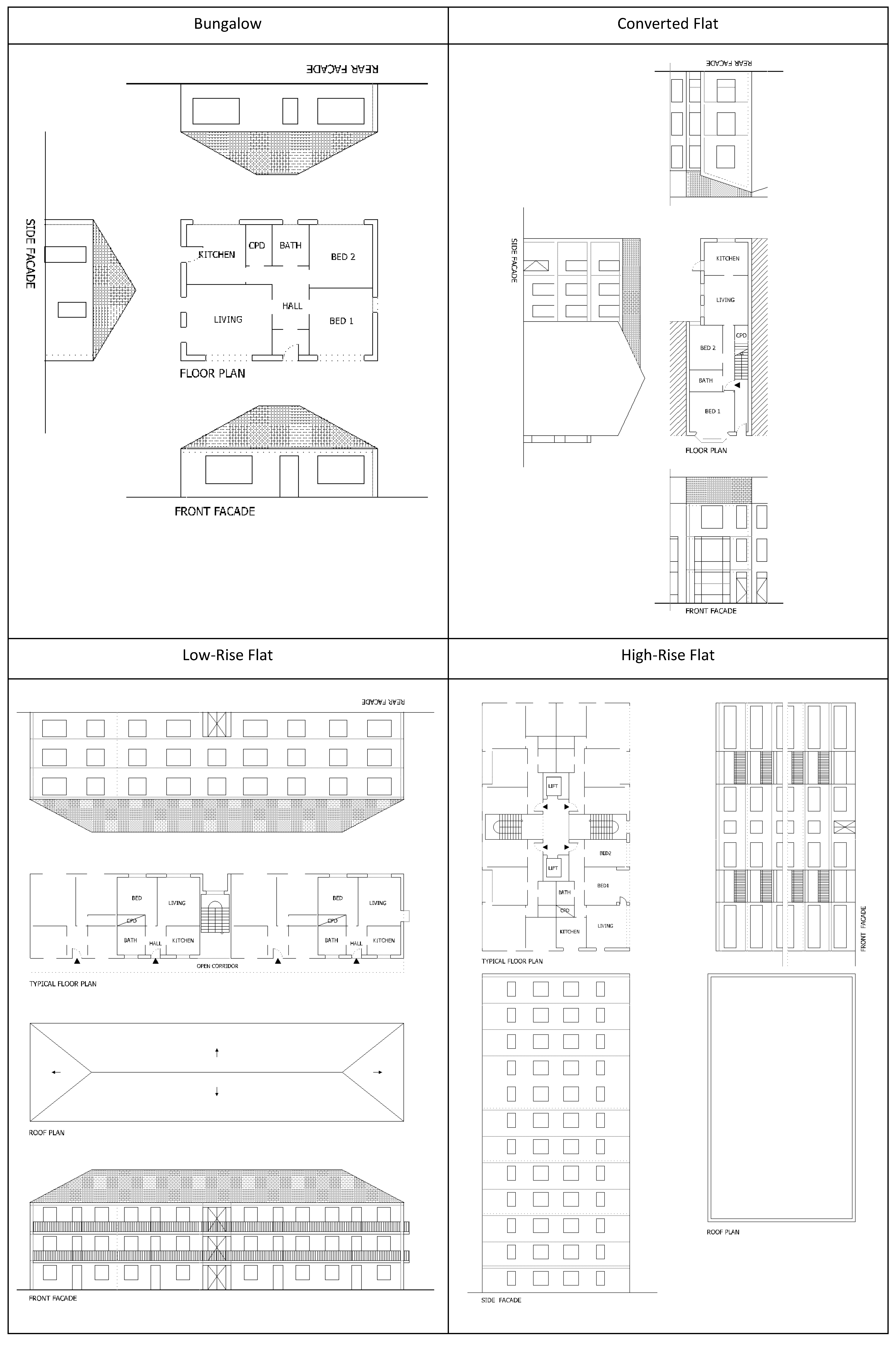
2.1. Building Modelling
2.2. Mortality Calculations
3. Results
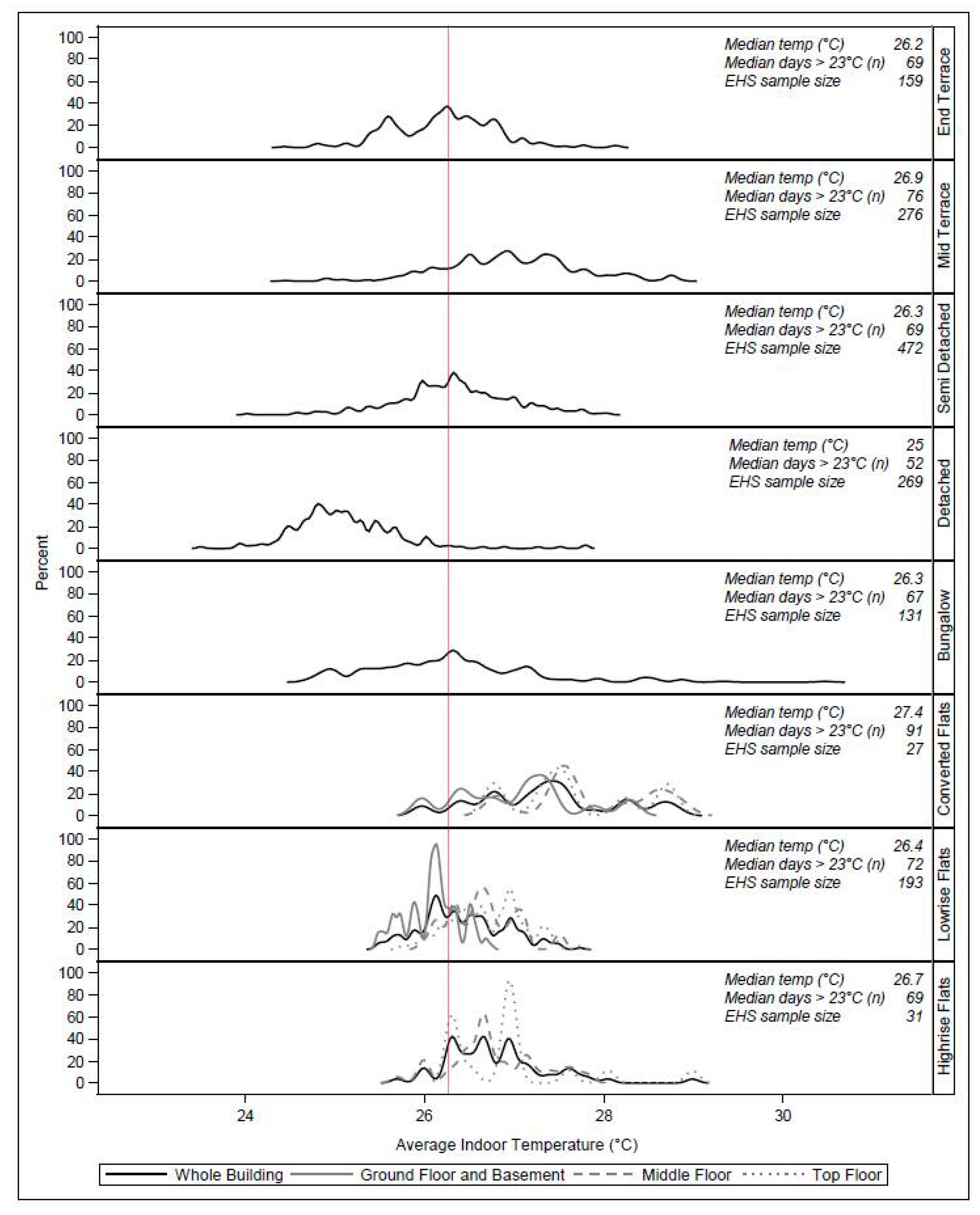
3.1. Heat Exposure across Dwelling Variants
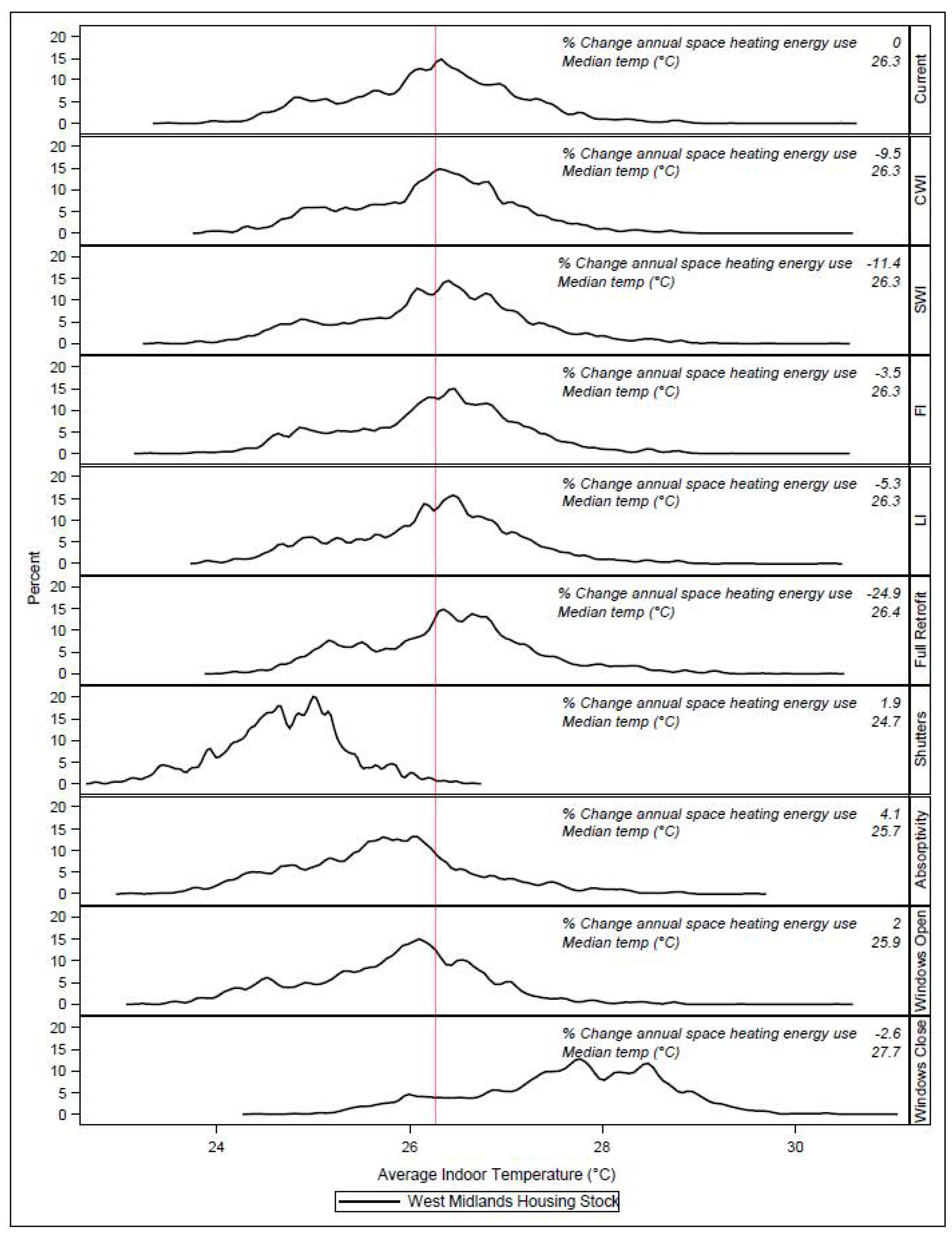
3.2. Housing Adaptations and Heat Exposure
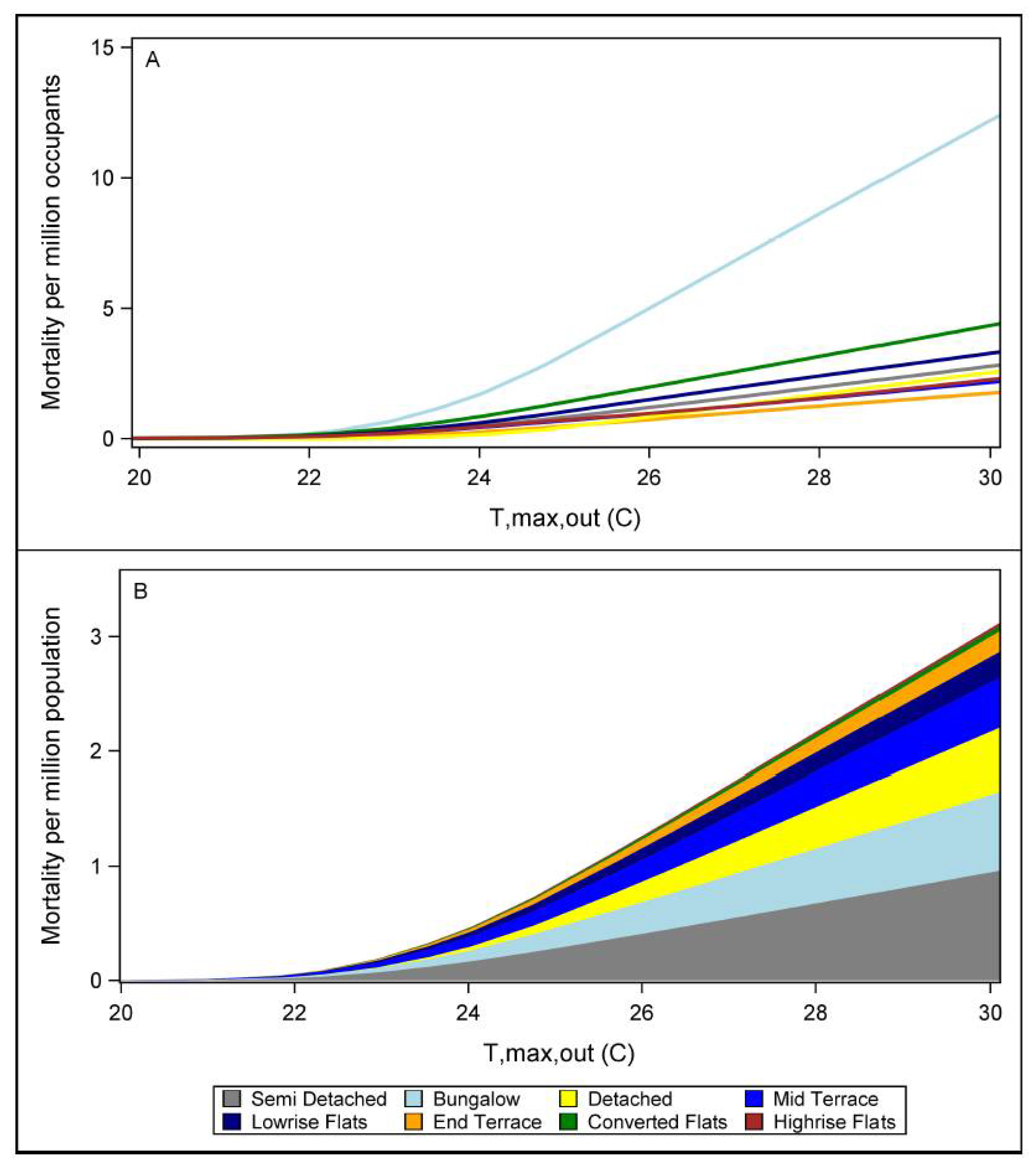
3.3. Mortality across Dwelling Variants
3.4. Housing Stock Adaptation and Mortality
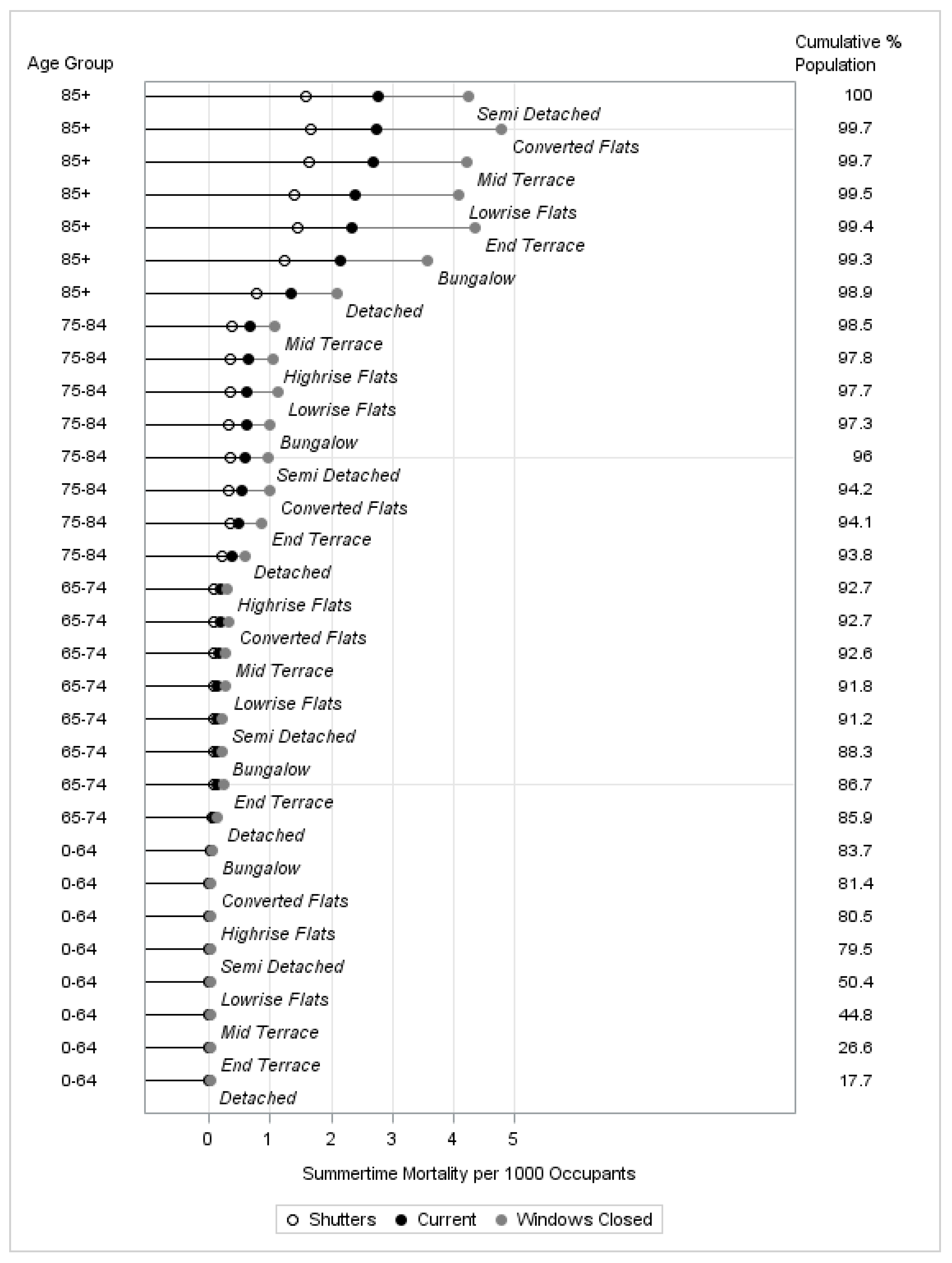
3.5. Mortality across Adapted Dwelling Variants
4. Discussion and Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
Appendix A
References
- Gasparrini, A.; Armstrong, B.; Kovats, S.; Wilkinson, P. The effect of high temperatures on cause-specific mortality in England and Wales. Occup. Environ. Med. 2012, 69, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Johnson, H.; Kovats, R.S.; McGregor, G.; Stedman, J.; Gibbs, M.; Walton, H.; Cook, L.; Black, E. The impact of the 2003 heat wave on mortality and hospital admissions in England. Health Stat. Q. 2005, 25, 6–11. [Google Scholar] [CrossRef]
- PHE Heatwave Plan for England 2015; Public Health England: London, UK, 2015.
- Murphy, J.; Sexton, D.; Jenkins, G.; Boorman, P.; Booth, B.; Brown, K.; Clark, R.; Collins, M.; Harris, G.; Kendon, E. UKCP09 Climate Change Projections; Met Office, Hadley Centre: Exeter, UK, 2009. Available online: http://ukclimateprojections.metoffice.gov.uk/media.jsp?mediaid=87894&filetype=pdf (accessed on 1 October 2017).
- Hajat, S.; Vardoulakis, S.; Heaviside, C.; Eggen, B. Climate change effects on human health: Projections of temperature-related mortality for the UK during the 2020s, 2050s and 2080s. J. Epidemiol. Community Health 2014, 68, 641–648. [Google Scholar] [CrossRef] [PubMed]
- Zuo, J.; Pullen, S.; Palmer, J.; Bennetts, H.; Chileshe, N.; Ma, T. Impacts of heat waves and corresponding measures: A review. J. Clean. Prod. 2015, 92, 1–2. [Google Scholar] [CrossRef]
- Vandentorren, S.; Bretin, P.; Zeghnoun, A.; Mandereau-Bruno, L.; Croisier, A.; Cochet, C.; Ribéron, J.; Siberan, I.; Declercq, B.; Ledrans, M. August 2003 heat wave in France: Risk factors for death of elderly people living at home. Eur. J. Public Health 2006, 16, 583–591. [Google Scholar] [CrossRef] [PubMed]
- Beizaee, A.; Lomas, K.J.; Firth, S.K. National survey of summertime temperatures and overheating risk in English homes. Build. Environ. 2013, 65, 1–17. [Google Scholar] [CrossRef]
- Lomas, K.; Kane, T. Summertime temperatures in 282 UK homes: Thermal comfort and overheating risk. In Proceedings of the 7th Windsor Conference, the Changing Context of Comfort in an Unpredictable World, Windsor, UK, 12–15 April 2012. [Google Scholar]
- Mavrogianni, A.; Wilkinson, P.; Davies, M.; Biddulph, P.; Oikonomou, E. Building characteristics as determinants of propensity to high indoor summer temperatures in London dwellings. Build. Environ. 2012, 55, 117–130. [Google Scholar] [CrossRef]
- Taylor, J.; Mavrogianni, A.; Davies, M.; Das, P.; Shrubsole, C.; Biddulph, P.; Oikonomou, E. Understanding and mitigating overheating and indoor PM2.5 risks using coupled temperature and indoor air quality models. Build. Serv. Eng. Res. Technol. 2015, 36, 275–289. [Google Scholar] [CrossRef]
- Taylor, J.; Davies, M.; Mavrogianni, A.; Shrubsole, C.; Hamilton, I.; Das, P.; Jones, B.; Oikonomou, E.; Biddulph, P. Mapping indoor overheating and air pollution risk modification across Great Britain: A modelling study. Build. Environ. 2016. [CrossRef]
- Gupta, R.; Gregg, M. Preventing the overheating of English suburban homes in a warming climate. Build. Res. Inf. 2013, 41, 281–300. [Google Scholar] [CrossRef]
- Porritt, S.M.; Cropper, P.C.; Shao, L.; Goodier, C.I. Ranking of interventions to reduce dwelling overheating during heat waves. Energy Build. 2012, 55, 16–27. [Google Scholar] [CrossRef]
- Heaviside, C.; Cai, X.-M.; Vardoulakis, S. Attribution of mortality to the Urban Heat Island during heatwaves in the West Midlands, UK. Environ. Health 2016, 15, S27. [Google Scholar] [CrossRef] [PubMed]
- Wolf, T.; McGregor, G. The development of a heat wave vulnerability index for London, United Kingdom. Weather Clim. Extremes 2013, 1, 59–68. [Google Scholar] [CrossRef]
- Jenkins, K.; Hall, J.; Glenis, V.; Kilsby, C.; McCarthy, M.; Goodess, C.; Smith, D.; Malleson, N.; Birkin, M. Probabilistic spatial risk assessment of heat impacts and adaptations for London. Clim. Chang. 2014, 124, 105–117. [Google Scholar] [CrossRef]
- Tomlinson, C.J.; Chapman, L.; Thornes, J.E.; Baker, C.J. Including the urban heat island in spatial heat health risk assessment strategies: A case study for Birmingham, UK. Int. J. Health Geogr. 2011, 10, 42. [Google Scholar] [CrossRef] [PubMed]
- Macintyre, H.L.; Heaviside, C.; Taylor, J.; Picetti, R.; Symonds, P.; Cai, X.-M.; Vardoulakis, S. Assessing urban population vulnerability and environmental risks across an urban area during heatwaves—Implications for health protection. Sci. Total Environ. 2018, 610–611. [Google Scholar] [CrossRef] [PubMed]
- Loughnan, M.; Nicholls, N.; Tapper, N. Mapping heat health risks in urban areas. Int. J. Popul. Res. 2012, 2012, 518687. [Google Scholar] [CrossRef]
- Klein Rosenthal, J.; Kinney, P.L.; Metzger, K.B. Intra-urban vulnerability to heat-related mortality in New York City, 1997–2006. Health Place 2014, 30, 45–60. [Google Scholar] [CrossRef] [PubMed]
- Reid, C.E.; O’Neill, M.S.; Gronlund, C.J.; Brines, S.J.; Brown, D.G.; Diez-Roux, A.V.; Schwartz, J. Mapping community determinants of heat vulnerability. Environ. Health Perspect. 2009, 117, 1730–1736. [Google Scholar] [CrossRef] [PubMed]
- Taylor, J.; Wilkinson, P.; Davies, M.; Armstrong, B.; Chalabi, Z.; Mavrogianni, A.; Symonds, P.; Oikonomou, E.; Bohnenstengel, S.I. Mapping the effects of Urban Heat Island, housing, and age on excess heat-related mortality in London. Urban Clim. 2015, 14, 517–528. [Google Scholar] [CrossRef]
- Liu, C.; Kershaw, T.; Fosas, D.; Ramallo Gonzalez, A.P.; Natarajan, S.; Coley, D.A. High resolution mapping of overheating and mortality risk. Build. Environ. 2017, 122, 1–14. [Google Scholar] [CrossRef]
- Taylor, J.; Wilkinson, P.; Picetti, R.; Symonds, P.; Heaviside, C.; Macintyre, H.; Davies, M.; Mavrogianni, A.; Hutchinson, E. Comparison of built environment adaptations to heat exposure and mortality during hot weather, West Midlands region, UK. Environ. Int. 2017. [CrossRef] [PubMed]
- ONS. 2011 Census: Aggregate Data (England and Wales); Office for National Statistics: London, UK, 2011; Available online: https://census.ukdataservice.ac.uk/get-data/aggregatedata (accessed on 9 May 2018).
- DCLG. English Housing Survey 2010–2011; Department for Communities and Local Government: London, UK, 2011.
- Hughes, M.; Armitage, P.; Palmer, J.; Stone, A. Converting English Housing Survey Data for Use in Energy Models; Cambridge Architectural Research Ltd.: Cambridge, UK; University College London: London, UK, 2012. [Google Scholar]
- Symonds, P.; Taylor, J.; Chalabi, Z.; Mavrogianni, A.; Davies, M.; Hamilton, I.; Vardoulakis, S.; Heaviside, C.; MacIntyre, H. Development of an adaptable England-wide indoor overheating and air pollution model. J. Build. Perform. Simul. 2016, 9, 606–619. [Google Scholar] [CrossRef]
- Symonds, P.; Taylor, J.; Mavrogianni, A.; Davies, M.; Shrubsole, C.; Hamilton, I.; Chalabi, Z. Overheating in English dwellings: Comparing modelled and monitored large-scale datasets. Build. Res. Inf. 2016, 45, 195–208. [Google Scholar] [CrossRef]
- BRE. Energy Follow Up Survey 2011: Report 9: Domestic Appliances, Cooking, and Cooling Equipment; Building Research Establishment: Watford, UK, 2013. [Google Scholar]
- Stephen, R. Airtightness in UK Dwellings; Building Research Establishment: Watford, UK, 2000. [Google Scholar]
- Eames, M.; Kershaw, T.; Coley, D. On the creation of future probabilistic design weather years from UKCP09. Build. Serv. Eng. Res. Technol. 2010, 32, 127–142. [Google Scholar] [CrossRef]
- Schaul, T.; Bayer, J.; Wierstra, D.; Sun, Y.; Felder, M.; Sehnke, F.; Rückstieß, T.; Schmidhuber, J. PyBrain. J. Mach. Learn. Res. 2010, 11, 743–746. [Google Scholar]
- BRE. The Government’s Standard Assessment Procedure for Energy Rating of Dwellings; Building Research Establishment: Watford, UK, 2009. [Google Scholar]
- Hong, S.; Ridley, I.; Oreszczyn, T.; Warm Front Study Group. The impact of energy efficient refurbishment on the airtightness in English dwellings. In Proceedings of the 25th AVIC Conference, Prague, Czech Republic, 23–29 August 2004; pp. 7–12. [Google Scholar]
- Hamilton, I.; Milner, J.; Chalabi, Z.; Das, P.; Jones, B.; Shrubsole, C.; Davies, M.; Wilkinson, P. Health effects of home energy efficiency interventions in England: A modelling study. BMJ Open 2015, 5, e007298. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, B.G.; Chalabi, Z.; Fenn, B.; Hajat, S.; Kovats, S.; Milojevic, A.; Wilkinson, P. Association of mortality with high temperatures in a temperate climate: England and Wales. J. Epidemiol. Community Health 2011, 65, 340–345. [Google Scholar] [CrossRef] [PubMed]
- Vardoulakis, S.; Dimitroulopoulou, C.; Thornes, J.; Lai, K.-M.; Taylor, J.; Myers, I.; Heaviside, C.; Mavrogianni, A.; Shrubsole, C.; Chalabi, Z.; et al. Impact of climate change on the domestic indoor environment and associated health risks in the UK. Environ. Int. 2015, 85, 299–313. [Google Scholar] [CrossRef] [PubMed]
- Vardoulakis, S.; Heaviside, C. Health Effects of Climate Change in the UK 2012: Current Evidence, Recommendations and Research Gaps; Health Protection Agency: London, UK, 2012; pp. 1–242.
- Gasparrini, A.; Guo, Y.; Hashizume, M.; Lavigne, E.; Zanobetti, A.; Schwartz, J.; Tobias, A.; Tong, S.; Rocklöv, J.; Forsberg, B.; et al. Mortality risk attributable to high and low ambient temperature: A multicountry observational study. Lancet 2015, 386, 369–375. [Google Scholar] [CrossRef]
| Adaptation | Details | |
|---|---|---|
| Energy Efficiency | Cavity wall insulation (CWI) | All cavity walls are modelled as insulated, reducing wall U-value, and the infiltration rate in previously uninsulated dwellings reduced by 0.2 air changes per hour (ach) a |
| Internal solid wall insulation (SWI) | All solid walls are modelled as internally insulated, reducing wall U-value, and the infiltration rate in previously uninsulated dwellings reduced by 0.3 ach a | |
| Floor insulation (FI) | All floors are modelled as insulated, reducing floor U-value, and the infiltration rate in previously uninsulated dwellings reduced by 0.1 ach b | |
| Loft insulation (LI) | All lofts are modelled as insulated, reducing loft U-value, and the infiltration rate in previously uninsulated dwellings reduced by 0.1 ach a | |
| Full Retrofit | A full retrofit (floors, loft, walls, and triple-glazed windows) is modelled, with reductions in U-value as above and the infiltration rate reduced by 0.7 ach to a Building Regulations minimum permeability of 3 m3/h/m2 | |
| Heat Adaptation | Shutters | External shutters are closed daily between 9 a.m. and 6 p.m. during the summer |
| Absorptance | The solar absorptance of the building façade is reduced from 0.7 to 0.1 | |
| Occupant Behaviour | Windows Open | Windows are opened when indoor temperatures exceed 18 °C during summer, representing a scenario were windows are continuously open |
| Windows Closed | Windows are opened when indoor temperatures exceed 35 °C, representing a scenario were windows are continuously closed |
| Dwelling Type | Age Group | ||||
|---|---|---|---|---|---|
| 0–64 | 65–74 | 75–85 | 85+ | TOTAL | |
| End Terrace | 88.3% | 7.8% | 3.3% | 0.6% | 541,917 |
| Mid Terrace | 91.7% | 3.7% | 3.8% | 0.9% | 1,060,700 |
| Semi Detached | 85.3% | 8.7% | 5.6% | 0.7% | 1,826,175 |
| Detached | 83.0% | 10.3% | 5.8% | 0.9% | 1,145,396 |
| Bungalow | 42.5% | 28.1% | 22.3% | 7.1% | 297,168 |
| Converted Flat | 78.6% | 11.2% | 8.0% | 2.1% | 56,047 |
| Low-rise Flat | 83.3% | 9.0% | 6.1% | 1.7% | 366,618 |
| High-rise Flat | 88.1% | 4.8% | 7.1% | 0.0% | 65,942 |
| TOTAL | 4,495,026 | 484,724 | 325,129 | 64,301 | 5,359,963 |
| Mortality Per Million (Percent Change from Unadapted Stock) | ||||||
|---|---|---|---|---|---|---|
| Adaptation | 2030 | 2050 | 2080 | |||
| Current | 93 | 126 | 194 | |||
| Adaptation-Energy | ||||||
| CWI | 93 | (0%) | 126 | (0%) | 194 | (0%) |
| SWI | 93 | (0%) | 126 | (0%) | 194 | (0%) |
| FI | 93 | (0%) | 126 | (0%) | 194 | (0%) |
| LI | 92 | (−0.6%) | 126 | (0%) | 193 | (−0.6%) |
| Full Retrofit | 97 | (4.4%) | 131 | (3.5%) | 199 | (2.5%) |
| Adaptation–Heat | ||||||
| Shutters | 53 | (−42.9%) | 76 | (−39.9%) | 122 | (−36.9%) |
| Absorptivity | 78 | (−15.3%) | 108 | (−14.2%) | 170 | (−12.4%) |
| Adaptation-Behaviour | ||||||
| Windows Open | 83 | (−10.1%) | 116 | (−8.1%) | 182 | (−5.9%) |
| Windows Closed | 151 | (63.5%) | 184 | (45.9%) | 249 | (28.7%) |
| Targeted Intervention | ||||||
| Scenario 1 | 85 | (−8.5%) | 117 | (−7.3%) | 184 | (−4.8%) |
| Scenario 2 | 62 | (−32.7%) | 88 | (−30.3%) | 139 | (−28.1%) |
| Scenario 3 | 58 | (−37.5%) | 82 | (−34.8%) | 131 | (−32.2%) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Taylor, J.; Symonds, P.; Wilkinson, P.; Heaviside, C.; Macintyre, H.; Davies, M.; Mavrogianni, A.; Hutchinson, E. Estimating the Influence of Housing Energy Efficiency and Overheating Adaptations on Heat-Related Mortality in the West Midlands, UK. Atmosphere 2018, 9, 190. https://doi.org/10.3390/atmos9050190
Taylor J, Symonds P, Wilkinson P, Heaviside C, Macintyre H, Davies M, Mavrogianni A, Hutchinson E. Estimating the Influence of Housing Energy Efficiency and Overheating Adaptations on Heat-Related Mortality in the West Midlands, UK. Atmosphere. 2018; 9(5):190. https://doi.org/10.3390/atmos9050190
Chicago/Turabian StyleTaylor, Jonathon, Phil Symonds, Paul Wilkinson, Clare Heaviside, Helen Macintyre, Michael Davies, Anna Mavrogianni, and Emma Hutchinson. 2018. "Estimating the Influence of Housing Energy Efficiency and Overheating Adaptations on Heat-Related Mortality in the West Midlands, UK" Atmosphere 9, no. 5: 190. https://doi.org/10.3390/atmos9050190
APA StyleTaylor, J., Symonds, P., Wilkinson, P., Heaviside, C., Macintyre, H., Davies, M., Mavrogianni, A., & Hutchinson, E. (2018). Estimating the Influence of Housing Energy Efficiency and Overheating Adaptations on Heat-Related Mortality in the West Midlands, UK. Atmosphere, 9(5), 190. https://doi.org/10.3390/atmos9050190





