Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge
Abstract
:1. Introduction
2. Experimental Section
2.1. Study Design and Patients
2.2. Protocol
2.3. Randomization and Masking
2.4. Statistical Analysis
2.5. Funding Sources
3. Results
3.1. Phase 1: Outcome of Patients Following the Gluten Free Diet

| Variable | Overall (n = 134 *) | GFD | p | |
|---|---|---|---|---|
| Responsive (n = 101) | Non-Responsive (n = 29) | |||
| Sex | ||||
| Male | 17 (12.7%) | 10 (9.9%) | 7 (24.1%) | 0.06 |
| Female | 117 (87.3%) | 91 (90.1%) | 22 (75.9%) | |
| Age: years | 39.1 (11.7) | 39.3 (11.0) | 38.5 (13.6) | 0.75 |
| BMI | 22.4 (3.8) | 22.3 (4.0) | 22.4 (3.2) | 0.96 |
| Functional disease | ||||
| IBS | 77 (57.5%) | 55 (54.5%) | 20 (69.0%) | 0.80 |
| Dyspepsia | 22 (16.4%) | 18 (17.8%) | 3 (10.3%) | |
| Other | 35 (26.1%) | 28 (17.7%) | 6 (20.7%) | |
| IDA | 27 (20.1%) | 21 (20.8%) | 6 (20.6%) | 0.47 |
| AST increased | 0 (0%) | 0 (0%) | 0 (0%) | - |
| ALT increased | 3 (2.2%) | 3 (2.9%) | 0 (0%) | 0.61 |
| CRP increased | 4 (2.9%) | 3 (2.9%) | 1 (3.4%) | 0.54 |
| Presence of a first-degree relative with CD | 16 (11.9%) | 13 (12.9%) | 1 (3.4%) | 0.19 |
| Variable | VAS Values | p (0–21) | p (R vs. NR) | |
|---|---|---|---|---|
| At Enrollment | After 3 Weeks on GFD | |||
| Abdominal pain | ||||
| Overall | 5.9 ± 2.8 | 2.7 ± 2.6 | 0.001 | 0.001 |
| GFD responsive | 6.1 ± 2.7 | 2.0 ± 2.1 | 0.001 | |
| GFD non-responsive | 5.2 ± 3.0 | 5.0 ± 2.6 | 0.66 | |
| Stool Consistency satisfaction | ||||
| Overall | 3.5 ± 2.7 | 6.3 ± 2.7 | 0.001 | 0.001 |
| GFD responsive | 3.6 ± 2.7 | 7.1 ± 2.2 | 0.001 | |
| GFD non-responsive | 3.3 ± 2.6 | 3.7 ± 2.6 | 0.47 | |
| Bloating | ||||
| Overall | 6.8 ± 2.7 | 3.4 ± 2.9 | 0.001 | 0.001 |
| GFD responsive | 7.1 ± 2.4 | 2.7 ± 2.5 | 0.001 | |
| GFD non-responsive | 6.0 ± 3.3 | 5.8 ± 3.0 | 0.80 | |
| Postprandial fullness | ||||
| Overall | 7.2 ± 2.4 | 3.9 ± 2.5 | 0.001 | 0.580 |
| GFD responsive | 7.6 ± 2.1 | 3.8 ± 2.4 | 0.001 | |
| GFD non-responsive | 5.2 ± 3.4 | 4.1 ± 3.5 | 0.47 | |
| Early Satiety | ||||
| Overall | 5.7 ± 3.3 | 2.4 ± 2.4 | 0.001 | 0.770 |
| GFD responsive | 6.2 ± 3.1 | 2.5 ± 2.5 | 0.001 | |
| GFD non-responsive | 3.0 ± 3.3 | 1.6 ± 1.5 | 0.32 | |
| Epigastric pain | ||||
| Overall | 6.1 ± 2.9 | 2.9 ± 2.9 | 0.001 | 0.470 |
| GFD responsive | 6.4 ± 2.8 | 2.8 ± 2.9 | 0.001 | |
| GFD non-responsive | 4.7 ± 3.0 | 3.2 ± 3.1 | 0.06 | |
| Other symptoms | ||||
| Overall | 7.3 ± 2.4 | 3.8 ± 3.5 | 0.005 | 0.100 |
| GFD responsive | 7.5 ± 1.9 | 3.1 ± 2.9 | 0.001 | |
| GFD non-responsive | 6.2 ± 4.5 | 7.0 ± 5.1 | 0.87 | |
| Global satisfaction | ||||
| Overall | 2.3 ± 1.2 | 6.5 ± 2.2 | 0.0001 | 0.001 |
| GFD responsive | 2.2 ± 1.0 | 7.4 ± 1.4 | 0.0001 | |
| GFD non-responsive | 2.5 ± 1.3 | 3.4 ± 1.5 | 0.001 | |
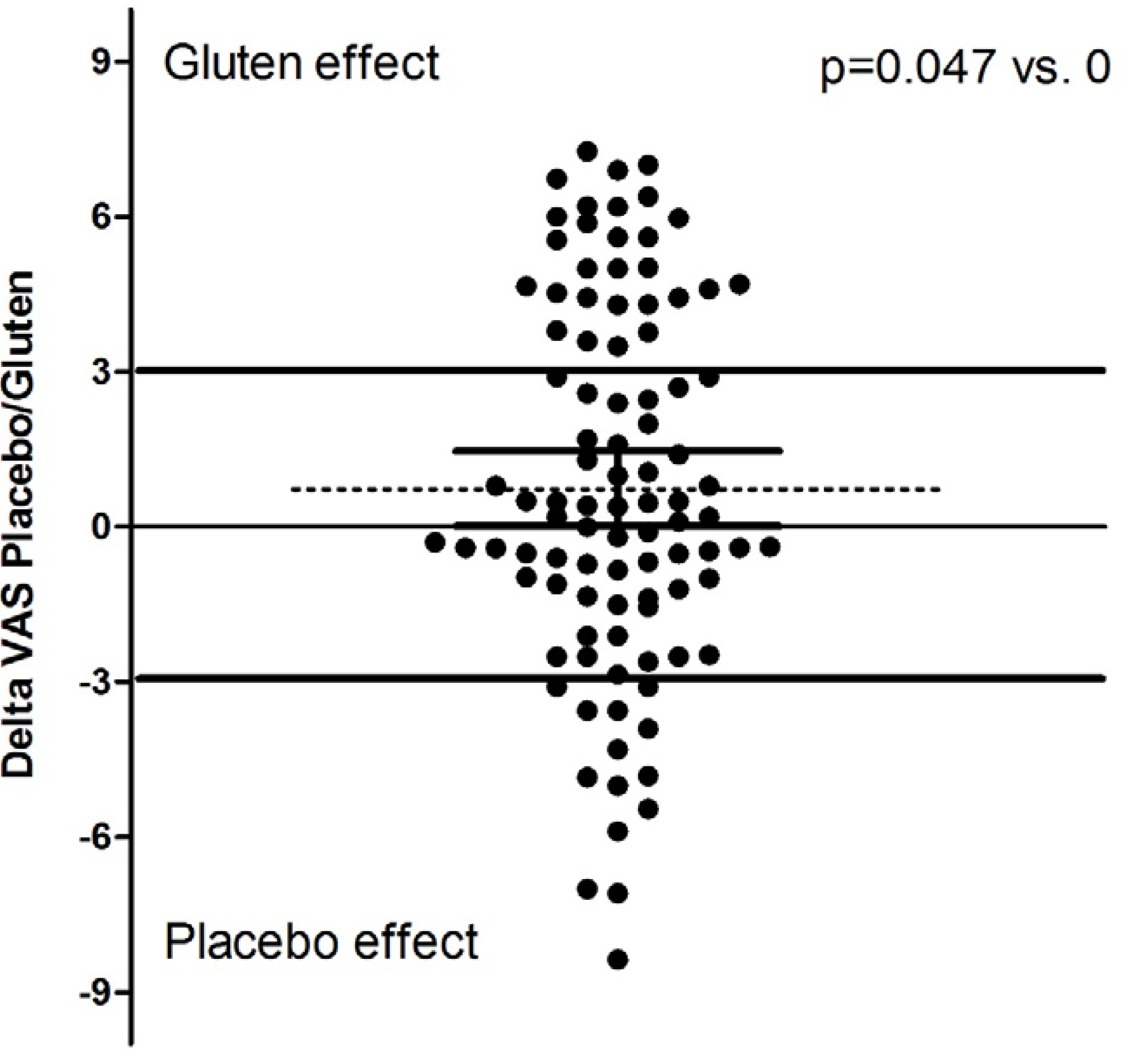
3.2. Phase 2: Outcome of the Gluten Challenge
| Variable | Overall (n = 98) | DBPCC Positive (n = 28) | DBPCC Negative (n = 69) | p |
|---|---|---|---|---|
| Sex | ||||
| Male | 10 (10.2%) | 0 (0%) | 10 (14.5%) | 0.08 |
| Female | 88 (89.8%) | 28 (100%) | 59 (85.5%) | |
| Age years | 39.4 ± 11.1 | 39.9 ± 12.7 | 39.2 ± 10.6 | 0.79 |
| BMI | 22.4 ± 4.1 | 22.0 ± 2.9 | 22.6 ± 4.5 | 0.51 |
| Functional disease | ||||
| IBS | 53 (54.1%) | 18 (64.3%) | 35 (50.7%) | 0.26 |
| Dyspepsia | 17 (17.3%) | 4 (14.3%) | 13 (18.8%) | |
| Other | 28 (28.6%) | 6 (21.4%) | 21 (30.5%) | |
| IDA | 10 (10.2%) | 4 (14.2%) | 3 (4.3%) | 0.47 |
| AST increased | 0 (0%) | 0 (0%) | 0 (0%) | |
| ALT increased | 3 (3.0%) | 0 (0%) | 0 (0%) | 0.61 |
| CRP increased | 1 (1.0%) | 0 (0%) | 1 (1.4%) | 0.54 |
| Presence of a first-degree relative with CD | 14 (14.3%) | 5 (21.4%) | 9 (3.4%) | 0.19 |
| Variable | VAS Values | p | |
|---|---|---|---|
| DBPCC Positive | DBPCC Negative | ||
| Abdominal pain | 5.4 ± 2.4 | 3.2 ± 2.8 | 0.006 |
| Stool consistency satisfaction | 4.5 ± 2.9 | 5.7 ± 3.0 | 0.08 |
| Bloating | 8.2 ± 2.8 | 3.6 ± 2.9 | 0.0001 |
| Postprandial Fullness | 6.6 ± 3.0 | 4.9 ± 2.9 | 0.01 |
| Early satiety | 6.4 ± 2.8 | 4.4 ± 2.9 | 0.03 |
| Epigastric pain | 2.3 ± 2.3 | 3.0 ± 3.0 | 0.27 |
| Other gastrointestinal symptoms | 4.6 ± 4.0 | 3.4 ± 3.0 | 0.41 |
| Variable | SF36 Values | p | |
|---|---|---|---|
| DBPCC Positive (n = 28) | DBPCC Negative (n = 69) | ||
| Physical Functioning | 46.9 ± 11.6 | 52.3 ± 6.8 | 0.030 |
| Role Limitation—Physical | 42.6 ± 11.6 | 49.6 ± 9.7 | 0.003 |
| Bodily Pain | 46.9 ± 9.9 | 41.0 ± 10.5 | 0.010 |
| General Medical Health | 44.0 ± 9.2 | 45.6 ± 10.2 | 0.480 |
| Vitality | 44.2 ± 9.2 | 50.7 ± 8.5 | 0.001 |
| Social Functioning | 41.6 ± 11.2 | 47.9 ± 9.6 | 0.007 |
| Role Limitation Emotional | 42.6 ± 11.9) | 50.5 ± 9.4 | 0.003 |
| Mental Health | 44.7 ± 8.0 | 48.4 ± 8.5 | 0.050 |
| Physical Summary Component | 44.4 ± 9.2 | 49.1 ± 7.6 | 0.010 |
| Mental Summary Component | 43.0 ± 8.8 | 48.9 ± 8.6 | 0.004 |
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Catassi, C.; Bai, J.C.; Bonaz, B.; Bouma, G.; Calabrò, A.; Carroccio, A.; Castillejo, G.; Ciacci, C.; Cristofori, F.; Dolinsek, J.; et al. Non-Celiac Gluten sensitivity: The new frontier of gluten related disorders. Nutrients 2013, 5, 3839–3853. [Google Scholar] [CrossRef] [PubMed]
- Volta, U.; Bardella, M.T.; Calabro, A.; Troncone, R.; Corazza, G.R. Study Group for Non-Celiac Gluten Sensitivity. An Italian prospective multicenter survey on patients suspected of having non-celiac gluten sensitivity. BMC Med. 2014, 12, 85. [Google Scholar] [CrossRef] [PubMed]
- Fasano, A.; Sapone, A.; Zevallos, V.; Schuppan, D. Nonceliac Gluten Sensitivity. Gastroenterology 2015, 148, 1195–1204. [Google Scholar] [CrossRef] [PubMed]
- Cooper, B.T.; Holmes, G.K.; Ferguson, R.; Thompson, R.A.; Allan, R.N.; Cooke, W.T. Gluten-sensitive diarrhea without evidence of celiac disease. Gastroenterology 1980, 79, 801–806. [Google Scholar] [PubMed]
- Ellis, A.; Linaker, B.D. Non-coeliac gluten sensitivity? Lancet 1978, 1, 1358–1359. [Google Scholar] [CrossRef]
- Sapone, A.; Bai, J.C.; Ciacci, C.; Dolinsek, J.; Green, P.H.; Hadjivassiliou, M.; Kaukinen, K.; Rostami, K.; Sanders, D.S.; Schumann, M.; et al. Spectrum of gluten-related disorders: Consensus on new nomenclature and classification. BMC Med. 2012. [Google Scholar] [CrossRef] [PubMed]
- Catassi, C.; Elli, L.; Bonaz, B.; Bouma, G.; Carroccio, A.; Castillejo, G.; Cellier, C.; Cristofori, F.; de Magistris, L.; Dolinsek, J.; et al. Diagnosis of Non-Celiac Gluten Sensitivity (NCGS): The Salerno Experts’ Criteria. Nutrients 2015, 7, 4966–4977. [Google Scholar] [CrossRef] [PubMed]
- Shah, E.; Pimentel, M. Placebo effect in clinical trial design for irritable bowel syndrome. J. Neurogastroenterol. Motil. 2014, 20, 163–170. [Google Scholar] [CrossRef] [PubMed]
- Gibson, P.R.; Varney, J.; Malakar, S.; Muir, J.G. Food components and irritable bowel syndrome. Gastroenterology 2015. [Google Scholar] [CrossRef] [PubMed]
- Farre, R.; Tack, J. Food and symptom generation in functional gastrointestinal disorders: Physiological aspects. Am. J. Gastroenterol. 2013, 108, 698–706. [Google Scholar] [CrossRef] [PubMed]
- Di Giacomo, D.V.; Tennyson, C.A.; Green, P.H.; Demmer, R.T. Prevalence of gluten-free diet adherence among individuals without celiac disease in the USA: Results from the Continuous National Health and Nutrition Examination Survey 2009–2010. Scand. J. Gastroenterol. 2013, 48, 921–925. [Google Scholar] [CrossRef] [PubMed]
- Di Sabatino, A.; Corazza, G.R. Nonceliac gluten sensitivity: Sense or sensibility? Ann. Intern. Med. 2012, 156, 309–311. [Google Scholar] [CrossRef] [PubMed]
- Shahbazkhani, B.; Sadeghi, A.; Malekzadeh, R.; Khatavi, F.; Etemadi, M.; Kalantri, E.; Rostami-Nejad, M.; Rostami, K. Non-Celiac Gluten Sensitivity Has Narrowed the Spectrum of Irritable Bowel Syndrome: A Double-Blind Randomized Placebo-Controlled Trial. Nutrients 2015, 7, 4542–4554. [Google Scholar] [CrossRef] [PubMed]
- Carroccio, A.; Mansueto, P.; Iacono, G.; Soresi, M.; D’Alcamo, A.; Cavataio, F.; Brusca, I.; Florena, A.M.; Ambrosiano, G.; Seidita, A.; et al. Non-celiac wheat sensitivity diagnosed by double-blind placebo-controlled challenge: Exploring a new clinical entity. Am. J. Gastroenterol. 2012, 107, 1898–1906. [Google Scholar] [CrossRef] [PubMed]
- Di Sabatino, A.; Volta, U.; Salvatore, C.; Biancheri, P.; Caio, G.; De Giorgio, R.; Di Stefano, M.; Corazza, G.R. Small Amounts of Gluten in Subjects with Suspected Nonceliac Gluten Sensitivity: A Randomized, Double-Blind, Placebo-Controlled, Cross-Over Trial. Clin. Gastroenterol. Hepatol. 2015. [Google Scholar] [CrossRef] [PubMed]
- Zanini, B.; Basche, R.; Ferraresi, A.; Ricci, C.; Lanzarotto, F.; Marullo, M.; Villanacci, V.; Hidalgo, A.; Lanzini, A. Randomised clinical study: Gluten challenge induces symptom recurrence in only a minority of patients who meet clinical criteria for non-coeliac gluten sensitivity. Aliment. Pharmacol. Ther. 2015, 42, 968–976. [Google Scholar] [CrossRef] [PubMed]
- Biesiekierski, J.R.; Newnham, E.D.; Irving, P.M.; Barrett, J.S.; Haines, M.; Doecke, J.D.; Shepherd, S.J.; Muir, J.G.; Gibson, P.R. Gluten causes gastrointestinal symptoms in subjects without celiac disease: A double-blind randomized placebo-controlled trial. Am. J. Gastroenterol. 2011, 106, 508–514. [Google Scholar] [CrossRef] [PubMed]
- Biesiekierski, J.R.; Peters, S.L.; Newnham, E.D.; Rosella, O.; Muir, J.G.; Gibson, P.R. No effects of gluten in patients with self-reported non-celiac gluten sensitivity after dietary reduction of fermentable, poorly absorbed, short-chain carbohydrates. Gastroenterology 2013. [Google Scholar] [CrossRef] [PubMed]
- Glutoxtrial. Available online: https://sites.google.com/site/glutoxitalia (accessed on 5 February 2016).
- Spiegazione Glutox. Available online: https://www.youtube.com/watch?v=ztacjBTAppo (accessed on 5 February 2016).
- Rome Foundation. Rome III Diagnostic Criteria. Available online: http://www.romecriteria.org/criteria/ (accessed on 5 February 2016).
- Protocollo_diagn. Available online: http://www.salute.gov.it/speciali/documenti/protocollo_diagn.pdf (accessed on 5 February 2016).
- Fasano, A.; Catassi, C. Clinical practice. Celiac disease. N. Engl. J. Med. 2012, 367, 2419–2426. [Google Scholar] [CrossRef] [PubMed]
- Levitt, M.D.; Hirsh, P.; Fetzer, C.A.; Sheahan, M.; Levine, A.S. H2 excretion after ingestion of complex carbohydrates. Gastroenterology 1987, 92, 383–389. [Google Scholar] [PubMed]
- Profilo individuale dell'SF 36. Available online: http://crc.marionegri.it/qdv/questionari/sf36/scoreSF.html?form (accessed on 5 February 2016).
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Universität Düsseldorf: G*power. Available online: http://www.gpower.hhu.de (accessed on 5 February 2016).
- Elli, L. Where’s the evidence for gluten sensitivity? BMJ 2012, 345, e7360. [Google Scholar] [CrossRef] [PubMed]
- Sanders, D.S.; Aziz, I. Non-celiac wheat sensitivity: Separating the wheat from the chat! Am. J. Gastroenterol. 2012, 107, 1908–1912. [Google Scholar] [CrossRef] [PubMed]
- Carroccio, A.; Mansueto, P.; D’Alcamo, A.; Iacono, G. Non-celiac wheat sensitivity as an allergic condition: Personal experience and narrative review. Am. J. Gastroenterol. 2013, 108, 1845–1852. [Google Scholar] [CrossRef] [PubMed]
- Junker, Y.; Zeissig, S.; Kim, S.J.; Barisani, D.; Wieser, H.; Leffler, D.A.; Zevallos, V.; Libermann, T.A.; Dillon, S.; Freitag, T.L.; et al. Wheat amylase trypsin inhibitors drive intestinal inflammation via activation of toll-like receptor 4. J. Exp. Med. 2012, 209, 2395–2408. [Google Scholar] [CrossRef] [PubMed]
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Elli, L.; Tomba, C.; Branchi, F.; Roncoroni, L.; Lombardo, V.; Bardella, M.T.; Ferretti, F.; Conte, D.; Valiante, F.; Fini, L.; et al. Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge. Nutrients 2016, 8, 84. https://doi.org/10.3390/nu8020084
Elli L, Tomba C, Branchi F, Roncoroni L, Lombardo V, Bardella MT, Ferretti F, Conte D, Valiante F, Fini L, et al. Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge. Nutrients. 2016; 8(2):84. https://doi.org/10.3390/nu8020084
Chicago/Turabian StyleElli, Luca, Carolina Tomba, Federica Branchi, Leda Roncoroni, Vincenza Lombardo, Maria Teresa Bardella, Francesca Ferretti, Dario Conte, Flavio Valiante, Lucia Fini, and et al. 2016. "Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge" Nutrients 8, no. 2: 84. https://doi.org/10.3390/nu8020084
APA StyleElli, L., Tomba, C., Branchi, F., Roncoroni, L., Lombardo, V., Bardella, M. T., Ferretti, F., Conte, D., Valiante, F., Fini, L., Forti, E., Cannizzaro, R., Maiero, S., Londoni, C., Lauri, A., Fornaciari, G., Lenoci, N., Spagnuolo, R., Basilisco, G., ... Buscarini, E. (2016). Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge. Nutrients, 8(2), 84. https://doi.org/10.3390/nu8020084






