Geographical Variation in Antibiotic-Resistant Escherichia coli Isolates from Stool, Cow-Dung and Drinking Water
Abstract
:1. Introduction
2. Experimental Section
2.1. Study Settings
| Geographical regions and environmental variables | Malkangiri (Non-coastal) | Puri (Coastal) |
|---|---|---|
| Physical components | ||
| Temperature (Maximum, Minimum) | 47 °C, 11 °C | 36 °C, 13 °C |
| Average yearly rainfall in mm | 1465 | 1586 |
| Natural components | ||
| Height from the sea level in metres | 196 | 6 |
| Forest cover in percentage | 38 | 3 |
| Social components | ||
| Total population in million | 0.61 | 1.69 |
| Population Density per Sq. Km | 106 | 488 |
| Literacy Rate in percentage | 49 | 85 |
2.2. Sampling and Data Collection
2.3. Isolation and Identification of E. coli
2.4. Antibiotic Susceptibility Testing
2.5. Determination of Ciprofloxacin Minimum Inhibitory Concentration
2.6. Statistical Analysis
3. Results
3.1. Information on Households and Isolation Rate of E. coli
| Information on households | NCE (N = 230), n (%) | CE (N = 187), n (%) |
|---|---|---|
| Socioeconomic status | ||
| Lower | 197 (86) | 148 (79) |
| Upper | 33 (14) | 39 (21) |
| Education of family head | ||
| Illiterate | 37 (16) | 18 (10) |
| Primary (1–5 years) | 101 (44) | 77 (41) |
| Secondary (6–12 years) | 81 (35) | 76 (41) |
| Higher (more than 12 years) | 11 (5) | 16 (8) |
| Drinking water sources | ||
| Tube well | 192 (83) | 169 (90) |
| Water supply system | 28 (12) | 5 (3) |
| Well | 4 (2) | 13 (7) |
| Pond | 6 (3) | 0 |
| Defecation | ||
| Latrine | 26 (11) | 30 (16) |
| Open-air | 204 (89) | 157 (84) |
| Age of child | ||
| 3 to 5 years | 105 (46) | 74 (40) |
| 6 to 9 years | 125 (54) | 113 (60) |
| Sex of child | ||
| Boy | 128 (56) | 102 (55) |
| Girl | 102 (44) | 85 (45) |
| Antibiotic use in the child, last year | ||
| Yes | 175 (76) | 175 (94) |
| No | 3 (1) | 6 (3) |
| Not known | 52 (22) | 6 (3) |
| Antibiotic use in the cow, last year | ||
| Yes | 11 (5) | 7 (4) |
| No | 219 (95) | 180 (96) |
| Isolation rate of E. coli | ||
| Children’s stools | 139 (60) | 138 (74) |
| Cow-dung | 140 (61) | 128 (68) |
| Drinking water | 97 (42) | 54 (29) |
3.2. Antibiotic Resistance Pattern
| Antibiotics | Resistance in E. coli isolates from various sources | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Children’s stool, n (%) | Cow-dung, n (%) | Drinking water, n (%) | |||||||
| NCE N = 139 | CE N = 138 | P | NCE N = 140 | CE N = 128 | P | NCE N = 97 | CE N = 54 | P | |
| Tetracycline | 76 (55) | 70 (51) | 0.51 | 69 (49) | 46 (36) | 0.027 | 59 (61) | 16 (30) | <0.001 |
| Ampicillin/Sulbactam | 69 (50) | 55 (40) | 0.102 | 71 (51) | 35 (27) | <0.001 | 46 (47) | 16 (30) | 0.033 |
| Cefuroxime (2nd) | 88 (63) | 70 (51) | 0.034 | 89 (64) | 48 (37) | <0.001 | 63 (65) | 22 (41) | 0.004 |
| Cefotaxime (3rd) | 90 (65) | 68 (49) | 0.009 | 82 (59) | 39 (30) | <0.001 | 72 (74) | 23 (43) | <0.001 |
| Cefixime (3rd) | 95 (68) | 72 (52) | 0.006 | 86 (61) | 49 (38) | <0.001 | 52 (54) | 16 (30) | 0.005 |
| Cotrimoxazole | 79 (57) | 52 (38) | 0.001 | 69 (49) | 37 (29) | 0.001 | 51 (53) | 22 (41) | 0.163 |
| Amikacin | 39 (28) | 52 (38) | 0.088 | 58 (41) | 42 (33) | 0.145 | 25 (26) | 9 (17) | 0.199 |
| Ciprofloxacin | 60 (43) | 56 (41) | 0.663 | 43 (31) | 33 (26) | 0.371 | 40 (41) | 11 (20) | 0.009 |
| Norfloxacin | 70 (50) | 59 (43) | 0.204 | 71 (51) | 43 (34) | 0.005 | 47 (48) | 18 (33) | 0.072 |
| Nalidixic acid | 92 (66) | 71 (51) | 0.013 | 78 (56) | 48 (37) | 0.003 | 63 (65) | 20 (37) | 0.001 |
| Antibiotics | Penicillin (B) | Cephalosporin (C) (cefotaxime, cefixime) | Cotrimoxazole (D) | Aminoglycoside (E) | Fluoroquinolone (F) | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| NCE | CE | NCE | CE | NCE | CE | NCE | CE | NCE | CE | |
| 4A. Prevalence of resistance in children’s stool n (%) | ||||||||||
| Tetracycline (A) | 35 (25) | 34 (25) | 68 (49) | 52 (38) | 44 (32) | 30 (22) | 21 (15) | 33 (24) | 49 (35) | 41 (28) |
| Penicillin (B) | 60 (43) | 50 (36) | 49 (35) ** | 28 (20) | 23 (17) | 20 (14) | 51 (37) | 51 (37) | ||
| Cephalosporin (C) | 70 (50) ** | 42 (30) | 29 (21) | 38 (28) | 74 (53) | 62 (45) | ||||
| Cotrimoxazole (D) | 25 (18) | 18 (13) | 58 (42) * | 41 (30) | ||||||
| Aminoglycoside (E) | 24 (17) | 29 (21) | ||||||||
| AB | 32 (23) | 31 (22) | 21 (15) | 18 (13) | 9 (6) | 11 (8) | 26 (19) | 30 (22) | ||
| ABC | 21 (15) | 17 (12) | 9 (6) | 11 (8) | 25 (18) | 28 (20) | ||||
| ABCD | 5 (4) | 6 (4) | 17 (12) | 16 (12) | ||||||
| ABCDE | 4 (3) | 6 (4) | ||||||||
| 4B. Prevalence of resistance in cow-dung n (%) | ||||||||||
| Tetracycline (A) | 35 (25) ** | 16 (13) | 58 (41) ** | 29 (23) | 36 (26) * | 17 (13) | 28 (20) | 21 (16) | 44 (31) ** | 22 (17) |
| Penicillin (B) | 64 (46) *** | 26 (20) | 50 (36) ** | 22 (17) | 31 (22) ** | 12 (9) | 58 (41) ** | 31 (24) | ||
| Cephalosporin (C) | 61 (44) *** | 29 (23) | 43 (31) | 26 (20) | 73 (52) ** | 40 (31) | ||||
| Cotrimoxazole (D) | 30 (21) | 17 (13) | 53 (38) ** | 30 (23) | ||||||
| Aminoglycoside (E) | 34 (24) ** | 17 (13) | ||||||||
| AB | 33 (24) * | 15 (12) | 22 (16) | 11 (9) | 14 (10) | 6 (5) | 28 (20) * | 14 (11) | ||
| ABC | 20 (14) | 10 (8) | 12 (9) | 5 (4) | 26 (19) | 14 (11) | ||||
| ABCD | 6 (4) | 5 (4) | 14 (10) | 10 (8) | ||||||
| ABCDE | 3 (2) | 5 (4) | ||||||||
| 4C. Prevalence of resistance in drinking water n (%) | ||||||||||
| Tetracycline (A) | 29 (30) * | 8 (15) | 56 (58) *** | 13 (24) | 31 (32) * | 9 (17) | 11 (11) | 4 (7) | 38 (39) ** | 9 (17) |
| Penicillin (B) | 38 (39) * | 11 (20) | 37 (38) * | 11 (20) | 18 (19) ** | 1 (2) | 34 (35) * | 10 (19) | ||
| Cephalosporin (C) | 40 (41) | 16 (30) | 17 (18) | 4 (8) | 55 (57) ** | 17 (31) | ||||
| Cotrimoxazole (D) | 17 (18) * | 2 (4) | 37 (38) * | 11 (20) | ||||||
| Aminoglycoside (E) | 17 (18) * | 2 (4) | ||||||||
| AB | 28 (29) | 8 (15) | 22 (23) * | 5 (9) | 6 (6) | 1 (2) | 21 (22) | 6 (11) | ||
| ABC | 21 (22) | 5 (9) | 5 (5) | 1 (2) | 20 (21) | 6 (11) | ||||
| ABCD | 2 (2) | 0 | 16 (16) | 4 (7) | ||||||
| ABCDE | 2 (2) | 0 | ||||||||
3.3. Association of Resistance, Co-Resistance and Multi-Resistance
3.4. Ciprofloxacin MIC Determination
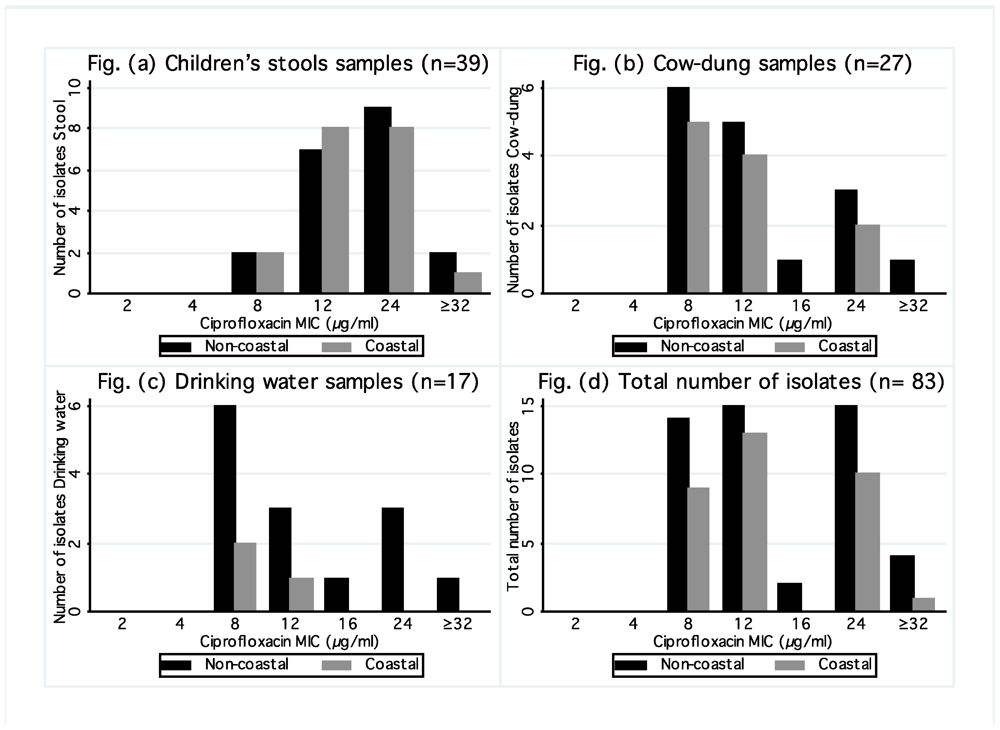
4. Discussion
5. Conclusions
Acknowledgments
Conflict of Interest
References
- McMahon, M.A.; Xu, J.; Moore, J.E.; Blair, I.S.; McDowell, D.A. Environmental stress and antibiotic resistance in food-related pathogens. Appl. Environ. Microbiol. 2007, 73, 211–217. [Google Scholar]
- Bush, K.; Courvalin, P.; Dantas, G.; Davies, J.; Eisenstein, B.; Huovinen, P.; Jacoby, G.A.; Kishony, R.; Kreiswirth, B.N.; Kutter, E.; et al. Tackling antibiotic resistance. Nat. Rev. Microbiol. 2011, 9, 894–896. [Google Scholar] [CrossRef]
- Smith, K.R.; Corvalan, C.F.; Kjellstrom, T. How much global ill health is attributable to environmental factors? Epidemiology 1999, 10, 573–584. [Google Scholar] [CrossRef]
- Yagupsky, P. Selection of antibiotic-resistant pathogens in the community. Pediatr. Infect. Dis. J. 2006, 25, 974–976. [Google Scholar]
- Ishii, S.; Sadowsky, M.J. Escherichia coli in the environment: Implications for water quality and human health. Microbes Environ. 2008, 23, 101–108. [Google Scholar]
- Bailey, J.K.; Pinyon, J.L.; Anantham, S.; Hall, R.M. Commensal Escherichia coli of healthy humans: A reservoir for antibiotic-resistance determinants. J. Med. Microbiol. 2010, 59, 1331–1339. [Google Scholar]
- Martinez, J.L. The role of natural environments in the evolution of resistance traits in pathogenic bacteria. Proc. Biol. Sci. 2009, 276, 2521–2530. [Google Scholar]
- van den Bogaard, A.E.; Stobberingh, E.E. Epidemiology of resistance to antibiotics. Links between animals and humans. Int. J. Antimicrob. Agents 2000, 14, 327–335. [Google Scholar] [CrossRef]
- World Health Organization (WHO), Antimicrobial Resistance; WHO: Geneva, Switzerland, 2011.
- Fabrega, A.; Sanchez-Cespedes, J.; Soto, S.; Vila, J. Quinolone resistance in the food chain. Int J Antimicrob Agents 2008, 31, 307–315. [Google Scholar]
- Hordijk, J.; Veldman, K.; Dierikx, C.; van Essen-Zandbergen, A.; Wagenaar, J.A.; Mevius, D. Prevalence and characteristics of quinolone resistance in Escherichia coli in veal calves. Vet. Microbiol. 2011. in print.. [Google Scholar]
- Chattopadyay, A.; Agnihotram, V.R. Burden of disease in rural India: An analysis through cause of death. Int. J. Third World Med. 2005, 2, 2. [Google Scholar]
- District Information, Orissa. Available online: http://www.123orissa.com/exploreorissa/distinfo/default.asp (assessed on 14 December 2011).
- Government of India. Orissa Census. 2011. Available online: http://censusindia.gov.in/2011-prov-results/prov_data_products_orissa.html (assessed on 14 December 2011).
- King, S.D.; Green, D.R. Redefining the limits of the coastal zone: Bridging the gap between land and sea using remote sensing, GIS, and the internet. GeoCoast 2001, 2, 1–15. [Google Scholar]
- Kumar, N.; Shekhar, C.; Kumar, P.; Kundu, A.S. Kuppuswamy’s socioeconomic status scale-updating for 2007. Indian J. Pediatr. 2007, 74, 1131–1132. [Google Scholar]
- Clinical and Laboratory Standards Institute, Performance Standard for Antimicrobial Disk Susceptibility Testing; Twentieth informational supplement (document M100-S20); The Cinical and Laboratory Standards Institute: Wayne, PA, USA, 2010.
- Environment Agency, The Microbiology of Drinking Water (2009) Part 4—Methods for the Isolation and Enumeration of Coliform Bacteria and Escherichia coli (including E. coli O157:H7), Methods for the Examination of Waters and Associated Materials; The Environment Agency: Rotherham, UK, 2009.
- Seidman, J.C.; Anitha, K.P.; Kanungo, R.; Bourgeois, A.L.; Coles, C.L. Risk factors for antibiotic-resistant E. coli in children in a rural area. Epidemiol. Infect. 2009, 137, 879–888. [Google Scholar] [CrossRef]
- Vatopoulos, A.C.; Varvaresou, E.; Petridou, E.; Moustaki, M.; Kyriakopoulos, M.; Kapogiannis, D.; Sarafoglou, S.; Fretzagias, A.; Kalapothaki, V. High rates of antibiotic resistance among normal fecal flora Escherichia coli isolates in children from Greece. Clin. Microbiol. Infect. 1998, 4, 563–569. [Google Scholar]
- Kalter, H.D.; Gilman, R.H.; Moulton, L.H.; Cullotta, A.R.; Cabrera, L.; Velapatino, B. Risk factors for antibiotic-resistant Escherichia coli carriage in young children in Peru: Community-based cross-sectional prevalence study. Am. J. Trop. Med. Hyg. 2010, 82, 879–888. [Google Scholar]
- Howard, A.J.; Magee, J.T.; Fitzgerald, K.A.; Dunstan, F.D. Factors associated with antibiotic resistance in coliform organisms from community urinary tract infection in Wales. J. Antimicrob. Chemother. 2001, 47, 305–313. [Google Scholar]
- Teuber, M. Veterinary use and antibiotic resistance. Curr. Opin. Microbiol. 2001, 4, 493–499. [Google Scholar]
- Sawant, A.A.; Hegde, N.V.; Straley, B.A.; Donaldson, S.C.; Love, B.C.; Knabel, S.J.; Jayarao, B.M. Antimicrobial-resistant enteric bacteria from dairy cattle. Appl. Environ. Microbiol. 2007, 73, 156–163. [Google Scholar]
- Ding, C.; He, J. Effect of antibiotics in the environment on microbial populations. Appl. Microbiol. Biotechnol. 2010, 87, 925–941. [Google Scholar]
- Ibekwe, A.M.; Murinda, S.E.; Graves, A.K. Genetic diversity and antimicrobial resistance of Escherichia coli from human and animal sources uncovers multiple resistances from human sources. PLoS One 2011, 6, e20819. [Google Scholar]
- Gullberg, E.; Cao, S.; Berg, O.G.; Ilback, C.; Sandegren, L.; Hughes, D.; Andersson, D.I. Selection of resistant bacteria at very low antibiotic concentrations. PLoS Pathog. 2011, 7, e1002158. [Google Scholar]
- Graves, A.K.; Hagedorn, C.; Brooks, A.; Hagedorn, R.L.; Martin, E. Microbial source tracking in a rural watershed dominated by cattle. Water Res. 2007, 41, 3729–3739. [Google Scholar]
- Patoli, A.A.; Patoli, B.B.; Mehraj, V. High Prevalence of Multi-drug Resistant Escherichia coli in Drinking Water Samples from Hyderabad. Gomal J. Med. Sci. 2010, 8, 23–26. [Google Scholar]
- Cabral, J.P. Water microbiology. Bacterial pathogens and water. Int. J. Environ. Res. Public Health 2010, 7, 3657–3703. [Google Scholar] [CrossRef]
- Diwan, V.; Tamhankar, A.J.; Khandal, R.K.; Sen, S.; Aggarwal, M.; Marothi, Y.; Iyer, R.V.; Sundblad-Tonderski, K.; Stalsby-Lundborg, C. Antibiotics and antibiotic-resistant bacteria in waters associated with a hospital in Ujjain, India. BMC Public Health 2010, 10, 414. [Google Scholar]
- Parveen, S.; Lukasik, J.; Scott, T.M.; Tamplin, M.L.; Portier, K.M.; Sheperd, S.; Braun, K.; Farrah, S.R. Geographical variation in antibiotic resistance profiles of Escherichia coli isolated from swine, poultry, beef and dairy cattle farm water retention ponds in Florida. J. Appl. Microbiol. 2006, 100, 50–57. [Google Scholar]
- Perez-Trallero, E.; Garcia-de-la-Fuente, C.; Garcia-Rey, C.; Baquero, F.; Aguilar, L.; Dal-Re, R.; Garcia-de-Lomas, J. Geographical and ecological analysis of resistance, coresistance, and coupled resistance to antimicrobials in respiratory pathogenic bacteria in Spain. Antimicrob. Agents Chemother. 2005, 49, 1965–1972. [Google Scholar]
- Parveen, S.; Murphree, R.L.; Edmiston, L.; Kaspar, C.W.; Portier, K.M.; Tamplin, M.L. Association of multiple-antibiotic-resistance profiles with point and nonpoint sources of Escherichia coli in Apalachicola Bay. Appl. Environ. Microbiol. 1997, 63, 2607–2612. [Google Scholar]
- Shanahan, P.M.; Wylie, B.A.; Adrian, P.V.; Koornhof, H.J.; Thomson, C.J.; Amyes, S.G. The prevalence of antimicrobial resistance in human faecal flora in South Africa. Epidemiol. Infect. 1993, 111, 221–228. [Google Scholar]
- Nys, S.; Okeke, I.N.; Kariuki, S.; Dinant, G.J.; Driessen, C.; Stobberingh, E.E. Antibiotic resistance of faecal Escherichia coli from healthy volunteers from eight developing countries. J. Antimicrob. Chemother. 2004, 54, 952–955. [Google Scholar]
- Sahoo, K.C.; Tamhankar, A.J.; Johansson, E.; Stalsby-Lundborg, C. Antibiotic use, resistance development and environmental factors: A qualitative study among healthcare professionals in Orissa, India. BMC Public Health 2010, 10, 629. [Google Scholar]
- Davidson, R.J.; Davis, I.; Willey, B.M.; Rizg, K.; Bolotin, S.; Porter, V.; Polsky, J.; Daneman, N.; McGeer, A.; Yang, P.; et al. Antimalarial therapy selection for quinolone resistance among Escherichia coli in the absence of quinolone exposure, in tropical South America. PLoS One 2008, 3, e2727. [Google Scholar]
- Summers, A.O. Genetic linkage and horizontal gene transfer, the roots of the antibiotic multi-resistance problem. Anim. Biotechnol. 2006, 17, 125–135. [Google Scholar]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Sahoo, K.C.; Tamhankar, A.J.; Sahoo, S.; Sahu, P.S.; Klintz, S.R.; Lundborg, C.S. Geographical Variation in Antibiotic-Resistant Escherichia coli Isolates from Stool, Cow-Dung and Drinking Water. Int. J. Environ. Res. Public Health 2012, 9, 746-759. https://doi.org/10.3390/ijerph9030746
Sahoo KC, Tamhankar AJ, Sahoo S, Sahu PS, Klintz SR, Lundborg CS. Geographical Variation in Antibiotic-Resistant Escherichia coli Isolates from Stool, Cow-Dung and Drinking Water. International Journal of Environmental Research and Public Health. 2012; 9(3):746-759. https://doi.org/10.3390/ijerph9030746
Chicago/Turabian StyleSahoo, Krushna Chandra, Ashok J. Tamhankar, Soumyakanta Sahoo, Priyadarshi Soumyaranjan Sahu, Senia Rosales Klintz, and Cecilia Stålsby Lundborg. 2012. "Geographical Variation in Antibiotic-Resistant Escherichia coli Isolates from Stool, Cow-Dung and Drinking Water" International Journal of Environmental Research and Public Health 9, no. 3: 746-759. https://doi.org/10.3390/ijerph9030746





