Validity of Self-Reported Weight and Height of Adolescents, Its Impact on Classification into BMI-Categories and the Association with Weighing Behaviour
Abstract
:1. Introduction
2. Methods
2.1. Study Population
2.2. Questionnaire and Self-Reported Anthropometry
2.3. Anthropometric Measurements
2.4. Procedures
2.5. Statistical Analysis
3. Results
3.1. Study Population
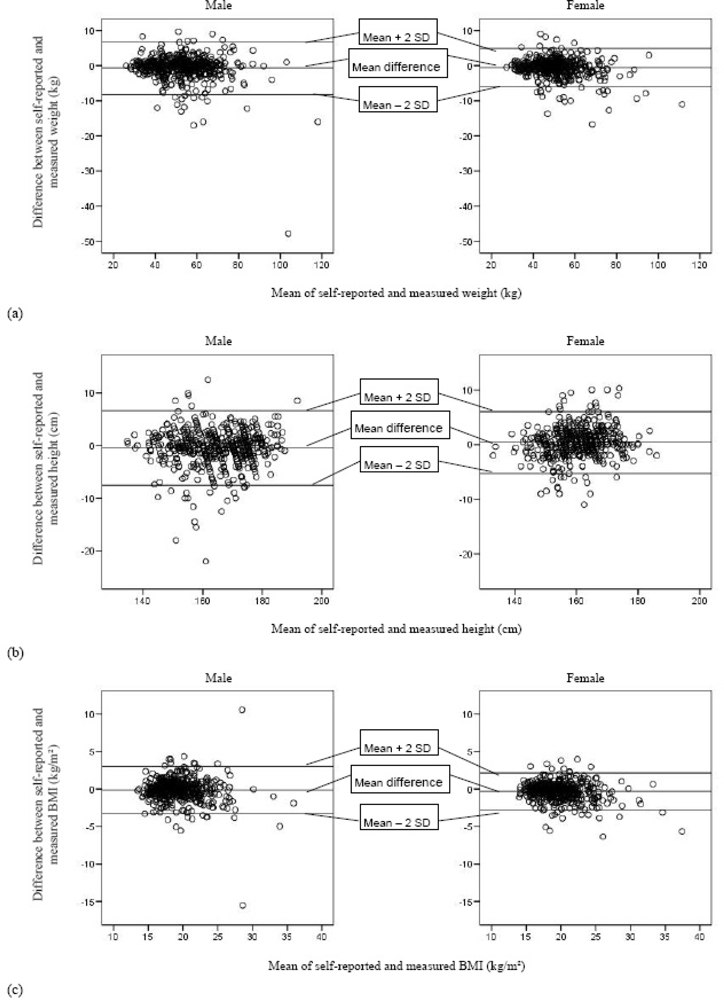
3.2. Agreement between Self-Reported and Measured Weight, Height and BMI
3.3. Impact of Self-Reported Height and Weight on Classification in BMI-Categories
3.4. Possible Factors Associated with Bias in Self-Reported Weight, Height and BMI
4. Discussion
4.1. Principal Findings and Comparison with Previous Studies
4.2. Strengths and Limitations
5. Conclusions
Acknowledgments
References and Notes
- Lobstein, T; Baur, L; Uauy, R. Obesity in children and young people: a crisis in public health. Obes. Rev 2004, 5, 4–85. [Google Scholar]
- Nieto-Garcia, FJ; Bush, TL; Keyl, PM. Body mass definitions of obesity: sensitivity and specificity using self-reported weight and height. Epidemiology 1990, 1, 146–152. [Google Scholar]
- Spencer, EA; Appleby, PN; Davey, GK; Key, TJ. Validity of self-reported height and weight in 4808 EPIC-Oxford participants. Public Health Nutr 2002, 5, 561–565. [Google Scholar]
- Niedhammer, I; Bugel, I; Bonenfant, S; Goldberg, M; Leclerc, A. Validity of self-reported weight and height in the French GAZEL cohort. Int. J. Obes 2000, 24, 1111–1118. [Google Scholar]
- World Health Organization Study Group on Young People and “Health for All by the Year 2000”. In Young People’s Health—A Challenge for Society; World Health Organization: Geneva, Switzerland, 1986.
- Strauss, RS. Comparison of measured and self-reported weight and height in a cross-sectional sample of young adolescents. Int. J. Obes 1999, 23, 904–908. [Google Scholar]
- Brener, ND; McManus, T; Galuska, DA; Lowry, R; Wechsler, H. Reliability and validity of self-reported height and weight among high school students. J. Adolesc. Health 2003, 32, 281–287. [Google Scholar]
- Elgar, FJ; Roberts, C; Tudor-Smith, C; Moore, L. Validity of self-reported height and weight and predictors of bias in adolescents. J. Adolesc. Health 2005, 37, 371–375. [Google Scholar]
- Tsigilis, N. Can secondary school students’ self-reported measures of height and weight be trusted? An effect size approach. Eur. J. Public Health 2006, 16, 532–535. [Google Scholar]
- Morrissey, SL; Whetstone, LM; Cummings, DM; Owen, LJ. Comparison of self-reported and measured height and weight in eighth-grade students. J. Sch. Health 2006, 76, 512–515. [Google Scholar]
- Tokmakidis, SP; Christodoulos, AD; Mantzouranis, NI. Validity of self-reported anthropometric values used to assess body mass index and estimate obesity in Greek school children. J. Adolesc. Health 2007, 40, 305–310. [Google Scholar]
- Goodman, E; Hinden, BR; Khandelwal, S. Accuracy of teen and parental reports of obesity and body mass index. Pediatrics 2000, 106, 52–58. [Google Scholar]
- Himes, JH; Hannan, P; Wall, M; Neumark-Sztainer, D. Factors associated with errors in self-reports of stature, weight and body mass index in Minnesota adolescents. Ann. Epidemiol 2005, 15, 272–278. [Google Scholar]
- Wang, ZM; Patterson, CM. A comparison of self-reported and measured height, weight and BMI in Australian adolescents. Aust. N. Z. J. Public Health 2002, 26, 473–478. [Google Scholar]
- Abalkhail, BA; Shawky, S; Soliman, NK. Validity of self-reported weight and height among Saudi school children and adolescents. Saudi Med. J 2002, 23, 831–837. [Google Scholar]
- Abraham, S; Luscombe, G; Boyd, C; Olesen, I. Predictors of the accuracy of self-reported height and weight in adolescent female school students. Int. J. Eat. Disord 2004, 36, 76–82. [Google Scholar]
- Danubio, ME; Miranda, G; Vinciguerra, MG; Vecchi, E; Rufo, F. Comparison of self-reported and measured height and weight: implications for obesity research among young adults. Econ. Hum. Biol 2008, 6, 181–190. [Google Scholar]
- Rosner, B. Fundamentals of Biostatistics, 5th ed; Duxbury Press: Forest Lodge Road Pacific Grove, CA, USA, 2000; p. 309. [Google Scholar]
- Ministry of Flanders and Education Department. CLB: Centrum voor Leerlingenbegeleiding. 2008.
- Laboratorium voor Antropogenetica, Vrije Universiteit Brussel. Growth Charts, Flanders. 2004.
- Cole, TJ; Bellizzi, MC; Flegal, KM; Dietz, WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. Brit. Med. J 2000, 320, 1240–1243. [Google Scholar]
- Cole, TJ; Flegal, KM; Nicholls, D; Jackson, AA. Body mass index cut offs to define thinness in children and adolescents: international survey. Brit. Med. J 2007, 335, 194. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed; Lawrence Earlbaum Associates: Hillsdale, NJ, USA, 1988; pp. 20–26. [Google Scholar]
- McGraw, KO; Wong, SP. Forming inferences about some intraclass correlation coefficients. Psychol. Methods 1996, 1, 30–46. [Google Scholar]
- Bland, JM; Altman, DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986, 327, 307–310. [Google Scholar]
- Agresti, A. Categorical Data Analysis, 2nd ed; Wiley: New York, NY, USA, 2002; pp. 410–414. [Google Scholar]
- Cohen, JA. A coefficient of agreement for nominal scales. Educ. Psychol. Meas 1960, 20, 37–46. [Google Scholar]
- Altman, DG. Practical Statistics for Medical Research; Chapman & Hall: London, UK, 1991; pp. 403–409. [Google Scholar]
- Altman, DG; Bland, JM. Statistics notes: diagnostic tests 1: sensitivity and specificity. Brit. Med. J 1994, 308, 1552. [Google Scholar]
- Altman, DG; Bland, JM. Statistics notes: diagnostic tests 2: predictive values. Brit. Med. J 1994, 309, 102. [Google Scholar]
- Sherry, B; Jefferds, ME; Grummer-Strawn, LM. Accuracy of adolescents self-report of height and weight in assessing overweight status: a literature review. Arch. Pediatr. Adolesc. Med 2007, 161, 1154–1161. [Google Scholar]
| Self-reported | Measured | Difference in Mean | Pb | dc | ||||
|---|---|---|---|---|---|---|---|---|
| Mean (SD) | Mean (SD) | (95% CI)a | ||||||
| Girls (n = 475) | ||||||||
| Weight (kg) | 50.9 | (10.8) | 51.5 | (11.4) | −0.60 | (−0.85 to −0.36) | <0.001 | 0.05 |
| Height (cm) | 160.9 | (8.7) | 160.5 | (8.2) | 0.38 | (0.13 to 0.64) | 0.004 | 0.05 |
| BMI (kg/m2) | 19.5 | (3.1) | 19.9 | (3.4) | −0.32 | (−0.43 to −0.20) | <0.001 | 0.12 |
| Boys (n = 507) | ||||||||
| Weight (kg) | 52.6 | (12.5) | 53.3 | (13.2) | −0.67 | (−1.00 to −0.34) | <0.001 | 0.06 |
| Height (cm) | 164.1 | (11.2) | 164.6 | (11.1) | −0.47 | (−0.78 to −0.16) | 0.003 | 0.05 |
| BMI (kg/m2) | 19.3 | (3.0) | 19.4 | (3.2) | −0.12 | (−0.25 to 0.02) | 0.098 | 0.03 |
| Self-reported | Measured | Differencea | Pb | ||||
|---|---|---|---|---|---|---|---|
| % (n) | % (n) | % (95% CI) | |||||
| Underweight (Nat. Class.) | 9.3 | (91) | 7.4 | (73) | 1.83 | (0.12 to 3.55) | 0.048 |
| Underweight (Int. Class.) | 10.1 | (99) | 7.9 | (78) | 2.14 | (0.35 to 3.93) | 0.026 |
| Normal weight (Nat. Class.) | 77.9 | (765) | 78.1 | (767) | −0.20 | (−2.46 to 2.05) | 0.930 |
| Normal weight (Int. Class.) | 77.5 | (761) | 76.8 | (754) | 0.71 | (−1.72 to 3.15) | 0.623 |
| Overweight (Nat. Class.) | 11.6 | (114) | 12.8 | (126) | −1.22 | (−2.71 to 0.27) | 0.142 |
| Overweight (Int. Class.) | 11.2 | (110) | 13.2 | (130) | −2.04 | (−3.73 to −0.35) | 0.025 |
| Obese (Nat. Class.) | 1.2 | (12) | 1.6 | (16) | −0.41 | (−.97 to 0.16) | 0.289 |
| Obese (Int. Class.) | 1.2 | (12) | 2.0 | (20) | −0.82 | (−1.44 to −0.19) | 0.021 |
| a) National classification cut-off values | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| BMI-category based on MEASURED BMI | Total n (%) | ||||||||||
| Underweight n (%) | Normal weight n (%) | Overweight n (%) | Obese n (%) | ||||||||
| BMI-category based on SELF-REPORTED BMI | Underweight | 45 | (4.6) | 46 | (4.7) | 0 | (0.0) | 0 | (0.0) | 91 | (9.3) |
| Normal weight | 28 | (2.9) | 702 | (71.5) | 33 | (3.4) | 2 | (0.2) | 765 | (77.9) | |
| Overweight | 0 | (0.0) | 18 | (1.8) | 92 | (9.4) | 4 | (0.4) | 114 | (11.6) | |
| Obese | 0 | (0.0) | 1 | (0.1) | 1 | (0.1) | 10 | (1.0) | 12 | (1.2) | |
| Total | 73 | (7.4) | 767 | (78.1) | 126 | (12.8) | 16 | (1.6) | 982 | (100) | |
| b) International classification cut-off values | |||||||||||
| BMI-category based on MEASURED BMI | Total n (%) | ||||||||||
| Underweight n (%) | Normal weight n (%) | Overweight n (%) | Obese n (%) | ||||||||
| BMI-category based on SELF-REPORTED BMI | Underweight | 48 | (4.9) | 51 | (5.2) | 0 | (0.0) | 0 | (0.0) | 99 | (10.1) |
| Normal weight | 30 | (3.1) | 683 | (69.6) | 46 | (4.7) | 2 | (0.2) | 761 | (77.5) | |
| Overweight | 0 | (0.0) | 19 | (1.9) | 84 | (8.6) | 7 | (0.7) | 110 | (11.2) | |
| Obese | 0 | (0.0) | 1 | (0.1) | 0 | (0.0) | 11 | (1.1) | 12 | (1.2) | |
| Total | 78 | (7.9) | 754 | (76.8) | 130 | (13.2) | 20 | (2.0) | 982 | (100) | |
| Sensitivity | Specificity | PPVa | NPVb | Kappa statistic | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| BMI categorie | % | (95% CI) | % | (95% CI) | % | (95% CI) | % | (95% CI) | κ | (95% CI) | |
| National classification [20] | |||||||||||
| Underweight | 61.6 | (50.2 to 72.0) | 94.9 | (93.3 to 96.2) | 49.5 | (38.3 to 60.7) | 96.9 | (95.5 to 97.8) | 0.51 | (0.36 to 0.66) | |
| Overweight | 73.0 | (64.7 to 80.0) | 97.4 | (96.1 to 98.3) | 80.7 | (72.9 to 86.6) | 96.1 | (94.6 to 97.2) | 0.73 | (0.61 to 0.85) | |
| Obese | 62.5 | (38.6 to 81.5) | 99.8 | (99.3 to 99.9) | 83.3 | (59.3 to 94.5) | 99.4 | (98.7 to 99.7) | 0.71 | (0.34 to 1.00) | |
| International classification [21,22] | |||||||||||
| Underweight | 61.5 | (50.4 to 71.6) | 94.4 | (92.7 to 95.7) | 48.5 | (37.8 to 59.4) | 96.6 | (95.2 to 97.6) | 0.50 | (0.36 to 0.64) | |
| Overweight | 64.6 | (56.1 to 72.3) | 97.0 | (95.6 to 97.9) | 76.4 | (68.4 to 82.8) | 94.7 | (93.0 to 96.0) | 0.66 | (0.54 to 0.78) | |
| Obese | 55.0 | (34.2 to 74.2) | 99.9 | (99.4 to 99.9) | 91.7 | (72.0 to 97.9) | 99.1 | (98.2 to 99.5) | 0.68 | (0.34 to 1.00) | |
| Difference in BMIa | Pb | ||
|---|---|---|---|
| Characteristic | Mean | (SD) | |
| Total | − 0.75 | (6.66) | |
| Gender | 0.014 | ||
| Male | −0.24 | (7.27) | |
| Female | −1.29 | (5.89) | |
| Age | 0.656 | ||
| 10–12 yrs | −0.68 | (6.85) | |
| 13–18 yrs | −0.89 | (6.24) | |
| Educational level | 0.058 | ||
| Secondary grammar or art school | −0.60 | (6.36) | |
| Technical or vocational training | −1.62 | (6.95) | |
| Self weighed during the past year | 0.122 | ||
| Yes | −1.48 | (9.46) | |
| No | −0.61 | (5.92) | |
| Balance at home | 0.968 | ||
| Yes | −0.75 | (6.14) | |
| No | −0.72 | (9.36) | |
| Frequency of weighing | 0.033 | ||
| Daily | −1.34 | (5.71) | |
| Weekly | −0.09 | (4.77) | |
| Monthly | −1.69 | (6.01) | |
| Less than once a month | −0.45 | (7.70) | |
| Following a diet | 0.098 | ||
| Yes | −2.17 | (9.40) | |
| No | −0.67 | (6.65) | |
| Having a specific food pattern | 0.352 | ||
| Yes | −1.73 | (7.36) | |
| No | −0.71 | (6.63) | |
| STEP 1 | STEP 2 | STEP 3 | STEP 4 | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Variable | B | SE B | β | B | SE B | β | B | SE B | β | B | SE B | β |
| Gender | −1.06 | 0.42 | −0.082* | −1.06 | 0.42 | −0.082* | −1.05 | 0.42 | −0.081* | −1.09 | 0.42 | −0.084* |
| Age | −0.15 | 0.45 | −0.011 | −0.42 | 0.47 | −0.030 | −0.43 | 0.47 | −0.031 | |||
| Educational level | 1.15 | 0.56 | 0.069* | 1.09 | 0.56 | 0.066 | ||||||
| Weighing behaviour | 0.72 | 0.56 | −0.042 | |||||||||
| R2 change | 0.007* | 0.000 | 0.004* | 0.002 | ||||||||
© 2009 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
De Vriendt, T.; Huybrechts, I.; Ottevaere, C.; Van Trimpont, I.; De Henauw, S. Validity of Self-Reported Weight and Height of Adolescents, Its Impact on Classification into BMI-Categories and the Association with Weighing Behaviour. Int. J. Environ. Res. Public Health 2009, 6, 2696-2711. https://doi.org/10.3390/ijerph6102696
De Vriendt T, Huybrechts I, Ottevaere C, Van Trimpont I, De Henauw S. Validity of Self-Reported Weight and Height of Adolescents, Its Impact on Classification into BMI-Categories and the Association with Weighing Behaviour. International Journal of Environmental Research and Public Health. 2009; 6(10):2696-2711. https://doi.org/10.3390/ijerph6102696
Chicago/Turabian StyleDe Vriendt, Tineke, Inge Huybrechts, Charlene Ottevaere, Inge Van Trimpont, and Stefaan De Henauw. 2009. "Validity of Self-Reported Weight and Height of Adolescents, Its Impact on Classification into BMI-Categories and the Association with Weighing Behaviour" International Journal of Environmental Research and Public Health 6, no. 10: 2696-2711. https://doi.org/10.3390/ijerph6102696
APA StyleDe Vriendt, T., Huybrechts, I., Ottevaere, C., Van Trimpont, I., & De Henauw, S. (2009). Validity of Self-Reported Weight and Height of Adolescents, Its Impact on Classification into BMI-Categories and the Association with Weighing Behaviour. International Journal of Environmental Research and Public Health, 6(10), 2696-2711. https://doi.org/10.3390/ijerph6102696





