Nutrition Transition and Biocultural Determinants of Obesity among Cameroonian Migrants in Urban Cameroon and France
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Qualitative Study
2.2.1. Study Process
2.2.2. Sampling
2.3. Quantitative Survey
2.3.1. Study Process
2.3.2. Sampling
2.3.3. Perceptions of Corpulence
2.3.4. Food Frequency
2.3.5. Physical Activity
2.3.6. Anthropometry and Blood Pressure
2.4. Data Analysis
2.4.1. Qualitative Study
2.4.2. Quantitative Study
Migration Status
Dietary Intake
PCA and MCAs
Body Image
Physical Activity
Relationships between Beliefs, Practices and Body Weight
2.5. Ethics
3. Results
3.1. Qualitative Study
3.1.1. The Social Perceptions of Stoutness
- Man, rural area, king, thirties:“In principle, only notables can wear this kind of clothes, the njocho, it means: “the clothes of titan”. In lacam, after nine weeks of confinement, you have to be like this (very large corpulence). Every day, you must eat palm oil, they even anoint you with it. Concerning my weight, it made me change. Being well means being with your belly, the administrative belly. The Chief’s belly announces fertility for the village in the near future.”
- Man, rural area, notable/farmer, sixties:“Some women before marriage were undergoing an initiation ritual, the mezin. Women who cannot easily grow, too feeble, they were in competition for the mezin path. They ate to become fat. Once they enter mezin, they embalm themselves with palm oil as makeup. During two or three weeks, they bathe in oil, they eat a lot, nkui couscous, pistachio sauce, tarot yellow sauce, they coddle. Afterwards their corpulence has changed, they become plump. They gain respect after that, they are pretty. For a while, they do even more work in the fields.”
- Man, urban area, pupil, twenties:“I want to get to 70 kilos (1.63 m; 67.1 kg). When I will have more money, I want a belly. When you see the belly, here’s a boss! When the man has money and he hasn’t got a belly, people say that he does nothing with it.”
- Woman, urban Area, student, twenties:“For a woman, being overweight suggests that her husband takes good care of her, that he is comfortable, he has money.”
- Man, Paris area, night watchman, thirties:“I enrolled in a sports club yesterday for a year. So, the goal is to maintain fitness and refine a little bit my body. I know that doing sport over a year, I will lose at least four or five kilograms. But after that, I can no longer lose. Sports must be regular, at least two three times a week. I have a BMI of 25.5. Normal is between 18 and 25. Between 25 and 30, one is overweight, between 30 and 35, one is obese, etc. Here I have a BMI of 25.5. My BMI was even higher before the diet. Now, doing sport, I bring it down below 25. I know that in Africa, when you’re like I am, that’s fine. At home (in Cameroon), you are told: “If it is not the food that kills someone, it will be something else”. In Cameroon, I have even heard people telling me that I need to drink more beer because I do not have enough belly”.
3.1.2. Diet Perceptions and Practices
- Man, rural area, notable/farmer, sixties:“In traditional food, we eat taro, yams, corn couscous, but rarely fruits. In our tradition, we ate what was particularly good. Fruit like guava are food for children. A man of my age cannot eat it. But we ate vegetables; moreover, some of our traditional vegetables, they are not eaten today. At that time, there were no shortages, with agriculture, there was no famine. Historically, in the village, I have never known people who were hungry. Palm oil is the basis of our diet; without palm oil, people would panic. Palm oil is essential, everything is prepared with it. This is a good food, it gives strength everywhere.”
- Man, rural area, king, thirties:“The traditional oil is oil-based palm nuts. Today, concerning the industry, it is not the oil of the village anymore, it is not nutritious. So much has changed, it has blown all the vitamins. We bleached oil, after there is no more carotene. Traditionally, we did not fry the oil like that, we also did not fry vegetables constantly, they are boiled. We ate well, there is not even a concept to express “snack” in tradition, we only ate three times a day.”
- Man, Paris area, manager, thirties:“Since we introduced frozen chicken at home, things like that, and people eat because they think it’s quick, they directly have the “Western diseases”, those did not exist before, such as diabetes. All this is due to modern food. I have many friends, when I visit them at home, it is only modern food. So they are big, they are potbellied, there is the belly, they abnormally gain weight while I’m still frail. I see the difference. The food from the home country gives strength to the body, but it is not fattening because in fact it is healthy. In fact, there are less unnatural things in the diet that will be added to the body to swell it.”
- Woman, Paris area, housewife, fifties:“It bothers me! But fortunately, I started with my children from an early age, already little, giving them Cameroonian dishes. I am Cameroonian, so: “You need to eat Cameroonian dishes". They began to eat that a little, so that when they went to Cameroon, they do not really discover anything.”
- Man, Paris area, Paris area, handler, thirties:“Here, the real problem with food from the home country is the price. Home country foods are expensive. Frozen costs less.”
3.1.3. Physical Activity
- Woman, Paris area, housewife, sixties:“In fact, as we are too sedentary in our country, we do not practice sports. I’m talking about moms who are now in town, because our moms were physically active. They worked in the fields. So they did not have all these problems. But after people moved into town, the settlement and all that...”
- Woman, Paris area, housewife, sixties:“When I can, I walk. I would not take my car to buy bread as some people do. Sometimes, I go to the same post office five times a day by foot. I try to avoid the damage (of a sedentary lifestyle). There are some moments when we can do this. In winter, you cannot. The weather now is sad. At 3pm, it is already dark, we do not have the courage to go out.”
- Man, Paris area, handler, thirties:“I do not run anymore because there is not really enough time. Time is saturated by work at the store.”
3.2. Quantitative Survey
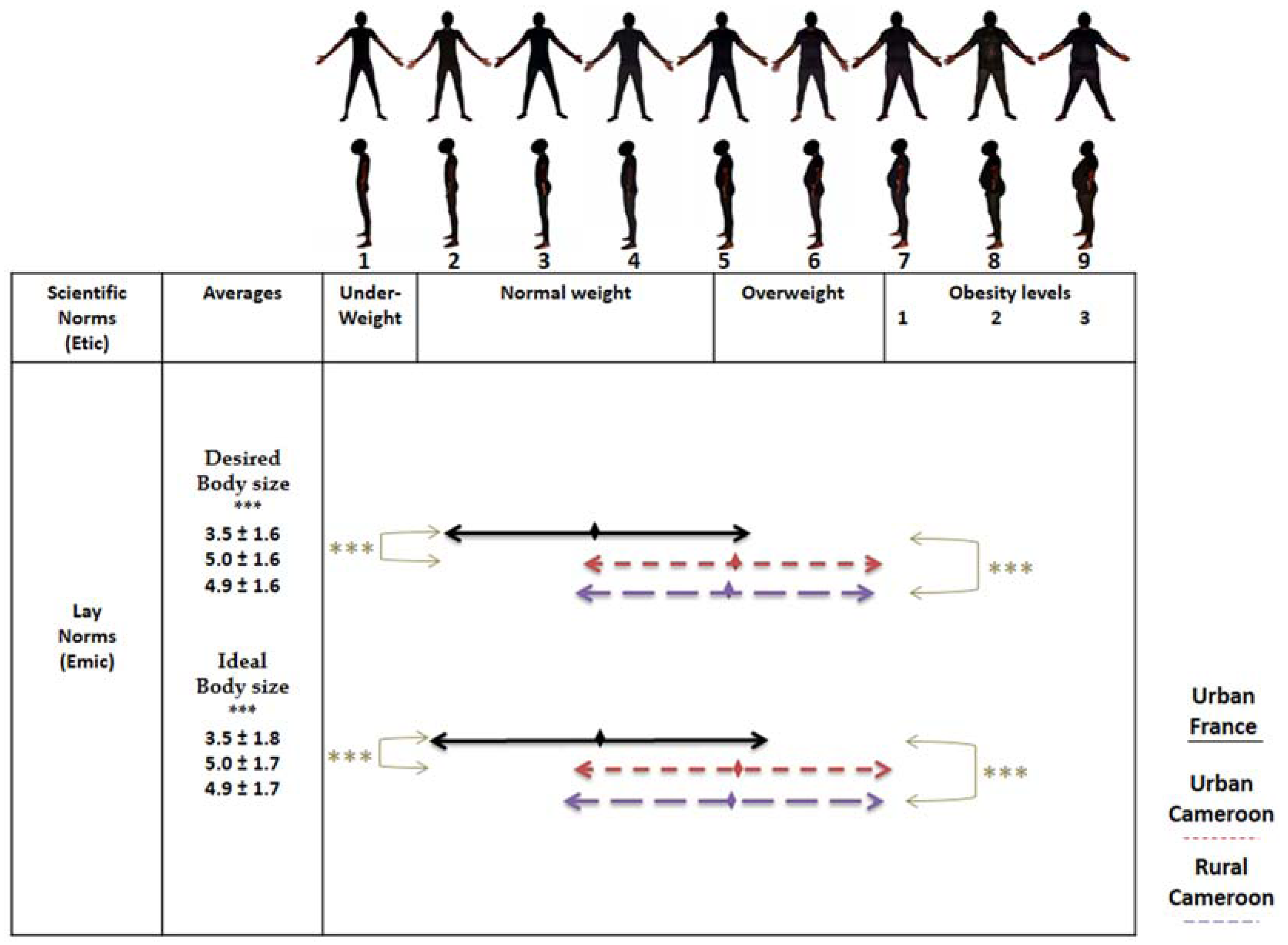
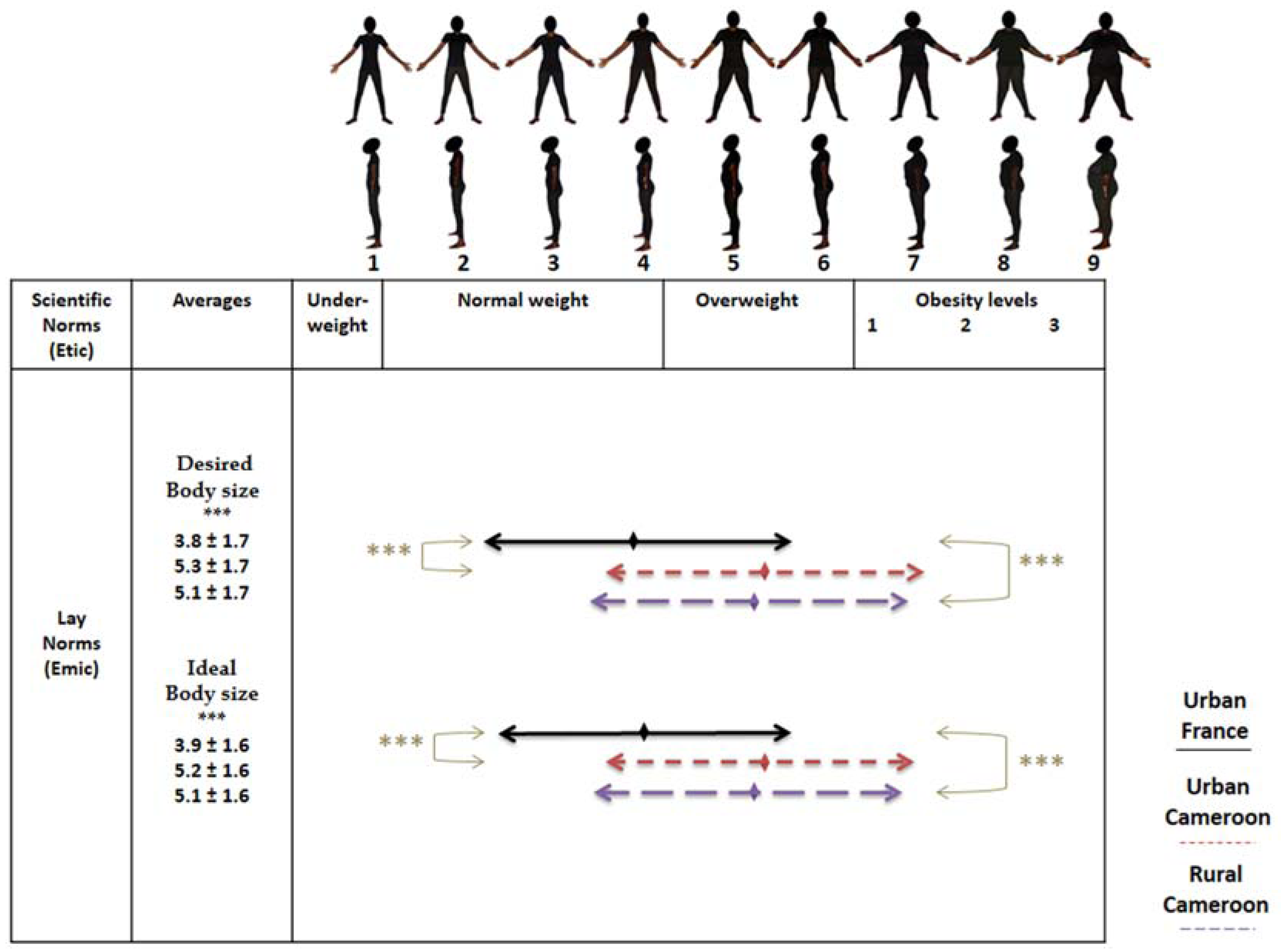
3.2.1. Perceptions of Corpulence
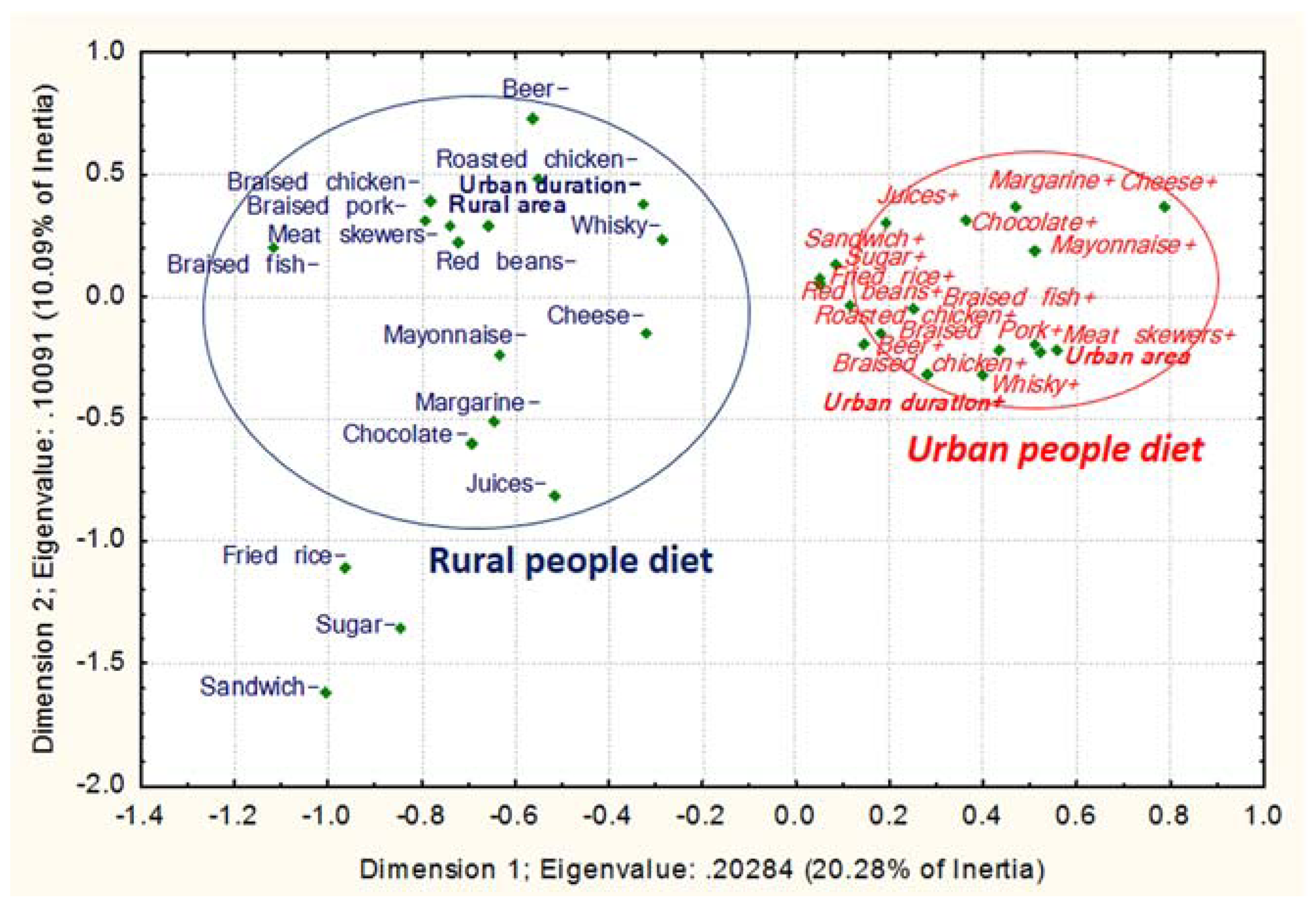
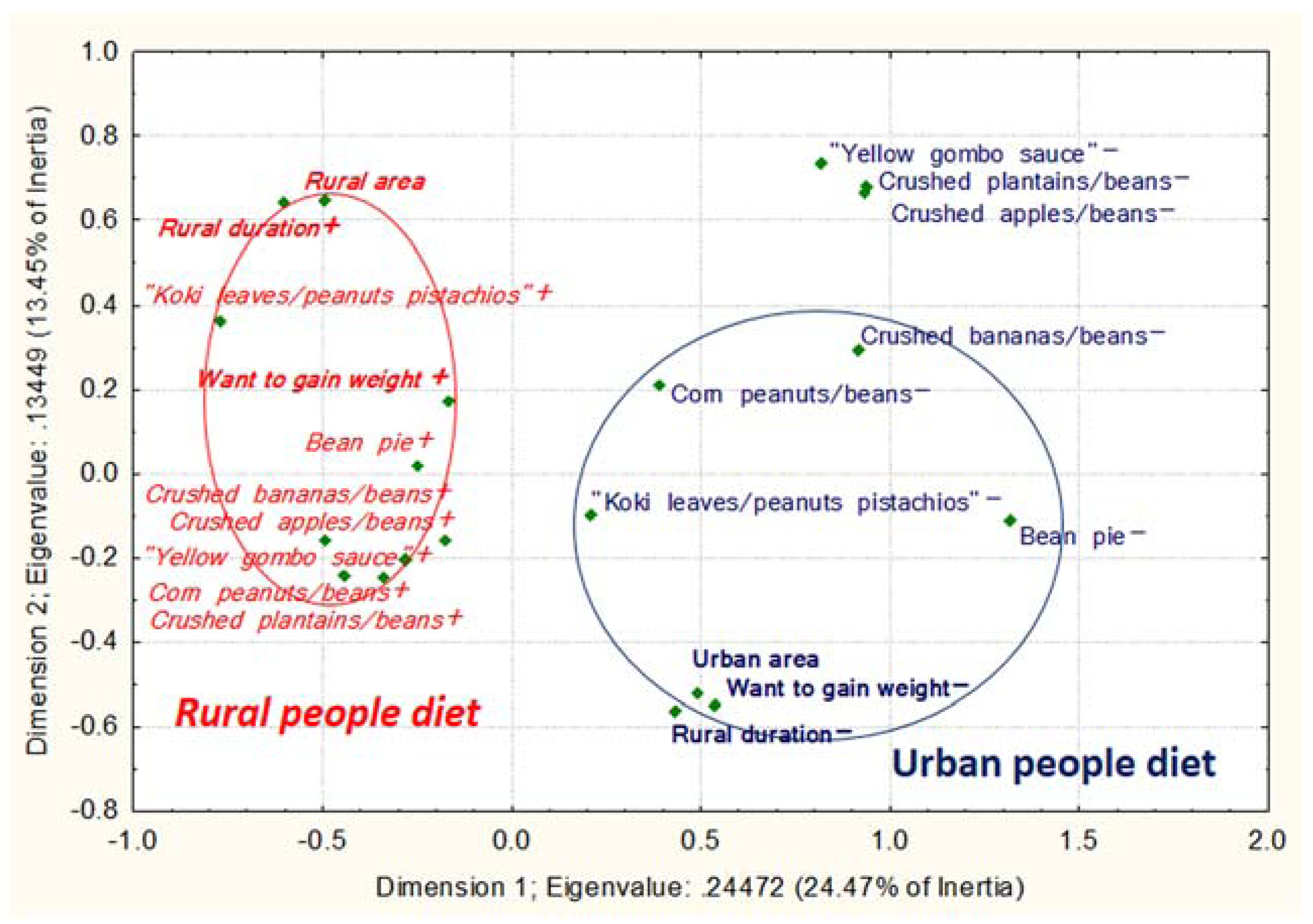
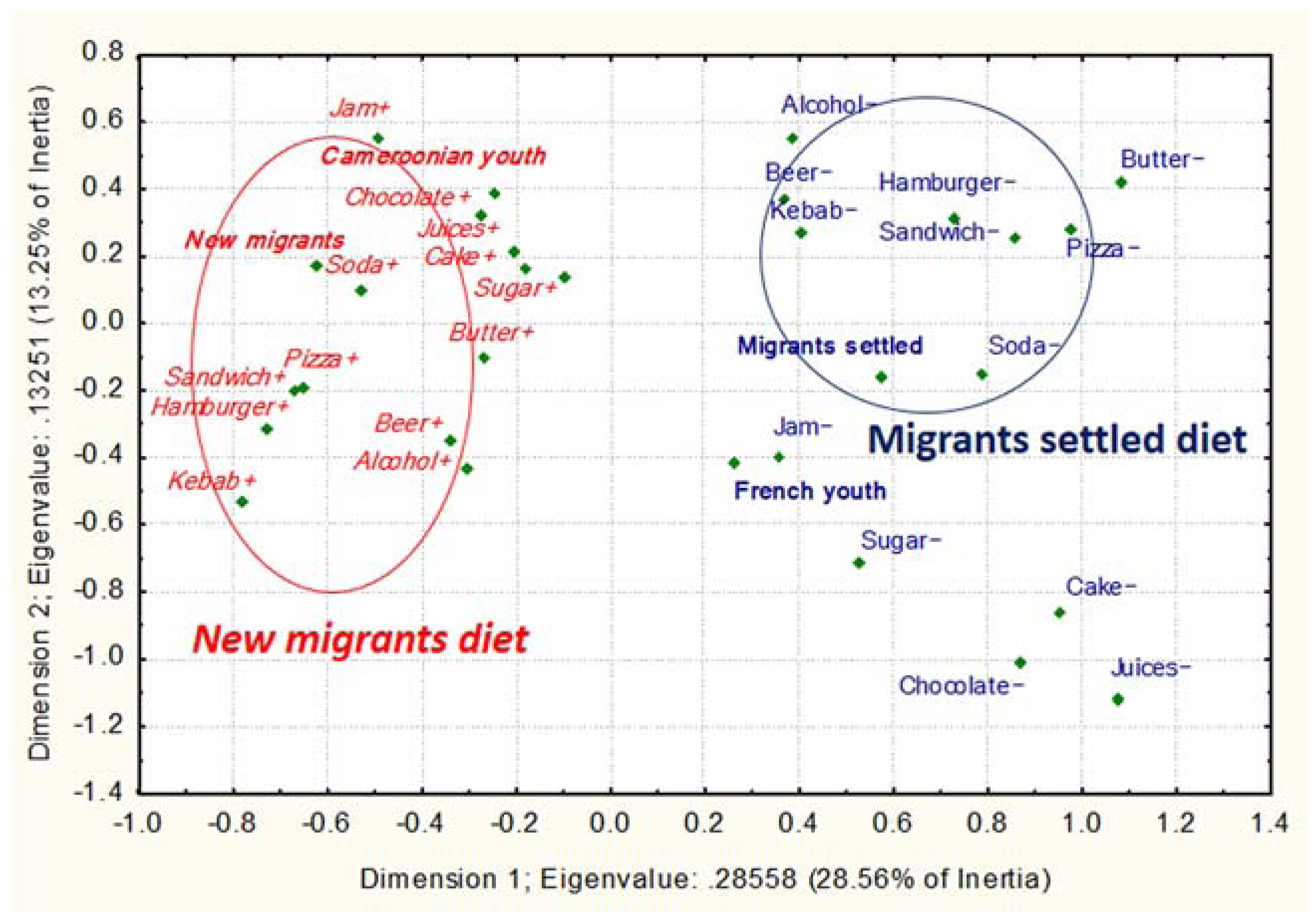
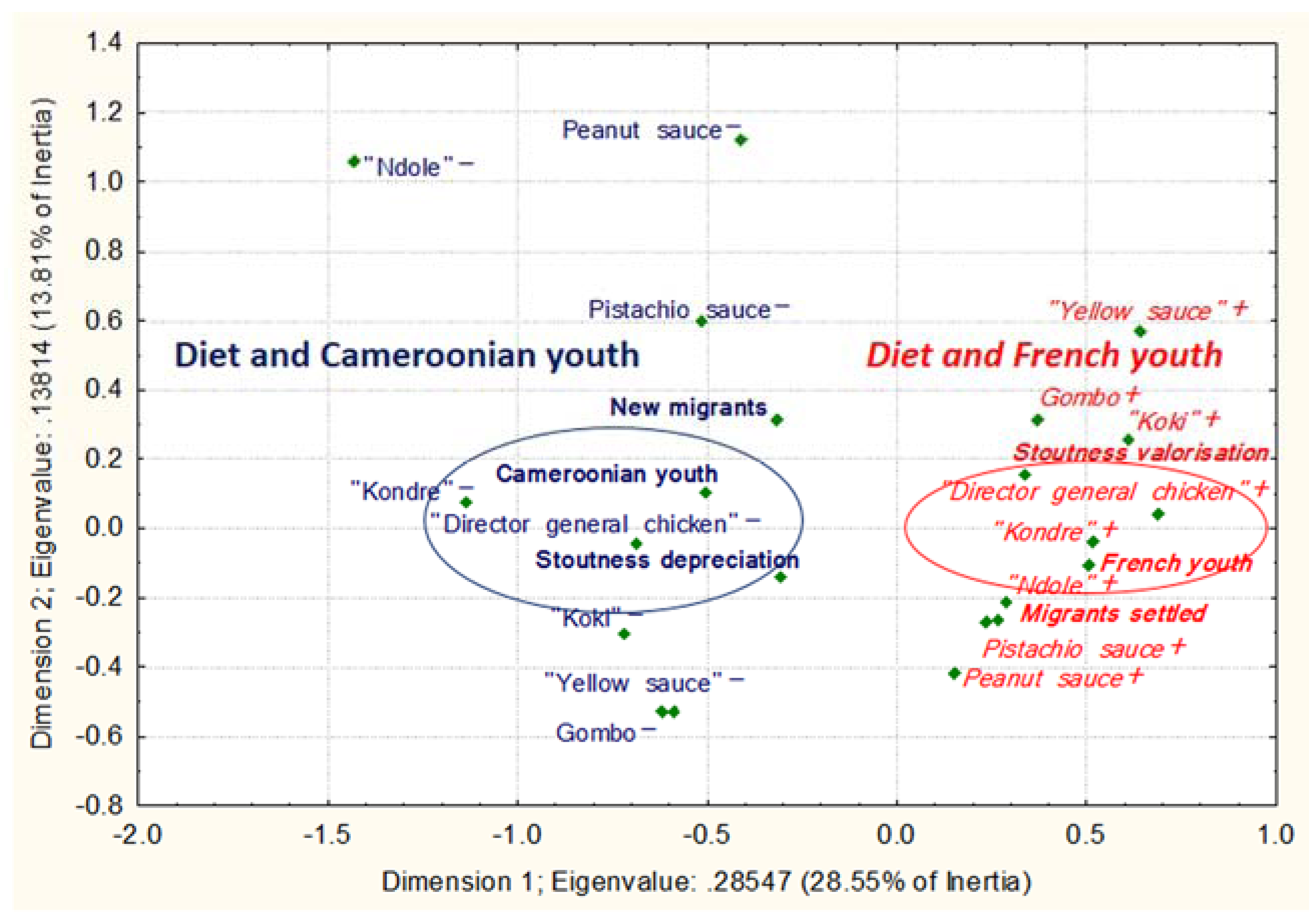
3.2.2. Dietary Intake
3.3. Physical Activity
3.4. Migration Status and Determinants of Obesity
3.5. Anthropometry and Blood Pressure
3.6. Analysis of Obesity Determinants
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contribution
Conflicts of Interest
References
- World Health Organization. Obesity: Preventing and Managing the Global Epidemic; WHO: Geneva, Switzerland, 2000. [Google Scholar]
- Popkin, B.M.; Adair, L.S.; Ng, S.W. Global nutrition transition and the pandemic of obesity in developing countries. Nutr. Rev. 2012, 70, 3–21. [Google Scholar] [CrossRef] [PubMed]
- Morris, K. UN raises priority of non-communicable diseases. Lancet 2010, 375, 1859. [Google Scholar] [CrossRef]
- Stevens, G.A.; Singh, G.M.; Lu, Y.; Danaei, G.; Lin, J.K.; Finucane, M.M.; Bahalim, A.N.; McIntire, R.K.; Gutierrez, H.R.; Cowan, M.; et al. Global burden of metabolic risk factors of chronic diseases collaborating group, national, regional, and global trends in adult overweight and obesity prevalences. Popul. Health Metr. 2012, 10, 22. [Google Scholar] [CrossRef] [PubMed]
- Cadot, E.; Lapostolle, A.; Spira, A. Déterminants socioéconomiques et contextuels de l’obésité. Rev. Epidemiol. Sante Publique 2008, 56, S377–S378. [Google Scholar] [CrossRef]
- Connor Gorber, S.; Tremblay, M.; Moher, D.; Gorber, B. A comparison of direct vs. self-report measures for assessing height, weight and body mass index: A systematic review. Obes. Rev. 2007, 8, 307–326. [Google Scholar] [CrossRef] [PubMed]
- Delpeuch, F.; Maire, B.; Monnier, E.; Holdsworth, M. Globesity: A Planet Out of Control? 2nd ed.; Routledge: London, UK, 2013; p. 201. [Google Scholar]
- Saarloos, D.; Kim, J.E.; Timmermans, H. The built environment and health: Introducing individual space-time behavior. Int. J. Environ. Res. Publ. Health 2009, 6, 1724–1743. [Google Scholar] [CrossRef] [PubMed]
- Downey, G. Being human in cities: Phenotypic bias from urban niche construction. Curr. Anthropol. 2016, 57, 52–64. [Google Scholar] [CrossRef]
- Ebrahim, S.; Pearce, N.; Smeeth, L.; Casas, J.P.; Jaffar, S.; Piot, P. Tackling non-communicable diseases in low- and middle-income countries: Is the evidence from high-income countries all we need? PLoS Med. 2013, 10, e1001377. [Google Scholar] [CrossRef] [PubMed]
- Ogden, C.L.; Carroll, M.D. Prevalence of overweight, obesity, and extreme obesity among adults: United States, trends 1960–1962 through 2007–2008. Natl. Cent. Health Stat. 2010, 6, 1–6. [Google Scholar]
- Jusot, F.; Silva, J.; Dourgnon, P.; Sermet, C. Etat de Santé des Populations Immigrées en France; IRDES: Paris, France, 2008. [Google Scholar]
- Danaei, G.; Finucane, M.M.; Lu, Y.; Singh, G.M.; Cowan, M.J.; Paciorek, C.J.; Lin, J.K.; Farzadfar, F.; Khang, Y.-H.; Stevens, G.A.; et al. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: Systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2·7 million participants. Lancet 2011, 378, 31–40. [Google Scholar] [CrossRef]
- Drewnowski, A. Obesity, diets, and social inequalities. Nutr. Rev. 2009, 67, S36–S39. [Google Scholar] [CrossRef] [PubMed]
- Sobal, J.; Stunkard, A.J. Socioeconomic status and obesity: A review of the literature. Psychol. Bull. 1989, 105, 260–275. [Google Scholar] [CrossRef] [PubMed]
- Temple, N.J.; Steyn, N.P. The cost of a healthy diet: A South African perspective. Nutrition 2011, 27, 505–508. [Google Scholar] [CrossRef] [PubMed]
- Corbeau, J.-P. L’imaginaire du gras associé à divers types de consommation de gras et les perceptions de leur qualités. In Agro-Alimentaire, Une Economie de la Qualité; Nicolas, F., Valceschini, E., Eds.; INRA-Economica: Paris, France, 1995; pp. 93–107. [Google Scholar]
- Agyemang, C.; Addo, J.; Bhopal, R.; Aikins Ade, G.; Stronks, K. Cardiovascular disease, diabetes and established risk factors among populations of sub-Saharan African descent in Europe: A literature review. Glob. Health 2009, 5, 7. [Google Scholar] [CrossRef] [PubMed]
- Cohen, E.; Boëtsch, G.; Palstra, F.P.; Pasquet, P. Social valorisation of stoutness as a determinant of obesity in the context of nutritional transition in Cameroon: The Bamileke case. Soc. Sci. Med. 2013, 96, 24–32. [Google Scholar] [CrossRef] [PubMed]
- De Garine, I. Adaptation biologique et bien-être psycho-culturel. Bull. Mém. Soc. Anthropol. Paris 1990, 2, 151–173. [Google Scholar] [CrossRef]
- Sear, R.; Marlowe, F.W. How universal are human mate choices? Size does not matter when Hadza foragers are choosing a mate. Biol. Lett. 2009, 5, 606–609. [Google Scholar] [CrossRef] [PubMed]
- Brown, P.J.; Konner, M. An anthropological perspective on obesity. Ann. N. Y. Acad. Sci. 1987, 499, 29–46. [Google Scholar] [CrossRef] [PubMed]
- Flynn, K.J.; Fitzgibbon, M. Body images and obesity risk among black females: A review of the literature. Ann. Behav. Med. 1998, 20, 13–24. [Google Scholar] [CrossRef] [PubMed]
- Krauss, R.C.; Powell, L.M.; Wada, R. Weight misperceptions and racial and ethnic disparities in adolescent female body mass index. J. Obes. 2012, 2012, 205393. [Google Scholar] [CrossRef] [PubMed]
- Rguibi, M.; Belahsen, R. Fattening practices among Moroccan Saharawi women. East. Mediterr. Health J. 2006, 12, 619–624. [Google Scholar] [PubMed]
- Renzaho, A.M.; McCabe, M.; Swinburn, B. Intergenerational differences in food, physical activity, and body size perceptions among African migrants. Qual. Health Res. 2012, 22, 740–754. [Google Scholar] [CrossRef] [PubMed]
- De Saint Pol, T. Surpoids, normes et jugements en matière de poids: Comparaisons européennes. Popul. Soc. 2009, 455, 1–4. [Google Scholar]
- Wluczka, M.; Debska, E. La Santé des Primo-Migrants en 2006; ANAEM: Paris, France, 2006. [Google Scholar]
- De Capèle, B.; Delourme, V.; Fabbro, S. L’alimentation des Africains vivant en France. Aliment. Précarité (CERIN) 2004, 24, 1–20. [Google Scholar]
- Eschwege, E.; Charles, M.-A.; Basdevant, A. ObEpi: Enquête Epidémiologique Nationale sur le Surpoids et L’obésité; Roche: Basel, Switzerland, 2012; p. 16. [Google Scholar]
- Ndoye, F.; Diop, A. Evolution des Styles Alimentaires à Dakar; ENDA-GRAF/CIRAD: Dakar, Senegal, 2001. [Google Scholar]
- Puoane, T.; Fourie, J.M.; Shapiro, M.; Rosling, L.; Tshaka, N.C.; Oelefse, A. “Big is beautiful”—An exploration with urban black community health workers in a South African township. S. Afr. J. Clin. Nutr. 2005, 18, 6–15. [Google Scholar] [CrossRef]
- Fezeu, L.K.; Assah, F.K.; Balkau, B.; Mbanya, D.S.; Kengne, A.P.; Awah, P.K.; Mbanya, J.C. Ten-year changes in central obesity and BMI in rural and urban Cameroon. Obesity (Silver Spring) 2008, 16, 1144–1147. [Google Scholar] [CrossRef] [PubMed]
- Pasquet, P.; Temgoua, L.S.; Melaman-Sego, F.; Froment, A.; Rikong-Adie, H. Prevalence of overweight and obesity for urban adults in Cameroon. Ann. Hum. Biol. 2003, 30, 551–562. [Google Scholar] [CrossRef] [PubMed]
- Cavelier, C.; Le Berre, S. Études Relatives au Poids de Naissance Chez L’enfant Noir de Yaounde; ORSTOM: Yaoundé, Cameroon, 1969; p. 77. [Google Scholar]
- Bouly De Lesdain, S. Femmes Camerounaises en Région Parisienne: Trajectoires Migratoires et Réseaux D’approvisionnement; L’Harmattan: Paris, France, 1999. [Google Scholar]
- De Saint Pol, T. Obésité et milieux sociaux en France: Les inégalités augmentent. Bull. Epidémiol. AFSSA 2008, 20, 175–179. [Google Scholar]
- Brewis, A.A. Obesity: Cultural and Biocultural Perspectives; Rutgers University Press: New Brunswick, NJ, USA, 2011. [Google Scholar]
- Mvo, Z.; Dick, J.; Steyn, K. Perceptions of overweight African women about acceptable body size of women and children. Curationis 1999, 22, 27–31. [Google Scholar] [CrossRef] [PubMed]
- Berry, J.W. Immigration, acculturation, and adaptation. Appl. Psychol. 1997, 46, 5–34. [Google Scholar] [CrossRef]
- Copans, J. L’enquête et Ses Méthodes: L’enquête Ethnologique de Terrain; Armand Colin: Paris, France, 2008. [Google Scholar]
- Cohen, E.; Bernard, J.Y.; Ponty, A.; Ndao, A.; Amougou, N.; Said-Mohamed, R.; Pasquet, P. Development and validation of the body size scale for assessing body weight perception in African populations. PLoS ONE 2015, 10, e0138983. [Google Scholar] [CrossRef] [PubMed]
- Williamson, D.A.; Womble, L.G.; Zucker, N.L.; Reas, D.L.; White, M.A.; Blouin, D.C.; Greenway, F. Body image assessment for obesity (BIA-O): Development of a new procedure. Int. J. Obes. Relat. Metab. Disord. 2000, 24, 1326–1332. [Google Scholar] [CrossRef] [PubMed]
- Cohen, E.; Pasquet, P. Development of a new body image assessment scale in urban Cameroon: An anthropological approach. Ethn. Dis. 2011, 21, 288–293. [Google Scholar] [PubMed]
- Warnier, J.-P. Régner au Cameroun: Le Roi-Pot; Karthala: Paris, France, 2009. [Google Scholar]
- Amougou, N.; Cohen, E.; Mbala, M.L.; Grosdidier, B.; Bernard, J.Y.; Said-Mohamed, R.; Pasquet, P. Development and validation of two food portion photograph books to assess dietary intake among adults and children in Central Africa. Br. J. Nutr. 2016, 115, 895–902. [Google Scholar] [CrossRef] [PubMed]
- Sheehy, T.; Kolahdooz, F.; Mtshali, T.L.; Khamis, T.; Sharma, S. Development of a quantitative food frequency questionnaire for use among rural South Africans in KwaZulu-Natal. J. Hum. Nutr. Diet. 2014, 27, 443–449. [Google Scholar] [CrossRef] [PubMed]
- Craig, C.L.; Marshall, A.L.; Sjostrom, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-Country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef] [PubMed]
- Padrao, P.; Damasceno, A.; Silva-Matos, C.; Prista, A.; Lunet, N. Physical activity patterns in Mozambique: Urban/rural differences during epidemiological transition. Prev. Med. 2012, 55, 444–449. [Google Scholar] [CrossRef] [PubMed]
- Weiner, J.S.; Lourie, J.A. Practical Human Biology; Academic Press: London, UK, 1981; p. 439. [Google Scholar]
- Mason, J. Qualitative Researching; SAGE: London, UK, 2002. [Google Scholar]
- Nzefa Dapi, L.; Nouedoui, C.; Janlert, U.; Håglin, L. Adolescents´ food habits and nutritional status in urban and rural areas in Cameroon, Africa. Scand. J. Nutr. 2005, 49, 151–158. [Google Scholar] [CrossRef]
- Sharma, S.; Mbanya, J.C.; Cruickshank, K.; Cade, J.; Tanya, A.K.; Cao, X.; Hurbos, M.; Wong, M.R. Nutritional composition of commonly consumed composite dishes from the Central Province of Cameroon. Int. J. Food Sci. Nutr. 2007, 58, 475–485. [Google Scholar] [CrossRef] [PubMed]
- FAO/WHO/UNU. Energy and Protein Requirements: Report of a Joint FAO/WHO/UNU Expert Consultation; World Health Organization (WHO): Geneva, Switzerland, 1985; p. 206. [Google Scholar]
- Siervo, M.; Grey, P.; Nyan, O.A.; Prentice, A.M. A pilot study on body image, attractiveness and body size in Gambians living in an urban community. Eat. Weight Disord. 2006, 11, 100–109. [Google Scholar] [CrossRef] [PubMed]
- Tillin, T.; Hughes, A.D.; Godsland, I.F.; Whincup, P.; Forouhi, N.G.; Welsh, P.; Sattar, N.; McKeigue, P.M.; Chaturvedi, N. Insulin resistance and truncal obesity as important determinants of the greater incidence of diabetes in Indian Asians and African Caribbeans compared with Europeans: The Southall and Brent REvisited (SABRE) cohort. Diabetes Care 2013, 36, 383–393. [Google Scholar] [CrossRef] [PubMed]
- Agyemang, C.; Meeks, K.; Beune, E.; Owusu-Dabo, E.; Mockenhaupt, F.P.; Addo, J.; Aikins, A.G.; Bahendeka, S.; Danquah, I.; Schulze, M.B.; et al. Obesity and type 2 diabetes in sub-Saharan Africans–Is the burden in today’s Africa similar to African migrants in Europe? The RODAM study. BMC Med. 2016, 14, 166. [Google Scholar] [CrossRef] [PubMed]
- Abrahams, Z.; McHiza, Z.; Steyn, N.P. Diet and mortality rates in Sub-Saharan Africa: Stages in the nutrition transition. BMC Public Health 2011, 11, 801. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, C.A.; Conde, W.L.; Lu, B.; Popkin, B.M. Obesity and inequities in health in the developing world. Int. J. Obes. Relat. Metab. Disord. 2004, 28, 1181–1186. [Google Scholar] [CrossRef] [PubMed]
- Bush, H.M.; Williams, R.G.; Lean, M.E.; Anderson, A.S. Body image and weight consciousness among South Asian, Italian and general population women in Britain. Appetite 2001, 37, 207–215. [Google Scholar] [CrossRef] [PubMed]
- Cachelin, F.M.; Rebeck, R.M.; Chung, G.H.; Pelayo, E. Does ethnicity influence body-size preference? A comparison of body image and body size. Obes. Res. 2002, 10, 158–166. [Google Scholar] [CrossRef] [PubMed]
- Nicolaou, M.; Doak, C.; Dam, R.V.; Hosper, K.; Seidell, J.; Stronks, K. Body size preference and body weight perception among two migrant groups of non-Western origin. Public Health Nutr. 2008, 11, 1332–1341. [Google Scholar] [CrossRef] [PubMed]
- Kiawi, E.; Edwards, R.; Shu, J.; Unwin, N.; Kamadjeu, R.; Mbanya, J.C. Knowledge, attitudes, and behavior relating to diabetes and its main risk factors among urban residents in Cameroon: A qualitative survey. Ethn. Dis. 2006, 16, 503–509. [Google Scholar] [PubMed]
- Pradelles de Latour, C.H. Le cycle bisannuel chez les Bamiléké. Syst. Pensée Afr. Noire 1986. [Google Scholar] [CrossRef]
- Neveu Kringelbach, H. Le poids du succès: Construction du corps, danse et carrière à Dakar. Politique Afr. 2007, 107, 81–101. [Google Scholar] [CrossRef]
- Kouebou, C.P.; Achu, M.; Nzali, S.; Chelea, M.; Bonglaisin, J.; Kamda, A.; Djiele, P.; Yadang, G.; Ponka, R.; Ngoh Newilah, G.; et al. A review of composition studies of Cameroon traditional dishes: Macronutrients and minerals. Food Chem. 2013, 140, 483–494. [Google Scholar] [CrossRef] [PubMed]
- Renzaho, A.M.N.; Burns, C. Post-migration food habits of sub-Saharan African migrants in Victoria: A cross-sectional study. Nutr. Diet. 2006, 63, 91–102. [Google Scholar] [CrossRef]
- Tuomainen, H.M. Ethnic identity, (post) colonialism and foodways: Ghanaians in London. Food Cult. Soc. 2009, 12, 525–554. [Google Scholar] [CrossRef]
- Brami, A. L’acculturation : Etude d’un Concept. Revue DEES 2000, 121, 54–63. [Google Scholar]
- Pillarella, S. 4.5 Acculturation alimentaire des immigrants récents de l’Afrique de l’Ouest francophone établis à Montréal: Une analyse écologique. In Médias et le Façonnement des Normes en Matière de Santé; Presses de l’Université du Québec: Québec City, QC, Canada, 2006; p. 235. [Google Scholar]
- Sodjinou, R.; Agueh, V.; Fayomi, B.; Delisle, H. Obesity and cardio-metabolic risk factors in urban adults of Benin: Relationship with socio-economic status, urbanisation, and lifestyle patterns. BMC Public Health 2008, 8, 84. [Google Scholar] [CrossRef] [PubMed]
- Schaefer, E.J.; Augustin, J.L.; Schaefer, M.M.; Rasmussen, H.; Ordovas, J.M.; Dallal, G.E.; Dwyer, J.T. Lack of efficacy of a food-frequency questionnaire in assessing dietary macronutrient intakes in subjects consuming diets of known composition. Am. J. Clin. Nutr. 2000, 71, 746–751. [Google Scholar] [PubMed]
- Evina, R.C. Migration au Cameroun: Profil National 2009; Organisation Internationale pour les Migrations: Grand-Saconnex, Switzerland, 2009. [Google Scholar]
- Kristiansen, M.; Mygind, A.; Krasnik, A. Health effects of migration. Dan. Med. Bull. 2007, 54, 46–47. [Google Scholar] [PubMed]
- Besharat Pour, M.; Bergstrom, A.; Bottai, M.; Kull, I.; Wickman, M.; Hakansson, N.; Wolk, A.; Moradi, T. Effect of parental migration background on childhood nutrition, physical activity, and body mass index. J. Obes. 2014, 2014, 406529. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.W.; Ames, D.; Lickel, B. Views from the inside and outside: Integrating emic and etic insights about culture and justice judgment. Acad. Manag. Rev. 1999, 24, 781–796. [Google Scholar]
- Hesse-Biber, S.; Leavy, P.; Quinn, C.E.; Zoino, J. The mass marketing of disordered eating and eating disorders: The social psychology of women, thinness and culture. Women’s Stud. Int. Forum 2006, 29, 208–224. [Google Scholar] [CrossRef]
- Appiah, C.A.; Otoo, G.E.; Steiner-Asiedu, M. Preferred body size in urban Ghanaian women: Implication on the overweight/obesity problem. Pan Afr. Med. J. 2016, 23, 239. [Google Scholar] [CrossRef]
- Frank, L.D.; Andresen, M.A.; Schmid, T.L. Obesity relationships with community design, physical activity, and time spent in cars. Am. J. Prev. Med. 2004, 27, 87–96. [Google Scholar] [CrossRef] [PubMed]
- Booth, G.L.; Creatore, M.I.; Moineddin, R.; Gozdyra, P.; Weyman, J.T.; Matheson, F.I.; Glazier, R.H. Unwalkable neighborhoods, poverty, and the risk of diabetes among recent immigrants to Canada compared with long-term residents. Diabetes Care 2013, 36, 302–308. [Google Scholar] [CrossRef] [PubMed]
- Lara, M.; Gamboa, C.; Kahramanian, M.I.; Morales, L.S.; Bautista, D.E. Acculturation and Latino health in the United States: A review of the literature and its sociopolitical context. Annu. Rev. Public Health 2005, 26, 367–397. [Google Scholar] [CrossRef] [PubMed]
- Vander Veen, D.F. Obesity, obesity health risks, resilience, and acculturation in black African immigrants. Int. J. Migr. Health Soc. Care 2015, 11, 179–193. [Google Scholar] [CrossRef]
- Ettarh, R.; Van de Vijver, S.; Oti, S.; Kyobutungi, C. Overweight, obesity, and perception of body image among slum residents in Nairobi, Kenya, 2008–2009. Prev. Chronic Dis. 2013, 10, 212. [Google Scholar] [CrossRef] [PubMed]
- Jacobus, M.V.; Jalali, R. Challenges to food access among Lewiston’s African immigrants. Maine Policy Rev. 2011, 20, 151–158. [Google Scholar]
- Delavari, M.; Farrelly, A.; Renzaho, A.; Mellor, D.; Swinburn, B. Experiences of migration and the determinants of obesity among recent Iranian immigrants in Victoria, Australia. Ethn. Health 2013, 18, 66–82. [Google Scholar] [CrossRef] [PubMed]
- Delavari, M.; Sonderlund, A.L.; Mellor, D.; Mohebbi, M.; Swinburn, B. Migration, acculturation and environment: Determinants of obesity among Iranian migrants in Australia. Int. J. Environ. Res. Public Health 2015, 12, 1083–1098. [Google Scholar] [CrossRef] [PubMed]
- Himmelgreen, D.A.; Perez-Escamilla, R.; Martinez, D.; Bretnall, A.; Eells, B.; Peng, Y.; Bermudez, A. The longer you stay, the bigger you get: Length of time and language use in the U.S. are associated with obesity in Puerto Rican women. Am. J. Phys. Anthropol. 2004, 125, 90–96. [Google Scholar] [CrossRef] [PubMed]
- Abraido-Lanza, A.F.; Armbrister, A.N.; Florez, K.R.; Aguirre, A.N. Toward a theory-driven model of acculturation in public health research. Am. J. Public Health 2006, 96, 1342–1346. [Google Scholar] [CrossRef] [PubMed]
| Investigation Areas | Rural Cameroon | Urban Cameroon | Urban France |
|---|---|---|---|
| Qualitative survey | |||
| Sample size, n | 12 | 12 | 12 |
| Sex, % men | 50 | 50 | 50 |
| Age, % (18–30) years | 50 | 50 | 50 |
| Location | Village of Diambou | Bamiléké neighbourhoods of the capital | Bamiléké migrant associations |
| Quantitative Survey | |||
| Sample size, n | 258 | 319 | 50 |
| Sex, % men | 48.8 | 43.9 | 56.0 |
| Age, Mean | 40.2 ± 15.6 | 37.3 ± 11.9 | 46.4 ± 11.8 |
| Location | Village of Diambou | Bamiléké neighbourhoods of the capital | Bamiléké migrant associations. Cultural events: weddings, baptisms, community celebrations. Cameroonian restaurants and at home |
| Migration Status | Higher-Calorie Diet | Physical Activity | Desired Body Size | |||
|---|---|---|---|---|---|---|
| Cameroonian migrants | ||||||
| Yaoundé living duration | p | p | p | |||
| 0 years | 23.2% (n = 19) | 3.0 ± 1.8 (n = 84) | 5.1 ± 1.8 (n = 83) | |||
| (1–15) years | 30.7% (n = 55) | 2.6 ± 1.6 (n = 180) | 4.9 ± 1.5 (n = 178) | |||
| (16–30) years | 42.5% (n = 94) | 2.1 ± 1.4 (n = 222) | 5.1 ± 1.7 (n = 223) | |||
| >30 years | 26.7% (n = 23) | ** | 2.0 ± 1.5 (n = 85) | *** | 5.3 ± 1.7 (n = 84) | NS |
| Parisian Cameroonian migrants | ||||||
| Paris living duration | ||||||
| (1–15) years | 41.6% (n = 10) | 0.3 ± 0.3 (n = 24) | 3.6 ± 1.2 (n = 24) | |||
| (16–30) years | 14.3% (n = 2) | 0.2 ± 0.3 (n = 14) | 3.5 ± 1.1 (n = 14) | |||
| >30 years | 16.7% (n = 2) | NS | 0.1 ± 0.2 (n = 12) | NS | 4.1 ± 1.6 (n = 12) | NS |
| Cameroon living duration | ||||||
| (1–20) years | 18.2% (n = 2) | 0.2 ± 0.3 (n = 11) | 3.6 ± 0.8 (n = 11) | |||
| (21–30) years | 27.6% (n = 8) | 0.2 ± 0.3 (n = 29) | 3.8 ± 1.3 (n = 29) | |||
| >30 years | 40.0% (n = 4) | NS | 0.2 ± 0.3 (n = 10) | NS | 3.6 ± 1.5 (n = 10) | NS |
| Measures | Rural Cameroon | Urban Cameroon | Urban France | |
|---|---|---|---|---|
| Men | n = 126 | n = 140 | n = 28 | p |
| BMI | 24.2 ± 3.8 c–c | 26.9 ± 3.8 c–b | 29.4 ± 3.8 c–b | *** |
| Waist circumference (cm) | 84.1 ± 9.1 c–c | 90.3 ± 9.1 c–c | 98.8 ± 9.1 c–c | *** |
| Hip circumference (cm) | 94.4 ± 8.4 c–c | 100.6 ± 8.4 c–a | 105.5 ± 8.4 c–a | *** |
| Waist to hip ratio | 0.9 ± 0.06 x–b | 0.9 ± 0.06 x–b | 0.9 ± 0.06 b–b | ** |
| Systolic Blood Pressure (mmHg) | 128.4 ± 19.8 x–x | 131.1 ± 19.9 x–x | 133.0 ± 19.9 x–x | NS |
| Diastolic Blood Pressure (mmHg) | 80.6 ± 13.1 b–a | 85.2 ± 13.1 b–x | 86.6 ± 13.2 a–x | ** |
| Women | n = 132 | n = 179 | n = 22 | p |
| BMI | 27.0 ± 5.3 c–x | 29.2 ± 5.3 c–x | 28.4 ± 5.4 x–x | ** |
| Waist circumference (cm) | 90.1 ± 11.6 x–a | 91.7 ± 11.7 x–x | 96.8 ± 11.8 a–x | * |
| Hip circumference (cm) | 103.4 ± 12.2 c–x | 108.5 ± 12.2 c–x | 107.7± 12.4 x–x | ** |
| Waist to Hip Ratio | 0.87 ± 0.06 c–x | 0.85 ± 0.06 c–c | 0.9 ± 0.06 x–c | *** |
| Systolic Blood Pressure (mmHg) | 118.5 ± 19.4 a–x | 123.2 ± 19.5 a–x | 117.7 ± 19.8 x–x | NS |
| Diastolic Blood Pressure (mmHg) | 78.4 ± 12.3 c–x | 83.5 ± 12.4 c–x | 80.3 ± 12.6 x–x | ** |
| Predictors | Categories | Obesity | |
|---|---|---|---|
| uOR CI | aOR CI | ||
| Sex *** | Men † | ||
| Women | 2.4 (1.6–3.5c) | 2.5 (1.6–3.8c) | |
| Age *** | 1.0 (1.0–1.1c) | 1.0 (1.0–1.1b) | |
| Migration status *** | No or lower urban living duration † | ||
| >25 years of Yaoundé residency | 2.5 (1.7–3.8c) | 1.7 (1.1–2.6a) | |
| >10 years of Paris region residency | 3.1 (1.5–6.2b) | 3.3 (1.2–8.8a) | |
| Educational level | Others † | ||
| University | 0.7 (0.5–1.2) | 0.8 (0.4–1.5) | |
| Calorie-level of diet | Others † | ||
| Higher calorie diet | 1.0 (0.7–1.4) | 1.1 (0.7–1.7) | |
| Physical activity *** | 0.8 (0.7–0.9c) | 0.8 (0.7–0.9b) | |
| Overweight valorisation *** | Non-valorisation † | ||
| Valorisation | 3.4 (2.2–5.2c) | 3.5 (2.1–5.7c) | |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cohen, E.; Amougou, N.; Ponty, A.; Loinger-Beck, J.; Nkuintchua, T.; Monteillet, N.; Bernard, J.Y.; Saïd-Mohamed, R.; Holdsworth, M.; Pasquet, P. Nutrition Transition and Biocultural Determinants of Obesity among Cameroonian Migrants in Urban Cameroon and France. Int. J. Environ. Res. Public Health 2017, 14, 696. https://doi.org/10.3390/ijerph14070696
Cohen E, Amougou N, Ponty A, Loinger-Beck J, Nkuintchua T, Monteillet N, Bernard JY, Saïd-Mohamed R, Holdsworth M, Pasquet P. Nutrition Transition and Biocultural Determinants of Obesity among Cameroonian Migrants in Urban Cameroon and France. International Journal of Environmental Research and Public Health. 2017; 14(7):696. https://doi.org/10.3390/ijerph14070696
Chicago/Turabian StyleCohen, Emmanuel, Norbert Amougou, Amandine Ponty, Juliette Loinger-Beck, Téodyl Nkuintchua, Nicolas Monteillet, Jonathan Y. Bernard, Rihlat Saïd-Mohamed, Michelle Holdsworth, and Patrick Pasquet. 2017. "Nutrition Transition and Biocultural Determinants of Obesity among Cameroonian Migrants in Urban Cameroon and France" International Journal of Environmental Research and Public Health 14, no. 7: 696. https://doi.org/10.3390/ijerph14070696







