Prevalence of Diabetes and Associated Factors in the Uyghur and Han Population in Xinjiang, China
Abstract
:1. Introduction
2. Methods
2.1. Participants
2.2. Data Collection
2.3. Definitions
2.4. Statistical Analysis
3. Results
| Characteristics | Uyghur (n = 2863) | Han (n = 3060) | ||
|---|---|---|---|---|
| Urban (n = 1359) | Rural (n = 1504) | Urban (n = 1950) | Rural (n = 1110) | |
| Male (%) | 515 (37.90) | 501 (33.31) * | 809 (41.49) † | 442 (39.82) ‡ |
| Age, years | 41.03 ± 11.95 | 48.69 ± 12.33 * | 47.38 ± 13.74 † | 49.73 ± 11.20 ** ‡ |
| 20~ | 636 (48.80) | 381 (25.33) * | 596 (30.56) † | 220 (19.82) ** ‡ |
| 40~ | 442 (32.52) | 467 (31.05) | 611 (31.33) | 342 (30.81) |
| 50~ | 182 (13.39) | 363 (24.14) | 361 (18.51) | 339 (30.54) |
| 60~80 | 99 (7.28) | 293 (19.48) | 382 (19.59) | 209 (18.83) |
| BMI, kg/m2 | 25.87 ± 4.73 | 25.72 ± 4.22 | 24.56 ± 3.66 † | 24.66 ± 3.64 ‡ |
| <25.0 | 607 (44.80) | 661 (44.45) | 1114 (57.30) † | 614 (55.67) ‡ |
| 25.0~ | 517 (38.15) | 613 (41.22) | 679 (34.93) | 404 (36.63) |
| 30.0~ | 231 (17.05) | 213 (14.32) | 151 (7.77) | 85 (7.71) |
| TC (mmol/L) | 4.74 ± 1.00 | 4.84 ± 1.07 * | 4.83 ± 1.01 † | 4.65 ± 0.96 ** ‡ |
| <6.21 | 1248 (91.90%) | 1372 (91.65%) | 1775 (91.07%) | 1043 (94.22%) ** ‡ |
| ≥6.21 | 110 (8.10%) | 125 (8.35%) | 174 (8.93%) | 64 (5.78%) |
| TG (mmol/L) | 1.46 ± 1.28 | 1.74 ± 1.61 * | 1.75 ± 1.70 † | 1.66 ± 1.85 |
| <2.26 | 1148 (84.60%) | 1161 (77.71%) * | 1531 (78.55%) † | 915 (82.73%) ** ‡ |
| ≥2.26 | 209 (15.40%) | 333 (22.29%) | 418 (21.45%) | 191 (17.27%) |
| HDL-C (mmol/L) | 1.36 ± 0.26 | 1.37 ± 0.27 | 1.44 ± 0.31 † | 1.45 ± 0.30 ‡ |
| <1.03 | 132 (9.72%) | 135 (9.02%) | 135 (6.93%) † | 73 (6.59%) ‡ |
| ≥1.03 | 1226 (90.28%) | 1362 (90.98%) | 1814 (93.07%) | 1034 (93.41%) |
| LDL-C (mmol/L) | 2.90 ± 0.82 | 2.92 ± 0.79 | 2.81 ± 0.79 † | 2.68 ± 0.74 ** ‡ |
| <4.16 | 1267 (93.30%) | 1412 (94.32%) | 1848 (94.82%) | 1074 (97.02%) ** ‡ |
| ≥4.16 | 91(6.70%) | 85 (5.68%) | 101 (5.18%) | 33 (2.98%) |
| Ratio of TC/HDL-C | 3.60 ± 0.96 | 3.65 ± 1.02 | 3.46 ± 0.91 † | 3.31 ± 0.84 ** ‡ |
| <5.00 | 1247 (91.83%) | 1384 (92.45%) | 1864 (95.64%) | 1078 (97.38%) |
| ≥5.00 | 111 (8.17%) | 113 (7.55%) | 85 (4.36%) | 29 (2.62%) |
| Glucose level | 5.31 ± 1.62 | 5.08 ± 1.55 * | 5.19 ± 1.44 † | 5.33 ± 1.46 ** ‡ |
| Education level (%) | ||||
| Illiteracy and primary school | 139 (10.29) | 576 (38.61) * | 236 (12.13) † | 409 (36.91) ** ‡ |
| Junior and senior high school | 594 (43.97) | 745 (49.93) | 920 (47.28) | 640 (57.76) |
| Graduate or above | 618 (45.74) | 171 (11.46) | 790 (40.60) | 59 (5.32) |
| Physical activity (%) | ||||
| Light | 1028 (75.81) | 549 (36.65) * | 1602 (82.15) † | 312 (28.11) ** ‡ |
| Moderate | 279 (20.58) | 199 (13.28) | 276 (14.15) | 134 (12.07) |
| Heavy | 49 (3.61) | 750 (50.07) | 72 (3.69) | 664 (59.82) |
| SBP (mm Hg) | 116.80 ± 16.70 | 122.10 ± 18.33 * | 119.40 ± 16.46 † | 121.40 ± 17.08 ** |
| DBP (mmHg) | 71.93 ± 11.29 | 73.70 ± 11.96 * | 74.16 ± 10.95 † | 73.67 ± 10.98 |
| Smoking Status (%) | ||||
| Never smokers | 973 (71.65) | 1169 (77.88) * | 1353 (69.49) † | 752 (67.75) ‡ |
| Ex-smokers | 85 (6.26) | 105 (7.00) | 189 (9.71) | 110 (9.91) |
| Current smokers | 300 (22.09) | 227 (15.12) | 405 (20.80) | 248 (22.34) |
| Drinking Status (%) | ||||
| Never drinkers | 1017 (75.11) | 1232 (82.30) * | 1000 (51.68) † | 572 (51.91) ‡ |
| Ex-drinkers | 113 (8.35) | 144 (9.62) | 101 (5.22) | 76 (6.90) |
| Current drinkers | 224 (16.54) | 121 (8.08) | 834 (43.10) | 454 (41.20) |
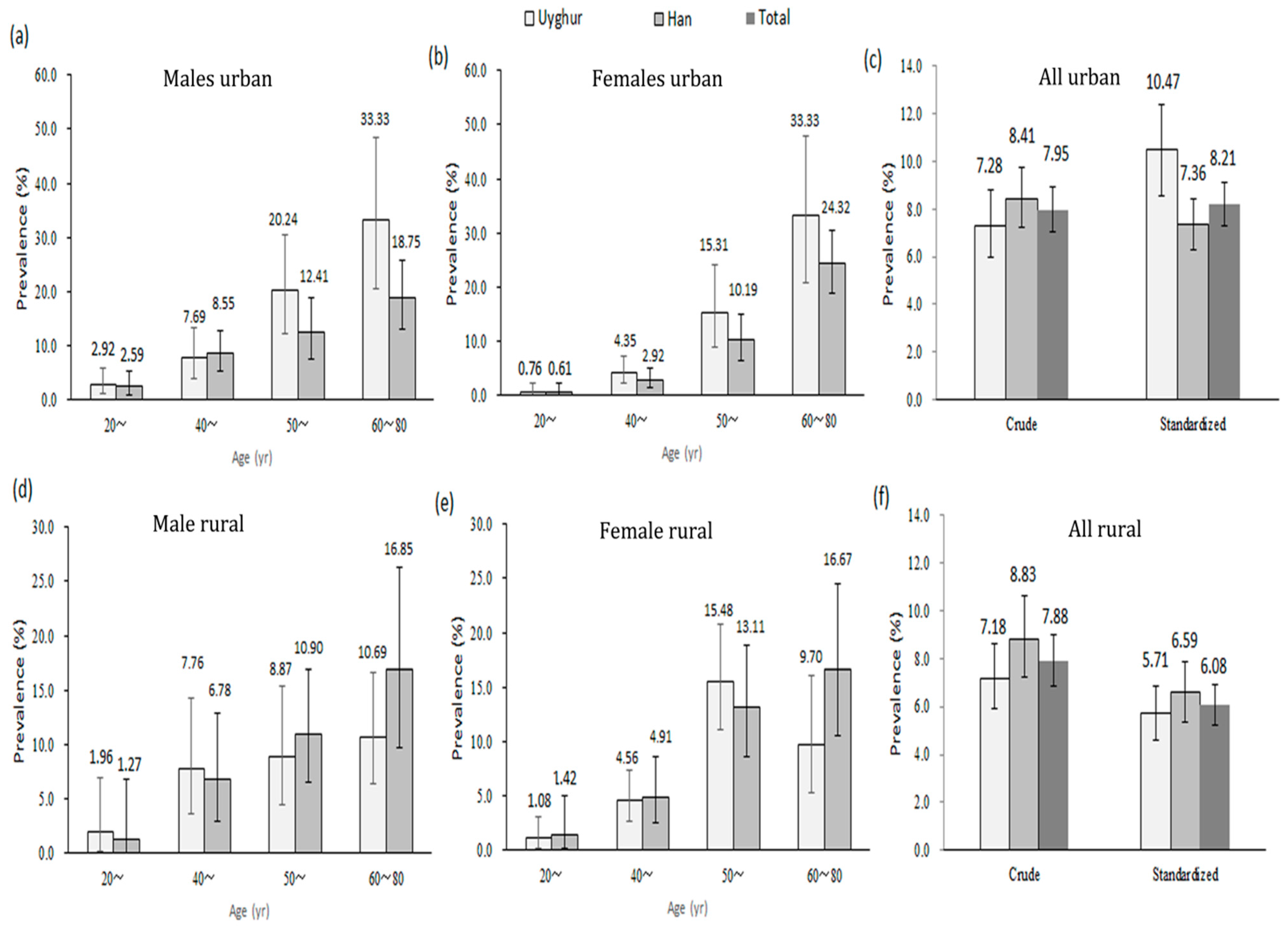
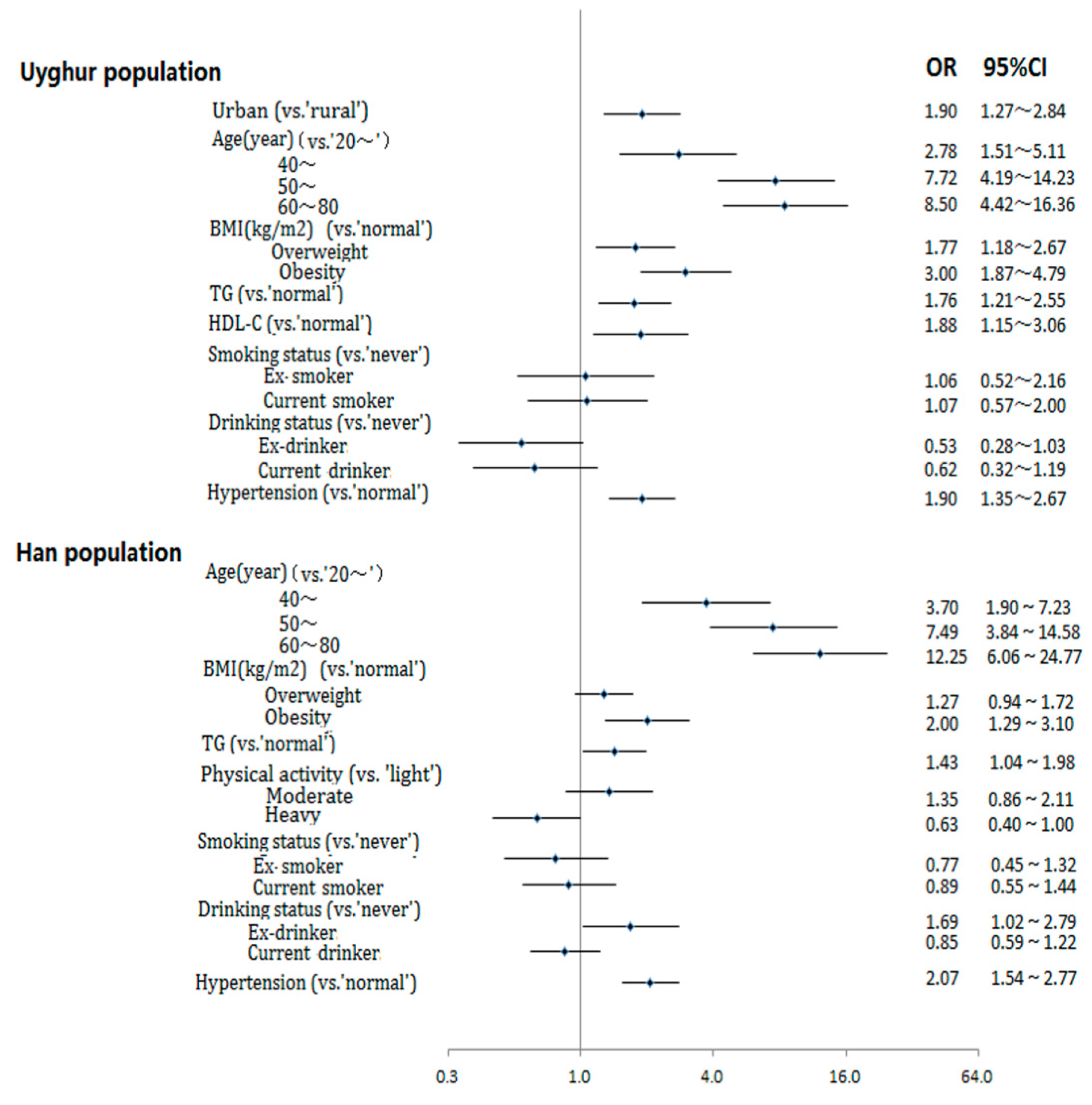
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Wang, C.; Zhang, Y.; Zhang, L.; Hou, X.; Lu, H.; Shen, Y.; Chen, R.; Fang, P.; Yu, H.; Li, M.; et al. Prevalence of type 2 diabetes among high-risk adults in Shanghai from 2002 to 2012. PLoS ONE 2014, 9. [Google Scholar] [CrossRef] [PubMed]
- Guariguata, L.; Whiting, D.R.; Hambleton, I.; Beagley, J.; Linnenkamp, U.; Shaw, J.E. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res Clin. Pract. 2014, 103, 137–149. [Google Scholar] [CrossRef]
- Zimmet, P.Z.; Magliano, D.J.; Herman, W.H.; Shaw, J.E. Diabetes: A 21st century challenge. Lancet. Diabetes Endocrinol. 2014, 2, 56–64. [Google Scholar] [CrossRef]
- National Diabetes Study Group. A mass survey of diabetes mellitus in a population of 300,000 in 14 provinces and municipalities in China. Zhonghua Nei Ke Za Zhi 1981, 20, 678–683. (in Chinese). [Google Scholar]
- Xu, Y.; Wang, L.; He, J.; Bi, Y.; Li, M.; Wang, T.; Wang, L.; Jiang, Y.; Dai, M.; Lu, J.; et al. Prevalence and control of diabetes in Chinese adults. JAMA 2013, 310, 948–959. [Google Scholar] [CrossRef] [PubMed]
- Zimmet, P.; Alberti, K.G.; Shaw, J. Global and societal implications of the diabetes epidemic. Nature 2001, 414, 782–787. [Google Scholar] [CrossRef] [PubMed]
- Yang, W.; Lu, J.; Weng, J.; Jia, W.; Ji, L.; Xiao, J.; Shan, Z.; Liu, J.; Tian, H.; Ji, Q.; et al. Prevalence of diabetes among men and women in China. N. Engl. J. Med. 2010, 362, 1090–1101. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.N.; Xie, X.; Ma, Y.T.; Li, X.M.; Fu, Z.Y.; Ma, X.; Huang, D.; Chen, B.D.; Liu, F.; Huang, Y.; et al. Type 2 diabetes in Xinjiang Uygur autonomous region, China. PLoS ONE 2012, 7. [Google Scholar] [CrossRef] [PubMed]
- Feng, L.; Li, P.; Wang, X.; Hu, Z.; Ma, Y.; Tang, W.; Ben, Y.; Mahapatra, T.; Cao, X.; Mahapatra, S.; et al. Distribution and determinants of non communicable diseases among elderly Uyghur ethnic group in Xinjiang, China. PLoS ONE 2014, 9. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Li, H.; Liu, F.; Chen, B.; Yang, Y.; Ma, Y. Association between the level of fasting blood glucose over 35-year-old and carotid intima-media thickness in Han, Uygur and Kazak population from Xinjiang Uygur autonomous region from 2007 to 2010. Zhonghua Yu Fang Yi Xue Za Zhi Chin. J. Prev. Med. 2014, 48, 878–882. (in Chinese). [Google Scholar]
- Awuti, G.; Younusi, K.; Li, L.; Upur, H.; Ren, J. Epidemiological survey on the prevalence of periodontitis and diabetes mellitus in Uyghur adults from rural Hotan area in Xinjiang. Exp. Diabetes Res. 2012, 2012. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Guo, S.; He, F.; Zhang, M.; He, J.; Yan, Y.; Ding, Y.; Zhang, J.; Liu, J.; Guo, H.; et al. Prevalence of diabetes mellitus and impaired fasting glucose, associated with risk factors in rural Kazakh adults in Xinjiang, China. Int. J. Environ. Res. Public Health 2015, 12, 554–565. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Obesity: Preventing and Managing the Global Epidemic; World Health Organization: Geneva, Switzerland, 2000. [Google Scholar]
- Tao, Y.; Mao, X.; Xie, Z.; Ran, X.; Liu, X.; Wang, Y.; Luo, X.; Hu, M.; Gen, W.; Zhang, M.; et al. The prevalence of type 2 diabetes and hypertension in Uygur and Kazak populations. Cardiovasc. Toxicol. 2008, 8, 155–159. [Google Scholar] [CrossRef] [PubMed]
- Tao, J.; Ma, Y.T.; Xiang, Y.; Xie, X.; Yang, Y.N.; Li, X.M.; Fu, Z.Y.; Ma, X.; Liu, F.; Chen, B.D.; et al. Prevalence of major cardiovascular risk factors and adverse risk profiles among three ethnic groups in the Xinjiang Uygur autonomous region, China. Lipids Health Dis. 2013, 12. [Google Scholar] [CrossRef] [PubMed]
- Finch, C.F.; Zimmet, P.Z.; Alberti, K.G. Determining diabetes prevalence: A rational basis for the use of fasting plasma glucose concentrations? Diabet. Med.: J. Br. Diabet. Assoc. 1990, 7, 603–610. [Google Scholar] [CrossRef]
- Zhou, X.; Guan, H.; Zheng, L.; Li, Z.; Guo, X.; Yang, H.; Yu, S.; Sun, G.; Li, W.; Hu, W.; et al. Prevalence and awareness of diabetes mellitus among a rural population in China: Results from Liaoning province. Diabet. Med.: J. Br. Diabet. Assoc. 2015, 32, 332–342. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.; Yang, Y.; Ma, X.; Chen, K.; Wu, N.; Wang, D.; Li, P.; Wang, M.; Li, Q.; Zhang, J. Prevalence of diabetes among Han, Manchu and Korean ethnicities in the Mudanjiang area of China: A cross-sectional survey. BMC Public Health 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Wiwanitkit, V. BMI, waist circumference and waist-to-hip ratio: Diabetes mellitus type 2. Eur. J. Clin. Nutr. 2010, 64. [Google Scholar] [CrossRef] [PubMed]
- Haffner, S.M.; Mitchell, B.D.; Stern, M.P.; Hazuda, H.P.; Patterson, J.K. Public health significance of upper body adiposity for non-insulin dependent diabetes mellitus in Mexican Americans. Int. J. Obes. Relat. Metab. Disord. 1992, 16, 177–184. [Google Scholar] [PubMed]
- Kodama, S.; Horikawa, C.; Fujihara, K.; Heianza, Y.; Hirasawa, R.; Yachi, Y.; Sugawara, A.; Tanaka, S.; Shimano, H.; Iida, K.T.; et al. Comparisons of the strength of associations with future type 2 diabetes risk among anthropometric obesity indicators, including waist-to-height ratio: A meta-analysis. Am. J. Epidemiol. 2012, 176, 959–969. [Google Scholar] [CrossRef]
- Ulijaszek, S.J.; Kerr, D.A. Anthropometric measurement error and the assessment of nutritional status. Brit. J. Nutr. 1999, 82, 165–177. [Google Scholar] [CrossRef] [PubMed]
- Salman, R.A.; Al-Rubeaan, K.A. Incidence and risk factors of hypertension among saudi type 2 diabetes adult patients: An 11-year prospective randomized study. J. Diabetes Its Complicat. 2009, 23, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Ghassibe-Sabbagh, M.; Deeb, M.; Salloum, A.K.; Mouzaya, F.; Haber, M.; Al-Sarraj, Y.; Chami, Y.; Akle, Y.; Hirbli, K.; Nemr, R.; et al. Multivariate epidemiologic analysis of type 2 diabetes mellitus risks in the Lebanese population. Diabetol. Metab. Syndr. 2014, 6. [Google Scholar] [CrossRef] [PubMed]
- Eckel, R.H.; Grundy, S.M.; Zimmet, P.Z. The metabolic syndrome. Lancet 2005, 365, 1416–1428. [Google Scholar] [CrossRef]
- Keogh, J.B.; Clifton, P. The effect of meal replacements high in glycomacropeptide on weight loss and markers of cardiovascular disease risk. Am. J. Clin. Nutr. 2008, 87, 1602–1605. [Google Scholar] [PubMed]
- Wang, L.; Tao, Y.; Xie, Z.; Ran, X.; Zhang, M.; Wang, Y.; Luo, X.; Hu, M.; Gen, W.; Wufuer, H.; et al. Prevalence of metabolic syndrome, insulin resistance, impaired fasting blood glucose, and dyslipidemia in Uygur and Kazak populations. J. Clin. Hypertens. 2010, 12, 741–745. [Google Scholar] [CrossRef] [PubMed]
- Zhao, G.; Ford, E.S.; Li, C.; Balluz, L.S. Physical activity in U.S. older adults with diabetes mellitus: Prevalence and correlates of meeting physical activity recommendations. J. Am. Geriatr. Soc. 2011, 59, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Hodge, A.M.; English, D.R.; O’Dea, K.; Giles, G.G. Alcohol intake, consumption pattern and beverage type, and the risk of type 2 diabetes. Diabet. Med.: J. Br. Diabet. Assoc. 2006, 23, 690–697. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gong, H.; Pa, L.; Wang, K.; Mu, H.; Dong, F.; Ya, S.; Xu, G.; Tao, N.; Pan, L.; Wang, B.; et al. Prevalence of Diabetes and Associated Factors in the Uyghur and Han Population in Xinjiang, China. Int. J. Environ. Res. Public Health 2015, 12, 12792-12802. https://doi.org/10.3390/ijerph121012792
Gong H, Pa L, Wang K, Mu H, Dong F, Ya S, Xu G, Tao N, Pan L, Wang B, et al. Prevalence of Diabetes and Associated Factors in the Uyghur and Han Population in Xinjiang, China. International Journal of Environmental Research and Public Health. 2015; 12(10):12792-12802. https://doi.org/10.3390/ijerph121012792
Chicago/Turabian StyleGong, Haiying, Lize Pa, Ke Wang, Hebuli Mu, Fen Dong, Shengjiang Ya, Guodong Xu, Ning Tao, Li Pan, Bin Wang, and et al. 2015. "Prevalence of Diabetes and Associated Factors in the Uyghur and Han Population in Xinjiang, China" International Journal of Environmental Research and Public Health 12, no. 10: 12792-12802. https://doi.org/10.3390/ijerph121012792






