Enhancement of Tendon–Bone Healing for Anterior Cruciate Ligament (ACL) Reconstruction Using Bone Marrow-Derived Mesenchymal Stem Cells Infected with BMP-2
Abstract
:1. Introduction
2. Results and Discussion
2.1. In Vitro Studies
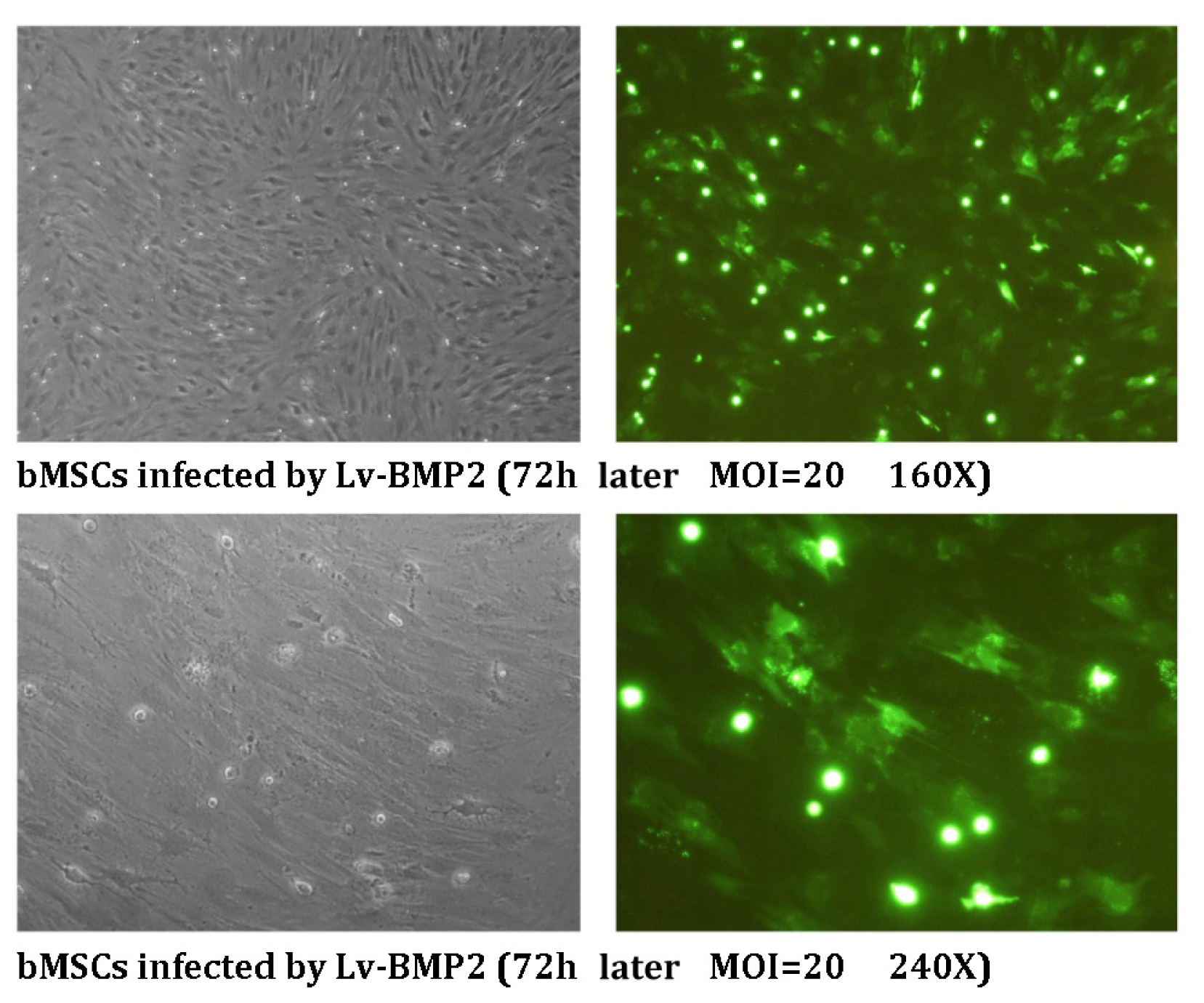
2.1.1. Infection of bMSCs with Lentivirus
2.1.2. MTT Assay
2.1.3. Real-Time Polymerase Chain Reaction
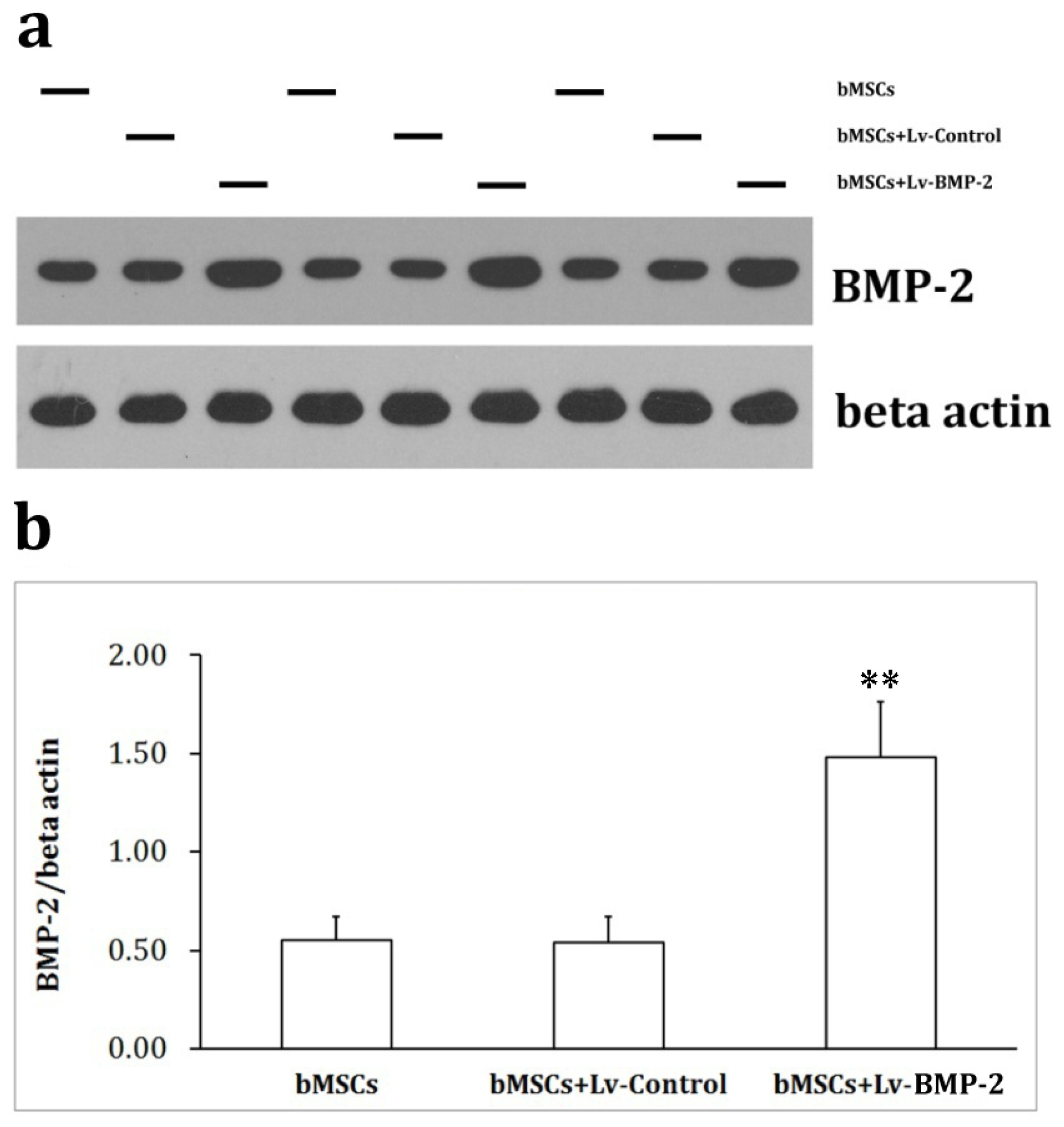
2.1.4. Western Blot Analysis
2.2. In Vivo Studies
2.2.1. Gross Observation
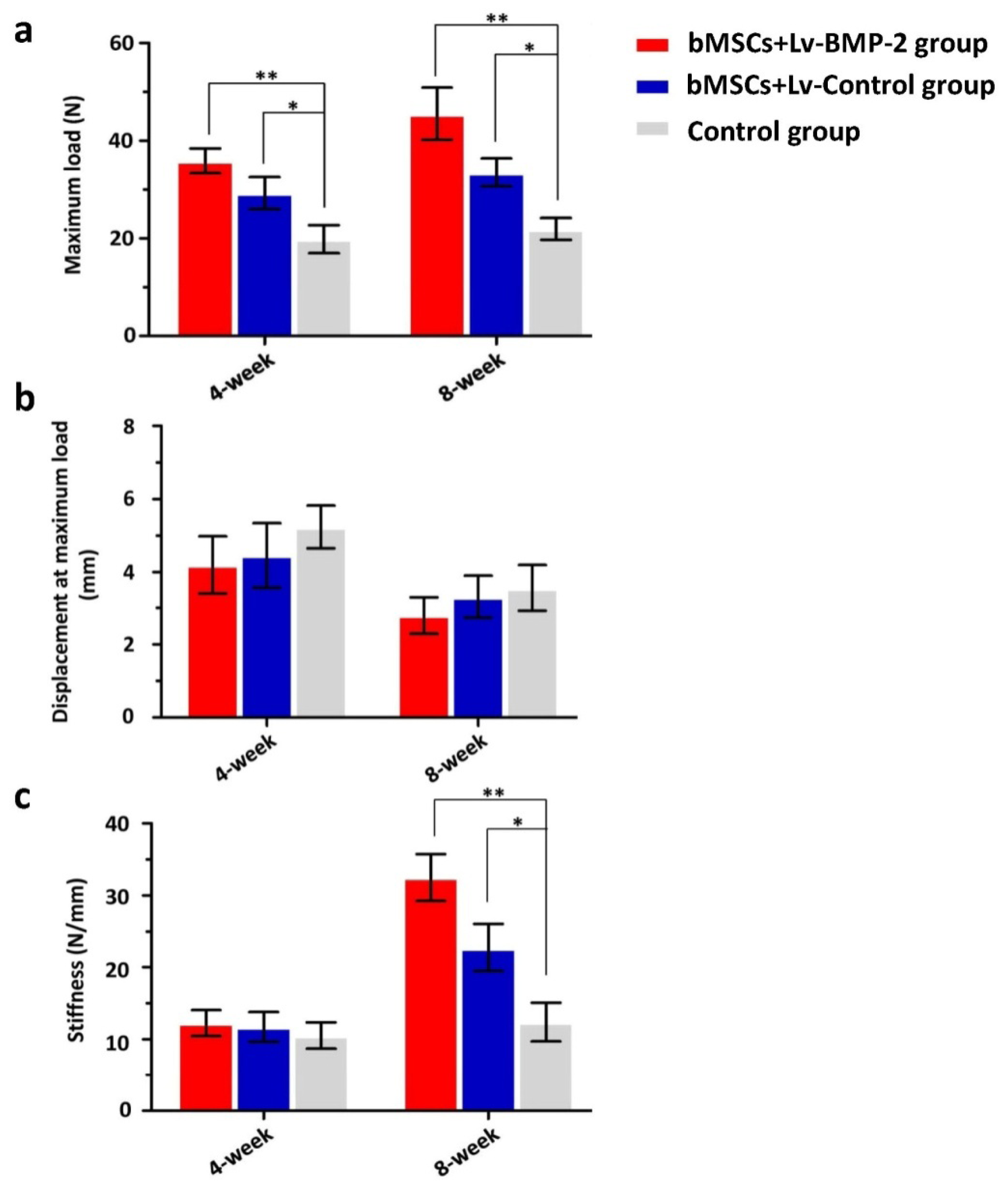
2.2.2. Mechanical Findings
2.2.3. Histological Findings
3. Experimental Section
3.1. In Vitro Studies
3.1.1. Cell Culture
3.1.2. Construction of the BMP-2 Eukaryotic Expression Vector and Packaging of the Recombinant Lentivirus
3.1.4. MTT Assay
3.1.5. Real-Time PCR
3.1.6. Western Blot Analysis
3.2. In Vivo Studies
3.2.1. Animal Study Design
3.2.2. Surgical Procedure
3.2.3. Mechanical Testing
3.2.4. Histological Examination
3.3. Statistical Analysis
4. Conclusions
Acknowledgements
- Conflict of InterestThe authors declare no conflict of interest.
References
- Spindler, K.P.; Wright, R.W. Anterior cruciate ligament tear. N. Engl. J. Med 2008, 359, 2135–2142. [Google Scholar]
- Frobell, R.B.; Roos, E.M.; Roos, H.P.; Ranstam, J.; Lohmander, L.S. A randomized trial of treatment for acute anterior cruciate ligament tears. N. Engl. J. Med 2010, 363, 331–342. [Google Scholar]
- Lohmander, L.S.; Englund, P.M.; Dahl, L.L.; Roos, E.M. The long-term consequence of anterior cruciate ligament and meniscus injuries: Osteoarthritis. Am. J. Sports Med 2007, 35, 1756–1769. [Google Scholar]
- Øiestad, B.E.; Engebretsen, L.; Storheim, K.; Risberg, M.A. Knee osteoarthritis after anterior cruciate ligament injury: A systematic review. Am. J. Sports Med 2009, 37, 1434–1443. [Google Scholar]
- Lohmander, L.S.; Ostenberg, A.; Englund, M.; Roos, H. High prevalence of knee osteoarthritis, pain, and functional limitations in female soccer players twelve years after anterior cruciate ligament injury. Arthritis Rheum 2004, 50, 3145–3152. [Google Scholar]
- Chanda, D.; Kumar, S.; Ponnazhagan, S. Therapeutic potential of adult bone marrow-derived mesenchymal stem cells in diseases of the skeleton. J. Cell Biochem 2010, 111, 249–257. [Google Scholar]
- Tucker, B.A.; Karamsadkar, S.S.; Khan, W.S.; Pastides, P. The role of bone marrow derived mesenchymal stem cells in sports injuries. J. Stem Cells 2010, 5, 155–166. [Google Scholar]
- Muruganandan, S.; Roman, A.A.; Sinal, C.J. Adipocyte differentiation of bone marrow-derived mesenchymal stem cells: Cross talk with the osteoblastogenic program. Cell Mol. Life Sci 2009, 66, 236–253. [Google Scholar]
- Yao, Y.; Wang, G.; Wang, Z.; Wang, C.; Zhang, H.; Liu, C. Synergistic enhancement of new bone formation by recombinant human bone morphogenetic protein-2 and osteoprotegerin in trans-sutural distraction osteogenesis: A pilot study in dogs. J. Oral Maxillofac. Surg 2011, 69, e446–e455. [Google Scholar]
- Ni, M.; Li, G.; Tang, P.F.; Chan, K.M.; Wang, Y. rhBMP-2 not alendronate combined with HA-TCP biomaterial and distraction osteogenesis enhance bone formation. Arch. Orthop. Trauma Surg 2011, 131, 1469–1476. [Google Scholar]
- Zhu, S.; Song, D.; Jiang, X.; Zhou, H.; Hu, J. Combined effects of recombinant human BMP-2 and Nell-1 on bone regeneration in rapid distraction osteogenesis of rabbit tibia. Injury 2011, 42, 1467–1473. [Google Scholar]
- Geuze, R.; Theyse, L.; Kempen, D.H.; Hazewinkel, H.; Kraak, H.; Oner, F.C.; Dhert, W.; Alblas, J. A differential effect of BMP-2 and VEGF release timing on osteogenesis at ectopic and orthotopic sites in a large animal model. Tissue Eng. Part A 2012, 18, 2052–2062. [Google Scholar]
- Garrison, K.R.; Shemilt, I.; Donell, S.; Ryder, J.J.; Mugford, M.; Harvey, I.; Song, F.; Alt, V. Bone morphogenetic protein (BMP) for fracture healing in adults. Cochrane Database Syst. Rev 2010. [Google Scholar] [CrossRef]
- Nistala, H.; Lee-Arteaga, S.; Siciliano, G.; Smaldone, S.; Ramirez, F. Extracellular regulation of transforming growth factor beta and bone morphogenetic protein signaling in bone. Ann. NY Acad. Sci 2010, 1192, 253–256. [Google Scholar]
- Zhang, Q.; He, Q.F.; Zhang, T.H.; Yu, X.L.; Liu, Q.; Deng, F.L. Improvement in the delivery system of bone morphogenetic protein-2: A new approach to promote bone formation. Biomed. Mater. Available online: http://iopscience.iop.org/1748-605X/7/4/045002 accessed on 9 October 2012. [CrossRef]
- Hunziker, E.B.; Enggist, L.; Küffer, A.; Buser, D.; Liu, Y. Osseointegration: The slow delivery of BMP-2 enhances osteoinductivity. Bone 2012, 51, 98–106. [Google Scholar]
- Kaipel, M.; Schützenberger, S.; Schultz, A.; Ferguson, J.; Slezak, P.; Morton, T.J.; Van Griensven, M.; Redl, H. BMP-2 but not VEGF or PDGF in fibrin matrix supports bone healing in a delayed-union rat model. J. Orthop. Res 2012, 10, 1563–1569. [Google Scholar]
- Starman, J.S.; Bosse, M.J.; Cates, C.A.; Norton, H.J. Recombinant human bone morphogenetic protein-2 use in the off-label treatment of nonunions and acute fractures: A retrospective review. J. Trauma Acute Care Surg 2012, 72, 676–681. [Google Scholar]
- Angle, S.R.; Sena, K.; Sumner, D.R.; Virkus, W.W.; Virdi, A.S. Healing of rat femoral segmental defect with bone morphogenetic protein-2: A dose response study. J. Musculoskelet. Neuronal Interact 2012, 12, 28–37. [Google Scholar]
- Sun, K.; Zhang, J.; Wang, Y.; Xia, C.; Zhang, C.; Yu, T.; Tian, S. Arthroscopic anterior cruciate ligament reconstruction with at least 2.5 years’ follow-up comparing hamstring tendon autograft and irradiated allograft. Arthroscopy 2011, 27, 1195–1202. [Google Scholar]
- Leal-Blanquet, J.; Alentorn-Geli, E.; Tuneu, J.; Valentí, J.R.; Maestro, A. Anterior cruciate ligament reconstruction: A multicenter prospective cohort study evaluating 3 different grafts using same bone drilling method. Clin. J. Sport Med 2011, 21, 294–300. [Google Scholar]
- Wipfler, B.; Donner, S.; Zechmann, C.M.; Springer, J.; Siebold, R.; Paessler, H.H. Anterior cruciate ligament reconstruction using patellar tendon versus hamstring tendon: A prospective comparative study with 9-year follow-up. Arthroscopy 2011, 27, 653–665. [Google Scholar]
- Radice, F.; Yánez, R.; Gutiérrez, V.; Rosales, J.; Pinedo, M.; Coda, S. Comparison of magnetic resonance imaging findings in anterior cruciate ligament grafts with and without autologous platelet-derived growth factors. Arthroscopy 2010, 26, 50–57. [Google Scholar]
- Jagodzinski, M.; Geiges, B.; Von Falck, C.; Knobloch, K.; Haasper, C.; Brand, J.; Hankemeier, S.; Krettek, C.; Meller, R. Biodegradable screw versus a press-fit bone plug fixation for hamstring anterior cruciate ligament reconstruction: A prospective randomized study. Am. J. Sports Med 2010, 38, 501–508. [Google Scholar]
- Kohno, T.; Ishibashi, Y.; Tsuda, E.; Kusumi, T.; Tanaka, M.; Toh, S. Immunohistochemical demonstration of growth factors at the tendon-bone interface in anterior cruciate ligament reconstruction using a rabbit model. J. Orthop. Sci 2007, 12, 67–73. [Google Scholar]
- Huangfu, X.; Zhao, J. Tendon-Bone healing enhancement using injectable tricalcium phosphate in a dog anterior cruciate ligament reconstruction model. Arthroscopy 2007, 23, 455–462. [Google Scholar]
- Demirag, B.; Sarisozen, B.; Ozer, O.; Kaplan, T.; Ozturk, C. Enhancement of tendon-bone healing of anterior cruciate ligament grafts by blockage of matrix metalloproteinases. J. Bone Joint Surg. Am 2005, 87, 2401–2410. [Google Scholar]
- Jones, E.; McGonagle, D. Human bone marrow mesenchymal stem cells in vivo. Rheumatology 2008, 47, 126–131. [Google Scholar]
- Lee, J.Y.; Zhou, Z.; Taub, P.J.; Ramcharan, M.; Li, Y.; Akinbiyi, T.; Maharam, E.R.; Leong, D.J.; Laudier, D.M.; Ruike, T.; et al. BMP-12 treatment of adult mesenchymal stem cells in vitro augments tendon-like tissue formation and defect repair in vivo. PLoS One 2011, 6, e17531. [Google Scholar]
- Haddad-Weber, M.; Prager, P.; Kunz, M.; Seefried, L.; Jakob, F.; Murray, M.M.; Evans, C.H.; Nöth, U.; Steinert, A.F. BMP12 and BMP13 gene transfer induce ligamentogenic differentiation in mesenchymal progenitor and anterior cruciate ligament cells. Cytotherapy 2010, 12, 505–513. [Google Scholar]
- Lim, J.K.; Hui, J.; Li, L.; Thambyah, A.; Goh, J.; Lee, E.H. Enhancement of tendon graft osteointegration using mesenchymal stem cells in a rabbit model of anterior cruciate ligament reconstruction. Arthroscopy 2004, 20, 899–910. [Google Scholar]
- Kanaya, A.; Deie, M.; Adachi, N.; Nishimori, M.; Yanada, S.; Ochi, M. Intra-Articular injection of mesenchymal stromal cells in partially torn anterior cruciate ligaments in a rat model. Arthroscopy 2007, 23, 610–617. [Google Scholar]
- Rodeo, S.A.; Arnoczky, S.P.; Torzilli, P.A.; Hidaka, C.; Warren, R.F. Tendon-Healing in a bone tunnel. A biomechanical and histological study in the dog. J. Bone Joint Surg. Am 1993, 75, 1795–1803. [Google Scholar]
- Ma, C.B.; Kawamura, S.; Deng, X.H.; Ying, L.; Schneidkraut, J.; Hays, P.; Rodeo, S.A. Bone morphogenetic proteins-signaling plays a role in tendon-to-bone healing: A study of rhBMP-2 and noggin. Am. J. Sports Med 2007, 35, 597–604. [Google Scholar]
- Hong, W.O.; James, J.C.; Eng, H.L. Use of bone marrow stromal cells for tendon graft-to-bone healing: Histological and immunohistochemical studies in a rabbit model. Am. J. Sports Med 2004, 32, 321–327. [Google Scholar]



© 2012 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Dong, Y.; Zhang, Q.; Li, Y.; Jiang, J.; Chen, S. Enhancement of Tendon–Bone Healing for Anterior Cruciate Ligament (ACL) Reconstruction Using Bone Marrow-Derived Mesenchymal Stem Cells Infected with BMP-2. Int. J. Mol. Sci. 2012, 13, 13605-13620. https://doi.org/10.3390/ijms131013605
Dong Y, Zhang Q, Li Y, Jiang J, Chen S. Enhancement of Tendon–Bone Healing for Anterior Cruciate Ligament (ACL) Reconstruction Using Bone Marrow-Derived Mesenchymal Stem Cells Infected with BMP-2. International Journal of Molecular Sciences. 2012; 13(10):13605-13620. https://doi.org/10.3390/ijms131013605
Chicago/Turabian StyleDong, Yu, Qingguo Zhang, Yunxia Li, Jia Jiang, and Shiyi Chen. 2012. "Enhancement of Tendon–Bone Healing for Anterior Cruciate Ligament (ACL) Reconstruction Using Bone Marrow-Derived Mesenchymal Stem Cells Infected with BMP-2" International Journal of Molecular Sciences 13, no. 10: 13605-13620. https://doi.org/10.3390/ijms131013605



