Optimization of the Preparation Conditions of Borneol-Modified Ginkgolide Liposomes by Response Surface Methodology and Study of Their Blood Brain Barrier Permeability
Abstract
:1. Introduction
2. Results and Discussion
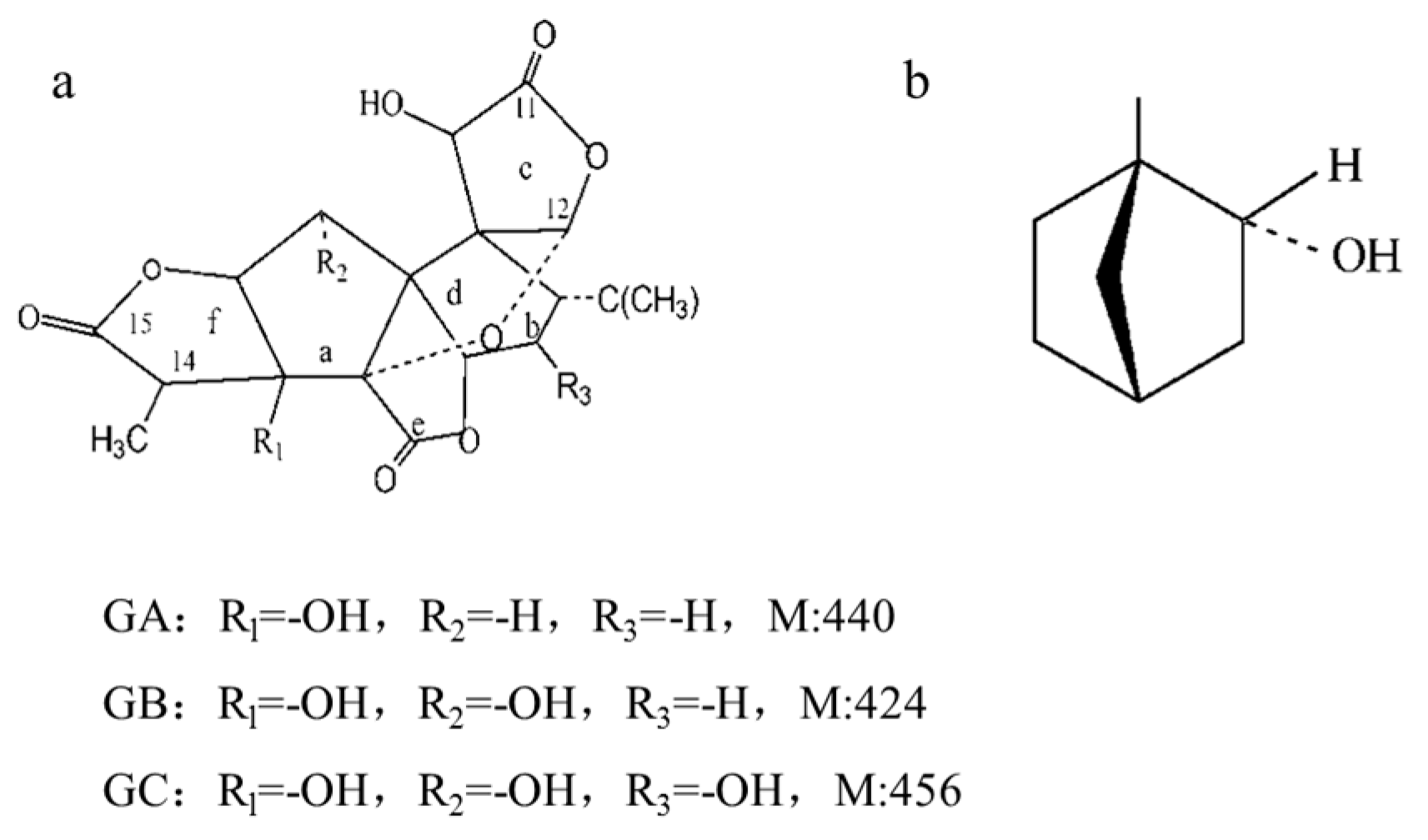
2.1. Preparation of GGB-LP
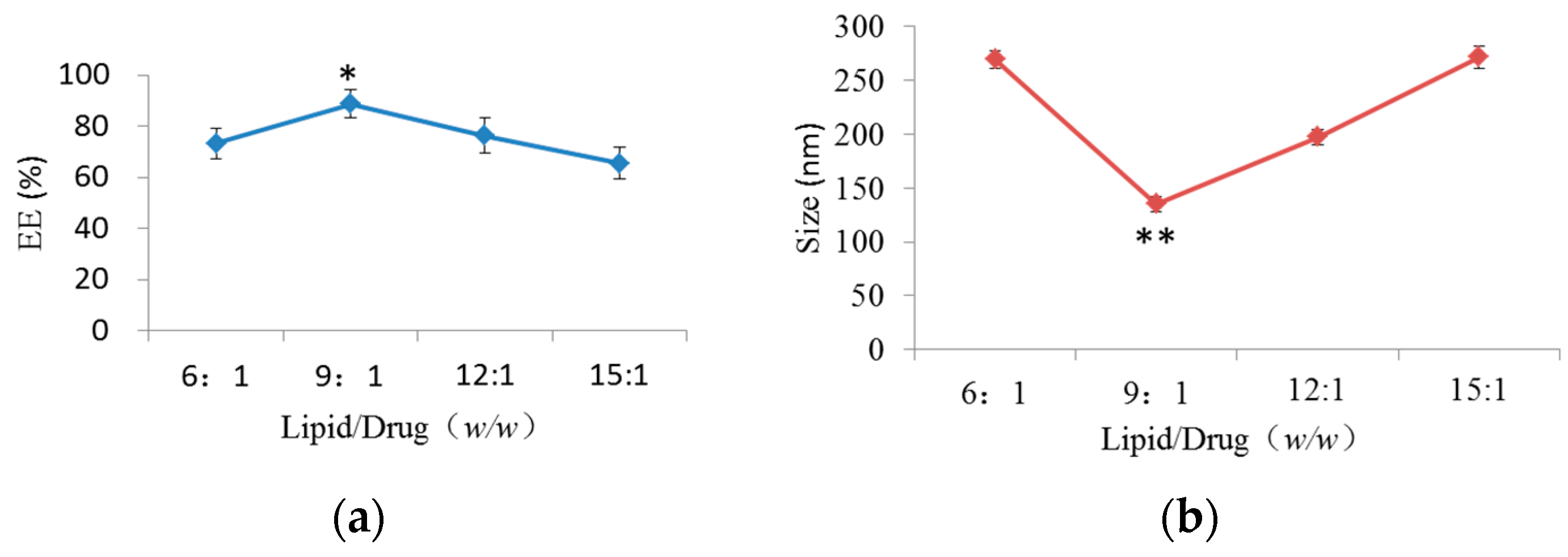
2.1.1. Effect of Phospholipid/Drug Weight Ratio on Encapsulation Efficiency (EE) and Size
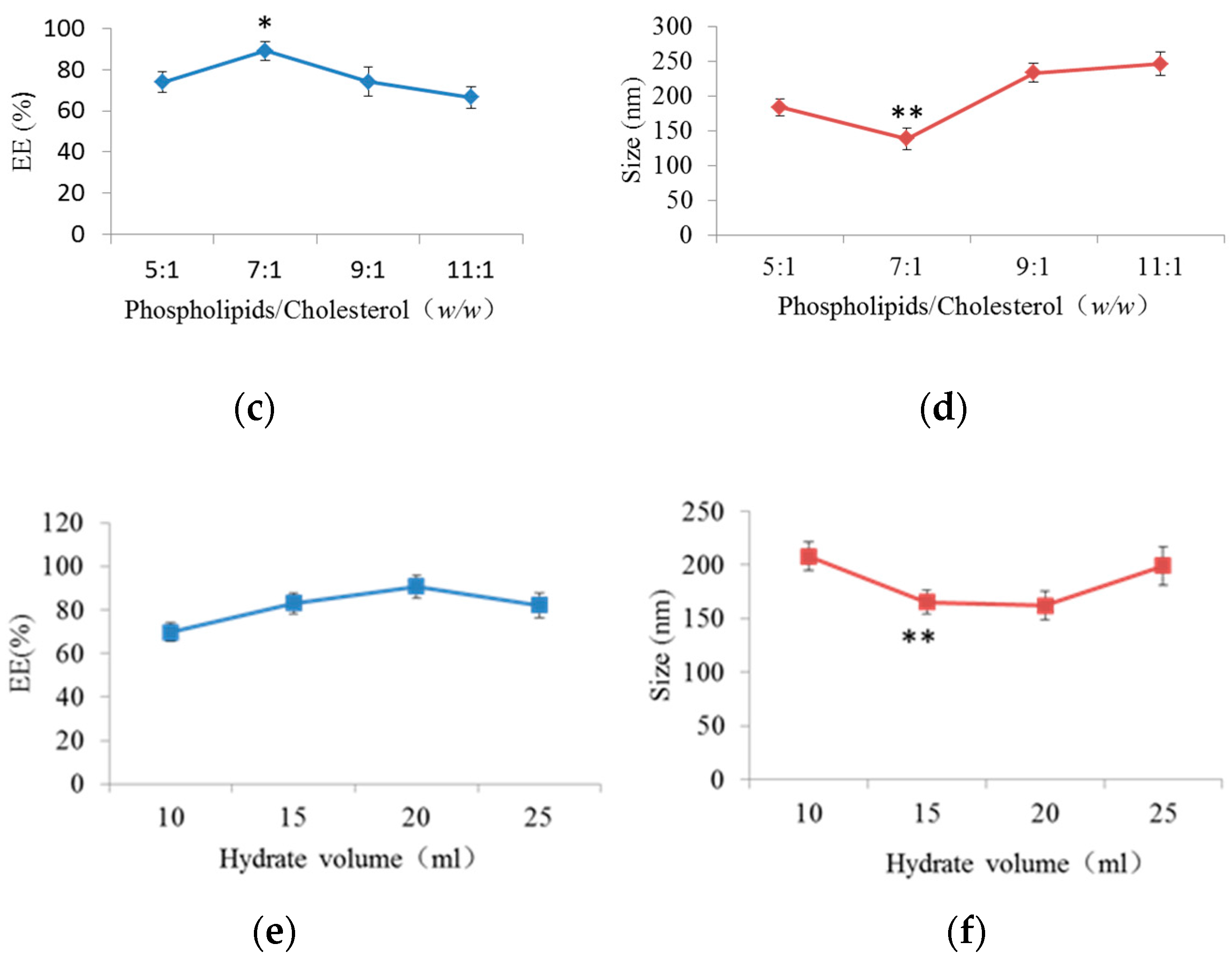
2.1.2. Effect of Phospholipid/Cholesterol Weight Ratio on EE and Size
2.1.3. Effect of Hydrate Volume on EE and Size
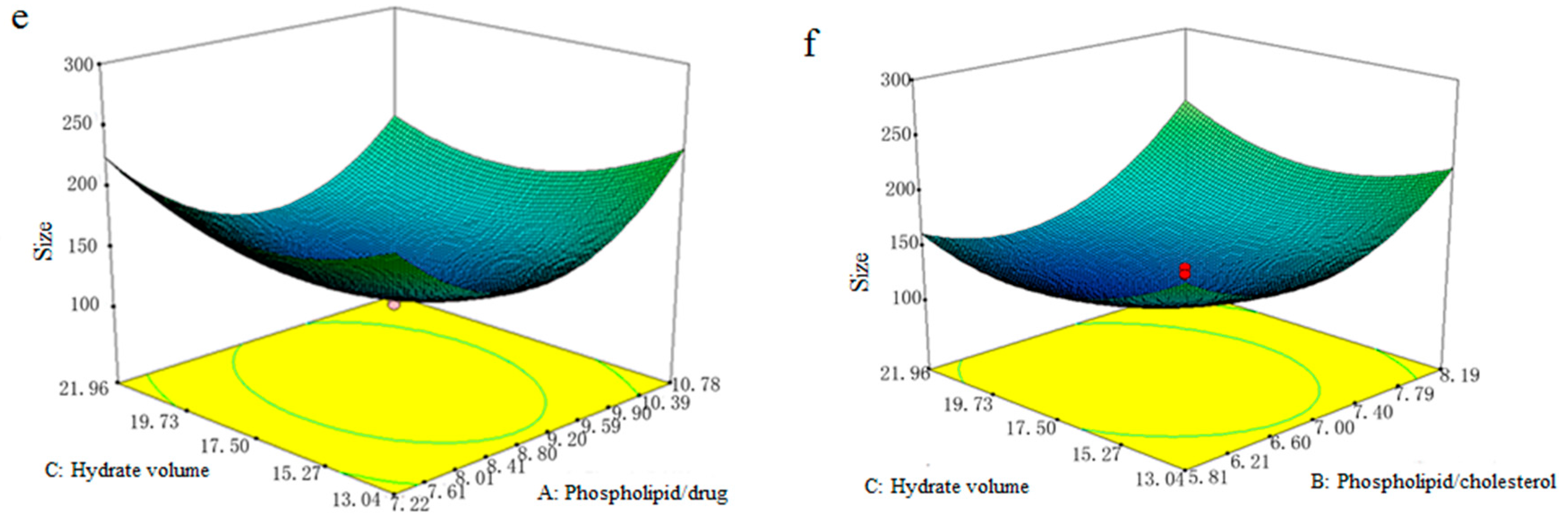
2.2. Optimization of GGB-LP Preparation by RSM
2.3. Verification of the Predictive Model
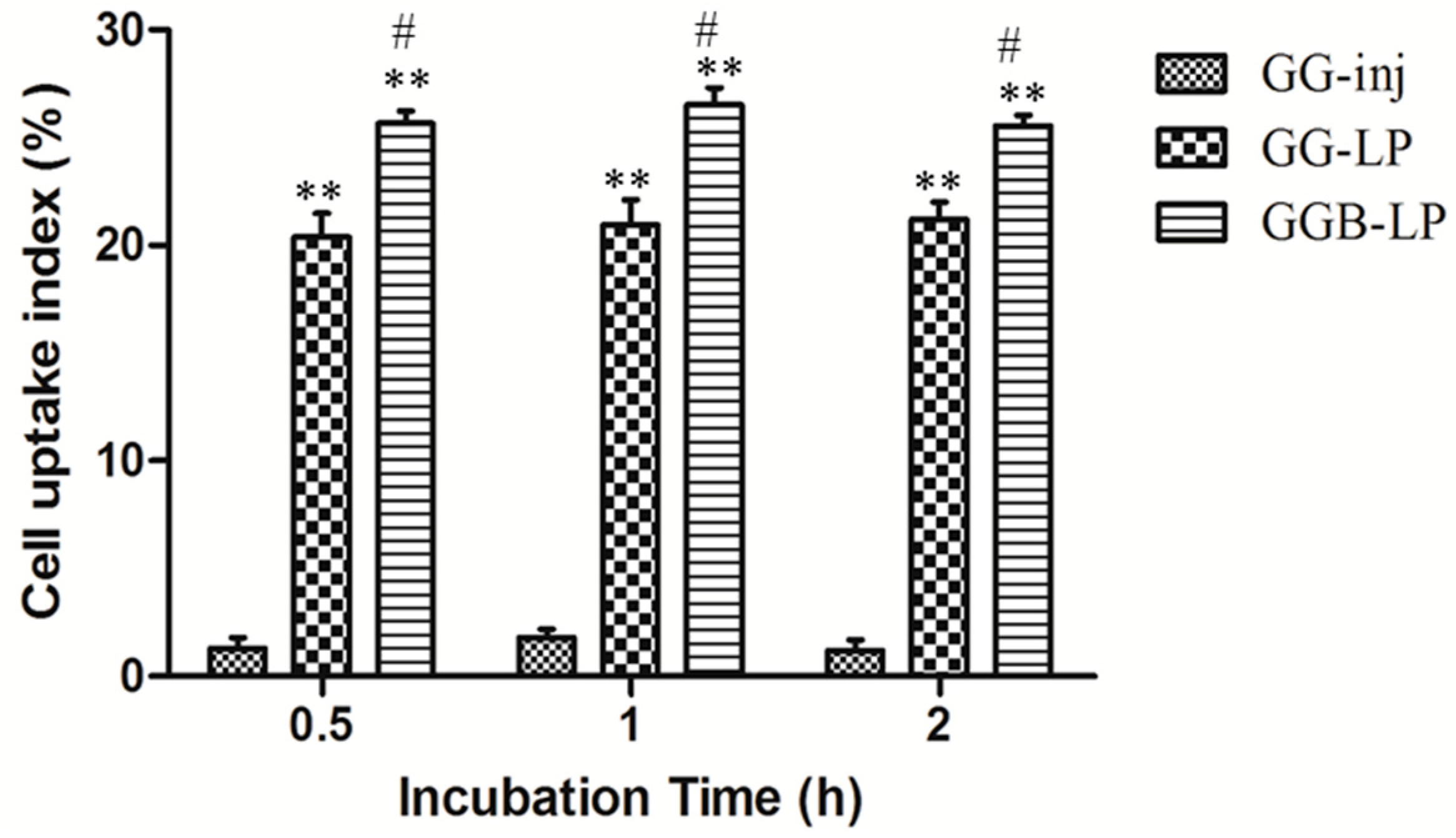
2.4. In Vitro Cell Uptake Study for Evaluation of BBB Penetration Potential of GGB-LP
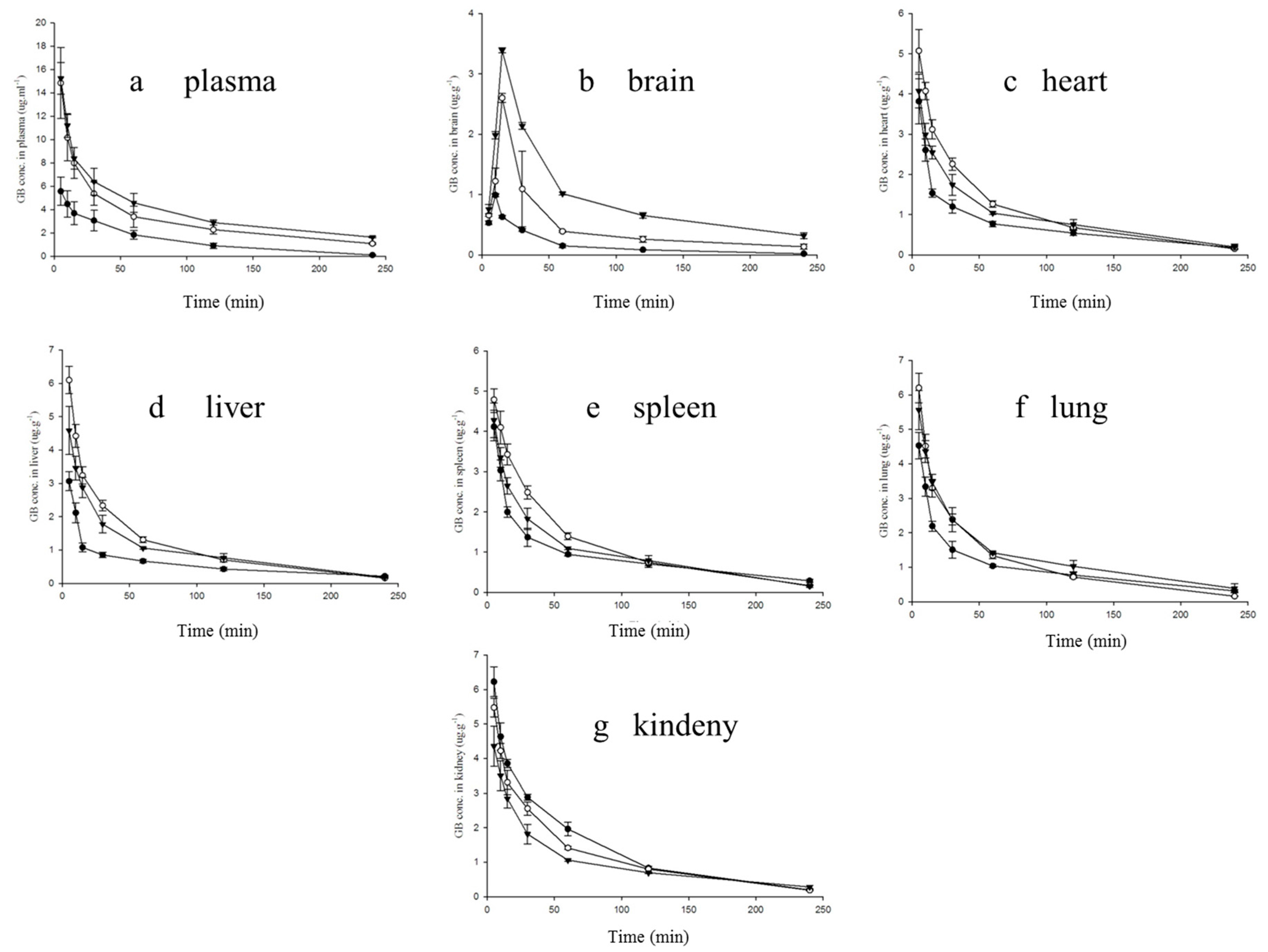
2.5. Brain Targeting and Biodistribution Studies of GGB-LP
2.5.1. Plasma Analysis
2.5.2. GB Distribution in Brain
2.5.3. GB Distribution in Other Tissues
3. Materials and Methods
3.1. Materials
3.2. Preparation of Ginkgolides Liposomes Modified by Borneol (GGB-LP)
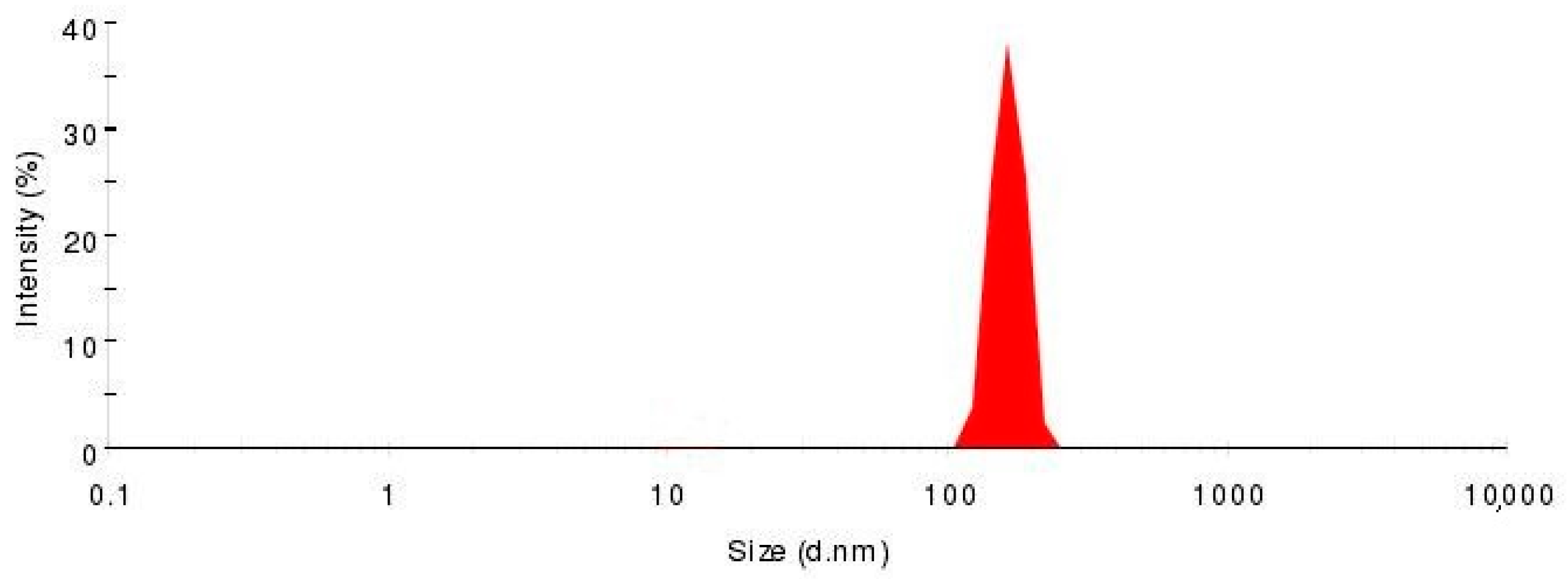
3.3. Characterization of GGB-LP
3.4. Optimization of GGB-LP Preparation by Response Surface-Central Composite Design
3.5. Blood-Brain Barrier Permeability of GGB-LP
3.5.1. In Vitro Cell Uptake Study for Evaluation of BBB Penetration Potential
3.5.2. Animals and Administration of GG Formulations
3.5.3. UPLC-MS Analysis of GB in Plasma and Tissues
3.6. Data Analysis
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Stromgaard, K.; Suehiro, M.; Nakanishi, K. Preparation of a tritiated ginkgolide. Bioorg. Med. Chem. Lett. 2004, 14, 5673–5675. [Google Scholar] [CrossRef] [PubMed]
- Chiu, H.L.; Lin, H.Y.; Yang, T.C. Determination of ginkgolide A, B, and bilobalide in biloba L. extracts by microdialysis-HPLC. Anal. Bioanal. Chem. 2004, 379, 445–448. [Google Scholar] [CrossRef] [PubMed]
- Hu, L.; Chen, Z.; Xie, Y.; Xie, Y.; Jiang, Y.; Zhen, H. Alkyl and alkoxycarbonyl derivatives of ginkgolide B: Synthesis and biological evaluation of PAF inhibitory activity. Bioorg. Med. Chem. 2000, 8, 1515–1521. [Google Scholar] [CrossRef]
- Amri, H.; Drieu, K.; Papadopoulos, V. Use of ginkgolide B and a ginkgolide-activated response element to control gene transcription: Example of the adrenocortical peripheral-type benzodiazepine receptor. Cell. Mol. Biol. 2002, 48, 633–639. [Google Scholar] [PubMed]
- Maclennan, K.M.; Darlington, C.L.; Smith, P.F. The CNS effects of Ginkgo biloba extracts and ginkgolide B. Prog. Neurobiol. 2002, 67, 235–257. [Google Scholar] [CrossRef]
- Farbiszewski, R.; Dudek, H.; Skrzydlewska, E.; Lewko, J. The role of platelet activating factor (PAF) in physiology and pathology of the central nervous system. Neurol. Neurochir. Polska 2001, 36, 801–808. [Google Scholar]
- Akisü, M.; Kültürsay, N.; Coker, I.; Hüseyinov, A. Platelet-activating factor is an important mediator in hypoxic ischemic brain injury in the newborn rat. Neonatology 1998, 74, 439–444. [Google Scholar] [CrossRef]
- Shen, S.; Zhang, W. ABC transporters and drug efflux at the blood-brain barrier. Rev. Neurosci. 2010, 21, 29–54. [Google Scholar] [CrossRef] [PubMed]
- Ravindranath, V. Animal models and molecular markers for cerebral ischemia-reperfusion injury in brain. Methods Enzymol. 1994, 233, 610–619. [Google Scholar] [PubMed]
- Díez-Tejedor, E.; Alonso, L.M.; Carceller, F.; Frank, A.; Roda, J.M. Physiopathology of cerebral ischemia: Ischemia-reperfusion injury. Rev. Clin. Esp. 1996, 196, 14–19. [Google Scholar] [PubMed]
- Chen, J.; Li, L.; Su, J.; Li, B.; Chen, T.; Ling, F.; Zhang, X. Enhancing effect of natural borneol on the cellular uptake of demethoxycurcumin and their combined induction of G2/M arrest in HepG2 cells via ROS generation. J. Funct. Foods 2015, 17, 103–114. [Google Scholar] [CrossRef]
- Qi, Z.; Dong, W.; Wu, J.; Ou, Y.; Mu, C.; Han, B.; Zhang, Q. Improved blood—Brain barrier distribution: Effect of borneol on the brain pharmacokinetics of kaempferol in rats by in vivo microdialysis sampling. J. Ethnopharmacol. 2015, 162, 270–277. [Google Scholar]
- Yu, B.; Ruan, M.; Dong, X.P.; Yu, Y.; Cheng, H.B. The mechanism of the opening of the blood—Brain barrier by borneol: A pharmacodynamics and pharmacokinetics combination study. J. Ethnopharmacol. 2013, 150, 1096–1108. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.Y.; Ying, T.; Gao, L.Y.; Sun, W.X.; Hua, Y.; Yang, S.B.; Zhang, Z.P.; Liao, G.Y.; Zhou, Q.G.; Luo, C.X.; et al. The synergetic effect of edaravone and borneol in the rat model of ischemic stroke. Eur. J. Pharmacol. 2014, 740, 522–531. [Google Scholar] [CrossRef] [PubMed]
- Ren, J.; Zou, M.; Gao, P.; Wang, Y.; Cheng, G. Tissue distribution of borneol-modified ganciclovir-loaded solid lipid nanoparticles in mice after intravenous administration. Eur. J. Pharm. Biopharm. 2013, 83, 141–148. [Google Scholar] [CrossRef] [PubMed]
- Cai, Z.; Hou, S.; Li, Y.; Zhao, B.B.; Yang, Z.X.; Xu, S.G.; Pu, J.X. Effect of borneol on the distribution of gastrodin to the brain in mice via oral administration. J. Drug Target. 2008, 83, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Du, S.; Chen, X.L.; Wu, Q.; Song, X.; Xu, B.; Zhai, Y.S. Enhancing effect of natural borneol on the absorption of geniposide in rat via intranasal administration. J. Zhejiang Univ. Sci. B 2011, 12, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Chen, R.; Yang, L.; Huang, T.L.; Xu, Q.W.; Mi, S.Q.; Wang, N.S. Pharmacokinetics of natural borneol after oral administration in mice brain and its effect on excitation ratio. Eur. J. Drug Metab. Pharmacokinet. 2012, 12, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Bansal, D.; Gulbake, A.; Tiwari, J.; Jain, S.K. Development of liposomes entrapped in alginate beads for the treatment of colorectal cancer. Int. J. Biol. Macromol. 2016, 82, 687–695. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Hu, M.; Yu, X.; Li, Y.; Fu, Y.S.; Zhou, X.X.; Zhang, D.; Li, J.Y. Design and evaluation of pH-sensitive liposomes constructed by poly (2-ethyl-2-oxazoline)-cholesterol hemisuccinate for doxorubicin delivery. Eur. J. Pharm. Biopharm. 2015, 91, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Kaminski, G.A.T.; Sierakowski, M.R.; Pontarolo, R.; dos Santos, L.A.; de Freitas, R.A. Layer-by-layer polysaccharide-coated liposomes for sustained delivery of epidermal growth factor. Carbohydr. Polym. 2016, 140, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Palchetti, S.; Colapicchioni, V.; Digiacomo, L.; Caracciolo, G.; Pozzi, D.; Capriotti, A.L.; La Barbera, G.; Laganà, A. The protein corona of circulating PEGylated liposomes. Biochim. Biophys. Acta 2016, 1858, 189–196. [Google Scholar] [CrossRef] [PubMed]
- Hatakeyama, H.; Akita, H.; Harashima, H. A multifunctional envelope type nano device (MEND) for gene delivery to tumours based on the EPR effect: A strategy for overcoming the PEG dilemma. Adv. Drug Deliv. Rev. 2011, 63, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Ren, W.; Zhong, T.; Zhang, S.; Huang, D.; Guo, Y.; Yao, X.; Wang, C.; Zhang, W.Q.; Zhang, X.; et al. Tumor-specific pH-responsive peptide-modified pH-sensitive liposomes containing doxorubicin for enhancing glioma targeting and anti-tumor activity. J. Control. Release 2016, 222, 56–66. [Google Scholar] [CrossRef] [PubMed]
- Chang, M.; Lu, S.; Zhang, F.; Zuo, T.; Guan, Y.; Wei, T.; Shao, W.; Lin, G. RGD-modified pH-sensitive liposomes for docetaxel tumor targeting. Colloid Surf. B Biointerfaces 2015, 129, 175–182. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; van Minh, L.; Liu, J.; Angelov, B.; Drechsler, M.; Garamus, V.M.; Willumeit-Römer, R.; Zou, A. Baicalin loaded in folate-PEG modified liposomes for enhanced stability and tumor targeting. Colloid Surf. B Biointerfaces 2016, 140, 74–82. [Google Scholar] [CrossRef] [PubMed]
- Ueno, M.; Wu, B.; Nakagawa, T.; Nagai, Y.; Onodera, M.; Huang, C.L.; Kusaka, T.; Kanenishi, K.; Sakamoto, H. The expression of LDL receptor in vessels with blood—Brain barrier impairment in a stroke-prone hypertensive model. Histochem. Cell Biol. 2010, 133, 669–676. [Google Scholar] [CrossRef] [PubMed]
- Shi, K.; Li, J.; Cao, Z.; Yang, P.; Qiu, Y.; Yang, B.; Wang, Y.; Long, Y.; Liu, Y.; Zhang, Q.; et al. A pH-responsive cell-penetrating peptide-modified liposomes with active recognizing of integrin α v β 3 for the treatment of melanoma. J. Controll. Release 2015, 217, 138–150. [Google Scholar] [CrossRef] [PubMed]
- Vieira, D.; Gamarra, L. Getting into the brain: Liposome-based strategies for effective drug delivery across the blood-brain barrier. Int. J. Nanomed. 2016, 11, 5381–5414. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Fu, B.; Zhang, Z. Borneol, a novel agent that improves central nervous system drug delivery by enhancing blood—Brain barrier permeability. Drug Deliv. 2017, 24, 1037–1044. [Google Scholar] [CrossRef] [PubMed]
- Jin, H.; Lu, Q.; Jiang, J. Curcumin liposomes prepared with milk fat globule membrane phospholipids and soybean lecithin. J. Dairy Sci. 2016, 99, 1780–1790. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Cheng, Y.; Chen, Y.; He, W.; Ni, L.; Xiong, P.; Wei, M. Vitamin E TPGS modified liposomes enhance cellular uptake and targeted delivery of luteolin: An in vivo/in vitro evaluation. Int. J. Pharm. 2016, 512, 262–272. [Google Scholar] [CrossRef] [PubMed]
- Zeng, C.; Jiang, W.; Tan, M.; Tan, M.; Yang, X.; He, C.; Huang, W.; Xing, J. Optimization of the process variables of tilianin-loaded composite phospholipid liposomes based on response surface-central composite design and pharmacokinetic study. Eur. J. Pharm. Sci. 2016, 85, 123–131. [Google Scholar] [CrossRef] [PubMed]
Sample Availability: Samples of the compounds a, b are available from the authors. |

| No. | Independent Variables a | Dependent Variables b | |||
|---|---|---|---|---|---|
| X1 | X2 | X3 | Y1 | Y2 | |
| 1 | 9.00 | 7.00 | 17.50 | 91.13 | 129.06 |
| 2 | 10.78 | 8.19 | 21.96 | 70.64 | 279.57 |
| 3 | 10.78 | 5.81 | 21.96 | 76.11 | 222.36 |
| 4 | 10.78 | 8.19 | 13.04 | 69.97 | 266.68 |
| 5 | 9.00 | 7.00 | 17.50 | 87.71 | 131.65 |
| 6 | 9.00 | 7.00 | 10.00 | 70.55 | 234.63 |
| 7 | 9.00 | 7.00 | 17.50 | 90.36 | 123.33 |
| 8 | 7.22 | 5.81 | 21.96 | 64.57 | 241.97 |
| 9 | 9.00 | 7.00 | 17.50 | 84.56 | 103.69 |
| 10 | 9.00 | 5.00 | 17.50 | 73.98 | 220.45 |
| 11 | 9.00 | 9.00 | 17.50 | 71.62 | 306.27 |
| 12 | 6.00 | 7.00 | 17.50 | 72.29 | 307.67 |
| 13 | 7.22 | 5.81 | 13.04 | 69.87 | 232.53 |
| 14 | 7.22 | 8.19 | 13.04 | 72.21 | 297.93 |
| 15 | 7.22 | 8.19 | 21.96 | 72.31 | 318.17 |
| 16 | 9.00 | 7.00 | 17.50 | 88.56 | 124.88 |
| 17 | 10.78 | 5.81 | 13.04 | 79.14 | 275.19 |
| 18 | 9.00 | 7.00 | 25.00 | 74.19 | 197.38 |
| 19 | 12.00 | 7.00 | 17.50 | 76.69 | 320.37 |
| 20 | 9.00 | 7.00 | 17.50 | 86.69 | 101.36 |
| Source | Sum of Squares | Df | Mean Square | F Value | p-Value Prob. > F | |
|---|---|---|---|---|---|---|
| Model | 1186.40 | 9 | 131.82 | 28.66 | <0.0001 | significant |
| X1 | 43.24 | 1 | 43.24 | 9.40 | 0.0119 | |
| X2 | 5.33 | 1 | 5.33 | 1.16 | 0.3072 | |
| X3 | 0.15 | 1 | 0.15 | 0.033 | 0.8596 | |
| X1X2 | 76.38 | 1 | 76.38 | 16.60 | 0.0022 | |
| X1X3 | 1.01 | 1 | 1.01 | 0.22 | 0.6497 | |
| X2X3 | 10.35 | 1 | 10.35 | 2.25 | 0.1645 | |
| X12 | 350.73 | 1 | 350.73 | 76.24 | <0.0001 | |
| X22 | 440.83 | 1 | 440.83 | 95.83 | <0.0001 | |
| X32 | 465.40 | 1 | 465.40 | 101.17 | <0.0001 | |
| Residual | 46.00 | 10 | 4.60 | |||
| Lack of fit | 16.86 | 5 | 3.37 | 0.58 | 0.58 | not significant |
| Pure error | 29.14 | 5 | 5.83 | |||
| Cor total | 1232.41 | 19 |
| Source | Sum of Squares | Df | Mean Square | F Value | p-Value Prob. > F | |
|---|---|---|---|---|---|---|
| Model | 1.111 × 105 | 9 | 12,340.24 | 61.51 | <0.0001 | significant |
| X1 | 47.39 | 1 | 47.39 | 0.24 | 0.6374 | |
| X2 | 8199.41 | 1 | 8199.41 | 40.87 | <0.0001 | |
| X3 | 389.21 | 1 | 389.21 | 1.94 | 0.1938 | |
| X1X2 | 1078.80 | 1 | 1078.80 | 5.38 | 0.0428 | |
| X1X3 | 605.87 | 1 | 605.87 | 3.02 | 0.1129 | |
| X2X3 | 731.91 | 1 | 731.91 | 3.65 | 0.0852 | |
| X12 | 65,823.24 | 1 | 65,823.24 | 328.11 | <0.0001 | |
| X22 | 35557.22 | 1 | 35,557.22 | 177.24 | <0.0001 | |
| X23 | 15,626.98 | 1 | 15,626.98 | 77.90 | <0.0001 | |
| Residual | 2006.12 | 10 | 200.61 | |||
| Lack of fit | 1146.01 | 5 | 229.20 | 1.33 | 0.3803 | Not significant |
| Pure error | 860.11 | 5 | 172.02 | |||
| Cor total | 1.131 × 105 | 19 |
| Index | Predicted Value | Actual Value | Deviation% |
|---|---|---|---|
| EE (%) | 87.56 | 89.73 ± 3.45 | 2.47 |
| Size (nm) | 129.04 | 128.01 ± 5.91 | 0.79 |
| Tissue | Formulation | AUC0→∞ (μg min mL−1) | MRT (min) | Tmax (min) | Cmax (μg mL−1) | CL (L/min/k) | re | DTI |
|---|---|---|---|---|---|---|---|---|
| Plasma | GG-inj | 349.59 | 61.25 | 5 | 5.56 | 0.0194 | ||
| GG-LP | 991.58 | 121.69 | 5 | 14.84 a,c | 0.0066 | |||
| GGB-LP | 1256.81 | 152.17 | 5 | 15.24 a,b | 0.0052 | |||
| Brain | GG-inj | 41.65 | 62.49 | 10 | 0.99 | 0.1562 | ||
| GG-LP | 136.85 | 105.08 | 15 | 2.60 a,c | 0.0488 | 3.29 | 1.16 | |
| GGB-LP | 272.12 | 134.95 | 15 | 3.39 a,b | 0.0239 | 6.53 | 1.82 | |
| Lung | GG-inj | 289.67 | 117.20 | 5 | 4.53 | 0.0224 | ||
| GG-LP | 308.80 | 66.25 | 5 | 6.20 | 0.0210 | 1.07 | 0.38 | |
| GGB-LP | 387.97 | 110.62 | 5 | 5.56 | 0.0167 | 1.34 | 0.37 | |
| Heart | GG-inj | 203.30 | 93.96 | 5 | 3.82 | 0.0319 | ||
| GG-LP | 283.04 | 68.34 | 5 | 5.07 | 0.0229 | 1.39 | 0.49 | |
| GGB-LP | 259.79 | 85.81 | 5 | 4.07 | 0.0250 | 1.28 | 0.36 | |
| Liver | GG-inj | 181.94 | 129.53 | 5 | 3.06 | 0.0357 | ||
| GG-LP | 303.15 | 66.19 | 5 | 6.09 | 0.0214 | 1.67 | 0.59 | |
| GGB-LP | 269.34 | 80.08 | 5 | 4.59 | 0.0241 | 1.48 | 0.41 | |
| Spleen | GG-inj | 242.15 | 94.53 | 5 | 4.12 | 0.0268 | ||
| GG-LP | 302.11 | 70.30 | 5 | 4.79 | 0.0215 | 1.25 | 0.44 | |
| GGB-LP | 261.93 | 75.79 | 5 | 4.28 | 0.0248 | 1.08 | 0.30 | |
| Kidney | GG-inj | 368.58 | 67.36 | 5 | 6.23 | 0.0176 | ||
| GG-LP | 319.93 | 72.15 | 5 | 5.48 | 0.0203 | 0.87 | 0.31 | |
| GGB-LP | 287.46 | 106.81 | 5 | 4.36 | 0.0226 | 0.78 | 0.22 |
| Independent Variables | Levels | ||||
|---|---|---|---|---|---|
| −1.682 | −1 | 0 | +1 | 1.682 | |
| X1 | 6 | 7.22 | 9 | 10.78 | 12 |
| X2 | 5 | 5.81 | 7 | 8.19 | 9 |
| X3 | 10 | 13.04 | 17.50 | 21.96 | 25 |
| Y1 = EE (%) | Maximize | ||||
| Y2 = particile size (nm) | Minimize | ||||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lv, Z.; Yang, Y.; Wang, J.; Chen, J.; Li, J.; Di, L. Optimization of the Preparation Conditions of Borneol-Modified Ginkgolide Liposomes by Response Surface Methodology and Study of Their Blood Brain Barrier Permeability. Molecules 2018, 23, 303. https://doi.org/10.3390/molecules23020303
Lv Z, Yang Y, Wang J, Chen J, Li J, Di L. Optimization of the Preparation Conditions of Borneol-Modified Ginkgolide Liposomes by Response Surface Methodology and Study of Their Blood Brain Barrier Permeability. Molecules. 2018; 23(2):303. https://doi.org/10.3390/molecules23020303
Chicago/Turabian StyleLv, Zhiyang, Yuwei Yang, Jie Wang, Jing Chen, Junsong Li, and Liuqing Di. 2018. "Optimization of the Preparation Conditions of Borneol-Modified Ginkgolide Liposomes by Response Surface Methodology and Study of Their Blood Brain Barrier Permeability" Molecules 23, no. 2: 303. https://doi.org/10.3390/molecules23020303
APA StyleLv, Z., Yang, Y., Wang, J., Chen, J., Li, J., & Di, L. (2018). Optimization of the Preparation Conditions of Borneol-Modified Ginkgolide Liposomes by Response Surface Methodology and Study of Their Blood Brain Barrier Permeability. Molecules, 23(2), 303. https://doi.org/10.3390/molecules23020303




