Fructus Ligustri Lucidi in Osteoporosis: A Review of its Pharmacology, Phytochemistry, Pharmacokinetics and Safety
Abstract
:1. Introduction
2. The Bone-Protective Actions of Fructus Ligustri Lucidi in the Theory of Traditional Chinese Medicine
3. Phytochemistry of Fructus Ligustri Lucidi
4. Pharmacokinetic of Fructus Ligustri Lucidi
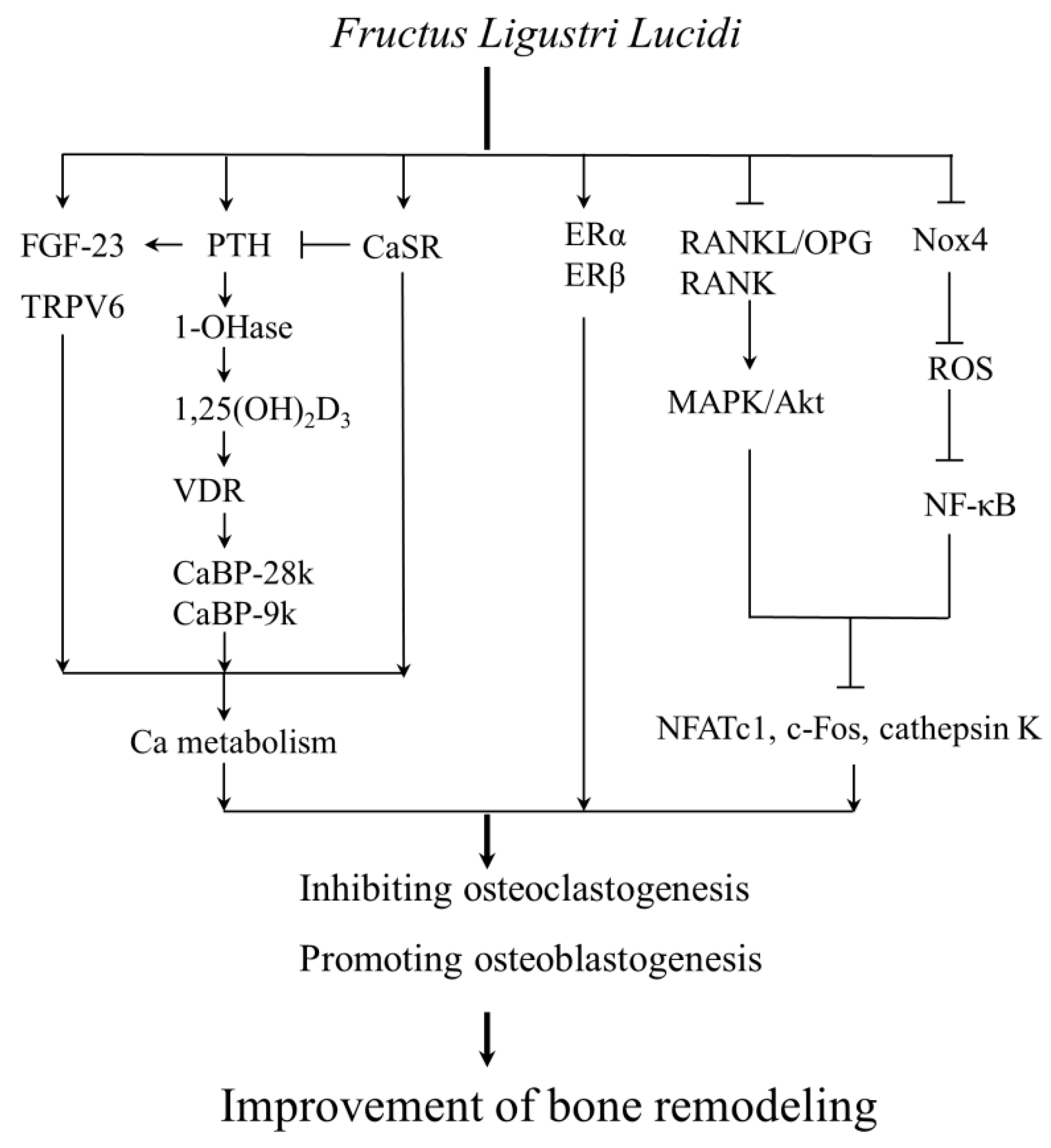
5. Anti-Bone Resorption and Pro-Anabolic Activities of Fructus Ligustri Lucidi in Bone Metabolism and Bone Quality
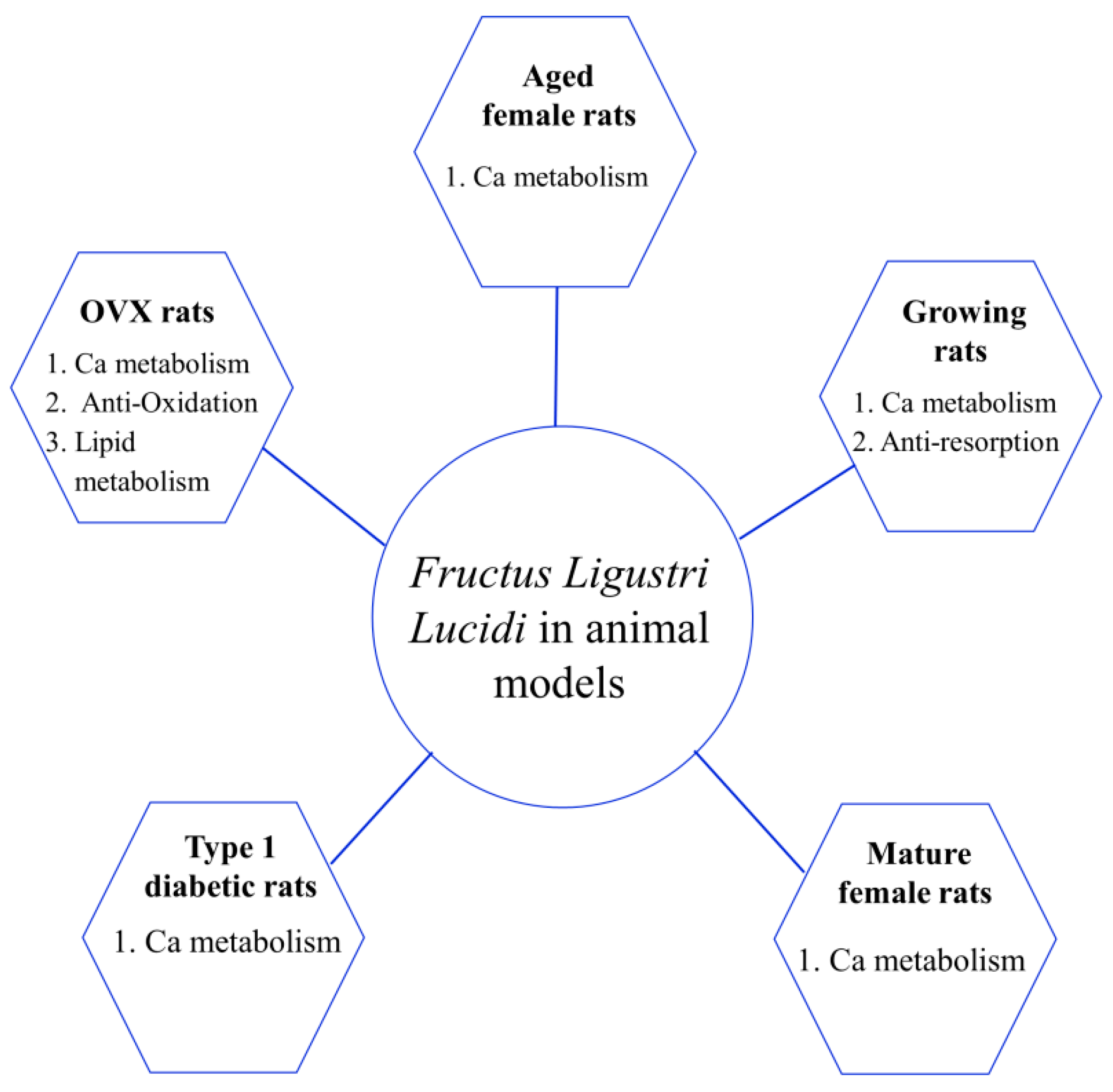
5.1. Effects of Fructus Ligustri Lucidi on Bone Metabolism and Quality in Animal Experiments
5.2. Effects of Fructus Ligustri Lucidi on Osteoblasts
5.3. Effects of Fructus Ligustri Lucidi on Osteoclasts
6. The Toxicity of Fructus Ligustri Lucidi
7. Conclusions and Outlook
Acknowledgments
Conflicts of Interest
Abbreviations
| 1,25-(OH)2D3 | 1,25-Dihydroxyvitamin D3; |
| 1-OHase | 1α-Hydroxylase; |
| ALP | Alkaline phosphatase; |
| AUC0-t | Area under the plasma concentration-time curve from zero (0) h to time (t); |
| BMC | Bone mineral content; |
| BMD | Bone mineral density; |
| Ca | Calcium; |
| CaBP | Calcium binding protein; |
| CaSR | Calcium-sensing receptor; |
| Cmax | Maximum plasma concentration; |
| CO2 | Carbon dioxide; |
| CT | Calcitonin; |
| DPD | Deoxypyridinoline; |
| EAF | Ethyl acetate-soluble fraction of EE; |
| ER | Estrogen receptor; |
| ERE | Estrogen receptor α/β-mediated estrogen response element; |
| FGF-23 | Fibroblast growth factor-23; |
| FLL | Fructus Ligustri Lucidi; |
| FLL-EAF | Ethyl acetate-soluble fraction of EE; |
| FLL-EE | FLL ethanol extract; |
| FLL-WF | Water-soluble fraction of EE; |
| K | Drug clearance rate constant from the central chamber to the outside in the one-compartment model. |
| MRT | The average time of drug molecules retained in vivo after rapid intravenous infusion; |
| Nox4 | NADPH oxidase 4; |
| NFATc1 | Nuclear factor of activated T cell-c1; |
| NF-κB | Nuclear factor of kappa B; |
| OA | Oleanolic acid; |
| OCN | Osteocalcin; |
| OPG | Osteoprotegerin; |
| OVX | ovariectomized; |
| PTH | Parathyroid hormone; |
| RANK | Receptor activator of nuclear factor kappa B; |
| RANKL | Receptor activator of nuclear factor kappa B ligand; |
| ROS | Reactive oxygen species; |
| T1/2 | The time taken a drug to clear from the highest concentration to half of this level; |
| TCM | Traditional Chinese Medicine; |
| Tmax | Time at maximum plasma concentration; |
| TRAP | Tartrate resistant acid phosphatase; |
| TRPV6 | Transient receptor potential vanilloid 6; |
| UA | Ursolic acid; |
| VDR | Vitamin D receptor. |
References
- Chen, G.; Wang, C.; Wang, J.; Yin, S.; Gao, H.; Xiang, L.; Liu, H.; Xiong, Y.; Wang, P.; Zhu, X.; et al. Antiosteoporotic effect of icariin in ovariectomized rats is mediated via the Wnt/beta-catenin pathway. Exp. Ther. Med. 2016, 12, 279–287. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Peng, Q.; Liu, Q.; Hu, J.; Tang, Z.; Cui, L.; Lin, Z.; Xu, B.; Lu, K.; Yang, F.; et al. Antioxidant activity against H2O2-induced cytotoxicity of the ethanol extract and compounds from Pyrola decorate leaves. Pharm. Biol. 2017, 55, 1843–1848. [Google Scholar] [CrossRef] [PubMed]
- Harvey, N.; Dennison, E.; Cooper, C. Osteoporosis: Impact on health and economics. Nat. Rev. Rheumatol. 2010, 6, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Cauley, J.A. Public health impact of osteoporosis. J. Gerontol. A Biol. Sci. Med. Sci. 2013, 68, 1243–1251. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.; Ma, R.; Wang, L.; Zhu, R.; Liu, H.; Guo, Y.; Zhao, B.; Zhao, S.; Tang, J.; Li, Y.; et al. Rehmanniae Radix in osteoporosis: A review of traditional Chinese medicinal uses, phytochemistry, pharmacokinetics and pharmacology. J. Ethnopharmacol. 2017, 198, 351–362. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Li, Y.; Guo, Y.; Ma, R.; Fu, M.; Niu, J.; Gao, S.; Zhang, D. Herba Epimedii: An Ancient Chinese Herbal Medicine in the Prevention and Treatment of Osteoporosis. Curr. Pharm. Des. 2016, 22, 328–349. [Google Scholar] [CrossRef] [PubMed]
- Pan, Y.; Niu, Y.; Li, C.; Zhai, Y.; Zhang, R.; Guo, X.; Mei, Q. Du-zhong (Eucommia ulmoides) prevents disuse-induced osteoporosis in hind limb suspension rats. Am. J. Chin. Med. 2014, 42, 143–155. [Google Scholar] [CrossRef] [PubMed]
- Pang, Z.T.; Zhou, Z.Y.; Wang, W.; Ma, Y.N.; Niu, F.J.; Zhang, X.L.; Han, C.C. The advances in research on the pharmacological effects of Fructus Ligustri Lucidi. Biomed. Res. Int. 2015, 2015, 281873. [Google Scholar] [CrossRef] [PubMed]
- Han, J.; Wei, L.; Xu, W.; Lu, J.; Wang, C.; Bao, Y.; Jia, W. CTSK inhibitor exert its anti-obesity effects through regulating adipocyte differentiation in high-fat diet induced obese mice. Endocr. J. 2015, 62, 309–317. [Google Scholar] [CrossRef] [PubMed]
- Rampal, S.; Yang, M.H.; Sung, J.; Son, H.J.; Choi, Y.H.; Lee, J.H.; Kim, Y.H.; Chang, D.K.; Rhee, P.L.; Rhee, J.C.; et al. Association between markers of glucose metabolism and risk of colorectal adenoma. Gastroenterology 2014, 147, 78–87. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Mukwaya, E.; Pan, H.; Li, X.M.; Yang, J.L.; Ge, J.; Wang, H.Y. Combination therapy of Chinese herbal medicine Fructus Ligustri Lucidi with high calcium diet on calcium imbalance induced by ovariectomy in mice. Pharm. Biol. 2015, 53, 1082–1085. [Google Scholar] [CrossRef] [PubMed]
- Yu, Z.L.; Zeng, W.C. Antioxidant, antibrowning, and cytoprotective activities of Ligustrum robustum (Rxob.). Blume. extract. J. Food Sci. 2013, 78, C1354–C1362. [Google Scholar] [CrossRef] [PubMed]
- Tan, X.L.; Zhang, Y.H.; Cai, J.P.; Zhu, L.H.; Ge, W.J.; Zhang, X. 5-(Hydroxymethyl)-2-furaldehyde inhibits adipogenic and enhances osteogenic differentiation of rat bone mesenchymal stem cells. Nat. Prod. Commun. 2014, 9, 529–532. [Google Scholar] [PubMed]
- Cai, J.; Zheng, T.; Zhang, L.; Tian, Y.; Yang, M.H.; Du, J. Effects of Herba epimedii and Fructus Ligustri Lucidi on the transcription factors in hypothalamus of aged rats. Chin. J. Integr. Med. 2011, 17, 758–763. [Google Scholar] [CrossRef] [PubMed]
- Hu, M.; Wang, X.; Yan, F.; Gao, F.; Ju, J. Advances in retinol-binding protein 4. Chin. J. Gastroenterol. Hepatol. 2015, 24, 879–882. [Google Scholar]
- Gao, Z.; Lu, Y.; Halmurat, U.; Jing, J.; Xu, D. Study of osteoporosis treatment principles used historically by ancient physicians in Chinese Medicine. Chin. J. Integr. Med. 2013, 19, 862–868. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Li, Y.; Xue, L.; Severino, R.P.; Gao, S.; Niu, J.; Qin, L.P.; Zhang, D.; Bromme, D. Salvia miltiorrhiza: An ancient Chinese herbal medicine as a source for anti-osteoporotic drugs. J. Ethnopharmacol. 2014, 155, 1401–1416. [Google Scholar] [CrossRef] [PubMed]
- He, F.Y.; Deng, K.W.; Yang, Y.T.; Zhou, Y.Q.; Shi, J.L.; Liu, W.L.; Tang, Y. Study on meridian tropism of medicinal property theory for Chines medicines by supramolecular chemistry (I). Zhongguo Zhong Yao Za Zhi 2015, 40, 1624–1629. [Google Scholar] [PubMed]
- Guo, Y.B.; Wang, L.L.; Ma, R.F.; Zhao, D.D.; Zhang, D.W.; Chen, J.X.; Niu, J.Z. Etiology, Pathology and Prospects of TCM in Osteoporosis Treatment. Mod. Tradit. Chin. Med. Mater. Med.-World Sci. Technol. 2015, 17, 768–772. [Google Scholar]
- Guo, Y.; Ma, R.; Wang, L.; Liu, H.; Zhu, R.; Shi, R.; Zhao, D.; Mo, F.; Gao, S.; Zhang, D. Research progress on effects and their mechanism of Ligustri Lucidi Fructus treat. osteoporosis. Chin. Tradit. Herb. Drugs 2016, 47, 851–856. [Google Scholar]
- Yang, Y.; Nian, H.; Tang, X.; Wang, X.; Liu, R. Effects of the combined Herba Epimedii and Fructus Ligustri Lucidi on bone turnover and TGF-beta1/Smads pathway in GIOP rats. J. Ethnopharmacol. 2017, 201, 91–99. [Google Scholar] [CrossRef] [PubMed]
- Chan, B.C.; Lee, H.Y.; Siu, W.S.; Yip, K.H.; Ko, C.H.; Lau, C.B.; Leung, P.C.; Lau, H.Y. Suppression of mast cell activity contributes to the osteoprotective effect of an herbal formula containing Herba Epimedii, Fructus Ligustri Lucidi and Fructus Psoraleae. J. Pharm. Pharmacol. 2014, 66, 437–444. [Google Scholar] [CrossRef] [PubMed]
- Sun, W.; Wang, Y.Q.; Yan, Q.; Lu, R.; Shi, B. Effects of Er-Zhi-Wan on microarchitecture and regulation of Wnt/beta-catenin signaling pathway in alveolar bone of ovariectomized rats. J. Huazhong Univ. Sci. Technol. Med. Sci. 2014, 34, 114–119. [Google Scholar] [CrossRef] [PubMed]
- Dong, X.L.; Cao, S.S.; Gao, Q.G.; Feng, H.T.; Wong, M.S.; Denney, L. Combination treatment with Fructus Ligustri Lucidi and Puerariae radix offsets their independent actions on bone and mineral metabolism in ovariectomized rats. Menopause 2014, 21, 286–294. [Google Scholar] [CrossRef] [PubMed]
- Kang, X.; Li, Z.; Zhang, W.H.; Zhou, Q.; Liu, R.H.; Wang, X.J. [Study on effect of combination of Epimedii Folium and Ligustri Lucidi Fructus on osteoporosis rats induced by retinoic acid]. Zhongguo Zhong Yao Za Zhi 2013, 38, 4124–4128. [Google Scholar] [PubMed]
- Leung, P.C.; Siu, W.S. Herbal treatment for osteoporosis: A current review. J. Tradit. Complement. Med. 2013, 3, 82–87. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.; Li, C.; Wang, Z.; Liu, X.; You, Y.; Wei, H.; Guo, T. Ligustri lucidi fructus as a traditional Chinese medicine: A review of its phytochemistry and pharmacology. Nat. Prod. Res. 2015, 29, 493–510. [Google Scholar] [CrossRef] [PubMed]
- Jin, H. Present situation of chemical compositions of Fructus Ligustri Lucidi. J. Jilin Inst. Chem. Techinol. 2008, 25, 35–37. [Google Scholar]
- Liu, L.; Wang, X. Solubility of Oleanolic Acid in Various Solvents from (288.3 to 328.3) K. J. Chem. Eng. Data 2007, 52, 2527–2528. [Google Scholar] [CrossRef]
- Liu, T.; Wang, M. Research Progress of Chemical Composition and Pharmacological Effects of Fructus Figustri Lucidi. Chin. J. Exp. Tradit. Med. Formul. 2014, 13, 228–234. [Google Scholar]
- Fan, J.; Kong, T.; Zhang, L.; Tong, S.; Tian, Z.; Duan, Y.; Zhang, X. Solubilities of Ursolic Acid and Oleanolic Acid in Four Solvents from (283.2 to 329.7) K. J. Chem. Eng. Data 2011, 56, 2723–2725. [Google Scholar] [CrossRef]
- Jager, S.; Winkler, K.; Pfuller, U.; Scheffler, A. Solubility studies of oleanolic acid and betulinic acid in aqueous solutions and plant extracts of Viscum album L. Planta Med. 2007, 73, 157–162. [Google Scholar] [CrossRef] [PubMed]
- Han, S.K.; Ko, Y.I.; Park, S.J.; Jin, I.J.; Kim, Y.M. Oleanolic acid and ursolic acid stabilize liposomal membranes. Lipids 1997, 32, 769–773. [Google Scholar] [CrossRef] [PubMed]
- Su, D.; Gao, Y.Q.; Dai, W.B.; Hu, Y.; Wu, Y.F.; Mei, Q.X. Helicteric Acid, Oleanic Acid, and Betulinic Acid, Three Triterpenes from Helicteres angustifolia L., Inhibit Proliferation and Induce Apoptosis in HT-29 Colorectal Cancer Cells via Suppressing NF-kappaB and STAT3 Signaling. Evid. Based Complement. Alternat. Med. 2017, 2017, 5180707. [Google Scholar] [CrossRef] [PubMed]
- Munhoz, A.C.M.; Frode, T.S. Isolated Compounds from Natural Products with Potential Antidiabetic Activity-a Systematic Review. Curr. Diabetes Rev. 2017. [Google Scholar] [CrossRef] [PubMed]
- Silva, F.S.; Oliveira, P.J.; Duarte, M.F. Oleanolic, Ursolic, and Betulinic Acids as Food Supplements or Pharmaceutical Agents for Type 2 Diabetes: Promise or Illusion? J. Agric. Food Chem. 2016, 64, 2991–3008. [Google Scholar] [CrossRef] [PubMed]
- Ramirez-Rodriguez, A.M.; Gonzalez-Ortiz, M.; Martinez-Abundis, E.; Acuna-Ortega, N. Effect of Ursolic Acid on Metabolic Syndrome, Insulin Sensitivity, and Inflammation. J. Med. Food 2017, 20. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.U.; Park, S.J.; Kwak, H.B.; Oh, J.; Min, Y.K.; Kim, S.H. Anabolic activity of ursolic acid in bone: Stimulating osteoblast differentiation in vitro and inducing new bone formation in vivo. Pharmacol. Res. 2008, 58, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Wozniak, L.; Skapska, S.; Marszalek, K. Ursolic Acid-A Pentacyclic Triterpenoid with a Wide Spectrum of Pharmacological Activities. Molecules 2015, 20, 20614–20641. [Google Scholar] [CrossRef] [PubMed]
- Yao, W.; Dai, J.; Zheng, C.; Bao, B.; Cheng, H.; Zhang, L.; Ding, A.; Li, W. Quality assessment of Fructus Ligustri Lucidi by the simultaneous determination of six compounds and chemometric analysis. J. Sep. Sci. 2015, 38, 1822–1827. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Liu, M.; Feng, W. The determination of oleanolic acid contentin in the different parts of Fructus Ligustri Lucidi. Chin. J. Chin. Mater. Med. 1995, 20, 216–217. [Google Scholar]
- Shi, L.; Ma, Y.; Cai, Z. Quantitative determination of salidroside and specnuezhenide in the fruits of Ligustrum lucidum Ait by high performance liquid chromatography. Biomed. Chromatogr. 1998, 12, 27–30. [Google Scholar] [CrossRef]
- Wu, D.; Yang, X.; Zheng, T.; Xing, S.; Wang, J.; Chi, J.; Bian, F.; Li, W.; Xu, G.; Bai, X.; et al. A novel mechanism of action for salidroside to alleviate diabetic albuminuria: Effects on albumin transcytosis across glomerular endothelial cells. Am. J. Physiol. Endocrinol. Metab. 2016, 310, E225–E237. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.R.; Fu, X.J.; Zhu, D.S.; Zhang, C.Z.; Hou, S.; Li, M.; Yang, X.H. Salidroside-regulated lipid metabolism with down-regulation of miR-370 in type 2 diabetic mice. Eur. J. Pharmacol. 2016, 779, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Fan, X.J.; Wang, Y.; Wang, L.; Zhu, M. Salidroside induces apoptosis and autophagy in human colorectal cancer cells through inhibition of PI3K/Akt/mTOR pathway. Oncol. Rep. 2016, 36, 3559–3567. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Qu, Y.; Jin, X.; Guo, X.Q.; Wang, Y.; Qi, L.; Yang, J.; Zhang, P.; Li, L.Z. Protective effect of salidroside against bone loss via hypoxia-inducible factor-1alpha pathway-induced angiogenesis. Sci. Rep. 2016, 6, 32131. [Google Scholar] [CrossRef] [PubMed]
- Zhu, L.; Chen, T.; Chang, X.; Zhou, R.; Luo, F.; Liu, J.; Zhang, K.; Wang, Y.; Yang, Y.; Long, H.; et al. Salidroside ameliorates arthritis-induced brain cognition deficits by regulating Rho/ROCK/NF-kappaB pathway. Neuropharmacology 2016, 103, 134–142. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.G.; Wang, J.W.; Bai, Y.G.; Liu, M.; Xie, M.J.; Dai, Z.J. Salidroside contributes to reducing blood pressure and alleviating cerebrovascular contractile activity in diabetic Goto-Kakizaki Rats by inhibition of L-type calcium channel in smooth muscle cells. BMC Pharmacol. Toxicol. 2017, 18, 30. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.; Zou, L.; Yu, X.; Chen, M.; Guo, R.; Cai, H.; Yao, D.; Xu, X.; Chen, Y.; Ding, C.; et al. Salidroside attenuates chronic hypoxia-induced pulmonary hypertension via adenosine A2a receptor related mitochondria-dependent apoptosis pathway. J. Mol. Cell. Cardiol. 2015, 82, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Chang, X.; Zhang, K.; Zhou, R.; Luo, F.; Zhu, L.; Gao, J.; He, H.; Wei, T.; Yan, T.; Ma, C. Cardioprotective effects of salidroside on myocardial ischemia-reperfusion injury in coronary artery occlusion-induced rats and Langendorff-perfused rat hearts. Int. J. Cardiol. 2016, 215, 532–544. [Google Scholar] [CrossRef] [PubMed]
- Chen, Q.; Yang, L.; Zhang, G.; Wang, F. Bioactivity-guided Isolation of antiosteoporotic compounds from Ligustrum lucidum. Phytother. Res. 2013, 27, 973–979. [Google Scholar] [CrossRef] [PubMed]
- He, Z.D.; But, P.P.H.; Chan, T.W.; Dong, H.; Xu, H.X.; Lau, C.P.; Sun, H.D. Antioxidative glucosides from the fruits of Ligustrum lucidum. Chem. Pharm. Bull. (Tokyo) 2001, 49, 780–784. [Google Scholar] [CrossRef] [PubMed]
- Ju, H.Y.; Chen, S.C.; Wu, K.J.; Kuo, H.C.; Hseu, Y.C.; Ching, H.; Wu, C.R. Antioxidant phenolic profile from ethyl acetate fraction of Fructus Ligustri Lucidi with protection against hydrogen peroxide-induced oxidative damage in SH-SY5Y cells. Food Chem. Toxicol. 2012, 50, 492–502. [Google Scholar] [CrossRef] [PubMed]
- National Pharmacopoeia Committee. The Pharmacopoeia of the People’s Republic of China; China Medical Science Press: Beijing, China, 2015.
- Peng, P.; Zhao, L.; Liu, B.; Jiang, Y.; Feng, D.; Sun, D.; Yang, S.; Zhu, N.; Shi, R. Pharmacokinetic characterization of salidroside extract from Ligustri Lucidi Fructus in rats. Glob. Tradit. Chin. Med. 2015, 8, 281–285. [Google Scholar]
- Peng, P.; Feng, D.; Sun, D.; Yang, S.; Zhao, L.; Zhu, N.; Jiang, Y.; Chang, H.; Liu, B.; Shi, R. Pharmacokinetic characteristics and correlation analysis of preparations of salidroside from Fructus Ligustri Lucidi and two pure bioactive components in rat model of migraine. J. Beijing Univ. Tradit. Chin. Med. 2014, 37, 696–700. [Google Scholar]
- Peng, P.; Sun, D.; Feng, D.; Zhao, L.; Yang, S.; Zhu, N.; Zhang, L.; Li, H.; She, G.; Shi, R. Study on the pharmacokinetic characterization of salidroside drugs in the insomnia model rats. Glob. Tradit. Chin. Med. 2015, 8, 286–289. [Google Scholar]
- Zhang, Y.; Lai, W.P.; Leung, P.C.; Wu, C.F.; Yao, X.S.; Wong, M.S. Effects of Fructus Ligustri Lucidi extract on bone turnover and calcium balance in ovariectomized rats. Biol. Pharm. Bull. 2006, 29, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Leung, P.C.; Che, C.T.; Chow, H.K.; Wu, C.F.; Wong, M.S. Improvement of bone properties and enhancement of mineralization by ethanol extract of Fructus Ligustri Lucidi. Br. J. Nutr. 2008, 99, 494–502. [Google Scholar] [CrossRef] [PubMed]
- Dong, X.L.; Zhang, Y.; Favus, M.J.; Che, C.T.; Wong, M.S. Ethanol extract of Fructus Ligustri Lucidi increases circulating 1,25-dihydroxyvitamin D3 by inducing renal 25-hydroxyvitamin D-1alpha hydroxylase activity. Menopause 2010, 17, 1174–1181. [Google Scholar] [CrossRef] [PubMed]
- Feng, X.; Lyu, Y.; Wu, Z.; Fang, Y.; Xu, H.; Zhao, P.; Xu, Y.; Feng, H. Fructus ligustri lucidi ethanol extract improves bone mineral density and properties through modulating calcium absorption-related gene expression in kidney and duodenum of growing rats. Calcif. Tissue Int. 2014, 94, 433–441. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Ma, R.; Guo, Y.; Sun, J.; Liu, H.; Zhu, R.; Liu, C.; Li, J.; Li, L.; Chen, B.; et al. Antioxidant Effect of Fructus Ligustri Lucidi Aqueous Extract in Ovariectomized Rats Is Mediated through Nox4-ROS-NF-kappaB Pathway. Front. Pharmacol. 2017, 8, 266. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Wang, L.; Ma, R.; Wang, L.; Yang, M.; Tang, Y.; Liu, C.; Zhu, R.; Liu, H.; Zhao, D.; et al. Effects of water extract from Fructus Ligustri Lucidi on bone structure and metabolism in ovariectomized rats. Chin. Tradit. Herb. Drugs 2016, 47, 1155–1162. [Google Scholar]
- Cheng, M.; Wang, Q.; Liu, X.; Deng, Y.; Jia, C. Treatment with FLL for osteoporosis in ovariectomized rats. Chin. Pharmacol. Bull. 2013, 29, 229–233. [Google Scholar]
- Dong, X.L.; Zhao, M.; Wong, K.K.; Che, C.T.; Wong, M.S. Improvement of calcium balance by Fructus Ligustri Lucidi extract in mature female rats was associated with the induction of serum parathyroid hormone levels. Br. J. Nutr. 2012, 108, 92–101. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Diao, T.Y.; Wang, L.; Che, C.T.; Wong, M.S. Protective effects of water fraction of Fructus Ligustri Lucidi extract against hypercalciuria and trabecular bone deterioration in experimentally type 1 diabetic mice. J. Ethnopharmacol. 2014, 158, 239–245. [Google Scholar] [CrossRef] [PubMed]
- Lyu, Y.; Feng, X.; Zhao, P.; Wu, Z.; Xu, H.; Fang, Y.; Hou, Y.; Denney, L.; Xu, Y.; Feng, H. Fructus Ligustri Lucidi (FLL) ethanol extract increases bone mineral density and improves bone properties in growing female rats. J. Bone Miner. Metab. 2014, 32, 616–626. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Lai, W.P.; Leung, P.C.; Che, C.T.; Wong, M.S. Improvement of Ca balance by Fructus Ligustri Lucidi extract in aged female rats. Osteoporos. Int. 2008, 19, 235–242. [Google Scholar] [CrossRef] [PubMed]
- Svanberg, M.; Knuuttila, M.; Hamalainen, M. Citric acid concentration compared to serum parathyroid hormone, 1,25(OH)2D3 and calcitonin during dietary Ca deficiency and rehabilitation enhanced with xylitol in rats. Miner. Electrolyte Metab. 1993, 19, 103–108. [Google Scholar] [PubMed]
- De Paula, F.J.A.; Rosen, C.J. Back to the future: Revisiting parathyroid hormone and calcitonin control of bone remodeling. Horm. Metab. Res. 2010, 42, 299–306. [Google Scholar] [CrossRef] [PubMed]
- Bronner, F.; Stein, W.D. Calcium homeostasis--an old problem revisited. J. Nutr. 1995, 125, 1987S–1995S. [Google Scholar] [PubMed]
- Fleet, J.C. The role of vitamin D in the endocrinology controlling calcium homeostasis. Mol. Cell. Endocrinol. 2017, 453, 36–45. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Lai, W.P.; Wu, C.F.; Favus, M.J.; Leung, P.C.; Wong, M.S. Ovariectomy worsens secondary hyperparathyroidism in mature rats during low-Ca diet. Am. J. Physiol. Endocrinol. Metab. 2007, 292, E723–E731. [Google Scholar] [CrossRef] [PubMed]
- Chau, T.S.; Lai, W.P.; Cheung, P.Y.; Favus, M.J.; Wong, M.S. Age-related alteration of vitamin D metabolism in response to low-phosphate diet in rats. Br. J. Nutr. 2005, 93, 299–307. [Google Scholar] [CrossRef] [PubMed]
- Ma, R.; Wang, L.; Zhao, B.; Liu, C.; Liu, H.; Zhu, R.; Chen, B.; Li, L.; Zhao, D.; Mo, F.; et al. Diabetes Perturbs Bone Microarchitecture and Bone Strength through Regulation of Sema3A/IGF-1/β-Catenin in Rats. Cell. Physiol. Biochem. 2017, 41, 55–56. [Google Scholar] [CrossRef] [PubMed]
- Palermo, A.; D’Onofrio, L.; Buzzetti, R.; Manfrini, S.; Napoli, N. Pathophysiology of Bone Fragility in Patients with Diabetes. Calcif. Tissue Int. 2017, 100, 122–132. [Google Scholar] [CrossRef] [PubMed]
- Starup-Linde, J.; Frost, M.; Vestergaard, P.; Abrahamsen, B. Epidemiology of Fractures in Diabetes. Calcif. Tissue Int. 2017, 100, 109–121. [Google Scholar] [CrossRef] [PubMed]
- Napoli, N.; Chandran, M.; Pierroz, D.D.; Abrahamsen, B.; Schwartz, A.V.; Ferrari, S.L.; IOF Bone and Diabetes Working Group. Mechanisms of diabetes mellitus-induced bone fragility. Nat. Rev. Endocrinol. 2017, 13, 208–219. [Google Scholar] [CrossRef] [PubMed]
- Ghodsi, M.; Larijani, B.; Keshtkar, A.A.; Nasli-Esfahani, E.; Alatab, S.; Mohajeri-Tehrani, M.R. Mechanisms involved in altered bone metabolism in diabetes: A narrative review. J. Diabetes Metab. Disord. 2016, 15, 52. [Google Scholar] [CrossRef] [PubMed]
- Kalaitzoglou, E.; Popescu, I.; Bunn, R.C.; Fowlkes, J.L.; Thrailkill, K.M. Effects of Type 1 Diabetes on Osteoblasts, Osteocytes, and Osteoclasts. Curr. Osteoporos. Rep. 2016, 14, 310–319. [Google Scholar] [CrossRef] [PubMed]
- Ma, R.; Zhu, R.; Wang, L.; Guo, Y.; Liu, C.; Liu, H.; Liu, F.; Li, H.; Li, Y.; Fu, M.; et al. Diabetic Osteoporosis: A Review of Its Traditional Chinese Medicinal Use and Clinical and Preclinical Research. Evid. Based Complement. Alternat. Med. 2016, 2016, 3218313. [Google Scholar] [CrossRef] [PubMed]
- Yuan, Q.; Sato, T.; Densmore, M.; Saito, H.; Schuler, C.; Erben, R.G.; Lanske, B. FGF-23/Klotho signaling is not essential for the phosphaturic and anabolic functions of PTH. J. Bone Miner. Res. 2011, 26, 2026–2035. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.J.; Ritter, C.S. The vitamin D analog 1alpha; 25-Dihydroxy-2beta-(3-Hydroxypropyloxy) vitamin D(3) (Eldecalcitol) is a potent regulator of calcium and phosphate metabolism. Calcif. Tissue Int. 2011, 89, 372–378. [Google Scholar] [CrossRef] [PubMed]
- Areco, V.; Rivoira, M.A.; Rodriguez, V.; Marchionatti, A.M.; Carpentieri, A.; De Tolosa, N.T. Dietary and pharmacological compounds altering intestinal calcium absorption in humans and animals. Nutr. Res. Rev. 2015, 28, 83–99. [Google Scholar] [CrossRef] [PubMed]
- Conigrave, A.D. The Calcium-Sensing Receptor and the Parathyroid: Past, Present, Future. Front. Physiol. 2016, 7, 563. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Zhang, X. Receptor activator of nuclear factor-kappaB ligand (RANKL)/RANK/osteoprotegerin system in bone and other tissues (review). Mol. Med. Rep. 2015, 11, 3212–3218. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, R.R.; Diaz, M.M.; Santos, T.V.; Bernardes, J.T.; Peixoto, L.G.; Bocanegra, O.L.; Neto, M.B.; Espindola, F.S. Chronic stress induces a hyporeactivity of the autonomic nervous system in response to acute mental stressor and impairs cognitive performance in business executives. PLoS ONE 2015, 10, e0119025. [Google Scholar] [CrossRef] [PubMed]
- Dai, P.; Mao, Y.; Sun, X.; Li, X.; Muhammad, I.; Gu, W.; Zhang, D.; Zhou, Y.; Ma, J.; Ni, Z.; Huang, S. Attenuation of Oxidative Stress-Induced Osteoblast Apoptosis by Curcumin is Associated with Preservation of Mitochondrial Functions and Increased Akt-GSK3beta Signaling. Cell. Physiol. Biochem. 2017, 41, 661–677. [Google Scholar] [CrossRef] [PubMed]
- Tian, L.; Yu, X. Lipid metabolism disorders and bone dysfunction-interrelated and mutually regulated (review). Mol. Med. Rep. 2015, 12, 783–794. [Google Scholar] [CrossRef] [PubMed]
- Guido, G.; Scaglione, M.; Fabbri, L.; Ceglia, M.J. The “osteoporosis disease”. Clin. Cases Miner. Bone Metab. 2009, 6, 114–116. [Google Scholar] [PubMed]
- Marie, P.J.; Kassem, M. Osteoblasts in osteoporosis: Past, emerging, and future anabolic targets. Eur. J. Endocrinol. 2011, 165, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Martin, T.J.; Sims, N.A. RANKL/OPG; Critical role in bone physiology. Rev. Endocr. Metab. Disord. 2015, 16, 131–139. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Fan, Y.S.; Gao, Z.Q.; Fan, K.; Liu, Z.J. Effect of Fructus Ligustri Lucidi on osteoblastic like cell-line MC3T3-E1. J. Ethnopharmacol. 2015, 170, 88–95. [Google Scholar] [CrossRef] [PubMed]
- Hao, Y.; Liu, C.; Huang, J.; Gu, Y.; Li, H.; Yang, Z.; Liu, J.; Wang, W.; Li, R. Ghrelin protects against depleted uranium-induced apoptosis of MC3T3-E1 cells through oxidative stress-mediated p38-mitogen-activated protein kinase pathway. Toxicol. Appl. Pharmacol. 2016, 290, 116–125. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.H.; Cai, W.J.; Wen, H.; Sha, L.Q.; Zhao, C.W.; Zhang, T.Z.; Zhao, W.H. Pilose antler peptide protects osteoblasts from inflammatory and oxidative injury through EGF/EGFR signaling. Int. J. Biol. Macromol. 2017, 99, 15–20. [Google Scholar]
- Monroe, D.G.; Secreto, F.J.; Subramaniam, M.; Getz, B.J.; Khosla, S.; Spelsberg, T.C. Estrogen receptor alpha and beta heterodimers exert unique effects on estrogen- and tamoxifen-dependent gene expression in human U2OS osteosarcoma cells. Mol. Endocrinol 2005, 19, 1555–1568. [Google Scholar] [CrossRef] [PubMed]
- Miki, Y.; Suzuki, T.; Hatori, M.; Igarashi, K.; Aisaki, K.I.; Kanno, J.; Nakamura, Y.; Uzuki, M.; Sawai, T.; Sasano, H. Effects of aromatase inhibitors on human osteoblast and osteoblast-like cells: A possible androgenic bone protective effects induced by exemestane. Bone 2007, 40, 876–887. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Chen, Q.; Yang, L.; Wang, F. Effects of Aqueous Extract of Fructus Ligustri Lucidi on the Proliferation and Differentiation of Osteoblastic UMR-106 cells. Nat. Prod. Res. Dev. 2011, 23, 232–235. [Google Scholar]
- Shen, P.; Guo, B.L.; Gong, Y.; Hong, D.Y.; Hong, Y.; Yong, E.L. Taxonomic, genetic, chemical and estrogenic characteristics of Epimedium species. Phytochemistry 2007, 68, 1448–1458. [Google Scholar] [CrossRef] [PubMed]
- Michalski, M.N.; McCauley, L.K. Macrophages and skeletal health. Pharmacol. Ther. 2017, 174, 43–54. [Google Scholar] [CrossRef] [PubMed]
- Xu, D.; Lyu, Y.; Chen, X.; Zhu, X.; Feng, J.; Xu, Y. Fructus Ligustri Lucidi ethanol extract inhibits osteoclastogenesis in RAW264.7 cells via the RANKL signaling pathway. Mol. Med. Rep. 2016, 14, 4767–4774. [Google Scholar] [CrossRef] [PubMed]
- Lin, M.; Zhang, W.; Su, J. Toxic polyacetylenes in the genus Bupleurum (Apiaceae)-Distribution, toxicity, molecular mechanism and analysis. J. Ethnopharmacol. 2016, 193, 566–573. [Google Scholar] [CrossRef] [PubMed]
- Zhou, M.; Hong, Y.; Lin, X.; Shen, L.; Feng, Y. Recent pharmaceutical evidence on the compatibility rationality of traditional Chinese medicine. J. Ethnopharmacol. 2017, 206, 363–375. [Google Scholar] [CrossRef] [PubMed]
- Frenzel, C.; Teschke, R. Herbal Hepatotoxicity: Clinical Characteristics and Listing Compilation. Int. J. Mol. Sci. 2016, 17. [Google Scholar] [CrossRef] [PubMed]
- Dong, Q.; Shan, A.; Liu, H.; Lv, W. Study on acute peroral toxicity and 30 d feeding test of supercritical CO2 extract of Ligustrum lucidum. J. Northeast Agric. Univ. 2011, 42, 29–33. [Google Scholar]
- Dong, Q.; Shan, A.; Shan, Y.P. Genetic toxicity and subacute toxicity tests of supercritical CO2 extract of Ligustrum lucidum in rats. Chin. J. Public Health 2011, 27, 1424–1426. [Google Scholar]
- Xu, L.L.; Shan, A.S.; Chen, Z.H.; Bi, C.P.; Li, F. Acute toxicity of the extract from Ligustrum lucidum in broilers. Chin. Vet. Sci. 2010, 42, 1312–1315. [Google Scholar]
- Zhang, P.; Feng, Q. The recent advances of Fructus Ligustri Lucidi in pharmacology and clinical applications. China Pharm. 2002, 11, 78–80. [Google Scholar]
- Anonymous. A report on the pharmacological effects of ethyl acetate extracts of Fructus Ligustri Lucidi leaves. Zhong Cao Yao Tong Xun 1979, 10, 357–360. [Google Scholar]


| Animal Models | Fractions or Components of FLL | Dosage and Route | Duration of Treatment | Refs. |
|---|---|---|---|---|
| OVX rats | FLL extract | Oral gavage; 550 mg/kg/d | 14 weeks | [58] |
| OVX rat | FLL ethanol extract | Oral gavage; 700 mg/kg/d | 12 weeks | [59] |
| OVX rats | FLL ethanol extract | Oral gavage; 700 mg/kg/d | 12 weeks | [60] |
| Male growing rats | FLL ethanol extract | 0.40, 0.65 and 0.90% FLL extract with AIN-93G | 4 months | [61] |
| OVX rats | FLL water extract | Oral gavage; 3.5 g/kg/d | 12 weeks | [62,63] |
| OVX rats | FLL ethanol extract | Oral gavage; 9, 4.5, and 2.25 g/kg/d | 26 weeks | [64] |
| Female mature rats | FLL ethanol extract (EE), ethyl acetate-soluble fraction of EE (EAF), water fraction of EE (WF) | Oral gavage; 700, 574 and 126 mg/kg/d | 12 weeks | [65] |
| Male type 1 diabetic DBA/2J mice | water fraction of FLL ethanol extract | Oral gavage; 574 mg/kg | 6 weeks | [66] |
| Female growing rats | FLL ethanol extract | 0.40, 0.65 and 0.90% FLL extract in AIN-93G diet | 16 weeks | [67] |
| Female aged rats | FLL ethanol extract | Oral gavage; 700 mg/kg/d | 12 weeks | [68] |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, B.; Wang, L.; Li, L.; Zhu, R.; Liu, H.; Liu, C.; Ma, R.; Jia, Q.; Zhao, D.; Niu, J.; et al. Fructus Ligustri Lucidi in Osteoporosis: A Review of its Pharmacology, Phytochemistry, Pharmacokinetics and Safety. Molecules 2017, 22, 1469. https://doi.org/10.3390/molecules22091469
Chen B, Wang L, Li L, Zhu R, Liu H, Liu C, Ma R, Jia Q, Zhao D, Niu J, et al. Fructus Ligustri Lucidi in Osteoporosis: A Review of its Pharmacology, Phytochemistry, Pharmacokinetics and Safety. Molecules. 2017; 22(9):1469. https://doi.org/10.3390/molecules22091469
Chicago/Turabian StyleChen, Beibei, Lili Wang, Lin Li, Ruyuan Zhu, Haixia Liu, Chenyue Liu, Rufeng Ma, Qiangqiang Jia, Dandan Zhao, Jianzhao Niu, and et al. 2017. "Fructus Ligustri Lucidi in Osteoporosis: A Review of its Pharmacology, Phytochemistry, Pharmacokinetics and Safety" Molecules 22, no. 9: 1469. https://doi.org/10.3390/molecules22091469




