Novel [99mTcN]2+ Labeled EGFR Inhibitors as Potential Radiotracers for Single Photon Emission Computed Tomography (SPECT) Tumor Imaging
Abstract
:1. Introduction
2. Results and Discussion
2.1. Chemistry
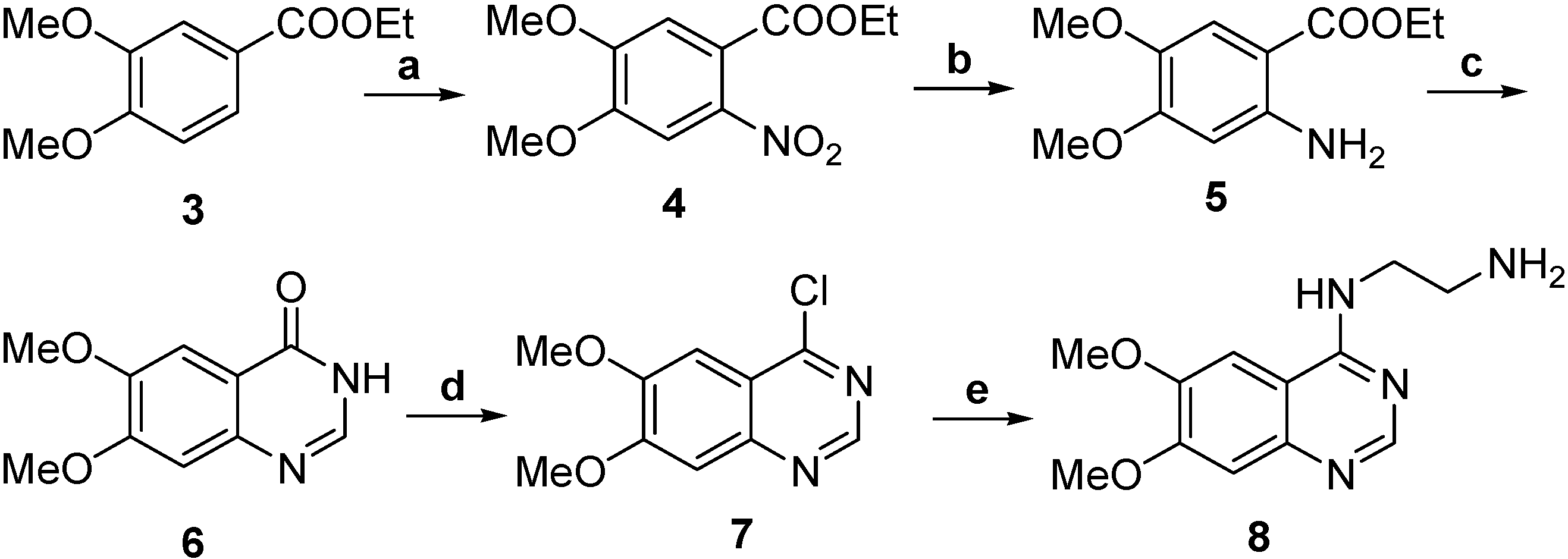
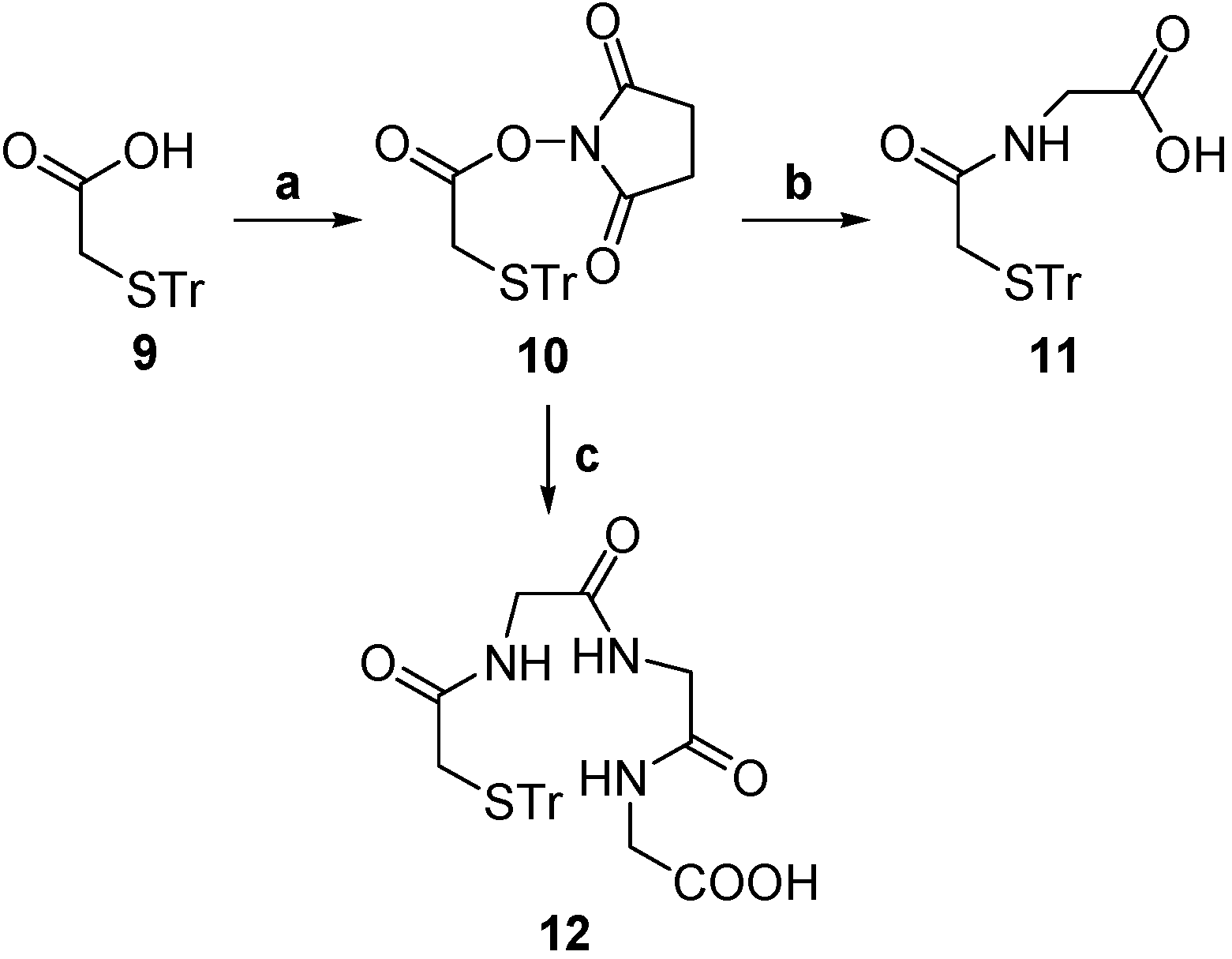
2.2. Radiochemistry
2.2.1. Synthesis of 99mTcN-MAG-ADMQ and 99mTcN-MAG3-ADMQ
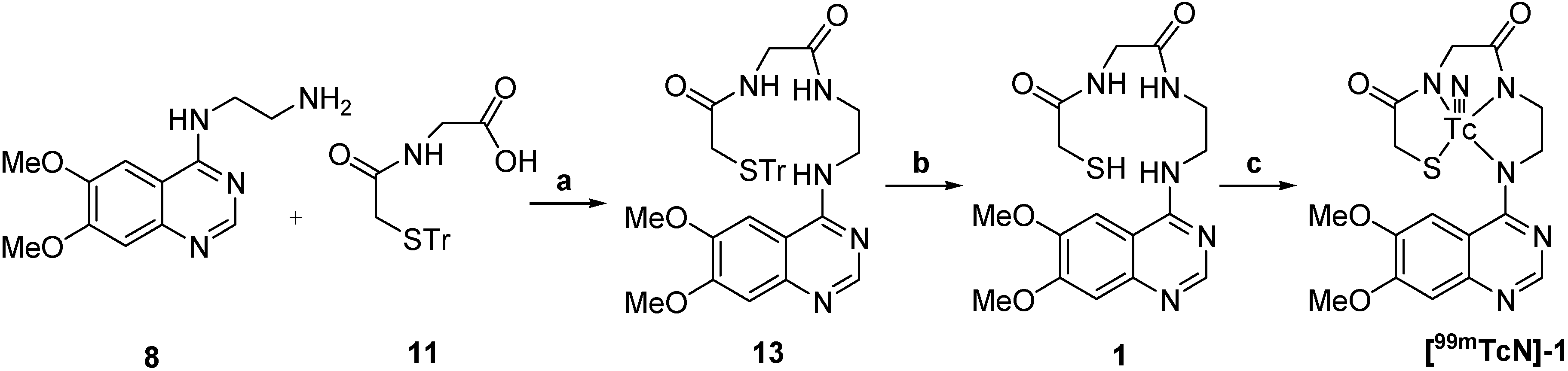

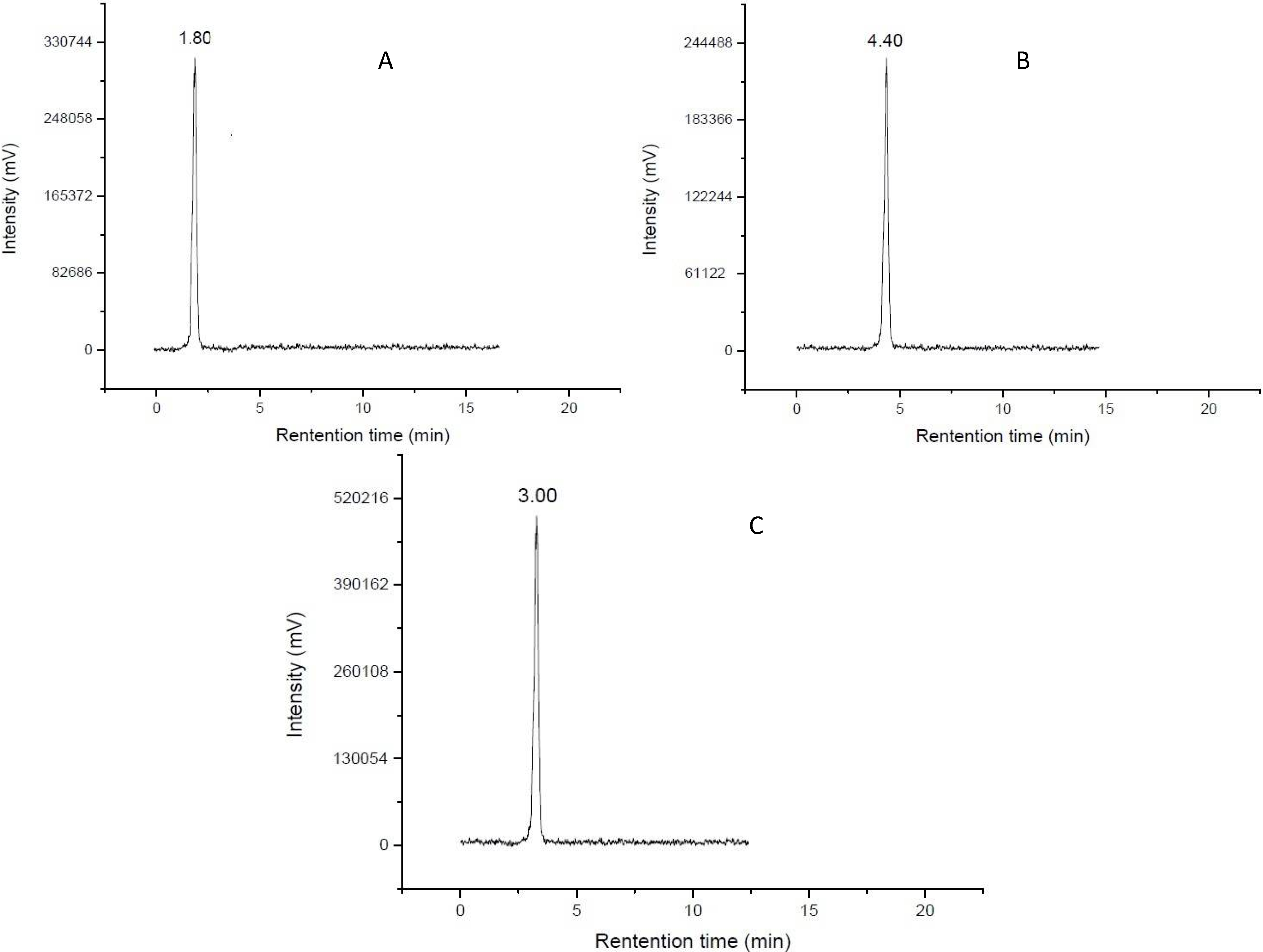
2.2.2. In Vitro Stability
2.2.3. Paper Electrophoresis
2.2.4. Partition coefficients
| [99mTcN]-1 | [99mTcN]-2 | |
|---|---|---|
| log P | −1.81 ± 0.02 | −1.57 ± 0.01 |
2.2.5. Biological Evaluation
| Tissue | 30 min | 60 min | 120 min |
|---|---|---|---|
| Heart | 0.27 ± 0.02 | 0.11 ± 0.01 | 0.05 ± 0.01 |
| Liver | 2.71 ± 0.16 | 1.01 ± 0.08 | 0.55 ± 0.11 |
| Spleen | 0.31 ± 0.03 | 0.15 ± 0.01 | 0.07 ± 0.02 |
| Lung | 1.36 ± 0.13 | 0.94 ± 0.06 | 0.44 ± 0.09 |
| Kidney | 2.42 ± 0.10 | 2.3 ± 0.07 | 1.35 ± 0.11 |
| Muscle | 0.27 ± 0.01 | 0.07 ± 0.01 | 0.06 ± 0.02 |
| Bone | 0.19 ± 0.02 | 0.16 ± 0.04 | 0.04 ± 0.01 |
| Large Intestine | 0.71 ± 0.22 | 0.79 ± 0.12 | 0.51 ± 0.10 |
| Small Intestine | 0.31 ± 0.01 | 0.25 ± 0.03 | 0.18 ± 0.03 |
| Stomach | 0.43 ± 0.05 | 0.04 ± 0.01 | 0.07 ± 0.03 |
| Brain | 0.04 ± 0.01 | 0.03 ± 0.02 | 0.01 ± 0.01 |
| Tumor | 0.35 ± 0.03 | 0.31 ± 0.04 | 0.07 ± 0.01 |
| Blood | 1.09 ± 0.11 | 0.82 ± 0.03 | 0.11 ± 0.04 |
| T/M ratio | 1.29 ± 0.14 | 1.82 ± 0.33 | 1.17 ± 0.13 |
| T/B ratio | 1.84 ± 0.07 | 1.94 ± 0.24 | 1.75 ± 0.16 |
| Tissue | 30 min | 60 min | 120 min |
|---|---|---|---|
| Heart | 0.40 ± 0.05 | 0.12 ± 0.03 | 0.08 ± 0.01 |
| Liver | 0.78 ± 0.09 | 0.79 ± 0.04 | 0.39 ± 0.05 |
| Spleen | 0.16 ± 0.01 | 0.08 ± 0.02 | 0.05 ± 0.01 |
| Lung | 0.50 ± 0.11 | 0.30 ± 0.08 | 0.14 ± 0.04 |
| Kidney | 1.64 ± 0.15 | 1.97 ± 0.21 | 1.65 ± 0.16 |
| Muscle | 0.25 ± 0.06 | 0.19 ± 0.02 | 0.05 ± 0.02 |
| Bone | 0.55 ± 0.15 | 0.21 ± 0.06 | 0.20 ± 0.01 |
| Large Intestine | 0.39 ± 0.17 | 0.51 ± 0.04 | 1.22 ± 0.24 |
| Small Intestine | 0.99 ± 0.14 | 0.56 ± 0.09 | 0.20 ± 0.05 |
| Stomach | 0.15 ± 0.03 | 0.14 ± 0.07 | 0.04 ± 0.02 |
| Brain | 0.02 ± 0.01 | 0.01 ± 0.01 | 0.01 ± 0.005 |
| Tumor | 0.21 ± 0.07 | 0.40 ± 0.05 | 0.21 ± 0.08 |
| Blood | 0.96 ± 0.23 | 0.87 ± 0.16 | 0.13 ± 0.06 |
| T/M ratio | 0.84 ± 0.09 | 2.11 ± 0.18 | 4.20 ± 0.25 |
| T/B ratio | 0.38 ± 0.05 | 1.90 ± 0.16 | 1.10 ± 0.08 |
3. Experimental
3.1. General Information
3.2. Synthesis
Synthesis of 99mTcN-MAG-ADMQ ([99mTcN]-1)
Synthesis of 99mTcN-MAG3- ADMQ ([99mTcN]-2)
3.3. In Vitro Stability Study
3.4. Radio-HPLC Analysis
3.5. Paper Electrophoresis
3.6. Measurement of Partition Coefficients
3.7. Biodistribution Study
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Hunter, T. Growth factors: The epidermal growth factor receptor gene and its product. Nature 1984, 311, 414–416. [Google Scholar] [CrossRef]
- Yarden, Y.; Schlessinger, J. Self-phosphorylation of epidermal growth factor receptor: Evidence for a model of intermolecular allosteric activation. Biochemistry 1987, 26, 1434–1442. [Google Scholar] [CrossRef]
- Iwashita, S.; Kobayashi, M. Signal transduction system for growth factor receptors associated with tyrosine kinase activity: Epidermal growth factor receptor signalling and its regulation. Cell Signal. 1992, 4, 123–132. [Google Scholar] [CrossRef]
- Voldborg, B.R.; Damstrup, L.; Spang-Thomsen, M.; Poulsen, H.S. Epidermal growth factor receptor (EGFR) and EGFR mutations, function and possible role in clinical trials. Ann. Oncol. 1997, 8, 1197–1206. [Google Scholar] [CrossRef]
- Olayioye, M.A.; Neve, R.M.; Lane, H.A.; Hynes, N.E. The ErbB signaling network: Receptor heterodimerization in development and cancer. EMBO J. 2000, 19, 3159–3167. [Google Scholar] [CrossRef]
- Prenzel, N.; Fischer, O.; Streit, S.; Hart, S.; Ullrich, A. The epidermal growth factor receptor family as a central element for cellular signal transduction and diversification. Endocr-Related Cancer 2001, 8, 11–31. [Google Scholar] [CrossRef]
- Yarden, Y.; Sliwkowski, M.X. Untangling the ErbB signalling network. Nat. Rev. Mol. Cell Biol. 2001, 2, 127–137. [Google Scholar] [CrossRef]
- Levitzki, A. EGF receptor as a therapeutic target. Lung Cancer 2003, 41, 9–14. [Google Scholar] [CrossRef]
- Dissoki, S.; Eshet, R.; Billauer, H.; Mishani, E. Modified PEG-anilinoquinazoline derivatives as potential EGFR PET agents. J. Label. Compound. Radiopharm. 2009, 52, 41–52. [Google Scholar] [CrossRef]
- Mamot, C.; Drummond, D.C.; Greiser, U.; Hong, K.; Kirpotin, D.B.; Marks, J.D.; Park, J.W. Epidermal growth factor receptor (EGFR)-targeted immunoliposomes mediate specific and efficient drug delivery to EGFR-and EGFRvIII-overexpressing tumor cells. Cancer Res. 2003, 63, 3154–3161. [Google Scholar]
- Shir, A.; Ogris, M.; Wagner, E.; Levitzki, A. EGF receptor-targeted synthetic double-stranded RNA eliminates glioblastoma, breast cancer, and adenocarcinoma tumors in mice. PLoS Med. 2005, 3, e6. [Google Scholar] [CrossRef]
- Levitzki, A.; Mishani, E. Tyrphostins and other tyrosine kinase inhibitors. Annu. Rev. Biochem. 2006, 75, 93–109. [Google Scholar] [CrossRef]
- Paez, J.G.; Jänne, P.A.; Lee, J.C.; Tracy, S.; Greulich, H.; Gabriel, S.; Herman, P.; Kaye, F.J.; Lindeman, N.; Boggon, T.J. EGFR mutations in lung cancer: Correlation with clinical response to gefitinib therapy. Science 2004, 304, 1497–1500. [Google Scholar]
- Lynch, T.J.; Bell, D.W.; Sordella, R.; Gurubhagavatula, S.; Okimoto, R.A.; Brannigan, B.W.; Harris, P.L.; Haserlat, S.M.; Supko, J.G.; Haluska, F.G. Activating mutations in the epidermal growth factor receptor underlying responsiveness of non–small-cell lung cancer to gefitinib. N. Engl. J. Med. 2004, 350, 2129–2139. [Google Scholar] [CrossRef]
- Tsao, M.-S.; Sakurada, A.; Cutz, J.-C.; Zhu, C.-Q.; Kamel-Reid, S.; Squire, J.; Lorimer, I.; Zhang, T.; Liu, N.; Daneshmand, M. Erlotinib in lung cancer—molecular and clinical predictors of outcome. N. Engl. J. Med. 2005, 353, 133–144. [Google Scholar] [CrossRef]
- Pao, W.; Miller, V.; Zakowski, M.; Doherty, J.; Politi, K.; Sarkaria, I.; Singh, B.; Heelan, R.; Rusch, V.; Fulton, L. EGF receptor gene mutations are common in lung cancers from “never smokers” and are associated with sensitivity of tumors to gefitinib and erlotinib. Proc. Natl. Acad. Sci. USA 2004, 101, 13306–13311. [Google Scholar] [CrossRef]
- Riely, G.J.; Politi, K.A.; Miller, V.A.; Pao, W. Update on epidermal growth factor receptor mutations in non–small cell lung cancer. Clin. Cancer Res. 2006, 12, 7232–7241. [Google Scholar] [CrossRef]
- Hoy, S.M.; Wagstaff, A.J. Panitumumab. Drugs 2006, 66, 2005–2014. [Google Scholar] [CrossRef]
- Berlin, J.; Posey, J.; Tchekmedyian, S.; Hu, E.; Chan, D.; Malik, I.; Yang, L.; Amado, R.G.; Hecht, J.R. Panitumumab with irinotecan/leucovorin/5-fluorouracil for first-line treatment of metastatic colorectal cancer. Clin. Colorectal Cancer 2007, 6, 427–432. [Google Scholar] [CrossRef]
- Cohenuram, M.; Saif, M.W. Panitumumab the first fully human monoclonal antibody: From the bench to the clinic. Anti-Cancer Drug. 2007, 18, 7–15. [Google Scholar] [CrossRef]
- Kwak, E.L.; Sordella, R.; Bell, D.W.; Godin-Heymann, N.; Okimoto, R.A.; Brannigan, B.W.; Harris, P.L.; Driscoll, D.R.; Fidias, P.; Lynch, T.J. Irreversible inhibitors of the EGF receptor may circumvent acquired resistance to gefitinib. Proc. Natl. Acad. Sci. USA 2005, 102, 7665–7670. [Google Scholar] [CrossRef]
- Mishani, E.; Abourbeh, G.; Rozen, Y.; Jacobson, O.; Laky, D.; Ben David, I.; Levitzki, A.; Shaul, M. Novel carbon-11 labeled 4-dimethylamino-but-2-enoic acid [4-(phenylamino)-quinazoline-6-yl]- amides: Potential PET bioprobes for molecular imaging of EGFR-positive tumors. Nucl. Med. Biol. 2004, 31, 469–476. [Google Scholar] [CrossRef]
- Shaul, M.; Abourbeh, G.; Jacobson, O.; Rozen, Y.; Laky, D.; Levitzki, A.; Mishani, E. Novel iodine-124 labeled EGFR inhibitors as potential PET agents for molecular imaging in cancer. Bioorgan. Med. Chem. 2004, 12, 3421–3429. [Google Scholar] [CrossRef]
- Bonasera, T.A.; Ortu, G.; Rozen, Y.; Krais, R.; Freedman, N.M.T.; Chisin, R.; Gazit, A.; Levitzki, A.; Mishani, E. Potential 18F-labeled biomarkers for epidermal growth factor receptor tyrosine kinase. Nucl. Med. Biol. 2001, 28, 359–374. [Google Scholar] [CrossRef]
- Neto, C.; Fernandes, C.; Oliveira, M.C.; Gano, L.; Mendes, F.; Kniess, T.; Santos, I. Radiohalogenated 4-anilinoquinazoline-based EGFR-TK inhibitors as potential cancer imaging agents. Nucl. Med. Biol. 2012, 39, 247–260. [Google Scholar] [CrossRef]
- Mang’era, K.O.; Vanbilloen, H.P.; Bellande, E.; Pasqualini, R.; Verbruggen, A.M. Influence of a 99mTcN core on the biological and physicochemical behavior of 99mTc complexes of L, L-EC and L, L-ECD. Nucl. Med. Biol. 1996, 23, 987–993. [Google Scholar] [CrossRef]
- Grummon, G.; Rajagopalan, R.; Palenik, G.J.; Koziol, A.E.; Nosco, D.L. Synthesis, characterization and crystal structures of technetium (V)-Oxo complexes useful in nuclear medicine. 1. Complexes of mercaptoacetylglycylglycylglycine (MAG3) and its methyl ester derivative (MAG3OMe). Inorg. Chem. 1995, 34, 1764–1772. [Google Scholar] [CrossRef]
- Hansen, L.; Cini, R.; Taylor, A., Jr.; Marzilli, L.G. Rhenium (V) oxo complexes relevant to technetium renal imaging agents derived from mercaptoacetylglycylglycylaminobenzoic acid isomers. Structural and molecular mechanics studies. Inorg. Chem. 1992, 31, 2801–2808. [Google Scholar] [CrossRef]
- Purcell, W.P.; Bass, G.E.; Clayton, J.M. Strategy of Drug Design: A Guide to Biological Activity; Wiley: New York, NY, USA, 1973. [Google Scholar]
- Pandey, A.; Volkots, D.L.; Seroogy, J.M.; Rose, J.W.; Yu, J.-C.; Lambing, J.L.; Hutchaleelaha, A.; Hollenbach, S.J.; Abe, K.; Giese, N.A. Identification of orally active, potent, and selective 4-piperazinylquinazolines as antagonists of the platelet-derived growth factor receptor tyrosine kinase family. J. Med. Chem. 2002, 45, 3772–3793. [Google Scholar] [CrossRef]
- Kanter, J.; Pandey, A.; Robinson, J.; Scarborough, R.M. Preparation of substituted piperazinoquinazolines as kinase inhibitors. PCT Int. Appl. WO 2002036587, 2002. [Google Scholar]
- Ding, R.; He, Y.; Xu, J.L.; Liu, H.; Wang, X.; Feng, M.; Qi, C.M.; Zhang, J.B. Synthesis and biological evaluation of pyrazolo[1,5-a]-pyrimidine-containing 99mTc nitrido radiopharmaceuticals as imaging agents for tumors. Molecules 2010, 15, 8723–8733. [Google Scholar] [CrossRef]
- Sample Availability: Not available.
© 2014 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Zhao, M.; Ning, H.; Feng, M.; Li, S.; Chang, J.; Qi, C. Novel [99mTcN]2+ Labeled EGFR Inhibitors as Potential Radiotracers for Single Photon Emission Computed Tomography (SPECT) Tumor Imaging. Molecules 2014, 19, 5508-5521. https://doi.org/10.3390/molecules19055508
Zhao M, Ning H, Feng M, Li S, Chang J, Qi C. Novel [99mTcN]2+ Labeled EGFR Inhibitors as Potential Radiotracers for Single Photon Emission Computed Tomography (SPECT) Tumor Imaging. Molecules. 2014; 19(5):5508-5521. https://doi.org/10.3390/molecules19055508
Chicago/Turabian StyleZhao, Mingxia, Hongyu Ning, Man Feng, Shilei Li, Jin Chang, and Chuanmin Qi. 2014. "Novel [99mTcN]2+ Labeled EGFR Inhibitors as Potential Radiotracers for Single Photon Emission Computed Tomography (SPECT) Tumor Imaging" Molecules 19, no. 5: 5508-5521. https://doi.org/10.3390/molecules19055508
APA StyleZhao, M., Ning, H., Feng, M., Li, S., Chang, J., & Qi, C. (2014). Novel [99mTcN]2+ Labeled EGFR Inhibitors as Potential Radiotracers for Single Photon Emission Computed Tomography (SPECT) Tumor Imaging. Molecules, 19(5), 5508-5521. https://doi.org/10.3390/molecules19055508




