Implementing Integrative Nursing in a Pediatric Setting
Abstract
:1. Introduction
2. Methods
2.1. Integrative Nursing as a Framework for Practice
2.2. Program Design and Components
- Stakeholder dialogue—Interviews were conducted with clinical and administrative leadership as well as with frontline clinical staff.
- Shadowing practice—Current state of nursing and supportive care staff practice was observed to identify areas of opportunity.
- Prototyping—Experiential and educational sessions were conducted to engage staff and enhance their understanding of integrative modalities.
- Benchmarking—Other pediatric integrative therapy programs were examined through site visits, phone interviews, and extensive internet searches. These were reviewed for best practices.
- Staff survey—Nursing staff (N = 32) on the unit were surveyed to assess the knowledge, perceptions and comfort level with integrative modalities and care delivery.
2.2.1. Challenges
- Skepticism from staff—Due to historic start/stop efforts and initiatives that lacked structure, momentum and institutional support, staff doubted the likelihood of ever forming a sustainable, consistent and reliable integrative therapy program. There was distrust of the system and fatigue from working around system failures.
- Perceived barriers—Ranked by nursing staff in descending order: time, lack of skills, lack of knowledge, and comfort with integrative modalities.
- Inconsistencies in infrastructure—Processes, policies, procedure and methods of providing staff education had many variations across the board between the clinic and the hospital settings. These inconsistencies made it challenging to assess what existed, let alone what could be built.
- Lack of clinical expertise—The system did not employ any clinician with the level of training necessary to ensure that safe and effective integrative therapies were being utilized to the fullest potential to meet the needs of patients and families.
2.2.2. Vision
2.2.3. Goals
- Improve symptom management.
- Improve patient experience.
- Enhance patient and family resilience and capacity to cope.
- Provide patient and family with tools for incorporating integrative health practices before, during and after hospitalization.
- Improve care team well-being.
- Grow and support integrative health and healing research.
- Embed integrative approaches in every patient’s care plan and every clinician’s workflow.
2.2.4. Recommendations
- Create an infrastructure and commit resources that are commensurate with the program vision and goals.
- ◦
- Hire or appoint an organizational lead.
- ◦
- Establish standards of care as well as policies and procedures that support those standards.
- ◦
- Create flowsheets and templates in the electronic medical record that not only allow for documentation of integrative approaches to care, but also allow for easy assessment of outcomes.
- Design a robust and comprehensive program evaluation strategy.
- Establish strong staff education and support.
- Offer access to a consistent set of therapeutic approaches that are evidenced-informed and focused on improved symptom management and quality of life.
- Expand patient and family education.
- Develop parent support resources to engage them in self-care and stress management, and to empower them to participate in comforting and caring for their child through the use of integrative approaches.
- Create an integrative health consult service for expertise, leadership and guidance to staff, patients and families.
- Establish an integrative health and healing research program focused on pediatric BMT patients’ needs and clinical outcomes.
2.2.5. Care Delivery Model
2.3. Program Evaluation
2.4. Emerging Research Agenda
3. Results and Discussion
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Institute for Healthcare Improvement: IHI Home Page. Available online: http://www.ihi.org:80/ (accessed on 29 June 2018).
- Clinician Resilience and Well-Being. National Academy of Medicine. Available online: https://nam.edu/initiatives/clinician-resilience-and-well-being/ (accessed on 29 June 2018).
- Kreitzer, M.J.; Koithan, M. Integrative Nursing; Oxford University Press: New York, NY, USA, 2018. [Google Scholar]
- Koithan, M.S.; Kreitzer, M.J.; Watson, J. Linking the unitary paradigm to policy through a synthesis of caring science and integrative nursing, linking the unitary paradigm to policy through a synthesis of caring science and integrative nursing. Nurs. Sci. Q. 2017, 30, 262–268. [Google Scholar] [CrossRef] [PubMed]
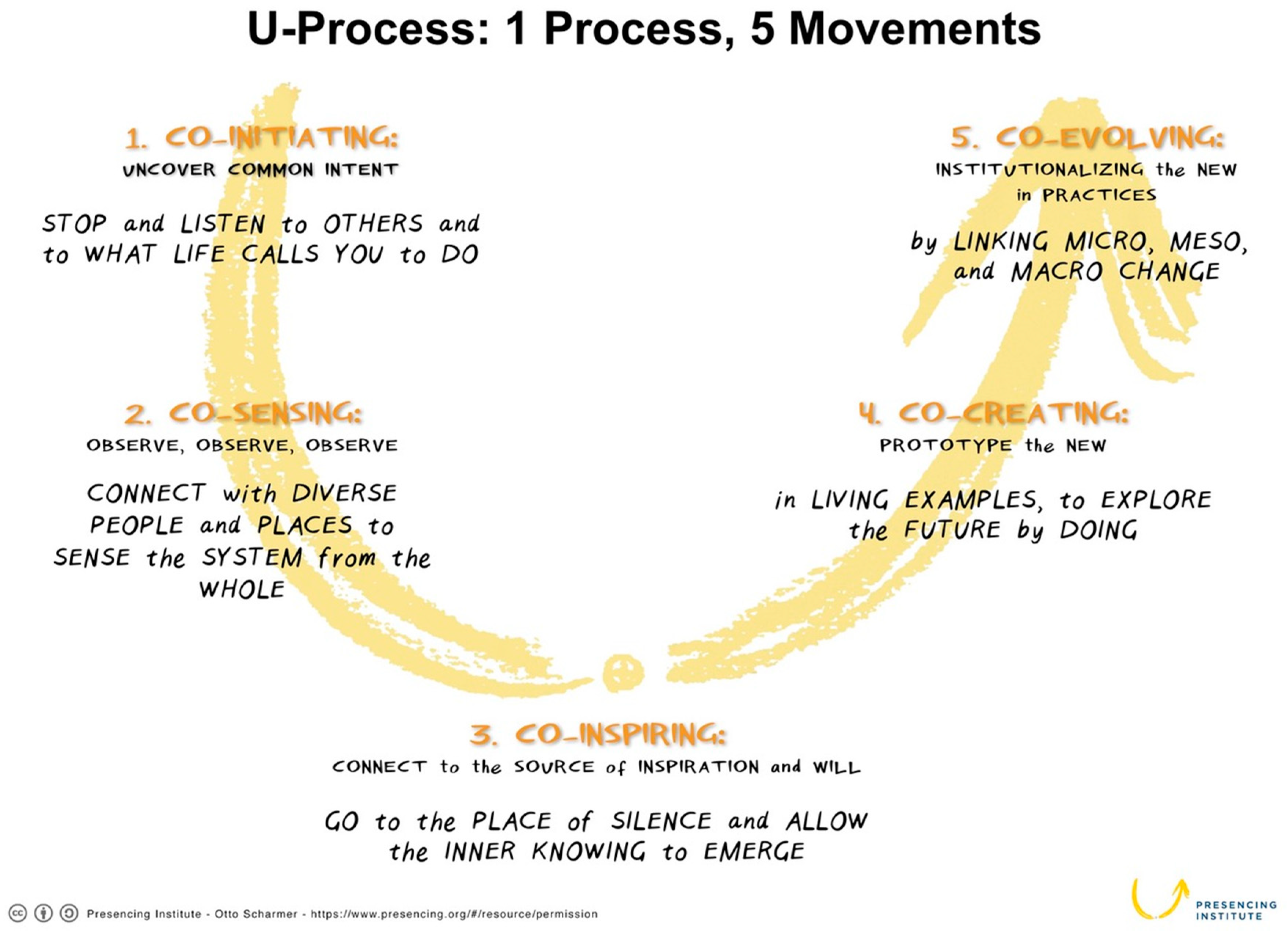
- Presencing Institute—Theory U: Leading from the Future as It Emerges. Available online: https://www.presencing.org/#/aboutus/theory-u (accessed on 29 June 2018).
- Integrative Nursing. Available online: https://www.csh.umn.edu/education/focus-areas/integrative-nursing (accessed on 6 July 2018).
- Jacobs, S.S. Integrative therapy use for management of side effects and toxicities experienced by pediatric oncology patients. Children 2014, 1, 424–440. [Google Scholar] [CrossRef] [PubMed]
- Roscoe, J.A.; Morrow, G.R.; Aapro, M.S.; Molassiotis, A.; Olver, I. Anticipatory nausea and vomiting. Support. Care Cancer 2011, 19, 1533–1538. [Google Scholar] [CrossRef] [PubMed]
- Yates, G.J.; Beckmann, N.B.; Anderson, M.R.; Voss, M.E.; Silverman, M.J. Caregiver perceptions of music therapy for children hospitalized for a blood and marrow transplant: An interpretivist investigation. Glob. Adv. Health Med. 2018. [Google Scholar] [CrossRef] [PubMed]

| Human beings are whole systems inseparable from their environments. |
| Human beings have the innate capacity for health and well-being. |
| Nature has healing and restorative properties that contribute to health and well-being. |
| Integrative nursing is person-centered and relationship-based. |
| Integrative nursing practice is informed by evidence and uses the full range of therapeutic modalities to support/augment the healing process, moving from least intensive/invasive to more, depending on need and context. |
| Integrative nursing focuses on the health and well-being of caregivers as well as those they serve. |
| Study Concept | Description |
|---|---|
| Music therapy as a method to physical rehabilitation | Qualitative data has revealed that even when children are too physically ill or mentally reluctant to participate in physical rehabilitation therapies, many are still motivated to get out of bed and participate in music therapy. It is hypothesized that active participation in music therapy can help achieve physical rehabilitation goals in some patients [9]. |
| Retrospective review of utilization and safety | Data mining will be done to assess the most common therapy used by each age group, adverse reactions in patients with safety considerations such as thrombocytopenia or impaired skin integrity, responses of pain, nausea and anxiety to integrative therapy, and average length and number of visits (inpatient and outpatient) each patient requests. |
| Self-assessment of change after the implementation of an integrative iherapy ilan of care | The self-assessment of change is a retrospective pre/post assessment that measures a variety of psychosocial indicators. The tool was designed specifically to capture change produced by integrative therapy. |
| Survivorship well-being for patients and families | Interactive online content based on the University of Minnesota’s Wellbeing Model (Figure 2) will be developed and focused on teenagers and young adults. Virtual support groups will accompany content. Groups will be facilitated by a variety of healthcare professionals with an integrative lens. Data will be collected to assess the impact on overall well-being including indicators such as self-management, perceived stress, quality of life, anxiety, depression and resilience. |
| Microbiome | This study will examine the effects of chemotherapy and prolonged prophylactic antibiotic use on patients after engraftment and full recovery from pancytopenia. It will also look at the potential for the safe and judicial use of supplements to restore intestinal tissue integrity and the microbiome. |
| Staff self-care | Continuous data collection efforts have been and will continue to be underway assessing staff burnout and other components of well-being. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Voss, M.E.; Kreitzer, M.J. Implementing Integrative Nursing in a Pediatric Setting. Children 2018, 5, 103. https://doi.org/10.3390/children5080103
Voss ME, Kreitzer MJ. Implementing Integrative Nursing in a Pediatric Setting. Children. 2018; 5(8):103. https://doi.org/10.3390/children5080103
Chicago/Turabian StyleVoss, Megan E., and Mary Jo Kreitzer. 2018. "Implementing Integrative Nursing in a Pediatric Setting" Children 5, no. 8: 103. https://doi.org/10.3390/children5080103




