Minimally Disruptive Medicine: A Pragmatically Comprehensive Model for Delivering Care to Patients with Multiple Chronic Conditions
Abstract
:1. Introduction
2. Minimally Disruptive Medicine: The Rationale
3. Strategy 1: Identify the Right Care
3.1. Acknowledge the Work
3.2. Acknowledge the Capacity
3.3. Acknowledge the Complexity
3.4. Integrate the Inputs
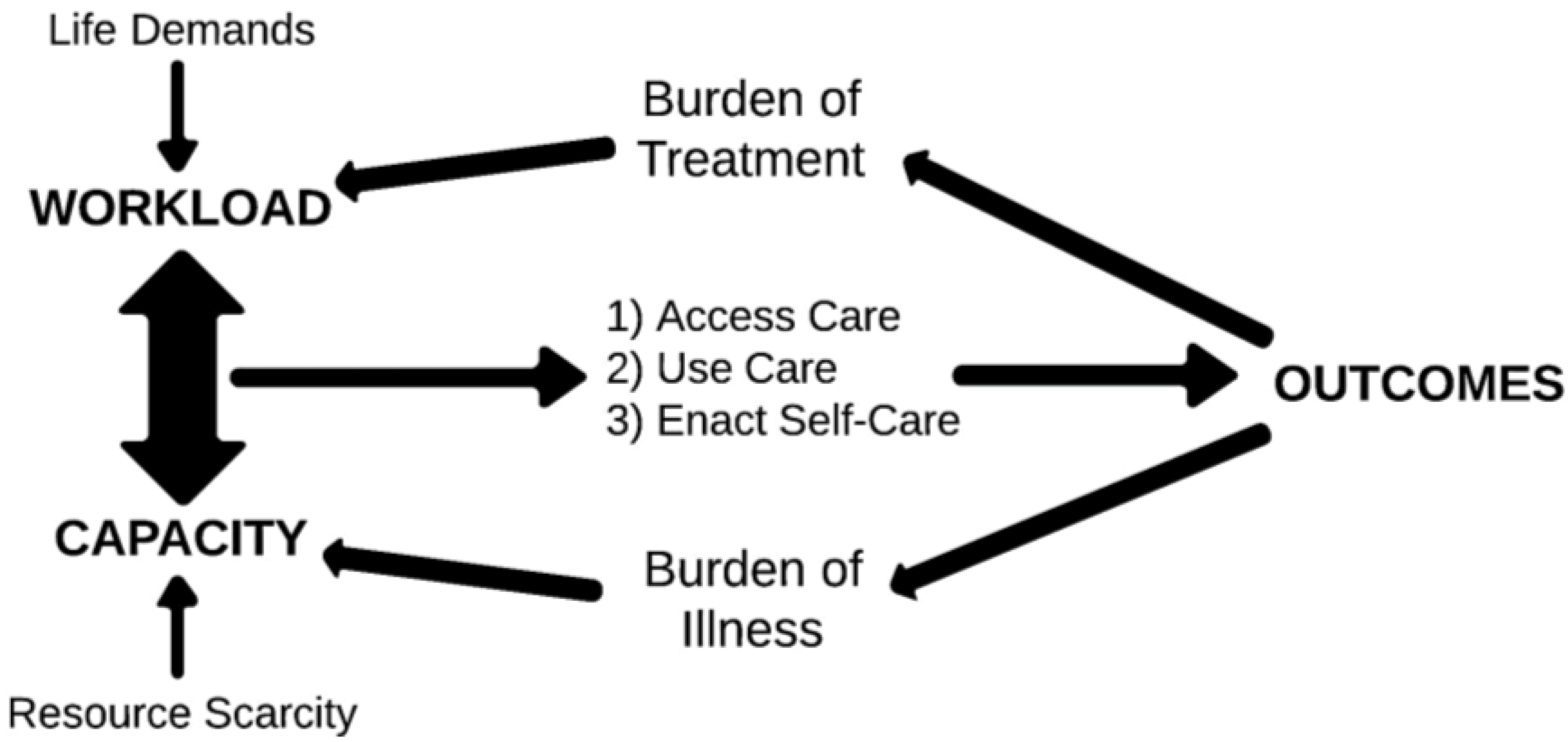
4. Strategy 2: Make the Right Care Happen
4.1. Prioritize Feasibility
4.2. Make Sense of It All
4.3. Use Available Resources
4.4. Monitor and Respond
5. Minimally Disruptive Medicine: Comprehensive Tools for Implementation
6. Conclusions
6.1. The MDM Difference
| Tool | Description |
|---|---|
| Tools to Identify the Right Care | |
| Goal-elicitation | An attempt to identify transcendent patient goals for life that can be entered into the medical record and used to orient care |
| Patient partnerships | A structured commitment among patients and clinicians to work together to identify the right care and to make the right care happen |
| Shared decision making | Used to incorporate patient values and preferences into management decisions, legitimize partnership, and arrive at feasible care strategies |
| Capacity assessments | Structured, within-encounter screens used to identify contextual limitations in patient capacity that impact care effectiveness and that may be amenable to support or intervention |
| Workload assessments | Structured, within-encounter screens used to identify the intrusiveness of health on life and to find opportunities for treatment plan augmentation |
| Capacity coaching | Between-clinician encounter interactions that screen for progress in goals and the influence of capacity and workload on health and wellness |
| Patient-reported outcome tracking | Systematic, ongoing recording of patient-reported health status, burdens of life and health, and changes in the quality or availability of support |
| Tools to Make the Right Care Happen | |
| Resource registries | Lists of resources within and outside of the health system that have explicit and predefined agreements to provide specific support to specific patients |
| Lean consumption | Healthcare provider-initiated efforts to improve the efficiency of interacting with health care from the patient’s perspective (e.g., by shortening waiting times, streamlining administrative hurdles) |
| Medication therapy management | A version of medication therapy management that focuses on optimization of medication regimens in regards to not only patient need, but also want and fit; best implemented with the power to “deprescribe” low-value and burdensome medications |
| Community navigators | Individuals that can be used to more intimately connect patients to community resources |
| Relational coordination | Method of organizing care based on shared aims and understanding that uses specific analytics to identify within-team relationships that are impeding care effectiveness |
| Wisdom leadership | Training for team and system leaders to enhance their capacity to lead with wisdom and to remove barriers impeding care effectiveness—often through the use of reflective team huddles |
| Choosing Wisely Campaign | Used to promote a practice or system-level culture of parsimonious and patient-centered care and to establish social norms that counteract the bias toward intervention |
6.2. Opportunities for Further Study
Acknowledgments
Author Contributions
Conflicts of Interest
Disclaimer
References
- Porter, M.E. What is value in health care? N. Engl. J. Med. 2010, 363, 2477–2481. [Google Scholar] [CrossRef] [PubMed]
- Anderson, G.F. Chronic Care: Making the Case for Ongoing Care; Robert Wood Johnson Foundation: Princeton, NJ, USA, 2010. [Google Scholar]
- Parekh, A.K.; Kronick, R.; Tavenner, M. Optimizing health for persons with multiple chronic conditions. JAMA 2014, 312, 1199–1200. [Google Scholar] [CrossRef] [PubMed]
- May, C.; Montori, V.M.; Mair, F.S. We need minimally disruptive medicine. BMJ 2009, 339, b2803. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine Committee on Quality of Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century; National Academies Press: Washington, DC, USA, 2001. [Google Scholar]
- Sav, A.; Kendall, E.; McMillan, S.S.; Kelly, F.; Whitty, J.A.; King, M.A.; Wheeler, A.J. ‘You say treatment, I say hard work’: Treatment burden among people with chronic illness and their carers in Australia. Health Soc. Care Commun. 2013, 21, 665–674. [Google Scholar]
- Bohlen, K.; Scoville, E.; Shippee, N.D.; May, C.R.; Montori, V.M. Overwhelmed patients: A videographic analysis of how patients with type 2 diabetes and clinicians articulate and address treatment burden during clinical encounters. Diabetes Care 2012, 35, 47–49. [Google Scholar] [CrossRef] [PubMed]
- Jowsey, T.; Yen, L.; Mathews W, P. Time spent on health related activities associated with chronic illness: A scoping literature review. BMC Public Health 2012, 12, 1044. [Google Scholar] [CrossRef] [PubMed]
- Gallacher, K.; May, C.R.; Montori, V.M.; Mair, F.S. Understanding patients’ experiences of treatment burden in chronic heart failure using normalization process theory. Ann. Fam. Med. 2011, 9, 235–243. [Google Scholar] [CrossRef] [PubMed]
- May, C.R.; Mair, F.; Finch, T.; MacFarlane, A.; Dowrick, C.; Treweek, S.; Rapley, T.; Ballini, L.; Ong, B.N.; Rogers, A.; et al. Development of a theory of implementation and integration: Normalization process theory. Implement. Sci. 2009, 4, 29. [Google Scholar] [CrossRef] [PubMed]
- May, C.R.; Eton, D.T.; Boehmer, K.; Gallacher, K.; Hunt, K.; MacDonald, S.; Mair, F.S.; May, C.M.; Montori, V.M.; Richardson, A.; et al. Rethinking the patient: Using burden of treatment theory to understand the changing dynamics of illness. BMC Health Serv. Res. 2014, 14, 281. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, R.S.; Folkman, S. Transactional theory and research on emotions and coping. Eur. J. Pers. 1987, 1, 141–169. [Google Scholar] [CrossRef]
- Barnett, K.; Mercer, S.W.; Norbury, M.; Watt, G.; Wyke, S.; Guthrie, B. Epidemiology of multimorbidity and implications for health care, research, and medical education: A cross-sectional study. Lancet 2012, 380, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Durso, S.C. Using clinical guidelines designed for older adults with diabetes mellitus and complex health status. JAMA 2006, 295, 1935–1940. [Google Scholar] [CrossRef] [PubMed]
- Wyatt, K.D.; Stuart, L.M.; Brito, J.P.; Carranza Leon, B.; Domecq, J.P.; Prutsky, G.J.; Egginton, J.S.; Calvin, A.D.; Shah, N.D.; Murad, M.H.; et al. Out of context: Clinical practice guidelines and patients with multiple chronic conditions: A systematic review. Med. Care 2013, 52, S92–S100. [Google Scholar] [CrossRef]
- Payne, R.A.; Abel, G.A.; Guthrie, B.; Mercer, S.W. The effect of physical multimorbidity, mental health conditions and socioeconomic deprivation on unplanned admissions to hospital: A retrospective cohort study. CMAJ 2013, 185, E221–E228. [Google Scholar] [CrossRef] [PubMed]
- Weiner, S.J.; Schwartz, A.; Sharma, G.; Binns-Calvey, A.; Ashley, N.; Kelly, B.; Dayal, A.; Patel, S.; Weaver, F.M.; Harris, I. Patient-centered decision making and health care outcomes: An observational study. Ann. Intern. Med. 2013, 158, 573–579. [Google Scholar] [CrossRef] [PubMed]
- Litaker, D.; Tomolo, A.; Liberatore, V.; Stange, K.C.; Aron, D. Using complexity theory to build interventions that improve health care delivery in primary care. J. Gen. Intern. Med. 2006, 21, S30–S34. [Google Scholar] [CrossRef] [PubMed]
- Kernick, D. Complexity and Healthcare Organization: A View From the Street; Radcliffe Publishing: London, UK, 2004. [Google Scholar]
- Phelan, S.E. What is complexity science, really? Emergence J. Complexity Issues Organ. Manag. 2001, 3, 120–136. [Google Scholar]
- Manson, S.M. Simplifying complexity: A review of complexity theory. Geoforum 2001, 32, 405–414. [Google Scholar] [CrossRef]
- Sturmberg, J.P. Multimorbidity and chronic disease: An emergent perspective. J. Eval. Clin. Pract. 2014, 20, 508–512. [Google Scholar] [CrossRef] [PubMed]
- Shippee, N.D.; Shah, N.D.; May, C.R.; Mair, F.S.; Montori, V.M. Cumulative complexity: A functional, patient-centered model of patient complexity can improve research and practice. J. Clin. Epidemiol. 2012, 65, 1041–1051. [Google Scholar] [CrossRef] [PubMed]
- Leppin, A.L.; Gionfriddo, M.R.; Kessler, M.; Brito, J.P.; Mair, F.S.; Gallacher, K.; Wang, Z.; Erwin, P.J.; Sylvester, T.; Boehmer, K.; et al. Preventing 30-day hospital readmissions: A systematic review and meta-analysis of randomized trials. JAMA Intern. Med. 2014, 174, 1095–1107. [Google Scholar] [CrossRef] [PubMed]
- Siegel, D.J. Toward an interpersonal neurobiology of the developing mind: Attachment relationships, “mindsight”, and neural integration. Infant Ment. Health J. 2001, 22, 67–94. [Google Scholar] [CrossRef]
- Stange, K.C. The generalist approach. Ann. Fam. Med. 2009, 7, 198–203. [Google Scholar] [CrossRef] [PubMed]
- Tinetti, M.E.; Fried, T. The end of the disease era. Am. J. Med. 2004, 116, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Ayanian, J.Z.; Berwick, D.M. Do physicians have a bias toward action? A classic study revisited. Med. Decis. Mak. 1991, 11, 154–158. [Google Scholar] [CrossRef]
- Foy, A.J.; Filippone, E.J. The case for intervention bias in the practice of medicine. Yale J. Biol. Med. 2013, 86, 271–280. [Google Scholar] [PubMed]
- Weiner, S.J.; Schwartz, A.; Weaver, F.; Goldberg, J.; Yudkowsky, R.; Sharma, G.; Binns-Calvey, A.; Preyss, B.; Schapira, M.M.; Persell, S.D.; et al. Contextual errors and failures in individualizing patient care: A multicenter study. Ann. Intern. Med. 2010, 153, 69–75. [Google Scholar] [CrossRef] [PubMed]
- Horne, R.; Weinman, J. Patients’ beliefs about prescribed medicines and their role in adherence to treatment in chronic physical illness. J. Psychosom. Res. 1999, 47, 555–567. [Google Scholar] [CrossRef] [PubMed]
- Crabtree, B.F.; Nutting, P.A.; Miller, W.L.; Stange, K.C.; Stewart, E.E.; Jaén, C.R. Summary of the national demonstration project and recommendations for the patient-centered medical home. Ann. Fam. Med. 2010, 8, S80–S90. [Google Scholar] [CrossRef] [PubMed]
- Pearson, M.L.; Wu, S.; Schaefer, J.; Bonomi, A.E.; Shortell, S.M.; Mendel, P.J.; Marsteller, J.A.; Louis, T.A.; Rosen, M.; Keeler, E.B. Assessing the implementation of the chronic care model in quality improvement collaboratives. Health Serv. Res. 2005, 40, 978–996. [Google Scholar] [CrossRef] [PubMed]
- Greenhalgh, T.; Robert, G.; Macfarlane, F.; Bate, P.; Kyriakidou, O. Diffusion of innovations in service organizations: Systematic review and recommendations. Milbank Q. 2004, 82, 581–629. [Google Scholar] [CrossRef]
- Shojania, K.G.; Ranji, S.R.; McDonald, K.M.; Grimshaw, J.M.; Sundaram, V.; Rushakoff, R.J.; Owens, D.K. Effects of quality improvement strategies for type 2 diabetes on glycemic control: A meta-regression analysis. JAMA 2006, 296, 427–440. [Google Scholar] [CrossRef]
- Berwick, D.M. A primer on leading the improvement of systems. BMJ 1996, 312, 619–622. [Google Scholar] [CrossRef] [PubMed]
- Finch, T. Teledermatology for chronic disease management: Coherence and normalization. Chronic Illn. 2008, 4, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Lloyd, A.; Joseph-Williams, N.; Edwards, A.; Rix, A.; Elwyn, G. Patchy ‘coherence’: Using normalization process theory to evaluate a multi-faceted shared decision making implementation program (magic). Implement. Sci. 2013, 8, 102. [Google Scholar] [CrossRef] [PubMed]
- State of the American Workplace: Employee Engagement Insights for US Business Leaders. Available online: http://nicic.gov/library/027419 (accessed on 20 December 2014).
- Harter, J.K.; Schmidt, F.L.; Keyes, C.L. Well-being in the workplace and its relationship to business outcomes: A review of the gallup studies. Flourishing 2003, 2, 205–224. [Google Scholar]
- Cameron, K.; Mora, C.; Leutscher, T.; Calarco, M. Effects of positive practices on organizational effectiveness. J. Appl. Behav. Sci. 2011, 47, 266–308. [Google Scholar] [CrossRef]
- Reeve, J.; Dowrick, C.F.; Freeman, G.K.; Gunn, J.; Mair, F.; May, C.; Mercer, S.; Palmer, V.; Howe, A.; Irving, G.; et al. Examining the practice of generalist expertise: A qualitative study identifying constraints and solutions. JRSM Short Rep. 2013, 4. 2042533313510155. [Google Scholar] [CrossRef]
- Plews-Ogan, M.; Beyt, G. Wisdom Leadership in Academic Health Science Centers: Leading Positive Change; Radcliffe Publishing: New York, NY, USA, 2013. [Google Scholar]
- Gittell, J.H.; Godfrey, M.; Thistlethwaite, J. Interprofessional collaborative practice and relational coordination: Improving healthcare through relationships. J. Interprof. Care 2013, 27, 210–213. [Google Scholar] [CrossRef] [PubMed]
- Cramm, J.M.; Nieboer, A.P. Relational coordination promotes quality of chronic care delivery in dutch disease-management programs. Health Care Manag. Rev. 2012, 37, 301–309. [Google Scholar] [CrossRef]
- Cramm, J.M.; Nieboer, A.P. In The Netherlands, rich interaction among professionals conducting disease management led to better chronic care. Health Aff. (Millwood) 2012, 31, 2493–2500. [Google Scholar] [CrossRef]
- Pariser, G.; Hager, K.; Gillette, P.; Golemboski, K.; Jackson, K. Active steps for diabetes: A community-campus partnership addressing frailty and diabetes. Diabetes Educ. 2014, 40, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Wagner, E.H.; Austin, B.T.; Davis, C.; Hindmarsh, M.; Schaefer, J.; Bonomi, A. Improving chronic illness care: Translating evidence into action. Health Aff. (Millwood) 2001, 20, 64–78. [Google Scholar] [CrossRef]
- Ory, M.G.; Ahn, S.; Jiang, L.; Smith, M.L.; Ritter, P.L.; Whitelaw, N.; Lorig, K. Successes of a national study of the chronic disease self-management program: Meeting the triple aim of health care reform. Med. Care 2013, 51, 992–998. [Google Scholar] [CrossRef] [PubMed]
- Eton, D.T.; Elraiyah, T.A.; Yost, K.J.; Ridgeway, J.L.; Johnson, A.; Egginton, J.S.; Mullan, R.J.; Murad, M.H.; Erwin, P.J.; Montori, V.M. A systematic review of patient-reported measures of burden of treatment in three chronic diseases. Patient Relat. Outcome Meas. 2013, 4, 7–20. [Google Scholar] [CrossRef] [PubMed]
- Krumholz, H.M. Post-hospital syndrome—An acquired, transient condition of generalized risk. N. Engl. J. Med. 2013, 368, 100–102. [Google Scholar] [CrossRef] [PubMed]
- Leppin, A.L.; Bora, P.R.; Tilburt, J.C.; Gionfriddo, M.R.; Zeballos-Palacios, C.; Dulohery, M.M.; Sood, A.; Erwin, P.J.; Brito, J.P.; Boehmer, K.R.; et al. The efficacy of resiliency training programs: A systematic review and meta-analysis of randomized trials. PLoS One 2014, 9, e111420. [Google Scholar] [CrossRef] [PubMed]
- Miller, W.L.; Crabtree, B.F.; McDaniel, R.; Stange, K.C. Understanding change in primary care practice using complexity theory. J. Fam. Pract. 1998, 46, 369–376. [Google Scholar] [PubMed]
- Rogers, E.M. A prospective and retrospective look at the diffusion model. J. Health Commun. 2004, 9, 13–19. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.M.; Soubhi, H.; Fortin, M.; Hudon, C.; O’Dowd, T. Interventions for improving outcomes in patients with multimorbidity in primary care and community settings. Cochrane Database Syst. Rev. 2012, 4. CD006560. [Google Scholar] [PubMed]
- Reeve, J.; Blakeman, T.; Freeman, G.K.; Green, L.A.; James, P.A.; Lucassen, P.; Martin, C.M.; Sturmberg, J.P.; van Weel, C. Generalist solutions to complex problems: Generating practice-based evidence—The example of managing multi-morbidity. BMC Fam. Pract. 2013, 14, 112. [Google Scholar] [CrossRef] [PubMed]
- Mair, F.S.; May, C.R. Thinking about the burden of treatment. BMJ 2014, 349, g6680. [Google Scholar] [CrossRef] [PubMed]
- Martin, C.; Sturmberg, J. Complex adaptive chronic care. J. Eval. Clin. Pract. 2009, 15, 571–577. [Google Scholar] [CrossRef] [PubMed]
- Reuben, D.B.; Tinetti, M.E. Goal-oriented patient care—An alternative health outcomes paradigm. N. Engl. J. Med. 2012, 366, 777–779. [Google Scholar] [CrossRef] [PubMed]
- Stange, K.C.; Nutting, P.A.; Miller, W.L.; Jaen, C.R.; Crabtree, B.F.; Flocke, S.A.; Gill, J.M. Defining and measuring the patient-centered medical home. J. Gen. Intern. Med. 2010, 25, 601–612. [Google Scholar] [CrossRef] [PubMed]
- Boult, C.; Wieland, G.D. Comprehensive primary care for older patients with multiple chronic conditions: “Nobody rushes you through”. JAMA 2010, 304, 1936–1943. [Google Scholar] [CrossRef] [PubMed]
- Dorr, D.A.; Wilcox, A.; Burns, L.; Brunker, C.P.; Narus, S.P.; Clayton, P.D. Implementing a multidisease chronic care model in primary care using people and technology. Disease Manag. 2006, 9, 1–15. [Google Scholar] [CrossRef]
- Katon, W.J.; Lin, E.H.; von Korff, M.; Ciechanowski, P.; Ludman, E.J.; Young, B.; Peterson, D.; Rutter, C.M.; McGregor, M.; McCulloch, D. Collaborative care for patients with depression and chronic illnesses. N. Engl. J. Med. 2010, 363, 2611–2620. [Google Scholar] [CrossRef] [PubMed]
- McGregor, M.; Lin, E.H.; Katon, W.J. Teamcare: An integrated multicondition collaborative care program for chronic illnesses and depression. J. Ambul. Care Manag. 2011, 34, 152–162. [Google Scholar] [CrossRef]
- Muth, C.; van den Akker, M.; Blom, J.W.; Mallen, C.D.; Rochon, J.; Schellevis, F.G.; Becker, A.; Beyer, M.; Gensichen, J.; Kirchner, H.; et al. The ariadne principles: How to handle multimorbidity in primary care consultations. BMC Med. 2014, 12, 223. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Leppin, A.L.; Montori, V.M.; Gionfriddo, M.R. Minimally Disruptive Medicine: A Pragmatically Comprehensive Model for Delivering Care to Patients with Multiple Chronic Conditions. Healthcare 2015, 3, 50-63. https://doi.org/10.3390/healthcare3010050
Leppin AL, Montori VM, Gionfriddo MR. Minimally Disruptive Medicine: A Pragmatically Comprehensive Model for Delivering Care to Patients with Multiple Chronic Conditions. Healthcare. 2015; 3(1):50-63. https://doi.org/10.3390/healthcare3010050
Chicago/Turabian StyleLeppin, Aaron L., Victor M. Montori, and Michael R. Gionfriddo. 2015. "Minimally Disruptive Medicine: A Pragmatically Comprehensive Model for Delivering Care to Patients with Multiple Chronic Conditions" Healthcare 3, no. 1: 50-63. https://doi.org/10.3390/healthcare3010050
APA StyleLeppin, A. L., Montori, V. M., & Gionfriddo, M. R. (2015). Minimally Disruptive Medicine: A Pragmatically Comprehensive Model for Delivering Care to Patients with Multiple Chronic Conditions. Healthcare, 3(1), 50-63. https://doi.org/10.3390/healthcare3010050





