No Borders for Tobacco Smoke in Hospitality Venues in Vienna
Abstract
: In public places many countries banned smoking as the most important indoor source of fine airborne particulate matter. In Austria partial bans have been in force since 2009, with exemptions for the hospitality industry. From February to October 2010 we investigated PM2.5 concentrations in the breathing area of guests in well frequented Viennese establishments of all sizes, and compared these chance indoor samples with PM2.5 concentrations measured during the same half hour at the next outdoor monitoring station. The laser particle counter (OPC1.108, Grimm®) used for indoor measurements had been calibrated by ß-attenuation (FH 62 I-R, Eberline®), which was used outdoors. 48% of 112 venues visited did not fully comply with the law, notwithstanding its weakness. Highest median concentrations (in μg/m3) were found in bars (443.7), followed by nightclubs/discotheques (421.1), pubs (147.7), cafes (106.1) and restaurants (23.4). Concentrations increased with number of smokers present (p < 0.01), with medians of 282.4/241,3/67.6/6.9 μg/m3 in smoking venues/smoking rooms/adjacent non-smoking rooms/exclusive non-smoking venues. Only for the latter, a significant correlation was found with outdoor concentrations (r = 0.48, p < 0.01), while concentrations in non-smoking rooms were higher (p < 0.01) and unrelated to outdoor concentrations, but significantly dependent on concentrations in the adjacent smoking room (r = 0.64, p < 0.01). In conclusion, the partial smoking ban failed and guests of Viennese hospitality venues continue to risk disease from passive smoking, even in so-called “non-smoking rooms”, which are second-hand smoke rooms.1. Introduction
Environmental Tobacco Smoke (ETS) or Secondhand-Smoke (SHS) holds responsibility for severe health effects [1], particularly for the cardiovascular system [2], being associated mainly with fine particulate matter (aerodynamic diameter below 2.5 μm, PM2.5) [3]. Earlier studies reported high concentrations of nicotine, fine and ultrafine particulates in the indoor air of hospitality establishments [4-6], a correlation between air nicotine and active particle surface [7], with relatively highest exposures in Vienna in international comparison [4], but a systematic exposure assessment in comparison with outdoor concentrations over several months was lacking.
Due to expected health benefits of legal interventions restricting the right to smoke in gastronomic facilities spokespersons of the European Commission had already announced in 2009 that the commission would focus on implementing a complete smoking ban in enclosed public places by the end of 2012 [8]. With enforcement of smoke-free legislation declines of PM2.5 were documented [9,10], as well as decreases of myocardial infarction in the general population and improvement of respiratory health in hospitality industry workers. The Austrian government, however, decided in 2008 for a partial smoking ban [11] as introduced in Spain 2006, but replaced in 2010 by a total ban.
In principle Austrian hospitality venues have been required to offer a smoke-free room since 2009 and smoking may optionally be allowed only in separate smoking rooms, “if smoke does not invade into the protected area”, but so many exceptions have been made from this rule that owners are invited to adapt some of them to their establishment: If the venue does not consist of more than one room for the provision of food or drinks to the guests and if the size of the floor space of this room measures less than 50 m2, the owners can decide for themselves whether they allow smoking or not; those of over 80 m2 would have to separate a smoking from a non-smoking section, if they wish to allow their customers to smoke, whilst those in between can claim the former's right to decide sovereignly in case of monument protection or building inspection department forbidding reconstruction [11]. No inspections had been foreseen unless violations of the law are reported by customers.
Bearing this legal background in mind, our goal was to investigate the effect of the Austrian law, especially on the air quality in the non-smoking sections of mixed facilities. Prior studies showed weak but significant positive correlations between PM2.5 concentrations of adjacent smoking and non-smoking rooms, e.g., in Catalonian hospitals [12], and suggested room segregation would be an insufficient measure to avoid relevant air pollution [13], since penetration rates for small particles like tobacco smoke or diesel soot reach up to 70% [14].
2. Methods
All hospitality establishments on main shopping and dining streets in the inner nine districts of Vienna were checked and if open and used by customers at the time of the visit air samples were taken without prior warning, usually while ordering and having a drink. An optical particle counter (OPC 1.108, Grimm®) was put on a table (near the breathing area of guests) and run for 20 minutes per smoking/non-smoking section. Investigators deliberately tried to keep away from open doors and open fireplaces and omitted the immediate vicinity of active smokers. Thereby the representativeness of the sample for room air breathed by customers should be increased. 112 hospitality venues were visited between February 2 and October 17, 2010 and a total of 133 air measurements performed, until the collection was found to contain a representative sample of all types of venues. Wherever possible further parameters were documented including the sizes of the floor areas of the salesrooms (using a laser distance meter), the number of customers, number of smoking customers, whether doors/windows were open, open fire places or pizza ovens and tea lights. In ‘mixed venues’, consisting of separated smoking and non-smoking areas, consecutive measurements in both sections were conducted, starting with the smoke-free one. Outside air pollution concentrations were provided by the city's municipal department for air control. Ambient air quality monitoring for PM2.5 was done by the same apparatus as used for calibration of the OPC: ß-attenuation (FH 62 I-R, Eberline®) [15].
The Grimm OPC1.108 can be used for secret measurements, because it is small (24 × 13 × 7 cm) and emits little noise. Ambient air is drawn into a laser chamber, where the light scattering depending on size and concentration of particles in the air stream is being detected [16]. The apparatus distinguishes 15 particle dimensions, detectable particle sizes range from 0.3 to 20 μm [17]. Particle number concentrations are translated into mass concentration figures using manufacturer-specific conversion factors [18]. In comparison to results produced by Differential Mobility Analyzer OPC1.108 gathers on average only 6% of the total atmospheric aerosol particle concentration, but in the relevant size range for PM2.5 differences are less than 10%. In terms of mass concentration the spectrometer underestimates the actual count by up to 36% (compared to gravimetric analysis of TSP on filter), which seems acceptable for the purpose [18]. Data was loaded to PCs using Grimm software. For each measurement one arithmetic mean was calculated using Microsoft Excel Starter v. 14.0.5128.5001 and later transferred into SPSS v. 16.00 files where other parameters were added.
Groups were formed according to the observed venue types (smoking/non-smoking) and not according to the labeled type. Descriptive statistical methods applied to the data include calculations of arithmetic mean, median, and variance of PM2.5 concentration values. To illustrate the range of obtained values in dependence on presence and number of smokers and other parameters as well as to detect statistical outliers we used box plots. Cross tabulations are used to display the influence of venue type (i.e., smoking, non-smoking or mixed) and size on their conformity with law. Investigating the correlation of PM2.5 in smoking areas and corresponding non-smoking sections of mixed type venues we integrated a linear regression model together with the Spearman rank correlation test, which also elucidated the linkage between PM2.5 inside enclosed public places and the outside air pollution. Wilcoxon rank-sum test was conducted to determine how tea lights and open doors/windows affected air quality. Finally, Kruskal-Wallis one-way analysis of variance was run to detect significant differences in venues grouped by number of smokers.
3. Results and Discussion
We conducted a total of 133 measurements of PM2.5 in 112 hospitality venues, some of which were sampled twice taking mixed type facilities into account. One sampled venue had to be eliminated, because of the use of fog machines and the exorbitant result of more than 6 mg/m3, which had to be interpreted as an artifact (exceedance of measurement range by fog mixed with smoke). In the first 25 visits a median PM2.5 concentration of 471.5 (range 18.1–2,064.7) was found, but the size (and in three of them also the type of venue) had been registered incompletely, so that these data had to be eliminated from the corresponding analyses.
The overall median of all measurements (except for the venue with the fog machine) was 200.2 μg/m3 (range 1.1–3085 μg/m3). 38 measurements in bars presented with the highest median concentration (443.7 μg/m3), closely followed by 22 in nightclubs/discotheques (421.05 μg/m3), and, more distant, 16 in pubs (147.7 μg/m3), 29 in cafes (106.1 μg/m3) and 22 in restaurants (23.35 μg/m3).
Floor space of the guest room (of smoking + non-smoking + mixed facilities) was controlled in 86 venues and found to be below 50 m2 in 10 (7 + 3 + 0), between 50 and 80 m2 in 15 (13 + 1 + 1) and above 80 m2 in 61 (27 + 12 + 22).
3.1. How does Smoking Affect Air Quality?
The median (geometric mean) of all non-smoking areas was 23.5 (23.8) μg/m3, whilst that for smoking areas averaged 264.95 (290.4) μg/m3. Inspected more closely, non-smoking areas of exclusive non-smoking venues showed a median (geometric mean) of 6.9 (7.7) μg/m3, non-smoking areas of mixed type facilities 67.6 (66.1) μg/m3 smoking areas of mixed type venues 241.3 (235.4) μg/m3 and exclusive smoking premises 282.4 (316.6) μg/m3. Figure 1 illustrates box plots of fine particulate air pollution arranged by type of venue.
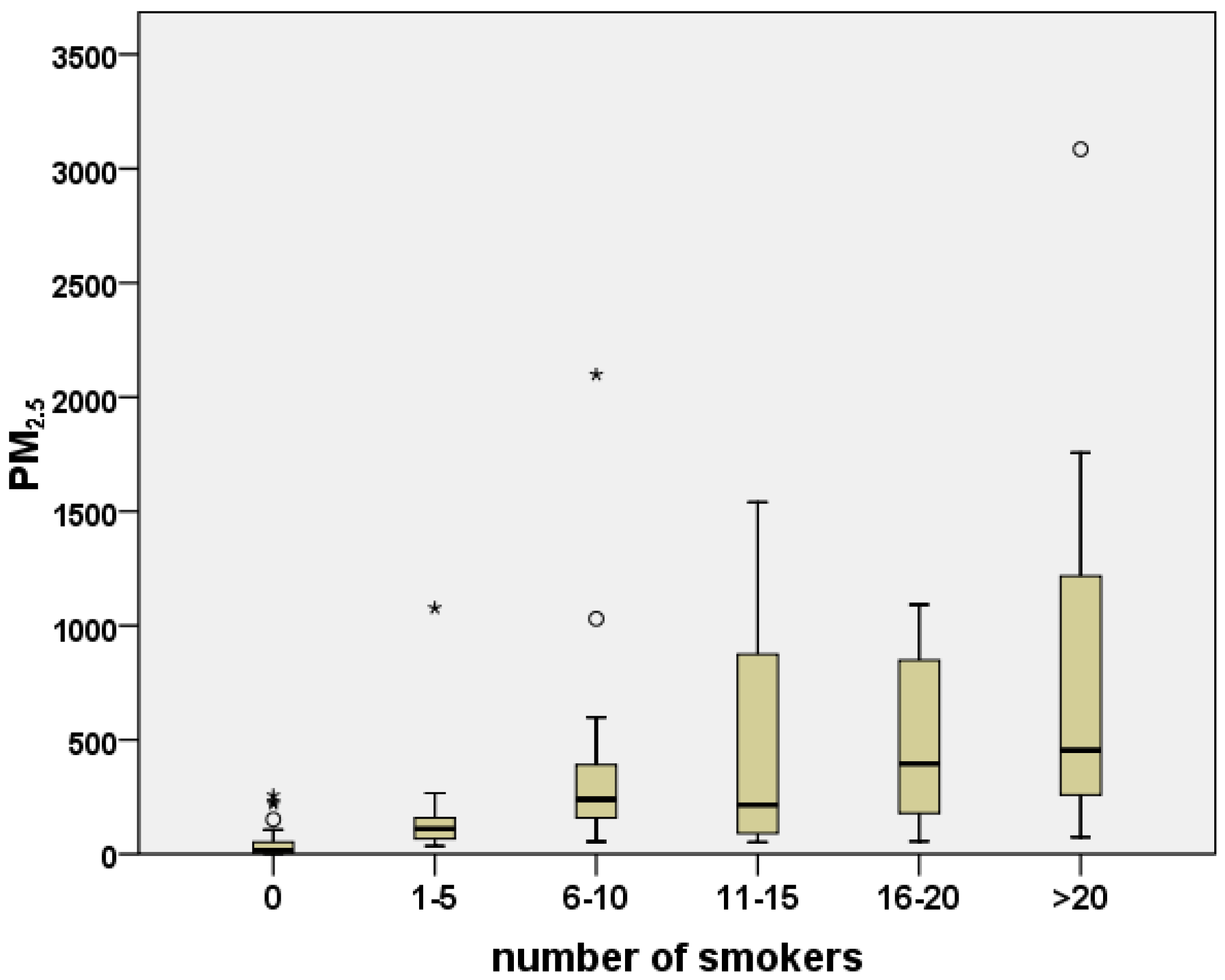
As a non-parametric testing procedure investigating inequalities among groups of interest Kruskal-Wallis one-way analysis of variance was carried out to corroborate the theory of the degree of air pollution being a direct consequence of the observed number of smoking customers. For this purpose we assorted measurements by number of smokers (Figure 2). Differences in PM2.5 between the groups turned out to be significant at the 0.01 level, which concedes the inference that the number of smoking customers is a strong predictor of the expectable particulate mass concentration below 2.5 μm diameter.
3.2. What Affects Air Quality in Non-Smoking Areas ?
Focusing especially on the non-smoking areas' air quality Mann-Whitney U test was applied to quantify the impact of tea lights, open doors/windows, and the presence of adjacent smoking sections (the Wilcoxon rank sum test was designed to work out whether or not differences of two independent groups' medians are of above-chance dimension). For neither tea lights (asymptotic significance (2-tailed) being 0.824) nor open doors/windows (0.315) significant differences could be verified. By contrast the vicinity of declared smoking areas was found to be a key influencing variable, showing a linkage significant at the 0.01 level. We went into that discovery and calculated Spearman's rank correlation coefficient for non-smoking areas' PM2.5 concentrations as a function of adjacent smoking sections' PM2.5 concentrations, leading to a result significant at the 0.01 level with a correlation factor of 0.644 (see Figure 3). Calculations of Spearman's rho for non-smoking areas' air quality in dependence on ambient air pollution revealed significance at the 0.01 level too, albeit accompanied by smaller correlation factors. Table 1 gives an insight on how the abovementioned characteristics were distributed amongst non-smoking areas.
3.3. Who Abides by the Law?
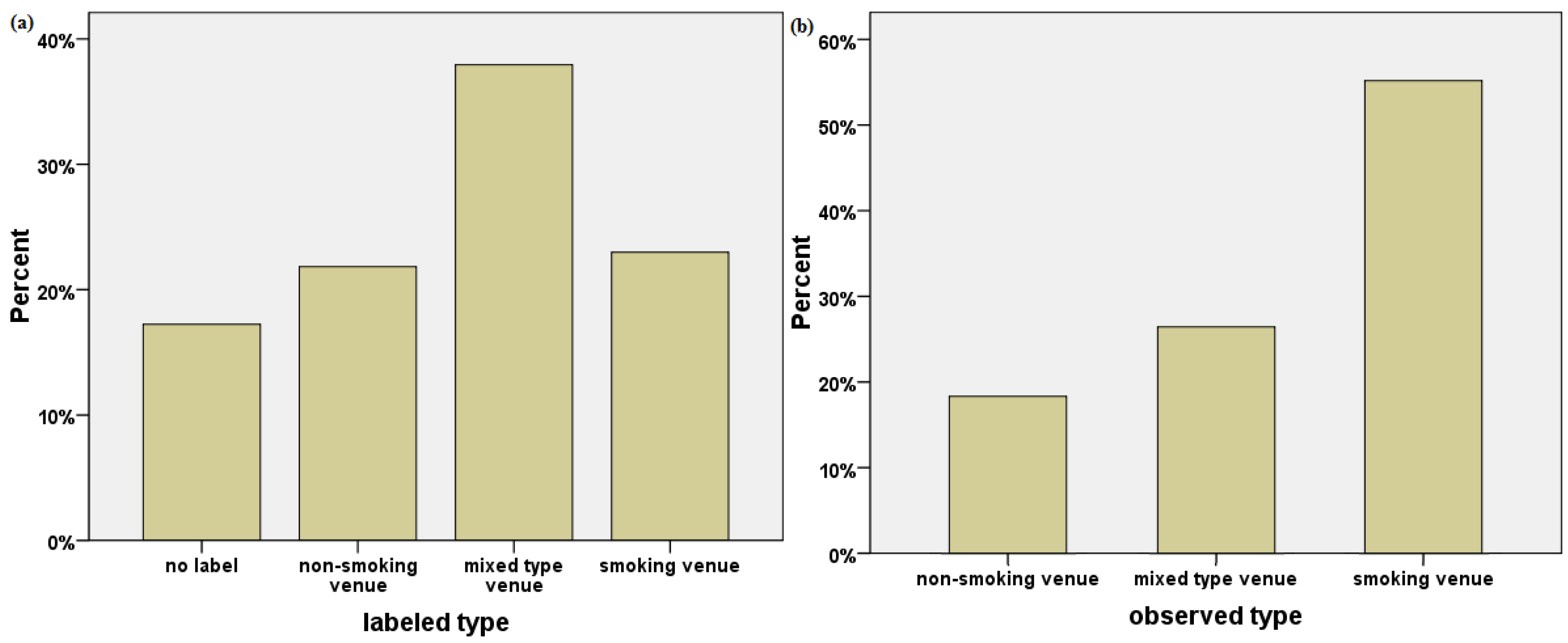
The Austrian tobacco law requires to visibly signpost premises as smoking or non-smoking areas [11]. In the course of our fieldwork, we soon became aware that many venues had not been labeled correctly. Broken down to two crucial characteristics of the obtained venues, namely size (documented for 86 establishments) and type (i.e., smoking, non-smoking or mixed), particularly medium sized facilities and those labeled as mere smoking venues seemed to have the greatest difficulties abiding by the law (see Table 2). Based on a total of 111 venues with documented labeling or its absence, 33 (29.7%) observed the law at the time of our visit, whereas 53 (47.7%) did not. Figure 4 illustrates the difference between labeled and observed use.
3.4. Discussion
The dangers of active and passive smoking have been clarified sufficiently [1-3], so have the increased mortality and morbidity caused by ambient air pollution characterized by PM2.5 [3,19]. Similar pathogenetic mechanisms are suspected for cardiovascular disease from outdoor PM2.5 and indoor tobacco smoke [3,20]. In our study PM2.5 was confirmed to be a good indicator for the extent of air pollution from cigarette smoke in hospitality venues as had been suggested by earlier works [7]. Also from a convenience sample of hospitality venues in nine of 26 cantons in Switzerland the authors concluded, that partial smoking restriction is ineffective, even if smoking and non-smoking areas are separated into different rooms [13]. In central Zurich a random sample of hospitality establishments was sampled during 14 warm, sunny days, and despite of the use of outdoor seats by part of the smokers, they were identified as the most important PM2.5 source [6]. In our study covering a longer period, smoking areas' PM2.5 pollution exceeded non-smoking areas' PM2.5 concentration levels by (at least) a factor of 10, even if venues of the mixed sort were included. In comparison to Swiss restaurants, cafes and bars indoor pollution in Vienna hospitality venues seems to be even worse and gives rise to serious concern. Patients with asthma or coronary heart disease should be warned, because they might suffer an acute attack when inhaling smoke-filled air during a meal. After a myocardial infarction or a stroke, a relapse might occur even in a so-called “non-smoking room” adjacent to a smoking room, because particulate exposure is higher there than in dense traffic outside, which has been identified as a risk [19,21]. Outdoor PM2.5 defines the baseline exposure, dominating the air quality of non-smoking venues without adjacent smoking rooms. Only in these rooms the influence of other indoor sources could possibly be investigated in a larger sample; however, no significant associations had been found with other indoor sources such as tea-lights or with open doors or windows, neither in Vienna, nor in Zürich. Austrian and Swiss results identified tobacco smoke as the dominant pollutant, penetrating into neighboring non-smoking rooms even when separated by a (usually) closed door.
85.1% (40/47) of all documented exclusive smoking establishments and 93.3% (14/15) of the mid-sized venues did not abide to the Austrian law, making it highly questionable whether the complicated regulation is understood and accepted. In public letters, owners had reported that they find it unfair having to invest in an expensive separation, while the neighbor competitor is free to allow smoking in a smaller establishment or got permission because of smaller size or dispensation from the building inspector. Employees are not protected by the law, not even trainees. In Austria, children may be brought to smoking rooms without age limit. No control of the partial smoking ban is foreseen until a victim complains. Follow up of complaints is left at the disposal of local authorities without any extra personnel and without central documentation. Two self-help groups of patients complained to the ombudsman about administrative barriers and intimidation by innkeepers, who received the names of the informants by the administration.
In contrast to other countries, such as in Northern and Western Europe, which have successfully introduced indoor smoking restrictions as part of their tobacco control strategy, tobacco industry influence and passive smoke exposure in hospitality venues are still major concerns in Central Europe [22] and in Austria in particular [23-25]. A smoking ban without exceptions for the hospitality industry would be the most cost-effective measure to reduce cardiovascular morbidity and mortality [3,26-28].
3.5. Limitations
Since Grimm OPC1.108 is not capable of detecting particles of less than 0.3 μm size, which are possibly more hazardous because of their large active surface, we plan to assess the ultrafine particle pollution with new technology in the next study. Samples collected before July 1, 2010, the deadline for renovations, should be repeated. Eventually a bigger sample size would be of use to quantify the difference in mixed venues' non-smoking sectors' air quality made by diverse kinds of partition. Simultaneous sampling in smoking room and non-smoking room over longer periods of time would be of advantage if equally calibrated instruments are available. If room height is measured in addition to ground space, numbers of smokers could be given by room space. We omitted to ask about running ventilation characteristics, because we preferred a sample unbiased by selection from participation.
4. Conclusions
We found evidence that compliance with the tobacco law is alarmingly low in the hospitality industry of Vienna, we have no reason to assume better results in other Austrian cities, and advise the Austrian government to rethink its ‘Spanish compromise solution’, which was abandoned in Spain in 2010, because it failed. We proved the insufficiency of non-smokers protection by physical barriers built to keep a room's air clean while people smoke next door. Consequently a 100% smoke-free regulation is necessary for effective protection of staff and customers.


| number | % of total sites | % of nonsmoking sites | PM2.5Median [μg/m3] | |
|---|---|---|---|---|
| Non-smoking areas | 40 | 36 | 100 | 23.5 |
| … + tea lights | 3 | 2.7 | 7.5 | 67.6 |
| … + open doors/windows | 12 | 10.8 | 30 | 12.9 |
| … adjacent to smoking area | 21 | 52.5 | 18.9 | 67.6 |
| In conformity with the law? | ||||
|---|---|---|---|---|
| Yes (%) | No (%) | Total | ||
| Type | non-smoking | 15 (93.8) | 1 (6.2) | 16 |
| mixed | 11 (47.8) | 12 (52.2) | 23 | |
| smoking | 7(14.9) | 40 (85.1) | 47 | |
| Total | 33 | 53 | 86 | |
| Size [m2] | <50 | 10(100) | 0(0) | 10 |
| 50–80 | 1 (6.7) | 14 (93.3) | 15 | |
| >80 | 22(36.1) | 39(63.9) | 61 | |
| Total | 33 | 53 | 86 | |
Acknowledgments
The authors are grateful to the Viennese city administration for providing outside air data, especially municipal department 22, and thank Hanns Moshammer and Benedikt Feichter for help with instrument calibration, data collection and analysis.
References
- US Surgeon General. US Dept. of Health & Human Services. The Health Consequences of Involuntary Smoking, Available online: http://www.surgeongeneral.gov/library/secondhandsmoke/ (accessed on 27 April 2011).
- Law, M.R.; Wald, N.J. Environmental tobacco smoke and ischemic heart disease. Prog. Cardiovasc. Dis. 2003, 46, 31–38. [Google Scholar]
- Pope, C.A., 3rd; Burnett, R.T.; Krewski, D.; Jerrett, M.; Shi, Y.; Calle, E.E.; Thun, M.J. Cardiovascular mortality and exposure to airborne fine particulate matter and cigarette smoke: Shape of the exposure-response relationship. Circulation 2009, 120, 941–948. [Google Scholar]
- Nebot, M.; Lopez, M.J.; Gorini, G.; Neuberger, M.; Axelsson, S.; Pilali, M.; Fonseca, C.; Abdennbi, K.; Hackshaw, A.; Moshammer, H.; et al. Environmental tobacco smoke exposure in public places of European cities. Tob. Control 2005, 14, 60–63. [Google Scholar]
- Gorini, G.; Moshammer, H.; Sbrogio, L.; Gasparrini, A.; Nebot, M.; Neuberger, M.; Tamang, E.; Lopez, M.J.; Galeone, D.; Serrahima, E. Italy and Austria before and after study: Second-hand smoke exposure in hospitality premises before and after 2 years from the introduction of the Italian smoking ban. Indoor Air 2008, 18, 328–334. [Google Scholar]
- Daly, B.J.; Schmid, K.; Riediker, M. Contribution of fine particulate matter sources to indoor exposure in bars, restaurants, and cafes. Indoor Air 2010, 20, 204–212. [Google Scholar]
- Moshammer, H.; Neuberger, M.; Nebot, M. Nicotine and surface of particulates as indicators of exposure to environmental tobacco smoke in public places in Austria. Int. J. Hyg. Environ. Health 2004, 207, 337–343. [Google Scholar]
- Tuffs, A. EU commissioner pursues smoking ban in enclosed public spaces for Europe. BMJ 2010, 341, c5708. [Google Scholar]
- Rosen, L.J.; Zucker, D.M.; Rosen, B.J.; Connolly, G.N. Second-hand smoke levels in Israeli bars, pubs and cafes before and after implementation of smoke-free legislation. Eur. J. Public Health 2011, 21, 15–20. [Google Scholar]
- Semple, S.; van Tongeren, M.; Galea, K.S.; MacCalman, L.; Gee, I.; Parry, O.; Naji, A.; Ayres, J.G. UK smoke-free legislation: Changes in PM2.5 concentrations in bars in Scotland, England, and Wales. Ann. Occup. Hyg. 2010, 54, 272–280. [Google Scholar]
- Bundesgesetzblatt für die Republik Österreich—Änderung des Tabakgesetzes, Available online: https://www.ris.bka.gv.at/Dokumente/BgblAuth/BGBLA_2008_I_120/BGBLA_2008_I_120.html (accessed on 27 April 2011).
- Sureda, X.; Fu, M.; Lopez, M.J.; Martinez-Sanchez, J.M.; Carabasa, E.; Salto, E.; Martinez, C.; Nebot, M.; Fernandez, E. Second-hand smoke in hospitals in Catalonia (2009): A cross-sectional study measuring PM2.5 and vapor-phase nicotine. Environ. Res. 2010, 110, 750–755. [Google Scholar]
- Huss, A.; Kooijman, C.; Breuer, M.; Bohler, P.; Zund, T.; Wenk, S.; Roosli, M. Fine particulate matter measurements in Swiss restaurants, cafes and bars: What is the effect of spatial separation between smoking and non-smoking areas? Indoor Air 2010, 20, 52–60. [Google Scholar]
- Hanninen, O.O.; Lebret, E.; Ilacqua, V.; Katsouyanni, K.; Kunzli, F.; Sram, R.J.; Jantunen, M. Infiltration of ambient PM2.5 and levels of indoor generated non-ETS PM2.5 in residences of four European cities. Atmos. Environ. 2004, 38, 6411–6423. [Google Scholar]
- Hauck, H.; Berner, A.; Gomiscek, B.; Stopper, S.; Puxbaum, H.; Kundi, M.; Preining, O. On the equivalence of gravimetric PM data with TEOM and betaattenuation measurements. Aerosol Sci. 2004, 35, 1135–1149. [Google Scholar]
- Stieβ, M. Mechanische Verfahrenstechnik—Partikeltechnologie 1, 3rd ed.; Springer: Berlin, Germany, 2009; pp. 197–208. [Google Scholar]
- Grimm Aerosol Technik GmbH & Co Kg Homepage. Available online: http://www.grimmaerosol.com/en/Indoor-Air-Quality/2/2/index.html (accessed on 27 April 2011).
- Burkart, J.; Steiner, G.; Reischl, G.; Moshammer, H.; Neuberger, M.; Hitzenberger, R. Characterizing the performance of two optical particle counters (Grimm OPC1.108 and OPC1.109) under urban aerosol conditions. J. Aerosol Sci. 2010, 41, 953–962. [Google Scholar]
- Neuberger, M.; Moshammer, H.; Rabczenko, D. Extended effects of air pollution on cardiopulmonary mortality in Vienna. Atmos. Environ. 2007, 41, 8549–8556. [Google Scholar]
- Brook, R.D.; Rajagopalan, S.; Pope, C.A., 3rd; Brook, J.R.; Bhatnagar, A.; Diez-Roux, A.V.; Holguin, F.; Hong, Y.; Luepker, R.V.; Mittleman, M.A.; et al. Particulate matter air pollution and cardiovascular disease: An update to the scientific statement from the American Heart Association. Circulation 2010, 121, 2331–2378. [Google Scholar]
- Peters, A.; von Klot, S.; Heier, M.; Trentinaglia, I.; Hormann, A.; Wichmann, H.E.; Lowel, H. Exposure to traffic and the onset of myocardial infarction. N. Engl. J. Med. 2004, 351, 1721–1730. [Google Scholar]
- Joossens, L.; Raw, M. The Tobacco Control Scale: a new scale to measure country activity. Tob. Control, 2006, 15, pp. 247–253. Update 2010 Available online: http://www.cancer.be/images/journaliste/rapport-TCS.pdf (accessed 2 June 2011). [Google Scholar]
- Simpson, D. Austria: Small but deadly. Tob. Control 2005, 14, 3–4. [Google Scholar]
- Neuberger, M. Nichtraucherschutz: Jahrzehnt der verpassten Chance. Universum Innere Medizin, 2009; Sonderausgabe. pp. 90–91. Available online: http://www.medmedia.at/media/sidebar/UIM-10-Jahre.pdf (accessed 2 June 2011). [Google Scholar]
- Smolle-Jüttner, F.M. Rauchverbot ohne Kompromisse ist der einzige Weg aus der Misere. Wien Klin Wochenschr 2009, 121, 486–490. [Google Scholar]
- Lightwood, J.M.; Glantz, S.A. Declines in acute myocardial infarction after smoke-free laws and individual risk attributable to secondhand smoke. Circulation 2009, 120, 1373–1379. [Google Scholar]
- Meyers, D.G.; Neuberger, J.S.; He, J. Cardiovascular effect of bans on smoking in public places: a systematic review and meta-analysis. J. Am. Coll. Cardiol. 2009, 54, 1249–1255. [Google Scholar]
- Hauri, D.D.; Lieb, C.M.; Rajkumar, S.; Kooijman, C.; Sommer, H.L.; Roosli, M. Direct health costs of environmental tobacco smoke exposure and indirect health benefits due to smoking ban introduction. Eur. J. Public Health 2010, 21, 316–322. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Pletz, H.; Neuberger, M. No Borders for Tobacco Smoke in Hospitality Venues in Vienna. Atmosphere 2011, 2, 171-181. https://doi.org/10.3390/atmos2020171
Pletz H, Neuberger M. No Borders for Tobacco Smoke in Hospitality Venues in Vienna. Atmosphere. 2011; 2(2):171-181. https://doi.org/10.3390/atmos2020171
Chicago/Turabian StylePletz, Herbert, and Manfred Neuberger. 2011. "No Borders for Tobacco Smoke in Hospitality Venues in Vienna" Atmosphere 2, no. 2: 171-181. https://doi.org/10.3390/atmos2020171
APA StylePletz, H., & Neuberger, M. (2011). No Borders for Tobacco Smoke in Hospitality Venues in Vienna. Atmosphere, 2(2), 171-181. https://doi.org/10.3390/atmos2020171





