Overcoming the Cutaneous Barrier with Microemulsions
Abstract
:1. Introduction
2. Basic Concepts
| Parameter | Microemulsion | Emulsion | Nanoemulsion |
|---|---|---|---|
| Type of dispersion | colloidal | coarse | colloidal |
| Internal phase size (μm) * | up to 0.15 | above 0.5 | up to 0.25 |
| Thermodynamic stability | stable | not stable | not stable |
| Formation | spontaneous | require energy | require energy |
| Composition | requires greater amounts of surfactant and co-surfactant combination | requires less surfactant | requires less surfactant |
| Visual characteristics | |||
| Consistency | fluid | fluid/semi-solid | fluid |
| Turbidity | transparent | milky | may vary |
3. Why Use Microemulsions as Topical/Transdermal Delivery Systems?
- thermodynamic stability;
- the ease of preparation, as only low energy input is required;
- the cost of preparation being generally low, since no specialized equipment is necessary;
- the possibility of incorporating both hydrophilic and lipophilic drugs (at the same time, if desirable), due to the presence of hydrophilic and lipophilic domains;
- the increased drug loading, since the amphiphilic interface can be viewed as an additional region for drug solubilization if compared to non-structured oily or aqueous vehicles;
- the penetration-enhancing ability.
4. Mechanisms of Penetration Enhancement
5. Microemulsion Composition, Characteristics and Skin Penetration
| Surfactant blend or surfactant/co-surfactant | Components of the oil phase | Drug | Reference |
|---|---|---|---|
| Aerosol OT-based microemulsions | |||
| Aerosol OT/butanol | isopropyl palmitate | hydrophilic and lipophilic anesthetics | [50] |
| Aerosol OT/Tween 85 | isopropyl myristate | cyclosporine A | [51] |
| Aerosol OT | isopropyl myristate | 5-fluorouracil | [37] |
| PEGylated fatty alcohol (Brij)-based microemulsions | |||
| Polyoxyethylene (10) oleyl ether and1-hexanol | paraffin oil, isopropyl myristate or jojoba oil | sodium diclofenac | [52] |
| polyoxyethylene (20) cetyl ether and Span 80, ethanol, isopropyl alcohol, and propanol | soybean oil | sodium diclofenac | [48] |
| polyoxyethylene (10) dodecyl ether | tributyrin | progesterone | [53] |
| polyoxyethylene (10) oleyl ether, propylene glycol | glycerides of caprylic and capric acid | lycopene | [34] |
| polyoxyethylene (10) oleyl ether, propylene glycol, ethanol | monocaprylin | paclitaxel | [54] |
| Polysorbate (Tween)-based microemulsions | |||
| Tween 80 and Span 20/ethanol | isopropyl myristate | sodium nonivamide acetate | [55] |
| Tween 80, ethanol, isopropanol or propylene glycol | eucalyptus oil | hydrocortisone | [27] |
| Tween 80/propylene glycol | oleic acid, menthol | triptolide | [32] |
| Tween 80/ethanol | isopropyl myristate, n-hexylamine and iso-octylamine | diclofenac | [56] |
| Tween 80 or Span 80/ ethanol or isopropanol | lecithin, oleic acid or isopropyl myristate | estradiol | [57] |
| Tween 80/propylene glycol, ethanol, isopropanol | limonene, 1,8-cineole, α-terpineol | curcumin | [49] |
| polysorbate 80/ medium-chain glyceride | isopropyl myristate | celecoxib | [58] |
| PEGylated fatty acid esters-based microemulsions | |||
| PEG-8 glyceryl caprylate and caprate, diethylene glycol monoethyl ether (Transcutol P) | oleic acid | vinpocetine | [59] |
| PEG-8 caprylic and capric glycerides, polyglyceryl-6 dioleate | isopropyl myristate | diclofenac diethylamine | [60] |
| PEG-8 caprylic and capric glycerides/ polyglyceryl-6-dioleate | miglyol 812 | ascorbyl palmitate | [61] |
| caprylocaproyl macrogol-8- glycerides, Transcutol P | oleic acid | terbinafine | [62] |
| polyoxyl-35-castor oil, ethanol | oleoyl macrogol-6 glycerides EP | aceclofenac | [63] |
| polyoxyl-35-castor oil, ethanol | oleic acid | penciclovir | [47] |
| Phosphatidylcholine-based microemulsions | |||
| lecithin and linkers (sorbitan monooleate, sodium caprylate and caprylic acid) | isopropyl myristate | lidocaine | [64] |
| lecithin/n-propanol | isopropyl myristate | tetracaine hydrochloride | [65] |
| lecithin, isopropanol | isopropyl myristate, oleic acid | fluconazole | [66] |
| Other systems | |||
| glyceryl oleate/polyoxyl 40 fatty acid derivatives/tetraglycol | isopropyl myristate | lidocaine | [67] |
| tocopheryl polyethylene glycol 1000 succinate | oleic acid, isopropyl myristate | temozolomide hexyl ester | [68] |
| decylglucoside, propylene glycol, phytosphingosine | medium chain mono-diglycerides | α-tocopherol and lipoic acid | [69] |
| decyl polyglucoside, lecithin, propylene glycol, 1,2-hexanediol | 1-decanol, 1-dodecanol | miconazole nitrate | [70] |
| coco-glucoside, decylglucoside, lecithin | Labrafil M1944CS | 5-fluorouracil | [71] |
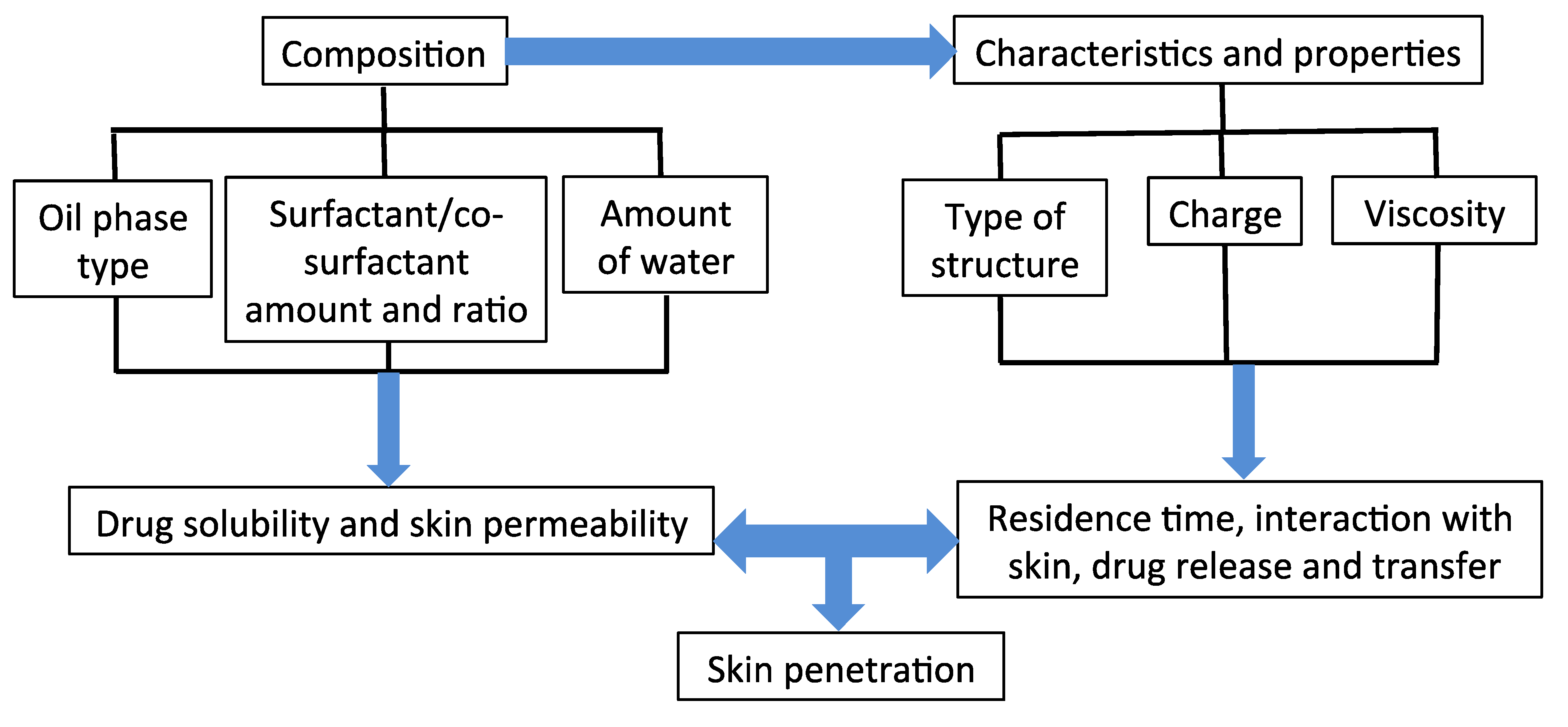
5.1. Influence of Microemulsion Components
5.1.1. Components of the Oil Phase
5.1.2. Surfactant/Co-Surfactant Blend
5.2. Influence of Microemulsion Characteristics
5.3. Influence of Water Content and Internal Structure
6. Use of Microemulsions for Topical and Transdermal Delivery
6.1. Transdermal Delivery
6.2. Local Effect
6.3. Commercial Formulations and Microemulsions
7. Potential Adverse Effects of Microemulsions
8. Conclusions
Acknowledgments
Conflicts of Interest
References
- Menon, G.K. New insights into skin structure: Scratching the surface. Adv. Drug Deliv. Rev. 2002, 54, S3–S17. [Google Scholar] [CrossRef]
- Madison, K.C. Barrier function of the skin: “La raison d’etre” of the epidermis. J. Investig. Dermatol. 2003, 121, 231–241. [Google Scholar] [CrossRef]
- Jepps, O.G.; Dancik, Y.; Anissimov, Y.G.; Roberts, M.S. Modeling the human skin barrier—Towards a better understanding of dermal absorption. Adv. Drug Deliv. Rev. 2013, 65, 152–168. [Google Scholar] [CrossRef]
- Bouwstra, J.A.; Honeywell-Nguyen, P.L.; Gooris, G.S.; Ponec, M. Structure of the skin barrier and its modulation by vesicular formulations. Prog. Lipid Res. 2003, 42, 1–36. [Google Scholar] [CrossRef]
- Van Smeden, J.; Janssens, M.; Gooris, G.S.; Bouwstra, J.A. The important role of stratum corneum lipids for the cutaneous barrier function. Biochim. Biophys. Acta 2013, 1841, 295–313. [Google Scholar]
- Otto, A.; du Plessis, J.; Wiechers, J.W. Formulation effects of topical emulsions on transdermal and dermal delivery. Int. J. Cosmet. Sci. 2009, 31, 1–19. [Google Scholar] [CrossRef]
- Peppin, J.F.; Pappagallo, M. Capsaicinoids in the treatment of neuropathic pain: A review. Ther. Adv. Neurol. Disord. 2014, 7, 22–32. [Google Scholar] [CrossRef]
- Lawrence, M.J.; Rees, G.D. Microemulsion-based media as novel drug delivery systems. Adv. Drug Deliv. Rev. 2000, 45, 89–121. [Google Scholar] [CrossRef]
- Kogan, A.; Garti, N. Microemulsions as transdermal drug delivery vehicles. Adv. Colloid Interface Sci. 2006, 123–126, 369–385. [Google Scholar] [CrossRef]
- Hathout, R.M.; Woodman, T.J.; Mansour, S.; Mortada, N.D.; Geneidi, A.S.; Guy, R.H. Microemulsion formulations for the transdermal delivery of testosterone. Eur. J. Pharm. Sci. 2010, 40, 188–196. [Google Scholar] [CrossRef] [Green Version]
- Santos, P.; Watkinson, A.C.; Hadgraft, J.; Lane, M.E. Application of microemulsions in dermal and transdermal drug delivery. Skin Pharmacol. Physiol. 2008, 21, 246–259. [Google Scholar] [CrossRef]
- Lawrence, M.; Warisnoicharoen, E. Recent Advances in Microemulsions as Drug Delivery Vehicles. In Nanoparticulates as Drug Carriers; Torchilin, V.P., Ed.; Imperial College Press: London, UK, 2006; pp. 125–172. [Google Scholar]
- Kumar, K.; Mittal, K.L. Handbook of Microemulsion Science and Technology; Marcel Dekker Inc.: New York, NY, USA, 1999. [Google Scholar]
- Russell-Jones, G.; Himes, R. Water-in-oil microemulsions for effective transdermal delivery of proteins. Expert Opin. Drug Deliv. 2011, 8, 537–546. [Google Scholar] [CrossRef]
- Kreilgaard, M. Influence of microemulsions on cutaneous drug delivery. Adv. Drug Deliv. Rev. 2002, 54, S77–S98. [Google Scholar] [CrossRef]
- Lindman, B.; Shinoda, K.; Olsson, U.; Andersson, D.; Karlstrom, G.; Wenner-Strom, H. On the demonstration of bicontinuous structures in microemulsions. Colloids Surf. 1989, 38, 205–224. [Google Scholar] [CrossRef]
- Hoar, T.P.; Schulman, J.H. Transparent water-in-oil dispersions: The oleophatic hydro-micelle. Nature 1943, 152, 102–103. [Google Scholar] [CrossRef]
- Heuschkel, S.; Goebel, A.; Neubert, R.H. Microemulsions—Modern colloidal carrier for dermal and transdermal drug delivery. J. Pharm. Sci. 2008, 97, 603–631. [Google Scholar] [CrossRef]
- McClements, D.J. Nanoemulsions versus microemulsions: Terminology, differences, and similarities. Soft Matter 2012, 8, 1719–1729. [Google Scholar] [CrossRef]
- Balogh, J.; Olsson, U.; Jan, S.P.; Kaper, H.; Wennerstrom, H.; Schillén, K.; Miguel, M. Non-Ionic Microemulsions: Dependence of Oil Chain Lenght and Active Component. In Self-Organized Surfactant Structure; Tadros, T.F., Ed.; Wiley-VCH: Weinheim, Germany, 2010. [Google Scholar]
- Tadros, T.F. Applied Surfactants; Wiley-VHC: Weinheim, Germany, 2005. [Google Scholar]
- Sjoblom, J.; Lindbergh, R.; Friberg, S. Microemulsions—Phase equilibria characterization, structures, applications and chemical reactions. Adv. Colloid Interface Sci. 1986, 95, 125–287. [Google Scholar]
- Kogan, A.; Aserin, A.; Garti, N. Improved solubilization of carbamazepine and structural transitions in nonionic microemulsions upon aqueous phase dilution. J. Colloid Interface Sci. 2007, 315, 637–647. [Google Scholar] [CrossRef]
- Malheiro, A.R.; Varanda, L.C.; Perez, J.; Villullas, H.M. The Aerosol OT + n-butanol + n-heptane + water system: Phase behavior, structure characterization, and application to Pt70Fe30 nanoparticle synthesis. Langmuir 2007, 23, 11015–11020. [Google Scholar]
- Cabaleiro-Lago, C.; Garcia-Rio, L.; Hervella, P. The effect of changing the microstructure of a microemulsion on chemical reactivity. Langmuir 2007, 23, 9586–9595. [Google Scholar] [CrossRef]
- Pepe, D.; Phelps, J.; Lewis, K.; Dujack, J.; Scarlett, K.; Jahan, S.; Bonnier, E.; Milic-Pasetto, T.; Hass, M.A.; Lopes, L.B. Decylglucoside-based microemulsions for cutaneous localization of lycopene and ascorbic acid. Int. J. Pharm. 2012, 434, 420–428. [Google Scholar] [CrossRef]
- El Maghraby, G.M. Transdermal delivery of hydrocortisone from eucalyptus oil microemulsion: Effects of cosurfactants. Int. J. Pharm. 2008, 355, 285–292. [Google Scholar] [CrossRef]
- Schwarz, J.; Weisspapir, M.; Friedman, D. Enhanced transdermal delivery of diazepam by submicron emulsion (sme) creams. Pharm. Res. 1995, 12, 687–692. [Google Scholar] [CrossRef]
- Friedman, D.; Schwarz, J.S.; Weisspapir, M. Submicron emulsion vehicle for enhanced transdermal delivery of steroidal and nonsteroidal antiinflammatory drugs. J. Pharm. Sci. 1995, 84, 324–329. [Google Scholar] [CrossRef]
- Shim, J.; Kim, M.J.; Kim, H.K.; Kim, D.H.; Oh, S.G.; Ko, S.Y.; Jang, H.G.; Kim, J.W. Morphological effect of lipid carriers on permeation of lidocaine hydrochloride through lipid membranes. Int. J. Pharm. 2010, 388, 251–256. [Google Scholar] [CrossRef]
- Baroli, B.; Lopez-Quintela, M.A.; Delgado-Charro, M.B.; Fadda, A.M.; Blanco-Mendez, J. Microemulsions for topical delivery of 8-methoxsalen. J. Control. Release 2000, 69, 209–218. [Google Scholar] [CrossRef]
- Chen, H.; Chang, X.; Weng, T.; Zhao, X.; Gao, Z.; Yang, Y.; Xu, H.; Yang, X. A study of microemulsion systems for transdermal delivery of triptolide. J. Control. Release 2004, 98, 427–436. [Google Scholar] [CrossRef]
- Biruss, B.; Kahlig, H.; Valenta, C. Evaluation of an eucalyptus oil containing topical drug delivery system for selected steroid hormones. Int. J. Pharm. 2007, 328, 142–151. [Google Scholar] [CrossRef]
- Lopes, L.B.; VanDeWall, H.; Li, H.T.; Venugopal, V.; Li, H.K.; Naydin, S.; Hosmer, J.; Levendusky, M.; Zheng, H.; Bentley, M.V.; et al. Topical delivery of lycopene using microemulsions: Enhanced skin penetration and tissue antioxidant activity. J. Pharm. Sci. 2010, 99, 1346–1357. [Google Scholar] [CrossRef]
- Hathout, R.M.; Mansour, S.; Mortada, N.D.; Geneidi, A.S.; Guy, R.H. Uptake of microemulsion components into the stratum corneum and their molecular effects on skin barrier function. Mol. Pharm. 2010, 7, 1266–1273. [Google Scholar] [CrossRef]
- Williams, A.C.; Barry, B.W. Penetration enhancers. Adv. Drug Deliv. Rev. 2004, 56, 603–618. [Google Scholar] [CrossRef]
- Gupta, R.R.; Jain, S.K.; Varshney, M. Aot water-in-oil microemulsions as a penetration enhancer in transdermal drug delivery of 5-fluorouracil. Colloids Surf. 2005, 41, 25–32. [Google Scholar] [CrossRef]
- Patzelt, A.; Lademann, J.; Richter, H.; Darvin, M.E.; Schanzer, S.; Thiede, G.; Sterry, W.; Vergou, T.; Hauser, M. In vivo investigations on the penetration of various oils and their influence on the skin barrier. Skin Res. Technol. 2012, 18, 364–369. [Google Scholar] [CrossRef]
- Dederen, J.C.; Chavan, B.; Rawlings, A.V. Emollients are more than sensory ingredients: The case of isostearyl isostearate. Int. J. Cosmet. Sci. 2012, 34, 502–510. [Google Scholar] [CrossRef]
- Fluhr, J.; Holleran, W.M.; Beradesca, E. Clinical Effects of Emollients on Skin. In Skin Moisturization; Leyden, J.J., Rwalings, A.V., Eds.; Marcel Dekker, Inc.: New York, NY, USA, 2005; pp. 220–242. [Google Scholar]
- Malcolmson, C.; Satra, C.; Kantaria, S.; Sidhu, A.; Lawrence, M.J. Effect of oil on the level of solubilization of testosterone propionate into nonionic oil-in-water microemulsions. J. Pharm. Sci. 1998, 87, 109–116. [Google Scholar] [CrossRef]
- Bolko, K.; Zvonar, A.; Gasperlin, M. Mixed lipid phase smedds as an innovative approach to enhance resveratrol solubility. Drug Dev. Ind. Pharm. 2014, 40, 102–109. [Google Scholar] [CrossRef]
- Land, L.M.; Li, P.; Bummer, P.M. Mass transport properties of progesterone and estradiol in model microemulsion formulations. Pharm. Res. 2006, 23, 2482–2490. [Google Scholar] [CrossRef]
- Rhee, Y.S.; Choi, J.G.; Park, E.S.; Chi, S.C. Transdermal delivery of ketoprofen using microemulsions. Int. J. Pharm. 2001, 228, 161–170. [Google Scholar] [CrossRef]
- Zhang, J.; Michniak-Kohn, B. Investigation of microemulsion microstructures and their relationship to transdermal permeation of model drugs: Ketoprofen, lidocaine, and caffeine. Int. J. Pharm. 2011, 421, 34–44. [Google Scholar] [CrossRef]
- Junyaprasert, V.B.; Boonme, P.; Songkro, S.; Krauel, K.; Rades, T. Transdermal delivery of hydrophobic and hydrophilic local anesthetics from O/W and W/O BRIJ 97-based microemulsions. J. Pharm. Pharm. Sci. 2007, 10, 288–298. [Google Scholar]
- Zhu, W.; Yu, A.; Wang, W.; Dong, R.; Wu, J.; Zhai, G. Formulation design of microemulsion for dermal delivery of penciclovir. Int. J. Pharm. 2008, 360, 184–190. [Google Scholar] [CrossRef]
- Kantarci, G.; Ozguney, I.; Karasulu, H.Y.; Arzik, S.; Guneri, T. Comparison of different water/oil microemulsions containing diclofenac sodium: Preparation, characterization, release rate, and skin irritation studies. AAPS PharmSciTech 2007, 8, E91. [Google Scholar] [CrossRef]
- Liu, C.H.; Chang, F.Y.; Hung, D.K. Terpene microemulsions for transdermal curcumin delivery: Effects of terpenes and cosurfactants. Colloids Surf. 2011, 82, 63–70. [Google Scholar] [CrossRef]
- Junyaprasert, V.B.; Boonme, P.; Wurster, D.E.; Rades, T. Aerosol OT microemulsions as carriers for transdermal delivery of hydrophobic and hydrophilic local anesthetics. Drug Deliv. 2008, 15, 323–330. [Google Scholar] [CrossRef]
- Liu, C.; Wu, J.; Shi, B.; Zhang, Y.; Gao, T.; Pei, Y. Enhancing the bioavailability of cyclosporine a using solid dispersion containing polyoxyethylene (40) stearate. Drug Dev. Ind. Pharm. 2006, 32, 115–123. [Google Scholar] [CrossRef]
- Shevachman, M.; Garti, N.; Shani, A.; Sintov, A.C. Enhanced percutaneous permeability of diclofenac using a new U-type dilutable microemulsion. Drug Dev. Ind. Pharm. 2008, 34, 403–412. [Google Scholar] [CrossRef]
- Biruss, B.; Valenta, C. The advantage of polymer addition to a non-ionic oil in water microemulsion for the dermal delivery of progesterone. Int. J. Pharm. 2008, 349, 269–273. [Google Scholar] [CrossRef]
- Pepe, D.; McCall, M.; Zheng, H.; Lopes, L.B. Protein transduction domain-containing microemulsions as cutaneous delivery systems for an anticancer agent. J. Pharm. Sci. 2013, 102, 1476–1487. [Google Scholar] [CrossRef]
- Huang, Y.B.; Lin, Y.H.; Lu, T.M.; Wang, R.J.; Tsai, Y.H.; Wu, P.C. Transdermal delivery of capsaicin derivative-sodium nonivamide acetate using microemulsions as vehicles. Int. J. Pharm. 2008, 349, 206–211. [Google Scholar] [CrossRef]
- Kamal, M.A.; Iimura, N.; Nabekura, T.; Kitagawa, S. Enhanced skin permeation of diclofenac by ion-pair formation and further enhancement by microemulsion. Chem. Pharm. Bull. 2007, 55, 368–371. [Google Scholar] [CrossRef]
- Peltola, S.; Saarinen-Savolainen, P.; Kiesvaara, J.; Suhonen, T.M.; Urtti, A. Microemulsions for topical delivery of estradiol. Int. J. Pharm. 2003, 254, 99–107. [Google Scholar] [CrossRef]
- Subramanian, N.; Ghosal, S.K.; Acharya, A.; Moulik, S.P. Formulation and physicochemical characterization of microemulsion system using isopropyl myristate, medium-chain glyceride, polysorbate 80 and water. Chem. Pharm. Bull. 2005, 53, 1530–1535. [Google Scholar] [CrossRef]
- Hua, L.; Weisan, P.; Jiayu, L.; Ying, Z. Preparation, evaluation, and NMR characterization of vinpocetine microemulsion for transdermal delivery. Drug Dev. Ind. Pharm. 2004, 30, 657–666. [Google Scholar] [CrossRef]
- Djordjevic, L.; Primorac, M.; Stupar, M.; Krajisnik, D. Characterization of caprylocaproyl macrogolglycerides based microemulsion drug delivery vehicles for an amphiphilic drug. Int. J. Pharm. 2004, 271, 11–19. [Google Scholar] [CrossRef]
- Jurkovic, P.; Sentjurc, M.; Gasperlin, M.; Kristl, J.; Pecar, S. Skin protection against ultraviolet induced free radicals with ascorbyl palmitate in microemulsions. Eur. J. Pharm. Biopharm. 2003, 56, 59–66. [Google Scholar] [CrossRef]
- Baboota, S.; Al-Azaki, A.; Kohli, K.; Ali, J.; Dixit, N.; Shakeel, F. Development and evaluation of a microemulsion formulation for transdermal delivery of terbinafine. PDA J. Pharm. Sci. Technol. 2007, 61, 276–285. [Google Scholar]
- Lee, J.; Lee, Y.; Kim, J.; Yoon, M.; Choi, Y.W. Formulation of microemulsion systems for transdermal delivery of aceclofenac. Arch. Pharm. Res. 2005, 28, 1097–1102. [Google Scholar] [CrossRef]
- Yuan, J.S.; Ansari, M.; Samaan, M.; Acosta, E.J. Linker-based lecithin microemulsions for transdermal delivery of lidocaine. Int. J. Pharm. 2008, 349, 130–143. [Google Scholar] [CrossRef]
- Changez, M.; Varshney, M.; Chander, J.; Dinda, A.K. Effect of the composition of lecithin/n-propanol/isopropyl myristate/water microemulsions on barrier properties of mice skin for transdermal permeation of tetracaine hydrochloride: In vitro. Colloids Surf. 2006, 50, 18–25. [Google Scholar] [CrossRef]
- Hoeller, S.; Klang, V.; Valenta, C. Skin-compatible lecithin drug delivery systems for fluconazole: Effect of phosphatidylethanolamine and oleic acid on skin permeation. J. Pharm. Pharmacol. 2008, 60, 587–591. [Google Scholar] [CrossRef]
- Sintov, A.C.; Shapiro, L. New microemulsion vehicle facilitates percutaneous penetration in vitro and cutaneous drug bioavailability in vivo. J. Control. Release 2004, 95, 173–183. [Google Scholar] [CrossRef]
- Suppasansatorn, P.; Nimmannit, U.; Conway, B.R.; Du, L.; Wang, Y. Microemulsions as topical delivery vehicles for the anti-melanoma prodrug, temozolomide hexyl ester (TMZA-HE). J. Pharm. Pharmacol. 2007, 59, 787–794. [Google Scholar] [CrossRef]
- Cichewicz, A.; Pacleb, C.; Connors, A.; Hass, M.A.; Lopes, L.B. Cutaneous delivery of α-tocopherol and lipoic acid using microemulsions: Influence of composition and charge. J. Pharm. Pharmacol. 2013, 65, 817–826. [Google Scholar] [CrossRef]
- Peira, E.; Carlotti, M.E.; Trotta, C.; Cavalli, R.; Trotta, M. Positively charged microemulsions for topical application. Int. J. Pharm. 2008, 346, 119–123. [Google Scholar] [CrossRef]
- El Meshad, A.N.; Tadros, M.I. Transdermal delivery of an anti-cancer drug via W/O emulsions based on alkyl polyglycosides and lecithin: Design, characterization, and in vivo evaluation of the possible irritation potential in rats. AAPS PharmSciTech 2011, 12, 1–9. [Google Scholar] [CrossRef]
- Djekic, L.; Primorac, M. The influence of cosurfactants and oils on the formation of pharmaceutical microemulsions based on PEG-8 caprylic/capric glycerides. Int. J. Pharm. 2008, 352, 231–239. [Google Scholar] [CrossRef]
- Hashem, F.M.; Shaker, D.S.; Ghorab, M.K.; Nasr, M.; Ismail, A. Formulation, characterization, and clinical evaluation of microemulsion containing clotrimazole for topical delivery. AAPS PharmSciTech 2011, 12, 879–886. [Google Scholar] [CrossRef]
- Hosmer, J.; Reed, R.; Bentley, M.V.; Nornoo, A.; Lopes, L.B. Microemulsions containing medium-chain glycerides as transdermal delivery systems for hydrophilic and hydrophobic drugs. AAPS PharmSciTech 2009, 10, 589–596. [Google Scholar] [CrossRef]
- Patel, N.; Schmid, U.; Lawrence, M.J. Phospholipid-based microemulsions suitable for use in foods. J. Agric. Food Chem. 2006, 54, 7817–7824. [Google Scholar] [CrossRef]
- Montenegro, L.; Carbone, C.; Puglisi, G. Vehicle effects onin vitro release and skin permeation of octylmethoxycinnamate from microemulsions. Int. J. Pharm. 2011, 405, 162–168. [Google Scholar] [CrossRef]
- Yuan, J.S.; Yip, A.; Nguyen, N.; Chu, J.; Wen, X.Y.; Acosta, E.J. Effect of surfactant concentration on transdermal lidocaine delivery with linker microemulsions. Int. J. Pharm. 2010, 392, 274–284. [Google Scholar] [CrossRef]
- McCarley, K.D.; Bunge, A.L. Pharmacokinetic models of dermal absorption. J. Pharm. Sci. 2001, 90, 1699–1719. [Google Scholar] [CrossRef]
- Reddy, M.B.; McCarley, K.D.; Bunge, A.L. Physiologically relevant one-compartment pharmacokinetic models for skin. 2. Comparison of models when combined with a systemic pharmacokinetic model. J. Pharm. Sci. 1998, 87, 482–490. [Google Scholar] [CrossRef]
- Mitragotri, S.; Anissimov, Y.G.; Bunge, A.L.; Frasch, H.F.; Guy, R.H.; Hadgraft, J.; Kasting, G.B.; Lane, M.E.; Roberts, M.S. Mathematical models of skin permeability: An overview. Int. J. Pharm. 2011, 418, 115–129. [Google Scholar] [CrossRef] [Green Version]
- Anissimov, Y.G.; Jepps, O.G.; Dancik, Y.; Roberts, M.S. Mathematical and pharmacokinetic modelling of epidermal and dermal transport processes. Adv. Drug Deliv. Rev. 2013, 65, 169–190. [Google Scholar] [CrossRef]
- Singh, P.; Roberts, M.S. Effects of vasoconstriction on dermal pharmacokinetics and local tissue distribution of compounds. J. Pharm. Sci. 1994, 83, 783–791. [Google Scholar] [CrossRef]
- Al Abood, R.M.; Talegaonkar, S.; Tariq, M.; Ahmad, F.J. Microemulsion as a tool for the transdermal delivery of ondansetron for the treatment of chemotherapy induced nausea and vomiting. Colloids Surf. 2013, 101, 143–151. [Google Scholar] [CrossRef]
- Kogan, A.; Rozner, S.; Mehta, S.; Somasundaran, P.; Aserin, A.; Garti, N.; Ottaviani, M.F. Characterization of the nonionic microemulsions by EPR. I. Effect of solubilized drug on nanostructure. J. Phys. Chem. 2009, 113, 691–699. [Google Scholar]
- Garti, N.; Avrahami, M.; Aserin, A. Improved solubilization of celecoxib in U-type nonionic microemulsions and their structural transitions with progressive aqueous dilution. J. Colloid Interface Sci. 2006, 299, 352–365. [Google Scholar] [CrossRef]
- Alvarez-Lorenzo, C.; Gomez-Amoza, J.L.; Martinez-Pacheco, R.; Souto, C.; Concheiro, A. Microviscosity of hydroxypropylcellulose gels as a basis for prediction of drug diffusion rates. Int. J. Pharm. 1999, 180, 91–103. [Google Scholar] [CrossRef]
- Rojanasakul, Y.; Wang, L.Y.; Bhat, M.; Glover, D.D.; Malanga, C.J.; Ma, J.K. The transport barrier of epithelia: A comparative study on membrane permeability and charge selectivity in the rabbit. Pharm. Res. 1992, 9, 1029–1034. [Google Scholar] [CrossRef]
- Yilmaz, E.; Borchert, H.H. Design of a phytosphingosine-containing, positively-charged nanoemulsion as a colloidal carrier system for dermal application of ceramides. Eur. J. Pharm. Biopharm. 2005, 60, 91–98. [Google Scholar] [CrossRef]
- Hoeller, S.; Sperger, A.; Valenta, C. Lecithin based nanoemulsions: A comparative study of the influence of non-ionic surfactants and the cationic phytosphingosine on physicochemical behaviour and skin permeation. Int. J. Pharm. 2009, 370, 181–186. [Google Scholar] [CrossRef]
- Baspinar, Y.; Borchert, H.H. Penetration and release studies of positively and negatively charged nanoemulsions—Is there a benefit of the positive charge? Int. J. Pharm. 2012, 430, 247–252. [Google Scholar] [CrossRef]
- Zhou, H.; Yue, Y.; Liu, G.; Li, Y.; Zhang, J.; Gong, Q.; Yan, Z.; Duan, M. Preparation and characterization of a lecithin nanoemulsion as a topical delivery system. Nanoscale Res. Lett. 2009, 5, 224–230. [Google Scholar]
- Sahle, F.F.; Wohlrab, J.; Neubert, R.H.H. Controlled penetration of ceramides into and across the stratum corneum using various types of microemulsions and formulation associated toxicity studies. Eur. J. Pharm. Biopharm. 2013. [Google Scholar] [CrossRef]
- Izquierdo, P.; Wiechers, J.W.; Escribano, E.; Garcia-Celma, M.J.; Tadros, T.F.; Esquena, J.; Dederen, J.C.; Solans, C. A study on the influence of emulsion droplet size on the skin penetration of tetracaine. Skin Pharmacol. Physiol. 2007, 20, 263–270. [Google Scholar] [CrossRef]
- Valenta, C.; Schultz, K. Influence of carrageenan on the rheology and skin permeation of microemulsion formulations. J. Control. Release 2004, 95, 257–265. [Google Scholar] [CrossRef]
- Rozman, B.; Zvonar, A.; Falson, F.; Gasperlin, M. Temperature-sensitive microemulsion gel: An effective topical delivery system for simultaneous delivery of vitamins C and E. AAPS PharmSciTech 2009, 10, 54–61. [Google Scholar] [CrossRef]
- Araujo, L.M.; Thomazine, J.A.; Lopez, R.F. Development of microemulsions to topically deliver 5-aminolevulinic acid in photodynamic therapy. Eur. J. Pharm. Biopharm. 2010, 75, 48–55. [Google Scholar] [CrossRef]
- Delgado-Charro, M.B.; Iglesias-Vilas, G.; Blanco-Mendez, J.; Lopez-Quintela, M.A.; Marty, J.P.; Guy, R.H. Delivery of a hydrophobic solute through the skin from novel microemulsion systems. Eur. J. Pharm. Biopharm. 1997, 43, 37–42. [Google Scholar] [CrossRef]
- Naoui, W.; Bolzinger, M.A.; Fenet, B.; Pelletier, J.; Valour, J.P.; Kalfat, R.; Chevalier, Y. Microemulsion microstructure influences the skin delivery of an hydrophilic drug. Pharm. Res. 2011, 28, 1683–1695. [Google Scholar] [CrossRef]
- Lopes, L.B.; Lopes, J.L.; Oliveira, D.C.; Thomazini, J.A.; Garcia, M.T.; Fantini, M.C.; Collett, J.H.; Bentley, M.V. Liquid crystalline phases of monoolein and water for topical delivery of cyclosporin a: Characterization and study of in vitro and in vivo delivery. Eur. J. Pharm. Biopharm. 2006, 63, 146–155. [Google Scholar] [CrossRef]
- Lee, C.M.; Maibach, H.I. Deep percutaneous penetration into muscles and joints. J. Pharm. Sci. 2006, 95, 1405–1413. [Google Scholar] [CrossRef]
- Huang, C.T.; Tsai, M.J.; Lin, Y.H.; Fu, Y.S.; Huang, Y.B.; Tsai, Y.H.; Wu, P.C. Effect of microemulsions on transdermal delivery of citalopram: Optimization studies using mixture design and response surface methodology. Int. J. Nanomed. 2013, 8, 2295–2304. [Google Scholar]
- Tashtoush, B.M.; Bennamani, A.N.; Al-Taani, B.M. Preparation and characterization of microemulsion formulations of nicotinic acid and its prodrugs for transdermal delivery. Pharm. Dev. Technol. 2013, 18, 834–843. [Google Scholar] [CrossRef]
- Zhao, J.H.; Ji, L.; Wang, H.; Chen, Z.Q.; Zhang, Y.T.; Liu, Y.; Feng, N.P. Microemulsion-based novel transdermal delivery system of tetramethylpyrazine: Preparation and evaluation in vitro and in vivo. Int. J. Nanomed. 2011, 6, 1611–1619. [Google Scholar]
- Tsai, Y.H.; Chang, J.T.; Chang, J.S.; Huang, C.T.; Huang, Y.B.; Wu, P.C. The effect of component of microemulsions on transdermal delivery of buspirone hydrochloride. J. Pharm. Sci. 2011, 100, 2358–2365. [Google Scholar] [CrossRef]
- Elshafeey, A.H.; Kamel, A.O.; Fathallah, M.M. Utility of nanosized microemulsion for transdermal delivery of tolterodine tartrate: Ex vivo permeation and in vivo pharmacokinetic studies. Pharm. Res. 2009, 26, 2446–2453. [Google Scholar]
- Patel, P.A.; Patil, S.C.; Kalaria, D.R.; Kalia, Y.N.; Patravale, V.B. Comparative in vitro and in vivo evaluation of lipid based nanocarriers of huperzine A. Int. J. Pharm. 2013, 446, 16–23. [Google Scholar] [CrossRef]
- Yuan, Y.; Li, S.M.; Mo, F.K.; Zhong, D.F. Investigation of microemulsion system for transdermal delivery of meloxicam. Int. J. Pharm. 2006, 321, 117–123. [Google Scholar] [CrossRef]
- Fouad, S.A.; Basalious, E.B.; El-Nabarawi, M.A.; Tayel, S.A. Microemulsion and poloxamer microemulsion-based gel for sustained transdermal delivery of diclofenac epolamine using in-skin drug depot: In vitro/in vivo evaluation. Int. J. Pharm. 2013, 453, 569–578. [Google Scholar] [CrossRef]
- Hathout, R.M.; Elshafeey, A.H. Development and characterization of colloidal soft nano-carriers for transdermal delivery and bioavailability enhancement of an angiotensin II receptor blocker. Eur. J. Pharm. Biopharm. 2012, 82, 230–240. [Google Scholar] [CrossRef]
- Bhatia, G.; Zhou, Y.; Banga, A.K. Adapalene microemulsion for transfollicular drug delivery. J. Pharm. Sci. 2013, 102, 2622–2631. [Google Scholar] [CrossRef]
- Hathout, R.M.; Nasr, M. Transdermal delivery of betahistine hydrochloride using microemulsions: Physical characterization, biophysical assessment, confocal imaging and permeation studies. Colloids Surf. 2013, 110, 254–260. [Google Scholar] [CrossRef]
- Pakpayat, N.; Nielloud, F.; Fortune, R.; Tourne-Peteilh, C.; Villareal, A.; Grillo, I.; Bataille, B. Formulation of ascorbic acid microemulsions with alkyl polyglycosides. Eur. J. Pharm. Biopharm. 2009, 72, 444–452. [Google Scholar] [CrossRef]
- Carlotti, M.E.; Gallarate, M.; Rossatto, V. O/W microemulsion as a vehicle for sunscreens. J. Cosmet. Sci. 2003, 54, 451–462. [Google Scholar]
- Arevalo, M.I.; Escribano, E.; Calpena, A.; Domenech, J.; Queralt, J. Rapid skin anesthesia using a new topical amethocaine formulation: A preclinical study. Anesth. Analg. 2004, 98, 1407–1412. [Google Scholar]
- Escribano, E.; Obach, M.; Arevalo, M.I.; Calpena, A.C.; Domenech, J.; Queralt, J. Rapid human skin permeation and topical anaesthetic activity of a new amethocaine microemulsion. Skin Pharmacol. Physiol. 2005, 18, 294–300. [Google Scholar] [CrossRef]
- Liu, H.; Wang, Y.; Lang, Y.; Yao, H.; Dong, Y.; Li, S. Bicontinuous cyclosporin a loaded water-AOT/Tween 85-isopropylmyristate microemulsion: Structural characterization and dermal pharmacokinetics in vivo. J. Pharm. Sci. 2009, 98, 1167–1176. [Google Scholar] [CrossRef]
- Rangarajan, M.; Zatz, J.L. Effect of formulation on the topical delivery of alpha-tocopherol. J. Cosmet. Sci. 2003, 54, 161–174. [Google Scholar]
- Rozman, B.; Gasperlin, M.; Tinois-Tessoneaud, E.; Pirot, F.; Falson, F. Simultaneous absorption of vitamins C and E from topical microemulsions using reconstructed human epidermis as a skin model. Eur. J. Pharm. Biopharm. 2009, 72, 69–75. [Google Scholar] [CrossRef]
- Getie, M.; Wohlrab, J.; Neubert, R.H. Dermal delivery of desmopressin acetate using colloidal carrier systems. J. Pharm. Pharmacol. 2005, 57, 423–427. [Google Scholar] [CrossRef]
- Rossetti, F.C.; Lopes, L.B.; Carollo, A.R.; Thomazini, J.A.; Tedesco, A.C.; Bentley, M.V. A delivery system to avoid self-aggregation and to improve in vitro and in vivo skin delivery of a phthalocyanine derivative used in the photodynamic therapy. J. Control. Release 2011, 155, 400–408. [Google Scholar] [CrossRef]
- Goebel, A.S.; Knie, U.; Abels, C.; Wohlrab, J.; Neubert, R.H. Dermal targeting using colloidal carrier systems with linoleic acid. Eur. J. Pharm. Biopharm. 2010, 75, 162–172. [Google Scholar] [CrossRef]
- Draelos, Z.D.; DiNardo, J.C. A re-evaluation of the comedogenicity concept. J. Am. Acad. Dermatol. 2006, 54, 507–512. [Google Scholar] [CrossRef]
- Fulton, J.E. Comedogenicity and irritancy of commonly used ingredients in skin care products. J. Soc. Cosmet. Chem. 1989, 40, 321–333. [Google Scholar]
- Nguyen, S.H.; Dang, T.P.; Maibach, H.I. Comedogenicity in rabbit: Some cosmetic ingredients/vehicles. Cutan. Ocul. Toxicol 2007, 26, 287–292. [Google Scholar] [CrossRef]
- Savic, S.; Savic, M.; Tamburic, S.; Vuleta, G.; Vesic, S.; Muller-Goymann, C.C. An alkyl polyglucoside surfactant as a prospective pharmaceutical excipient for topical formulations: The influence of oil polarity on the colloidal structure and hydrocortisone in vitro/in vivo permeation. Eur. J. Pharm. Sci. 2007, 30, 441–450. [Google Scholar] [CrossRef]
- Karande, P.; Jain, A.; Mitragotri, S. Insights into synergistic interactions in binary mixtures of chemical permeation enhancers for transdermal drug delivery. J. Control. Release 2006, 115, 85–93. [Google Scholar] [CrossRef]
- Newby, C.S.; Barr, R.M.; Greaves, M.W.; Mallet, A.I. Cytokine release and cytotoxicity in human keratinocytes and fibroblasts induced by phenols and sodium dodecyl sulfate. J. Invest. Dermatol. 2000, 115, 292–298. [Google Scholar] [CrossRef]
- Kandárová, H.; Hayden, P.; Klausner, M.; Kubilus, J.; Sheasgreen, J. An in vitro skin irritation test (SIT) using the epiderm reconstructed human epidermal (RHE) model. J. Vis. Exp. 2009. [Google Scholar] [CrossRef]
- Mehling, A.; Kleber, M.; Hensen, H. Comparative studies on the ocular and dermal irritation potential of surfactants. Food Chem. Toxicol. 2007, 45, 747–758. [Google Scholar] [CrossRef]
- Basketter, D.A.; Chamberlain, M.; Griffiths, H.A.; Rowson, M.; Whittle, E.; York, M. The classification of skin irritants by human patch test. Food Chem. Toxicol. 1997, 35, 845–852. [Google Scholar] [CrossRef]
- Savic, S.; Weber, C.; Savic, M.M.; Muller-Goymann, C. Natural surfactant-based topical vehicles for two model drugs: Influence of different lipophilic excipients on in vitro/in vivo skin performance. Int. J. Pharm. 2009, 381, 220–230. [Google Scholar] [CrossRef]
- Moniruzzaman, M.; Tamura, M.; Tahara, Y.; Kamiya, N.; Goto, M. Ionic liquid-in-oil microemulsion as a potential carrier of sparingly soluble drug: Characterization and cytotoxicity evaluation. Int. J. Pharm. 2010, 400, 243–250. [Google Scholar] [CrossRef]
- Ayehunie, S.; Cannon, C.; Lamore, S.; Kubilus, J.; Anderson, D.J.; Pudney, J.; Klausner, M. Organotypic human vaginal-ectocervical tissue model for irritation studies of spermicides, microbicides, and feminine-care products. Toxicol. In Vitro 2006, 20, 689–698. [Google Scholar] [CrossRef]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Lopes, L.B. Overcoming the Cutaneous Barrier with Microemulsions. Pharmaceutics 2014, 6, 52-77. https://doi.org/10.3390/pharmaceutics6010052
Lopes LB. Overcoming the Cutaneous Barrier with Microemulsions. Pharmaceutics. 2014; 6(1):52-77. https://doi.org/10.3390/pharmaceutics6010052
Chicago/Turabian StyleLopes, Luciana B. 2014. "Overcoming the Cutaneous Barrier with Microemulsions" Pharmaceutics 6, no. 1: 52-77. https://doi.org/10.3390/pharmaceutics6010052





