Journal Description
Société Internationale d’Urologie Journal
Société Internationale d’Urologie Journal
(SIUJ) is an international, peer-reviewed, open access journal that covers all aspects of urology and related fields. The journal is owned by the Société Internationale d’Urologie (SIU) and is published bimonthly online by MDPI (since Volume 5, Issue 1 - 2024).
- Open Access— free for readers and authors (diamond open access), with article processing charges (APC) paid by the Société Internationale d’Urologie.
- Rapid Publication: first decisions in 16 days; acceptance to publication in 5.8 days (median values for MDPI journals in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
subject
Imprint Information
Open Access
ISSN: 2563-6499
Latest Articles
Publishing Urologic Research from Low- and Middle-Income Countries
Soc. Int. Urol. J. 2024, 5(3), 225-226; https://doi.org/10.3390/siuj5030033 (registering DOI) - 16 Jun 2024
Abstract
Global reach is a key component of the mission of the SIUJ [...]
Full article
Open AccessArticle
The Role of Artificial Intelligence in Patient Education: A Bladder Cancer Consultation with ChatGPT
by
Allen Ao Guo, Basil Razi, Paul Kim, Ashan Canagasingham, Justin Vass, Venu Chalasani, Krishan Rasiah and Amanda Chung
Soc. Int. Urol. J. 2024, 5(3), 214-224; https://doi.org/10.3390/siuj5030032 - 14 Jun 2024
Abstract
►▼
Show Figures
Objectives: ChatGPT is a large language model that is able to generate human-like text. The aim of this study was to evaluate ChatGPT as a potential supplement to urological clinical practice by exploring its capacity, efficacy and accuracy when delivering information on frequently
[...] Read more.
Objectives: ChatGPT is a large language model that is able to generate human-like text. The aim of this study was to evaluate ChatGPT as a potential supplement to urological clinical practice by exploring its capacity, efficacy and accuracy when delivering information on frequently asked questions from patients with bladder cancer. Methods: We proposed 10 hypothetical questions to ChatGPT to simulate a doctor–patient consultation for patients recently diagnosed with bladder cancer. The responses were then assessed using two predefined scales of accuracy and completeness by Specialist Urologists. Results: ChatGPT provided coherent answers that were concise and easily comprehensible. Overall, mean accuracy scores for the 10 questions ranged from 3.7 to 6.0, with a median of 5.0. Mean completeness scores ranged from 1.3 to 2.3, with a median of 1.8. ChatGPT was also cognizant of its own limitations and recommended all patients should adhere closely to medical advice dispensed by their healthcare provider. Conclusions: This study provides further insight into the role of ChatGPT as an adjunct consultation tool for answering frequently asked questions from patients with bladder cancer diagnosis. Whilst it was able to provide information in a concise and coherent manner, there were concerns regarding the completeness of information conveyed. Further development and research into this rapidly evolving tool are required to ascertain the potential impacts of AI models such as ChatGPT in urology and the broader healthcare landscape.
Full article

Figure 1
Open AccessArticle
Perioperative Blood Transfusion Is Associated with Worse Survival in Patients Undergoing Radical Cystectomy after Neoadjuvant Chemotherapy for Muscle-Invasive Bladder Cancer
by
Tessa Ladner, Anna J. Black, Homayoun Zargar, Jonathan L. Wright, Andrew C. Thorpe, Todd M. Morgan, Jeff M. Holzbeierlein, Michael S. Cookson, Niels-Erik Jacobsen, Adrian S. Fairey, Colin P. N. Dinney, Maria C. Mir, Laura-Maria Krabbe, Jeffrey S. Montgomery, Nikhil Vasdev, Evan Y. Yu, Evanguelos Xylinas, Andrew J. Stephenson, Jay B. Shah, Siamak Daneshmand, Kamran Zargar-Shoshtari, Philippe E. Spiess, Laura S. Mertens, Bas W. G. van Rhijn, Petros Grivas, Wassim Kassouf, Marc A. Dall’Era, Srikala S. Sridhar, Jonathan S. McGrath, Jonathan Aning, Shahrokh F. Shariat, Trinity J. Bivalacqua, Scott A. North, Daniel A. Barocas, Yair Lotan and Peter C. Blackadd
Show full author list
remove
Hide full author list
Soc. Int. Urol. J. 2024, 5(3), 202-213; https://doi.org/10.3390/siuj5030031 - 14 Jun 2024
Abstract
►▼
Show Figures
Objectives: Perioperative blood transfusion (PBT) has been associated with worse survival after radical cystectomy (RC) in patients with muscle-invasive bladder cancer (MIBC). Here, we evaluated the association between PBT and survival after RC that was preceded by neoadjuvant chemotherapy (NAC). Methods: A retrospective
[...] Read more.
Objectives: Perioperative blood transfusion (PBT) has been associated with worse survival after radical cystectomy (RC) in patients with muscle-invasive bladder cancer (MIBC). Here, we evaluated the association between PBT and survival after RC that was preceded by neoadjuvant chemotherapy (NAC). Methods: A retrospective analysis was performed on 949 patients with cT2-4aN0M0 bladder cancer who received NAC prior to RC between 2000 and 2013 at 19 centers. Kaplan–Meier estimates of overall survival (OS) were made. Presumed risk factors for OS were analyzed using Cox regression analysis. PBT was defined by the administration of any packed red blood cells during surgery or during the post-operative hospital stay. Results: A transfusion was given to 608 patients (64%). Transfused patients were more likely to have adverse clinical and pathologic parameters, including clinical stage and performance status. Transfused patients had worse OS (p = 0.01). On multivariable Cox regression, PBT was found to be independently associated with worse OS (HR 1.53 (95% CI 1.13–2.08), p = 0.007). Conclusions: PBT is common after NAC and RC, which may be linked, in part, to the anemia induced by NAC. PBT was associated with several adverse risk factors that correlate with poor outcomes after NAC and RC, and it was an independent predictor of adverse OS on multivariable analysis. Further study should determine if measures to avoid blood loss can reduce the need for PBT and thereby improve patient outcomes.
Full article

Figure 1
Open AccessCommentary
RE: Prevalence of MRI Lesions in Men Responding to a GP-Led Invitation for a Prostate Health Check: A Prospective Cohort Study
by
Alice Thomson, Haidar Al Saffar, Marlon Perera and Declan G. Murphy
Soc. Int. Urol. J. 2024, 5(3), 200-201; https://doi.org/10.3390/siuj5030030 - 10 Jun 2024
Abstract
Controversy surrounds population-based screening for prostate cancer, which has typically relied on PSA level for risk stratification. This commentary examines the recent prospective trial examining the use of biphasic prostate MRI scans as a screening tool for prostate cancer. Using a reliable test,
[...] Read more.
Controversy surrounds population-based screening for prostate cancer, which has typically relied on PSA level for risk stratification. This commentary examines the recent prospective trial examining the use of biphasic prostate MRI scans as a screening tool for prostate cancer. Using a reliable test, such as MRI prostate, at an earlier point along the diagnostic pathway, the authors provide a novel solution to a difficult problem. Further research is warranted to assess how biphasic MRI might be feasible at a population level.
Full article
Open AccessArticle
Quality and Readability of Google Search Information on HoLEP for Benign Prostate Hyperplasia
by
Yam Ting Ho, Jeremy Saad, Femi E. Ayeni, Sachinka Ranasinghe, Mohan Arianayagam, Bertram Canagasingham, Ahmed Goolam, Nicola Jeffery, Mohamed Khadra, Raymond Ko, Nicholas Mehan, Celi Varol, Jonathan Kam and Isaac A. Thangasamy
Soc. Int. Urol. J. 2024, 5(3), 192-199; https://doi.org/10.3390/siuj5030029 - 5 Jun 2024
Abstract
Objective: To assess the quality and readability of online information on holmium laser enucleation of the prostate in managing benign prostate hyperplasia using the most-used search engine worldwide, Google. Methods: Google search terms “Holmium laser surgery” and “enlarged prostate” were used
[...] Read more.
Objective: To assess the quality and readability of online information on holmium laser enucleation of the prostate in managing benign prostate hyperplasia using the most-used search engine worldwide, Google. Methods: Google search terms “Holmium laser surgery” and “enlarged prostate” were used to generate 150 search results. Two independent authors (i) excluded any paywall, scientific literature, or advertisement and (ii) conducted an independent assessment on information quality, which was based on DISCERN, QUEST, and JAMA criteria, and readability, which was based on the FKG, GFI, SMOG, and FRE scores on qualified webpages. A third author was involved if there were any discrepancies between the assessments. Results: 107 qualified webpages were included in the data analysis. The median DISCERN score was 42 out of 80 (IQR 35–49). The median JAMA score was 0 out of 4 (IQR 0–1). The median QUEST score was 9 out of 28 (IQR 9–12). Using the non-parametric ANOVA and post hoc Games–Howell test, significant differences were identified between rankings of webpages. Sponsorship had no influence on the quality of webpages. The overall readability level required a minimum reading level of grade 11. Linear regression analysis showed that a higher ranked webpage is a positive predictor for all three quality assessment tools. Conclusions: The overall quality of online information on HoLEP is poor. We identify that the top-ranked google searches have a higher DISCERN score and are a positive predictor for DISCERN/QUEST/JAMA. Quality online information can benefit patients but should be used in conjunction with professional medical consultation.
Full article
Open AccessArticle
A Quality and Completeness Assessment of Testicular Cancer Health Information on TikTok
by
Hoi Pong Nicholas Wong, Lee Jing Yang, Vikneshwaren SO Senthamil Selvan, Jamie Yong Qi Lim, Wei Zheng So, Vineet Gauhar and Ho Yee Tiong
Soc. Int. Urol. J. 2024, 5(3), 182-191; https://doi.org/10.3390/siuj5030028 - 5 Jun 2024
Abstract
TikTok has become a hub for easily accessible medical information. However, the quality and completeness of this information for testicular cancer has not been examined. Our study aims to assess the quality and completeness of testicular cancer information on TikTok. A search was
[...] Read more.
TikTok has become a hub for easily accessible medical information. However, the quality and completeness of this information for testicular cancer has not been examined. Our study aims to assess the quality and completeness of testicular cancer information on TikTok. A search was performed on TikTok using the search terms “Testicular Cancer” and “Testicle Cancer”. Inclusion criteria encompassed videos about testicular cancer in English. We excluded non-English videos, irrelevant videos, and videos without audio. We evaluated these videos using the DISCERN instrument and a completeness assessment. A total of 361 videos were considered for screening and 116 videos were included. Of these, 57 were created by healthcare professionals (HCPs). The median video length was 40 s (5–277 s), with >25 million cumulative views and a median of 446,400 views per video. The average DISCERN score was 29.0 ± 5.7, with HCPs providing higher-quality videos than non-HCPs (30.8 vs. 5.5, p < 0.05). HCPs also had more reliable videos (21.2 vs. 18.1, p < 0.05). Overall quality levels were mostly poor or very poor (97.4%), with none being good or excellent. Most HCP videos were poor (63.2%), whilst many non-HCP videos were very poor (61.0%). The most viewed video had 2,800,000 views but scored a 31 on the DISCERN tool and one on the completeness assessment. The highest DISCERN score had 11,700 views. HCP videos better defined the disease and were more complete (p < 0.05). Most videos discussed self-assessment but were lacking in definitions, risk factors, symptoms, evaluation, management, and outcomes. Most of TikTok’s testicular cancer information lacks quality and completeness, whilst higher-quality videos have limited reach.
Full article
Open AccessArticle
Prevalence of Genetic Mutations in Patients with Metastatic Prostate Cancer in a Cohort of Mexican Patients
by
Orión Erenhú Rodríguez González, Edgar Iván Bravo Castro, Jesus Eduardo Osorio, Habiram Pacheco Guerrero, Brenda Suaste Carmona, Luis David Arreola Peralta, Noe Esaul Martinez Juárez, Juan Samuel Izquierdo Luna, José de Jesús Oswaldo Islas García, Omar Dimas Victorio Vargas, Rafael Alberto Valdez Flores, Jesús Javier Torres Gómez and José Gadú Campos Salcedo
Soc. Int. Urol. J. 2024, 5(3), 172-181; https://doi.org/10.3390/siuj5030027 - 5 Jun 2024
Abstract
Background: Prostate cancer is a malignant neoplasm of the male genitourinary system with the highest incidence worldwide. Susceptibility genes related to aggressiveness and prognosis, such as BRCA1/2, ATM, PTEN, have been identified. Currently, reports related to germline mutations in patients with prostate cancer
[...] Read more.
Background: Prostate cancer is a malignant neoplasm of the male genitourinary system with the highest incidence worldwide. Susceptibility genes related to aggressiveness and prognosis, such as BRCA1/2, ATM, PTEN, have been identified. Currently, reports related to germline mutations in patients with prostate cancer in Latin American populations are very limited or absent. In the Mexican population, reports are also limited, especially in the context of metastatic prostate cancer. Determining the prevalence of these mutations is relevant to predict the potential aggressiveness of tumors and allow the use of targeted therapies, such as PARPi inhibitors. Objective: Determine the prevalence of germline mutations in patients with metastatic prostate cancer and establish their clinical characteristics at diagnosis. Material and Methods: Sixty-nine patients with metastatic PCa underwent testing and genetic analysis using the Comprehensive Multi-Cancer Hereditary Cancer Panel. The prevalence of germline mutations was assessed, and the cohort was divided into two groups for the evaluation and analysis of clinical characteristics between the mutated and non-mutated populations. Results: We identified mutations in 15 out of 69 patients (21.73%), while 54 patients (78.26%) had no mutations. Pathogenic mutations were observed in 15.9% of patients, Variants of Uncertain Significance (VUS) in 34.78%, and 5.79% had both. The most frequent mutations included ATM (11.54%), BRCA1 (11.54%), BRCA2 (7.69%), FANCA (7.69%), and FANCM (7.69%). No statistically significant differences were found in PSA levels, age at diagnosis, and resistance to castration between the two groups. Conclusions: Our study unveiled a mutation rate of 21.73%, marked by a significant prevalence of ATM, FANCA, FANCM, and Variants of Uncertain Significance (VUS). This pattern deviates from findings in other series, underscoring the necessity for improved access to clinical genetic testing in our population.
Full article
Open AccessInteresting Images
Arteriovenous Malformation of the Prostate Vasculature as a Cause of Torrential Bleeding during Transurethral Resection of the Prostate
by
Darshan Sitharthan, Athos Katelaris and Gordon O’Neill
Soc. Int. Urol. J. 2024, 5(3), 169-171; https://doi.org/10.3390/siuj5030026 - 5 Jun 2024
Abstract
►▼
Show Figures
An 82-year-old male experienced severe bleeding during transurethral resection of the prostate (TURP) due to an undetected prostatic arteriovenous malformation (AVM). Initial management with a catheter was followed by successful transarterial embolisation. This case highlights the effectiveness of endovascular angioembolisation for unexpected prostatic
[...] Read more.
An 82-year-old male experienced severe bleeding during transurethral resection of the prostate (TURP) due to an undetected prostatic arteriovenous malformation (AVM). Initial management with a catheter was followed by successful transarterial embolisation. This case highlights the effectiveness of endovascular angioembolisation for unexpected prostatic AVMs.
Full article

Figure 1
Open AccessArticle
Early Results after Thulium Laser Enucleation of the Prostate in Patients with Urodynamically Proven Detrusor Underactivity
by
Pawel Trotsenko, Christian Wetterauer, Martin Haydter, Lukas Lusuardi and Thomas R. W. Herrmann
Soc. Int. Urol. J. 2024, 5(3), 160-168; https://doi.org/10.3390/siuj5030025 - 3 Jun 2024
Abstract
Objectives: Benign prostatic hyperplasia is one of the most common urological diseases. Among these patients, the presence of detrusor underactivity or acontractility represents a challenging condition since no medical treatment is available. Our objective is to evaluate early term outcomes following transurethral
[...] Read more.
Objectives: Benign prostatic hyperplasia is one of the most common urological diseases. Among these patients, the presence of detrusor underactivity or acontractility represents a challenging condition since no medical treatment is available. Our objective is to evaluate early term outcomes following transurethral anatomical enucleation of the prostate with Tm:YAG support. Methods: In a retrospective analysis of 115 patients who underwent this procedure between January 2019 and March 2022 due to lower urinary tract symptoms, 8 patients with urodynamic evidence of detrusor underactivity secondary to a non-neurogenic aetiology were identified. Detrusor underactivity was defined as a bladder contractility index of <100. Results: Median age, prostate volume and bladder contractility index were 73.2 years, 78.5 cm3 and 63.9, respectively. Median International Prostate Symptom Score/quality of life, Qmax and post-void residual volume were 15/3.5 points, 4.4 mL/s and 189 mL, respectively. Postoperatively, immediate catheter-removal success rate was 87.5% (7/8), at 2 months all patients were catheter-free and remained so at 1-year follow-up. Significant improvements for quality of life, Qmax and post-void residual volume were detected. Median postoperative International Prostate Symptom Score/Quality of life, Qmax and post-void residual volume were 7/2, 21.6 mL/s and 0 mL, respectively. Conclusions: This surgical approach offers high catheter-free rates, significantly improves functional voiding parameters and increases patient satisfaction in patients with benign prostatic hyperplasia and concomitant detrusor underactivity. Therefore, it can be regarded as an effective approach for such patients.
Full article
Open AccessArticle
Protocol for the RoboSling Trial: A Randomised Study Assessing Urinary Continence Following Robotic Radical Prostatectomy with or without an Intraoperative Retropubic Vascularised Fascial Sling (RoboSling)
by
Amandeep Virk, Patrick-Julien Treacy, Wenjie Zhong, Stuart Robert Jackson, Nariman Ahmadi, Nicola Nadia Jeffery, Lewis Chan, Paul Sved, Arthur Vasilaras, Ruban Thanigasalam and Scott Leslie
Soc. Int. Urol. J. 2024, 5(2), 148-159; https://doi.org/10.3390/siuj5020024 - 17 Apr 2024
Abstract
►▼
Show Figures
Objectives: To determine if early (three months) and late (one year) post-operative continence is improved by performing a novel retropubic vascularised fascial sling (RoboSling) procedure concurrently with robot-assisted radical prostatectomy in men undergoing treatment for localised prostate cancer. To additionally assess surgical outcomes,
[...] Read more.
Objectives: To determine if early (three months) and late (one year) post-operative continence is improved by performing a novel retropubic vascularised fascial sling (RoboSling) procedure concurrently with robot-assisted radical prostatectomy in men undergoing treatment for localised prostate cancer. To additionally assess surgical outcomes, quality of life and health economic outcomes in patients undergoing the novel RoboSling technique. Methods: This study aims to recruit 120 consecutive patients with clinically localised prostate cancer who have chosen to undergo robot-assisted radical prostatectomy in the Sydney Local Health District, Australia. A prospective assessment of early and late post-operative continence following robot-assisted radical prostatectomy with and without a RoboSling procedure will be performed in a two-group, 1:1, parallel, randomized controlled trial. Four surgeons will take part in the study, all of whom are beyond their learning curve. Patients will be blinded as to whether the RoboSling procedure is performed for them, as will be the research officers collecting the post-operative data on urinary function. Trial Registration: ACTRN12618002058257. Results: The trial is currently underway. Conclusions: The RoboSling technique is unique in that the sling is vascularised and has a broad surface area compared to previously described slings in the literature. If a clinically significant improvement in post-operative continence is established with the RoboSling, then, we can in turn expect improvements in quality of life for men undergoing this technique with radical prostatectomy.
Full article
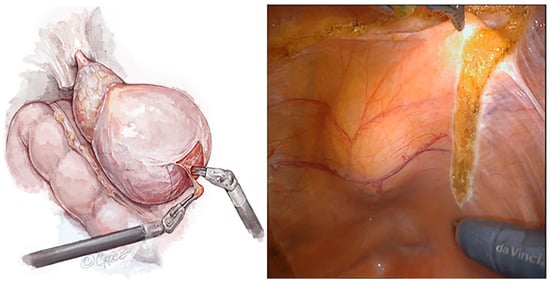
Figure 1
Open AccessUrology around the World
Robot-Assisted Surgery in Poland: The Past, the Present, and the Perspectives for the Future
by
Roman Sosnowski, Krzysztof Jakubiak, Hubert Kamecki, Grzegorz Kade, Tomasz Drewa, Tomasz Szydełko, Piotr Chłosta, Piotr Kania and Piotr Jarzemski
Soc. Int. Urol. J. 2024, 5(2), 142-147; https://doi.org/10.3390/siuj5020023 - 16 Apr 2024
Abstract
►▼
Show Figures
In recent decades, we have been witnessing a technological revolution in the area of minimally invasive urologic surgery, with robot-assisted surgery being one of the most game-changing inventions [...]
Full article
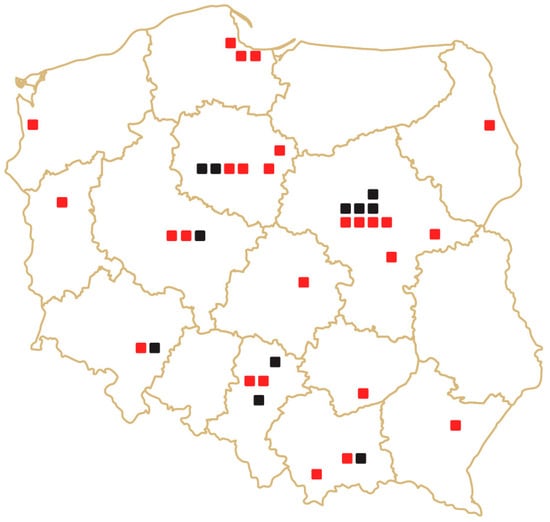
Figure 1
Open AccessSystematic Review
Systematic Review: Seventy-Seven Cases of Signet Ring Cell Adenocarcinoma of the Bladder
by
Kenneth Keen Yip Chew, Madison Boot, Katelyn Wilson, Cameron Sowter, Wei Xuan, Raymond Stanton and Paul Bergamin
Soc. Int. Urol. J. 2024, 5(2), 133-141; https://doi.org/10.3390/siuj5020022 - 16 Apr 2024
Abstract
►▼
Show Figures
Background: Signet ring cell adenocarcinoma (SRCC) of the bladder is a rare and aggressive histological subtype of bladder cancer. Due to its infrequency, the understanding of its clinical behaviour, treatment strategies, and outcomes remains limited, being primarily derived from isolated case reports
[...] Read more.
Background: Signet ring cell adenocarcinoma (SRCC) of the bladder is a rare and aggressive histological subtype of bladder cancer. Due to its infrequency, the understanding of its clinical behaviour, treatment strategies, and outcomes remains limited, being primarily derived from isolated case reports and series. Objective: To systematically review and analyse the available literature on SRCC of the bladder, emphasizing its clinical characteristics, diagnostic approaches, treatment modalities, and outcomes. Material and Methods: A comprehensive search was conducted across PubMed, Embase, and Medline following the PRISMA guidelines, including case reports, case series, observational studies, and clinical trials reporting on bladder SRCC. Results: We included 38 articles reporting on 77 patients, primarily males (79.2%), with a median age of 64 years. The most common presenting symptoms were haematuria (64.8%) and lower urinary tract symptoms (46.3%). All the diagnoses were based on histopathological examination of bladder tissue samples and immunohistochemistry. Mixed histological types of bladder cancer were found in 20.7% of cases, most commonly urothelial carcinoma (61.1%). The treatments varied, with 53.2% of patients undergoing radical cystectomy, 24.7% receiving radiotherapy, and 16.9% receiving chemotherapy. The five-year survival rates were 9.4%. Conclusion: Bladder SRCC presents aggressively, with varied treatment strategies; however, radical cystectomy appears to be the optimal means of surgical management for organ-confined disease. The overall survival rate is low, highlighting the need for further research to understand and manage this rare bladder cancer variant. All patients should undergo evaluation to exclude extravesical primaries. This systematic review contributes to a better understanding of this disease and may guide clinical management strategies.
Full article

Figure 1
Open AccessArticle
Role of Multiparametric Magnetic Resonance Imaging and Targeted Biopsy in the Detection of Clinically Significant Prostate Cancer in Patients with Suspicious Digital Rectal Examination
by
Vincenzo Ficarra, Alessandro Buttitta, Marta Rossanese, Angela Alibrandi, Giuseppina Anastasi, Alfredo Blandino, Antonio Ieni, Maurizio Martini and Gianluca Giannarini
Soc. Int. Urol. J. 2024, 5(2), 122-132; https://doi.org/10.3390/siuj5020021 - 16 Apr 2024
Abstract
►▼
Show Figures
Objectives: Few studies have examined the role of prostate MRI in patients with suspicious digital rectal examination (DRE) and/or PSA > 10 ng/mL. In a cohort of non-screened patients with suspicious DRE, we investigated the rate of avoidable prostate biopsies and potentially
[...] Read more.
Objectives: Few studies have examined the role of prostate MRI in patients with suspicious digital rectal examination (DRE) and/or PSA > 10 ng/mL. In a cohort of non-screened patients with suspicious DRE, we investigated the rate of avoidable prostate biopsies and potentially missed clinically significant prostate cancer (csPCa) with negative MRI, and the concordance between targeted biopsy (TBx) and systematic biopsy (SBx) in detecting csPCa with positive MRI. Methods: We retrospectively examined 199 biopsy-naïve patients with suspicious DRE who underwent prostate MRI before transperineal biopsy. Prostate Imaging—Reporting and Data System (PI-RADS) v2.1 ≥ 3 category of the index lesion defined a positive MRI. Combined TBx/SBx and SBx alone were performed for positive and negative MRI, respectively. An International Society of Urogenital Pathology Grade Group ≥ 2 defined csPCa. We calculated the csPCa detection rate of TBx, SBx, and combined TBx/SBx. The Cohen kappa statistic was used to measure the concordance between TBx and SBx. Results: Ninety-one (45.7%) csPCa cases were detected. MRI was positive in 153 (76.9%) patients. In the 46 patients with negative MRI, SBx detected 5 (10.9%) csPCa cases. Prostate biopsy could, thus, be avoided in 41/199 (20.6%) patients at the cost of missing 5/91 (5.5%) csPCa cases. The concordance between TBx and SBx in detecting csPCa with positive mpMRI was substantial (k = 0.70). Specifically, 6/86 (6.9%) csPCa cases were detected with TBx, and 17/86 (19.7%) with SBx alone. Concordance was almost perfect (k = 0.82) in patients with PSA > 10 ng/mL. Only 4/38 (10.5%) csPCa cases were missed by TBx, and only 1 (2.6%) csPCa case was identified by TBx alone. Conclusions: MRI in patients with suspicious DRE could avoid roughly 21% of unnecessary biopsies at the cost of missing approximately 6% of csPCa cases. Moreover, MRI and TBx complemented SBx in detecting csPCa in the subgroup with PSA > 10 ng/mL.
Full article

Figure 1
Open AccessArticle
Rectal Spacer Reduces Gastrointestinal Side Effects of Radiation Post Radical Prostatectomy
by
Anne Hong, Damien Bolton, Trung Pham, David Angus, David Pan, Daryl Lim Joon, Alwin Tan, Kevin McMillan, Yee Chan, Paul Manohar, Joe Thomas, Huong Ho, Peter Orio, Emily Holt, Margaret Cokelek, Nathan Lawrentschuk, Farshad Foroudi and Michael Chao
Soc. Int. Urol. J. 2024, 5(2), 111-121; https://doi.org/10.3390/siuj5020020 - 16 Apr 2024
Abstract
►▼
Show Figures
Objectives: Our objective was to assess the rate of complications and gastrointestinal adverse effects of rectal spacer insertion for salvage post prostatectomy radiation therapy. Methods: A retrospective observational study was performed. Between September 2018 and March 2022, 64 post-radical prostatectomy patients who were
[...] Read more.
Objectives: Our objective was to assess the rate of complications and gastrointestinal adverse effects of rectal spacer insertion for salvage post prostatectomy radiation therapy. Methods: A retrospective observational study was performed. Between September 2018 and March 2022, 64 post-radical prostatectomy patients who were planned for salvage radiation therapy received a rectal spacer. The selected patients were those who had nerve-sparing prostatectomy with intrafascial or interfascial dissections (where Denonvillier’s fascia is retained). Radiation dose to the rectal wall and gastrointestinal symptoms were assessed. Symptoms were graded using the National Cancer Center Institute Common Terminology Criteria for Adverse Events v4.0 grading scheme. A total of 39 patients had pre-spacer planning computer tomography (CT) scans, and the rectal dose before and after the spacer insertion was calculated. Comparisons were made using the Student’s t-test, with a p-value < 0.05 representing statistical significance. Finally, clinicians were surveyed to rate the ease of the procedure using a 5-point Likert scale of 1 to 5 (1: very difficult, 2: difficult, 3: moderate, 4: easy, 5: very easy). Results: A total of 64 patients successfully underwent rectal spacer insertion. The mean age was 64.4 years (standard deviation: 5.7 years). After a median of 14 months’ (range 6 to 35) follow up, acute grade 1 and above gastrointestinal (GI) toxicities were seen in 28% of patients (grade 2 in 1.5%), and late grade 1 and above GI toxicities were seen in 12% of patients (grade 2 in 1.5%). Amongst the 39 patients with pre-spacer planning CT images, the volume of the rectum receiving 60%, 70%, 80%, 90%, and 100% of the prescribed radiation dose was reduced by 25.9%, 34.2%, 35.4%, 43.7%, and 61.7%, respectively. All dose reductions were statistically significant. The procedure was rated as “easy” or “very easy” to perform in 56% of cases. Conclusions: The insertion of a rectal spacer in selected patients undergoing PPRT is feasible and safe and significantly improves rectal wall radiation dosimetry in salvage post prostatectomy radiation therapy. It was accomplished in >95% of patients, increasing vesico-rectal separation from ‘immediate vicinity’ to 11 mm without any post-operative complications in experienced hands. In addition, it achieved significant reduction in rectal radiation doses, leading to low rates of acute and late grade 2 toxicity.
Full article
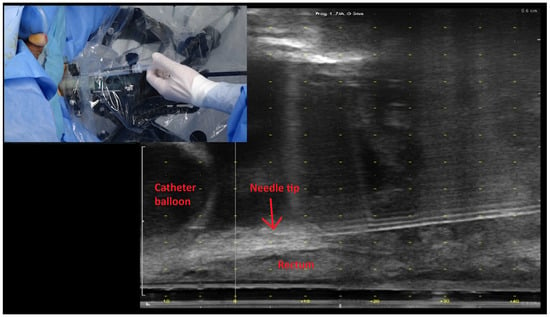
Figure 1
Open AccessGiants in Urology
Dr. Samuel Henry (Harry) Harris (22 August 1881 to 25 December 1936)
by
Darshan Sitharthan and Andrew Mitterdorfer
Soc. Int. Urol. J. 2024, 5(2), 108-110; https://doi.org/10.3390/siuj5020019 - 12 Apr 2024
Abstract
In the original article [...]
Full article
Open AccessCommunication
Can Artificial Intelligence Treat My Urinary Tract Infections?—Evaluation of Health Information Provided by OpenAI™ ChatGPT on Urinary Tract Infections
by
Kevin Yinkit Zhuo, Paul Kim, James Kovacic, Venu Chalasani, Krishan Rasiah, Stuart Menogue and Amanda Chung
Soc. Int. Urol. J. 2024, 5(2), 104-107; https://doi.org/10.3390/siuj5020018 - 11 Apr 2024
Abstract
Urinary tract infections (UTIs) are highly prevalent and have significant implications for patients. As internet-based health information becomes more relied upon, ChatGPT has emerged as a potential source of healthcare advice. In this study, ChatGPT-3.5 was subjected to 16 patient-like UTI queries, with
[...] Read more.
Urinary tract infections (UTIs) are highly prevalent and have significant implications for patients. As internet-based health information becomes more relied upon, ChatGPT has emerged as a potential source of healthcare advice. In this study, ChatGPT-3.5 was subjected to 16 patient-like UTI queries, with its responses evaluated by a panel of urologists. ChatGPT can address general UTI questions and exhibits some reasoning capacity in specific contexts. Nevertheless, it lacks source verification, occasionally overlooks vital information, and struggles with contextual clinical advice. ChatGPT holds promise as a supplementary tool in the urologist’s toolkit, demanding further refinement and validation for optimal integration.
Full article
Open AccessCommunication
Beware of Bipolar Transurethral Resection of Prostate in Patients with Previously Inserted Metallic Prostate Stapling Devices
by
Jianliang Liu, Nathan Lawrentschuk and Dixon T. S. Woon
Soc. Int. Urol. J. 2024, 5(2), 101-103; https://doi.org/10.3390/siuj5020017 - 10 Apr 2024
Abstract
►▼
Show Figures
Metallic prostate stapling (e.g., UroLift) is a minimally invasive treatment option for men with bladder outlet obstruction from benign prostatic hyperplasia (BPH). While it provides rapid relief and preserves sexual function, unexpected interactions with other medical devices can compromise surgical procedures. In this
[...] Read more.
Metallic prostate stapling (e.g., UroLift) is a minimally invasive treatment option for men with bladder outlet obstruction from benign prostatic hyperplasia (BPH). While it provides rapid relief and preserves sexual function, unexpected interactions with other medical devices can compromise surgical procedures. In this letter, we highlight five cases where stapled metallic implants resulted in damage to bipolar energy device during transurethral resection of the prostate (TURP) and stimulation of obturator nerve. Laser may also reflect off metallic prostate implants which can result in laser equipment malfunction. Monopolar TURP should be considered in patients with existing metallic prostate implants who need further transurethral surgery for obstructive BPH to prevent bipolar instrument damage and obturator kick.
Full article
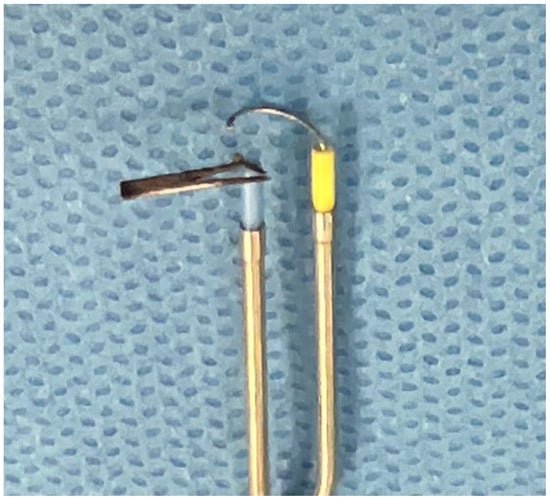
Figure 1
Open AccessCommentary
Smoking Cessation Tools in the Urological Context: Considering the Genitourinary Impacts of Smoking Cessation Tools
by
Nilanga Aki Bandara, Xuan Randy Zhou, Abdullah Alhamam, Peter C. Black and Marie-Pier St-Laurent
Soc. Int. Urol. J. 2024, 5(2), 97-100; https://doi.org/10.3390/siuj5020016 - 9 Apr 2024
Abstract
Electronic cigarette use is rising globally. Although it may represent a potential smoking cessation tool, amidst misinformation and social media promotion, there is a growing concern regarding the health risks associated with its usage. These risks include adverse effects on the genitourinary system.
[...] Read more.
Electronic cigarette use is rising globally. Although it may represent a potential smoking cessation tool, amidst misinformation and social media promotion, there is a growing concern regarding the health risks associated with its usage. These risks include adverse effects on the genitourinary system. This commentary investigates the genitourinary effects of approved smoking cessation tools versus electronic cigarettes, urging urologists to prioritize established methods over electronic cigarettes due to their potential for multisystem toxicity and uncertain long-term health implications. Further research is warranted to evaluate comprehensively the genitourinary effects of these interventions.
Full article
Open AccessInteresting Images
The “Spiked Helmet Sign”, a Mimic of ST-Elevation Myocardial Infarction in Post-Nephrectomy Ileus
by
Jessica Wynn, Jonathan McCafferty and Robert Forsyth
Soc. Int. Urol. J. 2024, 5(2), 93-96; https://doi.org/10.3390/siuj5020015 - 4 Apr 2024
Abstract
►▼
Show Figures
There are many causes of ST-elevation on electrocardiogram (ECG). ECG changes in the setting of intra-abdominal pathology is a rare and under characterised and includes the “spiked helmet sign”. We report a rare case of the “spiked helmet sign” that presented with ST-elevation
[...] Read more.
There are many causes of ST-elevation on electrocardiogram (ECG). ECG changes in the setting of intra-abdominal pathology is a rare and under characterised and includes the “spiked helmet sign”. We report a rare case of the “spiked helmet sign” that presented with ST-elevation in the precordial leads due to post-operative ileus.
Full article
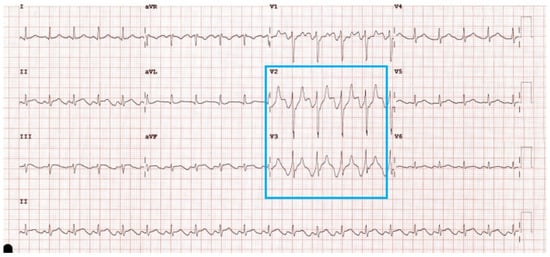
Figure 1
Open AccessArticle
Is the Bulbar Urethral Stricture a Single and Uniform Disease?
by
Tadashi Tabei, Akio Horiguchi, Masayuki Shinchi, Yusuke Hirano, Kenichiro Ojima, Keiichi Ito and Ryuichi Azuma
Soc. Int. Urol. J. 2024, 5(2), 85-92; https://doi.org/10.3390/siuj5020014 - 4 Apr 2024
Abstract
►▼
Show Figures
Objectives: Proximal and distal bulbar urethral strictures (BUS) have different disease characteristics and require different treatment strategies despite being regarded as a single condition. To clarify the differences, we analyzed our database by distinguishing the two types of BUS. Methods: We retrospectively reviewed
[...] Read more.
Objectives: Proximal and distal bulbar urethral strictures (BUS) have different disease characteristics and require different treatment strategies despite being regarded as a single condition. To clarify the differences, we analyzed our database by distinguishing the two types of BUS. Methods: We retrospectively reviewed the data of 196 patients with BUS who underwent urethroplasty at the National Defense Medical College (Japan) between August 2004 and March 2022. We divided patients into proximal (group 1) or distal (group 2) groups based on the stricture segment and compared patient background and surgical techniques for each group. We assessed whether the stricture segment was an independent predictive factor for substitution urethroplasty selection using multivariate logistic regression analysis. The recurrence rates were calculated and compared using the Kaplan–Meier method and log-rank test, respectively. Results: Patients in group 1 had a less frequent non-obliterated lumen (73% vs. 94%, p = 0.020) and significantly shorter strictures (10 mm vs. 23 mm, p < 0.001) more frequently caused by external traumas (47% vs. 26%, p = 0.010) than those in group 2. Logistic regression analysis revealed that the stricture segment (distal) (p < 0.001), stricture length (≥20 mm) (p < 0.001), ≥2 prior transurethral procedures (p = 0.030), and a non-obliterated lumen (p = 0.020) were independent predictive factors for substitution urethroplasty. However, the recurrence rate (p = 0.18) did not significantly differ between the two groups. Conclusions: Proximal and distal BUS have substantially different anatomical characteristics and etiologies and require different reconstructive techniques.
Full article
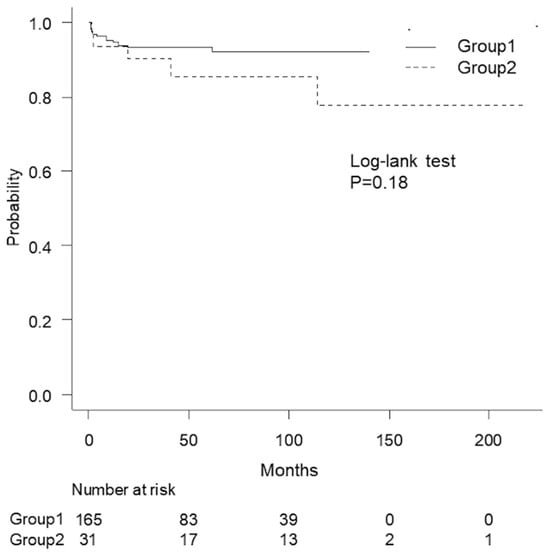
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics





