-
 Addressing the Shortage of GLP-1 RA and Dual GIP/GLP-1 RA-Based Therapies—A Systematic Review
Addressing the Shortage of GLP-1 RA and Dual GIP/GLP-1 RA-Based Therapies—A Systematic Review -
 The Intricate Relationship Between Thyroid Disorders and Type 2 Diabetes—A Narrative Review
The Intricate Relationship Between Thyroid Disorders and Type 2 Diabetes—A Narrative Review -
 Medication Adherence and Glycemic Control in Older Adults with Type 2 Diabetes: A Cross-Sectional Study in a Community Setting
Medication Adherence and Glycemic Control in Older Adults with Type 2 Diabetes: A Cross-Sectional Study in a Community Setting -
 The Relationship Between Quality of Life, Diabetes Distress, and Metabolic Control in Hungarian Type 1 Diabetic Patients: A Cross-Sectional Study
The Relationship Between Quality of Life, Diabetes Distress, and Metabolic Control in Hungarian Type 1 Diabetic Patients: A Cross-Sectional Study -
 The Role of Vitamin C in Wound Healing in Surgically Managed Diabetic Foot Disease
The Role of Vitamin C in Wound Healing in Surgically Managed Diabetic Foot Disease
Journal Description
Diabetology
Diabetology
is an international, peer-reviewed, open access journal on diabetes research published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), Scopus, EBSCO, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 24.4 days after submission; acceptance to publication is undertaken in 8.9 days (median values for papers published in this journal in the second half of 2025).
- Journal Rank: CiteScore - Q2 (Medicine (miscellaneous))
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
2.2 (2024);
5-Year Impact Factor:
2.5 (2024)
Latest Articles
Photodynamic Therapy as an Adjunctive Approach for Diabetic Foot Osteomyelitis: A Prospective Case Series
Diabetology 2026, 7(5), 88; https://doi.org/10.3390/diabetology7050088 - 2 May 2026
Abstract
Introduction: Type 2 diabetes mellitus predisposes patients to neuropathy, peripheral arterial disease, and diabetic foot ulcers, which may become infected and progress to osteomyelitis, increasing the risk of amputation. The growing prevalence of multidrug-resistant organisms complicates management. Photodynamic therapy (PDT), which combines a
[...] Read more.
Introduction: Type 2 diabetes mellitus predisposes patients to neuropathy, peripheral arterial disease, and diabetic foot ulcers, which may become infected and progress to osteomyelitis, increasing the risk of amputation. The growing prevalence of multidrug-resistant organisms complicates management. Photodynamic therapy (PDT), which combines a photosensitizer with light-emitting diode irradiation to generate reactive oxygen species, has emerged as a potential adjunctive antimicrobial strategy without inducing resistance. Objective: To describe clinical outcomes observed in patients with diabetic foot osteomyelitis treated with adjunctive photodynamic therapy (PDT), with emphasis on wound evolution, limb preservation, and healing time. Methods: This prospective case series included patients with osteomyelitis secondary to infected diabetic foot ulcers treated at a university hospital. Demographic and clinical data were collected from medical records. Serial photographic documentation was used to monitor wound progression and tissue response during therapy. Results: Sixteen patients with diabetic foot osteomyelitis were included. Complete healing was achieved in 13 patients (81.25%), while 2 patients (12.5%) remained under treatment with partial healing and 1 (6.25%) underwent major amputation. Among healed patients, healing time ranged from 19 to 546 days, with a median of 118 days. The number of photodynamic therapy sessions ranged from 2 to 12, depending on the clinical course of each case. Healing time varied among patients, and the hallux was the most frequent site of osteomyelitis. During follow-up, only one patient underwent major amputation, whereas the remaining patients either achieved complete healing or were still under treatment at the time of analysis. Healing time was comparable between insulin-dependent and non-insulin-dependent diabetes, although numerically shorter in the latter. Longer healing periods were associated with more treatment sessions. Conclusions: In this prospective uncontrolled case series, adjunctive PDT was associated with favorable clinical evolution in a subset of patients with diabetic foot osteomyelitis. However, because of the small sample size and the absence of a control group, these findings should be considered preliminary and hypothesis-generating.
Full article
(This article belongs to the Special Issue Advances in Diabetic Wound Healing: From Mechanisms to Therapies)
►
Show Figures
Open AccessArticle
Longitudinal Adherence Patterns of Oral Antidiabetics Among Older Adults with Diabetes and Concomitant Hypertension and Hyperlipidemia Using Group-Based Trajectory Modeling
by
Isaiah Olumeko, Sai S. Cheruvu, Samuel C. Ofili and Susan Abughosh
Diabetology 2026, 7(5), 87; https://doi.org/10.3390/diabetology7050087 - 2 May 2026
Abstract
Background/Objectives: Diabetes is a prevalent chronic condition and a major contributor to morbidity, mortality, and healthcare costs in the U.S., particularly among older adults with comorbidities such as hypertension and dyslipidemia. Complex medication regimens increase the risk of nonadherence, which can worsen
[...] Read more.
Background/Objectives: Diabetes is a prevalent chronic condition and a major contributor to morbidity, mortality, and healthcare costs in the U.S., particularly among older adults with comorbidities such as hypertension and dyslipidemia. Complex medication regimens increase the risk of nonadherence, which can worsen glycemic control, cardiovascular outcomes, and healthcare utilization. This study assessed longitudinal adherence patterns to oral antidiabetic medications among high-risk older adults and identified predictors using group-based trajectory modeling (GBTM). Methods: This retrospective cohort study used 2016–2017 Texas Medicare Advantage claims. Participants were older adults with diagnoses of diabetes, hypertension, and hyperlipidemia who had continuous plan coverage throughout the study period and at least one prescription fill for an oral antidiabetic, a statin, and a renin–angiotensin system (RAS) antagonist. Adherence was measured monthly over 12 months using the proportion of days covered (PDC). GBTM identified adherence trajectories, and multinomial logistic regression, based on the Andersen Behavioral Model, evaluated predictors using perfect adherence as the reference. Results: Among 7847 patients, three trajectories were observed: perfect adherence (59.50%), near-perfect adherence (29.21%), and rapid decline (11.29%). Female sex (OR, 1.38; 95% CI, 1.19–1.60) and absence of health plan subsidy (OR, 0.79; 95% CI, 0.68–0.92) were associated with rapid decline. Female sex (OR, 1.13; 95% CI, 1.02–1.25) and age ≥ 75 years (OR, 1.20; 95% CI, 1.00–1.43) were associated with near-perfect adherence. Conclusions: Older adults with diabetes and comorbidities exhibit distinct medication adherence patterns. Trajectory-based methods can identify those at risk for declining adherence and guide interventions to improve outcomes.
Full article
(This article belongs to the Special Issue Efficacy, Safety and Real-World Evidence of Hypoglycemic Drugs)
►▼
Show Figures

Figure 1
Open AccessArticle
Association of Social Determinants of Health with Primary and Cost-Related Medication Nonadherence Among Adult Patients with Diabetes
by
Yamini Mallisetty, Shruti Chaudhary, Ashley W. Ellis, Rushin Shah and Satya Surbhi
Diabetology 2026, 7(5), 86; https://doi.org/10.3390/diabetology7050086 - 2 May 2026
Abstract
Background/Objectives: To examine the association of social determinants of health (SDOHs) with primary and cost-related medication nonadherence among adults with diabetes. Methods: A retrospective cross-sectional analysis was conducted using 2021 data from the Medical Expenditure Panel Survey (MEPS), a nationally representative sample of
[...] Read more.
Background/Objectives: To examine the association of social determinants of health (SDOHs) with primary and cost-related medication nonadherence among adults with diabetes. Methods: A retrospective cross-sectional analysis was conducted using 2021 data from the Medical Expenditure Panel Survey (MEPS), a nationally representative sample of the United States civilian noninstitutionalized population. Adults aged ≥ 18 years with a diagnosis of diabetes in 2021 were included. The outcomes include primary medication nonadherence (no antidiabetic prescriptions filled) and cost-related medication nonadherence (delaying prescriptions due to cost). The exposure variables include SDOHs such as financial stress, food insecurity, transportation barriers, social support, access to medical care in the neighborhood, and healthcare discrimination. Weighted multivariable logistic regression analyses were conducted to assess the association between SDOHs and medication nonadherence. Results: Among 21.9 million patients with diabetes, 6.5% reported cost-related nonadherence and 17.4% exhibited primary nonadherence. Difficulty paying rent or mortgage (OR 2.32, 95% CI: 1.27–4.23), food insecurity (OR 2.13, 95% CI: 1.27–3.58), and transportation barriers (OR = 2.15; 95% CI: 1.20–3.63) were significantly associated with cost-related nonadherence. In the Medicare subgroup, both difficulty paying rent or mortgage (OR = 2.41, 95% CI: 1.03–5.64) and food insecurity (OR = 2.16, 95% CI: 1.18–3.96) significantly increased cost-related nonadherence. Conclusions: Financial strain, food insecurity, and transportation barriers are associated with cost-related nonadherence. These findings suggest considering social and economic factors in strategies supporting diabetes medication adherence across populations, including Medicare beneficiaries.
Full article
(This article belongs to the Special Issue Advances in Diabetes: Prevalence, Risk Factors, Complications, Costs and Disparities)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Waist Circumference and Handgrip Strength as Potential Nursing Vital Signs in Type 2 Diabetes: A Preliminary Assessment
by
Barbara Gómez-Taylor, Jorge Casaña Mohedo, Alma María Palau-Ferrè, Rocío Práxedes Gómez, Aáron Quesada Hernández, Ernesto Navarro Escobar, Elena Sandri and Sara Morales Palomares
Diabetology 2026, 7(5), 85; https://doi.org/10.3390/diabetology7050085 (registering DOI) - 1 May 2026
Abstract
►▼
Show Figures
Background and aims: The aim of this study was to examine the relationships between muscle function, dietary quality, body composition markers, and metabolic status in ambulatory patients with type 2 diabetes. The study sought to validate low-cost tools, such as handgrip strength
[...] Read more.
Background and aims: The aim of this study was to examine the relationships between muscle function, dietary quality, body composition markers, and metabolic status in ambulatory patients with type 2 diabetes. The study sought to validate low-cost tools, such as handgrip strength and waist circumference, as potential “nursing vital signs” for metabolic risk stratification. Methods: A cross-sectional observational study was conducted with adult patients with type 2 diabetes. Muscle function was assessed through handgrip strength (dynamometry) and metabolic status via the HOMA-IR index. Visceral adiposity was estimated using waist circumference and the Lipid Accumulation Product (LAP); dietary quality was evaluated with the Spanish Healthy Eating Index (IASE), and cellular health through the phase angle (PhA) obtained by electrical bioimpedance. Non-parametric tests and Spearman correlations were applied due to the non-normal distribution of the data. Conclusions: In this ambulatory diabetic population, waist circumference emerged as a practical and potent surrogate for insulin resistance burden. Although metabolic dysfunction was not directly associated with dietary quality or phase angle, a high prevalence of probable sarcopenia (36.1%) and poor dietary quality (77.8%) were detected. The implementation of non-invasive tools like waist circumference and handgrip strength in nursing consultations could optimize early risk stratification and allow for more targeted lifestyle interventions.
Full article

Graphical abstract
Open AccessReview
Mineralocorticoid Receptor Antagonism in Diabetic Kidney Disease: From Pathophysiological Mechanisms to Clinical Paradigm Shifts
by
Gui-Hwa Jeong
Diabetology 2026, 7(5), 84; https://doi.org/10.3390/diabetology7050084 - 1 May 2026
Abstract
Diabetic kidney disease (DKD) remains a primary driver of end-stage kidney disease and cardiovascular morbidity despite the optimized use of renin–angiotensin system (RAS) inhibitors and sodium-glucose cotransporter-2 (SGLT2) inhibitors. Recent evidence identifies the overactivation of the mineralocorticoid receptor (MR) as a critical, independent
[...] Read more.
Diabetic kidney disease (DKD) remains a primary driver of end-stage kidney disease and cardiovascular morbidity despite the optimized use of renin–angiotensin system (RAS) inhibitors and sodium-glucose cotransporter-2 (SGLT2) inhibitors. Recent evidence identifies the overactivation of the mineralocorticoid receptor (MR) as a critical, independent pathway leading to persistent renal inflammation and fibrosis. In the diabetic milieu, MR overactivation—driven by both aldosterone and ligand-independent factors such as Rac1 GTPase and oxidative stress—triggers pro-inflammatory and pro-fibrotic gene networks. Unlike traditional steroidal mineralocorticoid receptor antagonists (MRAs), the novel non-steroidal MRA finerenone exhibits a distinct binding mode that more effectively blocks the recruitment of transcriptional co-activators, thereby silencing detrimental downstream signaling in podocytes, fibroblasts, and myeloid cells. Preclinical models have demonstrated that MR blockade significantly reduces albuminuria and preserves podocyte integrity independent of systemic blood pressure. These findings translated into landmark clinical trials; the FIDELIO-DKD and FIGARO-DKD trials established that finerenone significantly reduces the risk of kidney disease progression and cardiovascular events across a broad spectrum of chronic kidney disease stages in type 2 diabetes. Furthermore, recent data from the FINEARTS-HF and CONFIDENCE trials suggest a synergetic benefit when combined with SGLT2 inhibitors, offering more robust cardiorenal protection with a manageable risk of hyperkalemia. This review synthesizes the current understanding of MR pathophysiology and clinical evidence, providing a comprehensive framework for the integration of MRAs into the evolving standard of care for patients with diabetic kidney disease.
Full article
(This article belongs to the Special Issue New Insights into the Diagnosis, Prevention and Treatment of Diabetic Complications)
►▼
Show Figures

Figure 1
Open AccessReview
Inhibition of SGLT1: The Alternative Way Toward Incretin Protection
by
Alessio Mazzieri and Livia Maria Rita Marcon
Diabetology 2026, 7(5), 83; https://doi.org/10.3390/diabetology7050083 - 28 Apr 2026
Abstract
Sodium glucose-1 cotransporter (SGLT1) is a low-capacity, high-affinity glucose transporter expressed in the proximal renal tubule. It is also expressed in different human tissues and, primarily, in the brush border of the small intestine. At this level, SGLT1 inhibition results in an increase
[...] Read more.
Sodium glucose-1 cotransporter (SGLT1) is a low-capacity, high-affinity glucose transporter expressed in the proximal renal tubule. It is also expressed in different human tissues and, primarily, in the brush border of the small intestine. At this level, SGLT1 inhibition results in an increase in glucose supply to the distal intestine with a reduction in intestinal pH and a consequent alteration of the intestinal microbiota. Specifically, SGLT1 inhibitors (SGLT1is) lead to an intensification of the production of short-chain fatty acids (SCFAs) and an enhancement of the incretin pathway. Potential mechanisms by which SGLT1is could reduce the occurrence of stroke and myocardial infarction may therefore involve the anti-inflammatory, anti-fibrotic and anti-atherosclerotic effects associated with an increased production of endogenous glucagon-like peptide-1 (GLP-1).
Full article
(This article belongs to the Special Issue Early Intervention and Treatment Strategies for Diabetes)
►▼
Show Figures

Figure 1
Open AccessArticle
Accelerometer-Measured Physical Activity and Its Association with Metabolic Markers of Type 2 Diabetes Mellitus: A Cross-Sectional NHANES Study
by
Sophia C. Bremer, Rodrigo D. Raimundo, Andrey A. Porto, David M. Garner, Luana P. Oliveira, Caroline S. Ferrari, Edilaine A. Nascimento, Sandra Maria Barbalho and Vitor E. Valenti
Diabetology 2026, 7(5), 82; https://doi.org/10.3390/diabetology7050082 - 24 Apr 2026
Abstract
►▼
Show Figures
Background: We aimed to study the association between accelerometer-measured physical activity and metabolic markers of diabetes in a nationwide representative sample of U.S. adults. Methods: This cross-sectional analysis included 1259 adults aged ≥18 years from the 2003–2004 National Health and Nutrition Examination Survey
[...] Read more.
Background: We aimed to study the association between accelerometer-measured physical activity and metabolic markers of diabetes in a nationwide representative sample of U.S. adults. Methods: This cross-sectional analysis included 1259 adults aged ≥18 years from the 2003–2004 National Health and Nutrition Examination Survey (NHANES), the only cycle incorporating objective accelerometry. Physical activity was assessed using hip-worn accelerometers, with moderate-to-vigorous physical activity (MVPA) and sedentary time derived from validated count thresholds. Metabolic outcomes included fasting glucose, fasting insulin, glycated hemoglobin (HbA1c), and insulin resistance estimated by the Homeostatic Model Assessment (HOMA-IR). Survey-weighted linear regression models accounting for the complex sampling design were applied, with sequential adjustment for demographic, socioeconomic, anthropometric, and behavioral covariates. Sensitivity analyses tested alternative MVPA thresholds and wear-time criteria. Results: In unadjusted models, higher MVPA was inversely linked with fasting glucose and insulin concentrations; but, these associations were attenuated after full multivariable adjustment. In contrast, MVPA established a constant inverse association with insulin resistance. Higher MVPA was connected with lower HOMA-IR values, and this relationship remained statistically significant in fully adjusted models and across all sensitivity analyses (all p < 0.001). Associations between sedentary time and metabolic markers were non-sustainable after multivariable adjustment. No significant effect modification by sex was detected. Conclusions: Objectively measured moderate-to-vigorous physical activity is independently linked with lower insulin resistance in U.S. adults. These results emphasize the value of accelerometer-based assessments for identifying early metabolic risk and reinforce physical activity promotion as a key strategy for improving insulin sensitivity.
Full article

Figure 1
Open AccessReview
QSAR Insights into Antidiabetic Activity of Natural Sulfur-Containing Compounds
by
Valery M. Dembitsky and Alexander O. Terent’ev
Diabetology 2026, 7(4), 81; https://doi.org/10.3390/diabetology7040081 - 20 Apr 2026
Abstract
►▼
Show Figures
Plants of the genus Salacia (Celastraceae) have long been used in traditional medical systems of South and Southeast Asia for the management of diabetes and related metabolic disorders. Modern phytochemical and pharmacological studies have confirmed the antidiabetic potential of several Salacia species, leading
[...] Read more.
Plants of the genus Salacia (Celastraceae) have long been used in traditional medical systems of South and Southeast Asia for the management of diabetes and related metabolic disorders. Modern phytochemical and pharmacological studies have confirmed the antidiabetic potential of several Salacia species, leading to the identification of a distinctive group of sulfur-containing sugars as their principal bioactive constituents. Salacinol, neosalacinol, kotalanol, neokotalanol, and related analogues represent a novel class of thiosugar sulfonium compounds that act as potent and selective α-glucosidase inhibitors, providing a clear mechanistic basis for their glucose-lowering effects. Simpler thiosugars, such as 5-thiomannose, further contribute to the overall metabolic activity of Salacia extracts and may serve as biosynthetic or functional precursors. Beyond Salacia, sulfur-containing natural products are widespread in nature and perform diverse biological roles. In particular, the genus Allium is well known for producing organosulfur compounds, including thioethers and polysulfides, which exhibit antidiabetic, hypolipidemic, antioxidant, and cardioprotective activities. In a different context, sulfur-containing hopanes have been identified in sediments and petroleum as products of early diagenetic sulfurization of bacterial hopanoids. Although these compounds have been studied primarily as geochemical biomarkers, recent QSAR/PASS analyses suggest that sulfur hopanes may also possess biologically relevant activities, particularly related to metabolic and cardiovascular regulation. Recent PASS-based QSAR evaluations of Salacia-derived thiosugars and sulfur hopanes predict significant antidiabetic activity, including potential type 2 diabetes-related pharmacological effects, supported by predicted α-glucosidase inhibitory, hypoglycemic, hepatic, and gastrointestinal activities. Collectively, these findings highlight sulfur-containing natural products from both plant and sedimentary sources as chemically diverse yet functionally convergent scaffolds with promising potential for the development of functional foods and therapeutic agents targeting metabolic disorders.
Full article

Graphical abstract
Open AccessArticle
A Thematic Analysis of Sleep Behavior Self-Regulation in Young Adults with Type 1 Diabetes
by
Madeline Long, Dayna A. Johnson, Youjeong Kang and Stephanie Alisha Griggs
Diabetology 2026, 7(4), 80; https://doi.org/10.3390/diabetology7040080 - 14 Apr 2026
Abstract
Background/Objectives: Sleep is critical for young adults, particularly those with type 1 diabetes (T1D), who face unique challenges in achieving recommended sleep and diabetes health targets. The purpose of this study guided by the theoretical framework of self-regulation theory is to explore
[...] Read more.
Background/Objectives: Sleep is critical for young adults, particularly those with type 1 diabetes (T1D), who face unique challenges in achieving recommended sleep and diabetes health targets. The purpose of this study guided by the theoretical framework of self-regulation theory is to explore how these individuals navigate self-regulatory processes in their sleep behaviors through mechanisms of self-monitoring, self-judgment, and self-evaluation. Methods: A qualitative descriptive design was implemented using semi-structured interviews with 34 young adults (ages 18–30) living with T1D. Data were collected through focused interviews, sleep diaries, actigraphy, and continuous glucose monitoring, followed by thematic analysis to identify sleep behavior self-regulation patterns. Results: Three primary themes were identified: (1) Sleep Behavior Self-Monitoring—highlighting participants’ awareness of their sleep habits and the diabetes-related impacts on these habits; (2) Sleep Behavior Self-Judgment—reflecting how personal and societal standards inform their evaluation of sleep health; (3) Sleep Behavior Self-Evaluation—showing emotional responses associated with sleep out-comes, where good sleep led to positive feelings and motivation, while poor sleep resulted in frustration. Conclusions: Understanding sleep behavior self-regulation among young adults with T1D is crucial for improving sleep health and diabetes management. Targeted interventions incorporating sleep education and self-regulatory strategies may enhance both perceived sleep quality and overall well-being in this population.
Full article
(This article belongs to the Special Issue Advances in Sleep Disorders in Patients with Diabetes)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Trabecular and Cortical Bone and Ossified Vessel Analysis in Rat Tibiae and Femora in a Polygenic Rat Model for Type 2 Diabetes Mellitus
by
Jason McIntire, Hope Oyeyemi, Michelle L. Harrison, Suchit Chidurala, Richard K. McCuller, Milena Samora, Yu Huo, Ann-Katrin Grotle, Audrey J. Stone, Kimber L. Stanhope, Peter J. Havel and Rhonda D. Prisby
Diabetology 2026, 7(4), 79; https://doi.org/10.3390/diabetology7040079 - 14 Apr 2026
Abstract
►▼
Show Figures
Background: In type 2 diabetes mellitus (T2DM), bone and microvascular complications may be linked. Methods: The University of California Davis (UCD) polygenic T2DM and Sprague Dawley healthy control (CTL) rats (N = 48) were divided equally into diabetic and age-matched groups: (1) pre-diabetes,
[...] Read more.
Background: In type 2 diabetes mellitus (T2DM), bone and microvascular complications may be linked. Methods: The University of California Davis (UCD) polygenic T2DM and Sprague Dawley healthy control (CTL) rats (N = 48) were divided equally into diabetic and age-matched groups: (1) pre-diabetes, (2) diabetes onset, (3) early-stage T2DM, and (4) late-stage T2DM. Body mass, HbA1c, fasted blood glucose and femoral and tibial lengths were measured. Bones were scanned (μCT; 15 µm) to assess trabecular microarchitecture and density and mid-shaft cortical thickness (Ct.Th, µm), density and porosity. Ossified vessel volume (OsVV, %) and thickness (OsV.Th, µm) were also analyzed. A GLM determined significance at p < 0.05. Body mass and HbA1c were higher (p < 0.05) in all T2DM groups and blood glucose became elevated (p < 0.05) in early-stage T2DM and late-stage T2DM. Results: Tibiae and femora were longer (p < 0.05) with diabetes. Tibial bone volume was lower (p < 0.05) in pre-diabetes (4 ± 1% vs. CTL, 9 ± 2%) and late-stage T2DM (5 ± 2% vs. CTL, 8 ± 2%), and femoral bone volume was lower (p < 0.05) in pre-diabetes (7 ± 1% vs. 12 ± 4%). Cortical density (tibia) was lower (p < 0.05) in pre-diabetes and early-stage T2DM. Trabecular density in the femur was lower (p < 0.05) in all T2DM groups and cortical density was reduced (p < 0.05) in pre-diabetes, diabetes onset, and late-stage T2DM. OsVV in both bones were lower (p < 0.05) during early-stage T2DM. Tibial OsV.Th was higher (p < 0.05) in pre-diabetes (69 ± 14 µm vs. CTL, 56 ± 13 µm) and late-stage T2DM (80 ± 10 µm vs. CTL, 59 ± 13 µm) and higher (p < 0.05) in the femur at diabetes onset (58 ± 14 µm vs. CTL, 40 ± 10 µm). Conclusions: Trabecular and cortical bone varied as diabetes progressed, and the thicker ossified vessels may represent microangiopathy.
Full article

Figure 1
Open AccessArticle
Long-Term Hyperglycemia Affects the Expression of Diaph1 and Its Cytoskeleton Ligands in the Epidermis of Diabetic Patients—A Quantitative Study
by
Bernard Kordas, Wojciech Matuszewski, Robert Modzelewski, Jarosław Szuszkiewicz, Michał Załęcki, Joanna Wojtkiewicz and Judyta Juranek
Diabetology 2026, 7(4), 78; https://doi.org/10.3390/diabetology7040078 - 10 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Diabetic small fiber neuropathy and related sensory and epidermal problems affect up to 70% of all patients with diabetes. Long-term hyperglycemia disrupts cytoskeletal organization and axonal transport; however, molecular changes within human diabetic epidermis remain understudied. Diaph1 and its cytoskeletal ligands,
[...] Read more.
Background/Objectives: Diabetic small fiber neuropathy and related sensory and epidermal problems affect up to 70% of all patients with diabetes. Long-term hyperglycemia disrupts cytoskeletal organization and axonal transport; however, molecular changes within human diabetic epidermis remain understudied. Diaph1 and its cytoskeletal ligands, including β-Actin and Profilin, are key regulators of cytoskeletal dynamics and may be associated with diabetes-related alterations in skin structure and innervation. Methods: Sixteen patients with type 2 diabetes, aged 43.3 ± 9.6 years (disease duration 18.9 ± 8.7 years), and twelve non-diabetic controls, aged 43.9 ± 8.9 years, were enrolled in the study. All participants provided informed consent. Skin punch biopsies were obtained under local anesthesia and processed for staining of PGP 9.5, Diaph1, β-Actin, and Profilin. Quantitative image analysis was performed to assess stained area fraction, signal intensity, and intraepidermal nerve fiber density. Statistical comparisons and Spearman’s rank correlation analyses were used to evaluate group differences and associations between staining parameters. Results: Diabetic skin samples exhibited a significant reduction in PGP 9.5-positive intraepidermal nerve fibers, indicating reduced cutaneous innervation. In contrast, Diaph1 and Profilin showed broader and more diffuse epidermal staining, while β-Actin displayed altered staining patterns and intensity. Significant correlations between Diaph1- and β-Actin-related staining measures indicated an association consistent with altered cytoskeletal organization under chronic hyperglycemic conditions. Conclusions: Long-standing type 2 diabetes was associated with reduced PGP 9.5-positive intraepidermal nerve fibers, together with altered epidermal staining patterns of Diaph1, Profilin and β-Actin. These findings indicate coexisting cutaneous denervation and cytoskeletal alterations in diabetic skin.
Full article

Graphical abstract
Open AccessArticle
Sexual Dimorphism in the Association Between Vitamin D and Depressive Symptoms in Diabetic Patients and the Mediating Role of BMI: A Cross-Sectional Study
by
Miriam Hernández-López, Rafael Ramírez-Carracedo, Mónica Grande-Alonso, Alba Sebastián-Martín and Rafael Moreno-Gómez-Toledano
Diabetology 2026, 7(4), 77; https://doi.org/10.3390/diabetology7040077 - 9 Apr 2026
Abstract
►▼
Show Figures
Background: The interplay between vitamin D deficiency, obesity, and depressive symptoms in type 2 diabetes remains poorly understood. Potential sex-specific differences in these associations have not been fully explored. Methods: We conducted a cross-sectional analysis of patients with type 2 diabetes
[...] Read more.
Background: The interplay between vitamin D deficiency, obesity, and depressive symptoms in type 2 diabetes remains poorly understood. Potential sex-specific differences in these associations have not been fully explored. Methods: We conducted a cross-sectional analysis of patients with type 2 diabetes (N = 917) from the NHANES 2017–2018 cycle. Restricted cubic spline models were used to assess potential non-linear associations between serum 25-hydroxyvitamin D3 and PHQ-9 depression scores. Regression-based mediation analysis was performed to estimate total, direct, and indirect associations, with body mass index (BMI) considered as a potential mediator. Models were adjusted for relevant demographic and cardiometabolic covariates. Results: In the overall diabetic cohort, higher vitamin D levels were modestly associated with lower depressive symptom scores. Mediation analysis suggested that this association was statistically accounted for by BMI. In sex-stratified analyses, significant total and indirect associations were observed among men, with a remaining direct association after adjustment for BMI, whereas no statistically significant associations were detected among women. Formal interaction testing supported differential association patterns by sex. Conclusions: Among adults with type 2 diabetes, serum vitamin D levels were inversely associated with depressive symptoms, with evidence suggesting sex-specific association patterns. These findings warrant further investigation in prospective studies to clarify potential underlying mechanisms and clinical implications.
Full article

Figure 1
Open AccessArticle
Identifying Risk Factors Associated with the Severity of Foot Ulcers in Type 2 Diabetic Patients: Evidence from a Hospital-Based Study in Rajshahi, Bangladesh
by
Shah Tanzen Jahan, Durga H. Kutal, Anicha Akter, Md. Selim Reza, Md. Kabirul Islam and Md. Monimul Huq
Diabetology 2026, 7(4), 76; https://doi.org/10.3390/diabetology7040076 - 8 Apr 2026
Abstract
►▼
Show Figures
Background: Diabetic foot ulcer (DFU) is a major complication of type 2 diabetes (T2D), frequently resulting in disability, lower-limb amputation, and substantial healthcare burden. Early identification of patients at high risk of progressing to severe DFU is essential for timely intervention, yet evidence
[...] Read more.
Background: Diabetic foot ulcer (DFU) is a major complication of type 2 diabetes (T2D), frequently resulting in disability, lower-limb amputation, and substantial healthcare burden. Early identification of patients at high risk of progressing to severe DFU is essential for timely intervention, yet evidence on associated risk factors remains limited in Bangladesh. This study aims to identify demographic, clinical, and behavioral predictors of severe DFU to support early management strategies. Methods: A cross-sectional study was conducted among 159 DFU patients attending the Rajshahi Diabetic Association General Hospital, Bangladesh. Data on demographic characteristics, clinical variables, and behavioral factors were obtained through structured questionnaires and standardized examinations. Severe DFU was defined as Wagner grades 3–5, while grades 0–2 were considered non-severe. Firth’s penalized logistic regression was used to identify determinants of severe DFU. Model performance was assessed using ROC analysis, calibration belt analysis, and decision curve analysis (DCA). Results: Among the 159 participants, 101 (63.5%) presented with severe DFU. Patients with severe DFU had significantly higher BMI (26.1 vs. 23.7 kg/m2), treatment costs (50,000 vs. 20,000 BDT), and were older (57 vs. 54 years). Severe DFU was also associated with higher prevalence of peripheral arterial disease (PAD) (29.7% vs. 3.4%), prior amputation (31.7% vs. 3.4%), peripheral neuropathy (PN) (86.1% vs. 58.6%), and poor glycemic control (71.3% vs. 30.7%) (all p < 0.05). Firth’s regression identified older age (aOR 1.08), poor glycemic control (aOR 3.90), PN (aOR 3.41), PAD (aOR 7.54), and previous amputation (aOR 13.67) as independent predictors of severe DFU. Conclusions: Older age, uncontrolled glycemia, PN, PAD, and prior amputation were significantly associated with severe stages of DFU. Early detection and targeted management of these factors are critical to reducing complications and lowering the healthcare burden.
Full article
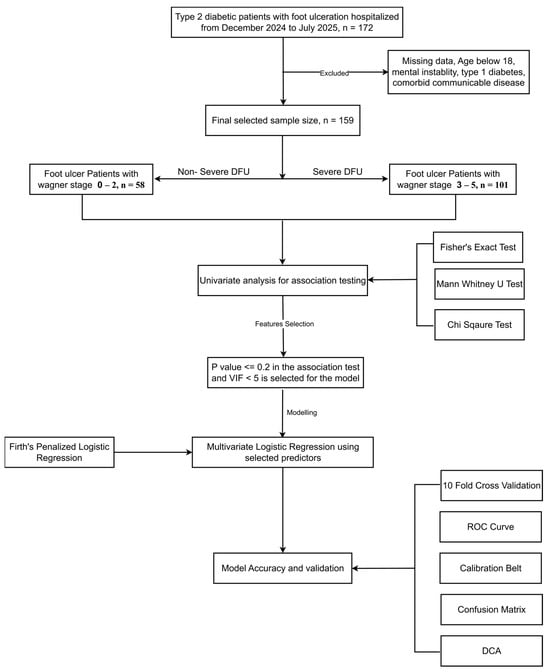
Figure 1
Open AccessArticle
Effect of Metformin on Sleep Architecture in Patients with Comorbid Diabetes and Sleep Apnea
by
Kristen Masada, Daniel Nguyen and Madhu Varma
Diabetology 2026, 7(4), 75; https://doi.org/10.3390/diabetology7040075 - 7 Apr 2026
Abstract
Background/Objectives: Patients with poor sleep are at high risk of developing type II diabetes mellitus (T2DM). Since T2DM is linked to increased risk of obstructive sleep apnea (OSA), and Metformin is commonly used to treat T2DM, we examined how Metformin affects sleep stages
[...] Read more.
Background/Objectives: Patients with poor sleep are at high risk of developing type II diabetes mellitus (T2DM). Since T2DM is linked to increased risk of obstructive sleep apnea (OSA), and Metformin is commonly used to treat T2DM, we examined how Metformin affects sleep stages in patients with concurrent T2DM and OSA-related symptoms of snoring and fatigue. Patients with T2DM on Metformin progressively develop increased insulin resistance associated with sleep disturbances and poor glycemic control. We therefore explored sleep pattern changes in patients with OSA symptoms and T2DM on Metformin, with a special focus on whether Metformin affects sleep architecture. Methods: Polysomnogram (PSG) data from patients with T2DM on Metformin was evaluated along with data on age, body-mass index (BMI), and biological sex. Data analysis included mean ± standard deviation, t-test with p < 0.05 taken as significant, and linear regression. Results: Patients with a BMI of less than 30 (non-obese) and taking Metformin exhibited a significantly shorter rapid eye movement sleep stage (REM) duration than patients on alternative therapies (p = 0.036). No such difference in REM was found for patients with a BMI of 30 or greater (obese) taking Metformin. While there was also no significant difference in slow-wave sleep stage (N3) duration with Metformin use, linear regression identified a moderate negative correlation between N3 and age in patients taking non-Metformin therapies (R2 = 0.4555). No significant correlations between sleep stage duration and patient sex, smoking status, or BMI greater than 30 were identified. Conclusions: Overall, patients with OSA and T2DM on Metformin had lower mean quantities of N3, and REM sleep compared to those not on Metformin. Non-obese patients with T2DM and OSA being treated with Metformin were observed to have less REM sleep, regardless of sex or smoking history. N3 and REM sleep are needed for the timely secretion of growth hormone and memory consolidation. Since Metformin is correlated with differences in N3 and REM sleep, it may contribute to the development of insulin resistance. Future studies are needed to explore potential causes for this relationship and how it may affect the treatment of T2DM.
Full article
(This article belongs to the Special Issue Advances in Sleep Disorders in Patients with Diabetes)
►▼
Show Figures

Figure 1
Open AccessArticle
Effect of Glycemic Management on Severity of Functional Impairment in Elderly Individuals with Type 2 Diabetes
by
Kohei Ueda, Rie Saito, Akiko Matsunaga, Takayuki Sonoda, Misako Kawaguchi, Saori Kaeriyama, Satsuki Sato, Yasuo Zenimaru, Masamichi Ikawa and Norio Harada
Diabetology 2026, 7(4), 74; https://doi.org/10.3390/diabetology7040074 - 3 Apr 2026
Abstract
Background/Objectives: Diabetes threatens independent living among elderly individuals. However, the effects of glycemic management on the severity of functional impairment are unclear. This study aimed to elucidate the relationship between glycemic management and functional impairment severity in elderly individuals with type 2 diabetes
[...] Read more.
Background/Objectives: Diabetes threatens independent living among elderly individuals. However, the effects of glycemic management on the severity of functional impairment are unclear. This study aimed to elucidate the relationship between glycemic management and functional impairment severity in elderly individuals with type 2 diabetes (T2D). Methods: We used data from the Japanese National Health Insurance Database from 2017 to 2024. The database included 11,411 elderly individuals (≥65 years) with Long-Term Care Insurance evaluations. Functional status was classified into three categories based on independence—Group A (non-mild impairment), Group B (moderate impairment), and Group C (severe impairment). The factors associated with the severity of functional impairment in patients with T2D were elucidated. Results: The severity of functional impairment was significantly greater in patients with T2D than in those without T2D. In participants with T2D, low glycated hemoglobin (HbA1c) levels were associated with the severity of functional impairment (odds ratio [OR]: 0.78; p < 0.001). In contrast, the use of antidiabetic drugs that could induce severe hypoglycemia (high-risk drugs) was positively associated with the severity of functional impairment (Group A vs. B/C: OR: 1.42; p < 0.001; Group C vs. A/B: OR: 1.90; p < 0.001). The frequency of high-risk drug use increased as functional impairment increased. Conclusions: The use of high-risk drugs is associated with the severity of functional impairment in elderly individuals with T2D. Elucidating the factors associated with the severity of functional impairment in elderly individuals with T2D may contribute to maintaining their quality of life and reducing the economic burden on healthcare and long-term care systems.
Full article
(This article belongs to the Special Issue Advances in Diabetes: Prevalence, Risk Factors, Complications, Costs and Disparities)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Adipose Tissue Grafting: A New Paradigm in Diabetic Foot Treatment
by
Roberto Da Ros, Roberta Assaloni, Andrea Michelli, Barbara Brunato, Enrica Barro, Marta Nardi, Giovanni Papa and Cesare Miranda
Diabetology 2026, 7(4), 73; https://doi.org/10.3390/diabetology7040073 - 3 Apr 2026
Abstract
►▼
Show Figures
Background: Adipose tissue grafting is a regenerative medicine approach based on the use of autologous adipose tissue showing significant potential for the treatment of diabetic foot lesions. In subjects with diabetes, impaired wound healing, peripheral neuropathy, and vascular insufficiency contribute to the development
[...] Read more.
Background: Adipose tissue grafting is a regenerative medicine approach based on the use of autologous adipose tissue showing significant potential for the treatment of diabetic foot lesions. In subjects with diabetes, impaired wound healing, peripheral neuropathy, and vascular insufficiency contribute to the development of chronic ulcers and osteomyelitis, complicating traditional treatment strategies. Materials and Methods: We conducted a retrospective analysis of our center’s database, including all subjects treated for chronic diabetic foot ulcers who underwent adipose grafting with a follow-up of at least six months. For the control group, we included patients who received artificial dermis grafts rather than adipose grafts. Results: We identified 45 patients in the adipose group and 39 in the control group. Baseline characteristics were similar between the two groups for: mean age, diabetes duration, creatinine level, HbA1c, peripheral neuropathy, peripheral vascular disease and osteomyelitis. Coronary artery disease was prevalent in the control group. Wound location demonstrates a prevalent heel involvement for the adipose group. No patients experienced severe complications due to adipose graft: four patients (9%) developed a hematoma at the adipose tissue harvesting site, which was resolved spontaneously. At a mean follow-up of 12 ± 5 months, 30 (67%) patients achieved healing with a mean healing time of 202 ± 82 days, without requiring further surgical interventions. The control group achieved 51% of healing (p = 0.04), with a mean healing time longer than in the adipose graft group: 275 ± 132 days (p = 0.02). Moreover adipose graft permitted the best performance in rearfoot lesions. Conclusions: Adipose grafting is a safe and minimally invasive procedure with no major adverse events. Our data demonstrate its efficacy in promoting healing, even in chronic lesions with osteomyelitis and those located on the heel. Efficacy was found to be superior to that of the artificial dermis graft group.
Full article

Graphical abstract
Open AccessReview
Lipoprotein (a) and Apolipoproteins in Diabetes and Atherosclerotic Cardiovascular Disease: A Comprehensive Review of the Current Evidence
by
Albion Luzha, Michael Y. Henein, Guxim Bytyçi, Rina Tafarshiku, Gani Bajraktari and Venera Berisha-Muharremi
Diabetology 2026, 7(4), 72; https://doi.org/10.3390/diabetology7040072 - 3 Apr 2026
Abstract
Atherosclerosis, manifesting as acute myocardial infarction, stroke and peripheral artery disease, is the main cause of death worldwide. Conventional risk factors contributing to the development and progression of atherosclerosis are well established, including diabetes mellitus, hypertension, hypercholesterolemia, smoking and obesity. In recent decades,
[...] Read more.
Atherosclerosis, manifesting as acute myocardial infarction, stroke and peripheral artery disease, is the main cause of death worldwide. Conventional risk factors contributing to the development and progression of atherosclerosis are well established, including diabetes mellitus, hypertension, hypercholesterolemia, smoking and obesity. In recent decades, other lipid molecules have been identified as risk factors for atherosclerosis and arterial calcification, including lipoprotein (a) and apolipoproteins. Despite the available evidence for the association between those biomarkers and atherosclerosis in the general population, their impact on diabetic patients is incompletely characterized. This review aims to summarize the current evidence on the relationship between lipoprotein (a), apolipoproteins and atherosclerotic cardiovascular disease in diabetic patients. By integrating genetic, epidemiological, and mechanistic data, this review highlights the dual and context-dependent associations of lipoprotein (a) with incident type 2 diabetes and atherosclerotic cardiovascular risk, supporting more nuanced interpretation of Lp(a) in diabetes-related risk assessment.
Full article
(This article belongs to the Special Issue Precision Medicine for Diabetes: From Screening to Personalized Management)
►▼
Show Figures

Figure 1
Open AccessArticle
Diabetes-Related β-Cell Dysfunction Across COVID-19 and Metabolic Syndrome Is More Closely Associated with Chronic Oxidative Stress than with Transient Hypoxia
by
Victoria Tsvetkova, Malvina Todorova, Milena Atanasova, Irena Gencheva and Katya Todorova
Diabetology 2026, 7(4), 71; https://doi.org/10.3390/diabetology7040071 - 2 Apr 2026
Abstract
Aims/hypothesis: Hypoxia and oxidative stress have been implicated in both metabolic syndrome and COVID-19-associated dysglycaemia, yet it remains unclear whether shared or distinct mechanisms underlie β-cell dysfunction across these conditions. We investigated hypoxia- and oxidative stress-related pathways in relation to β-cell function
[...] Read more.
Aims/hypothesis: Hypoxia and oxidative stress have been implicated in both metabolic syndrome and COVID-19-associated dysglycaemia, yet it remains unclear whether shared or distinct mechanisms underlie β-cell dysfunction across these conditions. We investigated hypoxia- and oxidative stress-related pathways in relation to β-cell function during acute COVID-19, post-COVID metabolic states, and COVID-negative metabolic syndrome. Methods: In this prospective observational study, 100 adults were stratified into three groups: active COVID-19 (n = 32), post-COVID with newly diagnosed carbohydrate metabolism disorders (n = 35), and COVID-negative individuals with metabolic syndrome (n = 33). Circulating markers of hypoxia (HIF-1α), oxidative stress (8-epi-prostaglandin F2α), and antioxidant response (NFE2L2) were measured alongside α- and β-cell functional markers, including C-peptide, proinsulin, glucagon, and derived indices of β-cell processing and secretory efficiency. Non-parametric statistical analyses were applied. Results: Circulating HIF-1α levels differed significantly across study groups (p < 0.001), with the highest concentrations observed during active COVID-19, intermediate levels in COVID-negative individuals with metabolic syndrome, and the lowest levels in the post-COVID group. In contrast, oxidative stress, assessed by 8-epi-prostaglandin F2α, differed significantly across groups (p < 0.001), increasing from acute COVID-19 to post-COVID and reaching the highest levels in metabolic syndrome; however, the difference between the post-COVID and metabolic syndrome groups did not remain significant after correction for multiple testing. NFE2L2 concentrations did not differ significantly between groups. Marked β-cell dysfunction was observed predominantly in COVID-negative individuals with metabolic syndrome, characterized by reduced C-peptide levels, elevated glucagon concentrations, increased proinsulin/C-peptide ratios, and reduced C-peptide/glucose ratios (all overall group comparisons p < 0.001). In contrast, β-cell secretory indices were relatively preserved during acute and post-COVID states despite pronounced alterations in hypoxia and oxidative stress markers. Conclusions/interpretation: Hypoxia- and oxidative stress-related pathways exhibit distinct, context-dependent patterns across acute COVID-19, post-COVID dysglycaemia, and metabolic syndrome. Acute COVID-19 is characterized by pronounced hypoxia signalling with relative preservation of β-cell function, whereas chronic metabolic syndrome is associated with sustained oxidative stress and impaired β-cell processing and secretory efficiency. These findings suggest that diabetes-related β-cell dysfunction is more closely associated with chronic oxidative and metabolic stress than with transient infection-related hypoxia during SARS-CoV-2 infection.
Full article
(This article belongs to the Special Issue Beta-Cell Failure and Death: A Cornerstone in Diabetes Pathogenesis)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Cost-Effectiveness of Pressure-Guided-Offloading-Improved Custom-Made Footwear for People with Diabetes at High Risk of Plantar Foot Ulceration
by
Sicco A. Bus, Jaap J. van Netten, Diekje R. Schouten and Marcel G. W. Dijkgraaf
Diabetology 2026, 7(4), 70; https://doi.org/10.3390/diabetology7040070 - 2 Apr 2026
Abstract
Background: Custom-made footwear that improves offloading using in-shoe pressure-guided techniques, when worn as recommended, reduces the risk of diabetic foot ulcer recurrence. We aimed to assess the cost-effectiveness of this approach, as it requires extra investments in equipment and personnel, and implementation is
[...] Read more.
Background: Custom-made footwear that improves offloading using in-shoe pressure-guided techniques, when worn as recommended, reduces the risk of diabetic foot ulcer recurrence. We aimed to assess the cost-effectiveness of this approach, as it requires extra investments in equipment and personnel, and implementation is not yet widespread. Methods: We conducted an economic evaluation using data from the DIAFOS RCT that randomized 171 participants at high ulcer risk to either pressure-guided-offloading-improved (intervention) or non-pressure-guided (usual care) custom-made footwear. The clinical outcome was the 18-month ulcer recurrence incidence, available from the RCT. Costs were modeled from a partial healthcare perspective using bottom-up unit cost calculation, with ulcer treatment costs obtained from reference data. Univariable regression analyses were executed to obtain incremental cost-effectiveness ratios (ICERs). Bootstrapping techniques accounted for uncertainty. Results: For the intervention, costs for ulcer recurrence were non-significantly lower (€−436; 95% CI: €−1434; €563) than for usual care. The ICER was €−8124 (i.e., costs saved to prevent one extra participant from having an ulcer), and the maximum probability for cost-effectiveness was 0.81. In the subgroup of participants who were adherent to wearing their prescribed footwear, costs for the intervention were non-significantly lower at €−1170 (95% CI: €−2595; €254), with ICER of €−5317, and a maximum probability for cost-effectiveness of 0.94. Conclusions: The use of in-shoe pressure-guided-offloading-improved custom-made footwear to help prevent diabetic foot ulcer recurrence is cost-effective with high probability when ulcer treatment costs are considered. Probability further increases when users adhere to their footwear. Future economic analyses should consider a full healthcare and societal perspective and use prospectively collected data on ulcer treatment costs.
Full article
(This article belongs to the Special Issue Prevention and Care of Diabetic Foot Ulcers)
►▼
Show Figures

Graphical abstract
Open AccessReview
Evaluation of the Present Perspective on Diabetic Foot Syndrome and Health Education and Analysis of the Impact of Educational Interventions: A Systematic Review and Meta-Analysis
by
Sol Tejeda-Ramírez, José Luis Lázaro-Martínez, Esther García-Morales, Sara García-Oreja, Laura Palacios-Abril and Aroa Tardáguila-García
Diabetology 2026, 7(4), 69; https://doi.org/10.3390/diabetology7040069 - 2 Apr 2026
Abstract
Aims: To evaluate the effectiveness of preventive educational interventions in individuals with diabetic foot syndrome (DFS) and to summarise current evidence on knowledge, self-care and health-education strategies related to this complication. Materials and methods: A systematic review and meta-analysis was conducted
[...] Read more.
Aims: To evaluate the effectiveness of preventive educational interventions in individuals with diabetic foot syndrome (DFS) and to summarise current evidence on knowledge, self-care and health-education strategies related to this complication. Materials and methods: A systematic review and meta-analysis was conducted in accordance with PRISMA guidelines. Risk of bias was evaluated using the Cochrane Handbook recommendations. Analyses were performed with Review Manager v5.4.1. Results: Educational interventions produced a significant improvement in patient knowledge and self-care practices compared with usual care. Despite some heterogeneity across studies, the overall effect favoured structured education as a preventive strategy for DFS-related complications. Conclusions: Preventive educational interventions enhance knowledge and self-care among individuals with DFS. Implementing structured education programs may help reduce complications and improve clinical outcomes.
Full article
(This article belongs to the Special Issue Prevention and Care of Diabetic Foot Ulcers)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomolecules, Diabetology, IJMS, JCM, Metabolites, Nutrients
Diabetes and Obesity Under Environmental Stressors: Mechanisms and Clinical Implications
Topic Editors: Ioanna Eleftheriadou, Dimitris KounatidisDeadline: 31 March 2027
Topic in
Antibiotics, Diabetology, JAPMA, JCM, Medicina
Diabetic Foot Disease: Current Challenges, Emerging Concepts and Future Directions
Topic Editors: José Luis Lázaro-Martínez, Marco Meloni, Prashanth VasDeadline: 31 March 2028

Conferences
Special Issues
Special Issue in
Diabetology
Insulin Therapy: New Technologies and Future Perspectives
Guest Editor: Betul HatipogluDeadline: 20 May 2026
Special Issue in
Diabetology
Treatment of Type 1 Diabetes: Transplantation of Insulin Producing Cells
Guest Editor: Naoaki SakataDeadline: 20 May 2026
Special Issue in
Diabetology
Advances in Sleep Disorders in Patients with Diabetes
Guest Editor: Stephanie A. GriggsDeadline: 20 May 2026
Special Issue in
Diabetology
All Toes Considered for Diabetic Foot: Prevention, Treatment, and Healthcare Policy
Guest Editors: Chia-Ding Shih, Miguel Manzur, Sofia Sakellaridi, David G. ArmstrongDeadline: 10 June 2026









