Effect of Sonic Application of Self-Adhesive Resin Cements on Push-Out Bond Strength of Glass Fiber Posts to Root Dentin
Abstract
:1. Introduction
2. Materials and Methods
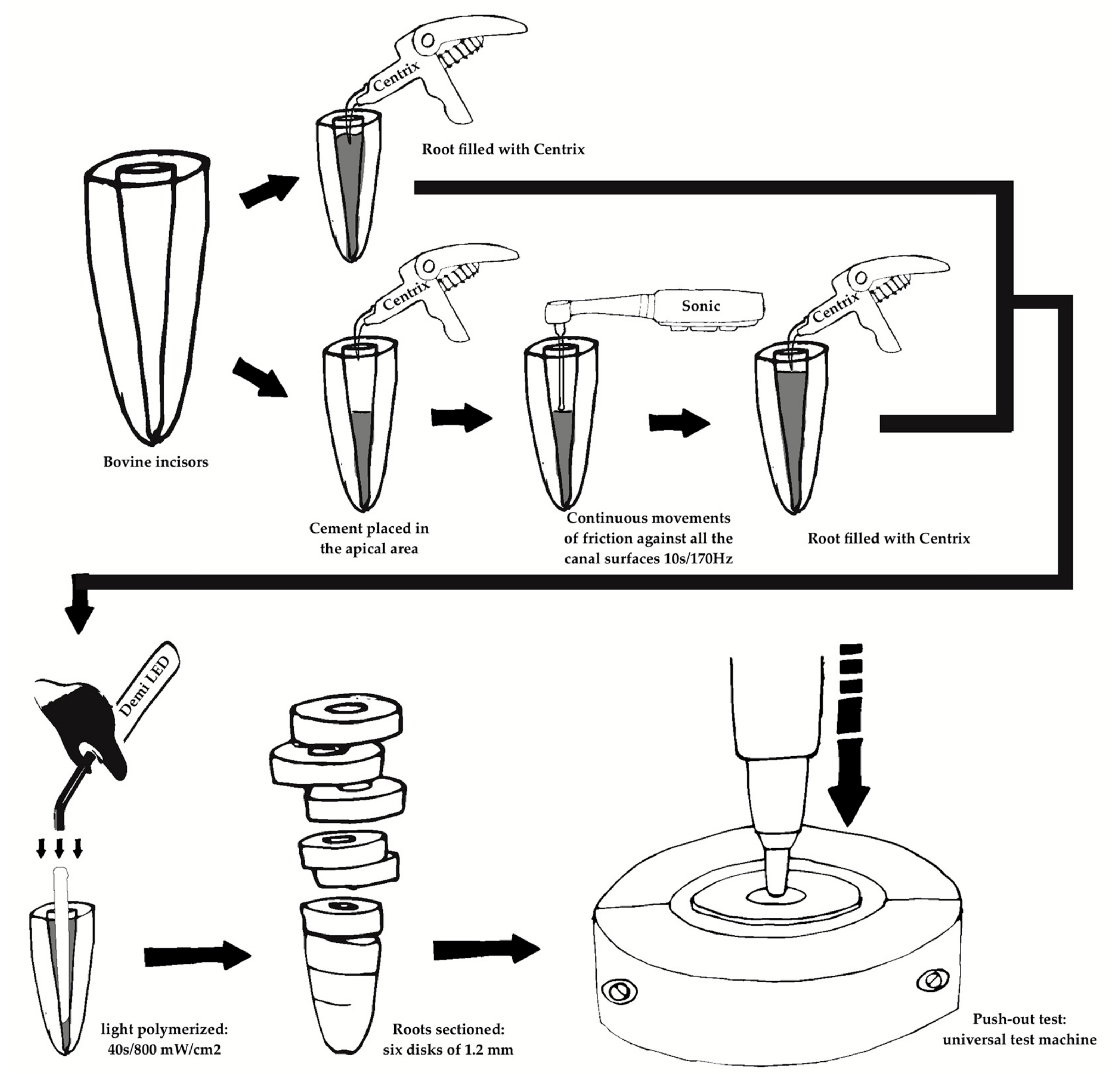
2.1. Preparation of Specimens
2.2. Post Cementation
2.3. Push-Out Bond Strength Test
2.4. Stereomicroscope Pattern Evaluation (Fracture Pattern)
2.5. Scanning Electron Microscopy (SEM)
2.6. Statistical Analysis
3. Results
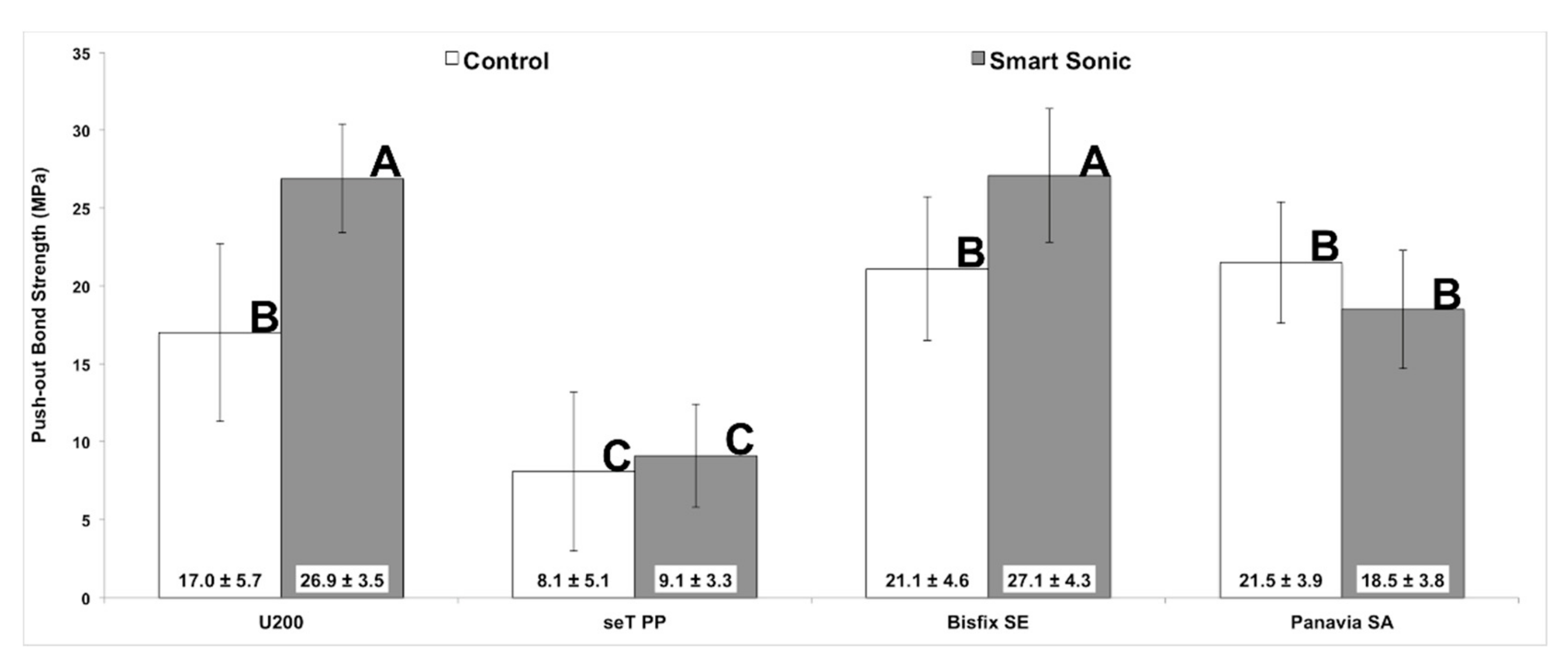
3.1. Push-Out Bond Strength Test
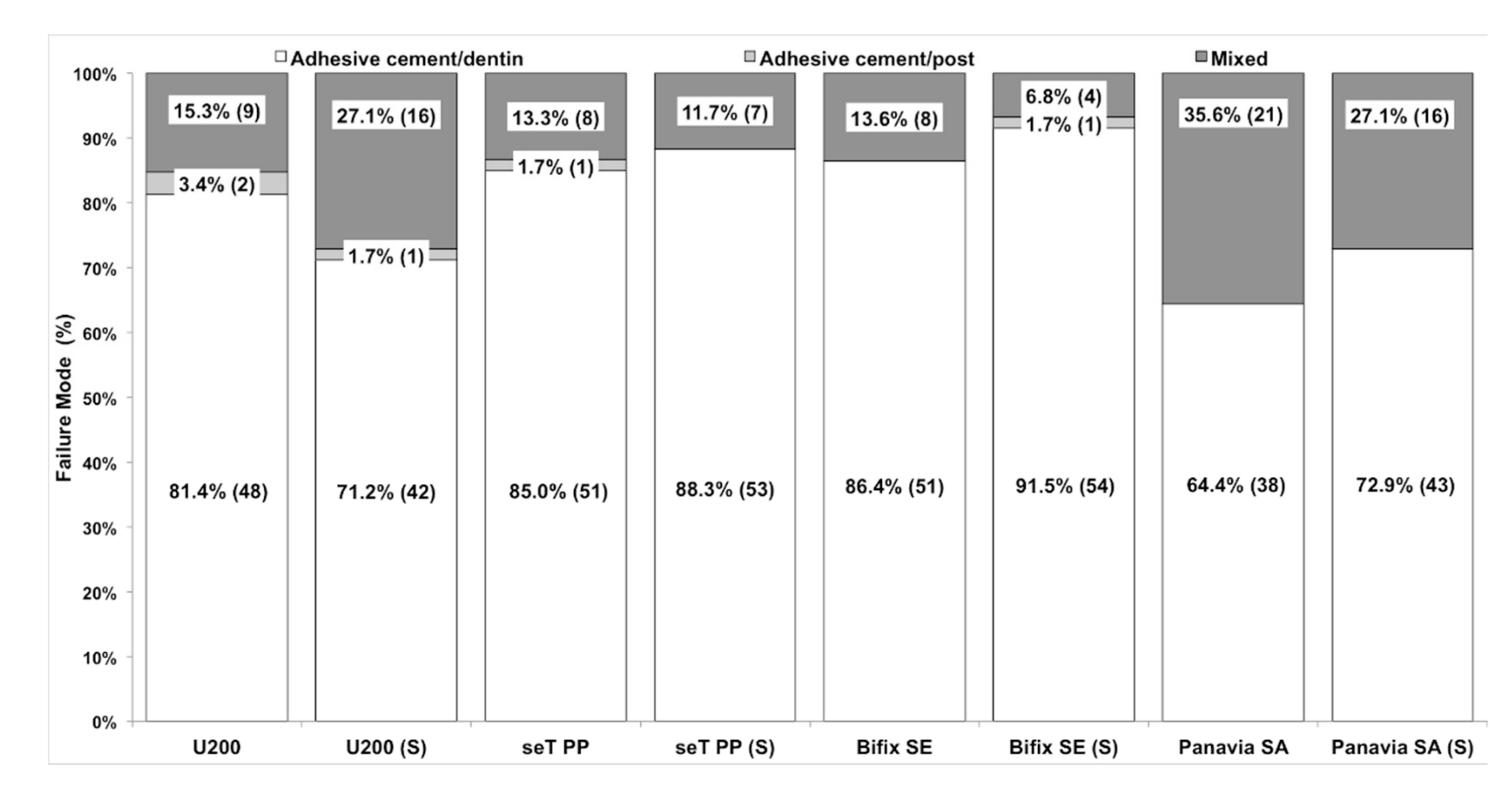
3.2. Stereomicroscope Pattern Evaluation (Fracture Pattern)
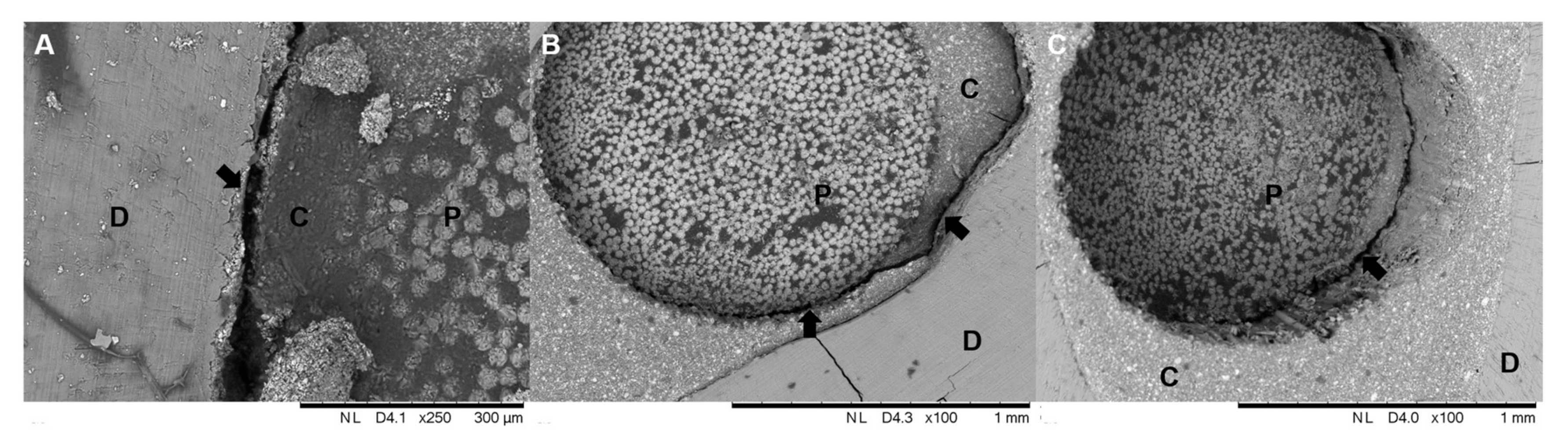
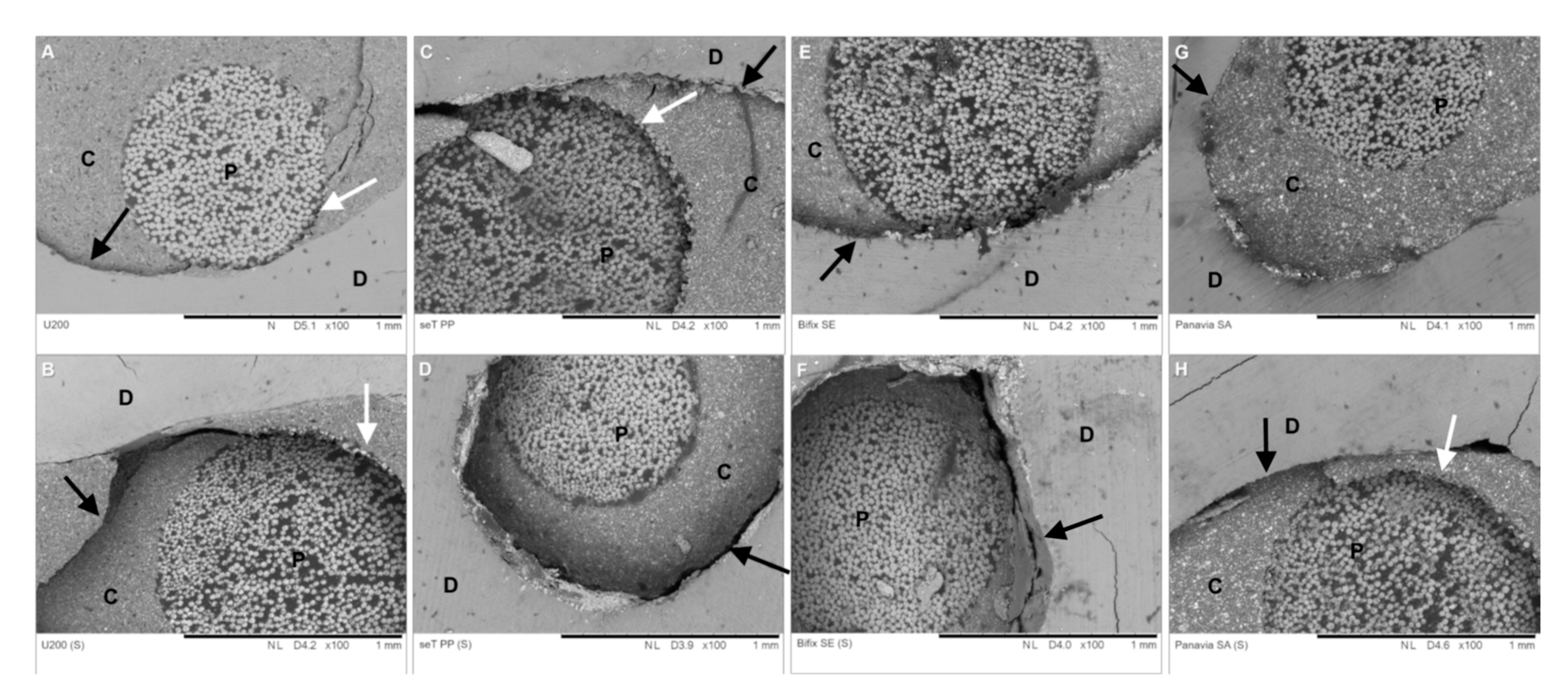
3.3. Scanning Electron Microscopy (SEM)
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Rasimick, B.J.; Wan, J.; Musikant, B.L.; Deutsch, A.S. A review of failure modes in teeth restored with adhesively luted endodontic dowels. J. Prosthodont. 2010, 19, 639–646. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; He, F.; Burrow, M.F.; Xie, H.; Zhu, Y.; Zhang, F. Bond strengths of two self-adhesive resin cements to dentin with different treatments. J. Med. Biol. Eng. 2011, 31, 73–77. [Google Scholar] [CrossRef]
- Viotti, R.G.; Kasaz, A.; Pena, C.E.; Alexandre, R.S.; Arrais, C.A.; Reis, A.F. Microtensile bond strength of new self-adhesive luting agents and conventional multistep systems. J. Prosthet. Dent. 2009, 102, 306–312. [Google Scholar] [CrossRef]
- Ferracane, J.L.; Stansbury, J.W.; Burke, F.J.T. Self-adhesive resin cements—Chemistry, properties and clinical considerations. J. Oral Rehabil. 2011, 38, 295–314. [Google Scholar] [CrossRef] [PubMed]
- Manso, A.P.; Carvalho, R.M. Dental cements for luting and bonding restorations: self-adhesive resin cements. Dent. Clin. N. Am. 2017, 61, 821–834. [Google Scholar] [CrossRef] [PubMed]
- Rezende, E.C.; Gomes, G.M.; Szesz, A.L.; da Silveira Bueno, C.E.; Reis, A.; Loguercio, A.D. Effects of dentin moisture on cementation of fiber posts to root canals. J. Adhes. Dent. 2016, 18, 29–34. [Google Scholar] [PubMed]
- Radovic, I.; Monticelli, F.; Goracci, C.; Vulicevic, Z.R.; Ferrari, M. Self-adhesive resin cements: A literature review. J. Adhes. Dent. 2008, 10, 251–258. [Google Scholar] [PubMed]
- De Munck, J.; Vargas, M.; van Landuyt, K.; Hikita, K.; Lambrechts, P.; Van Meerbeek, B. Bonding of an auto-adhesive luting material to enamel and dentin. Dent. Mater. 2004, 20, 963–971. [Google Scholar] [CrossRef] [PubMed]
- Durski, M.; Metz, M.; Thompson, J.; Mascarenhas, A.; Crim, G.; Vieira, S.; Mazur, R. Push-out bond strength evaluation of glass fiber posts with different resin cements and application techniques. Oper. Dent. 2016, 41, 103–110. [Google Scholar] [CrossRef] [PubMed]
- Do Vale Pedreira, A.P.R.; D’Alpino, P.H.P.; Pereira, P.N.R.; Chaves, S.B.; Wang, L.; Hilgert, L.; Garcia, F.C.P. Effects of the application techniques of self-adhesive resin cements on the interfacial integrity and bond strength of fiber posts to dentin. J. Appl. Oral Sci. 2016, 24, 437–446. [Google Scholar] [CrossRef] [Green Version]
- Mena-Serrano, A.; Garcia, E.J.; Loguercio, A.D.; Reis, A. Effect of sonic application mode on the resin-dentin bond strength and nanoleakage of simplified self-etch adhesive. Clin. Oral Investig. 2014, 18, 729–736. [Google Scholar] [CrossRef]
- Muñoz, M.A.; Luque-Martinez, I.; Hass, V.; Gutierrez, M.F.; Reis, A.; Loguercio, A.D. The sonic application of universal adhesives in self-etch mode improves their performance on enamel. Int. J. Adhes. Adhes. 2019, 88, 43–49. [Google Scholar] [CrossRef]
- Cuadros-Sanchez, J.; Szesz, A.; Hass, V.; Patzlaff, R.T.; Reis, A.; Loguercio, A.D. Effects of sonic application of adhesive systems on bonding fiber posts to root canals. J. Endod. 2014, 40, 1201–1205. [Google Scholar] [CrossRef]
- Mena-Serrano, A.; da Costa, T.R.F.; Patzlaff, R.T.; Loguercio, A.D.; Reis, A. Effect of sonic application mode on the resin-dentin bond strength and dentin permeability of self-etching systems. J. Adhes. Dent. 2014, 16, 435–440. [Google Scholar]
- Kirsch, J.; Schmidt, D.; Herzberg, D.; Weber, M.-T.; Gäbler, S.; Hannig, C. Effect of Sonic Application of Self-etch Adhesives on Bonding Fiber Posts to Root Canal Dentin. J. Adhes. Dent. 2017, 19, 295–304. [Google Scholar]
- Lin, J.; Shinya, A.; Gomi, H.; Shinya, A. Bonding of self-adhesive resin cements to enamel using different surface treatments: bond strength and etching pattern evaluations. Dent. Mater. J. 2010, 29, 425–432. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bernardi, S.; Bianchi, S.; Botticelli, G.; Rastelli, E.; Tomei, A.R.; Palmerini, M.G.; Continenza, M.A.; Macchiarelli, G. Scanning electron microscopy and microbiological approaches for the evaluation of salivary microorganisms behaviour on anatase titanium surfaces: In vitro study. Morphologie 2018, 102, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Skupien, J.A.; Sarkis-Onofre, R.; Cenci, M.S.; de Moraes, R.R.; Pereira-Cenci, T. A systematic review of factors associated with the retention of glass fiber posts. Braz. Oral Res. 2015, 29, 1–8. [Google Scholar] [CrossRef] [Green Version]
- Kambara, K.; Nakajima, M.; Hosaka, K.; Takahashi, M.; Thanatvarakorn, O.; Ichinose, S.; Foxton, R.M.; Tagami, J. Effect of smear layer treatment on dentin bond of self-adhesive cements. Dent. Mater. J. 2012, 31, 980–987. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carvalho, E.M.; de Souza, W.L.P.; Carvalho, C.N.; Maciel, A.P.; Loguercio, A.D.; Bauer, J. Effect of storage time on microtensile bond strength of self-adhesive and multi-step resin cements to dentin. Mater. Res. 2016, 19, 695–701. [Google Scholar] [CrossRef]
- Di Hipólito, V.; Rodrigues, F.P.; Piveta, F.B.; da Cuha Azevedo, L.; Bruschi Alonso, R.C.; Silikas, N.; Carvalho, R.M.; de Goes, M.F.; Perlatti D’Alpino, P.H. Effectiveness of self-adhesive luting cements in bonding to chlorhexidine-treated dentin. Dent. Mater. 2012, 28, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, E.M.; Lima, D.M.; Carvalho, C.N.; Loguercio, A.D.; Martinelli, J.R.; Bauer, J. Effect of airborne-particle abrasion on dentin with experimental niobophosphate bioactive glass on the microtensile bond strength of resin cements. J. Prosthodont. Res. 2015, 59, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Mushashe, A.M.; Fereirado Amaral, R.O.J.; Rezende, C.E.E.; Filho, F.B.; da Cunha, L.F.; Gonzaga, C.C. Effect of sonic vibrations on bond strength of fiberglass posts bonded to root Dentin. Braz. Dent. J. 2017, 28, 30–34. [Google Scholar] [CrossRef] [PubMed]
- Zarpellon, D.C.; Szesz, A.L.; Loguercio, A.D.; Arrais, C.A.G. Effect of sonic application of universal adhesive systems on bond strength of fiber posts to root Canal. J. Adhes. Dent. 2016, 18, 493–499. [Google Scholar] [PubMed]
- Yu, Z.; Strutz, J.M.; Kipnis, V.; White, S.N. Effect of dynamic loading methods on cement film thickness in vitro. J. Prosthodont. 1995, 4, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, F.; de Paiva Campos, L.M.; Rodrigues-Júnior, E.C.; Costa, F.V.; Marques, P.A.; Francci, C.E.; Braga, R.R.; Boaro, L.C.C. A comparative study of bulk-fill composites: degree of conversion, post-gel shrinkage and cytotoxicity. Braz. Oral Res. 2018, 32, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Gerth, H.U.V.; Dammaschke, T.; Züchner, H.; Schäfer, E. Chemical analysis and bonding reaction of RelyX Unicem and Bifix composites—A comparative study. Dent. Mater. 2006, 22, 934–941. [Google Scholar] [CrossRef]
- Ehlers, V.; Kampf, G.; Stender, E.; Willershausen, B.; Ernst, C.-P. Effect of thermocycling with or without 1 year of water storage on retentive strengths of luting cements for zirconia crowns. J. Prosthet. Dent. 2015, 113, 609–615. [Google Scholar] [CrossRef]
- D’Alpino, P.H.P.; Silva, M.S.; Vismara, M.V.G.; di Hipólito, V.; Miranda González, A.H.; de Oliveira Graeff, C.F. The effect of polymerization mode on monomer conversion, free radical entrapment, and interaction with hydroxyapatite of commercial self-adhesive cements. J. Mech. Behav. Biomed. Mater. 2015, 46, 83–92. [Google Scholar] [CrossRef]
- Turp, V.; Sen, D.; Tuncelli, B.; Ozcan, M. Adhesion of 10-MDP containing resin cements to dentin with and without the etch-and-rinse technique. J. Adv. Prosthodont. 2013, 5, 226–233. [Google Scholar] [CrossRef]
- Yoshida, Y.; van Meerbeek, B.; Nakayama, Y.; Yoshioka, M.; Snauwaert, J.; Abe, Y.; Lambrechts, P.; Vanherle, G.; Okazaki, M. Adhesion to and Decalcification of Hydroxyapatite by Carboxylic Acids. J. Dent. Res. 2001, 80, 1565–1569. [Google Scholar] [CrossRef] [PubMed]
- Feitosa, V.P.; Sauro, S.; Ogliari, F.A.; Ogliari, A.O.; Yoshihara, K.; Zanchi, C.H.; Correr-Sobrinho, L.; Sinhoreti, M.A.; Correr, A.B.; Watson, T.F.; et al. Impact of hydrophilicity and length of spacer chains on the bonding of functional monomers. Dent. Mater. 2014, 30, e317–e323. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, Y.; Yoshihara, K.; Nagaoka, N.; Hayakawa, S.; Torii, Y.; Ogawa, T.; Osaka, A.; Meerbeek, B. Van Self-assembled Nano-layering at the Adhesive interface. J. Dent. Res. 2012, 91, 376–381. [Google Scholar] [CrossRef] [PubMed]
- Kasaz, A.C.; Pena, C.E.; de Alexandre, R.S.; Viotti, R.G.; Santana, V.B.; Arrais, C.A.G.; Giannini, M.; Reis, A.F. Effects of a peripheral enamel margin on the long-term bond strength and nanoleakage of composite/dentin interfaces produced by self-adhesive and conventional resin cements. J. Adhes. Dent. 2012, 14, 251–263. [Google Scholar] [PubMed]
- Stona, P.; Borges, G.A.; Montes, M.A.; Júnior, L.H.; Weber, J.B.; Spohr, A.M. Effect of polyacrylic acid on the interface and bond strength of self-adhesive resin cements to dentin. J. Adhes. Dent. 2013, 15, 221–227. [Google Scholar] [PubMed]
| Cements | Composition | Application Mode |
|---|---|---|
| RELYX U200 (3M/ESPE, St.Paul, MN, USA) Lot Number (1509000193) | Base Paste: Silane-treated glass powder, 2-Propenoic acid, 2-methyl,1,1′-[1-(hydroxymethyl)-1,2-ethanodiyl] ester, triethylene glycol dimethacrylate (TEGDMA), silane-treated silica, glass fiber, sodium persulfate, and Tert-butyl peroxy-3,5,5-trimethylhexanoate. Catalyzer paste: Silane-treated glass powder, dimethacrylate substitute, silane-treated silica, Sodium p-toluenesulfonate, 1-Benzyl-5-phenylbarbituric acid, calcium salts, 1,12-Dodecanediol dimethacrylate, calcium hudroxide, and titanium dioxide. |
|
| BIFIX SE (Voco GmbH, Cuxhaven, Germany) Lot Number (1504155) | Base Paste: UDMA 25%, Bis-GMA 15%, Gli-DMA 10%, Kat N, N Bis 2%, Camphorquinone 1%, DABE 2%, BHT 0.1%, Glass Particles 39.9%, Silica 4.9%, and Ferric Oxide 0.1%. Catalyzer paste: UDMA 12%, Monomer BG 20%, Gli-DMA 20%, BHT 0.1%, DiHEMAPO4 1.9%, Glass Particles 38%, Silica 5%, BPO 50 FT 2%, and Titanium Dioxide 1%. |
|
| seT PP SDI, Bayswater, Australia) Lot Number (S1407381) | Phosphoric Methacrylate ester, UDMA, photoinitiator, Fluoroaluminosilicate, glass, and pyrogenic silica. |
|
| PANAVIA SA (Kuraray Medical, Inc, Tokyo, Japan) Lot Number (460039) | Base Paste: 10-Methacryloyloxydecyl dihydrogen phosphate (MDP), bisphenol A diglycidyl methacrylate (Bis-GMA), Triethylene Glycol Dimethacrylate (TEGDMA), hydrophobic dimethacrylate, 2-hydroxymethylmethacrylate, (HEMA), silanated barium, Silanated colloidal silica, dl-Camphorquinone, peroxide, catalyzers, and pigments. Catalyzer paste: Hydrophobic aromatic dimethacrylate, Hydrophobic aliphatic dimethacrylate, silinated barium, sodium fluoride, accelerators, and pigments. |
|
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lima, D.M.; Linhares, T.S.; Lima, S.N.L.; Carvalho, E.M.; Loguercio, A.D.; Bauer, J.; Carvalho, C.N. Effect of Sonic Application of Self-Adhesive Resin Cements on Push-Out Bond Strength of Glass Fiber Posts to Root Dentin. Materials 2019, 12, 1930. https://doi.org/10.3390/ma12121930
Lima DM, Linhares TS, Lima SNL, Carvalho EM, Loguercio AD, Bauer J, Carvalho CN. Effect of Sonic Application of Self-Adhesive Resin Cements on Push-Out Bond Strength of Glass Fiber Posts to Root Dentin. Materials. 2019; 12(12):1930. https://doi.org/10.3390/ma12121930
Chicago/Turabian StyleLima, Darlon Martins, Thátyla Silva Linhares, Suellen Nogueira Linares Lima, Edilausson Moreno Carvalho, Alessandro Dourado Loguercio, José Bauer, and Ceci Nunes Carvalho. 2019. "Effect of Sonic Application of Self-Adhesive Resin Cements on Push-Out Bond Strength of Glass Fiber Posts to Root Dentin" Materials 12, no. 12: 1930. https://doi.org/10.3390/ma12121930





