The Impact of Changes in Health and Social Care on Enteral Feeding in the Community
Abstract
:1. Introduction
2. Present State of Enteral Feeding in the Community

3. Main Factors Driving Changes in Health and Social Care in Relation to Enteral Feeding in the Community
4. What Are the Changes and the Implications for Enteral Feeding Practice in the Community?
- Integrating primary and secondary services (e.g., adding NNS to primary care teams, integrating health and social care). Integrating health and social care services is a useful strategy of managing changing demographics, enhancing the quality of patient care, improving innovation and development, and saving costs [23,24]. For example, the integration of Lewisham hospital NHS trust with Lewisham community health services which led to the formation of Lewisham healthcare NHS trust offers patients a continuous pathway of care through primary, community and hospital care [25]. This integration is useful for enteral feeding in the community in terms of managing the patients on HETF. In addition, enteral nutrition practitioners in the community can now effectively provide training for staff in the hospital and ensure better discharge arrangement for patients where there is no NNS in hospital settings and vice versa;
- changing location (e.g., providing care at home, intermediate care);
- substituting skills (e.g., service users for professionals, substituting nurses for other professionals and adding the skills of NNS);
- simplifying pathways;
- The Transforming Community Services’ (TCS) program includes rehabilitation of patients with long term neurological and other long term conditions who may be on HETF [24]. The TCS programs have involved mergers of Community Health NHS trusts and integration of acute with community services [20]. One of the strategies of bringing care closer home is the delivery of specialist care in community settings with the help of multidisciplinary teams such as the HEN service [9]. This will no doubt make the HEN services better accessible and convenient for patients in the community.
- Screening for malnutrition and risk of malnutrition;
- Nutritional assessment;
- Recording of nutritional information (e.g., nutritional status, goals, care plan and prescription);
- Nutritional prescription of total intake;
- Principles of treatment of underlying causes;
- Quality of documentation and audit;
- Continuity and consistency of care.
5. Challenges and Opportunities Resulting from Changes in Health and Social Care
- ♦ Finding out about professional indemnity/professional code of conduct for the different disciplines (NNS, Dietitian, Speech and Language Therapist–SLT);
- ♦ Agreeing what tasks can safely be shared between disciplines, e.g., application of MDT assessment tool, weighing patients and checking enteral feeding tubes;
- ♦ Deciding what knowledge, skills and competencies are needed and developing a framework for these;
- ♦ Training, support and supervision amongst members of the team (including 6 monthly in-service training day);
- ♦ Multidisciplinary clinical audit and research;
- ♦ Journal club;
- ♦ Team charter and weekly caseload meetings.
6. The Future of Enteral Feeding in the Community
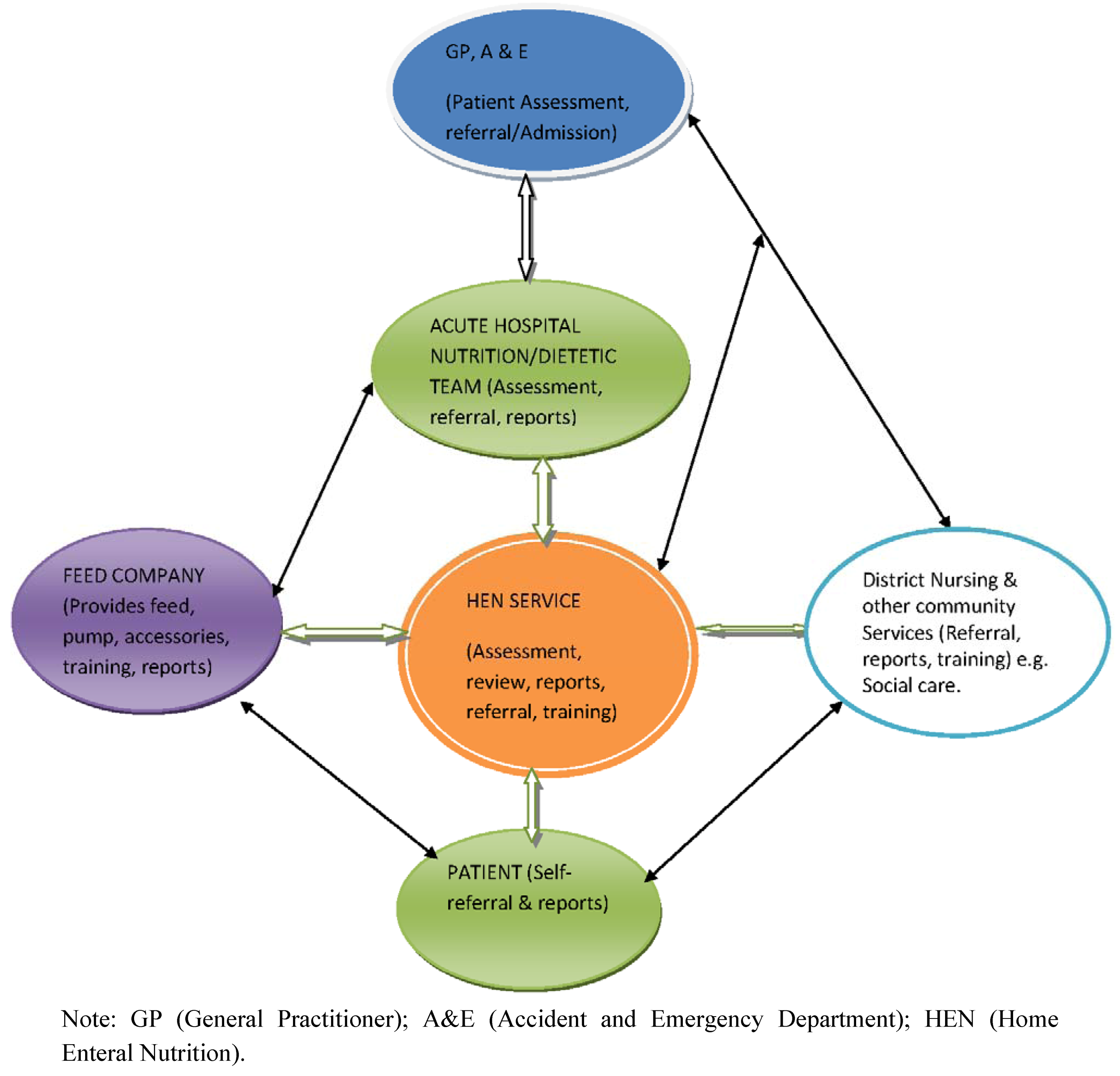
7. Conclusion
8. Recommendations
- ♦ Develop a national framework for HEN service including the establishment of effective HEN team in all Community Services;
- ♦ Provide training opportunities for healthcare professionals (HCPs) working in the area of enteral feeding in the community and ensure that the funding arrangements for training is incorporated into service level agreements;
- ♦ Ensure adequate training of patients by specialist HCPs so that the patients can be independent in managing their own enteral feeding in the community;
- ♦ Extend the roles of HCPs including increasing the number of independent prescribers amongst HCPs who should be able to prescribe medicines, feeds and enteral nutrition supplements and accessories.
Acknowledgements
Conflicts of Interest
References
- Shaping the Future NHS: Long Term Planning for Hospitals and Related Services; Department of Health (DH): London, UK, 2000. Available online: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4020470.pdf (accessed on 28 June 2012).
- Standards for Better Health; Department of Health: London, UK, 2004.
- 2008–2013 Action Plan for the Global Strategy for the Prevention and Control of Non-Communicable Diseases; World Health Organization (WHO): Geneva, Switzerland, 2008. Available online: http://whqlibdoc.who.int/publications/2009/9789241597418_eng.pdf (accessed on 4 July 2012).
- High Quality Care for All; Department of Health: London, UK, 2008. Available online: http://www.official-documents.gov.uk/document/cm74/7432/7432.pdf (accessed on 28 June 2012).
- Ojo, O. Managing patients on enteral feeding tubes in the community. Br. J. Community Nurs. 2010, 15, S6–S13. [Google Scholar]
- Ojo, O. Managing Diabetes in people on home enteral tube feeding. Diabetes Prim. Care 2012, 14, 113–119. [Google Scholar]
- Equity and Excellence: Liberating the NHS; Department of Health: London, UK, 2010. Available online: http://www.official-documents.gov.uk/document/cm78/7881/7881.pdf (accessed on 28 June 2012).
- Johnson, P.; Wistow, G.; Schulz, R.; Hardy, B. Interagency and interprofessional collaboration in community care. The interdependence of structures and values. J. Interprof. Care 2003, 17, 69–83. [Google Scholar]
- Shifting Care Closer to Home; Department of Health: London, UK, 2007. Available online: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_079801.pdf (accessed on 28 June 2012).
- Making the Shift: Key Success Factors; NHS Institute for Innovation and Improvement: London, UK, 2006. Available online: http://www.bhamlive2.bham.ac.uk/Documents/college-social-sciences/social-policy/HSMC/publications/2006/Making-the-Shift-Key-Success-Factors.pdf (accessed on 28 June 2012).
- A Vision for Adult Social Care: Capable Communities and Active Citizens; Department of Health: London, UK, 2010. Available online: http://www.cpa.org.uk/cpa_documents/vision_for_social_care2010.pdf (accessed on 4 July 2012).
- The NMC Code of Professional Conduct: Standards for Conduct, Performance and Ethics; Nursing and Midwifery Council: London, UK, 2004.
- Hansson, A.; Friberg, F.; Segesten, K.; Gedda, B.; Mattsson, B. Two sides of the coin-General Practitioners’ experience of working in multidisciplinary teams. J. Interprof. Care 2008, 22, 5–16. [Google Scholar] [CrossRef]
- Nicholson, D.; Artz, S.; Armitage, A.; Fagan, J. Working relationships and outcomes in multidisciplinary collaborative practice settings. Child Youth Care Forum 2000, 29, 39–73. [Google Scholar] [CrossRef]
- Doyle, J. Barriers and facilitators of multidisciplinary team working: A review. Paediatr. Nurs. 2008, 20, 26–29. [Google Scholar]
- Howard, P.; Bowen, N. The challenges of innovation in the organization of home enteral tube feeding. J. Hum. Nutr. Dietet. 2001, 14, 3–11. [Google Scholar] [CrossRef]
- Agenda for Change; Department of Health: London, UK, 2004. Available online: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4099423.pdf (accessed on 30 October 2012).
- Health and Social Care Act explained; Department of Health: London, UK, 2012. Available online: http://www.dh.gov.uk/health/2012/06/act-explained/ (accessed on 23 October 2012).
- Nicholson, D. NHS Chief Executive’s Annual Report 2011/12; NHS: London, UK, 2012. Available online: https://www.wp.dh.gov.uk/health/files/2012/06/the-year-and-quarter-4-210612-gw-17802-PDF-2.33MB.pdf (accessed on 19 July 2012).
- The State of Health Care and Adult Social Care in England; Care Quality Commission: London, UK, 2011. Available online: http://www.cqc.org.uk/sites/default/files/media/documents/state_of_care_2010_11.pdf (accessed on 17 July 2012).
- Caring for People beyond Tomorrow; Social Services and Public Safety (DHSSPS): Belfast, Ireland, 2005. Available online: http://www.dhsspsni.gov.uk/primarycare05.pdf (accessed on 19 July 2012).
- Annual Mid-Year Population Estimates, 2010; Office for National Statistics: London, UK, 2011. Available online: http://www.ons.gov.uk/ons/rel/pop-estimate/population-estimates-for-uk--england-and-wales--scotland-and-northern-ireland/mid-2010-population-estimates/index.html (accessed on 30 October 2012).
- Briefing 240: A Stitch in Time-The Future Is Integration; NHS Partners Network, NHS Confederation: London, UK, 2012. Available online: http://www.nhsconfed.org/Publications/Documents/A_stitch_in_time_the_future_is_integration.pdf (accessed on 2 July 2012).
- Transforming Community Services Evidence for Change; Health Services Management Centre (HSMC) for Department of Health: London, UK, 2009. Available online: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/documents/digitalasset/dh_102309.pdf (accessed on 2 July 2012).
- Uniting Community Health Services and University Hospital Lewisham; Lewisham Healthcare NHS Trust: London, UK, 2012. Available online: http://www.lewisham.nhs.uk/ (accessed on 30 October 2012).
- Ham, C. What will the Health and Social Care Bill mean for the NHS in England? BMJ 2012, 344, e2159. [Google Scholar] [CrossRef]
- Lewis, S. Primary Care Trust Cluster discussions revealed. 2011. Available online: http://www.hsj.co.uk/5024886.article?referrer=e2 (accessed on 4 July 2012).
- Davies, E. The health and social care bill: 10 things for the Lords to consider. BMJ 2011, 343, d6082. [Google Scholar] [CrossRef]
- NICE Clinical Guideline 139. Infection: Prevention and Control of Healthcare Associated Infections (HCAIs) in Primary and Community Care; National Institute for Health and Clinical Excellence: London, UK, 2012.
- Infection Control: Prevention of Healthcare Associated Infection (HCAI) in Primary and Community Care; National Institute for Health and Clinical Excellence: London, UK, 2003.
- NICE Quality Standard: Nutrition Support in Adults Scope; National Institute for Health and Clinical Excellence: London, UK, 2012. Available online: http://www.nice.org.uk/media/CEE/80/NutritionSupportInAdultsScope.pdf (accessed on 5 July 2012).
- Draft Quality Standard for Nutrition Support in Adults; National Institute for Health and Clinical Excellence: London, UK, 2012. Available online: http://www.nice.org.uk/media/4C8/88/NutritionSupportInAdultsFinalConsultation.pdf (accessed on 30 October 2012).
- Jeong, S.Y.; Keatinge, D. Innovative leadership and management in a nursing home. J. Nurs. Manag. 2004, 12, 445–451. [Google Scholar] [CrossRef]
- Ojo, O. Balloon gastrostomy tubes for long-term feeding in the community. Br. J. Nurs. 2011, 20, 34–38. [Google Scholar]
- Ojo, O. Home Enteral Nutrition NICE Guidelines and Nutrition Support in primary care. Br. J. Community Nurs. 2010, 15, 116–120. [Google Scholar]
- Ojo, O. Evaluating Care: Home enteral nutrition. J. Community Nurs. 2010, 24, 18–25. [Google Scholar]
- Gullo, S.R.; Gerstle, D.S. Transformational leadership and hospital restructuring: A descriptive study. Policy Polit. Nurs. Pract. 2004, 5, 259–266. [Google Scholar] [CrossRef]
- Bjuresater, K.; Larsson, M.; Nordstrom, G.; Athlin, E. Cooperation in the care for patients with home enteral tube throughout the care trajectory: nurses perspectives. J. Clin. Nurs. 2008, 17, 3021–3029. [Google Scholar] [CrossRef]
- Jones, A. Multidisciplinary team working: Collaboration and conflict. Int. J. Ment. Health Nurs. 2006, 15, 19–28. [Google Scholar] [CrossRef]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Ojo, O. The Impact of Changes in Health and Social Care on Enteral Feeding in the Community. Nutrients 2012, 4, 1709-1722. https://doi.org/10.3390/nu4111709
Ojo O. The Impact of Changes in Health and Social Care on Enteral Feeding in the Community. Nutrients. 2012; 4(11):1709-1722. https://doi.org/10.3390/nu4111709
Chicago/Turabian StyleOjo, Omorogieva. 2012. "The Impact of Changes in Health and Social Care on Enteral Feeding in the Community" Nutrients 4, no. 11: 1709-1722. https://doi.org/10.3390/nu4111709



