Changes in Depressive Symptoms among Older Adults with Multiple Chronic Conditions: Role of Positive and Negative Social Support
Abstract
:1. Introduction
2. Material and Methods
2.1. Sample and Design
2.2. Measures
2.3. Data Analysis
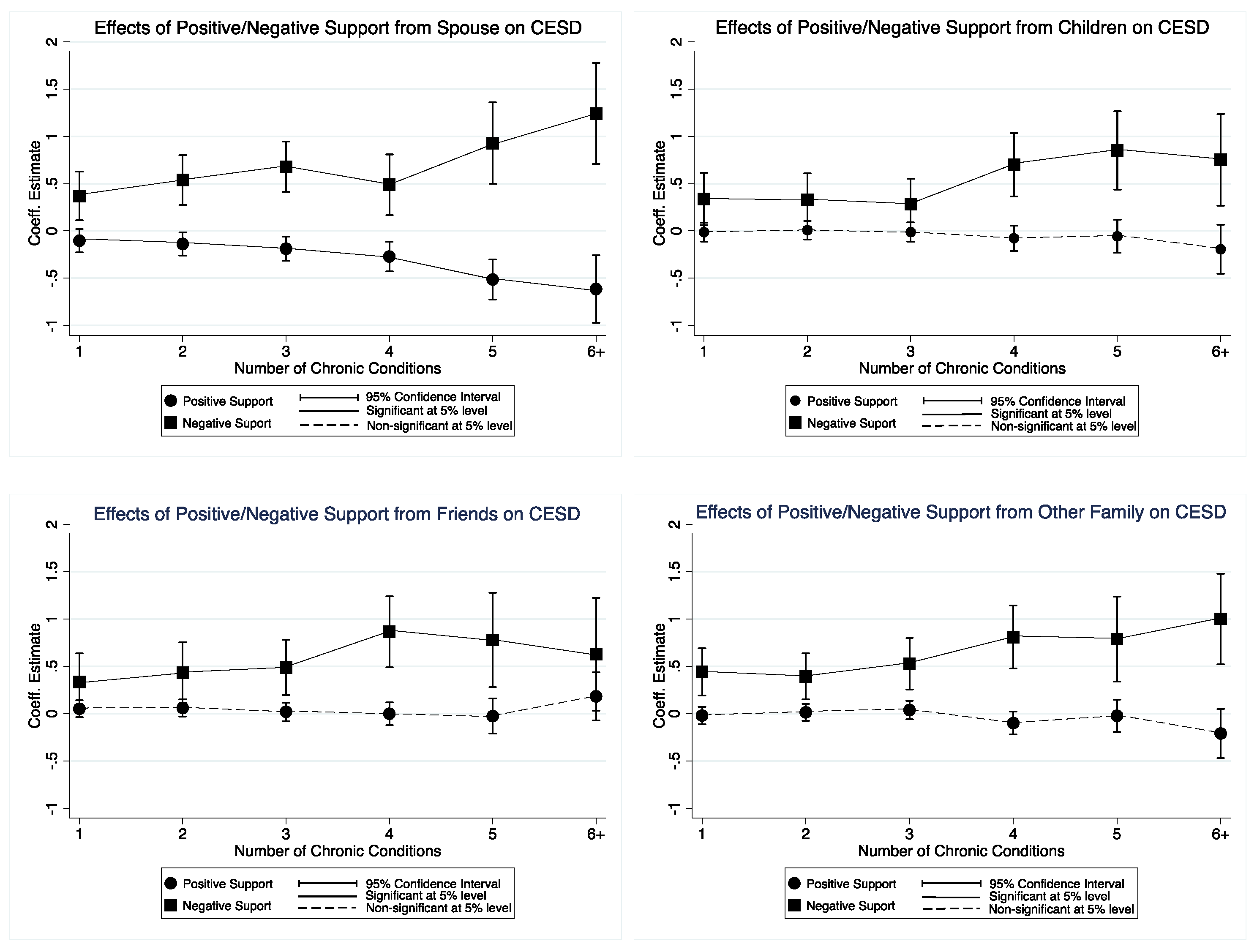
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Chapman, D.P.; Perry, G.S. Depression as a major component of public health for older adults. Prev. Chronic Dis. 2008, 5, 1–9. [Google Scholar]
- CDC. Depression Is Not a Normal Part of Growing Older; CDC: Atlanta, GA, USA, 2015. [Google Scholar]
- Heo, M.; Murphy, C.F.; Fontaine, K.R.; Bruce, M.L.; Alexopoulos, G.S. Population projection of U.S. adults with lifetime experience of depressive disorder by age and sex from year 2005 to 2050. Int. J. Geriatr. Psychiatry 2008, 23, 1266–1270. [Google Scholar] [CrossRef] [PubMed]
- Blazer, D.G. Depression in late life: Review and commentary. Biol. Sci. Med. Sci. 2003, 58, M249–M265. [Google Scholar] [CrossRef]
- Lockwood, K.A.; Alexopoulos, G.S.; van Gorp, W.G. Executive dysfunction in geriatric depression. Am. J. Psychiat. 2002, 159, 1119–1126. [Google Scholar] [CrossRef] [PubMed]
- Fiske, A.; Wetherell, J.L.; Gatz, M. Depression in older adults. Ann. Rev. Clin. Psychol. 2009, 5, 363–389. [Google Scholar] [CrossRef] [PubMed]
- Brett, C.E.; Gow, A.J.; Corley, J.; Pattie, A.; Starr, J.M.; Deary, I.J. Psychosocial factors and health as determinants of quality of life in community-dwelling older adults. Qual. Life Res. 2012, 21, 505–516. [Google Scholar] [CrossRef] [PubMed]
- U.S. Census Bureau. The Next Four Decades—The Older Population in the United States: 2010 to 2050; U.S. Census Bureau: Washington, DC, USA, 2010. [Google Scholar]
- Reynolds, C.F., III; Cuijpers, P.; Patel, V.; Cohen, A.; Dias, A.; Chowdhary, N.; Okereke, O.I.; Dew, M.A.; Anderson, S.J.; Mazumdar, S. Early intervention to reduce the global health and economic burden of major depression in older adults. Ann. Rev. Public Health 2012, 33, 123–135. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Donohue, J.M.; Pincus, H.A. Reducing the societal burden of depression. Pharmacoeconomics 2007, 25, 7–24. [Google Scholar] [CrossRef] [PubMed]
- Egede, L.E. Major depression in individuals with chronic medical disorders: Prevalence, correlates and association with health resource utilization, lost productivity and functional disability. Gen. Hosp. Psychiatry 2007, 29, 409–416. [Google Scholar] [CrossRef] [PubMed]
- Emptage, N.P.; Sturm, R.; Robinson, R.L. Depression and comorbid pain as predictors of disability, employment, insurance status, and health care costs. Psychiatry Serv. 2005, 56, 468–474. [Google Scholar] [CrossRef] [PubMed]
- Unützer, J. Late-life depression. N. Engl. J. Med. 2007, 357, 2269–2276. [Google Scholar] [CrossRef] [PubMed]
- DiNapoli, E.A.; Scogin, F.R. Late-Life Depression; Oxford University Press: London, UK, 2014; p. 412. [Google Scholar]
- Felger, J.C.; Haroon, E.; Miller, A.H. Risk and resilience: Animal models shed light on the pivotal role of inflammation in individual differences in stress-induced depression. Biol. Psychiatry 2015, 78, 7–9. [Google Scholar] [CrossRef] [PubMed]
- Köhler, O.; Petersen, L.; Mors, O.; Gasse, C. Inflammation and depression: Combined use of selective serotonin reuptake inhibitors and nsaids or paracetamol and psychiatric outcomes. Brain Behav. 2015, 5. [Google Scholar] [CrossRef] [PubMed]
- Marmorstein, N.R.; Iacono, W.G.; Legrand, L. Obesity and depression in adolescence and beyond: Reciprocal risks. Int. J. Obes. 2014, 38, 906–911. [Google Scholar] [CrossRef] [PubMed]
- Strine, T.W.; Mokdad, A.H.; Dube, S.R.; Balluz, L.S.; Gonzalez, O.; Berry, J.T.; Manderscheid, R.; Kroenke, K. The association of depression and anxiety with obesity and unhealthy behaviors among community-dwelling U.S. adults. Gen. Hosp. Psychiatry 2008, 30, 127–137. [Google Scholar] [CrossRef] [PubMed]
- Gold, D.T.; Solimeo, S. Osteoporosis and depression: A historical perspective. Curr. Osteoporos. Rep. 2006, 4, 134–139. [Google Scholar] [CrossRef]
- Wu, Q.; Magnus, J.H.; Liu, J.; Bencaz, A.F.; Hentz, J.G. Depression and low bone mineral density: A meta-analysis of epidemiologic studies. Osteoporos. Int. 2009, 20, 1309–1320. [Google Scholar] [CrossRef] [PubMed]
- Kuzava, S.; Doyle, C.; Gustafsson, H.; Werner, E.; Monk, C. Inflammation and depression in pregnant adolescents with asthma. Brain Behav. Immun. 2014, 40, e48–e49. [Google Scholar] [CrossRef]
- Mancuso, C.A.; Westermann, H.; Choi, T.N.; Wenderoth, S.; Briggs, W.M.; Charlson, M.E. Psychological and somatic symptoms in screening for depression in asthma patients. J. Asthma 2008, 45, 221–225. [Google Scholar] [CrossRef] [PubMed]
- Sale, J.E.M.; Gignac, M.; Hawker, G. The relationship between disease symptoms, life events, coping and treatment, and depression among older adults with osteoarthritis. J. Rheumatol. 2008, 35, 335–342. [Google Scholar] [PubMed]
- Golden, S.H.; Lazo, M.; Carnethon, M.; Bertoni, A.G.; Schreiner, P.J.; Roux, A.V.D.; Lee, H.B.; Lyketsos, C. Examining a bidirectional association between depressive symptoms and diabetes. JAMA 2008, 299, 2751–2759. [Google Scholar] [CrossRef] [PubMed]
- Maraldi, C.; Volpato, S.; Penninx, B.W.; Yaffe, K.; Simonsick, E.M.; Strotmeyer, E.S.; Cesari, M.; Kritchevsky, S.B.; Perry, S.; Ayonayon, H.N. Diabetes mellitus, glycemic control, and incident depressive symptoms among 70- to 79-year-old persons: The health, aging, and body composition study. Arch. Int. Med. 2007, 167, 1137–1144. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Ford, E.S.; Strine, T.W.; Mokdad, A.H. Prevalence of depression among U.S. adults with diabetes findings from the 2006 behavioral risk factor surveillance system. Diabetes Care 2008, 31, 105–107. [Google Scholar] [CrossRef] [PubMed]
- Krishnan, K.R.R.; Tupler, L.A.; Ritchie, J.C.; McDonald, W.M.; Knight, D.L.; Nemeroff, C.B.; Carroll, B.J. Apolipoprotein E-ε4 frequency in geriatric depression. Biol. Psychiatry 1996, 40, 69–71. [Google Scholar] [CrossRef]
- Pan, A.; Sun, Q.; Okereke, O.I.; Rexrode, K.M.; Hu, F.B. Depression and risk of stroke morbidity and mortality: A meta-analysis and systematic review. JAMA 2011, 306, 1241–1249. [Google Scholar] [CrossRef] [PubMed]
- Fann, J.R.; Fan, M.-Y.; Unützer, J. Improving primary care for older adults with cancer and depression. J. Gen. Int. Med. 2009, 24, 417–424. [Google Scholar] [CrossRef] [PubMed]
- Bosworth, H.B.; Bartash, R.M.; Olsen, M.K.; Steffens, D.C. The association of psychosocial factors and depression with hypertension among older adults. Int. J. Geriatr. Psychiatry 2003, 18, 1142–1148. [Google Scholar] [CrossRef] [PubMed]
- Bogner, H.R.; de Vries, H.F. Integration of depression and hypertension treatment: A pilot, randomized controlled trial. Ann. Fam. Med. 2008, 6, 295–301. [Google Scholar] [CrossRef] [PubMed]
- Yen, I.H.; Syme, S.L. The social environment and health: A discussion of the epidemiologic literature. Ann. Rev. Public Health 1999, 20, 287–308. [Google Scholar] [CrossRef] [PubMed]
- Ouellete Kobasa, S.C.; Spinetta, J.J.; Cohen, J.; Crano, W.D.; Hatchett, S.; Kaplan, B.H.; Lansky, S.B.; Prout, M.N.; Ruckdeschel, J.C.; Siegel, K. Social environment and social support. Cancer 1991, 67, 788–793. [Google Scholar] [CrossRef]
- Holtfreter, K.; Reisig, M.D.; Turanovic, J.J. Self-rated poor health and loneliness in late adulthood: Testing the moderating role of familial ties. Adv. Life Course Res. 2015, 27, 61–68. [Google Scholar] [CrossRef]
- Cornwell, E.Y.; Waite, L.J. Social disconnectedness, perceived isolation, and health among older adults. Health Soc. Behav. 2009, 50, 31–48. [Google Scholar] [CrossRef]
- Krause, N. Social support, stress, and well-being among older adults. J. Gerontol. 1986, 41, 512–519. [Google Scholar] [CrossRef] [PubMed]
- Penninx, B.W.J.H.; Van Tilburg, T.; Deeg, D.J.H.; Kriegsman, D.M.W.; Boeke, A.J.P.; Van Eijk, J.T.M. Direct and buffer effects of social support and personal coping resources in individuals with arthritis. Soc. Sci. Med. 1997, 44, 393–402. [Google Scholar] [CrossRef]
- Nolen-Hoeksema, S.; Ahrens, C. Age differences and similarities in the correlates of depressive symptoms. Psychol. Aging 2002, 17, 116–124. [Google Scholar] [CrossRef] [PubMed]
- George, L.K.; Blazer, D.G.; Hughes, D.C.; Fowler, N. Social support and the outcome of major depression. Br. J. Psychiatry 1989, 154, 478–485. [Google Scholar] [CrossRef]
- Kristof, L.; Fortinsky, R.H.; Kellett, K.; Porter, M.; Robison, J. Experiences of informal caregivers of older adults transitioned from nursing homes to the community through the money follows the person demonstration. J. Aging Soc. Policy 2016. [Google Scholar] [CrossRef] [PubMed]
- Adelman, R.D.; Tmanova, L.L.; Delgado, D.; Dion, S.; Lachs, M.S. Caregiver burden: A clinical review. JAMA 2014, 311, 1052–1060. [Google Scholar] [CrossRef] [PubMed]
- Wallace, R.B.; Herzog, A.R. Overview of the health measures in the health and retirement study. J. Hum. Resour. 1995, 30, S84–S107. [Google Scholar] [CrossRef]
- Chopik, W.J.; Kim, E.S.; Smith, J. Changes in optimism are associated with changes in health over time among older adults. Soc. Psychol. Personal. Sci. 2015, 6, 814–822. [Google Scholar] [CrossRef] [PubMed]
- Heeringa, S.G.; Connor, J. Technical Description of the Health and Retirement Study Sample Design; HRS/AHEAD Documentation Report DR-002; Institute for Social Research, University of Michigan: Ann Aebor, MI, USA, 1995. [Google Scholar]
- National Institute on Aging. Growing Oldear in America: The Health and Retirement Study; National Institute on Aging: Bethesda, MD, USA, 2007. [Google Scholar]
- Townsend, A.L.; Miller, B.; Guo, S. Depressive symptomatology in middle-aged and older married couples a dyadic analysis. Psychol. Sci. Soc. Sci. 2001, 56, S352–S364. [Google Scholar] [CrossRef]
- Radloff, L.S. The CES-D scale a self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Hann, D.; Winter, K.; Jacobsen, P. Measurement of depressive symptoms in cancer patients: Evaluation of the center for epidemiological studies depression scale (CES-D). J. Psychosom. Res. 1999, 46, 437–443. [Google Scholar] [CrossRef]
- Yang, F.M.; Cazorla-Lancaster, Y.; Jones, R.N. Within-group differences in depression among older hispanics living in the United States. Psychol. Sci. Soc. Sci. 2008, 63, P27–P32. [Google Scholar] [CrossRef]
- Lewinsohn, P.M.; Seeley, J.R.; Roberts, R.E.; Allen, N.B. Center for epidemiologic studies depression scale (CES-D) as a screening instrument for depression among community-residing older adults. Psychol. Aging 1997, 12, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Zivin, K.; Llewellyn, D.J.; Lang, I.A.; Vijan, S.; Kabeto, M.U.; Miller, E.M.; Langa, K.M. Depression among older adults in the United States and England. Am. J. Geriatr. Psychiatry 2010, 18, 1036–1044. [Google Scholar] [CrossRef] [PubMed]
- Morrow-Howell, N.; Putnam, M.; Lee, Y.S.; Greenfield, J.C.; Inoue, M.; Chen, H. An investigation of activity profiles of older adults. Psychol. Sci. Soc. Sci. 2014. [Google Scholar] [CrossRef] [PubMed]
- Clarke, P.; Fisher, G.; House, J.; Smith, J.; Weir, D. Guide to Content of the HRS Psychosocial Leave-Behind Participant Lifestyle Questionnaires: 2004 and 2006; University of Michigan Survey Research Center: Ann Arbor, MI, USA, 2008. [Google Scholar]
- House, J.S.; Landis, K.R.; Umberson, D. Social relationships and health. Science 1988, 241, 540–545. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S. Social relationships and health. Am. Psychol. 2004, 59, 676–684. [Google Scholar] [CrossRef] [PubMed]
- Brock, R.L.; Lawrence, E. A longitudinal investigation of stress spillover in marriage: Does spousal support adequacy buffer the effects? J. Fam. Psychol. 2008, 22, 11–20. [Google Scholar] [CrossRef] [PubMed]
- Umberson, D.; Montez, J.K. Social relationships and health a flashpoint for health policy. J. Health Soc. Behav. 2010, 51, S54–S66. [Google Scholar] [CrossRef] [PubMed]
- De Jong Gierveld, J.; van Groenou, M.B.; Hoogendoorn, A.W.; Smit, J.H. Quality of marriages in later life and emotional and social loneliness. Psychol. Sci. Soc. Sci. 2009. [Google Scholar] [CrossRef] [PubMed]
- Revenson, T.A.; Deborah Majerovitz, S. The effects of chronic illness on the spouse. Social resources as stress buffers. Arthritis Rheum. 1991, 4, 63–72. [Google Scholar] [CrossRef]
- Maly, R.C.; Umezawa, Y.; Leake, B.; Silliman, R.A. Mental health outcomes in older women with breast cancer: Impact of perceived family support and adjustment. Psycho-Oncology 2005, 14, 535–545. [Google Scholar] [CrossRef] [PubMed]
- Roberts, S. 51% of women are now living without spouse. The New York Times, 16 January 2007. [Google Scholar]
- Martire, L.M.; Lustig, A.P.; Schulz, R.; Miller, G.E.; Helgeson, V.S. Is it beneficial to involve a family member? A meta-analysis of psychosocial interventions for chronic illness. Health Psychol. 2004, 23, 599–611. [Google Scholar] [CrossRef] [PubMed]
- Kiecolt-Glaser, J.K.; Newton, T.L. Marriage and health: His and hers. Psychol. Bull. 2001, 127, 472–503. [Google Scholar] [CrossRef] [PubMed]
- Fekete, E.M.; Stephens, M.A.P.; Druley, J.A.; Greene, K.A. Effects of spousal control and support on older adults’ recovery from knee surgery. J. Fam. Psychol. 2006, 20, 302–310. [Google Scholar] [CrossRef] [PubMed]
- Dean, A.; Kolody, B.; Wood, P. Effects of social support from various sources on depression in elderly persons. J. Health Soc. Behav. 1990, 31, 148–161. [Google Scholar] [CrossRef] [PubMed]
- Druley, J.A.; Townsend, A.L. Self-esteem as a mediator between spousal support and depressive symptoms: A comparison of healthy individuals and individuals coping with arthritis. Health Psychol. 1998, 17, 255–261. [Google Scholar] [CrossRef] [PubMed]
- Matire, L.M.; Stephens, M.A.P.; Druley, J.A.; Wojno, W.C. Negative reactions to received spousal care: Predictors and consequences of miscarried support. Health Psychol. 2002, 21, 167–176. [Google Scholar] [CrossRef]
- Korporaal, M.; van Groenou, M.I.B.; van Tilburg, T.G. Effects of own and spousal disability on loneliness among older adults. J. Aging Health 2008, 20, 306–325. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Teel, C.S.; Press, A.N.; Lindgren, C.L.; Nichols, E.G. Fatigue among elders in caregiving and noncaregiving roles. Western J. Nurs. Res. 1999, 21, 498–520. [Google Scholar] [CrossRef]
- Dura, J.R.; Haywood-Niler, E.; Kiecolt-Glaser, J.K. Spousal caregivers of persons with alzheimer’s and parkinson’s disease dementia: A preliminary comparison. Gerontologist 1990, 30, 332–336. [Google Scholar] [CrossRef] [PubMed]
- Lavela, S.L.; Ather, N. Psychological health in older adult spousal caregivers of older adults. Chronic Ill. 2010, 6, 67–80. [Google Scholar] [CrossRef] [PubMed]
- Ahn, S.; Hochhalter, A.K.; Moudouni, D.K.M.; Smith, M.L.; Ory, M.G. Self-reported physical and mental health of older adults: The roles of caregiving and resources. Maturitas 2012, 71, 62–69. [Google Scholar] [CrossRef] [PubMed]
- Johannesen, M.; LoGiudice, D. Elder abuse: A systematic review of risk factors in community-dwelling elders. Age Ageing 2013. [Google Scholar] [CrossRef] [PubMed]
- CDC. Elder Abuse Prevention; CDC: Atlanta, GA, USA, 2015. [Google Scholar]
- Dong, X.; Simon, M. Association between elder abuse and metabolic syndromes: Findings from the Chicago Health and Aging Project. Gerontology 2015, 61, 389–398. [Google Scholar] [CrossRef] [PubMed]
- Luu, A.D.; Liang, B.A. Clinical case management; a strategy to coordinate detection, reporting, and prosecution of elder abuse. Cornell J. Law Public Policy 2005, 15, 165–196. [Google Scholar]
- Lachs, M.S.; Williams, C.S.; O’Brien, S.; Pillemer, K.A. Adult protective service use and nursing home placement. Gerontologist 2002, 42, 734–739. [Google Scholar] [CrossRef] [PubMed]
- Ezzati, M.; Martin, H.; Skjold, S.; Vander Hoorn, S.; Murray, C.J.L. Trends in national and state-level obesity in the USA after correction for self-report bias: Analysis of health surveys. J. R. Soc. Med. 2006, 99, 250–257. [Google Scholar] [CrossRef] [PubMed]
| Variables | 2006 (n = 11,400) | 2008 (n = 11,349) | 2010 (n = 10,950) | 2012 (n = 10,747) | p-Value |
|---|---|---|---|---|---|
| Mean (SD) | |||||
| CESD depression (0–8) | 1.48 (1.93) | 1.41 (1.91) | 1.34 (1.86) | 1.39 (1.89) | <0.001 |
| Number of chronic conditions (0–6) | 2.37 (1.42) | 2.48 (1.44) | 2.59 (1.43) | 2.71 (1.45) | <0.001 |
| Positive social support | |||||
| From spouse (1–4) | 2.94 (1.01) | 2.95 (1.02) | 3.02 (0.99) | 2.97 (1.00) | 0.2147 |
| From children (1–4) | 2.70 (1.04) | 2.71 (1.05) | 2.68 (1.04) | 2.69 (1.04) | 0.7066 |
| From other family (1–4) | 2.23 (1.04) | 2.26 (1.04) | 2.22 (1.05) | 2.25 (1.04) | 0.3899 |
| From friends (1–4) | 2.21 (1.05) | 2.24 (1.06) | 2.21 (1.04) | 2.25 (1.06) | 0.0784 |
| Negative social support | |||||
| From spouse (1–4) | 1.55 (0.48) | 1.55 (0.50) | 1.54 (0.48) | 1.54 (0.48) | 0.5833 |
| From children (1–4) | 1.41 (0.42) | 1.39 (0.42) | 1.40 (0.43) | 1.39 (0.43) | 0.1192 |
| From other family (1–4) | 1.33 (0.41) | 1.32 (0.42) | 1.32 (0.42) | 1.32 (0.43) | 0.2399 |
| From friends (1–4) | 1.27 (0.34) | 1.25 (0.32) | 1.26 (0.32) | 1.26 (0.34) | 0.1206 |
| CESD Depression | Positive Support | Negative Support | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Coef. | p-Value | 95% CI | Coef. | p-Value | 95% CI | |||||
| Model 1 | Spouse | Model 2 | Spouse | |||||||
| MCC | 0.489 | <0.001 | 0.387 | 0.591 | 0.033 | 0.489 | −0.060 | 0.125 | ||
| Support from spouse | −0.110 | 0.005 | −0.186 | −0.033 | 0.115 | 0.152 | −0.042 | 0.273 | ||
| MCC × Support from spouse | −0.071 | <0.001 | −0.103 | −0.039 | 0.155 | <0.001 | 0.098 | 0.212 | ||
| Intercept | 0.912 | 0.001 | 0.398 | 1.426 | 0.142 | 0.575 | −0.353 | 0.636 | ||
| R-squared | 0.1513 | 0.1474 | ||||||||
| Model 3 | Children | Model 4 | Children | |||||||
| MCC | 0.367 | <0.001 | 0.294 | 0.439 | 0.112 | 0.007 | 0.031 | 0.193 | ||
| Support from children | −0.148 | <0.001 | −0.205 | −0.090 | 0.162 | 0.042 | 0.006 | 0.318 | ||
| MCC × Support from children | −0.017 | 0.166 | −0.040 | 0.007 | 0.141 | <0.001 | 0.086 | 0.196 | ||
| Intercept | 0.218 | 0.284 | −0.181 | 0.618 | −0.324 | 0.156 | −0.772 | 0.124 | ||
| R-squared | 0.1306 | 0.1374 | ||||||||
| Model 5 | Other family | Model 6 | Other family | |||||||
| MCC | 0.340 | <0.001 | 0.280 | 0.400 | 0.084 | 0.034 | 0.006 | 0.161 | ||
| Support from other family | −0.054 | 0.050 | −0.109 | 0.000 | 0.091 | 0.231 | −0.058 | 0.240 | ||
| MCC × Support from other family | −0.018 | 0.118 | −0.041 | 0.005 | 0.163 | <0.001 | 0.107 | 0.219 | ||
| Intercept | 0.330 | 0.097 | −0.059 | 0.719 | −0.057 | 0.797 | −0.488 | 0.375 | ||
| R-squared | 0.1196 | 0.1341 | ||||||||
| Model 7 | Friend | Model 8 | Friend | |||||||
| MCC | 0.298 | <0.001 | 0.241 | 0.354 | 0.111 | 0.01 | 0.027 | 0.196 | ||
| Support from friend | −0.047 | 0.09 | −0.101 | 0.007 | 0.049 | 0.601 | −0.135 | 0.234 | ||
| MCC × Support from friend | 0.004 | 0.713 | −0.019 | 0.027 | 0.151 | <0.001 | 0.087 | 0.216 | ||
| Intercept | 0.231 | 0.253 | −0.165 | 0.628 | −0.091 | 0.682 | −0.530 | 0.347 | ||
| R-squared | 0.1133 | 0.1208 | ||||||||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ahn, S.; Kim, S.; Zhang, H. Changes in Depressive Symptoms among Older Adults with Multiple Chronic Conditions: Role of Positive and Negative Social Support. Int. J. Environ. Res. Public Health 2017, 14, 16. https://doi.org/10.3390/ijerph14010016
Ahn S, Kim S, Zhang H. Changes in Depressive Symptoms among Older Adults with Multiple Chronic Conditions: Role of Positive and Negative Social Support. International Journal of Environmental Research and Public Health. 2017; 14(1):16. https://doi.org/10.3390/ijerph14010016
Chicago/Turabian StyleAhn, SangNam, Seonghoon Kim, and Hongmei Zhang. 2017. "Changes in Depressive Symptoms among Older Adults with Multiple Chronic Conditions: Role of Positive and Negative Social Support" International Journal of Environmental Research and Public Health 14, no. 1: 16. https://doi.org/10.3390/ijerph14010016






