1. Introduction
Sick building syndrome (SBS) is a medical condition in which people in a building suffer from symptoms of illness or feeling unwell for no apparent reasons [
1]. The symptoms tend to increase in severity as a function of time spent in the building and improve over time or even disappear when people are away from the building [
1]. A variety of factors in the home environment are related to SBS [
2,
3,
4]. Indoor volatile organic compounds (VOCs) and their relationship to SBS were demonstrated in studies at nonmanufacturing workplaces [
3,
5,
6]. In addition, SBS was observed at indoor ambient air levels greater than 21.3, 15.5, 4.40, 3.90, 4.60, 3.80, 4.60 and 8.20 μg/m
3 for formaldehyde (HCHO), NO
2, butyl acetate, ethylbenzene, α-pinene,
p-dichlorobenzene, nonanal and xylene, respectively [
2,
6,
7]. However, for butanol, methyl isobutyl ketone, styrene, and toluene, no symptoms were reported at 4.20–190.2, 3.80–44.1, 4.70–171.3 and 3.00–3,104.7 μg/m
3, respectively [
2].
The home indoor environment is considered an important factor affecting health [
2,
4,
8,
9,
10,
11,
12,
13]. In recent years, indoor air pollution by interior decoration materials has become a major health problem in China; symptoms related to the nervous system or respiratory organs among inhabitants in Wuhan, Beijing, Ningbo and Taiyuan have been widely reported [
7,
10,
11,
12,
13]. Indoor air pollution, thus, has become a strong public concern in China. The present study reports subjective symptoms in the past and at the time of study, in relation to indoor concentrations of HCHO, VOCs, and NO
2 at the time of study. The health effects among residents in the dwellings with low levels of exposures were investigated.
3. Results and Discussion
Indoor air concentrations of HCHO, VOCs, and NO
2 in 59 houses are shown in
Table 2. Among substances with exposure limit values (
Table 1), HCHO concentrations exceeded the exposure limit (100 μg/m
3) in one bedroom (272 μg/m
3) and in one kitchen (167 μg/m
3). The number and percentage of the values under the exposure limits are listed in
Appendix 1. Point estimation and 95% confidence intervals of median concentrations are shown in
Appendix 2. None of other substances with exposure limits (
Table 1) showed indoor air concentrations greater than the exposure limits. Reasons for high HCHO levels observed could not be elucidated in this study.
Table 2.
Indoor concentrations a of HCHO, VOCs, and NO2 in 59 houses in Dalian, China (μg/m3, 5–23 August 2007).
Table 2.
Indoor concentrations a of HCHO, VOCs, and NO2 in 59 houses in Dalian, China (μg/m3, 5–23 August 2007).
| | Bedroom b | Kitchen b | Outdoor c | Detection limit |
|---|
| Median d | Range | Median d | Range | Median d | Range |
|---|
| Formaldehyde (HCHO) | 29 | 13–272 | 30.6 | 13–167 | 14 | <DL–40 | 15 |
| VOC (total) | 67.9 | 36.5–202 | 66.3 | 37.3–260 | 54.5 | 35.0–101 | 5.6 |
| Benzene (C6H6) | 2.4 | <DL–15.7 | 2.8 | <DL–32.4 | 2.5 | <DL–5.5 | 1.0 |
| Butanol (C4H10O) | 9.8 | <DL–65.2 | 8.6 | <DL–61.1 | 5.3 | <DL–10.5 | 4.4 |
| Butyl acetate (C6H12O2) | 3.7 | <DL–27.3 | 3.6 | <DL–31.7 | 3.07 | <DL–12.4 | 1.1 |
| Carbon tetrachloride (CCl4) | 0.7 | <DL–1.8 | 0.9 | <DL–11.9 | 0.7 | <DL–1.8 | 0.5 |
| Chloroform (CHCl3) | <DL | <DL–2.3 | <DL | <DL–2.2 | <DL | <DL–1.8 | 1.6 |
| 1,2-Dichloroethane (C2H4Cl2) | 1.0 | <DL–65.4 | 1.1 | <DL–11.3 | 1.0 | <DL–3.1 | 0.5 |
| p-Dichlorobenzene | <DL | <DL–111 | <DL | <DL–59.0 | <DL | <DL–8.5 | 0.5 |
| (C6 H4Cl2) |
| Ethyl acetate (C4H8O2) | <DL | <DL–<DL | <DL | <DL–<DL | <DL | <DL–<DL | 41 |
| Hexane (C6H14) | 1.5 | <DL–6.3 | 1.59 | <DL–18.1 | 1.6 | <DL–4.0 | 0.4 |
| Methyl ethyl ketone | <DL | <DL–3.3 | <DL | <DL–3.3 | <DL | <DL–6.5 | 1.2 |
| (CH3COC2H5) |
| Methyl isobutyl ketone | <DL | <DL–1.4 | <DL | <DL–1.1 | <DL | <DL–0.8 | 0.4 |
| (CH3COCH2CH(CH3)2) |
| Styrene (C6H5C2H3) | <DL | <DL–2.3 | <DL | <DL–2.8 | <DL | <DL–1.7 | 0.8 |
| 1,1,1-Trichloroethane (CH3CCl3) | 0.6 | <DL–3.0 | 0.6 | <DL–1.1 | 0.6 | <DL–1.1 | 0.4 |
| Tetrachloroethylene (C2Cl4) | <DL | <DL–10.0 | <DL | <DL–16.1 | <DL | <DL–22.3 | 0.4 |
| Trichloroethylene (C2HCl3) | <DL | <DL–1.7 | <DL | <DL–<DL | <DL | <DL–<DL | 0.9 |
| Toluene (C6H5CH3) | 14.1 | 2.4–97.4 | 12.0 | 3.0–80.0 | 10.8 | 3.9–40.6 | 0.5 |
| o-Xylene (C8H10) | 1.8 | <DL–9.6 | 1.7 | <DL–39.7 | 1.4 | <DL–5.1 | 0.5 |
| p-Xylene (C8H10) | 5.7 | 0.7–23.6 | 6.5 | 1.0–111 | 5.4 | <DL–17.0 | 0.7 |
| Total xylenes (C8H10) | 7.3 | <DL–33.3 | 8.3 | 1.2–151 | 6.9 | <DL–22.1 | 1.2 |
| NO2 | 20.5 | <DL–72.1 | 40.0 | <DL–205 | 27.1 | <DL–78.2 | 5.6 |
Geometric mean, geometric standard deviation after log transformation, and 5th and 95th percentiles of HCHO, VOCs, and NO
2 concentrations are presented in
Table 3. For chemicals with exposure limit values in
Table 1, their 95th percentile values were less than the exposure limit. Therefore, residents were exposed to very low level of chemicals at the time of study.
Table 3.
Geometric mean concentrations (GM), geometric standard deviation (GSD) and 5th and 95th percentiles of HCHO, VOCs, and NO
2 inside the bedroom and kitchen in the sampled flats (calculated from
Table 2).
Table 3.
Geometric mean concentrations (GM), geometric standard deviation (GSD) and 5th and 95th percentiles of HCHO, VOCs, and NO2 inside the bedroom and kitchen in the sampled flats (calculated from Table 2).
| | Bedroom | Kitchen |
|---|
| GM | GSD | 5th percentile | 95th percentile | GM | GSD | 5th percentile | 95th percentile |
|---|
| HCHO | 33.5 | 1.73 | 16 | 82 | 32.3 | 1.70 | 14.9 | 91.0 |
| VOCs (total) | 74.1 | 1.56 | 37.5 | 187 | 73.5 | 1.45 | 43.3 | 154 |
| Benzene | 2.54 | 1.78 | 1.1 | 8.7 | 2.89 | 1.86 | 1.1 | 8.6 |
| Butanol | 9.03 | 2.06 | 2.2 | 34 | 8.62 | 1.77 | 2.2 | 20.9 |
| Butyl acetate | 3.69 | 2.14 | 1.2 | 16.4 | 3.51 | 1.98 | 1.1 | 11.3 |
| Carbon tetrachloride | 0.64 | 2.00 | 0.2 | 1.6 | 0.72 | 2.09 | 0.2 | 1.4 |
| Chloroform | 0.89 | 1.28 | 0.8 | 2.2 | 0.86 | 1.23 | 0.8 | 2.0 |
| 1,2-Dichloroethane | 1.38 | 2.97 | 0.3 | 17.9 | 1.29 | 2.11 | 0.6 | 5.9 |
| p-Dichlorobenzene | 0.49 | 3.89 | 0.3 | 17.7 | 0.46 | 3.16 | 20.3 | 8.6 |
| Hexane | 1.43 | 1.97 | 0.2 | 4.0 | 1.61 | 2.14 | 0.2 | 8.0 |
| Methyl ethyl ketone | 0.80 | 1.63 | 0.6 | 2.3 | 0.79 | 1.67 | 0.6 | 2.5 |
| Methyl isobutyl ketone | 0.35 | 1.87 | 0.2 | 0.9 | 0.33 | 1.88 | 0.2 | 0.9 |
| Styrene | 0.57 | 1.83 | 0.4 | 1.8 | 0.61 | 2.0 | 0.4 | 2.2 |
| 1,1,1-Trichloroethane | 0.52 | 1.98 | 0.2 | 1.0 | 0.52 | 1.85 | 0.2 | 1.0 |
| Tetrachloroethylene | 0.27 | 2.21 | 0.2 | 1.3 | 0.27 | 2.25 | 0.2 | 1.6 |
| Trichloroethylene | 0.49 | 1.23 | 0.5 | 0.5 | - | - | - | - |
| Toluene | 13.4 | 2.07 | 4.4 | 45.6 | 13.6 | 2.04 | 4.3 | 52.2 |
| o-Xylene | 1.68 | 2.38 | 0.3 | 7.9 | 1.68 | 2.47 | 0.3 | 6.6 |
| p-Xylene | 5.77 | 1.88 | 1.7 | 17.4 | 6.08 | 1.96 | 1.9 | 17.9 |
| Total xylenes | 7.28 | 2.16 | 1.4 | 25.4 | 7.81 | 2.07 | 2.1 | 24.6 |
| NO2 | 18.7 | 2.07 | 2.5 | 49.1 | 36.3 | 2.36 | 5.2 | 141 |
Table 4 shows a list of residents who had reported that they had experienced symptoms since their move into the flats. A total of seven males and 10 females had experienced symptoms in their bedrooms; three males and five females had experienced symptoms in their kitchens. Among them, two males and two females still experienced symptoms when in their bedrooms, and two females experienced symptoms when in their kitchens at the time of study.
Table 5 presents the subjective symptoms reported by these residents (males of code 5 and 8 reported that they experienced some symptom, but did not specify it).
Table 4.
A list of residents reported that they experienced some symptom because they moved into flats: before and during the sampling period.
Table 4.
A list of residents reported that they experienced some symptom because they moved into flats: before and during the sampling period.
| | Code | Age (year) | Period living in this flat. (months) | Bedroom | Kitchen |
|---|
| Before | During | Before | During |
|---|
| Males | | | | | | | |
| | 1 | 27 | 10 | + | + | | |
| | 2 | 30 | 29 | + | | + | |
| | 3 | 31 | 36 | + | | | |
| | 4 | 32 | 41 | + | | | |
| | 5 | 34 | 30 | + | + | + | |
| | 6 | 52 | 130 | + | | | |
| | 7 | 67 | 9 | + | | | |
| | 8 | NA | NA | | | + | |
| Females | | | | | | | |
| | 1 | 27 | NA | + | | | |
| | 2 | 30 | 29 | + | + | + | + |
| | 3 | 27 | 36 | + | | | |
| | 4 | 34 | 41 | + | | | |
| | 5 | 30 | 30 | + | + | + | + |
| | 6 | 52 | NA | + | | + | |
| | 7 | 64 | 9 | + | | | |
| | 9 | 36 | NA | + | | | |
| | 10 | 51 | 19 | + | | + | |
| | 11 | NA | NA | + | | + | |
Table 5.
Symptoms experienced after residents moved into their flats (shown by code in
Table 3).
Table 5.
Symptoms experienced after residents moved into their flats (shown by code in Table 3).
| | Bedroom | Kitchen |
|---|
| Males (n = 59) | Females (n = 50) | Males (n = 59) | Females (n = 50) |
|---|
| Feeling of heavy-headedness | | 1, 7 | | |
| Headache | 3 | 3, 5 a | | |
| Nausea | 3, 7 | 3 | | |
| Nightmare | | 2 a, 7 | | |
| Sleeplessness | 6 | 1, 6 | | |
| Feel dizzy when stand up | 7 | 1, 2 a, 6 | | 2 a |
| Fatigue | | 1, 2 a,5 a, 10 | | 2 a |
| Slight fever | | 10 | | |
| Painful eye | | 9, 10 | | 5 a |
| Feeling of collapse | | 2 a, 10 | | 2 a |
| Itchy eyes | 4 | 4 | | |
| Nasal irritation | 2 | 11 | 2 | 11 |
| Whistles | 6 | | | |
| Sore throat | | | | 5 a |
| Strange taste | 1 a, 2 | 9 | 2 | 5 a |
| Itchy skin | | | | 10 |
| Rash | | 5 a | | 10 |
| Muscle pain | 1 a | | | |
| Smell of paints and adhesives | 4 | 4 | 5 | |
Figure 1,
Figure 2,
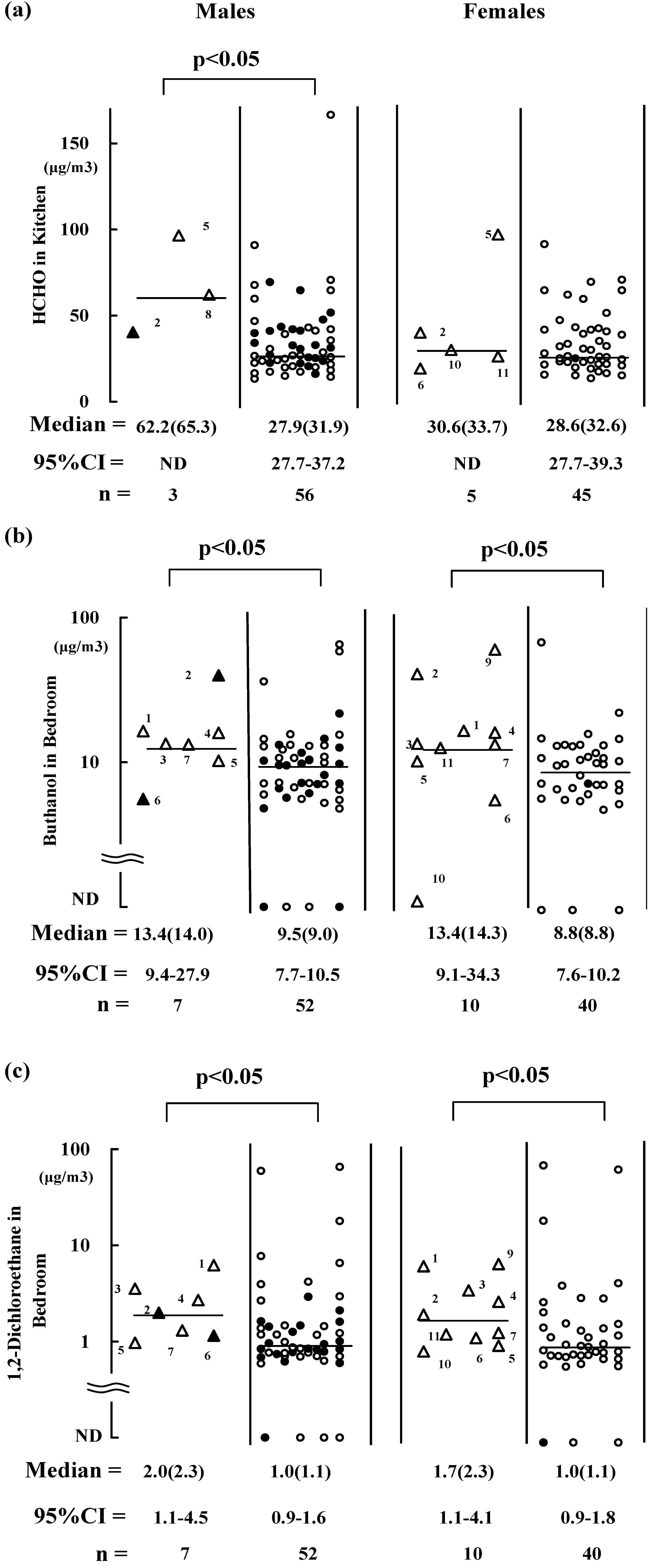
Figure 3 are presented to show the significant differences observed in indoor concentrations of chemicals between residents with and without symptoms before the sampling after they had moved into their flats or during the sampling. Residents with and without symptoms are indicated by triangles and circles, respectively (smokers are indicated as closed one). Three males experienced symptoms before the sampling in the kitchens where the median HCHO level was 62.2 μg/m
3 (
Figure 1(a)). Additionally, five females had symptoms before the sampling in the kitchens, although the present HCHO levels were not significantly elevated (
Figure 1(a)). No significant differences in indoor HCHO levels of the residents with symptoms were found compared with those without symptoms during the sampling (
p > 0.05, data not shown). Therefore, it has been suggested that HCHO levels before the sampling were greater than 60.0 μg/m
3, which has been reported to cause symptoms related to nervous or respiratory systems [
10] and that HCHO concentrations decreased with the aging of the sampled residences [
14].
Figure 1.
Air concentrations of HCHO, butanol, and 1, 2-dichloroethane in residences are shown in (a), (b), and (c), respectively. Residents with and without subjective symptoms after they moved into the flats are represented by (Δ,▲) and (○, ●), respectively (closed triangles and circles are smokers). Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
Figure 1.
Air concentrations of HCHO, butanol, and 1, 2-dichloroethane in residences are shown in (a), (b), and (c), respectively. Residents with and without subjective symptoms after they moved into the flats are represented by (Δ,▲) and (○, ●), respectively (closed triangles and circles are smokers). Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
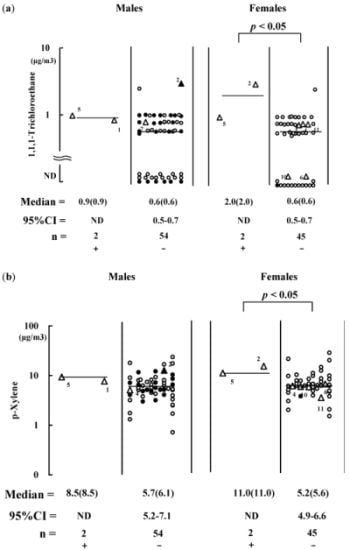
Figure 2.
Air concentrations of 1,1,1-trichloro-ethane (
a) and p-xylene (
b) in bedrooms. These values were compared between residents with (+) and without (−) symptoms during the sampling. Symbols are specified in
Figure 1. Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
Figure 2.
Air concentrations of 1,1,1-trichloro-ethane (
a) and p-xylene (
b) in bedrooms. These values were compared between residents with (+) and without (−) symptoms during the sampling. Symbols are specified in
Figure 1. Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
Figure 3.
Air concentrations of butanol (
a), methyl isobutyl ketone (
b), and styrene (
c) in kitchens. These values were compared between females with (+) and without (−) symptoms during the sampling. Symbols are specified in
Figure 1. Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
Figure 3.
Air concentrations of butanol (
a), methyl isobutyl ketone (
b), and styrene (
c) in kitchens. These values were compared between females with (+) and without (−) symptoms during the sampling. Symbols are specified in
Figure 1. Bar = median value. Point estimation of median is in parenthesis; 95% CI = 95% confidence interval. ND = not determined because of the small number of subjects.
Seven males and 10 females reported that they felt at least one of the symptoms when they were in their bedrooms before the sampling (
Figure 1(b,c)). The median butanol concentration in their bedrooms was 13.4 μg/m
3 for both males and females (
Figure 1(b)). This value was greater than the median butanol concentrations in the bedrooms in which the residents did not report any symptoms,
i.e., 9.53 μg/m
3 and 8.84 μg/m
3 for males and females, respectively (
Figure 1(b)). Among these 10 females, two (code 2 and 5) still had symptoms during the sampling in the kitchens where the median butanol level was 16.9 μg/m
3 (
Figure 3(a)). Therefore, relatively high-level exposure to butanol (
i.e., median 13–16.9 μg/m
3) might have caused the symptoms. Median values of 1,2-dichloroethane in the bedrooms (2.0 and 1.7 μg/m
3 for males and females, respectively) were significantly greater for those with symptoms before the sampling compared with those without symptoms (1.0 μg/m
3 ) (
Figure 1(c)), whereas a significantly elevated concentration of 1,2-dichloroethane was not observed for residents with symptoms during the sampling. It is also assumed that the concentration of 1,2-dichloroethane decreased with the aging of the sampled residences.
The two females (code 2 and 5) also had symptoms during the sampling related to elevated levels of 1,1,1-trichloroethane and p-xylene in the bedrooms,
i.e., at median levels of 2.00 and 11.0 μg/m
3, respectively (
Figure 2(a,b)). Two males (one was the husband of female code 5) complained of symptoms in the bedrooms, but their exposure to 1,1,1-trichloroethane and p-xylene levels were not significantly elevated (
Figure 2(a,b)). This might have been because the husband of female of code 2 did not manifest the symptom. The females (code 2 and 5) still had symptoms related to methyl isobutyl ketone and styrene in the kitchens, with median levels of 0.90 and 2.20 μg/m
3, respectively (
Figure 3(b,c)). Therefore, concentrations of butanol, 1,1,1-trichloroethane,
p-xylene, methyl isobutyl ketone and styrene were elevated for subjects with persisting symptoms most likely because these chemical concentrations did not rapidly decrease.
The subjective symptoms observed in the present study could be attributed to indoor chemicals. However, most of these chemical substances were detected at very low concentrations. The analysis was performed under a total-ion monitoring mode for some samples to detect all of the major peaks, followed by selected-ion monitoring mode to target the quantified VOCs, which did not reveal high levels of VOCs other than those reported here. To confirm that such low exposures can cause long-term adverse effects, further study is necessary. Several studies have reported that total VOC concentration was significantly related to symptoms of SBS [
2,
20,
21]. However, in the present study, no significant differences were observed in airborne total VOC between the rooms of participants with and without symptoms. Reasons for this discrepancy should be further studied. Additionally, short but higher-level exposure should be considered even though the measured average exposure level was low. In addition, decreases in air concentrations might have been caused by opened windows during the sampling.
Dampness is known to be associated with respiratory tract infections in dwellings [
22,
23,
24] and office buildings [
25]. It has been reported that environmental tobacco smoke [
26] is a risk for SBS symptoms. The effects of indoor dampness and environmental tobacco smoke on the health of residents should have been evaluated in the present study. The effects of indoor chemical substances on children should also be evaluated because it has been reported that childhood asthma is related to formaldehyde [
27,
28,
29] and VOC exposure [
30].