1. Introduction
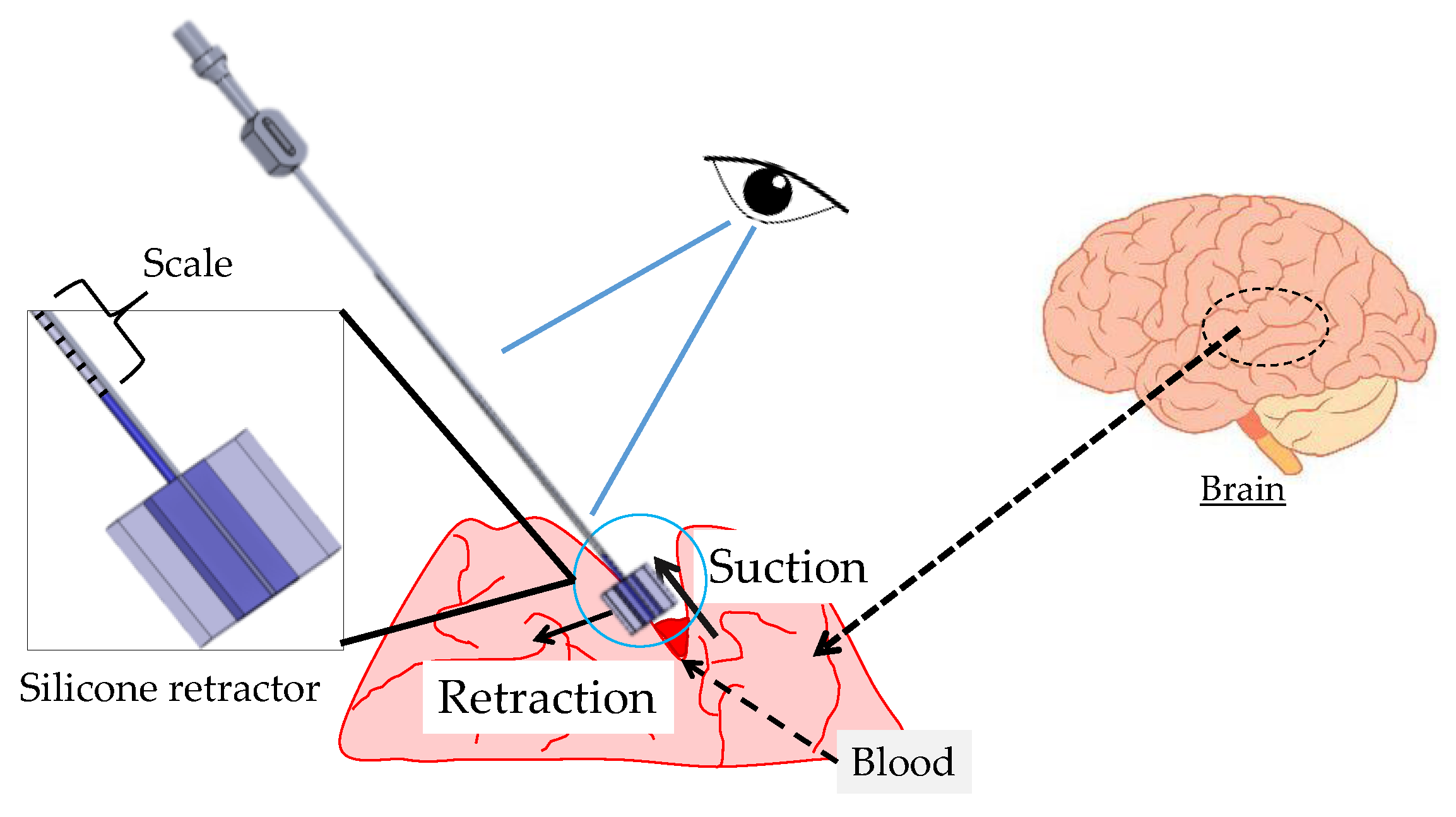
Retractors and suction devices are the most frequently used instruments in neurosurgery. Retractors are used to pull back tissues to produce a visible field and a space for surgeons. When retracting, an overload of retracting is a key issue. It could cause unexpected damage to brain tissues and bleeding. As the brain tissue is very soft and fragile, it can break or get damaged even with a small load. The brain is a very important organ in the human body, and any damage or injury to the brain tissue might led have serious consequences. Suction devices are mainly used to suck blood and saline for washing the brain tissue. They are also sometimes used for retracting tissues, although the retracting area is very small and limited in availability. If combining the functions of retraction and suction while avoiding the overload of retracting, surgeons can operate easily, safely, and speedily. With this in mind, we previously developed a force sensible silicone retractor that can be used by attaching it to the tip of a suction pipe [
1], as shown in
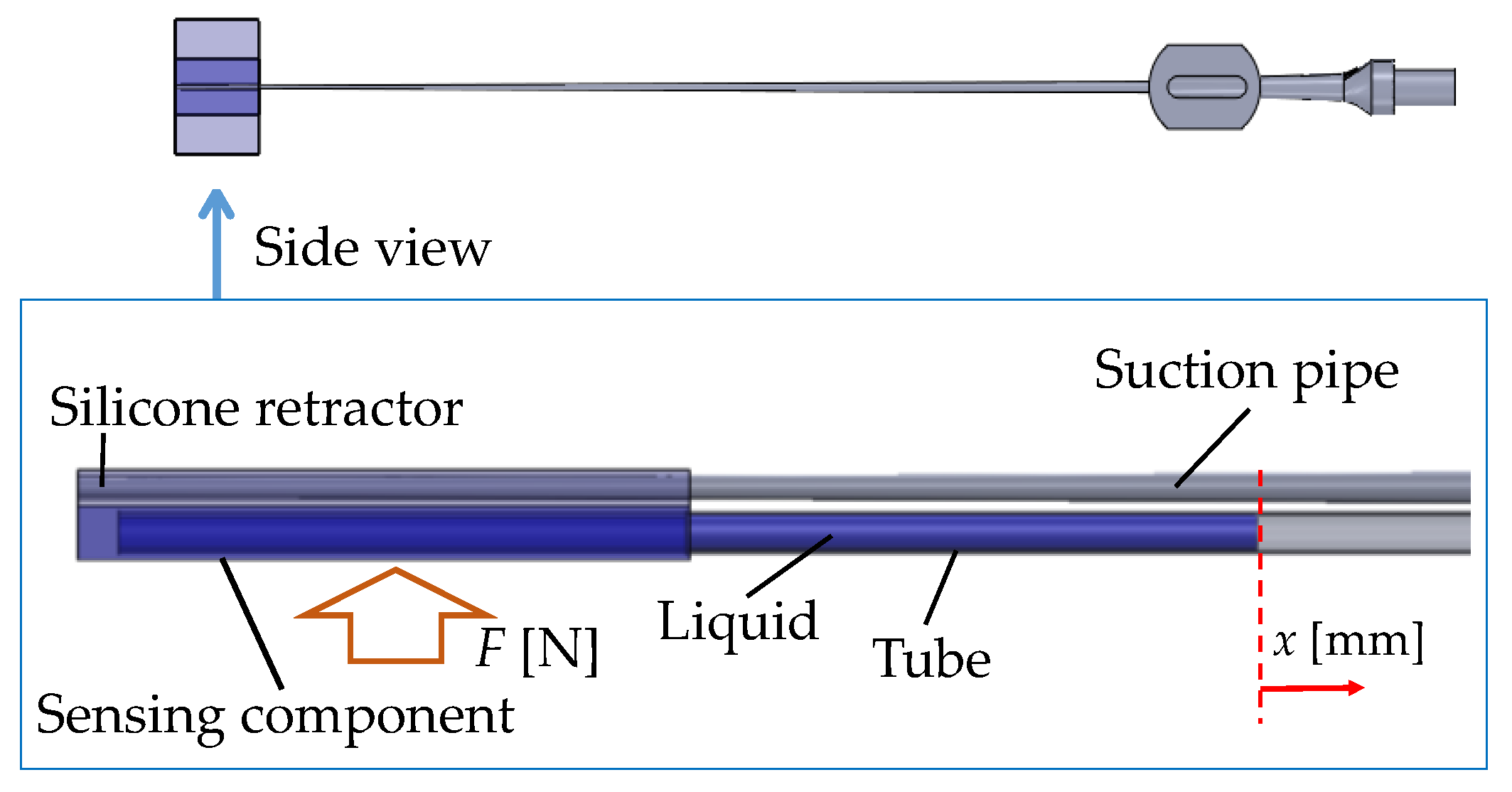
Figure 1. With this instrument, surgeons can perform the functions of suction, retraction, and force sensing, without changing instruments. However, the developed instrument has two drawbacks. First, available cases are limited due to its large thickness (4 mm). It was difficult to retract deep areas or to insert the instrument into narrow spaces; Second, the previously developed instrument has five independent force sensors. The distributed forces can be observed, although it is hard for surgeons to observe the separate force values simultaneously, and the space occupied by the five tubes for the sensors disturbs and reduces the usability of the instruments. With these points in mind, this paper presents an extended version of the silicone retractor that addresses these limitations. The key features of the new silicone retractor include the following:
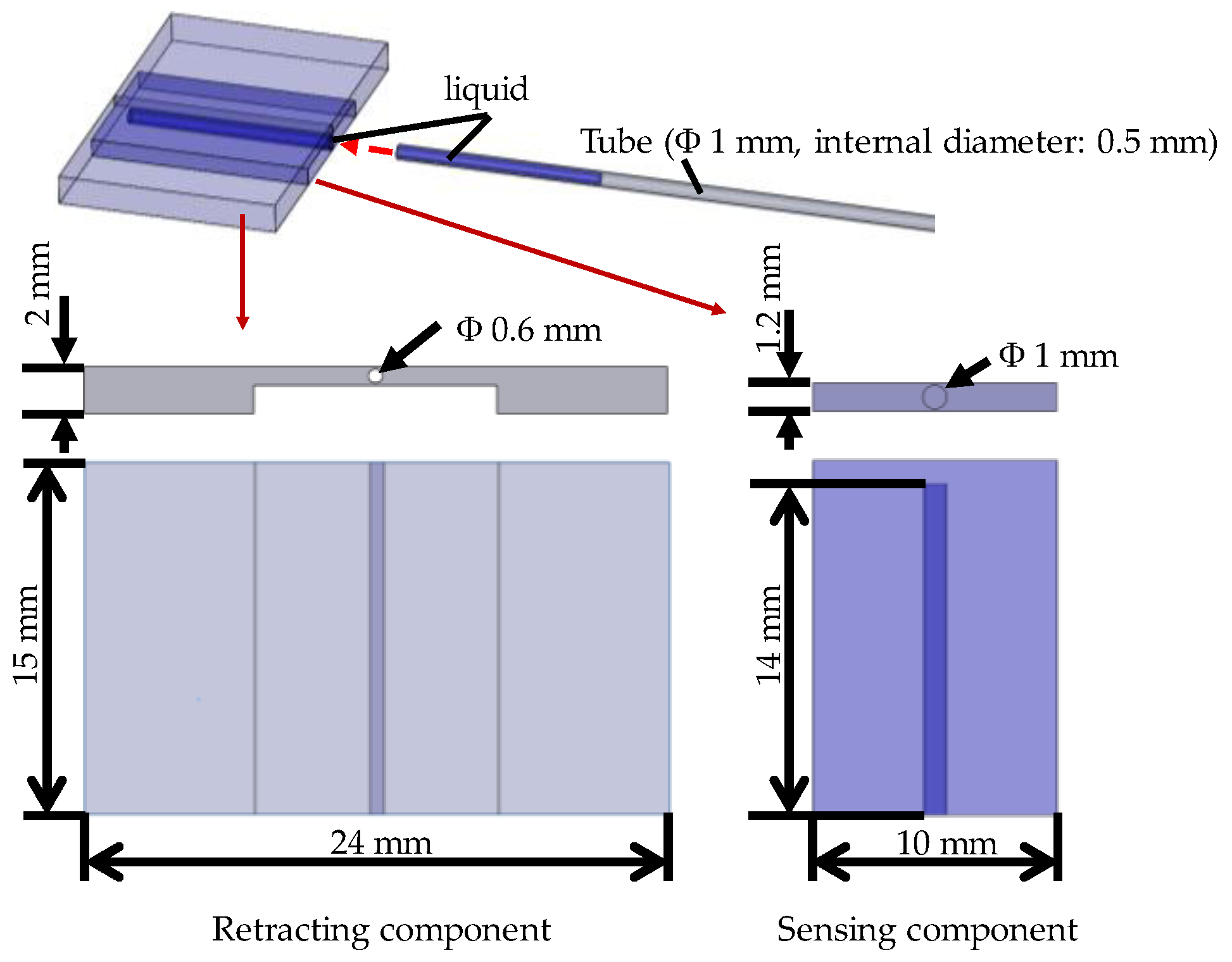
Force visualization mechanism utilizing a liquid: A liquid was installed into the sensing component of the silicone retractor. A transparent tube was connected to the sensing component to observe the liquid level, which is displaced according to the load. The load is visually measurable by the liquid displacement.
High usability: The silicone retractor is easily set up by installing a suction pipe into the hole in the retractor. The retractor was composed entirely of silicone and connected to PTFE tubes. Thus, the benefits of the system include the absence of electrical components, disposability, easy sterilization/disinfection, magnetic resonance imaging (MRI) compatibility, and low cost. The sensor was installed in only one area where the largest force is exerted to minimize the damage to the brain tissue. Moreover, the fact that there is only one sensing area minimizes the space occupied by the sensor and enhances the usability of the device.
Multiple functions: The proposed instrument provides the functions of retraction, suction, and force sensing via attachment to the suction pipe.
Hybrid soft and hard structure: The silicone retractor must be stiff for retracting tissues, while the sensing component inside the retractor must be soft to provide high sensitivity. To realize both these functions, a hybrid soft and hard structure was adapted. A thin retractor was developed using hard retracting and soft sensing parts.
The rest of this paper is organized as follows: after describing relevant literatures, the proposed instrument and the force sensing system are presented. Several versions of the silicone retractors are then described with an experimental evaluation.
2. Related Work
The key function of the presented medical instrument is force sensing. Here, we focus on force sensing [
2,
3,
4,
5,
6,
7]. Several force sensing systems have been developed for neurosurgery. Our group developed forceps where gripping and pulling forces are measureable [
8,
9,
10]. The group of Yang et al. developed a force-limiting dissector [
11] and demonstrated its effect at real operations [
12]. Interaction forces between tool and tissue were quantified by utilizing force sensors [
13,
14]. The used force sensors were based on strain gauges, and electrical components are needed for transferring the force information. No electrical components are preferred for easy disinfection or sterilization, which is necessary for medical operations.
Several approaches do not require electrical components for transferring the force information. A pneumatic force can be transferred via an air tube. Based on this concept, the group of Kawahara et al. [
15,
16] developed force sensor-embedded forceps whose tip has no electrical components. Kawahara et al. utilized air pressure with an endoscope for estimating organ stiffness [
17]. Acoustic information can also be transferred from the tip to the roots of the forceps without any electrical components. Fukuda et al. utilized acoustic reflection for estimating tissue softness [
18]. Optical information can be transferred via fibers without any electrical components. Peirs et al. utilized optical fibers to transfer the visualized deformation of a flexible structure [
19]. Tada et al. [
20] detected the peak illumination changes in a light source embedded in a deformable structure. Puangmali et al. [
21] utilized an optical sensing scheme and presented a three-axis force sensor. Polygerinos et al. [
22,
23,
24,
25] also utilized an optical sensing scheme and presented several types of force sensors for catheterization. Liu et al. [
26] identified tissue abnormality by a wheeled probe. Ahmadi et al. [
27] developed an MRI-compatible optical fiber tactile sensor. Xie et al. [
28] presented an optical tactile probe head for palpation. Tan et al. [
29] utilized intensity modulation of optical fibers for constructing an MRI-compatible force sensor. By utilizing optical fibers, Su et al. [
30,
31,
32] developed force/torque sensors for prostate needle placement and needle insertion. Turkseven and Ueda [
33] also utilized an optical fiber for sensing and feeding back the force information in robotic surgeries. Liu et al. [
34] developed an optical force sensor based on low-coherence Fabry–Perot interferometry. However, other related (electrical) components are required to acquire the force information from the transferred signals. This increases the size of the system as a whole and subsequently increases the cost. Magnets and magnetic sensors were also developed [
35,
36,
37]. However, for usage in MRI, no magnetic components are also preferred.
Force visualization is a key for transferring and acquiring the force information without any electrical or magnetic components and with low cost, because the visualized force information can be captured by the eyes of surgeons. Takaki et al. [
38] utilized moiré fringe patterns to visualize force information on the forceps. Watanabe et al. [
39,
40] visualized a small force magnitude by utilizing a highly elastic fabric. They also proposed a stiffness sensing system based on the force visualization mechanism [
41]. Although they were not for medical usage, Ohka et al. [
42] tracked the position and orientation of columnar and conical feelers made of silicone through a camera. Kamiyama et al. [
43] estimated the motion of two-layered markers with cameras to obtain the magnitude, distribution, and direction of the load. However, this paper targeted the development of the neurosurgical instrument, which can perform three functions of retraction, suction, and force-sensing, and its target range of the force information and size of the sensing part were different from those at [
38,
39,
40,
41,
42,
43]. A new suitable force visualization mechanism is required.
Our group has developed the first version of the instrument [
44]. However, there were drawbacks. The main drawbacks were the large thickness (16 mm) of the retractor and low force-visualized area. The force-visualized area was the surface of the retractor, that can become covered in blood if bleeding occurs, thus not allowing the force information to be visualized. While retracting deep areas, the surface of the retractor cannot be seen and the force information cannot be obtained. The system presented in this article will resolve these issues.
5. Experimental Evaluation on Soft Tissues
In real situations, the target object that is retracted with the silicone retractor is brain tissue (soft objects). Therefore, we investigated the performance of the force-sensing system of the developed silicone retractor when loading gelatin (
Figure 13 and
Table 2), which resembled the brain tissue. The experimental setup is shown in
Figure 14. The experimental setup was the same as that in the previous two experiments, except that the silicone retractor loads the gelatin. The target objects were two kinds of gelatin with different Young’s modulus values.
Table 2 shows the dimensions, Young’s modulus, and composition ratio of the two types of gelatin used in the experiment. The Young’s modulus can be controlled by the volume of the gelatin powder. The stiffness of the brain tissue takes various values. For example, the Young’s modulus of cerebral white matter takes the values in the range of 9.3–40.8 kPa [
45]. In this paper, Young’s modulus values of 10 kPa and 15 kPa were used as representative examples in order to simulate relatively soft tissue.
The experimental procedure was the same as that used in the previous two experiments, which the only difference being in the range of loading. The range of the applied load was 0.0 [N] to 0.7 [N] to avoid the fracture of gelatin. The experiment was repeated four times.
Figure 15 shows representative images captured while retracting the gelatin (Young’s modulus, 15 kPa) when the applied load was 0.30 N and 0.50 N.
5.1. Calibration While Retracting Flat and Rigid Surfaces
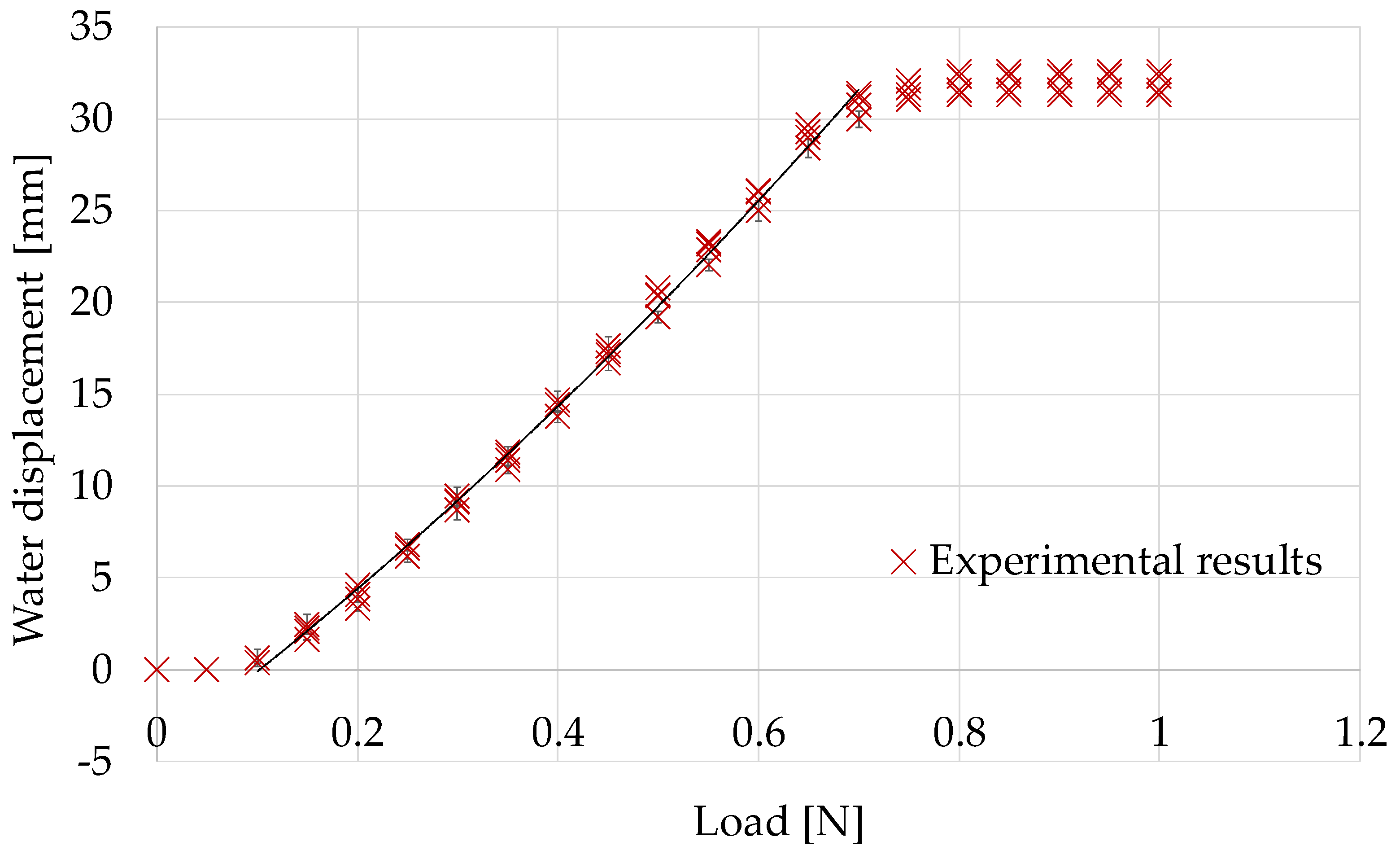
Figure 16 shows the experimental results. The black curve shows the regression curve defined in Equation (1) that was calibrated utilizing the experimental results when retracting flat and rigid surfaces (described in the previous section).
Table 3 shows the RMSE between the measured values and those derived from the regression curve (Equation (1)). It is observed that the differences were larger than 0.05 N, but the difference in the RMSE value for the two types of gelatin was very small. When retracting an object, the silicone retractor deformed to a V-shape, as shown in
Figure 15. If the target is soft, the deformation becomes is slightly larger than when the target is rigid. This is the reason for the difference. The results suggest that calibration should be done, considering the target stiffness.
5.2. Calibration While Retracting Gelatin (Young’s Modulus, 10 kPa)
With the previous suggestion in mind, we evaluated the experimental results in a way that the calibration and the evaluation targets have similar stiffness levels. Here, we focus on the different regression curve (the blue curve in
Figure 16) defined by:
Here, the regression curve was derived from the experimental results obtained when retracting gelatin with a Young’s modulus of 10 kPa.
Table 4 shows the RMSE between the measured values when retracting gelatin with a Young’s modulus of 15 kPa and those derived from the regression curve (Equation (2)). It can be observed that the regression curve can estimate the load for the gelatin with different stiffness values well. It indicates that the calibration should be performed by utilizing an object with a stiffness level close to that of the target. The results also validated the performance of the force sensing system developed by us.
5.3. Evaluation on Curved and Soft Surfaces
In real situations, the developed system can be used at different angles. Therefore, we investigated the performance of the system when loading semi-spherical gelatin (
Figure 17), which simulated the usages at different angles. The experimental setup and procedure are the same as those in the previous experiment, except for the target object and loading point. The target objects were four types of gelatin, whose properties are shown in
Table 5. The Young’s modulus was controlled by the volume of the gelatin powder. The loading point was at a distance of 5 mm from the center. The experiment was repeated four times.
Figure 17 shows representative images acquired when retracting the semi-spherical gelatin with a diameter of 60 mm (Young’s modulus, 10 kPa) and the semi-spherical gelatin with a diameter of 40 mm (Young’s modulus, 15 kPa).
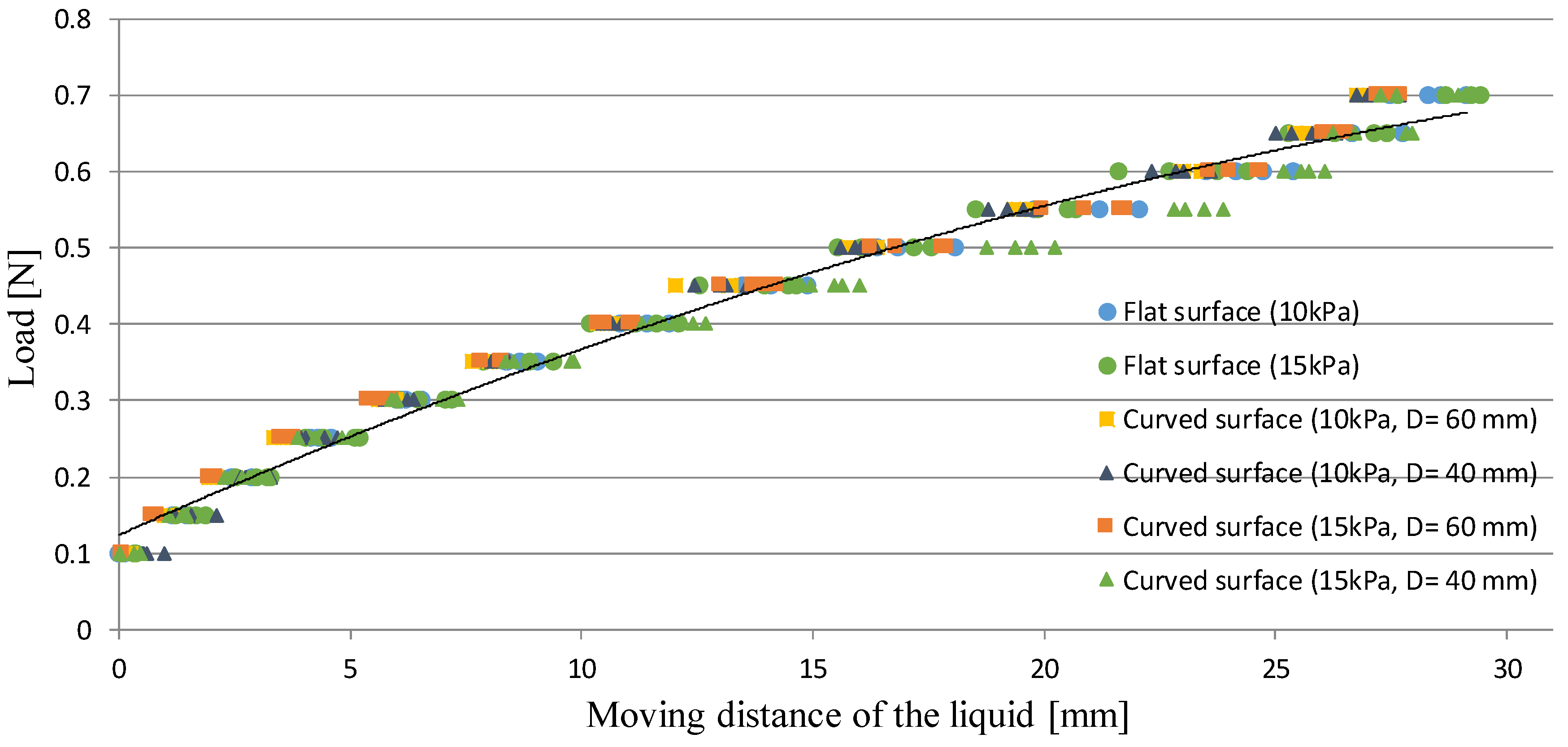
Figure 18 shows the experimental results. The black curve shows the regression curve defined in Equation (2) that was calibrated utilizing the experimental results when retracting the flat gelatin with a Young’s modulus of 10 kPa.
Table 6 shows the RMSE between the measured values and those derived from the regression curve (Equation (2)). From
Figure 18, the difference was observed at the range of 0.45–0.70 N when retracting the semi-spherical gelatin with a diameter of 40 mm (Young’s modulus, 15 kPa). The actual stiffness is different from Yong’s modulus. If loading a spherical object, the actual stiffness exponentially increases with an increase of loading. If the curvature of the object is high, the increasing rate is high. Therefore, the difference (due to the difference in stiffness) was observed at the range of 0.45–0.70 N when retracting the semi-spherical gelatin with a diameter of 40 mm (Young’s modulus, 15 kPa). Nonetheless, if evaluating RMSE in the separate range, RMSE was 0.018 N at the range of 0.10–0.40 N while RMSE was 0.034 N at the range of 0.45–0.70 N. From the values of RMSE and
Table 6, it can be concluded that the resolution was less than 0.05 N. It should be noted that from
Table 3, the maximum difference between the actual and estimated forces was less than 0.06 N. Therefore, practically, the retracting force should be estimated while keeping in mind that the resolution is less than 0.06 N even when the stiffness for the evaluation target is far from the one for the calibration target.
6. Conclusions
This paper presented a novel neurosurgical instrument, which performs three functions, including retraction, suction, and force sensing. Suction instruments and retractors are frequently used in neurosurgery. To reduce the number of times an instrument is changed and enhance the operation safety, we developed force-sensible silicon retractors, which are attachable to a suction pipe. It was constructed to contain retracting and sensing components. The sensing component contained a hole connected to a tube, and a liquid was placed inside the hole and the tubes. If a load is applied, the sensing component deforms and the liquid inside moves to the end of the tube. Thus, the liquid level corresponds to the retracting force, and the force information can be visually observed. This system is the improved version of our previously developed systems [
1,
44]. The previous versions had several serious limitations including large thickness, which limited the usability. We resolved this by utilizing a hybrid soft sensing and hard retracting structure, which drastically reduced the thickness of the structure. A medical doctor commented that the developed silicon retractor is able to be inserted into narrow spaces, different from the previously developed ones [
1,
44]. The comment indicates the improvement of the usability at the proposed system. The force sensing system utilized a force visualization mechanism. Another issue in [
44] was that the force-display area was the same as the surface of the silicone retractor, and the force information could not be obtained while inserting the retractor into narrow spaces or deep areas. The usage of a liquid moved the force-display area to around the fingers of the surgeon. The current version of the instrument benefits from the absence of any electrical components, disposability, easy sterilization/disinfection, MRI compatibility, and low cost. We also optimized the structure of the sensor, so that the sensor resolution was less than 0.05 N (0.028 N from
Table 6). The sensor range depends on the structure of the sensing component, and we had two types of the ranges (0.2–1.0 N and 0.1–0.7 N). While this is enough to avoid overload, sensing in the low load range (0.0–0.1 N) and accuracy require further improvement.