Interactions between Endostatin and Vascular Endothelial Growth Factor (VEGF) and Inhibition of Choroidal Neovascularization
Abstract
:1. Introduction
2. Results
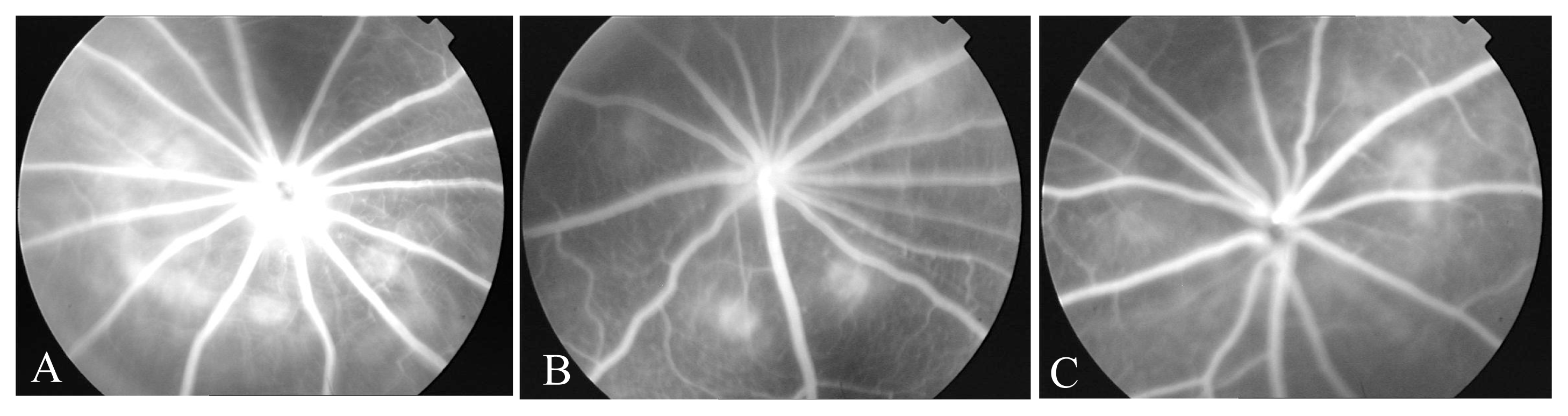
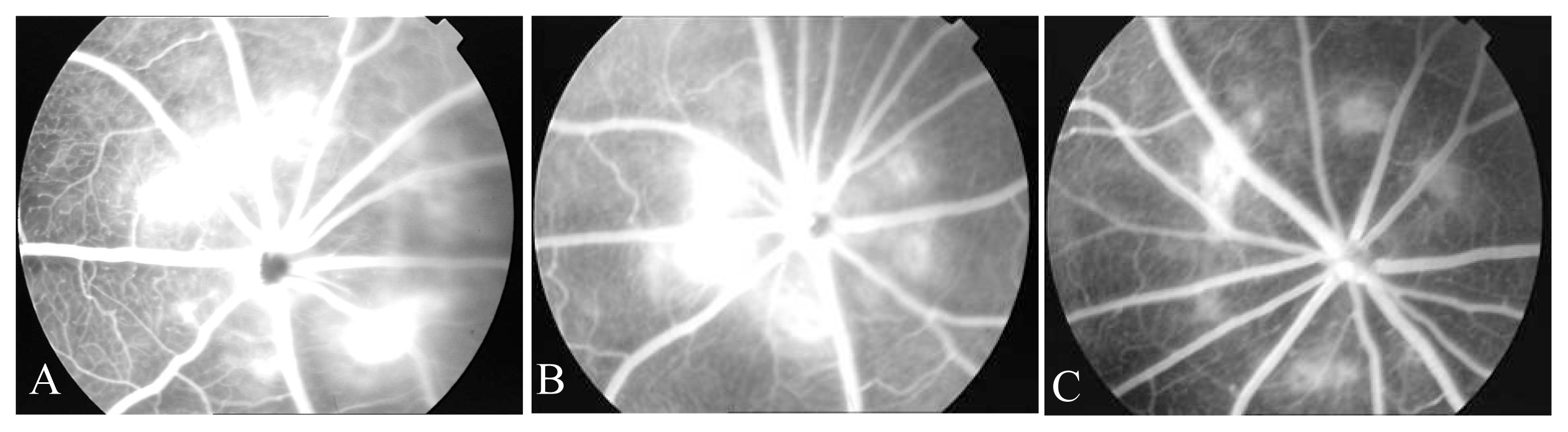
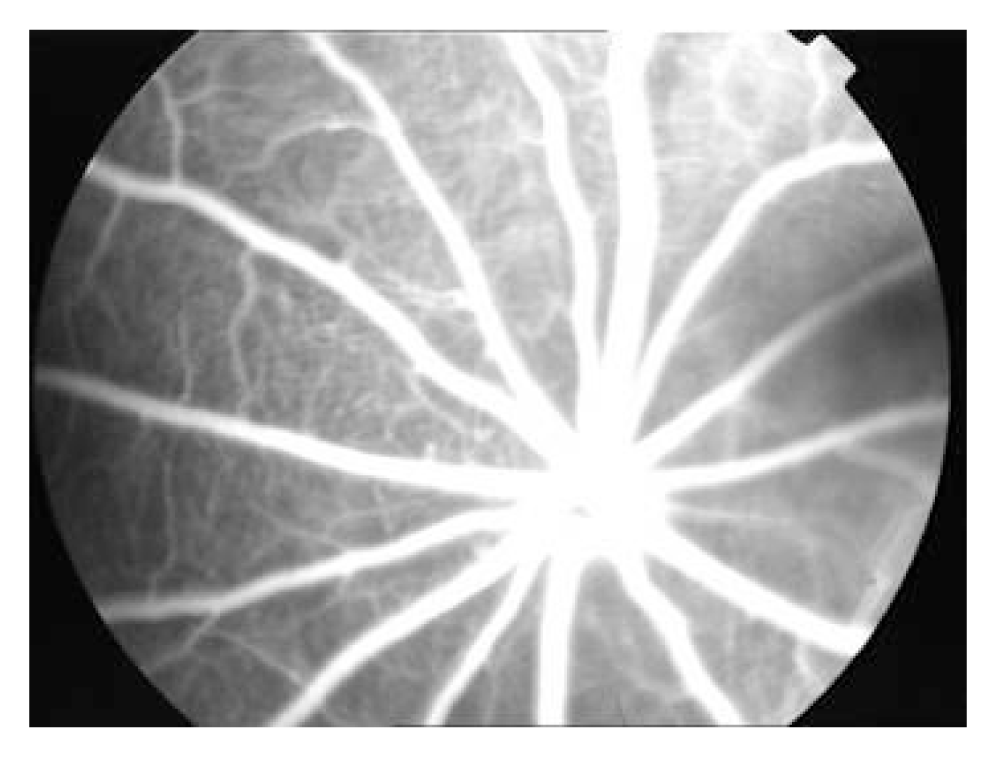
2.1. FFA
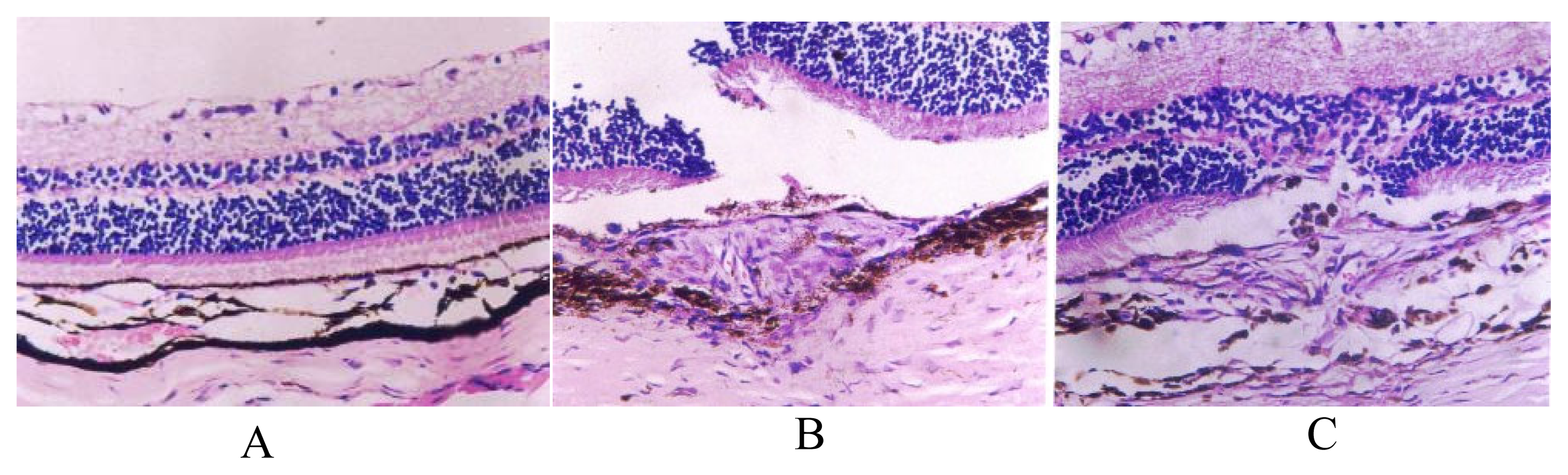
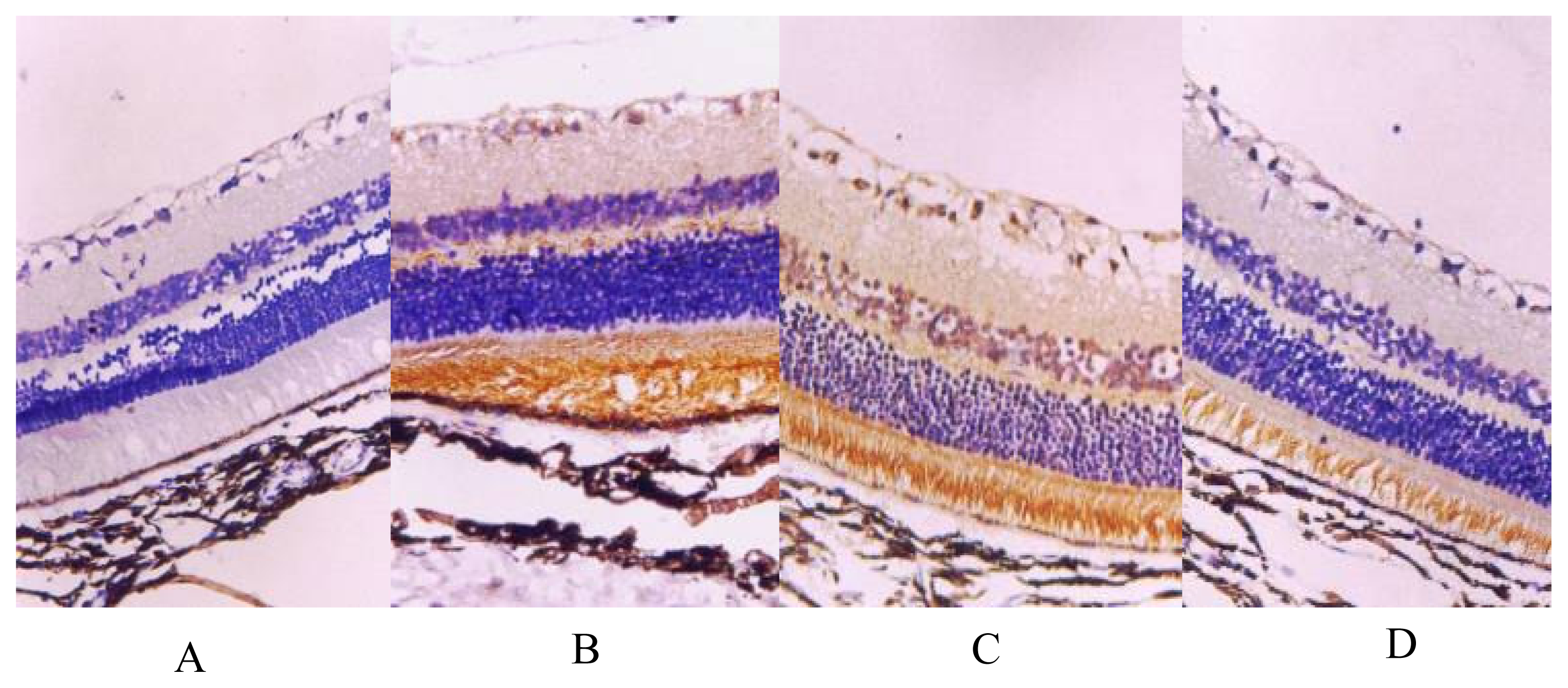
2.2. Histopathological examination
2.3. Expression of VEGF and bFGF mRNA
3. Discussion
4. Experimental
4.1. Reagents and equipments
4.2. Procedures
4.2.1. Preparation of animal models
4.2.2. Animal assignment
4.2.3. Fundus fluorescein angiography (FFA)
4.2.4. Light microscopic examination
4.2.5. Image analysis
4.2.6. Statistical analysis
Acknowledgments
References
- Hooper, C. Y.; Guymer, R. H. New treatments in age-related macular degeneration. Clin. Experiment Ophthalmol 2003, 31(5), 376–91. [Google Scholar]
- Lin, Y.; Hui, Y. N. Progress in the treatment of age-related macular degeneration. Ophthalmology 2001, 10(6), 353. [Google Scholar]
- Ciulla, T. A.; et al. Age-related macular degeneration: a review of experimental treatments. Surv Ophthalmol 1998, 43, 134–146. [Google Scholar]
- O’Reilly, M. S.; Boehw, T.; Shing, Y.; et al. Endostatin: an endogenous inhabitor of angionesis and tumor growth. Cell 1997, 88(2), 277–85. [Google Scholar]
- Kwak, N.; et al. VEGF is a major stimulator in model of choroidal neovacularization. Invest. Ophthalmol. Vis. Sci 2000, 41, 3158–3164. [Google Scholar]
- Dhanabal, M.; Volk, R.; Ramchandran, R.; et al. Cloning, expression, and in vitro activity of human endostatin. Biochem. Biophys. Res. Commun 1999, 258, 345–52. [Google Scholar]
- Mori, K.; Ando,, A.; Gehlbach,, P.; et al. Inhibition of choroidal neovascularization by intravenous injection of adenoviral vectors expressing secretable endostatin. Am. J. Pathol 2001, 159, 313–20. [Google Scholar]
- Dobi, E.T.; Puliafito, C.A.; Destro, M. A new model of experimental choroidal neovascularization in the rat. Arch. Ophthalmol 1989, 107(2), 264–9. [Google Scholar]
- Isbida, K.; Yosbimura, N.; Mandai, M.; et al. Inhibitory effect of TNP-470 on experimental choroidal neovascularization in a rat model. IOVS 1999, 40(7), 1512–9. [Google Scholar]
- Edelman, J.; Castro, M. Quantitative image analysis of laser-induced choroidal neovascularization in rat. Exp. Eye Res 2000, 71, 523–33. [Google Scholar]
- Hikichi, T.; Mori, F.; Takamiya, A.; et al. Inhibitory effect of bucillamine on laser-induced choroidal neovascularization in rats. Curr. Eye Res 2002, 24(1), 1–5. [Google Scholar]
- Kuroki, A.M.; Bhutto, I.A.; Kitaoka, T.; et al. Natural course of experimental choroidal neovascularization: three-dimensional study with corrosion cast and scanning electron microscope. Ophthalmic Res 2002, 34(4), 200–5. [Google Scholar]
- Shang, Q.L.; Ma, J.X.; Wei, J.S.; et al. Experimental study on endostatin inhibition of choroidal neovascularization. Chinese Journal of Ophthalmology 2004, 40(4), 266–71. [Google Scholar]
- Dhanabal, M.; Ramchdram, R.; Waterman, M.J.F.; et al. Endostatin induce endothelial cell apoptosis. J. Biol. Chem 1999, 274(17), 11721–6. [Google Scholar]
- Yamaguchi, N.; Anand-Apte, B.; Lee, M.; et al. Endostatin inhibits VEGF-induced endothelial cell migration and tumor growth independently of Zinc binding. EMBO J 1999, 18(16), 4414–23. [Google Scholar]
- Miosge, N.; Sasaki, T.; Timpl, R. Angiogenesis inhibitor endostatin is a distinct component of elastic fibers in vessel walls. FASEB J 1999, 13(13), 1743–50. [Google Scholar]
- Jia, Y.H.; Dong, X.S.; Wang, X.S. Effects of endostatin on expression of vascular endothelial growth factor and its receptors and neovascularization in colonic carcinoma implanted in nude mice. World J. Gastroenterol 2004, 10(22), 3361–4. [Google Scholar]
- Kim, Y.M.; Jang, J.W.; Lee, O.H.; et al. Endostatin inhibits endothelial and tumor cellular invasion by blocking the activation and catalytic activity of matrix metalloproteinase. Cancer Res 2000, 60(19), 5410–3. [Google Scholar]
- Yi, X.; Ogata, N.; Komada, M.; et al. Vascular endothelial growth factor expression in choroidal neovascularization in rats. Graefes. Arch. Clin. Exp. Ophthalmol 1997, 235(5), 313–9. [Google Scholar]
- Shen, W.J.; Yu, M.J.T.; Barry, C.J.; et al. Expression of cell adhesion molecules and vascular endothelial growth factor in experimental choroidal neovascularisation in the rat. Br. J. Ophthalmol 1998, 82, 1063–1071. [Google Scholar]
- Wada, M.; Ogata, N.; Otsuji, T.; et al. Expression of vascular endothelial growth factor and its receptor (KDR/flk-1) mRNA in experimental choroidal neovascularization. Curr. Eye Res 1999, 18(3), 203–13. [Google Scholar]
- Takebana, Y.; Kurokawa, T.; Kitamura, T.; et al. Suppression of laser-induced choroidal neovascularization by oral tranilast in the rat. Invest. Ophthalmol. Vis. Sci 1999, 40(2), 459–66. [Google Scholar]
| Group | Intensity of fluorescein leakage | Total | |||
|---|---|---|---|---|---|
| Grade 0 | Grade 1 | Grade 2 | Grade 3 | ||
| Laser injury | 99 | 24 | 27 | 15 | 165 |
| Normal saline | 93 | 24 | 21 | 12 | 150 |
| Endostatin group I | 138 | 24 | 24 | 18 | 204 |
| Endostatin group II | 141 | 9 | 6 | 0 | 156* |
| Group | Intensity of fluorescein leakage | Total | |||
|---|---|---|---|---|---|
| Grade 0 | Grade 1 | Grade 2 | Grade 3 | ||
| Laser injury | 37 | 15 | 23 | 40 | 115 |
| Normal saline | 31 | 17 | 21 | 35 | 104 |
| Endostatin group I | 75 | 13 | 21 | 26 | 135* |
| Endostatin group II | 84 | 11 | 12 | 3 | 110* |
| Optical density score | P1* | ||||
|---|---|---|---|---|---|
| Time | Blank control | Laser injury | Endostatin group I | Endostatin group II | |
| Day 7 | 22.9821±5.59801 | 157.1627±8.96718 | 114.1433±10.64936 | 76.6473±11.2825 | 0.00 |
| Day 14 | 22.9821±5.59801 | 147.5433±10.24009 | 100.7453±9.45678 | 54.8053±7.28959 | 0.00 |
| P2 | — | 0.01 | 0.00 | 0.00 | — |
© 2007 by MDPI Reproduction is permitted for noncommercial purposes.
Share and Cite
Wang, X.; Xu, X.; Tang, L.; Song, S.; Fan, C. Interactions between Endostatin and Vascular Endothelial Growth Factor (VEGF) and Inhibition of Choroidal Neovascularization. Int. J. Mol. Sci. 2007, 8, 61-69. https://doi.org/10.3390/i8010061
Wang X, Xu X, Tang L, Song S, Fan C. Interactions between Endostatin and Vascular Endothelial Growth Factor (VEGF) and Inhibition of Choroidal Neovascularization. International Journal of Molecular Sciences. 2007; 8(1):61-69. https://doi.org/10.3390/i8010061
Chicago/Turabian StyleWang, Xun, Xun Xu, Luosheng Tang, Shiping Song, and Chunhai Fan. 2007. "Interactions between Endostatin and Vascular Endothelial Growth Factor (VEGF) and Inhibition of Choroidal Neovascularization" International Journal of Molecular Sciences 8, no. 1: 61-69. https://doi.org/10.3390/i8010061




