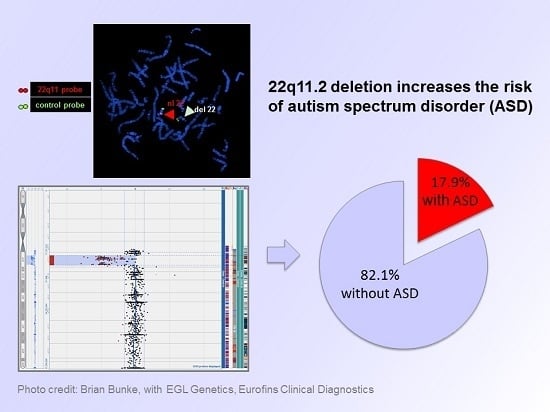
Examining the Overlap between Autism Spectrum Disorder and 22q11.2 Deletion Syndrome
Abstract
:1. Introduction
2. Results
3. Discussion
4. Materials and Methods
4.1. Participants
4.1.1. Overview
4.1.2. Recruitment and Eligibility
4.1.3. Demographic Characteristics
4.2. Diagnostic Procedures
4.3. Diagnostic Assessments
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| 22q11.2DS | 22q11.2 Deletion Syndrome |
| FISH | Fluorescent In Situ Hybridization |
| ASD | Autism Spectrum Disorder |
| ADOS | Autism Diagnostic Observation Schedule |
| ADI-R | Autism Diagnostic Interview-Revised |
| CNV | Copy Number Variation |
| PDD-NOS | Pervasive Developmental Disorder-Not Otherwise Specified |
| RDoC | Research Domain Criteria |
| DSM-IV | Diagnostic and Statistical Manual of Mental Disorders, Fourth edition |
References
- Artigas-Pallares, J.; Gabau-Vila, E.; Guitart-Feliubadalo, M. Syndromic autism: II. Genetic syndromes associated with autism. Rev. Neurol. 2005, 40, S151–S162. [Google Scholar] [PubMed]
- Bassett, A.S.; McDonald-McGinn, D.M.; Devriendt, K.; Digilio, M.C.; Goldenberg, P.; Habel, A.; Vorstman, J. Practical guidelines for managing patients with 22q11.2 deletion syndrome. J. Pediatr. 2011, 159, 332–339. [Google Scholar] [CrossRef] [PubMed]
- Botto, L.D.; May, K.; Fernhoff, P.M.; Correa, A.; Coleman, K.; Rasmussen, S.A.; Merritt, R.K.; O’Leary, L.A.; Wong, L.Y.; Elixson, E.M.; et al. A population-based study of the 22q11.2 deletion: Phenotype, incidence, and contribution to major birth defects in the population. Pediatrics 2003, 112, 101–107. [Google Scholar] [CrossRef] [PubMed]
- Oskarsdottir, S.; Vujic, M.; Fasth, A. Incidence and prevalence of the 22q11 deletion syndrome: A population-based study in Western Sweden. Arch. Dis. Child. 2004, 89, 148–151. [Google Scholar] [CrossRef] [PubMed]
- Tezenas Du Montcel, S.; Mendizabai, H.; Ayme, S.; Levy, A.; Philip, N. Prevalence of 22q11 microdeletion. J. Med. Genet. 1996, 33, 719. [Google Scholar] [CrossRef] [PubMed]
- Gothelf, D.; Frisch, A.; Michaelovsky, E.; Weizman, A.; Shprintzen, R.J. Velo-Cardio-Facial Syndrome. J. Ment. Health Res. Intellect. Disabil. 2009, 2, 149–167. [Google Scholar] [CrossRef] [PubMed]
- Ousley, O.; Rockers, K.; Dell, M.L.; Coleman, K.; Cubells, J.F. A review of neurocognitive and behavioral profiles associated with 22q11 deletion syndrome: Implications for clinical evaluation and treatment. Curr. Psychiatry Rep. 2007, 9, 148–158. [Google Scholar] [CrossRef] [PubMed]
- Fine, S.E.; Weissman, A.; Gerdes, M.; Pinto-Martin, J.; Zackai, E.H.; McDonald-McGinn, D.M.; Emanuel, B.S. Autism spectrum disorders and symptoms in children with molecularly confirmed 22q11.2 deletion syndrome. J. Autism Dev. Disord. 2005, 35, 461–470. [Google Scholar] [CrossRef] [PubMed]
- Vorstman, J.A.; Morcus, M.E.; Duijff, S.N.; Klaassen, P.W.; Heineman-de Boer, J.A.; Beemer, F.A.; van Engeland, H. The 22q11.2 deletion in children: High rate of autistic disorders and early onset of psychotic symptoms. J. Am. Acad. Child Adolesc. Psychiatry 2006, 45, 1104–1113. [Google Scholar] [CrossRef] [PubMed]
- Bruining, H.; de Sonneville, L.; Swaab, H.; de Jonge, M.; Kas, M.; van Engeland, H.; Vorstman, J. Dissecting the clinical heterogeneity of autism spectrum disorders through defined genotypes. PLoS ONE 2010, 5, e10887. [Google Scholar] [CrossRef] [PubMed]
- Antshel, K.M.; Aneja, A.; Strunge, L.; Peebles, J.; Fremont, W.P.; Stallone, K.; Kates, W.R. Autistic spectrum disorders in velo-cardio facial syndrome (22q11.2 deletion). J. Autism Dev. Disord. 2007, 37, 1776–1786. [Google Scholar] [CrossRef] [PubMed]
- Bassett, A.S.; Costain, G.; Fung, W.L.; Russell, K.J.; Pierce, L.; Kapadia, R.; Carter, R.F.; Chow, E.W.; Forsythe, P.J. Clinically detectable copy number variations in a Canadian catchment population of schizophrenia. J. Psychiatr. Res. 2010, 44, 1005–1009. [Google Scholar] [CrossRef] [PubMed]
- Levinson, D.F.; Duan, J.; Oh, S.; Wang, K.; Sanders, A.R.; Shi, J.; Zhang, N.; Mowry, B.J.; Olincy, A.; Amin, F.; et al. Copy number variants in schizophrenia: Confirmation of five previous findings and new evidence for 3q29 microdeletions and VIPR2 duplications. Am. J. Psychiatry 2011, 168, 302–316. [Google Scholar] [CrossRef] [PubMed]
- Karayiorgou, M.; Simon, T.J.; Gogos, J.A. 22q11.2 microdeletions: Linking DNA structural variation to brain dysfunction and schizophrenia. Nat. Rev. Neurosci. 2010, 11, 402–416. [Google Scholar] [CrossRef] [PubMed]
- Ogilvie, C.M.; Moore, J.; Daker, M.; Palferman, S.; Docherty, Z. Chromosome 22q11 deletions are not found in autistic patients identified using strict diagnostic criteria. Am. J. Med. Genet. 2000, 96, 15–17. [Google Scholar] [CrossRef]
- Einfeld, S.; Molony, H.; Hall, W. Autism is not associated with the fragile X syndrome. Am. J. Med. Genet. 1989, 34, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Fisch, G.S. Is autism associated with the fragile X syndrome? Am. J. Med. Genet. 1992, 43, 47–55. [Google Scholar] [CrossRef] [PubMed]
- Hall, S.S.; Lightbody, A.A.; Hirt, M.; Rezvani, A.; Reiss, A.L. Autism in fragile X syndrome: A category mistake? J. Am. Acad. Child Adolesc. Psychiatry 2010, 49, 921–933. [Google Scholar] [CrossRef] [PubMed]
- McCary, L.M.; Roberts, J.E. Early identification of autism in fragile X syndrome: A review. J. Intellect. Disabil. Res. 2012, 57, 803–814. [Google Scholar] [CrossRef] [PubMed]
- Schaefer, G.B.; Mendelsohn, N.J. Genetics evaluation for the etiologic diagnosis of autism spectrum disorders. Genet. Med. 2008, 10, 4–12. [Google Scholar] [CrossRef] [PubMed]
- Ousley, O.Y.; Smearman, E.; Fernandez-Carriba, S.; Rockers, K.A.; Coleman, K.; Walker, E.F.; Cubells, J.F. Axis I psychiatric diagnoses in adolescents and young adults with 22q11 deletion syndrome. Eur. Psychiatry 2013, 28, 417–422. [Google Scholar] [CrossRef] [PubMed]
- Lord, C.; Rutter, M.; Le Couteur, A. Autism diagnostic interview-revised: A revised version of a diagnostic interview for caregivers of individuals with possible pervasive developmental disorders. J. Autism Dev. Disord. 1994, 24, 659–685. [Google Scholar] [CrossRef] [PubMed]
- Gotham, K.; Risi, S.; Pickles, A.; Lord, C. The autism diagnostic observation schedule: Revised algorithms for improved diagnostic validity. J. Autism Dev. Disord. 2007, 7, 613–627. [Google Scholar] [CrossRef] [PubMed]
- Risi, S.; Lord, C.; Gotham, K.; Corsello, C.; Chrysler, C.; Szatmari, P.; Cook, E.H.; Leventhal, B.L.; Pickles, A. Combining information from multiple sources in the diagnosis of autism spectrum disorders. J. Am. Acad. Child Adolesc. Psychiatry 2006, 45, 1094–1103. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. DSM-IV: Diagnostic and Statistical Manual; American Psychiatric Association: Washington, DC, USA, 1994. [Google Scholar]
- Wang, P.P.; Woodin, M.F.; Kreps-Falk, R.; Moss, E.M. Research on behavioral phenotypes: Velocardiofacial syndrome (deletion 22q11.2). Dev. Med. Child Neurol. 2000, 42, 422–427. [Google Scholar] [CrossRef] [PubMed]
- Cuthbert, B.N.; Insel, T.R. Toward the future of psychiatric diagnosis: The seven pillars of RDoC. BMC Med. 2013, 11, 126. [Google Scholar] [CrossRef] [PubMed]
- Constantino, J.N.; Todd, R.D. Autistic traits in the general population: A twin study. Arch. Gen. Psychiatry 2003, 60, 524–530. [Google Scholar] [CrossRef] [PubMed]
- Evans, D.W.; Uljarevic, M.; Lusk, L.G.; Loth, E.; Frazier, T. Development of two dimensional measures of restricted and repetitive behaviors in parents and children. J. Am. Acad. Child Adolesc. Psychiatry 2017, 56, 51–58. [Google Scholar] [CrossRef] [PubMed]
- Moreno-De-Luca, A.; Myers, S.M.; Challman, T.D.; Moreno-De-Luca, D.; Evans, D.W.; Ledbetter, D.H. Developmental brain dysfunction (DBD): Revival and expansion of an old concept based on new genetic evidence. Lancet Neurol. 2013, 12, 406–414. [Google Scholar] [CrossRef]
- Moreno-De-Luca, A.; Evans, D.W.; Boomer, K.; Hanson, E.; Bernier, R.; Goin-Kochel, R.; Myers, S.M.; Challman, T.D.; Moreno-de-Luca, D.; Spiro, J.; et al. Parental cognitive, behavioral and motor profiles impact the neurodevelopmental profile of individuals with de novo mutations. JAMA Psychiatry 2015, 72, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Jonas, R.K.; Montojo, C.A.; Bearden, C.E. The 22q11.2 deletion syndrome as a window into complex neuropsychiatric disorders over the lifespan. Biol. Psychiatry 2014, 75, 351–360. [Google Scholar] [CrossRef] [PubMed]
- Grayton, H.M.; Fernandes, C.; Rujescu, D.; Collier, D.A. Copy number variations in neurodevelopmental disorders. Prog. Neurobiol. 2012, 99, 81–91. [Google Scholar] [CrossRef] [PubMed]
- Karam, C.S.; Ballon, J.S.; Bivens, N.M.; Freyberg, Z.; Girgis, R.R.; Lizardi-Ortiz, J.E.; Javitch, J.A. Signaling pathways in schizophrenia: Emerging targets and therapeutic strategies. Trends Pharmacol. Sci. 2010, 31, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Rockers, K.; Ousley, O.; Sutton, T.; Schoenberg, E.; Coleman, K.; Walker, E.; Cubells, J.F. Performance on the modified card sorting test and its relation to psychopathology in adolescents and young adults with 22q11.2 deletion syndrome. J. Intellect. Disabil. Res. 2009, 53, 665–676. [Google Scholar] [CrossRef] [PubMed]
- Lord, C; Rutter, M.; DiLavore, P.; Risi, S. Autism Diagnostic Observation Schedule Manual; Western Psychological Services: Los Angeles, CA, USA, 1999. [Google Scholar]
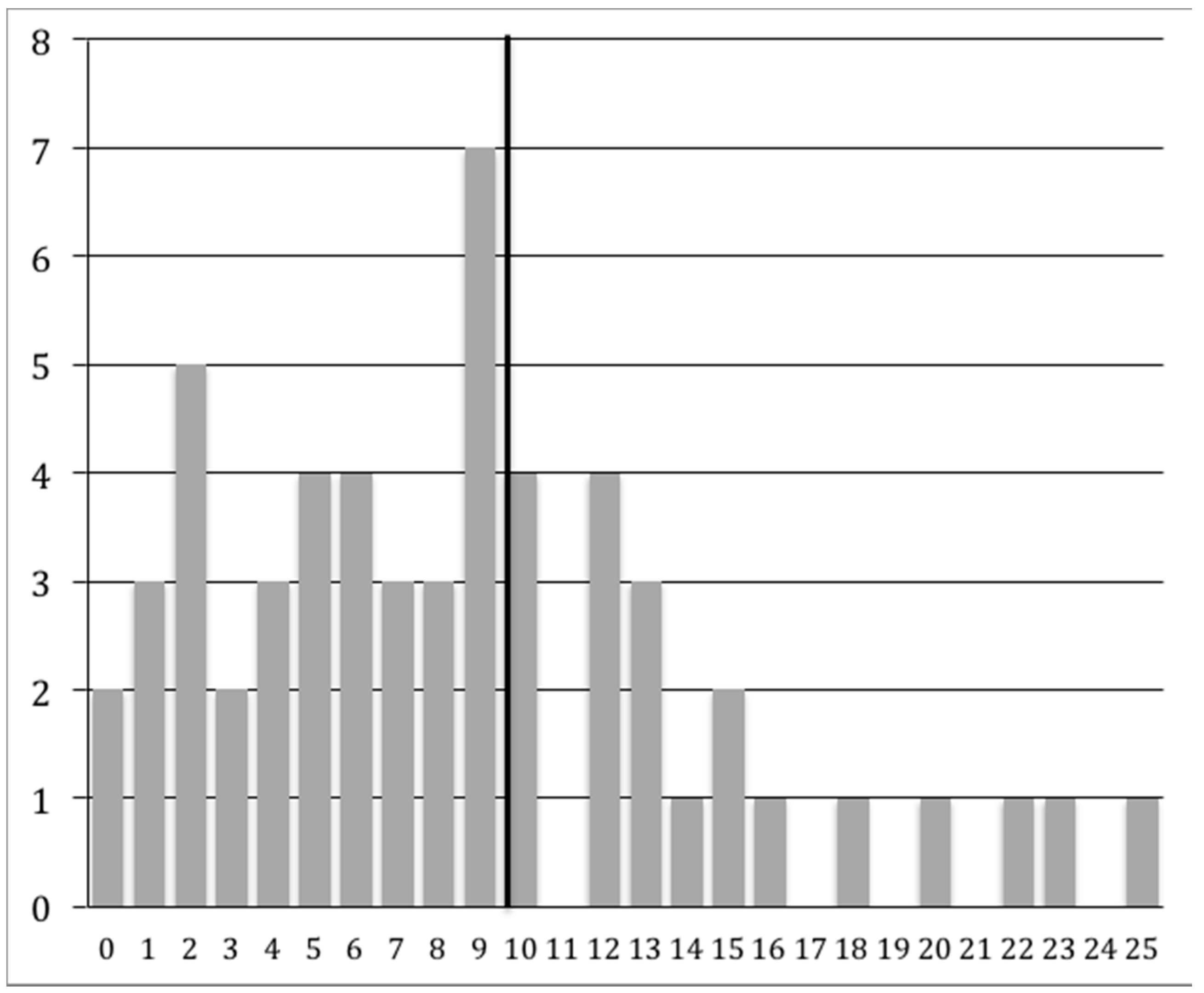
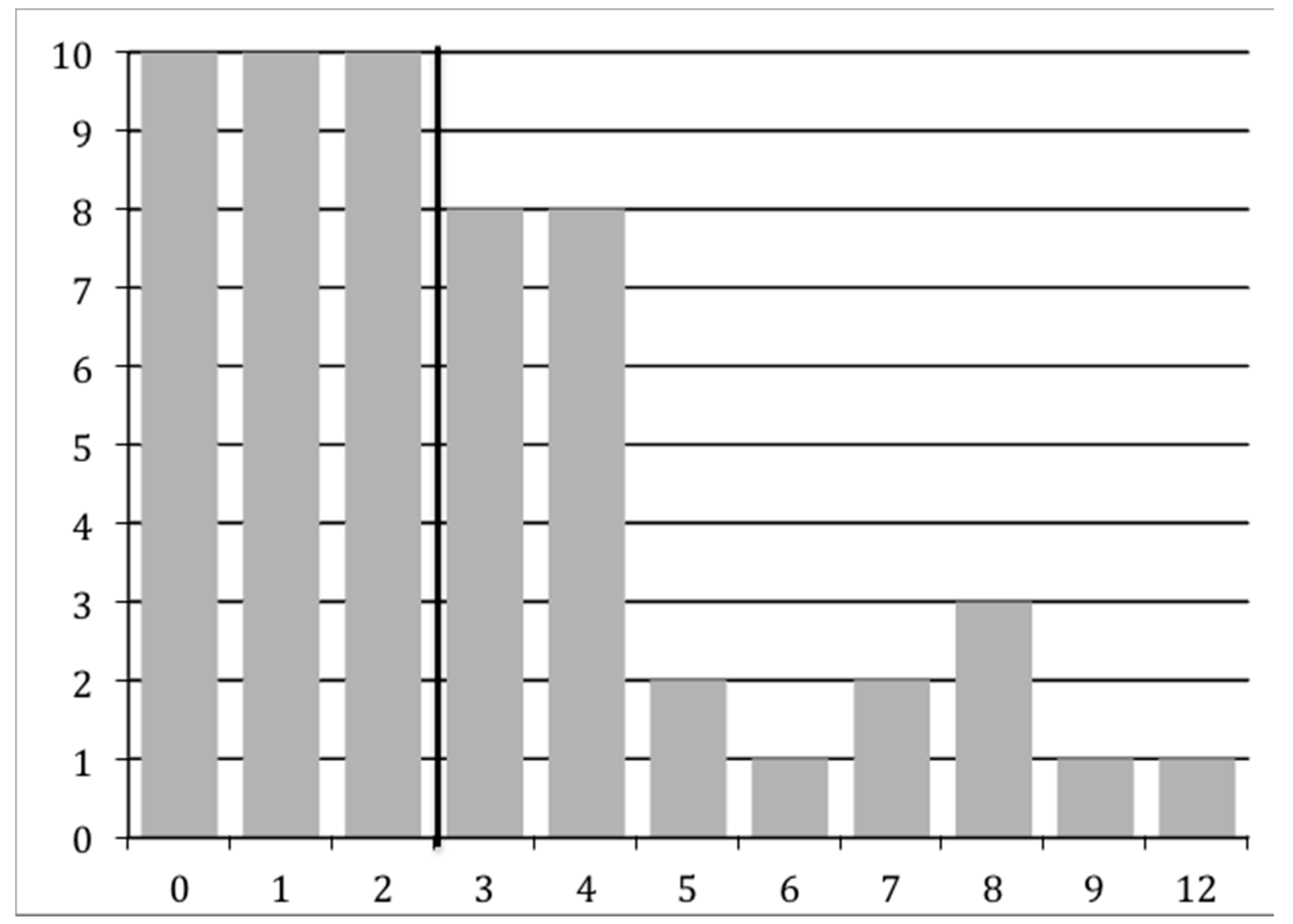

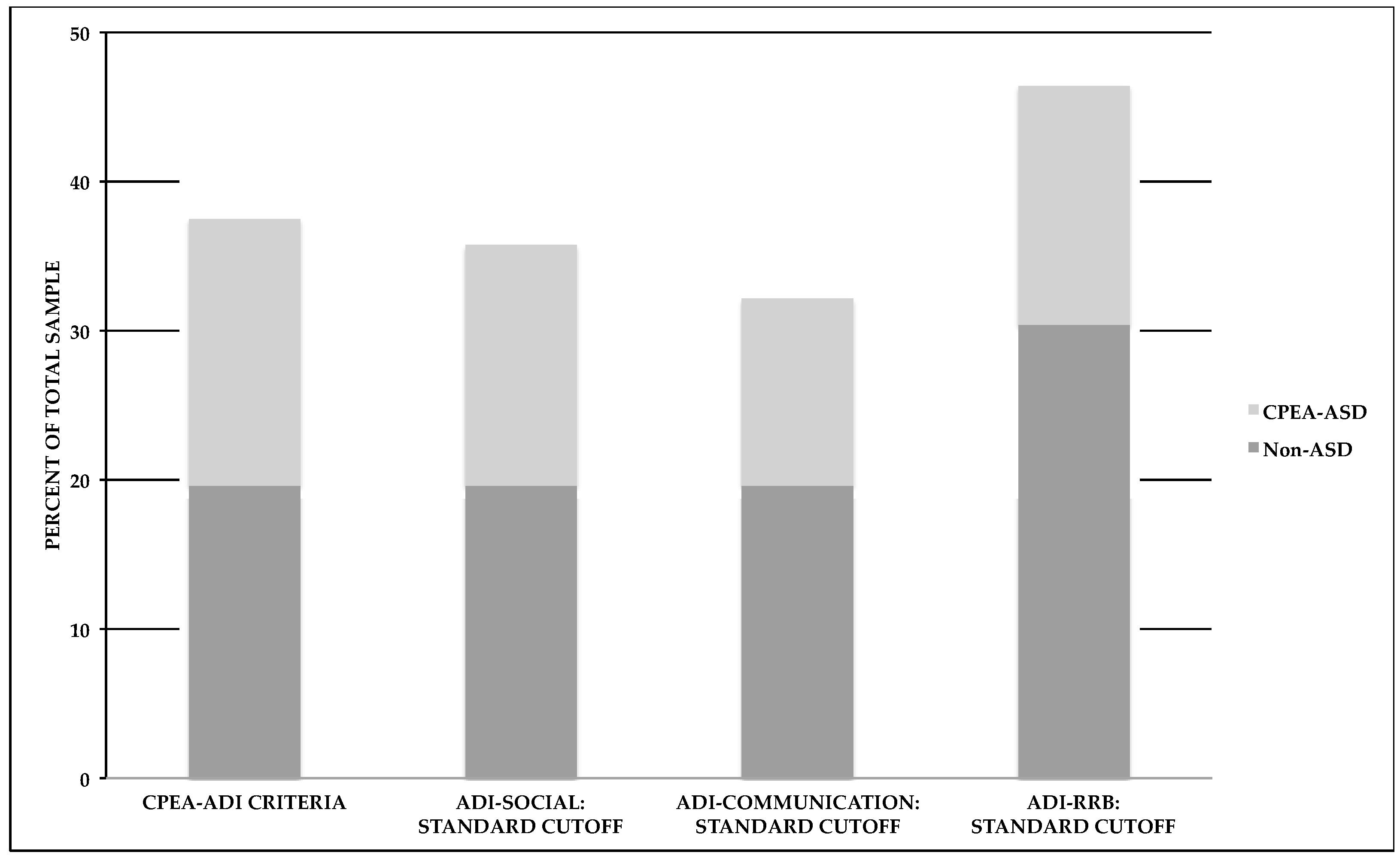
| Child | Adult | Total | Family | |
|---|---|---|---|---|
| n = 24 | n = 32 | n = 56 | ||
| Mean age (Standard deviation) | 9.58 (1.91) | 19.21 (4.12) | 15.1 (5.85) | - |
| Gender | ||||
| Female, n (percent, %) | 11 (45.8) | 17 (53.1) | 28 (50.0) | - |
| Male, n (%) | 13 (54.2) | 15 (46.9) | 28 (50.0) | - |
| Congenital heart defect | ||||
| n (%) | 16 (66.7) | 17 (53.1) | 33 (58.9) | 1 (1.8) |
| Immune deficiency | ||||
| n (%) | 15 (62.5) | 14 (43.8) | 29 (51.8) | 0 (0) |
| Palatal anomalies | ||||
| n (%) | 11 (45.8) | 19 (59.4) | 30 (53.6) | 0 (0) |
| Speech-language delay | ||||
| n (%) | 17 (70.8) | 15 (46.9) | 32 (57.1) | 8 (14.3) |
| Attention Deficit/Hyperactivity Disorder (ADHD) | ||||
| n (%) | 11 (45.8) | 7 (21.9) | 18 (32.1) | 12 (21.4) |
| Autism spectrum diagnosis (known prior to study entry) | ||||
| n (%) | 0 (0) | 1 (3.1) | 1 (1.8) | 2 (3.6) |
| 22q11.2 deletion | ||||
| n (%) | 24 (100) | 32(100) | 56 (100) | 1 (1.8) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ousley, O.; Evans, A.N.; Fernandez-Carriba, S.; Smearman, E.L.; Rockers, K.; Morrier, M.J.; Evans, D.W.; Coleman, K.; Cubells, J. Examining the Overlap between Autism Spectrum Disorder and 22q11.2 Deletion Syndrome. Int. J. Mol. Sci. 2017, 18, 1071. https://doi.org/10.3390/ijms18051071
Ousley O, Evans AN, Fernandez-Carriba S, Smearman EL, Rockers K, Morrier MJ, Evans DW, Coleman K, Cubells J. Examining the Overlap between Autism Spectrum Disorder and 22q11.2 Deletion Syndrome. International Journal of Molecular Sciences. 2017; 18(5):1071. https://doi.org/10.3390/ijms18051071
Chicago/Turabian StyleOusley, Opal, A. Nichole Evans, Samuel Fernandez-Carriba, Erica L. Smearman, Kimberly Rockers, Michael J. Morrier, David W. Evans, Karlene Coleman, and Joseph Cubells. 2017. "Examining the Overlap between Autism Spectrum Disorder and 22q11.2 Deletion Syndrome" International Journal of Molecular Sciences 18, no. 5: 1071. https://doi.org/10.3390/ijms18051071