Development, Optimization and In Vitro/In Vivo Characterization of Collagen-Dextran Spongious Wound Dressings Loaded with Flufenamic Acid
Abstract
:1. Introduction
2. Results and Discussion
2.1. Design of Experiments
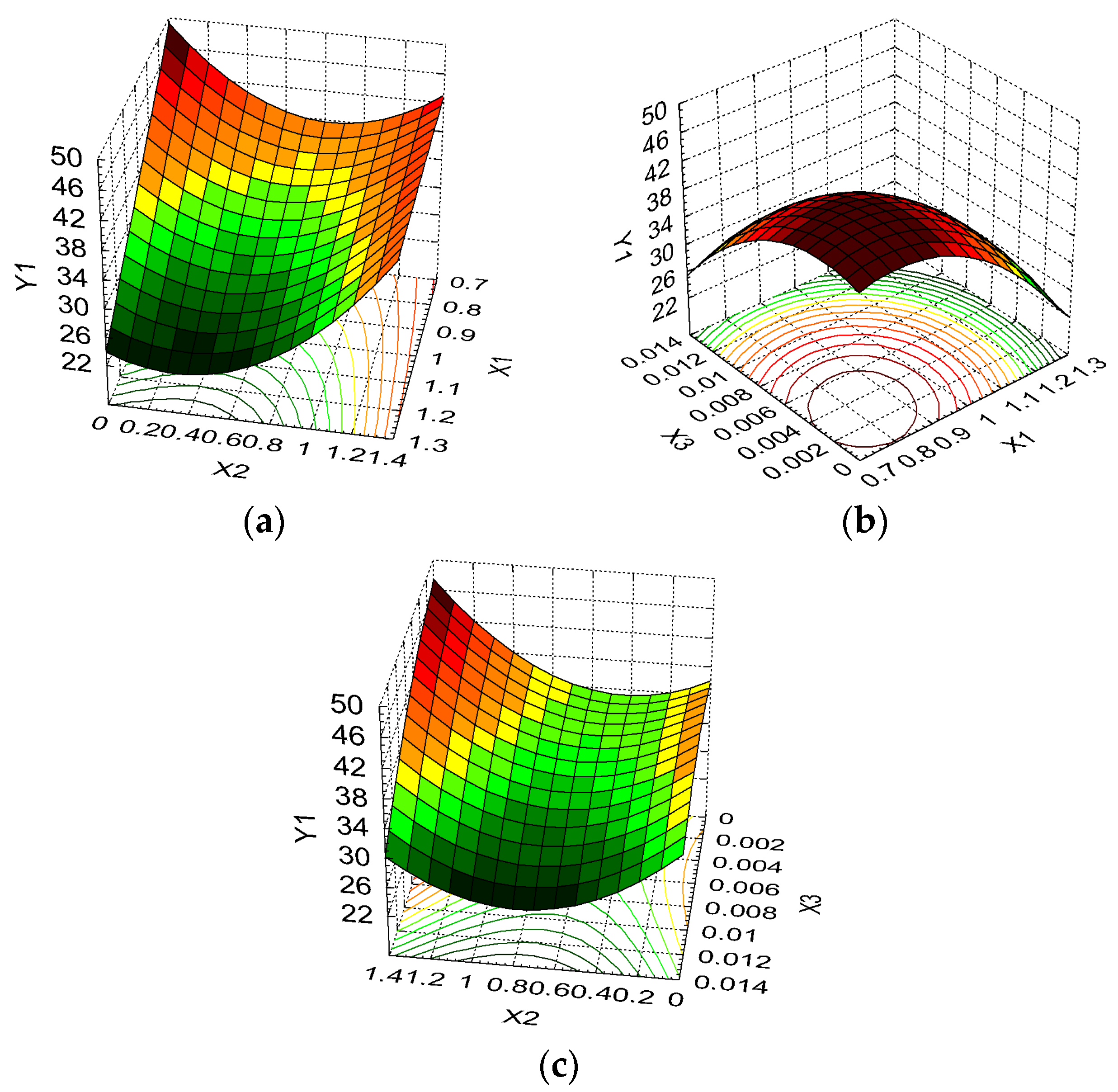
2.2. Swelling Study
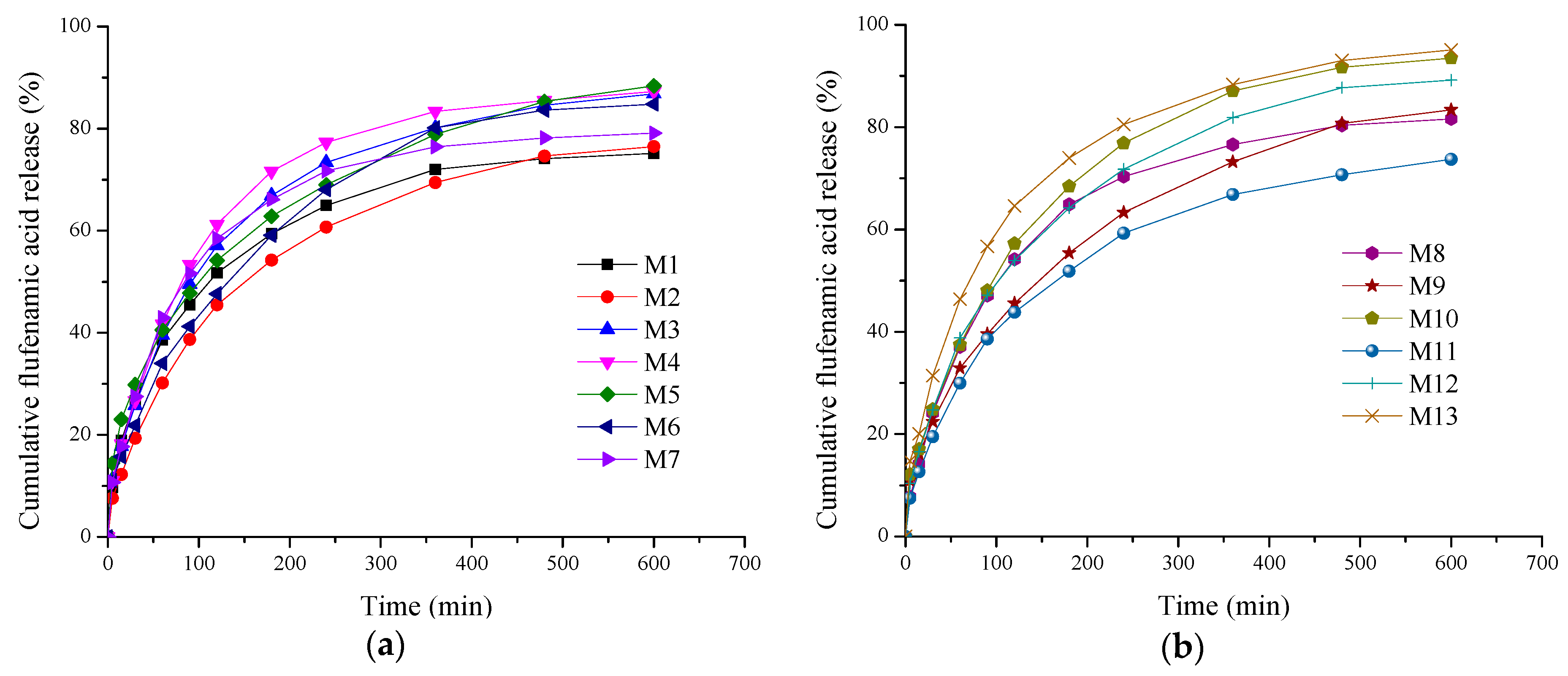
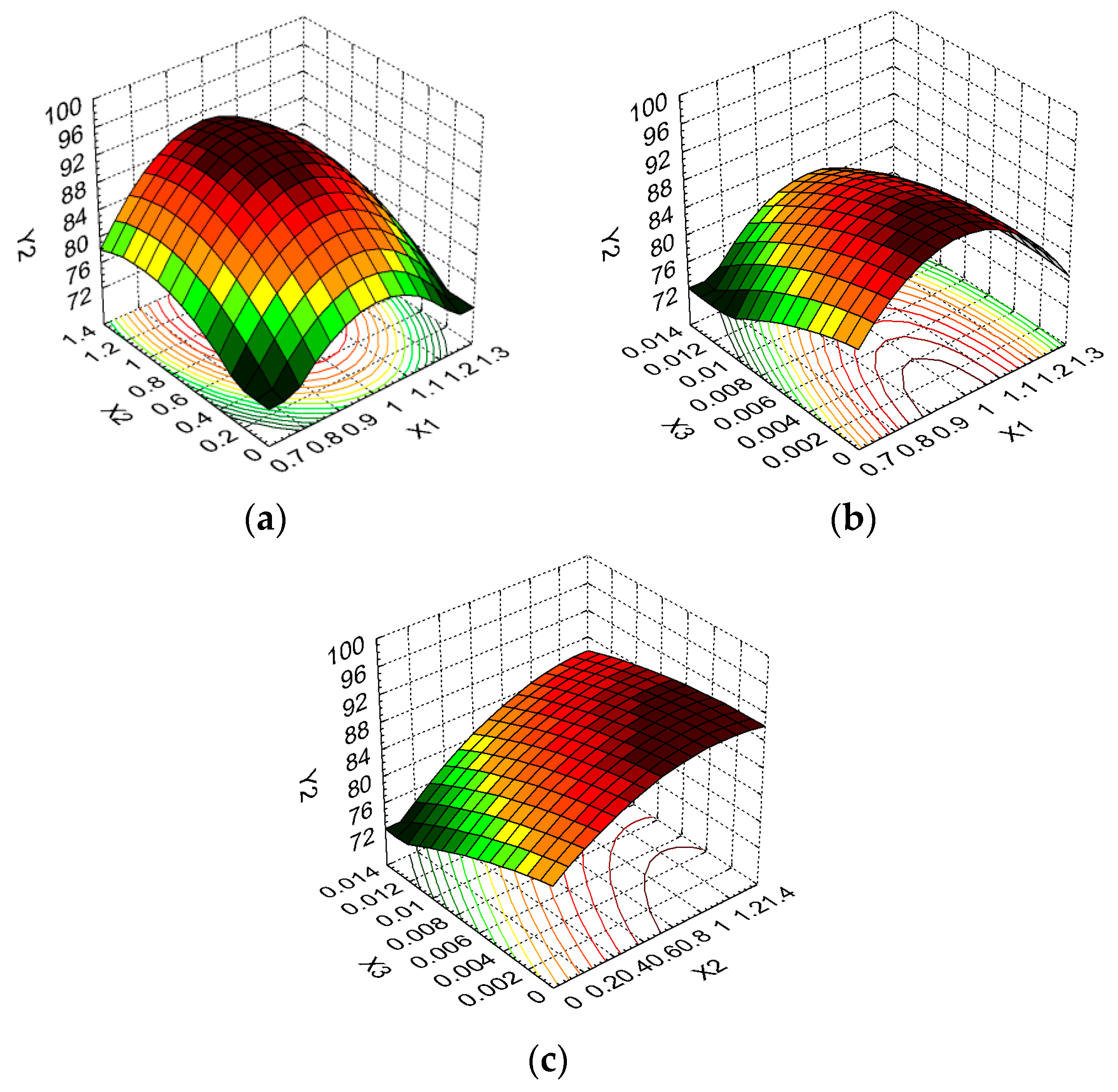
2.3. In Vitro Drug Release Kinetics Study and Data Modeling
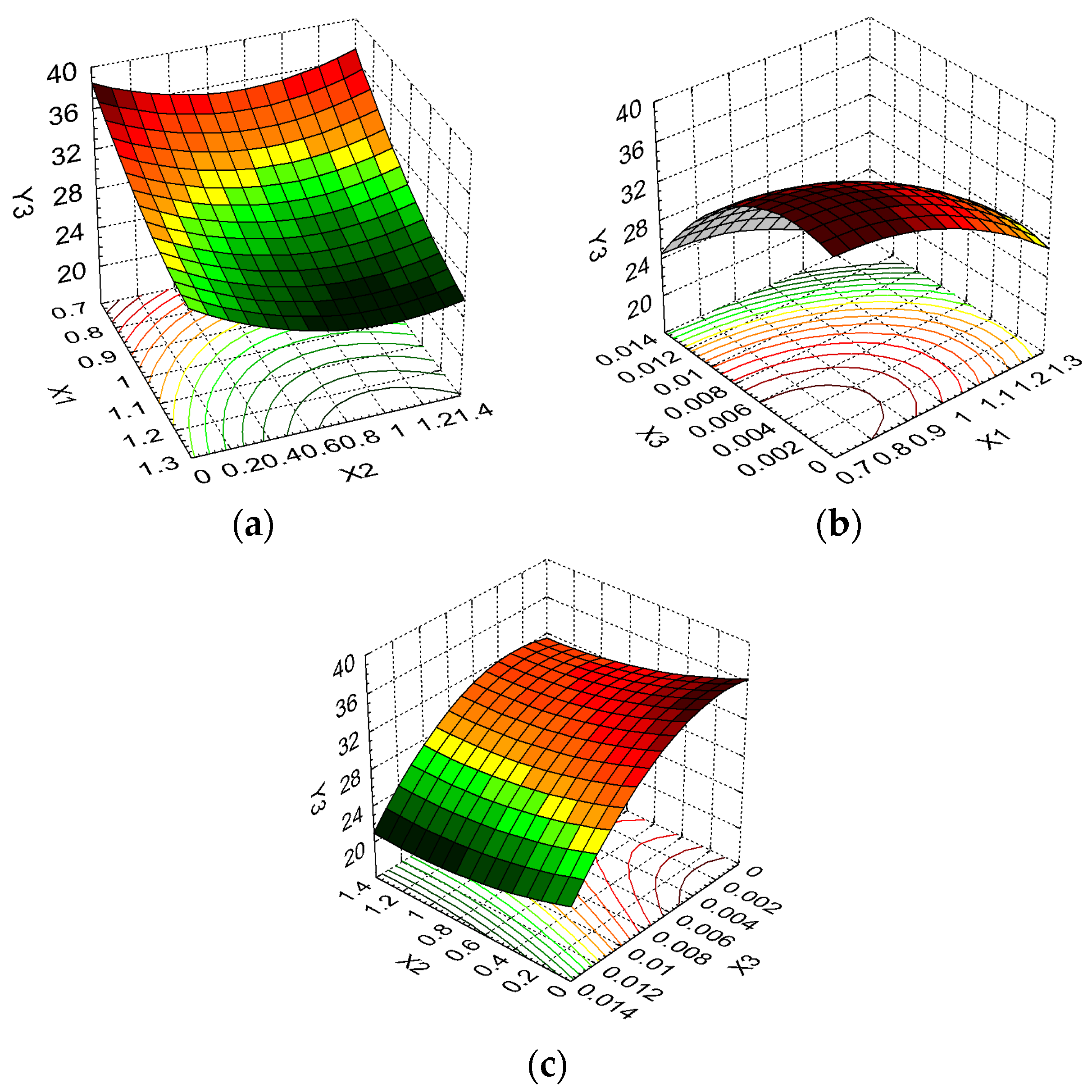
2.4. In Vitro Enzymatic Degradation Analysis
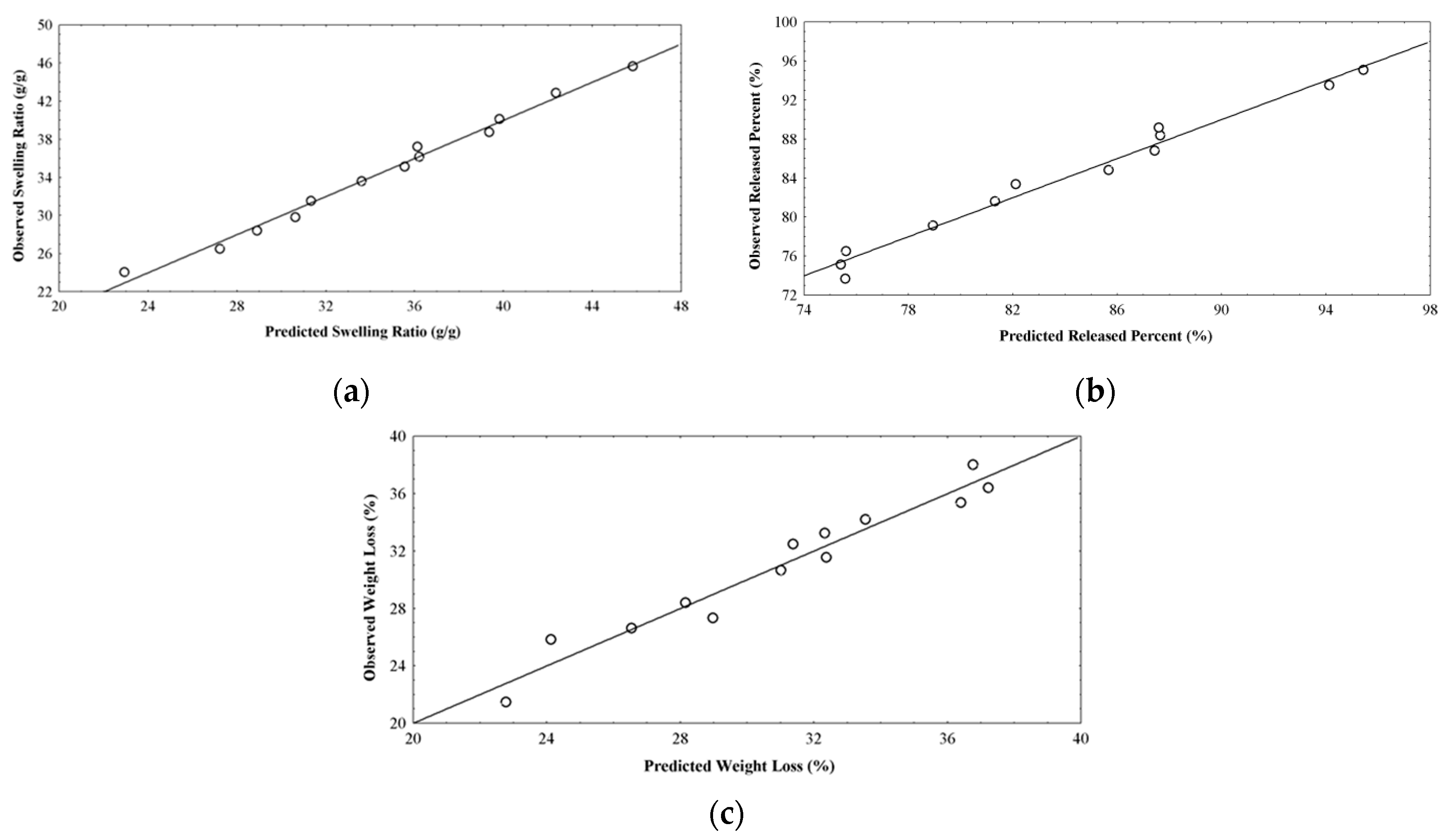
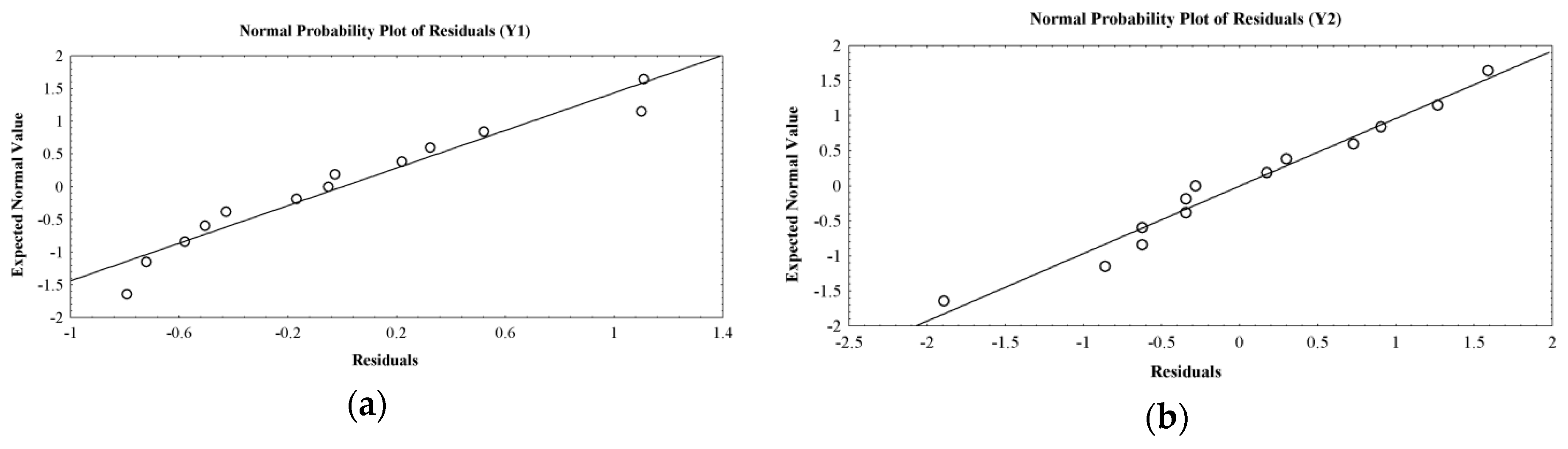
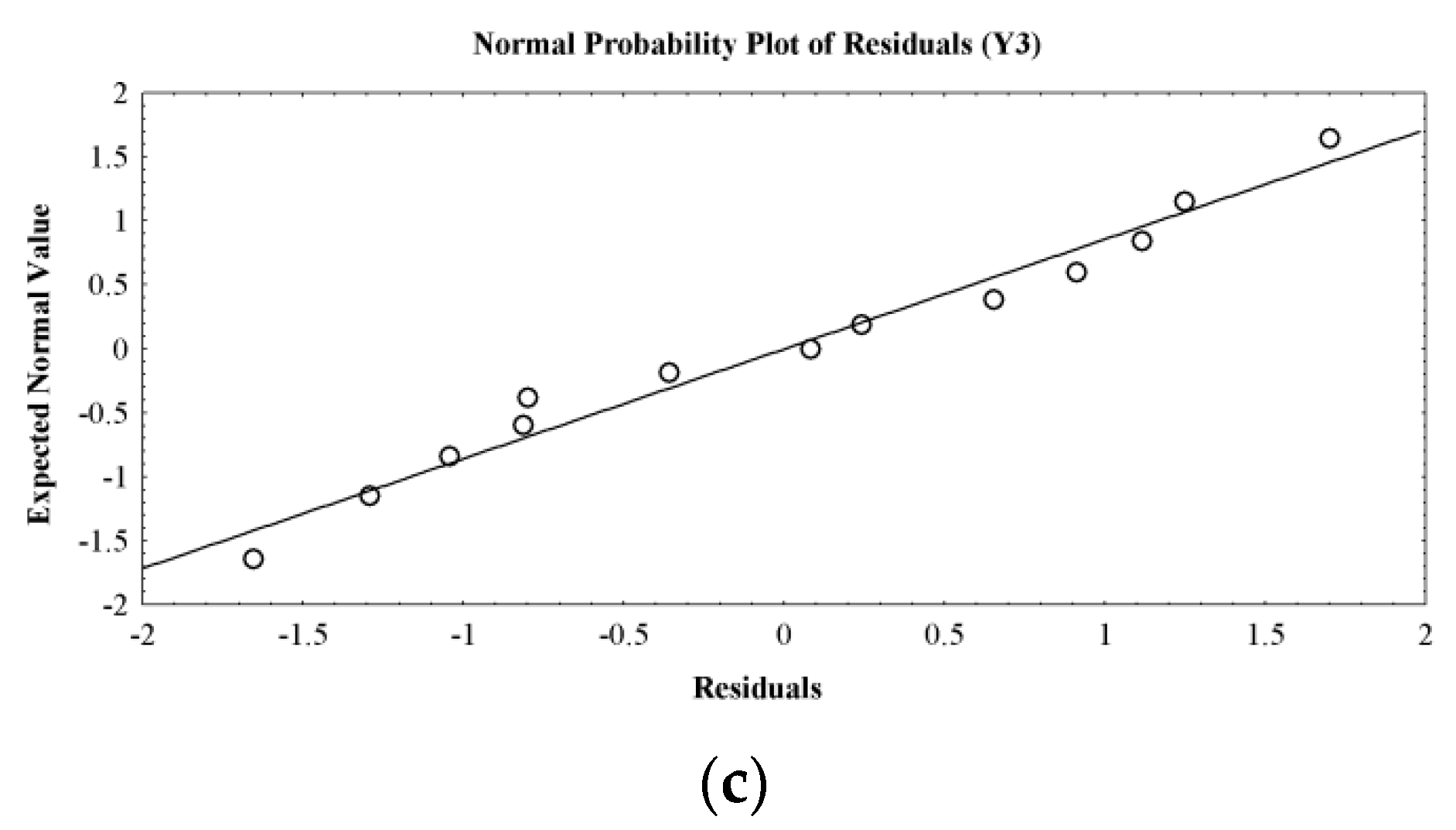
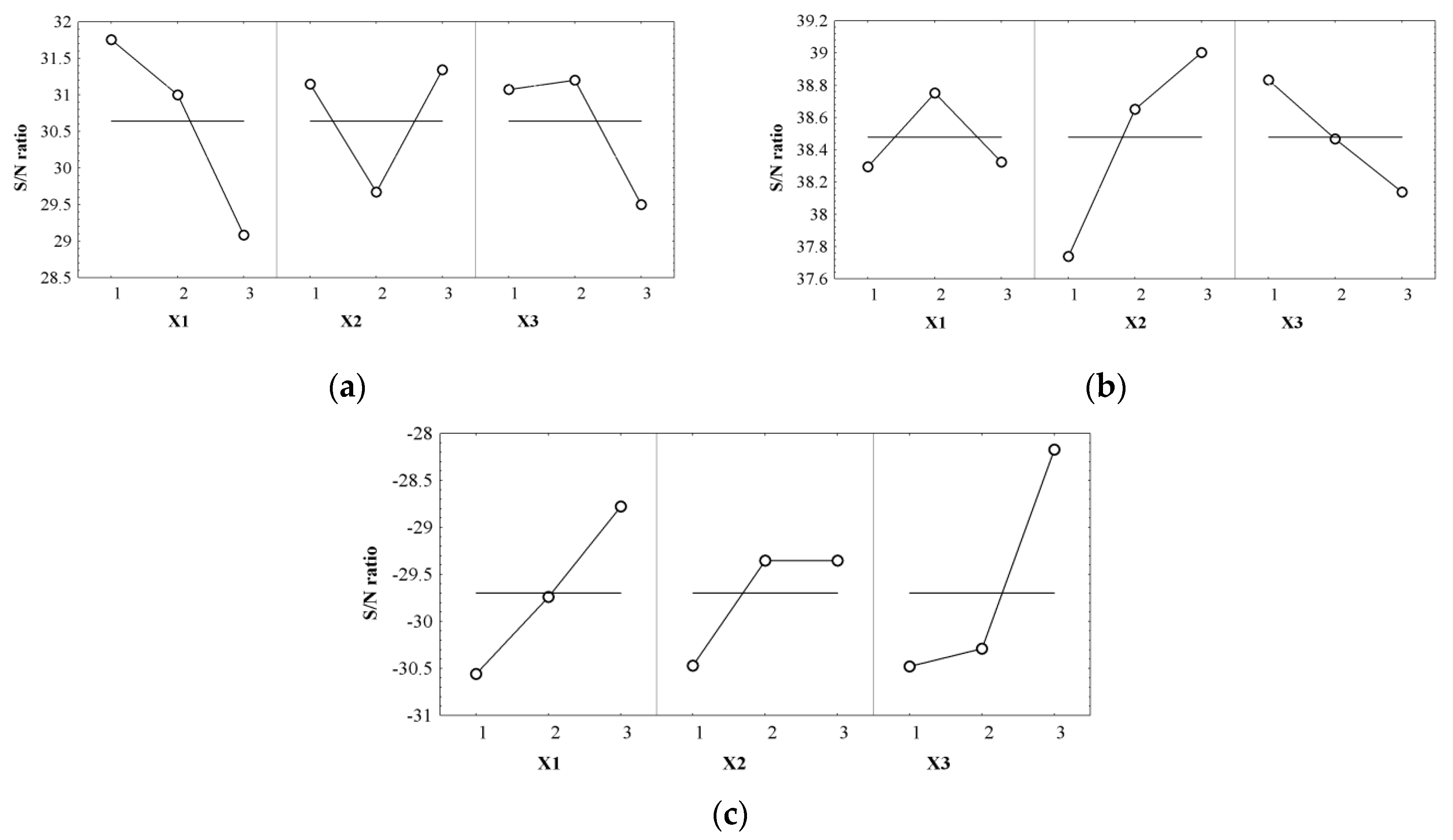
2.5. Optimization Technique
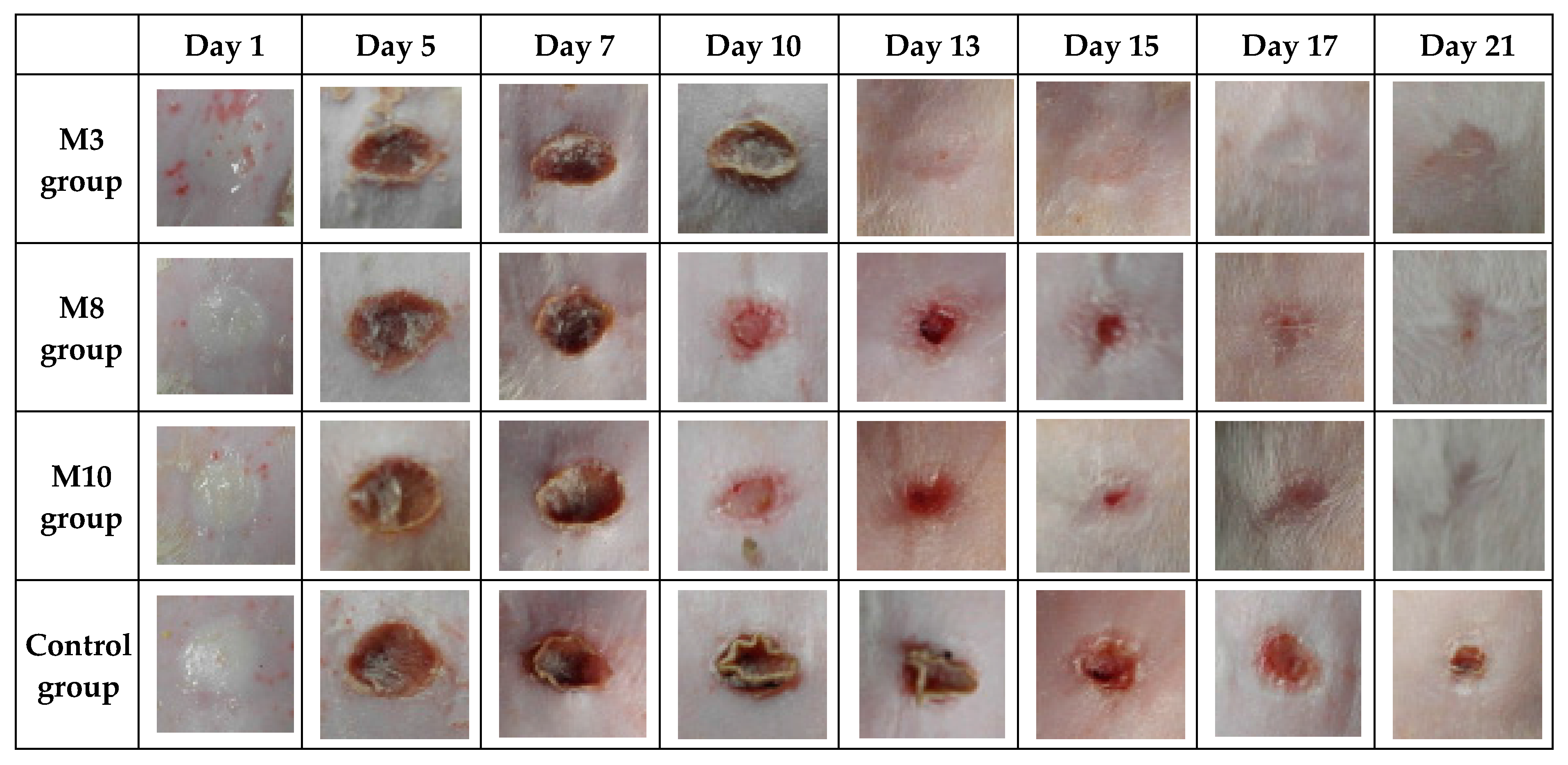
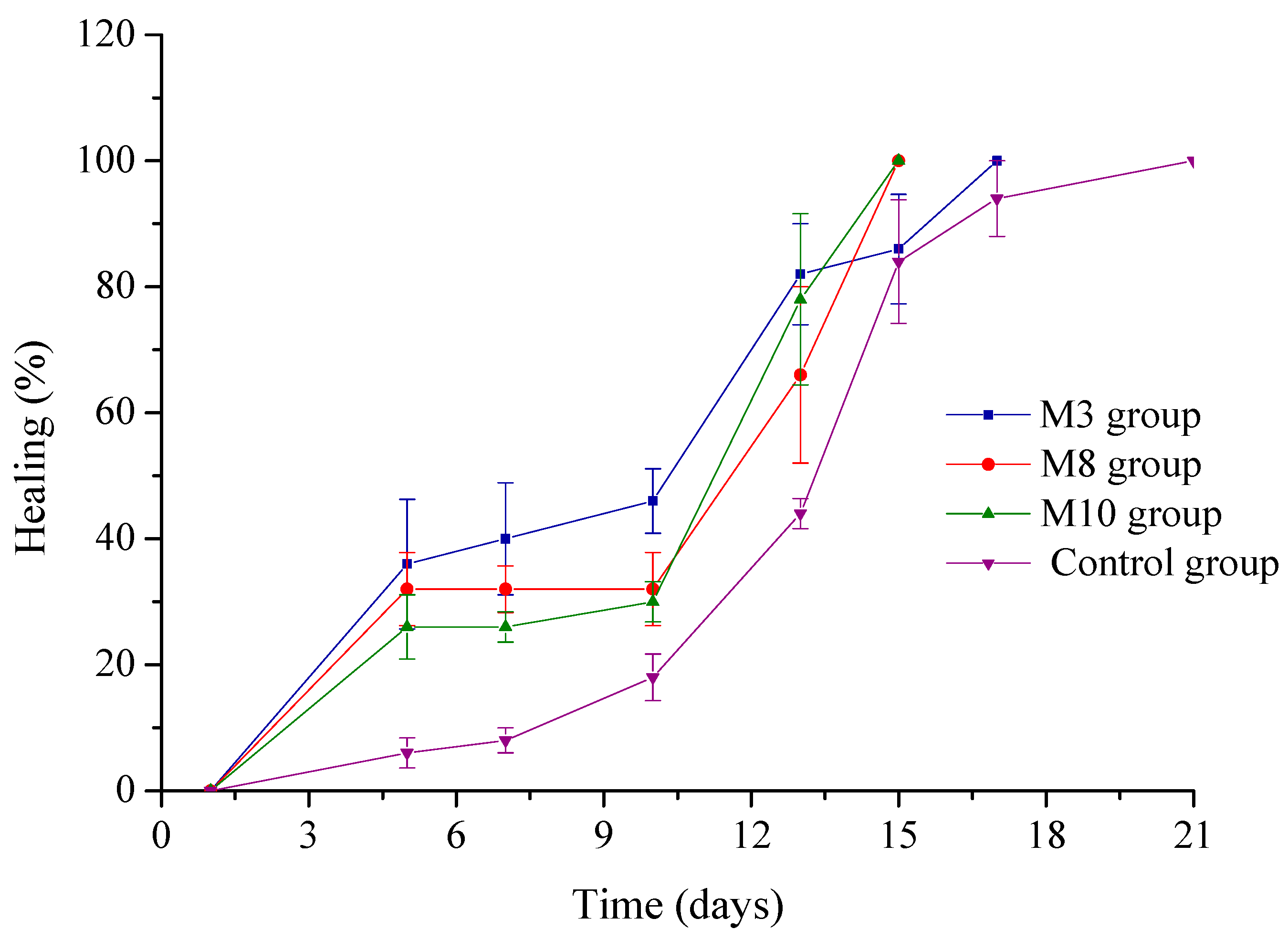
2.6. Evaluation of the Collagen Sponges’ Performance during the Wound Healing Process
3. Materials and Methods
3.1. Materials
3.2. Methods
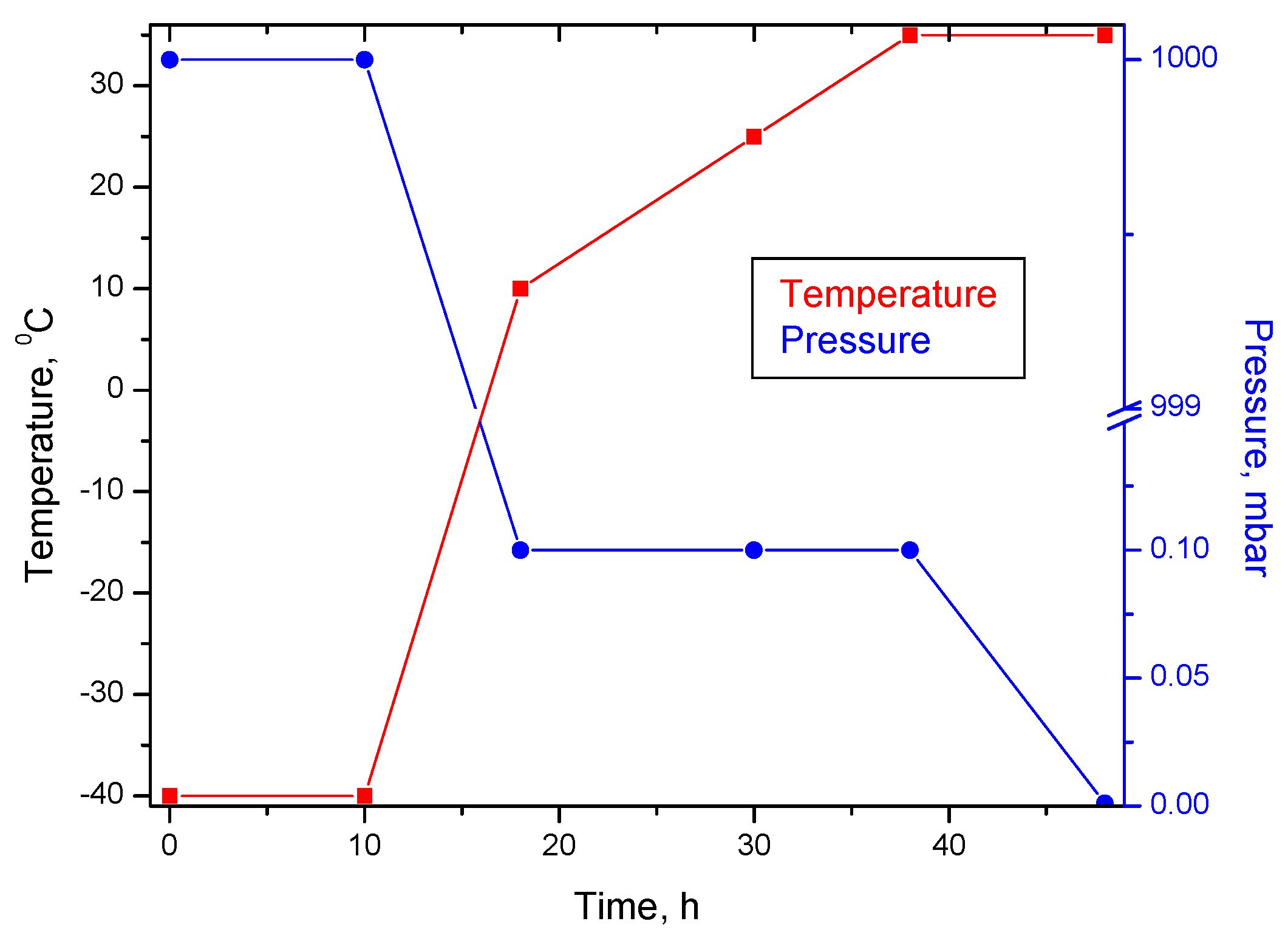
3.2.1. Preparation of Spongious Matrices
3.2.2. Swelling Study
3.2.3. In Vitro Drug Release Kinetics Study and Data Modeling
3.2.4. In Vitro Enzymatic Degradation Analysis
3.2.5. Design of Experiments and Optimization Technique
3.2.6. Evaluation of the Collagen Sponges Performance during the Wound Healing Process
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| FFA | Flufenamic acid |
| NSAID | Non-steroidal anti-inflammatory drug |
| DDS | drug delivery systems |
| C | collagen |
| DX | dextran |
| GA | glutaraldehyde |
| SR | swelling ratio |
| RP | released percent |
| WL | weight loss |
References
- Frieri, M.; Kumar, K.; Boutin, A. Wounds, burns, trauma, and injury. Wound Med. 2016, 13, 12–17. [Google Scholar] [CrossRef]
- Farina, J.A., Jr.; Junqueira Rosique, M.; Rosique, R.G. Curbing inflammation in burn patients. Int. J. Inflam. 2013, 2013. [Google Scholar] [CrossRef] [PubMed]
- Salibian, A.A.; Del Rosario, A.T.D.; Severo, L.A.M.; Nguyen, L.; Banyard, D.A.; Toranto, J.D.; Evans, G.R.D.; Widgerow, A.D. Current concepts on burn wound conversion—A review of recent advances in understanding the secondary progressions of burns. Burns 2016, 42, 1025–1035. [Google Scholar] [CrossRef] [PubMed]
- Chang, K.C.; Ma, H.; Liao, W.C.; Lee, C.K.; Lin, C.Y.; Chen, C.C. The optimal time for early burn wound excision to reduce pro-inflammatory cytokine production in a murine burn injury model. Burns 2010, 36, 1059–1066. [Google Scholar] [CrossRef] [PubMed]
- Widgerow, A.D.; Kalaria, S. Pain mediators and wound healing—Establishing the connection. Burns 2012, 38, 951–959. [Google Scholar] [CrossRef] [PubMed]
- Ekenseair, A.K.; Kurtis Kasper, F.; Mikos, A.G. Perspectives on the interface of drug delivery and tissue engineering. Adv. Drug Deliv. Rev. 2013, 65, 89–92. [Google Scholar] [CrossRef] [PubMed]
- Boateng, J.; Catanzano, O. Advanced therapeutic dressings for effective wound healing—A review. J. Pharm. Sci. 2015, 104, 3653–3680. [Google Scholar] [CrossRef] [PubMed]
- Hanafiah, Z.; Potparic, O.; Fernandez, T. Addressing pain in burn injury. Curr. Anaesth. Crit. Care 2008, 19, 287–292. [Google Scholar] [CrossRef]
- Shemesh, M.; Zilberman, M. Structure-property effects of novel bioresorbable hybrid structures with controlled release of analgesic drugs for wound healing applications. Acta Biomater. 2014, 10, 1380–1391. [Google Scholar] [CrossRef] [PubMed]
- Morgado, P.I.; Miguel, S.P.; Correia, I.J.; Aguiar-Ricardo, A. Ibuprofen loaded PVA/chitosan membranes: A highly efficient strategy towards an improved skin wound healing. Carbohydr. Polym. 2017, 159, 136–145. [Google Scholar] [CrossRef] [PubMed]
- Chang, Y.C.; Wang, J.D.; Hahn, R.A.; Gordon, M.K.; Joseph, L.B.; Heck, D.E.; Heindel, N.D.; Young, S.C.; Sinko, P.J.; Casillas, R.P.; et al. Therapeutic potential of a non-steroidal bifunctional anti-inflammatory and anti-cholinergic agent against skin injury induced by sulfur mustard. Toxicol. Appl. Pharmacol. 2014, 280, 236–244. [Google Scholar] [CrossRef] [PubMed]
- Norman, A.T.; Judkins, K.C. Pain in the patient with burns. Contin. Educ. Anaesth. Crit. Care Pain 2004, 4, 57–61. [Google Scholar] [CrossRef]
- Ghica, M.V.; Kaya, D.A.; Albu, M.G.; Popa, L.; Dinu-Pîrvu, C.E.; Cristescu, I.; Udeanu, D.I. Ibuprofen-collagen sponges for wound healing. In Proceedings of the 5th International Conference on Advanced Materials and Systems, Bucharest, Romania, 23–25 October 2014; pp. 213–218. [Google Scholar]
- Rasekh, M.; Karavasili, C.; Soong, Y.L.; Bouropoulos, N.; Morris, M.; Armitage, D.; Li, X.; Fatouros, D.G.; Ahmad, Z. Electrospun PVP-indomethacin constituents for transdermal dressings and drug delivery devices. Int. J. Pharm. 2014, 473, 95–104. [Google Scholar] [CrossRef] [PubMed]
- El-Badry, M.; Fetih, G. Preparation, characterization and anti-inflammatory activity of celecoxib chitosan gel formulations. J. Drug Deliv. Sci. Technol. 2011, 21, 201–206. [Google Scholar] [CrossRef]
- Ferreira, H.; Matamá, T.; Silva, R.; Silva, C.; Gomes, A.C.; Cavaco-Paulo, A. Functionalization of gauzes with liposomes entrapping an anti-inflammatory drug: A strategy to improve wound healing. React. Funct. Polym. 2013, 73, 1328–1334. [Google Scholar] [CrossRef] [Green Version]
- Ibolya, F.; Gyéresi, A.; Szabó-Révész, P.; Aigner, Z. Solid dispersions of flufenamic acid with PEG 4000 and PEG 6000. Farmacia 2011, 59, 60–69. [Google Scholar]
- Mohamed, A.A.; Matijević, E. Preparation and characterization of uniform particles of flufenamic acid and its calcium and barium salts. J. Colloid. Interface Sci. 2012, 381, 198–201. [Google Scholar] [CrossRef] [PubMed]
- Rubio, L.; Alonso, C.; Rodríguez, G.; Cócera, M.; López-Iglesias, C.; Coderch, L.; De la Maza, A.; Parra, J.L.; López, O. Bicellar systems as new delivery strategy for topical application of flufenamic acid. Int. J. Pharm. 2013, 444, 60–69. [Google Scholar] [CrossRef] [PubMed]
- Baek, J.S.; Yeo, E.W.; Lee, Y.H.; Tan, N.S.; Loo, S.C.J. Controlled-release nanoencapsulating microcapsules to combat inflammatory diseases. Drug Des. Dev. Ther. 2017, 11, 1707–1717. [Google Scholar] [CrossRef] [PubMed]
- Malinovskaja-Gomez, K.; Labouta, H.I.; Schneider, M.; Hirvonen, J.; Laaksonen, T. Transdermal iontophoresis of flufenamic acid loaded PLGA nanoparticles. Eur. J. Pharm. Sci. 2016, 89, 154–162. [Google Scholar] [CrossRef] [PubMed]
- Mahrhauser, D.S.; Kählig, H.; Partyka-Jankowska, E.; Peterlik, H.; Binder, L.; Kwizda, K.; Valenta, C. Investigation of microemulsion microstructure and its impact on skin delivery of flufenamic acid. Int. J. Pharm. 2015, 490, 292–297. [Google Scholar] [CrossRef] [PubMed]
- Huang, S.; Fu, X. Naturally derived materials-based cell and drug delivery systems in skin regeneration. J. Control. Release 2010, 142, 149–159. [Google Scholar] [CrossRef] [PubMed]
- Elsner, J.J.; Zilberman, M. Novel antibiotic-eluting wound dressings: An in vitro study and engineering aspects in the dressing’s design. J. Tissue Viabil. 2010, 19, 54–66. [Google Scholar] [CrossRef] [PubMed]
- Hu, D.; Qiang, T.; Wang, L. Quaternized chitosan/polyvinyl alcohol/sodium carboxymethylcellulose blend film for potential wound dressing application. Wound Med. 2017, 16, 15–21. [Google Scholar] [CrossRef]
- Brichacek, M.; Ning, C.; Gawaziuk, J.P.; Liu, S.; Logsetty, S. In vitro measurements of burn dressing adherence and the effect of interventions on reducing adherence. Burns 2017, 43, 1002–1010. [Google Scholar] [CrossRef] [PubMed]
- Khalid, A.; Khan, R.; Ul-Islam, M.; Khan, T.; Wahid, F. Bacterial cellulose-zinc oxide nanocomposites as a novel dressing system for burn wounds. Carbohydr. Polym. 2017, 64, 214–221. [Google Scholar] [CrossRef] [PubMed]
- Vedakumari, W.S.; Ayaz, N.; Karthick, A.S.; Senthil, R.; Sastry, T.P. Quercetin impregnated chitosan-fibrin composite scaffolds as potential wound dressing materials—Fabrication, characterization and in vivo analysis. Eur. J. Pharm. Sci. 2017, 97, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Puoci, F.; Piangiolino, C.; Givigliano, F.; Parisi, O.I.; Cassano, R.; Trombino, S.; Curcio, M.; Iemma, F.; Cirillo, G.; Spizzirri, U.G.; et al. Ciprofloxacin-collagen conjugate in the wound healing treatment. J. Funct. Biomater. 2012, 3, 361–371. [Google Scholar] [CrossRef] [PubMed]
- Albu, M.G.; Titorencu, I.; Ghica, M.V. Collagen-based drug delivery systems for tissue engineering. In Biomaterials Applications for Nanomedicine; Pignatello, R., Ed.; InTech Open Acces Publisher: Rijeka, Croatia, 2011; pp. 333–358. ISBN 978-953-307-661-4. [Google Scholar]
- Ghica, M.V.; Albu, M.G.; Popa, L.; Moisescu, S. Response surface methodology and Taguchi approach to assess the combined effect of formulation factors on minocycline delivery from collagen sponges. Pharmazie 2013, 68, 340–348. [Google Scholar] [PubMed]
- Ghica, M.V.; Albu, M.G.; Leca, M.; Popa, L.; Moisescu, S. Design and optimization of some collagen-minocycline based hydrogels potentially applicable for the treatment of cutaneous wounds infections. Pharmazie 2011, 66, 853–861. [Google Scholar] [PubMed]
- Antoniac, I.V.; Albu, M.G.; Antoniac, A.; Rusu, L.C.; Ghica, M.V. Collagen-bioceramic smart composites. In Handbook of Bioceramics and Biocomposites; Antoniac, I.V., Ed.; Springer: Basel, Switzerland, 2016; pp. 301–324. ISBN 978-3-319-12459-9. [Google Scholar]
- Abou Neel, E.A.; Bozec, L.; Knowles, J.C.; Syed, O.; Mudera, V.; Day, R.; Hyun, J.K. Collagen-emerging collagen based therapies hit the patient. Adv. Drug Deliv. Rev. 2013, 65, 429–456. [Google Scholar] [CrossRef] [PubMed]
- Nunes, P.S.; Rabelo, A.S.; Souza, J.C.; Santana, B.V.; da Silva, T.M.; Serafini, M.R.; Dos Passos Menezes, P.; Dos Santos Lima, B.; Cardoso, J.C.; Alves, J.C.; et al. Gelatin-based membrane containing usnic acid-loaded liposome improves dermal burn healing in a porcine model. Int. J. Pharm. 2016, 513, 473–482. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Li, K.; Xiao, W.; Zheng, L.; Xiao, Y.; Fan, H.; Zhang, X. Preparation of collagen-chondroitin sulfate-hyaluronic acid hybrid hydrogel scaffolds and cell compatibility in vitro. Carbohydr. Polym. 2011, 84, 118–125. [Google Scholar] [CrossRef]
- Lungu, A.; Titorencu, I.; Albu, M.G.; Florea, N.M.; Vasile, E.; Iovu, H.; Jinga, V.; Simionescu, M. The effect of BMP-4 loaded in 3D collagen-hyaluronic acid scaffolds on biocompatibility assessed with MG 63 osteoblast-like cells. Dig. J. Nanomater. Biostruct. 2011, 6, 1897–1908. [Google Scholar]
- Coelho, J.F.; Ferreira, P.C.; Alves, P.; Cordeiro, R.; Fonseca, A.C.; Góis, J.R.; Gil, M.H. Drug delivery systems: Advanced technologies potentially applicable in personalized treatments. EMPA 2010, 1, 164–209. [Google Scholar] [CrossRef] [PubMed]
- Unnithan, A.R.; Barakat, N.A.; Tirupathi Pichiah, P.B.; Gnanasekaran, G.; Nirmala, R.; Cha, Y.S.; Jung, C.H.; El-Newehy, M.; Kim, H.Y. Wound-dressing materials with antibacterial activity from electrospun polyurethane-dextran nanofiber mats containing ciprofloxacin HCl. Carbohydr. Polym. 2012, 90, 1786–1793. [Google Scholar] [CrossRef] [PubMed]
- Liao, N.; Unnithan, A.R.; Joshi, M.K.; Tiwari, A.P.; Hong, S.T.; Park, C.H.; Kima, C.S. Electrospun bioactive poly (ε-caprolactone)—Cellulose acetate-dextran antibacterial composite mats for wound dressing applications. Colloids Surf. A Physicochem. Eng. Asp. 2015, 469, 194–201. [Google Scholar] [CrossRef]
- Kim, M.K.; Kwak, H.W.; Kim, H.H.; Kwon, T.R.; Kim, S.Y.; Kim, B.J.; Park, Y.H.; Lee, K.H. Surface modification of silk fibroin nanofibrous mat with dextran for wound dressing. Fiber Polym. 2014, 15, 1137–1145. [Google Scholar] [CrossRef]
- Albu, M.G. Collagen Gels and Matrices for Biomedical Applications; Lambert Academic Publishing: Saarbrücken, Germany, 2011; ISBN 978-01-9850-970-7. [Google Scholar]
- Kumar, M.S.; Kirubanandan, S.; Sripriya, R.; Sehgal, P.K. Triphala incorporated collagen sponge—A smart biomaterial for infected dermal wound healing. J. Surg. Res. 2010, 58, 162–170. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.H.; Lee, Y. Collagen-based formulations for wound healing applications. In Wound Healing Biomaterials; Ågren, M., Ed.; Woodhead Publishing, Elsevier: Cambridge, UK, 2016; Volume 2, pp. 135–149. ISBN 978-1-78242-456-7. [Google Scholar]
- De Almeida, E.B.; Cardoso, J.C.; de Lima, A.K.; de Oliveira, N.L.; de Pontes-Filho, N.T.; Lima, S.O.; Souza, I.C.L.; de Albuquerque-Júnior, R.L.C. The incorporation of Brazilian propolis into collagen-based dressing films improves dermal burn healing. J. Ethnopharmacol. 2013, 147, 419–425. [Google Scholar] [CrossRef] [PubMed]
- Akturk, O.; Tezcaner, A.; Bilgili, H.; Deveci, M.S.; Gecit, M.R.; Keskin, D. Evaluation of sericin/collagen membranes as prospective wound dressing biomaterial. J. Biosci. Bioeng. 2011, 112, 279–288. [Google Scholar] [CrossRef] [PubMed]
- Metzmacher, I.; Radu, F.; Bause, M.; Knabner, P. A model describing the effect of enzymatic degradation on drug release from collagen minirods. Eur. J. Pharm. Biopharm. 2007, 67, 349–360. [Google Scholar] [CrossRef] [PubMed]
- Radu, F.A.; Bause, M.; Knabner, P.; Friess, W.; Metzmacher, I. Numerical simulation of drug release from collagen matrices by enzymatic degradation. Comput. Vis. Sci. 2009, 12, 409–420. [Google Scholar] [CrossRef]
- Boateng, J.S.; Matthews, K.H.; Stevens, H.N.E.; Eccleston, G.M. Wound healing dressings and drug delivery systems: A review. J. Pharm. Sci. 2008, 97, 2892–2923. [Google Scholar] [CrossRef] [PubMed]
- Siafaka, P.I.; Zisi, A.P.; Exindari, M.K.; Karantas, I.D.; Bikiaris, D.N. Porous dressings of modified chitosan with poly(2-hydroxyethyl acrylate) for topical wound delivery of levofloxacin. Carbohydr. Polym. 2016, 143, 90–99. [Google Scholar] [CrossRef] [PubMed]
- Abdelbary, A.A.; AbouGhaly, M.H.H. Design and optimization of topical methotrexate loaded niosomes for enhanced management of psoriasis: Application of Box-Behnken design, in vitro evaluation and in vivo skin deposition study. Int. J. Pharm. 2015, 485, 235–243. [Google Scholar] [CrossRef] [PubMed]
- Dinarvand, M.; Rezaee, M.; Foroughi, M. Optimizing culture conditions for production of intra and extracellular inulinase and invertase from Aspergillus niger ATCC 20611 by response surface methodology (RSM). Braz. J. Microbiol. 2017, 48, 427–441. [Google Scholar] [CrossRef] [PubMed]
- Koca, S.; Aksoy, D.O.; Cabuk, A.; Celik, P.A.; Sagol, E.; Toptas, Y.; Oluklulu, S.; Koca, H. Evaluation of combined lignite cleaning processes, flotation and microbial treatment, and its modelling by Box Behnken methodology. Fuel 2017, 192, 178–186. [Google Scholar] [CrossRef]
- Moghddam, S.R.M.; Ahad, A.; Aqil, M.; Imam, S.S.; Sultana, Y. Formulation and optimization of niosomes for topical diacerein delivery using 3-factor, 3-level Box-Behnken design for the management of psoriasis. Mater. Sci. Eng. C Mater. Biol. Appl. 2016, 69, 789–797. [Google Scholar] [CrossRef] [PubMed]
- Tan, Y.H.; Abdullah, M.O.; Nolasco-Hipolito, C.; Zauzi, N.S.A. Application of RSM and Taguchi methods for optimizing the transesterification of waste cooking oil catalyzed by solid ostrich and chicken-eggshell derived CaO. Renew. Energy 2017, 114, 437–447. [Google Scholar] [CrossRef]
- Tumbas Šaponjac, V.; Čanadanović-Brunet, J.; Ćetković, G.; Jakišić, M.; Djilas, S.; Vulić, J.; Stajčić, S. Encapsulation of beetroot pomace extract: RSM optimization, storage and gastrointestinal stability. Molecules 2016, 21, 584. [Google Scholar] [CrossRef] [PubMed]
- Li, H.Z.; Zhang, Z.J.; Hou, T.Y.; Li, X.J.; Chen, T. Optimization of ultrasound-assisted hexane extraction of perilla oil using response surface methodology. Ind. Crops Prod. 2015, 76, 18–24. [Google Scholar] [CrossRef]
- Wang, H.; Liu, Y.; Wei, S.; Yan, Z. Application of response surface methodology to optimise supercritical carbon dioxide extraction of essential oil from Cyperus rotundus Linn. Food Chem. 2012, 132, 582–587. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, X.H.; Bae, W.; Gunadi, T.; Park, Y. Using response surface design for optimizing operating conditions in recovering heavy oil process, Peace River oil sands. J. Pet. Sci. Eng. 2017, 17, 37–45. [Google Scholar] [CrossRef]
- Ghica, M.V.; Popa, L.; Saramet, G.; Leca, M.; Lupuliasa, D.; Moisescu, S. Optimization of the pharmaceutical products and process design applying Taguchi quality engineering principles. Farmacia 2011, 59, 321–328. [Google Scholar]
- Apparao, K.C.; Birru, A.K. Optimization of die casting process based on Taguchi approach. Mater. Today Proc. 2017, 4, 1852–1859. [Google Scholar] [CrossRef]
- Raza, Z.A.; Anwar, F. Fabrication of chitosan nanoparticles and multi-response optimization in their application on cotton fabric by using a Taguchi approach. Nano Struct. Nano Obj. 2017, 10, 80–90. [Google Scholar] [CrossRef]
- Yang, Q.; Zhong, Y.; Zhong, H.; Li, X.; Du, W.; Li, X.; Chen, R.; Zeng, G. A novel pretreatment process of mature landfilleachate with ultrasonic activated persulfate: Optimization using integrated Taguchi method and response surface methodology. Process Saf. Environ. Prot. 2015, 98, 268–275. [Google Scholar] [CrossRef]
- Ramli, N.A.; Wong, T.W. Sodium carboxymethylcellulose scaffolds and their physicochemical effects on partial thickness wound healing. Int. J. Pharm. 2011, 403, 73–82. [Google Scholar] [CrossRef] [PubMed]
- Perumal, S.; Ramadass, S.K.; Madhan, B. Sol-gel processed mupirocin silica microspheres loaded collagen scaffold: A synergistic bio-composite for wound healing. Eur. J. Pharm. Sci. 2014, 52, 26–33. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Niu, Y.; Chen, K.C.; Chen, S. Rapid hemostatic and mild polyurethane-urea foam wound dressing for promoting wound healing. Mater. Sci. Eng. C 2017, 71, 289–297. [Google Scholar] [CrossRef] [PubMed]
- Oyinade, A.; Kovo, A.S.; Hill, P. Synthesis, characterization and ion exchange isotherm of zeolite Y using Box–Behnken design. Adv. Powder Technol. 2016, 27, 750–755. [Google Scholar] [CrossRef]
- Ba-Abbad, M.M.; Chai, P.V.; Takriff, M.S.; Benamor, A.; Mohammad, A.W. Optimization of nickel oxide nanoparticle synthesis through the sol-gel method using Box—Behnken design. Mater. Des. 2015, 86, 948–956. [Google Scholar] [CrossRef]
- Tavakoli, J.; Tang, Y. Honey/PVA hybrid wound dressings with controlled release of antibiotics: Structural, physico-mechanical and in vitro biomedical studies. Mater. Sci. Eng. C 2017, 77, 318–325. [Google Scholar] [CrossRef] [PubMed]
- Morgado, P.I.; Lisboa, P.F.; Ribeiro, M.P.; Miguel, S.P.; Simões, P.C.; Correia, I.J.; Aguiar-Ricardo, A. Poly(vinyl alcohol)/chitosan asymmetrical membranes: Highly controlled morphology toward the ideal wound dressing. J. Membr. Sci. Technol. 2017, 159, 262–271. [Google Scholar] [CrossRef]
- Ritger, P.L.; Peppas, N.A. A simple equation for description of solute release II. Fickian and anomalous release from swellable devices. J. Control Release 1987, 5, 37–42. [Google Scholar] [CrossRef]
- Ritger, P.L.; Peppas, N.A. A simple equation for description of solute release I Fickian and non-fickian release from non-swellable devices in the form of slabs, spheres, cylinders or discs. J. Control. Release 1987, 5, 23–36. [Google Scholar] [CrossRef]
- Higuchi, W.I. Analysis of data on the medicament release from ointments. J. Pharm. Sci. 1962, 51, 802–804. [Google Scholar] [CrossRef] [PubMed]
- Ghica, M.V.; Ficai, A.; Marin, Ș.; Marin, M.; Ene, A.M.; Pătraşcu, J.M. Collagen/bioactive glass ceramic/doxycycline composites for bone defects. Rev. Rom. Mater. 2015, 45, 307–314. [Google Scholar]
- Paunică-Panea, G.; Ficai, A.; Marin, M.M.; Marin, S.; Albu, M.G.; Constantin, V.D.; Dinu-Pîrvu, C.; Vuluga, Z.; Corobea, M.C.; Ghica, M.V. New collagen-dextran-zinc oxide composites for wound dressing. J. Nanomater. 2016, 2016. [Google Scholar] [CrossRef]
- Albu, M.G.; Ghica, M.V. Spongious collagen-minocycline delivery systems. Farmacia 2015, 63, 20–25. [Google Scholar]
Sample Availability: No samples of the compounds are available from the authors. |
| Independent Variables | Coded Symbol | Coded and Uncoded Variation Levels | ||
|---|---|---|---|---|
| Low (1) | Middle (2) | High (3) | ||
| Collagen, C (g%) | X1 | 0.8 | 1.0 | 1.2 |
| Dextran, DX (g%) * | X2 | 0.0 | 0.6 | 1.2 |
| Glutaraldehyde, GA (g%) * | X3 | 0.0 | 0.0060 | 0.012 |
| Dependent Variables | Coded Symbol | Constraints | ||
| Swelling ratio, SR (g/g) | Y1 | Maximize | ||
| Released percent, RP (%) | Y2 | Maximize | ||
| Weight loss, WL (%) | Y3 | Minimize | ||
| Trials No. | Exp. Name | Independent Variables (Coded Level/Physical Level) | Responses | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| X1—C | X2—DX | X3—GA | Y1—SR (g/g) | Y2—RP (%) | Y3—WL (%) | |||||
| Obs. | Pred. | Obs. | Pred. | Obs. | Pred. | |||||
| 1 | M1 | 1 (0.8) | 1 (0.0) | 2 (0.006) | 45.65 | 45.81 | 75.13 | 75.41 | 38.02 | 36.77 |
| 2 | M2 | 3 (1.2) | 1 (0.0) | 2 (0.006) | 28.41 | 28.91 | 76.51 | 75.60 | 32.49 | 31.37 |
| 3 | M3 | 1 (0.8) | 3 (1.2) | 2 (0.006) | 40.14 | 39.81 | 86.81 | 87.43 | 34.20 | 33.54 |
| 4 | M4 | 3 (1.2) | 3 (1.2) | 2 (0.006) | 36.16 | 36.21 | 87.28 | 87.62 | 26.62 | 26.53 |
| 5 | M5 | 1 (0.8) | 2 (0.6) | 1 (0.000) | 38.77 | 39.34 | 88.38 | 87.65 | 36.42 | 37.21 |
| 6 | M6 | 3 (1.2) | 2 (0.6) | 1 (0.000) | 26.52 | 27.24 | 84.81 | 85.66 | 30.66 | 31.01 |
| 7 | M7 | 1 (0.8) | 2 (0.6) | 3 (0.012) | 31.56 | 31.34 | 79.12 | 78.94 | 27.32 | 28.97 |
| 8 | M8 | 3 (1.2) | 2 (0.6) | 3 (0.012) | 24.05 | 22.94 | 81.61 | 81.31 | 21.48 | 22.77 |
| 9 | M9 | 2 (1.0) | 1 (0.0) | 1 (0.000) | 37.23 | 36.12 | 83.38 | 82.11 | 35.36 | 36.40 |
| 10 | M10 | 2 (1.0) | 3 (1.2) | 1 (0.000) | 42.88 | 42.35 | 93.51 | 94.13 | 31.56 | 32.37 |
| 11 | M11 | 2 (1.0) | 1 (0.0) | 3 (0.012) | 35.13 | 35.55 | 73.69 | 75.58 | 28.40 | 28.15 |
| 12 | M12 | 2 (1.0) | 3 (1.2) | 3 (0.012) | 29.83 | 30.62 | 89.19 | 87.60 | 25.83 | 24.12 |
| 13 | M13 | 2 (1.0) | 2 (0.6) | 2 (0.006) | 33.59 | 33.61 | 95.09 | 95.43 | 33.24 | 32.32 |
| Formulation | Higuchi Model | Power Law Model | Release Exponent | Kinetic Constant (1/minn) |
|---|---|---|---|---|
| M1 | 0.9296 | 0.9727 | 0.33 | 0.094 |
| M2 | 0.9698 | 0.9803 | 0.41 | 0.056 |
| M3 | 0.9452 | 0.9730 | 0.37 | 0.089 |
| M4 | 0.9206 | 0.9577 | 0.36 | 0.099 |
| M5 | 0.9679 | 0.9945 | 0.35 | 0.095 |
| M6 | 0.9739 | 0.9830 | 0.42 | 0.062 |
| M7 | 0.9006 | 0.9531 | 0.33 | 0.108 |
| M8 | 0.9355 | 0.9618 | 0.38 | 0.079 |
| M9 | 0.9851 | 0.9932 | 0.41 | 0.060 |
| M10 | 0.9637 | 0.9779 | 0.40 | 0.077 |
| M11 | 0.9672 | 0.9807 | 0.41 | 0.057 |
| M12 | 0.9659 | 0.9822 | 0.39 | 0.076 |
| M13 | 0.9375 | 0.9740 | 0.34 | 0.110 |
| Responses | Sources of Variation | Sum of Squares | df | Mean Squares | F-Value | p-Value |
|---|---|---|---|---|---|---|
| Y1 | Regression | 491.473 | 7 | 70.210 0.963 | 72.862 | 0.000099 <0.001 |
| Residual | 4.8180 | 5 | ||||
| Total | 496.291 | 12 | ||||
| Y2 | Regression | 538.351 | 6 | 89.725 1.834 | 48.907 | 0.000078 <0.001 |
| Residual | 11.007 | 6 | ||||
| Total | 549.358 | 12 | ||||
| Y3 | Regression | 258.315 | 3 | 86.105 1.550 | 55.54 | 0.000004 <0.001 |
| Residual | 13.953 | 9 | ||||
| Total | 272.268 | 12 |
| Control Factors (Independent Variables) | Y1 | Y2 | Y3 | |||
|---|---|---|---|---|---|---|
| “Larger—the—Better” | Effect Size | “Larger—the—Better” | Effect Size | “Smaller—the—Better” | Effect Size | |
| X1 | 1 | 1.112 | 2 | 0.272 | 3 | 0.918 |
| X2 | 3 | 0.702 | 3 | 0.523 | 2 | 0.343 |
| X3 | 2 | 0.563 | 1 | 0.354 | 3 | 1.526 |
| S/N ratio expected (dB) | 33.018 | 39.629 | −26.909 | |||
| S/N ratio observed (dB) | 32.072 | 39.417 | −26.641 | |||
| Spongious Matrices | Composition of Optimal Formulation | Response Variable | Observed Value | Predictive Value | Predicted Error (%) |
|---|---|---|---|---|---|
| X1:X2:X3 | |||||
| C:DX:GA | |||||
| (g%:g%:g%) | |||||
| M3 | 0.8:1.2:0.006 | Y1 (g/g) | 40.14 | 39.81 | +0.82 |
| Y2 (%) | 86.81 | 87.43 | −0.71 | ||
| Y3 (%) | 34.20 | 33.54 | +1.97 | ||
| M8 | 1.2:0.6:0.012 | Y1 (g/g) | 24.05 | 22.94 | +4.84 |
| Y2 (%) | 81.61 | 81.31 | +0.37 | ||
| Y3 (%) | 21.48 | 22.77 | −5.67 | ||
| M10 | 1.0:1.2:0.000 | Y1 (g/g) | 42.88 | 42.35 | +1.25 |
| Y2 (%) | 93.51 | 94.13 | −0.65 | ||
| Y3 (%) | 31.56 | 32.37 | −2.50 |
| Wound Diameter (mm) | M3 Group | M8 Group | M10 Group | Control Group | ||||
|---|---|---|---|---|---|---|---|---|
| Mean | SEM | Mean | SEM | Mean | SEM | Mean | SEM | |
| Day 1 | 10 | 0 | 10 | 0 | 10 | 0 | 10 | 0 |
| Day 5 | 6.4 * | 1.03 | 6.8 ** | 0.58 | 7.4 ** | 0.51 | 9.4 | 0.24 |
| Day 7 | 6 ** | 0.89 | 6.8 ** | 0.37 | 7.4 *** | 0.24 | 9.2 | 0.20 |
| Day 10 | 5.4 ** | 0.51 | 6.8 * | 0.58 | 7 * | 0.32 | 8.2 | 0.37 |
| Day 13 | 1.8 * | 0.80 | 3.4 | 1.40 | 2.2 | 1.36 | 5.6 | 0.24 |
| Day 15 | 1.4 * | 0.87 | 0 | 0 | 0 | 0 | 1.6 | 0.98 |
| Day 17 | 0 | 0 | 0 | 0 | 0 | 0 | 0.6 | 0.60 |
| Day 21 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ghica, M.V.; Albu Kaya, M.G.; Dinu-Pîrvu, C.-E.; Lupuleasa, D.; Udeanu, D.I. Development, Optimization and In Vitro/In Vivo Characterization of Collagen-Dextran Spongious Wound Dressings Loaded with Flufenamic Acid. Molecules 2017, 22, 1552. https://doi.org/10.3390/molecules22091552
Ghica MV, Albu Kaya MG, Dinu-Pîrvu C-E, Lupuleasa D, Udeanu DI. Development, Optimization and In Vitro/In Vivo Characterization of Collagen-Dextran Spongious Wound Dressings Loaded with Flufenamic Acid. Molecules. 2017; 22(9):1552. https://doi.org/10.3390/molecules22091552
Chicago/Turabian StyleGhica, Mihaela Violeta, Mădălina Georgiana Albu Kaya, Cristina-Elena Dinu-Pîrvu, Dumitru Lupuleasa, and Denisa Ioana Udeanu. 2017. "Development, Optimization and In Vitro/In Vivo Characterization of Collagen-Dextran Spongious Wound Dressings Loaded with Flufenamic Acid" Molecules 22, no. 9: 1552. https://doi.org/10.3390/molecules22091552




