Anti-Trypanosomal Activity of Nigerian Plants and Their Constituents
Abstract
:1. Introduction
2. Acanthaceae, Amaryllidaceae, Anacardiaceae, Annonaceae, Apocynaceae, Araceae, Asclepiadaceae, Asteraceae and Burseraceae
| Family | Species | Traditional Uses | Plant Part | Ref. |
|---|---|---|---|---|
| Acanthaceae | Peristrophe bicalyculata | skin diseases, antidote for snake poison, diabetes | WP | [34] |
| Amaryllidaceae | Allium sativum | diabetes, tetanus, swellings | WP | [37] |
| Anacardiaceae | Lannea kerstingii | diarrhoea, cancer | R | [39] |
| Mangifera indica | clearing digestion and acidity due to pitta | R | [39] | |
| Spondias mombim | used as febrifuge and diuretic | R | [43] | |
| Lannea welwistchii | diarrhoea, dysentery, dropsy | L | [44] | |
| Haematostaphis barteri | trypanosomiasis | SB | [45] | |
| Annonaceae | Monodora myristica | stomachic, headaches, sores | SD | [43] |
| Anonna senegalensis | food and pneumonia | L, R, SB | [40] | |
| Apocynaceae | Carissa spinarum | analgesic | R | [47] |
| Adenium obesum | arrow poison for hunting | R | [39] | |
| Carrisa edulis | rheumatism, stomach disorder | R, B, L | [49] | |
| Holarrhena africana | dysentery, diarrhoea, snakebite, infertility, malarial, diabetics | L | [42] | |
| Saba florida | rheumatism, antidote against vomiting, diarrhoea and food poison | L | [50] | |
| Araceae | Anchomanes difformis | diabetes, diarrhoea | R | [48] |
| Asclepiadaceae | Gongronema latifolium | diabetes, high blood pressure | L, SB | [52] |
| Asteraceae | Tridax procumbens | inflammatory, microbial and protozoal diseases | WP | [53] |
| Artemisia maritima | worm, stomachic infusion | WP | [57] | |
| Burseraceae | Boswellia dalzielii | wound healing, diarrhea, syphilis, induce vomiting | L, SB, Re | [59] |
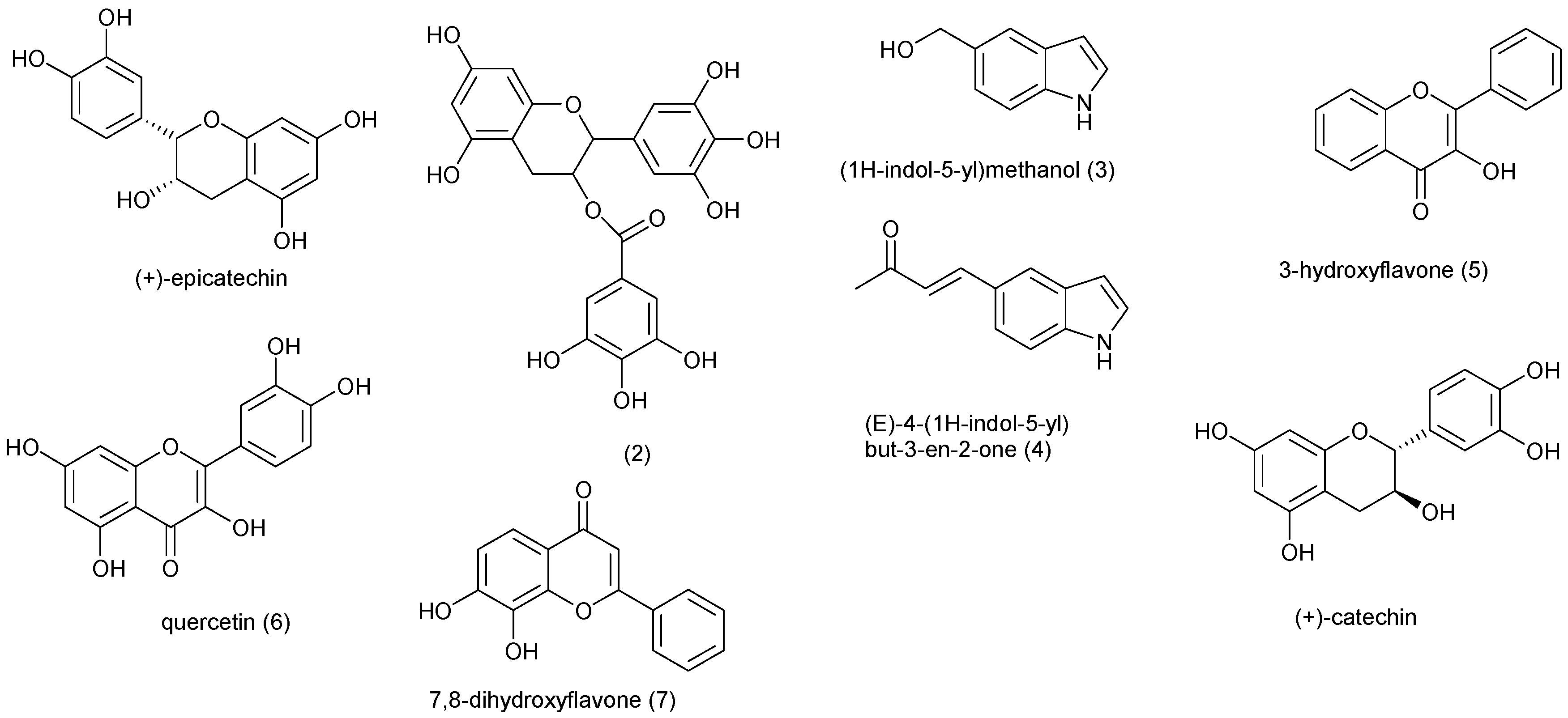
3. Capparaceae, Celastraceae, Clusiaceae, Combretaceae, Cucurbitaceae, Ebenaceae and Euphorbiaceae
| Family | Species | Traditional Uses | Plant Part | Ref. |
|---|---|---|---|---|
| Capparaceae | Crateva adansonii | stomach troubles, syphilis, jaundice and yellow fevers | L | [62] |
| Buchholzia coriacea | feverish, malaria | SD | [64] | |
| Celastraceae | Maytenus laevis | anti-inflammatory, analgesic | R | [67] |
| Clusiaceae | Garcinia kola | purgative, antiparasitic, antimicrobial | SD | [68] |
| Combretaceae | Anogeissus leiocarpus | trypanosomiasis, babesiosis | R, SB | [69] |
| Terminalia avicennioides | cancer, fungal, bacterial infections | B | [70] | |
| Terminalia superba | furniture making and musical instrument | B | [44] | |
| Cucurbitaceae | Mormordica balsamina | used to treat wound | WP | [48] |
| Ebenaceae | Diospyros mespiliformis | styptic to staunch bleeding, leprosy | L | [39] |
| Euphorbiaceae | Euphorbia poisonii | latex used as pesticides | B | [43] |
| Alchornea cordifolia | eye treatment, venereal diseases | S | [43] |

4. Fabaceae, Fagaceae, Hymenocardiaceae, Lamiaceae, Lauraceae, Loganiaceae, Lythraceae, Malvaceae and Melastomataceae

5. Meliaceae, Moraceae, Moringaceae, Myrtaceae, Ochnaceae, Phyllanthaceae, Poaceae, Polygalaceae, Rubiaceae, Rutaceae, Solanaceae, Ulmaceae, Verbenaceace, Vitaceae, Zingiberaceae
| Family | Species | Traditional Uses | Plant Part | Ref. |
|---|---|---|---|---|
| Fabaceae | Acacia nilotica | used to treat cancers and/or tumours of ear, eye | SB | [72,73] |
| Afzelia Africana | trypanosomiasis, convulsion, hernia | WP | [74] | |
| Parkia clappertoniana | dental caries, conjunctivitis | R | [75] | |
| Piliostigma reticulatum | ulcer, boils, wounds, cancer, syphilis and diarrhoea | L | [76] | |
| Prosopis Africana | used to prepare food in Northern Nigeria | SB | [77] | |
| Afrormosia laxiflora | epilepsy and psychosis | L | [39] | |
| Erythrophleum suaveolus | arthritis, rheumatism, dropsy, swelling, eye treatment, laxative | SB | [39] | |
| Lonchocarpus laxiflorus | dermatitis, headache, intestinal worm, jaundice, ulcer, anthelmintic | SB | [48] | |
| Swartzia madagascariensis | poison arrow and fishing, insecticide | R | [48] | |
| Senna occidentalis | bacterial and malaria infections | L | [ 89] | |
| Fagaceae | Quercus borealis | dyspnea, nausea, emesis, diarrhoea and muscular pain | L | [78] |
| Hymenocardiaceae | Hymenocardia acida | Hypertension | R, SB | [80] |
| Lamiaceae | Ocimum gratissimum | the oil is medicine for respiratory tract infections, diarrhoea, eye problem, skin diseases | L | [88] |
| Hyptis spicigera | Cold, insecticides | L | [59] | |
| Lauraceae | Cassytha filiformis | food and infectious diseases | L, S | [48] |
| Loganiaceae | Anthocleista vogelii | purgative, diuretic, ulcer, stomach-ache | R, SB | [87] |
| Strychnos spinosa | taken by lactating women to stimulate breast milk production | L | [96] | |
| Loranthaceae | Tapinanthus globiferus | hypertension epilepsy, relief pain, tinnitus and trypanosomiasis | L, SB | [99] |
| Lythraceae | Lawsonia inermis | used to adorn women’s bodies as part of social and holiday celebration | L | [39] |
| Punica granatum | diarrhoea, dysentery | L | [100] | |
| Malvaceae | Bombax buonopozense | to treat edema | SB | [102] |
| Adansonia digitata | to treat cancer | SD | [101] | |
| Sterculia setigera | used as a thickener and emulsifier | R | [39] | |
| Melastomataceae | Heterotis rotundifolia | malaria, rheumatism, diarrhoea | WP | [102] |
| Dissotis rotundifolia | trypanosomiasis treatment | L | [104] |
| Family | Species | Traditional Uses | Plant Part | Ref. |
|---|---|---|---|---|
| Meliaceae | Khaya senegalensis | to treat malaria | L, AS | [109] |
| Pseudocedrella kotschi | to treat diarrhoea, dysentery, epilepsy | SB | [39] | |
| Moraceae | Ficus sycomorus | to treat snakebite, jaundice, dysentery | SB | [39] |
| Moringaceae | Moringa oleifera | to treat diabetes and intestinal worms | L, S, SB, R | [116] |
| Myrtaceae | Psidium guajava | to treat diarrhoea, hypertension | L | [118] |
| Syzygium guineense | used to bath ill person | SB | [113] | |
| Eucalyptus camaldulensis | used to treat malaria and typhoid fevers | L | [120] | |
| Ochnaceae | Lophira lanceolata | dermatosis, toothache, muscular tiredness | L, SB | [87] |
| Ximenia americana | treatment of fever, jaundice, impotence, sleeping sickness | SB | [123] | |
| Plantaginaceae | Picrorhiza kurroa | to treat asthma, bronchitis, chronic dysentery, malaria | WP | [124] |
| Poaceae | Canarium schweinfurthii | burnt for fumigation | SB | [39] |
| Polygalaceae | Securidaca longepedunculata | to treat cough, chest pain, toothache and diabetes | R | [113] |
| Rubiaceae | Gardenia erubescens | used as dye | L | [92] |
| Nauclea latifolia | to treat fever, dental caries, sceptic mouth, malaria | B | [125] | |
| Nauclea pobeguinii | to treat fever, dental caries, sceptic mouth, malaria | B | [43] | |
| Keetia leucantha | to treat malaria | L | [127] | |
| Mitracarpus scaber | to treat headache, toothache, venereal disease, amenorrhoea, dyspepsia, leprosy | L | [128] | |
| Morinda lucida | used to treat malaria | L | [115] | |
| Rutaceae | Zanthoxylum zanthoxyloides | stomach disorder, worm infection | SB | [70] |
| Solanaceae | Withania somnifera | to treat external tumors, tubercular glands and ulcer | WP | [43] |
| Ulmaceae | Trema orientalis | to treat cough, sore throats, asthma, bronchitis, gonorrhea, yellow fever, toothaches | L | [70] |
| Verbenaceace | Vitex doniana | anemia, gonorrhea, dysentery and to improve fertility | L | [70] |
| Vitex simplicifolia | to treat malaria | L | [131] | |
| Vitaceae | Cissus multistriata | for the management of protein deficiency | L | [130] |
| Zingiberaceae | Zingiber officinale | gastrointestinal diseases, dyspnea, nausea, emesis, diarrhoea and muscular pain | R | [83] |


6. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- D’Archivio, S.; Medina, M.; Cosson, A.; Chamond, N.; Rotureau, B.; Minoprio, P. Genetic engineering of Trypanosoma (Dutonella) vivax and in vitro differentiation under axenic conditions. PLoS Negl. Trop. Dis. 2011, 5, e1461. [Google Scholar] [PubMed]
- Joshua, R.A.; Magaji, Y.; Kayit, Y.S. Isolation of human serum resistant Trypanozoon from cattle in Nigeria. Tropenmedizin Parasitol. 1983, 13, 201–202. [Google Scholar]
- Ayodele, O.M.; Akinyemi, F.; Charles, D.; Kim, P.; Michael, V.T.; Susan, C.W. A Longitudinal Survey of African Animal Trypanosomiasis in Domestic Cattle on the Jos Plateau, Nigeria: Prevalence, Distribution and Risk Factors. Parasites Vectors 2013, 6, 239. [Google Scholar] [CrossRef] [PubMed]
- Airauhi, L.; Unuigbe, E.I.; Airauchi, O.D. Human sleeping sickness (SS) in Nigeria: Knowledge, attitude and beliefs in a focus in the Abraka belt, Delta of Nigeria. Afr. J. Clin. Exp. Microbiol. 2001, 2, 6–9. [Google Scholar]
- Edeghere, H.; Elhassan, E.; Ukah, J.C.A.; Sanda, S.; Ikenga, M.; Audu, G. The scourge of human African trypanosomiasis in Abraka: possible control strategies. Nig. Soc. Parasitol. Abst. 1998, 46, 43. [Google Scholar]
- Bauer, B.; Amsler-Delafosse, S.; Kabore, I.; Kamunga, M. Improvement of cattle productivity through rapid alleviation of African management practice in the Agropastoral zone of Yale, Burkina Faso. Animal trypanosomosis by integrated disease. Trop. Anim. Health Prod. 1999, 31, 89–102. [Google Scholar] [CrossRef] [PubMed]
- Griffin, L.; Allonby, W.E. The economic effect of trypanosomiasis in sheep and goats at a range research station in Kenya. Trop. Anim. Health Prod. 1979, 11, 127–132. [Google Scholar] [CrossRef] [PubMed]
- Mulumba, K. Socio Economic and Agricultural Factors in the Research and Control of Trypanosomiasis; PAAT Technical and Scientific Series 4; FAO/WHO/IAEA/OAU: Rome, Italy, 03 01 2003. [Google Scholar]
- Abenga, J.N.; Lawal, I.A. Implicating roles of animal reservoir host in the resurgence of Gambian trypanosomiasis (Sleeping Sickiness). Afr. J. Biotechnol. 2005, 4, 134–137. [Google Scholar]
- Fact Sheet N°259: Trypanosomiasis, Human African (Sleeping Sickness); WHO Media Centre: Geneva, Switzerland, 1 June. 2013. Available online: http:www.who.int/mediacentre/factsheets/fs259/en (accessed on 27 February 2014).
- Maser, P.; Luscher, A.; Kaminsky, R. Drug transport and drug resistance in African trypanosomes. Drug Resist. Updates 2003, 6, 281–290. [Google Scholar] [CrossRef]
- Amaechi, N. Toxicity of antiprotozoan drug diminazene aceturate in rats. J. Sustain. Agric. Environ. 2001, 3, 365–370. [Google Scholar]
- Kaiser, M.; Bray, M.A.; Cal, M.; Trunz, B.B.; Torreele, E.; Brun, R. Antitrypanosomal activity of Fexinidazole, a new oral Nitroimidazole drug candidate for treatment of sleeping sickness. Antimicrob. Agents Chemother. 2011, 55, 5602–5608. [Google Scholar] [CrossRef] [PubMed]
- Ameenah, G.; Mohamad, F.M. African flora as potential sources of medicinal plants: Towards the chemotherapy of major parasitic and other infectious diseases—A review. Jordan J. Biol. Sci. 2013, 6, 77–84. [Google Scholar] [CrossRef]
- Mbaya, A.W.; Ibrahim, U.I. In vivo and in vitro activities of medicinal plants on haemic and humoral trypanosomes: A review. Int. J. Pharmacol. 2011, 7, 1–11. [Google Scholar]
- Malebo, H.M.; Tanja, W.; Cal, M.; Swaleh, S.A.M.; Omolo, M.O.; Hassanali, A.; Séquin, U.; Hamburger, M.; Brun, R.; Ndiege, I.O. Antiplasmodial, anti-trypanosomal, anti-leishmanial and cytotoxicity activity of selected Tanzanian medicinal plants. Tanzania J. Health Res. 2009, 11, 226–233. [Google Scholar]
- Hoet, S.; Opperdoes, F.; Brun, R.; Quetin-Leclercq, J. Natural products active against African trypanosomes: A step towards new drugs. Nat. Prod. Rep. 2004, 21, 353–364. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, M.A.; Mohammed, A.; Isah, M.B.; Aliyu, A.B. Anti-trypanosomal activity of African medicinal plants: A review update. J. Ethnopharmacol. 2014, 154, 26–54. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, T.J.; Khalid, S.A.; Romanha, A.J.; Alves, T.M.A.; Biavatti, M.W.; Brun, R.; Da Costa, F.B.; de Castro, S.L.; Ferreira, V.F.; de Lacerda, M.V.G.; et al. The Potential of Secondary Metabolites from Plants as Drugs or Leads against Protozoan Neglected Diseases Part I. Curr. Med. Chem. 2012, 19, 2128–2175. [Google Scholar] [PubMed]
- Schmidt, T.J.; Khalid, S.A.; Romanha, A.J.; Alves, T.M.A.; Biavatti, M.W.; Brun, R.; Da Costa, F.B.; de Castro, S.L.; Ferreira, V.F.; de Lacerda, M.V.G.; et al. The Potential of Secondary Metabolites from Plants as Drugs or Leads against Protozoan Neglected Diseases Part II. Curr. Med. Chem. 2012, 19, 2176–2228. [Google Scholar] [PubMed]
- Ogungbe, I.V.; Setzer, W.N. Comparative Molecular Docking of Antitrypanosomal Natural Products into Multiple Trypanosoma brucei Drug Targets. Molecules 2009, 14, 1513–1536. [Google Scholar] [CrossRef] [PubMed]
- Newmann, D.J.; Cragg, G.M. Natural products as sources of new drugs over the 30 years from 1981 to 2010. J. Nat. Prod. 2012, 75, 311–335. [Google Scholar] [CrossRef] [PubMed]
- Matthews, H.B.; Lucier, G.W.; Fisher, K.D. Medicinal herbs in the United States: Research needs. Environ. Health Perspect. 1999, 107, 773–778. [Google Scholar] [CrossRef] [PubMed]
- Yeh, G.Y.; Eisenberg, D.M.; Kaptchuk, T.J.; Phillips, R.S. Systematic review of herbs and dietary supplements for glycemic control in diabetes. Diabetes Care 2003, 26, 1277–1294. [Google Scholar] [CrossRef] [PubMed]
- Hamdan, I.I.; Afifi, F.U. Studies on the in vitro and in vivo hypoglycemic activities of some medicinal plants used in treatment of diabetes in Jordanian traditional medicine. J. Ethnopharmacol. 2004, 93, 117–121. [Google Scholar] [CrossRef] [PubMed]
- Rangasamy, O.; Raoelison, G.; Rakotoniriana, F.E. Screening for anti-infective properties of several medicinal plants of the Mauritians flora. J. Ethnopharmacol. 2007, 109, 331–337. [Google Scholar] [CrossRef] [PubMed]
- Mahomoodally, M.F.; Gurib-Fakim, A.; Subratty, A.H. Antimicrobial activities and phytochemical profiles of endemic medicinal plants of Mauritius. Pharm. Biol. 2005, 43, 237–242. [Google Scholar] [CrossRef]
- Mahomoodally, M.F.; Gurib-Fakim, A.; Subratty, A.H. Screening for alternative antibiotics: An investigation into the antimicrobial activities of medicinal food plants of Mauritius. J. Food Sci. 2010, 75, 173–177. [Google Scholar] [CrossRef]
- Ranilla, L.G.; Kwon, Y.I.; Apostolidis, E.; Shetty, K. Phenolic compounds, antioxidant activity and in vitro inhibitory potential against key enzymes relevant for hyperglycemia and hypertension of commonly used medicinal plants, herbs and spices in Latin America. Bioresour. Technol. 2010, 101, 4676–4689. [Google Scholar] [CrossRef] [PubMed]
- Ravi-Kumar, A.; Ponnusamy, S.; Ravindran, R.; Zinjarde, S.; Bhargava, S. Evaluation of traditional Indian antidiabetic medicinal plants for human pancreatic amylase inhibitory effect in vitro. Evid. Based Complement. Altern. Med. 2011, 2011. [Google Scholar] [CrossRef]
- Administrative Map of Nigeria—Nations Outline Project. Available online: http://www.nationsonline.org (accessed on 2 February 2015).
- Lifongo, L.L.; Simoben, V.C.; Ntie-Kang, F.; Babiaka, B.S.; Judson, N.P. A bioactivity versus ethnobotanical survey of medicinal plants from Nigeria, West Africa. Nat. Prod. Bioprospect. 2014, 4, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Cragg, G.M.; Newmann, D.J.; Snader, K.M. Natural products in drug discovery and development. J. Nat. Prod. 1997, 60, 52–60. [Google Scholar] [CrossRef] [PubMed]
- Guadani, R.; Patel, J.; Prajapati, H.; Mehta, B.; Agrawal, S. Peristrophe bicalculata—A review. Pharmacogn. J. 2010, 2, 39–45. [Google Scholar]
- Abdulazeez, M.A.; Ibrahim, A.B.; Edibo, Z.Y.; Sidali, J.O.; Idris, H.O. Anti-trypanosomal effect of Peristrophe bicalyculata extract on Trypanosoma brucei brucei-infected rats. Asian Pac. J. Trop. Biomed. 2013, 3, 523–531. [Google Scholar] [CrossRef] [PubMed]
- Awulu, E.A.; Oniye, S.J.; Adelanwa, M.A. Phytochemical Screening and in vivo Antitrypanosomal Activity of Methanol Extracts of Peristrophe bicalyculata in Mice Infected with Trypanosoma evansi. Int. J. Sci. Technol. 2013, 3, 34–39. [Google Scholar]
- Nok, A.J.; Williams, S. Allium sativum—Induced death of African Trypanosomes. Parasitol. Res. 1996, 82, 634–637. [Google Scholar] [CrossRef] [PubMed]
- Alawa, J.P.; Jokthan, G.E.; Akut, K. Ethnoveterinary medical practice for ruminants in the sub-humid zone of northern Nigeria. Prev. Vet. Med. 2002, 54, 79–90. [Google Scholar] [CrossRef] [PubMed]
- Atawodi, S.E.; Bulus, T.; Ibrahim, S.; Ameh, D.A.; Nok, A.J.; Mamman, M.; Galadima, M. In vitro trypanocidal effect of methanolic extract of some Nigerian savannah plants. Afr. J. Biotechnol. 2003, 2, 317–321. [Google Scholar]
- Adeiza, A.A.; Maikai, V.A.; Hassan, F.B. Phytochemical screening and evaluation of some medicinal plants for their in vitro activities on Trypanosoma evansi. J. Med. Plants Res. 2009, 3, 315–318. [Google Scholar]
- Ogbadoyi, E.O.; Abdulganiyu, A.O.; Adama, T.Z.; Okogun, J.J. In vivo Trypanocidal activity of Annona senegalensis. Pers leaf extract against T. brucei brucei. J. Ethnopharmacol. 2007, 112, 85–89. [Google Scholar]
- Nwodo, N.J.; Brun, R.; Osadebe, P.O. In vitro and in vivo evaluation of the antitrypanosomal of fraction of Holarrhena africana. J. Ethnopharmacol. 2007, 113, 556–559. [Google Scholar] [CrossRef] [PubMed]
- Igoli, J.O.; Gray, A.I.; Clements, C.J.; Mouad, H.A. Anti-Trypanosomal Activity and cytotoxicity of some compounds and extracts from Nigerian Medicinal Plants. In Phytochemicals—Bioactivities and Impact on Health; Rasooli, I., Ed.; In Tech: Shanghai, China, 2011; pp. 375–388. [Google Scholar]
- Antia, R.E.; Olayemi, J.O.; Aina, O.O.; Ajaiyeoba, E.O. In vitro and in vivo animal model antitrypanosomal evaluation of ten medicinal plant extracts from south west Nigeria. Afr. J. Biotechnol. 2009, 8, 1437–1440. [Google Scholar]
- Sofowora, A. Medicinal Plants and Traditional Medicines in Africa; Spectrum Books LTD: Ibadan, Nigeria, 1990; p. 289. [Google Scholar]
- Sofowora, A. Research on Medicinal Plants and Traditional Medicine in Africa. J. Altern. Complement. Med. 1996, 2, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Onotu, C.S.; Musa, U.B.; Fajinmi, A.O.; Mazadu, M.R.; Shaida, S.S. Physiochemical evaluation of ethanolic root extract of Carissa spinarum (Wild Karanda) on Trypanosoma brucei brucei (Federe Strain) infected mice. Int. J. Pharm. Sci. Invent. 2013, 2, 18–26. [Google Scholar]
- Atawodi, S.E. Comparative in vitro trypanocidal activities of petroleum ether, chloroform, methanol and aqueous extracts of some Nigerian savannah plants. Afr. J. Biotechnol. 2005, 4, 177–182. [Google Scholar]
- Wurochekke, A.U.; Nuhu, N.; Anyanwu, G.O. Trypanocidal potential of Carrisa edulis in male wistar rats infected with T. congolense. Am. J. Res. Commun. 2014, 2, 234–244. [Google Scholar]
- Omale, J.; Omajali, J.B. Studies on some nutritional characteristics of the fruit and leaf of Sabaflorida (Benth) from Ibaji forest. Int. J. Nutr. Metab. 2010, 2, 011–026. [Google Scholar]
- Omale, J.; Joseph, J.E. Comparative evaluation of trypanocidal activities of Cissus multistriata and Saba florida (benth) leaf extracts. J. Biosci. Technol. 2011, 2, 197–204. [Google Scholar]
- Abedo, J.A.; Jonah, O.A.; Abdullahi, R.S.; Mazadu, M.R.; Idris, H.Y.; Muhammed, H.; Shettima, F.T.; Ombugadu, S.; Daudu, M.; Garba, J.; et al. Evaluation of trypanosomal activity of Tapinanthus globiferus and Gongronema latifolium on Trypanosoma congolense. Biosci. Res. 2013, 10, 20–28. [Google Scholar]
- Abubakar, A.; Ogbadoyi, E.O.; Okogun, J.I.; Gbodi, T.I.; Ibikunle, G.F. The identification of putative antitrypanosomal compounds in Tridax procumbens extracts. Int. J. Med. Aromat. Plants 2012, 2, 185–194. [Google Scholar]
- Cordell, G.A.; Quinn-Beattie, M.L.; Farnsworth, N.R. The potential of alkaloids in drug discovery. Phytother. Res. 2001, 15, 183–205. [Google Scholar] [CrossRef] [PubMed]
- Tasdemir, D.; Kaiser, M.; Brun, R.; Yardley, V.; Schmidt, T.J.; Tosun, F.; Ruedi, P. Antitrypanosomal and antileishmanial activities of flavonoids and their analogues: In vitro, in vivo, structure-activity relationship, and quantitative structure-activity relationship studies. Antimicrob. Agents Chemother. 2006, 50, 1352–1364. [Google Scholar] [CrossRef] [PubMed]
- Mamani-Matsuda, M.; Rambert, J.; Malvy, D.; Lejoly-Boisseau, H.; Daulouede, S.; Thiolat, P.; Coves, S.; Courtois, P.; Vincendeau, P.; Djavad, M.M. Quercetin induces apoptosis of Trypanosoma brucei gambiense and diseases the proinflammatory response of human macrophages. Antimicrob. Agent Chemother. 2004, 48, 924–929. [Google Scholar] [CrossRef]
- Ene, A.C.; Atawodi, S.E.; Apeh, Y.E.O. In vitro and in vivo antitrypanosomal effects of petroleum ether, chloroform and methanol extracts of Artemisia maritima Linn. Br. J. Pharm. Res. 2014, 4, 751–758. [Google Scholar] [CrossRef]
- Nwude, N.; Ibrahim, M.A. Plants used in traditional veterinary medical practice in Nigeria. J. Vet. Pharmacol. Ther. 1980, 3, 261–273. [Google Scholar] [CrossRef]
- Dalziel, J.M. Useful Plants of West Tropical Africa; Crown Agent for Overseas Governments: London, UK, 1937; pp. 462–463. [Google Scholar]
- Freiburghaus, F.; Kaminsky, R.; Nkuna, M.H.N.; Brun, R. Evaluation of African medicinal plants for their in vitro trypanocidal activity. J. Ethnopharmacol. 1996, 55, 1–11. [Google Scholar] [CrossRef]
- Atawodi, S.E.; Joseph-Idrisu, J.; Uche, S.N.; Yusufu, L.M.L. Phytochemical and Antitrypanosomal Studies of Different Solvents Extracts of Boswellia dalzielii. Int. J. Biol. 2011, 3, 179–184. [Google Scholar]
- Burkill, H.M. Families A–D. In The Useful Plants of West Tropical Africa; Royal Botanic Garden, Kew Publishing: London, UK, 1985; Volume 1, p. 960. [Google Scholar]
- Igoli, N.P.; Gray, A.I.; Clements, C.J.; Igoli, J.O.; Nzekwe, U.; Singla, R.K. Scientific Investigation of Antitrypanosomal Activity of Crateva adansonii DC Leaves Extracts. Indo Glob. J. Pharm. Sci. 2012, 2, 226–229. [Google Scholar]
- Nweze, N.E.; Fakae, L.B.; Asuzu, I.U. Trypanocidal activity of the ethanolic extract of Buchholzia coriacea seed. Niger. Vet. J. 2009, 29, 1–6. [Google Scholar]
- Okere, O.S.; Iliemene, U.D. Proximate Analysis, Phytochemical Screening and Antitrypanocidal Potentials of Bucholzia coriacea in Trypanosoma brucei brucei-Infected Mice. J. Pharm. Biol. Sci. 2014, 9, 69–77. [Google Scholar]
- Nweze, N.E.; Anene, B.M.; Asuzu, I.U. Investigation of the antitrypanosomal activity of Buchholzia coriacea seed extract against a field strain of Trypanosoma congolense. Afr. J. Tradit. Complement. Altern. Med. 2011, 8, 175–180. [Google Scholar] [PubMed]
- Igoli, J.O.; Ogaji, O.G.; Tor-Anyiin, T.A.; Igoli, N.P. Traditional Medicine Practices Amongst the Igede people of Nigeria. Part II. Afr. J. Tradit. CAM 2005, 2, 134–152. [Google Scholar]
- Johnson, T.O.; Omoniwa, B.P. In Vivo Trypanocidal Activity of Ethanolic Crude Extract and Phytochemical Fractions of Garcinia kola Seeds. Ann. Res. Rev. Biol. 2014, 4, 212–222. [Google Scholar] [CrossRef]
- Wurochekke, A.U.; Anyanwu, G.O. Antitrypanosomal activity of Anogeissus leiocarpus in rats infected with Trypanosoma brucei brucei. Int. Res. J. Biotechnol. 2012, 3, 005–009. [Google Scholar]
- Mann, A.; Ogbadoyi, E.O. Evaluation of Medicinal Plants from Nupeland for Their in Vivo Antitrypanosomal Activity. Am. J. Biochem. 2012, 2, 1–6. [Google Scholar] [CrossRef]
- Mann, A.; Ibrahim, K.; Oyewale, A.O.; Amupitan, J.O.; Fatope, M.O.; Okogun, J.I. Antimycobacterial Friedelane-terpenoid from the Root Bark of Terminalia Avicennioides. Am. J. Chem. 2011, 1, 52–55. [Google Scholar] [CrossRef]
- Ahmad, M.; Zaman, F.; Sharif, T.; Zabta, C.M. Antidiabetic and hypolipidemic effects of aqueous methanolic extract of Acasia nilotica pods in alloxan-induced diabetic rabbits. Scand. J. Lab. Anim. Sci. 2008, 35, 29–34. [Google Scholar]
- Ogbadoyi, E.O.; Garba, M.H.; Kabiru, A.Y.; Mann, A.; Okogun, J. Therapeutic evaluation of Acacia nilotica (Linn) stem bark extract in experimental African trypanosomiasis. Int. J. Appl. Res. Nat. Prod. 2011, 4, 11–18. [Google Scholar]
- Akinpelu, D.A.; Aitegoro, A.O.; Okoh, A.I. Studies on the biocidal and cell membrane disruption potential s of stem bark extracts of Afzelia africana. Biol. Res. 2009, 42, 339–349. [Google Scholar] [CrossRef] [PubMed]
- Banwo, G.O.; Abdullahi, I.; Duguryil, M. The antimicrobial activity of the stem-bark and leaf of Parkia clappertoniana Keay family Leguminosae against selected microorganism. Niger. J. Pharm. Res. 2004, 3, 16–22. [Google Scholar]
- Dsso, K.; N’guessan, B.B.; Bidie, A.P.; Gnangoran, B.N.; Meite, S.; N’guessan, D.; Yapo, A.P.; Ehile, E.E. Antidiarrhoeal activity of an ethanolic extract of the stem bark of Pilistigma reticulatum (Caesalpiniaceae) in rats. Afr. J. Tradit. Complement. Altern. Med. 2012, 9, 242–249. [Google Scholar] [PubMed]
- Abiodun, O.O.; Gbotosho, G.O.; Ajaiyeoba, E.O.; Brun, R.; Oduola, A.M. Antitrypanosomal activity of some medicinal plants from Nigerian ethnomedicine. Parasitol. Res. 2012, 110, 521–526. [Google Scholar] [CrossRef] [PubMed]
- Tona, L.; Ngimbi, N.P.; Tsakala, M.; Mesia, K.; Cimanga, K.; Apers, S. Antimalaria activity of 20 crude extracts from nine African medicinal plants used in Kinshasa, Congo. J. Ethnopharmacol. 1999, 68, 193–203. [Google Scholar] [CrossRef] [PubMed]
- Samy, R.P.; Ignacimuthu, S. Antibacterial activity of some folklore medicinal plants used by tribals in Western Ghats of India. J. Ethnopharmacol. 2000, 69, 63–71. [Google Scholar] [CrossRef] [PubMed]
- Tona, L.; Mesia, K.; Ngimbi, N.P.; Chrimwami, B.; Cimanga, K. In vivo antimalarial activity of Cassia occentalis, Morinda morindoides and Phyllanthus niruri. Ann. Trop. Med. Parasitol. 2001, 95, 47–57. [Google Scholar] [CrossRef]
- Chukwujekwu, J.C.; Coombes, P.H.; Mulholland, D.A.; Vanstaden, J. Emordin, an antibacterial anthraquinone from the roots of Cassia occidentalis. S. Afr. J. Bot. 2006, 72, 295–297. [Google Scholar] [CrossRef]
- Barminas, J.T.; Maina, H.M.; Ali, J. Nutrient content of Prosopis africana seeds. Plant Food Hum. Nutr. 1998, 52, 325–328. [Google Scholar] [CrossRef]
- Shaba, P.; Pandey, N.N.; Sharma, O.P.; Rao, J.R.; Singh, R.K. In vitro trypanocidal activity of methanolic extracts of Quercus borealis leaves and Zingiber officinale roots against Trypanosoma evansi. Greener J. Agric. Sci. 2011, 1, 41–47. [Google Scholar]
- Denise, M.; Barret, M.P. Uptake and mode of activity of drugs used against sleeping sickness. J. Biochem. Pharmacol. 2001, 61, 1–5. [Google Scholar] [CrossRef]
- Ada, G.A.; Claffey, H. Trees of Idoma Land; Dik Publishers: Otukpo, Nigeria, 2003; p. 177. [Google Scholar]
- Igoli, J.O.; Gray, L.A. Friedelanone and other triterpenoids from Hymenocardia acida. Int. J. Phys. Sci. 2008, 3, 156–158. [Google Scholar]
- Sofidiya, M.; Lange, C.; Sattler, L.; Beukes, D.; Afolayan, A.; Odukoya, O.; Familoni, O. Bioactivity profile of compounds isolated from Hymenocardia acida Tul. leaves. Planta Med. 2010, 76, 141. [Google Scholar] [CrossRef]
- Mpiana, P.T.; Tshibanga, D.S.T.; Shetonde, O.M.; Ngobula, K.N. In vitro antidrepanocytary activity (antisickle cell anaemia) of some Congolese plants. Phytomedicine 2007, 14, 192–195. [Google Scholar] [CrossRef] [PubMed]
- Mahmout, Y.; Mianpeurem, T.; Dolmazon, R.; Bouchu, D.; Fenet, B. phiphile triterpenoids from Hymenorcardia acida Tul. Phytoantimalarial and anti-inflammatory activities. In Proceedings of 15 ème colloque sur la pharmacopée et la Médecine Traditionnelles Africaines, Libreville, Gabon, 1–4 December 2008.
- Abu, A.H.; Uchendu, C.N. In vivo trypanocidal activity of hydroethanolic extract of Hymenocardia acida stem bark in rats. Vet. World 2011, 4, 113–116. [Google Scholar]
- Amom, T.T.; Yahwe, S.R.; Vershima, A.J. Phytochemical and medicinal activities of Hymenocardia acida Tul (Euphorbiaceae): A Review. J. Nat. Prod. Plant Resour. 2013, 3, 11–16. [Google Scholar]
- Abu, A.H.; Uchendu, C.N.; Ofukwu, R.A. In vitro anti trypanosomal activity of crude extracts of some Nigerian medicinal plants. J. Appl. Biosci. 2009, 21, 1277–1282. [Google Scholar]
- Umar, I.A.; Ene, O.; Okodaso, D.; Kimeng, E.; Stancheva, G.; Omage, J.J. Amelioration of anaemia and organ damage by combined intraperitoneal administration of Vitamins A and C to Trypanosome brucei brucei infected rats. Afr. J. Biotechnol. 2007, 6, 2083–2086. [Google Scholar]
- Umar, I.A.; Toh, Z.A.; Igbalajobi, F.I.; Igbokwe, I.O.; Gidado, A. The effect of orally administered vitamins C and E on the severity of anaemia in T. brucei-infected rats. Trop. Vet. 1999, 18, 71–77. [Google Scholar]
- Ibrahim, M.A.; Aliyu, A.B.; Sallau, A.B.; Bashir, M.; Yunusa, I.; Umar, T.S. Senna occidentalis leaf extract possesses antitrypanosomal activity and ameliorates the trypanosome- induced anemia and organ damage. Pharmacog. Res. 2010, 2, 175–180. [Google Scholar] [CrossRef]
- Lockett, C.T.; Grivetti, L.E. Food related behaviour during drought: A study of rural Fulani, North Eastern Nigeria. Int. J. Food Sci. Nutr. 2000, 51, 91–107. [Google Scholar] [CrossRef] [PubMed]
- Hoet, S.; Pieters, L.; Muccioli, G.G.; Jean-Louis, H.; Opperdoes, F.R.; Quetin-Leclercq, J. Antitrypanosomal activity of triterpenoids and sterols from the leaves of Strychnos spinosa and related compounds. J. Nat. Prod. 2007, 70, 1360–1363. [Google Scholar] [CrossRef] [PubMed]
- Hoet, S.; Stevigny, C.; Herent, M.F.; Quetin-Leclerc, J. Antitrypanosomal compounds from the leave essential oil of Strychnos spinosa. Planta Med. 2006, 72, 480–482. [Google Scholar] [CrossRef] [PubMed]
- Adesina, S.K.; Illoh, H.C.; Imoh, I.J.; Imoh, E.J. African Mistletoes (Lornthacaee); Ethnopharmacology, Chemsitry and Medicinal values: An Update. Afr. J. Tradit. Complement. Altern. Med. 2013, 10, 161–170. [Google Scholar] [PubMed]
- Inabo, H.I.; Fathuddin, M.M. In vivo antitrypanosomal potentials of ethyl acetate leaf extracts of Punicagra natum against Trypanosoma brucei brucei. Adv. Agric. Biotechnol. 2011, 1, 82–88. [Google Scholar]
- Ibrahim, H.M.; Ogbadoyib, E.O.; Bellob, M.U.; Yemisi, I. Evaluation of antitrypanosomal activity of Adansonia digitata (methanol seed extract) in Albino mice. J. Sci. J. Vet. Adv. 2013, 2, 1–6. [Google Scholar]
- Mann, A.; Gbate, M.; Nda-Umar, A. Medicinal and Economic Plants of Nupeland; Jube-Evans Books and Publications: Bida, Nigeria, 2003; p. 276. [Google Scholar]
- Gills, L.S. Ethnomedical Uses of Plants in Nigeria; University of Nigerian Press: Benin City, Nigeria, 1992; p. 103. [Google Scholar]
- Mann, A.; Egwim, E.C.; Banji, B.; Nda-Umar, A.; Mohammed, G.; Ekanem, J.T. Efficacy of Dissotis rotundifolia on Trypanosoma brucei brucei infection in rats. Afr. J. Biochem. Res. 2009, 3, 005–008. [Google Scholar]
- Tchoumbougnang, F.; Zollo, P.H.A.; Boyom, F.F.; Ngegae, M.A.; Bessiere, J.M.; Menut, C. Aromatic plants of tropical Central Africa. XLVIII. Comparative study of the essential oils of four Hyptis species from Cameroun: H. lancedata Poit, H. pectinata (L) Poit, Hyptis spicigera Lam and Hyptis suaveoleus Poit. Flavour Fragr. J. 2005, 20, 340–343. [Google Scholar] [CrossRef]
- Onayade, O.A.; Looma, A.; Scheffer, J.J.; Svendsen, A.B. Composition of the leaf essential oil Hyptis Spicigera Lam. Flavour Fragr. J. 1990, 5, 101–105. [Google Scholar] [CrossRef]
- Ladan, Z.; Amupitan, J.O.; Oyewale, O.A.; Okonkwo, E.M.; Ladan, E.O.; Odjobo, B.; Habila, N. Chemical composition and biological activity of the volatile oils of Hyptisspicigera against Trypanosoma brucei brucei, (Tbb) found in Northern Nigeria. Afr. J. Pure Appl. Chem. 2011, 5, 53–58. [Google Scholar]
- Arbonnier, M. Trees, Shrubs and Lianas of West African Dry Zones; Cirad Margraf Publishers: Wageningen, The Netherlands, 2002; pp. 189–426. [Google Scholar]
- Ibrahim, M.A.; Njoku, G.C.; Sallau, A.B. In vivo activity of stem barks aqueous extract of Khaya senegalensis against Trypanosoma brucei. Afr. J. Biotechnol. 2008, 7, 661–663. [Google Scholar]
- Umar, I.A.; Ibrahim, M.A.; Fari, N.A.; Isah, S.; Balogun, D.A. J. In-vitro and -vivo anti-Trypanosoma evansi activities of extracts from different parts of Khaya senegalensis. Cell Anim. Biol. 2010, 4, 91–95. [Google Scholar]
- Takin, M.C.; Attindehou, S.; Sezan, A.; Attakpa, S.E.; Baba-Moussa, L. Bioactivity, therapeutic utility and toxicological risks of Khaya senegalensis. Ind. J. Pharm. Biol. Res. 2013, 1, 122–129. [Google Scholar]
- Haruna, Y.; Kwanashie, H.O.; Anuka, J.A.; Atawodi, S.E.; Hussaini, I.M. Bioassay- guided fractionation and Anti-trypanosocidal effect of fractions and crude methanol roots extracts of Securidaca longepedunculata in mice and rats. Int. J. Mod. Biochem. 2013, 2, 1–14. [Google Scholar]
- Gbile, Z.O.; Adesina, S.K. Nigerian Flora and its pharmaceutical potentials. J. Ethnopharmacol. 1987, 19, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Alli, L.A.; Okochi, V.I.; Adesokan, A.A. Anti-trypanosomal activity and haematological effects of aqueous extract of leaves of Morinda lucida on Trypanosoma brucei brucei infected rats. Asian J. Pharm. Health Sci. 2011, 1, 111–115. [Google Scholar]
- Asuzu, I.U.; Chineme, C.N. Effects of Morinda lucida leaf extract on Trypanosoma brucei brucei infection in mice. J. Ethnopharmacol. 1990, 30, 307–313. [Google Scholar] [CrossRef] [PubMed]
- Edoga, C.O.; Njoku, O.O.; Amadi, E.N.; Afomezie, P.I. Effect of aqueous extract of Moringa oleifera on serum protein of Trypanosoma brucei-infected rats. Int. J. Sci. Technol. 2013, 3, 85–87. [Google Scholar]
- Adeyemi, O.S.; Akanji, M.A.; Oguntoye, S.A. Ethanolic leaf extract of Psidium guajava: Phytochemical and trypanocidal activity in rats infected with Trypanosoma brucei brucei. J. Med. Plant Res. 2009, 3, 420–423. [Google Scholar]
- Oluyomi, S.A.; Melissa, L.S.; Musbau, A.A.; Vicky, M.A. Anti-trypanosomal and cytotoxic activity of ethanolic extracts of Psidium guajava leaves in Alamar Blue based assays. Vet. Arh. 2011, 81, 623–633. [Google Scholar]
- Adeyemi, O.S.; Akanji, M.A.; Ekanem, J.T. Ethanolic extract of Psidium guajava influences protein and bilirubin levels in Trypanosome brucei brucei infested rats. J. Biol. Sci. 2012, 12, 111–116. [Google Scholar] [CrossRef]
- Kabiru, Y.A.; Ogbadoyi, E.O.; Okogun, J.I.; Gbodi, T.A.; Makun, H.A. Anti-trypanosomal Potential of Eucalyptus camaldulensis. Br. J. Pharmacol. Toxicol. 2013, 4, 25–32. [Google Scholar]
- Shyam, K.; Hrubiec, R.T.; Furubayashi, R.; Cosby, L.A.; Sartorelli, A.C. Methylating agents for use in the treatment of trypanosomiasis. J. Med. Chem. 1987, 30, 2157–2161. [Google Scholar] [CrossRef] [PubMed]
- Philip, G.P.; Alan, A.D.; Krishnamurthy, S.; Curtis, L.P.; Alan, C.S. The effects of the methylating agent 1,2-Bis (methylsulfonyl)-1-methylhydrazine on morphology, DNA content and mitochondrial function of Trypanosoma brucei subspecies. J. Eukaryot. Microbiol. 1991, 38, 172–177. [Google Scholar]
- Maikai, V.A.; VivMaikai, B.; Kobo, P.I. In vitro Effect of Aqueous Extract and Fraction IV Portion of Ximenia americana Stem Bark on Trypanosoma congolense DNA. J. Parasit. Res. 2014, 2014. [Google Scholar] [CrossRef]
- Peter, S.; Nandal, P.N.; Prakash, S.O.; Rao, J.; Kumar, S.P. In vitro antitrypanosomal evaluation of Picrorhiza kurroa rhibomes. J. Pharm. 2012, 3, 205–208. [Google Scholar]
- Hotellier, F.; Delaveau, P.; Pousset, J.L. Naucleidinal et epinaucleidinal, alcaloides du Nauclea latifolia. Phytochemistry 1980, 19, 1884–1885. [Google Scholar] [CrossRef]
- Cerri, R.; Aquino, R.; de Simone, F.; Pizza, C. New quinovic acid glycosides from Uncaria tomentosa. J. Nat. Prod. 1988, 51, 257–261. [Google Scholar] [CrossRef]
- Bero, J.; Beaufay, C.; Hannaert, V.; Hérent, M.F.; Michels, P.; Quetin-Leclercq, J. Antitrypanosomal compounds from the essential oil and extracts of Keetia leucantha leaves with inhibitor activity on Trypanosoma brucei glyceraldehyde- 3-phosphate dehydrogenase. Phytomedicine 2013, 203, 270–274. [Google Scholar] [CrossRef]
- Benjamin, T.V.; Anucha, T.C.; Hugbo, P.G. An approach to the study of medicinal plants with antimicrobial activity with reference to Mitracarpus scaber. In The State of Medicinal Plants Research in Nigeria; Sofowora, A., Ed.; Nigerian Society of Pharmacognosy, Ibadan University Press: Ibadan, Nigeria, 1986; pp. 243–245. [Google Scholar]
- Nok, A.J. Azaanthraquinone inhibits respiration and in vitro growth of long slender blood stream forms of Trypanosoma congolense. Cell Biochem. Funct. 2002, 203, 205–212. [Google Scholar] [CrossRef]
- Omale, J.; Okafor, P.N. Comparative antioxidant capacity, membrane stabilization, polyphenol composition and cytotoxicity of the leaf and stem of Cissus multistriata. Afr. J. Biotechnol. 2008, 7, 3129–3133. [Google Scholar]
- Nwodo, N.; Okoye, F.; Lai, D.; Debbab, A.; Kaiser, M.; Brun, R.; Proksch, P. Evaluation of the in vitro trypanocidal activity of methylated flavonoid constituents of Vitex simplicifolia leaves. BMC Complem. Altern. Med. 2015, 15, 82. [Google Scholar] [CrossRef]
- Nwodo, N.J.; Agbo, M.O.; Brun, R. In vitro and in vivo Antitrypanosomal studies of the leaf extract of Vitex simplicifolia. Afr. J. Pharm. Res. Dev. 2012, 4, 35–40. [Google Scholar]
- Weniger, B.; Vonthron-Sénécheau, C.; Kaiser, M.; Brun, R.; Anton, R. Comparative antiplasmodial, leishmanicidal and antitrypanosomal activities of several biflavonoids. Phytomedicine 2006, 13, 176–180. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nwodo, N.J.; Ibezim, A.; Ntie-Kang, F.; Adikwu, M.U.; Mbah, C.J. Anti-Trypanosomal Activity of Nigerian Plants and Their Constituents. Molecules 2015, 20, 7750-7771. https://doi.org/10.3390/molecules20057750
Nwodo NJ, Ibezim A, Ntie-Kang F, Adikwu MU, Mbah CJ. Anti-Trypanosomal Activity of Nigerian Plants and Their Constituents. Molecules. 2015; 20(5):7750-7771. https://doi.org/10.3390/molecules20057750
Chicago/Turabian StyleNwodo, Ngozi Justina, Akachukwu Ibezim, Fidele Ntie-Kang, Michael Umale Adikwu, and Chika John Mbah. 2015. "Anti-Trypanosomal Activity of Nigerian Plants and Their Constituents" Molecules 20, no. 5: 7750-7771. https://doi.org/10.3390/molecules20057750







